2% Xylocaine Dental with adrenaline (epinephrine) 1:80,000
Brand Information
| Brand name | 2% Xylocaine Dental with adrenaline (epinephrine) 1:80,000 |
| Active ingredient | Lidocaine (lignocaine) hydrochloride + Adrenaline (epinephrine) |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the 2% Xylocaine Dental with adrenaline (epinephrine) 1:80,000.
Summary CMI
2% Xylocaine® DENTAL with adrenaline (epinephrine) 1:80,000
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using Xylocaine DENTAL
The medicine, 2% Xylocaine DENTAL with adrenaline (epinephrine) 1:80000, is hereafter referred to as Xylocaine DENTAL in this leaflet.
Xylocaine DENTAL contains the active ingredients lidocaine (lignocaine) and adrenaline (epinephrine). It is used to prevent or relieve pain during dental procedures.
For more information, see Section 1. Why am I using Xylocaine DENTAL? in the full CMI.
2. What should I know before I use Xylocaine DENTAL?
Do not use if you have ever had an allergic reaction to lidocaine, adrenaline or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I use Xylocaine DENTAL? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with Xylocaine DENTAL and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How Xylocaine DENTAL is given?
Xylocaine DENTAL is injected by your dentist into the gum near nerves.
More instructions can be found in Section 4. How Xylocaine DENTAL is given? in the full CMI.
5. What should I know while being given Xylocaine DENTAL?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Drinking alcohol |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while being given Xylocaine DENTAL? in the full CMI.
6. Are there any side effects?
Tell your doctor or nurse as soon as possible if you do not feel well while you are being given Xylocaine DENTAL.
Some of these mild side effects include: nervousness, dizziness, blurred vision, drowsiness, ringing in ears, numbness, nausea and vomiting.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
2% Xylocaine® DENTAL with adrenaline (epinephrine) 1:80,000
Active ingredients: Lidocaine (lignocaine) and adrenaline (epinephrine)
Consumer Medicine Information (CMI)
This leaflet provides important information about using Xylocaine DENTAL with adrenaline (epinephrine) 1:80,000, hereafter referred to as Xylocaine DENTAL in this CMI.
You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using Xylocaine DENTAL.
Where to find information in this leaflet:
1. Why am I using Xylocaine DENTAL?
2. What should I know before I use Xylocaine DENTAL?
3. What if I am taking other medicines?
4. How Xylocaine DENTAL is given?
5. What should I know while being given Xylocaine DENTAL?
6. Are there any side effects?
7. Product details
1. Why am I using Xylocaine DENTAL?
Xylocaine DENTAL contains the active ingredients lidocaine (lignocaine) and adrenaline (epinephrine). Xylocaine DENTAL belongs to a group of medicines called local anaesthetics.
This medicine is used to prevent or relieve pain during dental procedures, but it will not put you to sleep.
It is injected into the mouth, where it makes the nerves unable to pass messages to the brain. Depending on the amount used, Xylocaine DENTAL will either totally stop pain or will cause a partial loss of feeling.
The adrenaline (also known as epinephrine) makes it last longer. Adrenaline (epinephrine) makes the blood vessels at the site of injection narrower, which means you bleed less and it is easier for your dentist to see what is happening.
Your dentist will have explained why you are being treated with Xylocaine DENTAL. Follow all directions given to you by your dentist carefully. They may differ from the information contained in this leaflet. Ask your dentist if you want more information.
Xylocaine DENTAL is not addictive.
2. What should I know before I use Xylocaine DENTAL?
Warnings
Do not use Xylocaine DENTAL if:
- you are allergic to lidocaine (lignocaine), adrenaline (epinephrine), or any of the ingredients listed at the end of this leaflet.
- the expiry date printed on the pack has passed.
- the solution is not clear, or the packaging is torn or shows signs of tampering.
If you have an allergic reaction, you may get a skin rash, hayfever, an asthma episode or feel faint.
Check with your doctor if you:
- have any other medical conditions
- problems with your blood pressure or circulation
- blood poisoning
- problems with the clotting of your blood
- nerve problems
- heart problems
- liver problems
- kidney problems
- malignant hyperthermia (history or experience of a rapid rise in body temperature to a dangerously high level)
It may not be safe for you to be given Xylocaine DENTAL if you have any of these conditions.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Talk to your doctor if you are pregnant or breastfeeding, or planning to. Your dental practitioner can discuss with you the risks and benefits involved.
Xylocaine DENTAL has been widely used during pregnancy and there have been no reports of any ill effects on the baby.
Your baby can take in very small amounts of Xylocaine DENTAL from breast milk if you are breastfeeding, but it is unlikely that the amount available to the baby will do any harm.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with Xylocaine DENTAL and affect how it works.
If you have not told your dentist about any of these things, tell them before you are given any Xylocaine DENTAL.
4. How Xylocaine DENTAL is given?
How much is given
The dosage you will be given will depend on your body size, age and the type of dental work you will be having done.
Your dentist will have had a lot of experience injecting Xylocaine DENTAL or other local anaesthetics and will choose the best dose for you. They will be willing to discuss this decision with you.
How it is given/administered
Xylocaine DENTAL will be injected by your dentist into the gum inside your mouth near a single nerve, or into an area that contains a large number of nerves.
This will result in an area of numbness at the site or near the site of injection.
Xylocaine DENTAL should not be injected directly into the blood.
If you are given too much Xylocaine DENTAL
The dentist giving you Xylocaine DENTAL will be experienced in the use of local anaesthetics, so it is unlikely that you will be given an overdose.
However, if you are particularly sensitive to Xylocaine DENTAL, or the dose is accidentally injected directly into your blood, you may develop problems for a short time. You may get a numb feeling in or around the mouth, feel dizzy or stiff, or have twitchy muscles.
Whenever you are given Xylocaine Dental, equipment will be available to care for you if an overdose happens.
If an overdose occurs, you should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
You may need urgent medical attention.
5. What should I know while being given Xylocaine DENTAL?
Things you should do
Remind any doctor, dentist or pharmacist you visit that you have been recently given Xylocaine DENTAL.
Things you should not do
Do not eat or drink anything until the feeling has returned to your mouth. You may burn or bite yourself.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how Xylocaine DENTAL affects you.
Xylocaine DENTAL may cause dizziness in some people. You may be drowsy and your reflexes may be slow.
Drinking alcohol
Tell your doctor if you drink alcohol.
If you drink alcohol while you are being given Xylocaine DENTAL your blood pressure may drop making you feel dizzy and faint.
Looking after your medicine
Xylocaine DENTAL will be stored by your dentist under the recommended conditions.
It should be kept in a fridge where the temperature stays at 2°C to 8°C (Refrigerate. Do not freeze) and it is protected from light.
Once removed from refrigeration for use, it will be stored below 25°C and used within 4 weeks and not returned to the refrigerator.
Excursions outside the recommended storage temperature are permitted during transport.
When to discard your medicine
Any Xylocaine Dental from a single dose which is not used, will be disposed of in a safe manner by your dentist.
Do not use this medicine after the expiry date.
6. Are there any side effects?
Tell your doctor or nurse as soon as possible if you do not feel well while you are being given Xylocaine DENTAL. All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention. Xylocaine DENTAL will help relieve pain in most people, but it may have unwanted side effects.
If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
| Speak to your doctor if you have any of these mild side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
If Xylocaine DENTAL is given wrongly, or you are very sensitive to it, it sometimes causes
| Call your doctor straight away, if you notice any of these serious side effects. You may need urgent medical attention or hospitalisation. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What Xylocaine DENTAL contains
| Active ingredients (main ingredients) |
|
| Other ingredients (inactive ingredients) |
|
| Potential allergens |
|
Do not take this medicine if you are allergic to any of these ingredients.
What Xylocaine DENTAL looks like
Xylocaine DENTAL is a clear, colourless, sterile solution for injection and is available as 2.2 mL dental cartridges in carton packs of 100 cartridges.
It contains the active ingredients: lidocaine (lignocaine) 17.3 mg/mL and adrenaline (epinephrine) 12.5 microgram/mL.
Australian Registration Number: AUST R 12024
Who sponsors/distributes Xylocaine DENTAL
Dentsply Sirona Pty Ltd
11 – 21 Gilby Road
Mount Waverley, VIC 3149
Australia
Tel: 1300 552 929
® Trade Mark herein is the property of the AstraZeneca group
This leaflet was revised in December 2025 (Version 4).
Brand Information
| Brand name | 2% Xylocaine Dental with adrenaline (epinephrine) 1:80,000 |
| Active ingredient | Lidocaine (lignocaine) hydrochloride + Adrenaline (epinephrine) |
| Schedule | S4 |
MIMS Revision Date: 01 May 2026
1 Name of Medicine
Lidocaine hydrochloride monohydrate.
Adrenaline (epinephrine) acid tartrate.
2 Qualitative and Quantitative Composition
2% Xylocaine Dental with Adrenaline (epinephrine) 1:80,000 contains: lidocaine hydrochloride monohydrate 46.9 milligram/2.2 mL, equivalent to lidocaine base 38.1 milligram/2.2 mL; adrenaline (epinephrine) acid tartrate 49.9 microgram/2.2 mL, equivalent to adrenaline (epinephrine) base 27.5 microgram 2.2 mL.
Lidocaine is classed as a membrane stabilising agent, and is a local anaesthetic of the amide type. Adrenaline (epinephrine) is a potent sympathomimetic.
Excipient with known effect. Sulfites.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
2% Xylocaine Dental with Adrenaline (epinephrine) 1:80,000 is a clear, colourless solution, practically free of visible particles, and is available in 2.2 mL standard and self-aspirating cartridges.
Note. 1. Adrenaline (epinephrine)-containing solutions contain the antioxidant sodium metabisulphite, 1.1 mg/2.2 mL.
2. All Dentsply Sirona Xylocaine dental cartridges (with adrenaline (epinephrine)) are paraben free and for single use in a single patient only. Remaining unused contents should be discarded.
4 Clinical Particulars
4.1 Therapeutic Indications
Lidocaine solutions are indicated for the production of local anaesthesia in routine dental procedures and oral surgery by means of infiltration and nerve block techniques.
Lidocaine solutions with adrenaline (epinephrine) are recommended for oral surgery requiring prolonged duration of anaesthesia and haemostasis.
4.2 Dose and Method of Administration
The lowest dosage that results in effective anaesthesia for the planned treatment should be used. The dosage will also depend on the area of the oral cavity to be anaesthetised, the vascularity of the oral tissues and the technique of anaesthesia.
Adults. See Table 1.

2. Safe dose. The safe dose for people with acute or chronic disease, especially those on medications, may be substantially less.
Paediatric. For children, the dose may have to be reduced commensurate with bodyweight.
4.3 Contraindications
1. Allergy or hypersensitivity to amide type local anaesthetics or other components of the injection solution which may be present e.g. sodium metabisulfite (see Section 3 Pharmaceutical Form, Note).
2. Local anaesthetic techniques must not be used when there is inflammation and/or sepsis in the region of the proposed injection.
The following are additional contraindications for solutions with adrenaline (epinephrine).
3. Solutions with adrenaline (epinephrine) should not be used in patients with a known sensitivity to sympathomimetic amines.
4. Solutions with adrenaline (epinephrine) should not be used in most patients with cerebral arteriosclerosis.
Also see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions.
4.4 Special Warnings and Precautions for Use
1. When any local anaesthetic agent is used, resuscitative equipment and drugs, including oxygen, should be immediately available in order to manage possible adverse reactions involving the cardiovascular, respiratory or central nervous systems.
2. Injection should always be made slowly with frequent aspirations to avoid inadvertent intravascular injection which can produce toxic effects. Multiple injections should be administered at spaced intervals.
3. The safety and effectiveness of lidocaine depend on proper dosage, correct technique and adequate precautions. Standard textbooks should be consulted regarding specific techniques and precautions for various anaesthetic procedures.
4. Lidocaine should be given with great caution to patients with severe bradycardia, cardiac conduction disturbances or severe digitalis intoxication.
5. Lidocaine and/or its metabolites may accumulate during prolonged or repeated administration in patients with hepatic, renal or cardiac diseases. However, this is unlikely to occur at the doses normally used in dentistry.
6. Adrenaline (epinephrine)-containing solutions should be used with extreme caution in patients with severe or untreated hypertension, arteriosclerotic heart disease, heart block, cerebral vascular insufficiency, thyrotoxicosis, advanced diabetes or any other pathological condition that might be aggravated by the effects of adrenaline (epinephrine). Adrenaline (epinephrine) may induce anginal pain in patients suffering from ischaemic heart disease. The use of Citanest-Octapressin solutions may be preferable in these conditions.
7. Lidocaine should be used with caution in patients with known drug sensitivities. Patients allergic to ester derivatives of para-aminobenzoic acid (procaine, tetracaine, benzocaine etc.) have not shown cross sensitivity to agents of the amide type.
8. Lidocaine should be used with caution in patients with genetic predisposition to malignant hyperthermia as the safety of amide local anaesthetic agents in these patients has not been fully established.
9. The patient should be advised to exert caution to avoid inadvertent trauma to the lips, tongue, cheek mucosa or soft palate when these structures are anaesthetised. Eating and drinking hot liquids should therefore be postponed until normal function returns.
10. Lidocaine with adrenaline (epinephrine) solutions contain sodium metabisulfite, a sulfite that may cause allergic type reactions including anaphylactic symptoms and life threatening or less severe asthmatic episodes in certain susceptible people. The overall prevalence of sulfite sensitivity in the general population is unknown and probably low. Sulfite sensitivity is seen more frequently in asthmatic than non-asthmatic people.
11. Local anaesthetics react with certain metals and cause the release of their respective ions which, if injected, may cause severe local irritation. Adequate precautions should be taken to avoid prolonged contact between lidocaine solutions and metal surfaces e.g. cartridges should not be preloaded and connected to needles until just prior to use.
12. Cartridges showing discolouration or cracks should be discarded. Adrenaline (epinephrine)containing solutions should not be autoclaved. Surface sterilisation using pure, undiluted isopropyl alcohol (91%) or 70% ethyl alcohol (USP) may be carried out if desired.
Use in the elderly. Although the dose of Xylocaine with Adrenaline (epinephrine) administered in dental practice is generally small, some patients e.g. the elderly and patients in poor general health, may require special attention to reduce the risk of dangerous side effects.
Paediatric use. See Section 4.2 Dose and Method of Administration.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
1. Antiarrhythmic drugs. Local anaesthetics of the amide type should be used with caution in patients receiving antiarrhythmic drugs e.g. mexiletine, or any other agents structurally related to local anaesthetics, since potentiation of cardiac effects may occur.
2. Amiodarone. Amiodarone has been reported to reduce the clearance of lidocaine in two case reports, although a small prospective study of combined therapy on lidocaine pharmacokinetics found no change in clearance or other pharmacokinetic factor.
This combination has been reported to precipitate seizures and to lead to severe sinus bradycardia and a long sinoatrial arrest. Until more experience with concurrent use of lidocaine and amiodarone becomes available, patients receiving the combination should be monitored carefully.
3. Anticonvulsive agents. Phenytoin and other antiepileptic drugs such as phenobarbitone, primidone and carbamazepine appear to enhance the metabolism of lidocaine but the significance of this effect is not known. Phenytoin and lidocaine have additive cardiac depressant effects.
4. Inhalational anaesthetics. Lidocaine decreases the minimum effective concentration of inhalational anaesthetics, e.g. nitrous oxide.
The following interactions may occur with adrenaline (epinephrine) containing solutions:
5. CNS acting drugs. Solutions containing adrenaline (epinephrine) should be used with extreme caution in patients receiving tricyclic antidepressants since severe hypertension may result, or phenothiazines and butyrophenones which may reduce or reverse the pressor effects of adrenaline (epinephrine), giving rise to hypotensive response and tachycardia.
6. Oxytocic drugs of the ergot type. Adrenaline (epinephrine)-containing solutions should not be used in the presence of oxytocic drugs of the ergot type as they are known to interact to produce severe, persistent hypertension and its subsequent sequelae.
7. Adrenergic neuron blocking agents. Solutions containing adrenaline (epinephrine) should be used with caution in the presence of adrenergic neuron blocking agents (e.g. guanethidine, debrisoquine, bethanidine).
8. Inhalation anaesthetics. Serious cardiac arrhythmias may occur if preparations containing adrenaline (epinephrine) are employed in patients during or following the administration of chloroform, halothane, cyclopropane, trichlorethylene, or other halogenated compounds.
9. Cardiac glycosides. Solutions containing adrenaline (epinephrine) may interact with cardiac glycosides resulting in arrhythmias.
10. Quinidine. Solutions with adrenaline (epinephrine) may interact with quinidine resulting in cardiac arrhythmias.
11. Hypoglycaemics. Adrenaline (epinephrine) induced hyperglycaemia may lead to loss of blood sugar control in diabetic patients treated with hypoglycaemic agents.
12. Beta-blockers. Noncardioselective beta-blockers such as propranolol enhance the pressor effect of adrenaline (epinephrine), which may lead to severe hypertension and bradycardia.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. No data available.
Use in pregnancy. (Category A)
The safe use of lidocaine during pregnancy has not been established. Lidocaine has, however, been used extensively for dental procedures during pregnancy with no reports of ill effects to mother or foetus.
Use in lactation. Lidocaine passes into breast milk. The amount of lidocaine appearing in breast milk from a nursing mother receiving parenteral lidocaine is unlikely to lead to a significant accumulation of the parent drug in the breastfed infant. The remote possibility of an idiosyncratic or allergic reaction in the breastfed infant from lidocaine remains to be determined.
4.7 Effects on Ability to Drive and Use Machines
Depending on dosage, local anaesthetics may have a very mild effect on mental function and may temporarily impair locomotion and coordination.
4.8 Adverse Effects (Undesirable Effects)
Reactions to lidocaine are very rare in the doses used in dental procedures. If adverse reactions occur, they are similar in character to those observed with other local anaesthetics of the amide type.
Adverse reactions may be due to high plasma levels as a result of excessive dosage, rapid absorption, delayed elimination or metabolism, or inadvertent intravascular injection. Such reactions are systemic in nature and involve the central nervous system and/or the cardiovascular system (see Section 4.9 Overdose). Pronounced acidosis or hypoxia may increase the risk and severity of toxic reactions.
The following adverse events have been observed during use of lidocaine medical injections and have not necessarily been associated with the dental use of lidocaine.
More common reactions. Nervousness, dizziness, blurred vision, tremor, drowsiness, tinnitus, numbness, disorientation, nausea and vomiting.
Less common reactions. More serious but less common reactions that reflect an overdosage of lidocaine are convulsions, unconsciousness, respiratory depression or arrest, hypotension, cardiovascular collapse and bradycardia which may lead to cardiac arrest.
Allergy. Allergy to amide type local anaesthetics is very rare but may present as allergic dermatitis, bronchospasm or anaphylaxis. However, sodium metabisulfite (which is in the adrenaline (epinephrine) containing products) may cause this type of reaction.
Neurological reactions. The incidence of adverse neurological reactions directly caused by the use of local anaesthetics is very low.
Neurological reactions may be related to the total dose of the local anaesthetic administered and are also dependent upon the particular drug used, the route of administration and the physical status of the patient. Many of these effects may be related to local anaesthetic techniques, with or without contribution from the drug.
Neurological reactions following regional nerve blocks have included persistent numbness, paraesthesia and sensory disturbances.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia) and 0800 764 766 (New Zealand).
Systemic toxicity to amide type local anaesthetics is initially manifested as CNS excitation and may result in a slow onset of nervousness, dizziness, blurred vision and tremors followed by drowsiness, convulsions, unconsciousness and possibly respiratory arrest.
Toxic cardiovascular reactions to local anaesthetics are usually depressant in nature, may occur rapidly and with little warning and can lead to peripheral vasodilation, hypotension, myocardial depression, bradycardia and possibly cardiac arrest.
Treatment of a patient with toxic symptoms consists of ensuring a patent airway and supporting ventilation with oxygen and assisted or controlled respiration as required. This usually will be sufficient in the management of most reactions.
Further treatment depends on diagnosis. Medical assistance should be summoned.
If convulsions occur, intravenous diazepam should be administered incrementally. Sodium thiopentone (5 mg/kg) may be used if diazepam is unavailable or ineffective. If convulsions interfere with breathing and/or are not rapidly controlled by specific anticonvulsant medication, suxamethonium (1-2 mg/kg) may be used to paralyse the patient. Artificial ventilation must then be instituted.
If ventricular fibrillation or cardiac arrest occurs, effective cardiovascular resuscitation treatment must be instituted and maintained for a prolonged period if necessary.
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Lidocaine stabilises the neuronal membrane and reversibly prevents the initiation and conduction of nerve impulses thereby producing local anaesthesia.
The onset and duration of anaesthesia depend on the route of administration and the dosage (volume and concentration) employed. The addition of adrenaline (epinephrine) reduces the rate of absorption of lidocaine from the site of injection, thereby increasing the duration of action.
Lidocaine is metabolised mainly in the liver and excreted via the kidneys. Approximately 90% of administered lidocaine is excreted in the form of various metabolites while less than 10% is excreted unchanged. Lidocaine has an elimination half-life of approximately 1.8 hours in healthy adults, depending on the site of injection.
Clinical trials. No data available.
5.2 Pharmacokinetic Properties
No data available.
5.3 Preclinical Safety Data
Genotoxicity. The genotoxic potential of 2,6-xylidine, a metabolite of lidocaine, has been studied with mixed results: Positive results were reported in assays for gene mutations (weakly positive in the Ames test with metabolic activation and in the mouse lymphoma assay) and chromosomal damage (chromosomal aberrations in Chinese hamster ovary cells at concentrations at which the drug precipitated from solution). No evidence of genotoxicity was found in in vivo assays for chromosomal damage (micronucleus assay) and DNA damage (unscheduled DNA synthesis).
Covalent binding studies of DNA from liver and ethmoid turbinates in rats indicate that 2,6-xylidine may be genotoxic under certain conditions in vivo.
Carcinogenicity. A two-year oral toxicity study of 2,6-xylidine, has shown that in both male and female rats, 2,6xylidine in daily doses of 900 mg/m2 (150 mg/kg) resulted in carcinomas and adenomas of the nasal cavity. No nasal tumours were observed in the low dose (15 mg/kg or control animals). In addition, the compound also caused subcutaneous fibromas and or fibrosarcomas in male and female rats (significant at 150 mg/kg).
6 Pharmaceutical Particulars
6.1 List of Excipients
2% Xylocaine Dental with Adrenaline (epinephrine) 1:80,000 contains sodium chloride, sodium metabisulfite, water for injections, and may contain sodium hydroxide and/or hydrochloric acid for pH adjustment.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
2% Xylocaine Dental with Adrenaline (epinephrine) 1:80,000 should be stored at 2°C to 8°C (Refrigerate. Do not freeze) and protected from light. Once removed from refrigeration for use, store below 25°C and use within 4 weeks. Do not return to refrigerator.
Excursions outside the recommended storage temperature are permitted during transport.
6.5 Nature and Contents of Container
See Table 2.

6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
Chemical structure. The chemical structure of lidocaine hydrochloride monohydrate is:
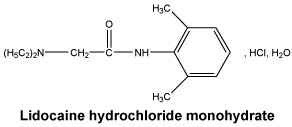
The Australian Approved Name (AAN) is lidocaine hydrochloride monohydrate.
Lidocaine base has a pKa of 7.85 (25°C) and a molecular weight of 234.3.
Lidocaine hydrochloride monohydrate is a white crystalline powder with a molecular weight of 288.8. It is very soluble in water and freely soluble in alcohol and chloroform. It must be protected from light.
The chemical structure of adrenaline (epinephrine) acid tartrate is:
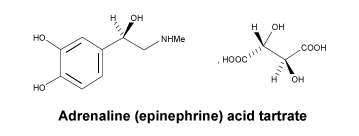
The Australian Approved Name is adrenaline (epinephrine) acid tartrate.
Adrenaline (epinephrine) acid tartrate is a white to greyish-white crystalline powder with a molecular weight of 333.3. It is freely soluble in water and slightly soluble in alcohol.
CAS number. The CAS number for lidocaine hydrochloride monohydrate is 6108-05-0.
The CAS number for adrenaline (epinephrine) acid tartrate is 51-42-3.
7 Medicine Schedule (Poisons Standard)
Australian Poisons Schedule: S4 - Prescription Only Medicine.
New Zealand Medicine Classification: Prescription Medicine.
Date of First Approval
13 August 1991
Date of Revision
24 March 2026
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.