Aerrane
Brand Information
| Brand name | Aerrane |
| Active ingredient | Isoflurane |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Aerrane.
Summary CMI
AERRANE
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor, nurse or pharmacist.
1. Why am I receiving AERRANE?
AERRANE contains the active ingredient isoflurane, a type of anaesthetic medicine. AERRANE is used to put and keep patients in a deep sleep during surgery (general anaesthesia).
For more information, see Section 1. Why am I receiving AERRANE? in the full CMI.
2. What should I know before I am given AERRANE?
Do not use if you have ever had an allergic reaction to isoflurane.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I am given AERRANE? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with AERRANE and affect how it works. A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How is AERRANE given?
- Your anaesthetist will give AERRANE through a specifically designed device that turns liquid to gas (vaporiser).
- They will decide how much AERRANE to use to put and keep you at the proper depth of sleep throughout your surgery.
- More instructions can be found in Section 4. How is AERRANE given? in the full CMI.
5. What should I know after having AERRANE?
| Things you should do |
|
| Driving or using machines |
|
| Drinking alcohol |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know after having AERRANE? in the full CMI.
6. Are there any side effects?
AERRANE can cause serious and less serious side effects. For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
If you experience any side effects, contact your doctor, nurse or pharmacist.
Full CMI
1. Why am I receiving AERRANE?
AERRANE contains the active ingredient isoflurane. It is a type of anaesthetic that you breathe in (inhale). It belongs to a group of medicines known as ‘halogenated anaesthetic agents’.
AERRANE is used to put and keep patients in a deep sleep during surgery (general anaesthesia).
It is given by your anaesthetist using a special device called a vaporiser. This device turns liquid into gas, which can then be inhaled. The vaporiser is specifically designed for use with AERRANE.
AERRANE wears off quickly when stopped, which means you wake up fast once your operation is over.
2. What should I know before I am given AERRANE?
Warnings
You should not be given AERRANE if:
- you are allergic or sensitive to isoflurane or anaesthetics known as ‘halogenated anaesthetic agents’
- you have been told by a doctor that you should not be given a general anaesthetic
- you have had, or anyone in your family has had, a condition called malignant hyperthermia (a rare type of severe fever)
- you have had any of the following problems after receiving a ‘halogenated anaesthetic agent’:
- a liver problem called hepatitis
- other liver problems that may have caused jaundice (yellowing of the skin), with an unexplained fever and/or low white or red blood cell count - you are delivering a baby
- you are taking monoamine oxidase inhibitors – special drugs used for depression
Check with your doctor if:
- you have previously had any problems with a general anaesthetic
- you have any other medical conditions, especially:
- any problems with your liver, including hepatitis
- myasthenia gravis, a rare disease that causes severe muscle weakness
- growth or abnormalities in your brain
- heart problems; for example, coronary artery disease, high or low blood pressure
- lung problems, for example asthma
- any problems with your nerves and muscles (neuromuscular disease) - you take any medicines for any other condition
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor if you are pregnant or intend to become pregnant.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
You should not breastfeed for at least 12 hours after receiving AERRANE
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with AERRANE and affect how it works.
- opioids or narcotic drugs like fentanyl or morphine
- sedatives like benzodiazepines, or any sort of sleeping tablets
- muscle-relaxing drugs
- monoamine oxidase inhibitors – special drugs used for depression
- drugs called beta-blockers, which are usually used to treat high blood pressure
- isoniazid, an antibiotic used for tuberculosis
- amphetamines like cocaine
- medicines with calcium antagonists (also called calcium channel blockers), used for high blood pressure or angina
- nitrous oxide – used for anaesthesia and pain relief
- St John's Wort – a herbal medicine used to manage depression
- medicines used in the treatment of severe heart problems like isoprenaline, adrenaline, or noradrenaline
- other medicines used in anaesthesia
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect AERRANE.
4. How is AERRANE given?
How it is given
- Your anaesthetist will give AERRANE through a specifically designed device that turns liquid to gas (vaporiser).
- They will place a mask over your mouth and nose, which allows you to inhale the medicine.
- Your anaesthetist closely monitors your vital signs to keep you safe and comfortable during surgery.
- When your surgery is finished, AERRANE is stopped, and you will wake up in the recovery area while nurses continue to monitor you until you are fully alert and stable.
How much is given
- Your anaesthetist will decide how much AERRANE to use to put and keep you at the proper depth of sleep throughout your surgery.
If too much AERRANE is used
AERRANE is used by your anaesthetist during surgery only, and it is unlikely that they will use too much (overdose).
Your anaesthetist can reduce the dose of AERRANE and provide oxygen if they assess that your depth of sleep is too deep.
5. What should I know after having AERRANE?
Things you should do
Talk to your doctor and surgeon about how you feel after your surgery.
Shivering, nausea and vomiting on waking are common after surgery and general anaesthesia. You may also have trouble thinking or changes in mood for several days after your surgery. Since AERRANE is given in a hospital, your healthcare team will monitor your progress and any side effects.
Remind any doctor, dentist or pharmacist you visit that you have received AERRANE during a previous surgery.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how AERRANE affects you.
AERRANE may affect your ability to drive or operate machinery. Avoid such tasks for 24 hours or longer after your surgery. Ask your doctor when you can return to work involving machinery or heavy equipment.
Leave the hospital with an accompanying adult who can ensure you get home safely.
Drinking alcohol
Avoid drinking alcohol following your procedure.
Ask your doctor when it will be safe to consume alcohol again.
Looking after your medicine
You will not have to store or handle this medicine.
This medicine is stored in the hospital pharmacy, below 30°C. Medical professionals handle and prepare it according to the manufacturer's instructions.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
AERRANE may cause a decrease in blood pressure and breathing rate. You will not know about these things since you will be asleep. Your anaesthetist will adjust the dose of AERRANE as necessary and will give other medicines if needed.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
Breathing and lung related
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
Signs of malignant hyperthermia
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people. Some side effects can only be detected by your doctor by physical examination, laboratory tests or scans.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
7. Product details
This medicine is only available with a doctor's prescription. It is only used in a hospital setting, during surgery.
What AERRANE contains
| Active ingredient (main ingredient) | isoflurane |
| Other ingredients (inactive ingredients) | none |
Do not take this medicine if you are allergic to any of these ingredients.
What AERRANE looks like
AERRANE is a clear, colourless liquid supplied in an amber coloured glass bottle. The bottle contains 1mL/mL of isoflurane in a 100 mL or 250mL bottle (Aust R 55105).
Not all bottle sizes may be marketed.
Who distributes AERRANE
Baxter Healthcare Pty Ltd
1 Baxter Drive
Old Toongabbie
NSW 2146
This leaflet was prepared in December 2025.
Brand Information
| Brand name | Aerrane |
| Active ingredient | Isoflurane |
| Schedule | S4 |
MIMS Revision Date: 01 March 2019
1 Name of Medicine
Isoflurane.
2 Qualitative and Quantitative Composition
Active ingredient: isoflurane 1 mL/mL.
3 Pharmaceutical Form
Liquid for inhalation. Isoflurane is a clear, colourless, stable volatile liquid containing no additives or chemical stabilisers: it has a mildly pungent, musty, ethereal odour. Isoflurane does not decompose in the presence of soda lime, and does not attack aluminum, tin, brass, iron or copper.
4 Clinical Particulars
4.1 Therapeutic Indications
Aerrane is a volatile halogenated anaesthetic for general inhalation anaesthesia.
4.2 Dose and Method of Administration
Isoflurane should be administered only by persons trained in the administration of general anaesthesia. Facilities for maintenance of a patent airway, artificial ventilation, oxygen enrichment, and circulatory resuscitation must be immediately available.
In order to be able to accurately control the precise concentration of Aerrane, vaporisers that have been specially designed and calibrated for isoflurane should be used. Dosage for induction and maintenance must be individualized and titrated to the desired effect according to the patient's age and clinical status.
With the exception of neonates, the minimum alveolar concentration (MAC) of isoflurane decreases with increasing patient age. Minimum alveolar concentration (MAC) of Aerrane in humans is shown in Table 1.
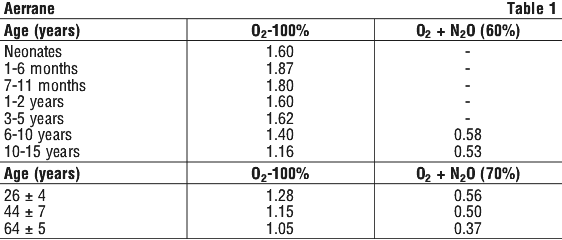
It is recommended that use be made of a hypnotic dose of a short acting barbiturate or another product such as propofol, etomidate, or midazolam in order to avoid coughing or laryngospasm, which can arise if induction is carried out with Aerrane alone or in combination with oxygen or with an oxygen/nitrous oxide mixture.
Maintenance of anaesthesia. Anaesthesia can be maintained during surgery using a concentration of 1.0-2.5% administered by inhalation, with the simultaneous administration of N2O and O2. A higher concentration of 1.5-3.5% of Aerrane is necessary if Aerrane is administered with pure oxygen.
Recovery. The concentration of Aerrane administered by inhalation must be reduced to 0.5% at the end of the operation, or to 0% during closure of the wound to allow prompt recovery. If all administration of anaesthetic agents has been stopped, the air passages of the patient should be ventilated several times with 100% oxygen until complete awakening occurs. If the vector gas is a mixture of 50% O2 and 50% N2O, the volume of the minimum alveolar concentration of Aerrane is approximately 0.65%.
4.3 Contraindications
Aerrane is contraindicated in those patients:
with known hypersensitivity to isoflurane or to other halogenated anaesthetics;
with known or suspected genetic disposition toward malignant hyperthermia;
with a history of malignant hyperthermia, or in whom liver dysfunction, jaundice or unexplained fever, leukocytosis and/or eosinophilia has occurred after a previous isoflurane or other halogenated anaesthetic administration;
with a history of confirmed hepatitis due to a halogenated inhalational anaesthetic;
in whom general anaesthesia is contraindicated;
undergoing an obstetric operation;
with concomitant nonselective MAOIs (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
4.4 Special Warnings and Precautions for Use
Aerrane must only be used by a licensed anaesthetist. Since the depth of anaesthesia can change easily and rapidly with Aerrane, only vaporisers that have been specially calibrated for this product may be used. The extent of blood pressure reduction and respiratory depression can be an indication of the extent or depth of anaesthesia; decreases may respond to reducing the inspired concentration of isoflurane.
Spontaneous respiration must be carefully and continuously monitored and must be assisted if necessary.
With the use of halogenated anaesthetics, disruption of the liver function, icterus, and fatal liver necrosis have been reported. Such reactions appear to indicate hypersensitivity reactions to anaesthetics. Cirrhosis, viral hepatitis, or other pre-existing liver disease can be a reason to select an anaesthetic other than a halogenated anaesthetic.
Relatively little metabolism of Aerrane occurs in the human body. In the postoperation period only 0.17% of the Aerrane taken up can be recovered as urinary metabolites. Peak serum inorganic fluoride values usually average less than 5 micromol/L and occur about four hours after anaesthesia, returning to normal levels within 24 hours. No signs of renal injury have been reported after Aerrane administration.
There is insufficient experience of use in repeated anaesthesia to make a definite recommendation in this regard. As with all halogenated anaesthetics repeat anaesthesia within a short period of time should be approached with caution.
It is recommended that ventilation be controlled in neurosurgery patients: cerebral blood flow remains unchanged in the course of light anaesthesia, but tends to rise in the course of deeper anaesthesia. An increase in intracranial pressure may be averted or abolished by hyperventilation of the subject before or during anaesthesia. Aerrane should not be administered to patients who can develop bronchoconstriction since bronchospasms can occur.
In the case of neurosurgical operations, respiration should be adequately checked. As with other halogenated anaesthetics, Aerrane increases the flow of blood through the brain and is accompanied by a transient increase in cerebrospinal fluid pressure. In most cases, this pressure increase can be prevented by hyperventilation.
In light of the fact that Aerrane acts in an irritating manner on the mucous membranes, the product is difficult to use if inhalation anaesthesia is applied via mask. During the induction of anaesthesia in children, saliva flow and tracheobronchial secretion can increase and can be the cause of laryngospasm.
In the case of patients who have undergone an abortion, an increased loss of blood has been found. A transient increase in bromsulfthalein retention, blood glucose and serum creatinine, with a decrease in the serum urea level, serum cholesterol level and alkaline phosphatase level, has been observed.
Malignant hyperthermia. In susceptible individuals, isoflurane anaesthesia may trigger a skeletal muscle hypermetabolic state in the skeletal muscle, leading to high oxygen consumption and the clinical syndrome known as malignant hyperthermia.
The clinical syndrome is signalled by hypercapnia and may include nonspecific features such as muscle rigidity, tachycardia, tachypnoea, cyanosis, arrhythmias, and/or unstable blood pressure. It should also be noted that many of these nonspecific signs may appear with light anaesthesia: acute hypoxia and hypovolaemia. An increase in overall metabolism may be reflected in an elevated temperature, (which may rise rapidly early or late in the case, but usually is not the first sign of augmented metabolism) and an increased usage of the CO2 absorption system (hot canister). PaO2 and pH may decrease, and hyperkalaemia and a base deficit may appear.
Treatment of malignant hyperthermia includes discontinuance of triggering agents (e.g. isoflurane), administration of intravenous dantrolene sodium, and application of supportive therapy. Such therapy includes vigorous efforts to decrease the patient’s body temperature, respiratory and circulatory support as indicated, and management of electrolyte-fluid-acid-base derangements (consult prescribing information for dantrolene sodium intravenous for additional information on patient management). Renal failure may appear later, and urine flow should be monitored and sustained if possible. Fatal outcome of malignant hyperthermia has been reported with isoflurane (see Section 4.3 Contraindications).
Perioperative hyperkalaemia. Use of inhaled anaesthetic agents has been associated with rare increases in serum potassium levels that have resulted in cardiac arrhythmias and death in paediatric patients during the postoperative period. Patients with latent as well as overt neuromuscular disease, particularly Duchenne muscular dystrophy, appear to be most vulnerable. Concomitant use of succinylcholine has been associated with most, but not all, of these cases. These patients also experienced significant elevations in serum creatinine kinase levels and, in some cases, changes in urine consistent with myoglobinuria. Despite the similarity in presentation to malignant hyperthermia, none of these patients exhibited signs or symptoms of muscle rigidity or hypermetabolic state. Early and aggressive intervention to treat the hyperkalaemia and resistant arrhythmias is recommended, as is subsequent evaluation for latent neuromuscular disease.
Hepatic reactions. Cases of mild, moderate, and severe postoperative hepatic dysfunction or hepatitis with or without jaundice, including fatal hepatic necrosis and hepatic failure, have been reported with isoflurane.
Such reactions can represent hypersensitivity hepatitis, a known risk of exposure to halogenated anaesthetics, including isoflurane. Clinical judgment should be exercised when isoflurane is used in patients with underlying hepatic conditions or under treatment with drugs known to cause hepatic dysfunction (see Section 4.3 Contraindications). As with all halogenated anaesthetics, repeated anaesthesia within a short period of time should be approached with caution.
Hypersensitivity reactions. Allergic type hypersensitivity reactions, including anaphylaxis, have been reported with isoflurane. Manifestations of such reactions have included hypotension, rash, difficulty breathing and cardiovascular collapse.
QT prolongation. Reports of QT prolongation, very rare associated with torsades de pointes, have been received. Caution should be exercised when administering isoflurane to susceptible patients.
General monitoring. All patients anesthetized with isoflurane should be continuously monitored (e.g. monitoring of the electrocardiogram, blood pressure, oxygen saturation, and end tidal CO2).
Respiratory reactions. Isoflurane is a profound respiratory depressant whose effect is accentuated by narcotic premedication or concurrent use of narcotics or other respiratory depressants. Excessive respiratory depression may be related to depth of anaesthesia and respond to decreasing the inspired concentration of isoflurane. The depressant effect is accentuated by concurrent use of narcotics and other respiratory depressants. Respiration should be closely monitored and assisted or controlled ventilation employed when necessary.
Patients with myasthenia gravis are extremely sensitive to drugs that produce respiratory depression. These effects are potentiated with some general anaesthetics. Aerrane should be used with caution in these patients.
Use in hypovolemic, hypotensive or haemodynamically compromised patients. Isoflurane causes a dose-dependent reduction in systemic vascular resistance and blood pressure. Particular care must be taken when selecting the dosage for patients who are hypovolemic, hypotensive, or otherwise haemodynamically compromised e.g. due to concomitant medications.
Use in patients with coronary artery disease. In patients with coronary artery disease, maintenance of normal haemodynamics is important in order to avoid myocardial ischaemia. Isoflurane, like some other coronary arteriolar dilators, can cause dose-dependent coronary vasodilation and has been shown to divert blood at the arteriolar level from collateral-dependent myocardium to normally perfused areas in selected animal models (“coronary steal”). The extent to which coronary steal occurs in patients with steal prone coronary anatomy is unclear. Clinical studies to date evaluating myocardial ischaemia, infarction and death as outcome parameters have not established that the coronary arteriolar dilation property of Aerrane is associated with coronary steal or myocardial ischaemia in patients with coronary artery disease. However, due to the phenomenon of coronary steal, isoflurane should be used with caution in patients with coronary artery disease. In particular, patients with subendocardial ischaemia may be considered to be more susceptible.
Use in patients with or at risk of elevations of intracranial pressure. In patients with or at risk for elevations of intracranial pressure (ICP), isoflurane should be administered cautiously and in conjunction with ICP reducing measures.
Reaction with CO2 absorbents. Aerrane, as with other halogenated anaesthetics, has been reported to interact with dry carbon dioxide absorbents to form carbon monoxide. In order to minimise the risk of formation of carbon monoxide in rebreathing circuits and the possibility of elevated carboxyhaemoglobin levels, fresh (moist) carbon dioxide absorbents should be used. In addition, consideration should be given to direct measurement of carboxyhaemoglobin levels in patients on closed circuit anaesthesia with isoflurane, if oxygen desaturation develops which does not respond to usual corrective steps.
Barium hydroxide lime and soda lime become desiccated when fresh gases are passed through the CO2 absorber canister at high flow rates over many hours or days. When a clinician suspects that CO2 absorbent may be desiccated, it should be replaced before the administration of isoflurane.
The colour indicator of most CO2 absorbents does not necessarily change as a result of desiccation. Therefore, the lack of significant colour change should not be taken as an assurance of adequate hydration. CO2 absorbents should be replaced routinely regardless of the state of the colour indicator, following current guidelines for use of anaesthesiology equipment.
Decrease in intellectual function. Isoflurane may cause a decrease in intellectual function as well as changes in mood for several days after general anaesthesia.
General. The following reactions have been reported following occupational exposure to isoflurane: dyspnoea, bronchospasm, stridor, cough, dizziness, paresthesia, hepatic reactions, flushing, rash, contact dermatitis, erythema, periorbital oedema, eye irritation, conjunctival hyperaemia, and headache (see Section 4.8 Adverse Effects (Undesirable Effects)).
Use in the elderly. No data available.
Paediatric use. Paediatric neurotoxicity. Some published studies in children have observed cognitive deficits after repeated or prolonged exposures to anaesthetic agents early in life. These studies have substantial limitations, and it is not clear if the observed effects are due to the anaesthetic/analgesic/sedation drug administration or other factors such as the surgery or underlying illness.
Published animal studies of some anaesthetic/analgesic/sedation drugs have reported adverse effects on brain development in early life and late pregnancy. The clinical significance of these nonclinical finding is yet to be determined.
With inhalation or infusion of such drugs, exposure is longer than the period of inhalation or infusion. Depending on the drug and patient characteristics, as well as dosage, the elimination phase may be prolonged relative to the period of administration.
Effects on laboratory tests. The effect of this medicine on laboratory tests has not been established.
4.5 Interactions with Other Medicines and Other Forms of Interactions
The simultaneous administration of Aerrane and the following products requires strict supervision of the clinical and biologic condition of the patient.
Opioids. Opioids decrease the minimum alveolar concentration (MAC) of isoflurane. Opioids such as fentanyl and its analogues, when combined with isoflurane, may lead to a synergistic fall in blood pressure and respiratory rate.
Nitrous oxide. N2O decreases the MAC of isoflurane (see Section 4.2 Dose and Method of Administration).
Neuromuscular blocking agents. Isoflurane decreases the required doses of neuromuscular blocking agents. If added relaxation is required, supplemental doses of muscle relaxants may be used.
St John's wort. Severe hypotension and delayed emergence from anaesthesia with halogenated inhalational anaesthetics have been reported in patients treated long-term with St John's wort.
Contraindicated combination. Nonselective monoamine oxidase inhibitors (MAOIs). Risk of haemodynamic instability and crisis during the operation or medical procedure. Treatment should be stopped 15 days prior to surgery.
Combinations advised against. Beta-sympathomimetics (isoprenaline) and alpha- and beta-sympathomimetics (adrenaline; noradrenaline). Risk of serious ventricular arrhythmia as a result of an increase in heart rate.
Combinations requiring precautions in using. In the majority of cases where a drug treatment is indispensable, there is no reason to suspend it before general anaesthesia. It suffices to inform the anaesthetist about it.
Beta-blockers. Concomitant use may exaggerate the cardiovascular effects of inhalational anaesthetics as there is a risk of blockage of the cardiovascular compensation mechanism, resulting in intensified hypotension and negative inotropic effects (see Section 4.4 Special Warnings and Precautions for Use). The action of beta-blockers can be suppressed during the operation with the use of beta-sympathomimetic agents. In general, any medication with a beta-blocker need not be stopped but any abrupt reductions of the dosage should be avoided.
Isoniazid. Risk of potentiating the hepatotoxic effect, with increased formation of toxic metabolites of isoniazid. Treatment with isoniazid should be suspended one week before the operation and should not be resumed until 15 days afterward.
Adrenaline utilised for its local haemostatic action, by subcutaneous or gingival injections. Risk of multiple and serious ventricular arrhythmia as a consequence of increased heart rate. Isoflurane is similar to sevoflurane in myocardium sensitisation to the arrhythmogenic effect of exogenous adrenaline, whereas myocardial sensitivity with adrenaline is lower with Aerrane than with other halogenated anaesthetics. Doses of adrenaline greater than 5 microgram/kg, when administered submucosally, may produce multiple ventricular arrhythmias. Thus, the dosage should be limited to, for example, 0.1 mg adrenaline within 10 minutes or 0.3 mg within one hour in adults.
Indirect sympathomimetics (amphetamines and their derivatives; psychostimulants, appetite suppressants, ephedrine and its derivatives). Risk of intraoperative hypersensitivity episode. In the case of a planned operation, it is preferable to interrupt the treatment a few days before the operation.
Muscle relaxing agents. Concomitant use increases the risk of intensification of the action of depolarising relaxants and in particular, non-depolarising relaxants. The disappearance of the myoneural effect takes longer with Aerrane than with other conventional anaesthetics. If such combinations are used and additional relaxation is required, supplemental doses of muscle relaxants should be administered with caution.
Neuromuscular blocking agents. In general, isoflurane decreases the required doses of neuromuscular blocking agents; it is recommended that approximately 1/3 to 1/2 of the usual dose of these substances is administered. Anaesthetic concentrations of isoflurane at equilibrium reduce the ED95 of succinylcholine, atracurium, pancuronium, rocuronium and vecuronium by approximately 25-40% or more compared to N2O/ opioid anaesthesia.
Neostigmine has an effect on the non-depolarising relaxants, but has no effect on the relaxing action of Aerrane itself.
Morphine analgesics. These products potentiate the depressive action of Aerrane on respiration.
Calcium antagonists. Aerrane may lead to marked hypotension in patients treated with calcium antagonists, particularly dihydropyridine derivatives.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. No data available.
Use in pregnancy. (Category B3)
All general anaesthetics cross the placenta and carry the potential to produce central nervous system and respiratory depression in the newborn infant. In routine practice, this does not appear to be a problem, however, in the compromised foetus, careful consideration should be given to this potential depression and to the selection of anaesthetic drugs, doses and techniques.
Isoflurane exerts a relaxant effect on uterine smooth muscle. This can lead to increased blood loss in situations where uterine muscle contraction aids haemostasis such as in obstetric surgery and in patients undergoing abortions or uterine curettage.
Concerning the use of this substance in pregnancy, in the case of humans, adequate data do not exist in order to judge possible injuriousness. In regards to effects in animal tests, in published fetal rhesus macaque studies, isoflurane exposed in utero, resulted in increased neuronal and oligodendrocyte apoptosis in developing brain of the offspring. Studies in juvenile animals suggest neuroapoptosis correlates with long-term cognitive deficits.
Published animal studies of some anaesthetic/analgesic/sedation drugs have reported adverse effects on brain development in early life and late pregnancy.
Published studies in pregnant and juvenile animals demonstrate that the use of anaesthetic/analgesic and sedation drugs that block NMDA receptors and/or potentiate GABA activity during the period of rapid brain growth or synaptogenesis may result in neuronal and oligodendrocyte cell loss in the developing brain and alterations in synaptic morphology and neurogenesis when used for longer than 3 hours. These studies included anaesthetic agents from a variety of drug classes. In light of the fact that it has not been established that Aerrane can be used safely in pregnant women, the use of this product must be avoided during pregnancy.
Insufficient information is available to recommend use in pregnancy or obstetrics.
Use in lactation. Breast feeding should not be given for up to 12 hours after the termination of anaesthesia. Because there is insufficient information regarding the excretion of isoflurane in human milk, the potential risks and benefits for each specific patient should be carefully considered before isoflurane is administered to nursing women.
4.7 Effects on Ability to Drive and Use Machines
Following anaesthesia with Aerrane, patients should be advised that performance of activities requiring mental alertness may be impaired for some time. Patients must not undertake hazardous tasks such as driving or operating machinery for at least 24 hours following administration of a general anaesthetic. The patient should only be sent home with an escort and should not consume any alcohol.
4.8 Adverse Effects (Undesirable Effects)
The following adverse reactions were identified from controlled clinical studies of adult and paediatric patients using a variety of premedications, other anaesthetics and surgical procedures of varying lengths.
Cardiac disorders. Intraoperative arterial hypotension or hypertension: this was dependent on the dose; postoperative hypotension (uncommon); postoperative hypertension (rare).
Increase in heart rate: this was intensified in case of the existence of hypercapnia. Serious ventricular rhythm disorders, including arrhythmias (postoperatively) and atrial, ventricular or nodal arrhythmias (intraoperatively), can arise commonly.
Respiratory, thoracic, and mediastinal disorders. The pungency of Aerrane can give rise to an irritating action on the mucous membranes during the induction of anaesthesia, which can be accompanied by respiratory depression, coughing (very common), secretions (uncommon), and a tendency toward laryngospasm (common) or bronchospasm (rare). Breath-holding was very commonly observed.
Hepatobiliary disorders. Disturbance of the liver function and liver damage (including blood bilirubin increased, alanine aminotransferase increased, aspartate aminotransferase increased, blood alkaline phosphatase increased, bromsulphthalein clearance decreased and blood lactate dehydrogenase increased), and jaundice were observed.
Metabolism and nutrition disorders. Blood glucose increased.
General disorders and administration site conditions. Chills/ shivering (very common); asthenia and fatigue; malignant hyperthermia (see Section 4.4 Special Warnings and Precautions for Use).
Psychiatric disorders. Delerium (common); mood changes and nightmares (uncommon); confusional state and nervousness.
Nervous system disorders. Agitation during induction (very common); movements during maintenance (common); convulsive pattern on ECG (uncommon); seizures (rare); ataxia, intellectual function decreased, dizziness and drowsiness.
Gastrointestinal disorders. Nausea on recovery (very common); vomiting on induction (uncommon) or recovery (common); and retching during induction (uncommon), maintenance (uncommon) or postoperatively.
Blood and lymphatic system disorders. The number of white blood cells increased very commonly (postoperatively), even in the absence of surgical stress.
Skin and subcutaneous tissue disorders. Diaphoresis (uncommon); rash.
Musculoskeletal connective tissue and bone disorders. Myalgia.
The following adverse reactions have been reported in postmarketing experience.
Blood and lymphatic system disorders. Carboxyhaemoglobin increased.
Immune system disorders. Anaphylactic reaction.
Metabolism and nutrition disorders. Hyperkalaemia.
Psychiatric disorders. Withdrawal syndrome (following multi-day exposure; symptoms included seizure, hallucination, ataxia, agitation, confusion).
Nervous system disorders. Brain oedema, intracranial pressure increased, migraine, myoclonus, nystagmus, pupils unequal, headache.
Cardiac disorders. Cardiac arrest, ventricular fibrillation, torsades de pointes, myocardial infarction, myocardial ischaemia, atrioventricular block complete, atrioventricular block second degree, atrial fibrillation, ECG QT prolonged, atrioventricular block first degree, ventricular tachycardia, ventricular extrasystoles, tachycardia, bradycardia, cardiac output decreased.
Vascular disorders. Flushing.
Respiratory, thoracic, and mediastinal disorders. Apnoea, hypoxia, bronchospasm, airway obstruction, respiratory depression, hypercapnia, stridor, hiccups.
Gastrointestinal disorders. Pancreatitis.
Hepatobiliary disorders. Hepatic failure, hepatic necrosis, hepatitis fulminant, cholestatic hepatitis, hepatitis, hepatic steatosis, jaundice, gammaglutamyltransferase increased.
Skin and subcutaneous tissue disorders. Rash.
Musculoskeletal, connective tissue and bone disorders. Rhabdomyolysis.
Renal and urinary disorders. Acute renal failure**, oliguria**.
General disorders and administration site conditions. Malignant hyperthermia, hypothermia.
Injury, poisoning, and procedural complications*. Unwanted awareness during anaesthesia, dyspnoea, bronchospasm, stridor, cough, dizziness, paresthesia, hepatic reactions, flushing, rash, contact dermatitis, erythema, periorbital oedema, eye irritation, conjunctival hyperaemia, headache.
*All reactions categorized in this section, with the exception of unwanted awareness during anaesthesia, were from occupational exposure in non-patients.
**Cases of acute renal failure and oliguria have been reported after isoflurane anaesthesia. These events may be secondary to hypotension or other effects of isoflurane.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
In case of overdosage, stop administration of the anaesthetic agent, check whether air passages are open, and depending on the circumstances, continue with assisted or controlled respiration using pure oxygen. Support and maintain adequate haemodynamics. For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Aerrane is an inhalation type anaesthetic, belonging to the group of halogenated anaesthetics. Induction and recovery from anaesthesia rapidly take place with Aerrane.
Aerrane has the slightly irritating odour of ether, which can limit the speed of induction.
Pharyngeal and laryngeal reflexes are rapidly diminished as a result of which tracheal intubation is rendered easy.
Clinical trials. No data available.
5.2 Pharmacokinetic Properties
Aerrane is metabolised minimally in comparison to other halogenated anaesthetics such as enflurane or halothane. On average, 95% of the Aerrane is recovered in the expired air; 0.2% of the Aerrane that is taken up with the body is metabolised. The principal metabolite is trifluoroacetic acid. The average serum level of inorganic fluoride in patients administered Aerrane anaesthesia is between 3 and 4 micromol/L.
In patients anaesthetised with Aerrane, the mean peak serum concentration of inorganic fluorides is usually less than 5 micromol/L and occurs about four hours after anaesthesia, returning to normal levels within 24 hours. This should not alter renal function in a normal subject.
5.3 Preclinical Safety Data
Genotoxicity. No data available.
Carcinogenicity. No data available.
6 Pharmaceutical Particulars
6.1 List of Excipients
None.
6.2 Incompatibilities
No data available.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 30°C. Store bottle in an upright position. To avoid leakage, apply bottle cap firmly but not too tightly. Aerrane must be kept in the original container until immediately prior to use.
6.5 Nature and Contents of Container
Aerrane is supplied in amber coloured glass bottles.
Pack size. 100 mL* and 250 mL.
*Not all packs are marketed.
6.6 Special Precautions for Disposal
In Australia, any unused product or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
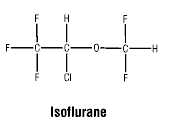
Active ingredient: isoflurane. Chemical Name: 1-chloro-2,2,2-trifluoroethyl difluoromethyl ether. Molecular Formula: C3H2ClF5O.
Some physical constants are the following. Molecular weight: 184.5; boiling point at 760 mmHg: 48.5°C (uncorr.); refractive index: 1.2990-1.3005; specific gravity 25°/25°C: 1.496; vapour pressure (mmHg): (20°C) 238, (25°C) 295, (30°C) 367, (35°C) 450.
Chemical structure.
7 Medicine Schedule (Poisons Standard)
S4.
Date of First Approval
01 July 1996
Date of Revision
07 November 2018
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.