Alimta
Brand Information
| Brand name | Alimta |
| Active ingredient | Pemetrexed |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Alimta.
Summary CMI
ALIMTA®
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using ALIMTA?
ALIMTA contains the active ingredient pemetrexed disodium heptahydrate. ALIMTA is used to treat different types of lung cancer.
For more information, see Section 1. Why am I using ALIMTA? in the full CMI.
2. What should I know before I use ALIMTA?
Do not use if you have ever had an allergic reaction to pemetrexed disodium heptahydrate or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I use ALIMTA? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with ALIMTA and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use ALIMTA?
- Your doctor will decide the dosage of ALIMTA that you are given. This will depend on your condition, if you have experienced any side effects, and other factors, such as your weight
- ALIMTA is given as an infusion (drip) into your veins over a 10-minute period by your doctor or nurse.
More instructions can be found in Section 4. How do I use ALIMTA? in the full CMI.
5. What should I know while using ALIMTA?
| Things you should do |
|
| Driving or using machines |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using ALIMTA? In the full CMI.
6. Are there any side effects?
Common side effects may include fatigue, nausea, vomiting, diarrhoea, mouth ulcers, being more prone to infections and bruising. Serious side effects may include inflammation of the large intestines, severe skin/allergic reactions, chest infection, kidney impairment or liver impairment.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? In the full CMI.
Full CMI
1. Why am I using ALIMTA?
ALIMTA contains the active ingredient pemetrexed disodium heptahydrate.
ALIMTA belongs to a group of medicines called cytotoxic or antineoplastic agents. They may also be called chemotherapy medicines.
It affects enzymes within cancer cells to kill cancer cells or prevent them growing and multiplying.
ALIMTA is used to treat:
- mesothelioma, a rare cancer of the lungs often related to exposure to asbestos.
- non-small cell lung cancer, a type of lung cancer.
2. What should I know before I use ALIMTA?
Warnings
Do not use ALIMTA if:
- you are allergic to any medicine containing pemetrexed disodium heptahydrate, or any of the ingredients listed at the end of this leaflet. Always check the ingredients to make sure you can use this medicine.
Check with your doctor if you:
- have kidney problems. Depending on the severity of your condition, your doctor may choose not to treat you with ALIMTA.
- have high blood pressure or diabetes as these conditions may increase your risk of developing kidney problems while being treated with ALIMTA.
- have heart problems or other cardiovascular risk factors (such as high cholesterol levels, are a smoker) as these may increase your risk of experiencing a heart attack or stroke while being treated with ALIMTA.
- have had radiation therapy (radiotherapy) as this may increase your risk of developing a lung condition called 'radiation pneumonitis' or a skin condition called 'radiation recall' while being treated with ALIMTA.
- have a build-up of fluid between your lungs and chest (called 'pleural effusion') or in your abdomen (belly) (called 'ascites'). Your doctor may choose to drain the excess liquid before starting treatment with ALIMTA.
- are taking non-steroidal anti-inflammatory drugs (e.g. aspirin, ibuprofen). Your doctor may choose to delay treatment with ALIMTA.
Tell your doctor if you are scheduled for any vaccinations or have recently been vaccinated. Some vaccines (live vaccines) should not be given while you are being treated with ALIMTA. Check with your doctor before receiving any vaccines.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Tell your doctor if you are pregnant or intend to become pregnant.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
Pregnancy and breastfeeding should be avoided during treatment with ALIMTA. Your doctor can discuss with you the risks and benefits involved.
Children 18 years of age and under
ALIMTA is not recommended for use in children under the age of 18 years.
The safety and effectiveness in children younger than 18 years have not been established.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with ALIMTA and affect how it works.
Medicines that may increase the effect of ALIMTA include:
- medicines used to treat arthritis or pain from inflammation such as ibuprofen or other non-steroidal anti-inflammatory medicines (NSAIDs).
- medicines used to treat heartburn and acid regurgitation such as omeprazole, esomeprazole, lansoprazole, pantoprazole and rabeprazole (proton pump inhibitors).
- medicines used to treat infections such as penicillin.
- medicines used to treat gout or gouty arthritis such as probenecid.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect ALIMTA.
4. How do I use ALIMTA?
How much to use
Your doctor will decide the dosage of ALIMTA that you are given. This will depend on your condition, if you have experienced any side effects, and other factors, such as your weight and height.
When to use ALIMTA
ALIMTA is given once every three weeks (one treatment cycle). Your doctor will advise how many treatment cycles you need.
Before each infusion you will have samples of your blood taken to check that you have enough blood cells to receive ALIMTA. Your doctor may decide to change your dose or delay treating you depending on your general condition and if your blood cell counts are too low.
How ALIMTA will be given
ALIMTA is given as an infusion (drip) into your veins over a 10-minute period.
Never inject ALIMTA yourself.
Your doctor or nurse will inject ALIMTA for you.
When treating certain cancers, you may also be given other chemotherapy medicines.
If you use too much ALIMTA
As ALIMTA is given to you under the supervision of your doctor, it is unlikely that you will use too much.
However, if you suspect that you have been given too much you may:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know while using ALIMTA?
Premedication
Your doctor should advise you to take certain medicines or vitamin while taking ALIMTA. These may help to minimise side effects.
Your doctor should advise you to take a folate supplement or a multivitamin containing folate once daily for at least five days in the week before your first ALIMTA dose. This should be continued throughout your treatment cycles and for at least three weeks following completion of ALIMTA treatment.
Your doctor should advise you to have a vitamin B12 injection during the week before your first dose of ALIMTA. Additional vitamin B12 injections should be given once every three treatment cycles.
Your doctor may advise you to take an oral corticosteroid such as dexamethasone to reduce the likelihood and severity of skin rashes.
Your doctor may advise you to take a medicine to help reduce nausea (antiemetic).
Your doctor may also advise you to receive an infusion (drip) of fluid into your veins for hydration.
Things you should do
- If you become pregnant while receiving this medicine, tell your doctor immediately.
- Remind any doctor, dentist or pharmacist you visit that you are using ALIMTA.
- If you are going to have surgery, tell the surgeon or anaesthetist that you are using ALIMTA. It may affect other medicines used during surgery.
- If you are about to have any blood tests, tell your doctor that you are using ALIMTA.
- Keep all your doctor's appointments so that your progress can be checked. Your doctor may do some tests from time to time to make sure the medicine is working and to prevent unwanted side effects.
- Take your daily folate supplement until your doctor tells you to stop.
- Check with your doctor that your vitamin B12injections are up to date.
- Remain well hydrated by drinking plenty of fluids while using ALIMTA. This will reduce your risk of developing kidney problems.
- Check with your doctor before receiving any vaccinations. Live vaccines are not recommended while you are using ALIMTA.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how ALIMTA affects you.
ALIMTA may cause tiredness or drowsiness in some people.
Looking after your medicine
ALIMTA will be stored in the hospital pharmacy or on the ward.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
General:
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
| Blood-cell related: Symptoms of abnormal blood cell counts may include:
Symptoms of liver impairment may include:
Symptoms of kidney impairment may include:
| Tell your doctor as soon as possible if you notice any of these side effects. |
| Stomach related: Inflammation of the large intestines. Symptoms may include:
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Some side effects (for example changes in liver enzymes, changes in kidney function, and blood cell levels) can only be found when your doctor does tests from time to time to check your progress.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
ALIMTA is only available with a doctor's prescription.
What ALIMTA contains
| Active ingredient (main ingredient) | pemetrexed disodium heptahydrate |
| Other ingredients (inactive ingredients) | hydrochloric acid mannitol sodium hydroxide |
Do not take this medicine if you are allergic to any of these ingredients.
What ALIMTA looks like
ALIMTA is a white to light yellow or green-yellow powder and is available in a glass vial container with a rubber stopper.
ALIMTA is supplied in 100 mg and 500 mg vials.
ALIMTA 100 mg, AUST R 146828.
ALIMTA 500 mg, AUST R 96731
Who distributes ALIMTA
ALIMTA is supplied by:
Eli Lilly Australia Pty Ltd
Level 9, 60 Margaret Street
SYDNEY NSW 2000
This leaflet was prepared in August 2025.
® = Registered Trademark
vA8_Aug2025
Brand Information
| Brand name | Alimta |
| Active ingredient | Pemetrexed |
| Schedule | S4 |
MIMS Revision Date: 01 October 2025
1 Name of Medicine
Pemetrexed disodium heptahydrate.
2 Qualitative and Quantitative Composition
Alimta is supplied in 500 mg and 100 mg vials.
Each 500 mg vial of Alimta contains pemetrexed disodium heptahydrate equivalent to 500 mg pemetrexed. Each 100 mg vial of Alimta contains pemetrexed disodium heptahydrate equivalent to 100 mg pemetrexed.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Alimta is supplied as a sterile lyophilised powder for intravenous infusion available in single dose vials. The product is a white to either light yellow or green yellow lyophilised solid.
4 Clinical Particulars
4.1 Therapeutic Indications
Malignant pleural mesothelioma. Alimta, in combination with cisplatin, is indicated for the treatment of patients with malignant pleural mesothelioma.
Non-small cell lung cancer. Alimta in combination with cisplatin is indicated for initial treatment of patients with locally advanced or metastatic non-small cell lung cancer other than predominantly squamous cell histology.
Alimta as monotherapy is indicated for the treatment of patients with locally advanced or metastatic non-small cell lung cancer other than predominantly squamous cell histology after prior platinum based chemotherapy.
4.2 Dose and Method of Administration
Alimta should be administered under the supervision of a qualified physician experienced in the use of antineoplastic agents.
Alimta in combination use with cisplatin. Adults. The recommended dose of Alimta is 500 mg/m2 as body surface area (BSA) administered as an intravenous infusion over 10 minutes on the first day of each 21 day cycle.
The recommended dose of cisplatin is 75 mg/m2 BSA infused over 2 hours approximately 30 minutes after completion of the Alimta infusion on the first day of each 21 day cycle. Patients must receive adequate anti-emetic treatment and appropriate hydration prior to and/or after receiving cisplatin. See cisplatin Product Information document for specific dosing advice.
Single agent use. Adults. The recommended dose of Alimta is 500 mg/m2 BSA administered as an intravenous infusion over 10 minutes on the first day of each 21 day cycle.
Premedication regimen. Skin rash has been reported in patients not pretreated with a corticosteroid. Pretreatment with dexamethasone (or equivalent) reduces the incidence and severity of cutaneous reaction. In clinical trials, dexamethasone 4 mg was given by mouth twice daily the day before, the day of and the day after Alimta administration.
To reduce toxicity, patients treated with Alimta must be instructed to take a low dose oral folic acid preparation or a multivitamin containing folic acid on a daily basis. At least 5 daily doses of folic acid must be taken during the 7-day period preceding the first dose of Alimta, and dosing should continue during the full course of therapy and for 21 days after the last dose of Alimta. Patients must also receive one intramuscular injection of vitamin B12 during the week preceding the first dose of Alimta and every 3 cycles thereafter. Subsequent vitamin B12 injections may be given the same day as Alimta. In clinical trials, the dose of folic acid studied ranged from 350 to 1,000 microgram, and the dose of vitamin B12 received was 1,000 microgram. The most commonly used dose of oral folic acid was 400 microgram.
Laboratory monitoring and dose reduction recommendations. Monitoring. It is recommended that patients receiving Alimta be monitored before each dose with a complete blood count, including a differential and platelet count. Periodic blood chemistry tests should be collected to evaluate renal and hepatic function.
Absolute neutrophil count (ANC) should be ≥ 1,500 cells/mm3 and platelets ≥ 100,000 cells/mm3 prior to scheduled administration of any cycle.
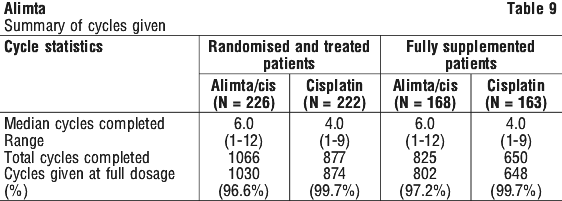
Dose reduction recommendations. Dose adjustments at the start of a subsequent cycle should be based on nadir haematologic counts or maximum nonhaematologic toxicity from the preceding cycle of therapy. Treatment may be delayed to allow sufficient time for recovery. Upon recovery, patients should be retreated using the guidelines in Tables 1-3, which are suitable for using Alimta as a single agent or in combination with cisplatin.



Elderly patients. In clinical trials, there has been no indication that patients 65 years of age or older are at increased risk of adverse events compared with patients younger than 65. No dose reductions other than those recommended for all patients are necessary.
Renally impaired patients. In clinical studies, patients with creatinine clearance of at least 45 mL/min required no dose adjustments other than those recommended for all patients. Insufficient numbers of patients with creatinine clearance below 45 mL/min have been treated to make dosage recommendations for this group of patients. Therefore, patients should not receive Alimta whose creatinine clearance is < 45 mL/min (using the standard Cockcroft and Gault formula or GFR measured by Tc99m-DPTA serum clearance method).
Preparation and administration instructions. Use aseptic technique.
Reconstitution and further dilution prior to intravenous infusion is only recommended with 0.9% sodium chloride injection. Alimta is physically incompatible with diluents containing calcium, including lactated Ringer's injection and Ringer's injection. Coadministration of Alimta with other drugs and diluents has not been studied, and therefore is not recommended.
1. Use appropriate aseptic technique during the reconstitution and further dilution of Alimta for intravenous infusion administration.
2. Calculate the dose and the number of Alimta vials needed. A 500 mg vial contains 500 mg of pemetrexed. A 100 mg vial contains 100 mg of pemetrexed. The vial contains an excess of pemetrexed to facilitate delivery of label amount.
3. Prior to administration, reconstitute 500 mg vials with 20 mL of 0.9% sodium chloride injection to give a solution containing 25 mg/mL pemetrexed. Reconstitute 100 mg vials with 4.2 mL of 0.9% sodium chloride injection to give a solution containing 25 mg/mL pemetrexed.
4. Gently swirl each vial until the powder is completely dissolved. The resulting solution is clear and ranges in colour from colourless to yellow or green yellow without adversely affecting product quality. The pH of the reconstituted Alimta solution is between 6.6 and 7.8. Further dilution is required.
5. The appropriate volume of reconstituted Alimta solution should be further diluted to 100 mL with 0.9% sodium chloride injection and administered as an intravenous infusion over 10 minutes.
6. Parenteral drug products should be inspected visually for particulate matter and discolouration prior to administration.
Chemical and physical stability of reconstituted and infusion solutions of Alimta was demonstrated for up to 24 hours after reconstitution of the original vial when refrigerated between 2 to 8°C. However, because Alimta and the recommended diluent contain no antimicrobial preservatives, to reduce antimicrobial hazard, reconstituted and infusion solutions should be used immediately. Discard any unused portion.
4.3 Contraindications
Alimta is contraindicated in patients who have a history of severe hypersensitivity reaction to pemetrexed or to any excipients in this product.
4.4 Special Warnings and Precautions for Use
Alimta can suppress bone marrow function as manifested by anaemia, neutropenia, thrombocytopenia or pancytopenia (see Section 4.8 Adverse Effects (Undesirable Effects)). Myelosuppression is usually the dose limiting toxicity. Patients should be monitored for myelosuppression during therapy and Alimta should not be given to patients until absolute neutrophil count (ANC) returns to ≥ 1,500 cells/mm3 and platelet count returns to ≥ 100,000 cells/mm3. Dose reductions for subsequent cycles are based on nadir ANC, platelet count and maximum nonhaematologic toxicity seen in the previous cycle (see Section 4.2 Dose and Method of Administration, Dose reduction recommendations).
Patients treated with Alimta must be instructed to take folic acid and vitamin B12 with Alimta as a prophylactic measure to reduce treatment related toxicity (see Section 4.2 Dose and Method of Administration). In the phase 3 mesothelioma EMPHACIS trial, less overall toxicity and reductions in grade 3/4 haematologic and nonhaematologic toxicities such as neutropenia, febrile neutropenia and infection with grade 3/4 neutropenia were reported when pretreatment with folic acid and vitamin B12 was administered.
Serious renal events, including acute renal failure, have been reported with pemetrexed alone or in association with other chemotherapeutic agents. Many of the patients in whom these occurred had underlying risk factors for the development of renal events including dehydration or pre-existing hypertension or diabetes.
Due to the gastrointestinal toxicity of pemetrexed given in combination with cisplatin, severe dehydration has been observed. Therefore, patients should receive adequate antiemetic treatment and appropriate hydration prior to and/or after receiving treatment.
Serious cardiovascular events, including myocardial infarction and cerebrovascular events have been uncommonly reported during clinical studies with pemetrexed, usually when given in combination with another cytotoxic agent. Most of the patients in whom these events have been observed had pre-existing cardiovascular risk factors.
Immunodepressed status is common in cancer patients. As a result, concomitant use of live attenuated vaccines is not recommended.
Cases of radiation pneumonitis have been reported in patients treated with radiation either prior, during or subsequent to their pemetrexed therapy. Particular attention should be paid to these patients and caution exercised with use of other radiosensitising agents. Cases of radiation recall have been reported in patients who received radiotherapy weeks or years previously.
Use in hepatic impairment. Alimta is not extensively metabolised by the liver. However, patients with hepatic impairment such as bilirubin > 1.5 times the upper limit of normal (ULN) or aminotransferase > 3 times the ULN (hepatic metastases absent) or > 5 times the ULN (hepatic metastases present) have not been specifically studied.
Alimta should be administered under the supervision of a qualified physician experienced in the use of antineoplastic agents. Appropriate management of complications is possible only when adequate diagnostic and treatment facilities are readily available. Treatment related adverse events of Alimta seen in clinical trials have been reversible. Skin rash has been reported in patients not pretreated with a corticosteroid in clinical trials. Pretreatment with dexamethasone (or equivalent) reduces the incidence and severity of cutaneous reaction (see Section 4.2 Dose and Method of Administration).
The effect of third space fluid, such as pleural effusion and ascites, on Alimta is unknown. In patients with clinically significant third space fluid, consideration should be given to draining the effusion prior to Alimta administration.
Use in renal impairment. Alimta is primarily eliminated unchanged by renal excretion. Insufficient numbers of patients have been studied with creatinine clearance below 45 mL/minute. Therefore, Alimta should not be administered to patients whose creatinine clearance is < 45 mL/min (see Section 4.2 Dose and Method of Administration, Dose reduction recommendations).
Use in the elderly. In clinical studies, there has been no indication that patients 65 years of age or older are at increased risk of adverse events compared to patients younger than 65 years old. No dose reductions other than those recommended for all patients are necessary.
Paediatric use. Alimta is not recommended for use in patients under 18 years of age, as safety and efficacy have not been established in this group of patients.
Effects on laboratory tests. There are no data available that shows that pemetrexed has an effect on laboratory tests.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Alimta is primarily eliminated unchanged renally as a result of glomerular filtration and tubular secretion. In vitro studies indicate that pemetrexed is actively secreted by the organic anion transporter 3 (OAT3) in the kidney. In vitro work also indicates that pemetrexed has affinity for OAT4 but the role of OAT4 in the renal elimination of molecules in not fully understood. Concomitant administration of nephrotoxic drugs and/or substances that are tubularly secreted could result in delayed clearance of Alimta.
Concomitant administration of pemetrexed with OAT3 (organic anion transporter 3) inhibitors (e.g. probenecid, penicillin, proton pump inhibitors (PPIs)) results in delayed clearance of pemetrexed. Caution should be made when these drugs are combined with pemetrexed.
Results from in vitro studies with human liver microsomes suggest that Alimta would not cause clinically significant interactions with drugs metabolised by CYP3A, CYP2D6, CYP2C9 and CYP1A2.
The pharmacokinetics of Alimta are not influenced by oral folic acid and intramuscular vitamin B12 supplementation or by concurrently administered cisplatin. Total platinum clearance is not affected by Alimta administration.
Although NSAIDs in moderate doses can be administered with Alimta in patients with normal renal function (creatinine clearance ≥ 80 mL/min), renal clearance was reduced by 16% when ibuprofen was concurrently administered with pemetrexed in patients with normal renal function. Caution should be used when administering NSAIDs concurrently with Alimta to patients with mild to moderate renal insufficiency (creatinine clearance of 45-79 mL/min). It is recommended that patients with mild to moderate renal insufficiency should avoid taking NSAIDs with short elimination half-lives for a period of 2 days before, the day of and 2 days following administration of Alimta.
In the absence of data regarding potential interaction between Alimta and NSAIDs with longer half-lives, in patients with mild to moderate renal insufficiency, patients with mild to moderate renal insufficiency taking these NSAIDs should interrupt dosing for at least 5 days before, the day of and 2 days following Alimta administration. If concomitant administration of NSAIDs is necessary, patients should be monitored closely for toxicity, especially myelosuppression and gastrointestinal toxicity.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. Administration of pemetrexed to male mice at intraperitoneal doses of ≥ 0.3 mg/m2/day resulted in reproductive toxicity characterised by reduced fertility, hypospermia and testicular atrophy.
Use in pregnancy. (Category D)
The use of Alimta should be avoided in pregnant women because of the potential hazard to the foetus. Pemetrexed was teratogenic (causing cleft palate) in mice at intravenous doses of ≥ 15 mg/m2/day. Other embryofetal toxic effects (embryofetal deaths, reduced fetal weights and incomplete ossification) were also observed. Embryofetal toxicity was observed at the lowest dose tested (0.6 mg/m2/day).
Use in lactation. It is not known whether pemetrexed is excreted in human milk. Therefore, breastfeeding should be discontinued during Alimta therapy.
4.7 Effects on Ability to Drive and Use Machines
No studies on the effects on the ability to drive and use machines have been performed. However, it has been reported that Alimta may cause fatigue. Therefore, patients should be cautioned against driving or operating machinery if this event occurs.
4.8 Adverse Effects (Undesirable Effects)
Single agent Alimta (NSCLC). Table 4 provides the frequency and severity of undesirable effects that have been reported in > 5% of 265 patients randomly assigned to receive single agent Alimta with folic acid and vitamin B12 supplementation and 276 patients randomly assigned to receive single agent docetaxel. All patients were diagnosed with locally advanced or metastatic NSCLC and received prior chemotherapy.
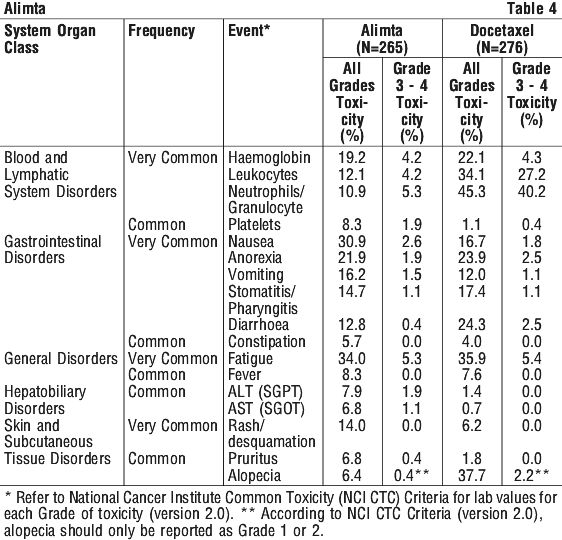
Clinically relevant CTC toxicity that was reported in ≥ 1% and ≤ 5% (common) of the patients that were randomly assigned to Alimta include sensory neuropathy, motor neuropathy, abdominal pain, increased creatinine, febrile neutropenia, infection without neutropenia, allergic reaction/ hypersensitivity and erythema multiforme.
Clinically relevant CTC toxicity that was reported in ≤ 1% (uncommon) of the patients that were randomly assigned to Alimta include supraventricular arrhythmias.
Clinically relevant grade 3 and grade 4 laboratory toxicities were similar between integrated phase 2 results from three single agent Alimta studies (n = 164) and the phase 3 single agent Alimta study described above, with the exception of neutropenia (12.8% versus 5.3%, respectively) and alanine aminotransferase elevation (15.2% versus 1.9%, respectively). These differences were likely due to differences in the patient population, since the phase 2 studies included chemonaive and heavily pretreated breast cancer patients with pre-existing liver metastases and/or abnormal baseline liver function tests.
Combination with cisplatin (MPM). Table 5 provides the frequency and severity of undesirable effects that have been reported in > 5% of 168 patients with mesothelioma who were randomly assigned to receive cisplatin and Alimta and 163 patients with mesothelioma randomly assigned to receive single agent cisplatin. In both treatment arms, these chemonaive patients were fully supplemented with folic acid and vitamin B12.
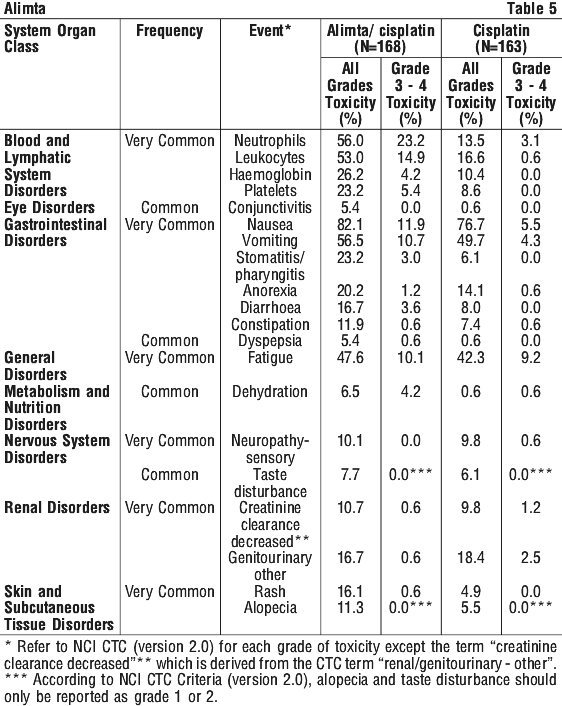
Clinically relevant toxicity that was reported in ≥ 1% and ≤ 5% (common) of the patients that were randomly assigned to receive cisplatin and Alimta include increased AST (SGOT), ALT (SGPT) and GGT, infection, febrile neutropenia, renal failure, chest pain, pyrexia and urticaria.
Clinically relevant toxicity that was reported in ≤ 1% (uncommon) of the patients that were randomly assigned to receive cisplatin and Alimta include arrhythmia and motor neuropathy.
Combination with cisplatin (NSCLC). Table 6 provides the frequency and severity of undesirable effects considered possibly related to study drug that have been reported in > 5% of 839 patients with NSCLC who were randomised to study and received cisplatin and pemetrexed and 830 patients with NSCLC who were randomised to study and received cisplatin and gemcitabine. All patients received study therapy as initial treatment for locally advanced or metastatic NSCLC and patients in both treatment groups were fully supplemented with folic acid and vitamin B12.
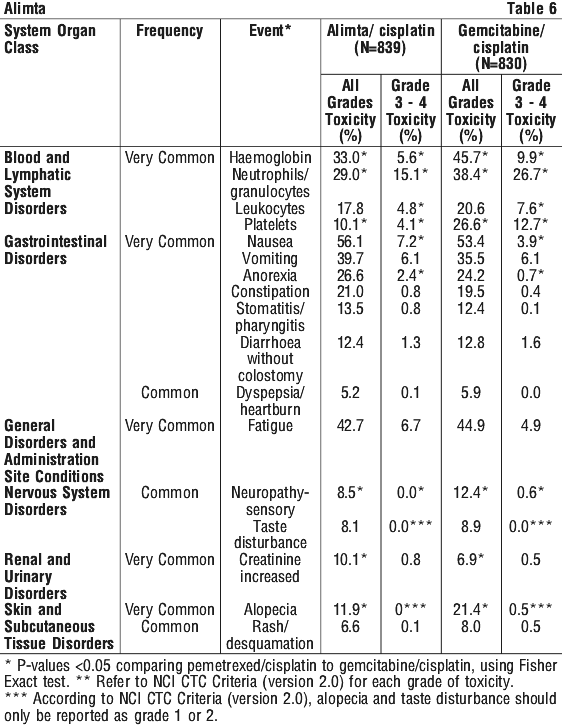
Clinically relevant toxicity that was reported in ≥ 1% and ≤ 5% (common) of the patients that were randomly assigned to receive cisplatin and pemetrexed include: AST increase, ALT increase, infection, febrile neutropenia, renal failure, pyrexia, dehydration, conjunctivitis, and creatinine clearance decrease.
Clinically relevant toxicity that was reported in < 1% (uncommon) of the patients that were randomly assigned to receive cisplatin and pemetrexed include: GGT increase, chest pain, arrhythmia, and motor neuropathy. Acute renal failure was observed more commonly in the pemetrexed/ cisplatin arm (6 cases, 0.7%) than in the gemcitabine/ cisplatin arm (0 cases).
Single agent Alimta (NSCLC maintenance). Table 7 provides the frequency and severity of undesirable effects considered possibly related to study drug that have been reported in > 5% of 800 patients randomly assigned to receive single agent pemetrexed and 402 patients randomly assigned to receive placebo in the single agent maintenance pemetrexed study (JMEN: N = 663) and continuation pemetrexed maintenance study (PARAMOUNT: N = 539). All patients were diagnosed with stage IIIB or IV NSCLC and had received prior platinum based chemotherapy. Patients in both study arms were fully supplemented with folic acid and vitamin B12.
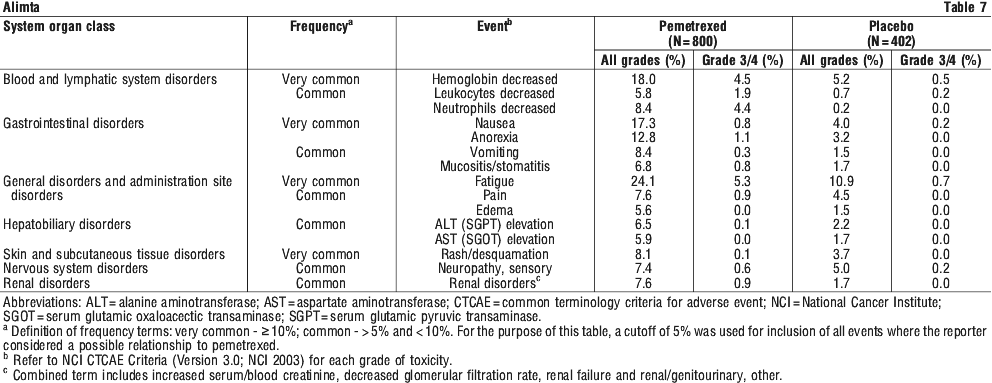
Clinically relevant CTC toxicity that was reported in < 1% (uncommon) of the patients that were randomly assigned to pemetrexed include: febrile neutropenia, allergic reaction/ hypersensitivity, motor neuropathy, erythema multiforme, renal failure, and supraventricular arrhythmia.
Safety was assessed for patients who were randomised to receive pemetrexed (N = 800). The incidence of adverse reactions was evaluated for patients who received ≤ 6 cycles of pemetrexed maintenance (N = 519), and compared to patients who received > 6 cycles of pemetrexed (N = 281). Increases in adverse reactions (all grades) were observed with longer exposure. A significant increase in the incidence of possibly study drug related grade 3-4 neutropenia was observed with longer exposure to pemetrexed (≤ 6 cycles: 3.3%, > 6 cycles: 6.4%, p = 0.046). No statistically significant differences in any other individual grade 3/4/5 adverse reactions were seen with longer exposure.
In clinical trials, sepsis which in some cases was fatal occurred in approximately 1% of patients.
Cases of oesophagitis have been reported uncommonly in clinical trials with pemetrexed.
Postmarketing data. Gastrointestinal disorders. Rare cases of colitis have been reported in patients treated with Alimta.
General disorders and administration site conditions. Rare cases of oedema have been reported in patients treated with Alimta.
Injury, poisoning and procedural complications. Rare cases of radiation recall have been reported in patients who have previously received radiotherapy.
Respiratory disorders. Rare cases of interstitial pneumonitis have been reported in patients treated with Alimta.
Skin. Rare cases of bullous conditions have been reported including Stevens-Johnson syndrome and Toxic epidermal necrolysis which in some cases were fatal.
Blood and lymphatic system. Rare cases of immune mediated haemolytic anaemia have been reported in patients treated with pemetrexed.
Hepatobiliary disorders. Rare cases of hepatitis, potentially serious, have been reported during clinical trials with Alimta.
Rare: ≤ 0.1% of patients treated with Alimta.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
Reported symptoms of Alimta overdose include neutropenia, anaemia, thrombocytopenia, mucositis and rash. Anticipated complications of overdose include bone marrow suppression as manifested by neutropenia, thrombocytopenia and anaemia. In addition, infection with or without fever, diarrhoea and mucositis may be seen.
If overdose occurs, general supportive measures should be instituted as deemed necessary by the treating physician. Management of Alimta overdose should include consideration of the use of leucovorin or thymidine rescue.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Pemetrexed is an antifolate antineoplastic agent. In vitro studies have shown that pemetrexed behaves as a multitargeted antifolate by inhibiting thymidylate synthase (TS), dihydrofolate reductase (DHFR) and glycinamide ribonucleotide formyltransferase (GARFT), which are key folate dependent enzymes for the de novo biosynthesis of thymidine and purine nucleotides that are essential for cell replication. Both the reduced folate carrier and membrane folate binding protein transport systems appear to be involved in transport of pemetrexed into cells. Once in the cell, pemetrexed is converted to polyglutamate forms by the enzyme folyl polyglutamate synthetase. The polyglutamate forms are even more potent inhibitors of TS and GARFT than pemetrexed. Polyglutamation is a time and concentration dependent process that occurs in tumour cells and, to a lesser extent, in normal tissues. Polyglutamated metabolites have a longer intracellular half-life than the parent drug, resulting in prolonged drug action in malignant cells. Data indicates that overexpression of thymidylate synthase (TS) correlates with reduced sensitivity to pemetrexed in antifolate resistant cell lines. Results in a study with specimens from chemonaive patients with NSCLC demonstrated lower levels of TS expression in adenocarcinoma as compared to squamous cell carcinoma tumors. This data suggests that pemetrexed may offer greater efficacy for patients with adenocarcinoma as compared to squamous carcinoma histology.
An in vitro study with the MSTO-211H mesothelioma cell line showed synergistic effects when pemetrexed was combined with cisplatin.
Clinical trials. Malignant pleural mesothelioma. The safety and efficacy of Alimta have been evaluated in chemonaive patients with malignant pleural mesothelioma (MPM) as a single agent and in combination with platinum based regimens.
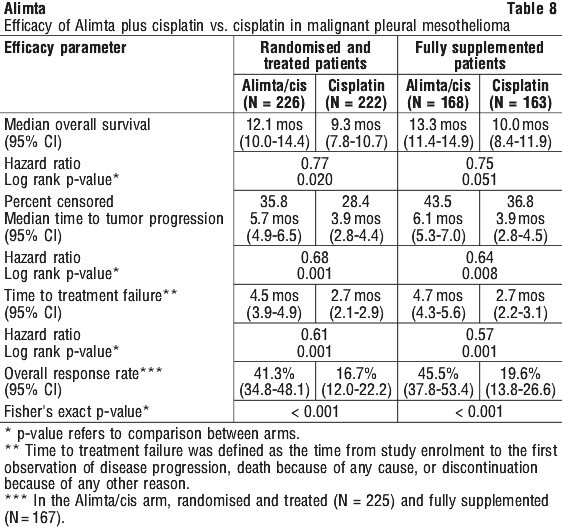
EMPHACIS, a multicentre, randomised, single blind phase 3 study of Alimta plus cisplatin versus cisplatin in chemonaive patients with malignant pleural mesothelioma, has shown that patients treated with Alimta and cisplatin had a clinically meaningful 2.8 month median survival advantage over patients receiving cisplatin alone. Alimta was administered intravenously over 10 minutes at a dose of 500 mg/m2 and cisplatin was administered intravenously over 2 hours at a dose of 75 mg/m2 beginning approximately 30 minutes after the end of administration of Alimta. Both drugs were given on day 1 of each 21 day cycle. On this study, treatment was administered up to 6 cycles. Additional cycles were permitted for patients who were receiving benefit from therapy.
During the study, low dose folic acid and vitamin B12 supplementation was introduced to patients' therapy to reduce toxicity. The primary analysis of this study was performed on the population of all patients randomly assigned to a treatment arm who received study drug (randomised and treated). A subgroup analysis was performed on patients who received folic acid and vitamin B12 supplementation during the entire course of study therapy (fully supplemented).
Table 8 summarises the efficacy results for all patients regardless of vitamin supplementation status and those patients receiving vitamin supplementation from the time of enrolment in the trial.
Non-small cell lung cancer. The safety and efficacy of Alimta have been evaluated in combination with cisplatin as initial treatment for non-small cell lung cancer (NSCLC) and as a single agent in patients who have previously received chemotherapy treatment.
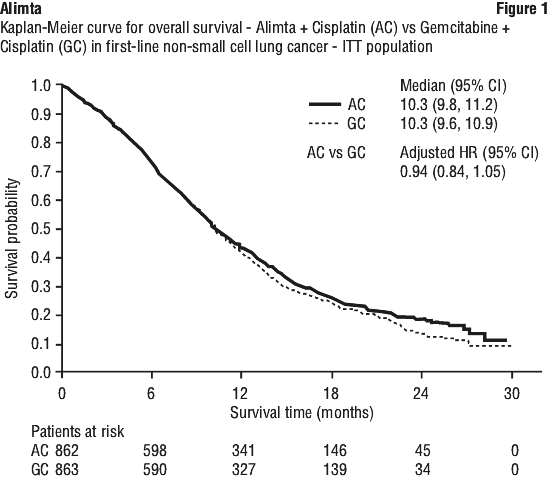
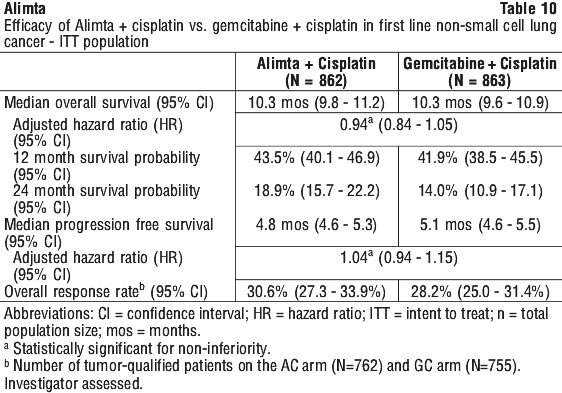
A multicentre, randomised, open label phase 3 study of Alimta plus cisplatin versus gemcitabine plus cisplatin (for up to 6 cycles) in chemonaive patients with locally advanced or metastatic (stage IIIb or IV) non-small cell lung cancer (NSCLC) showed that Alimta plus cisplatin (intent to treat [ITT] population n = 862) met its primary endpoint and showed similar clinical efficacy as gemcitabine plus cisplatin (ITT n = 863) in overall survival (adjusted hazard ratio 0.94; 95% CI 0.84-1.05). See Figure 1 and Table 10.
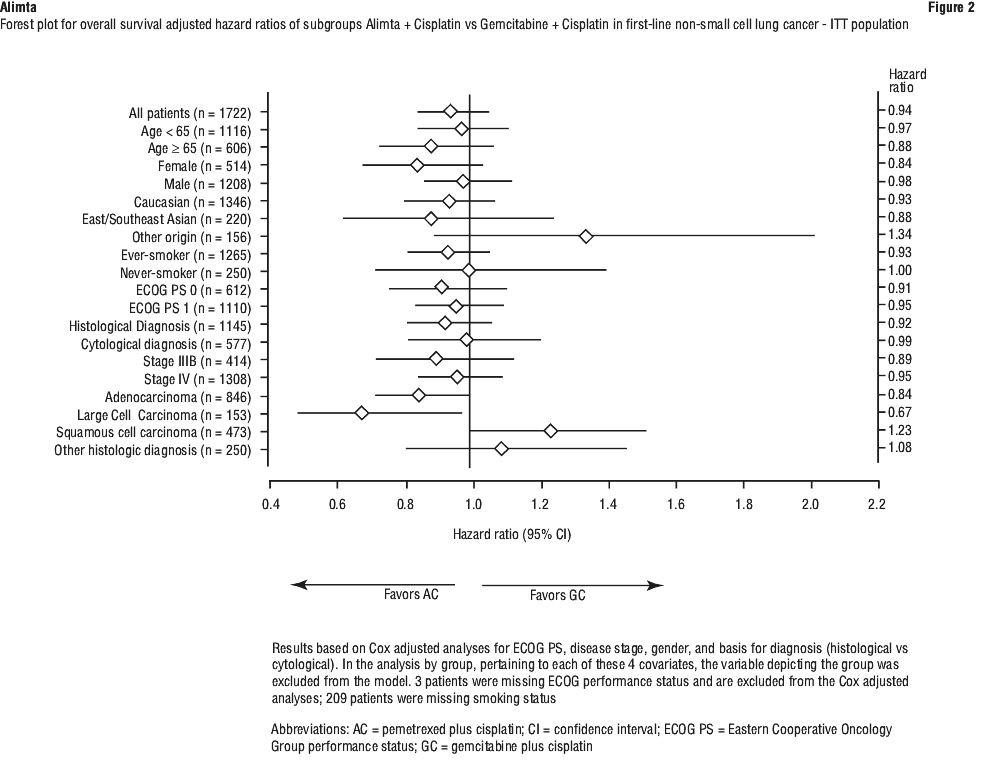
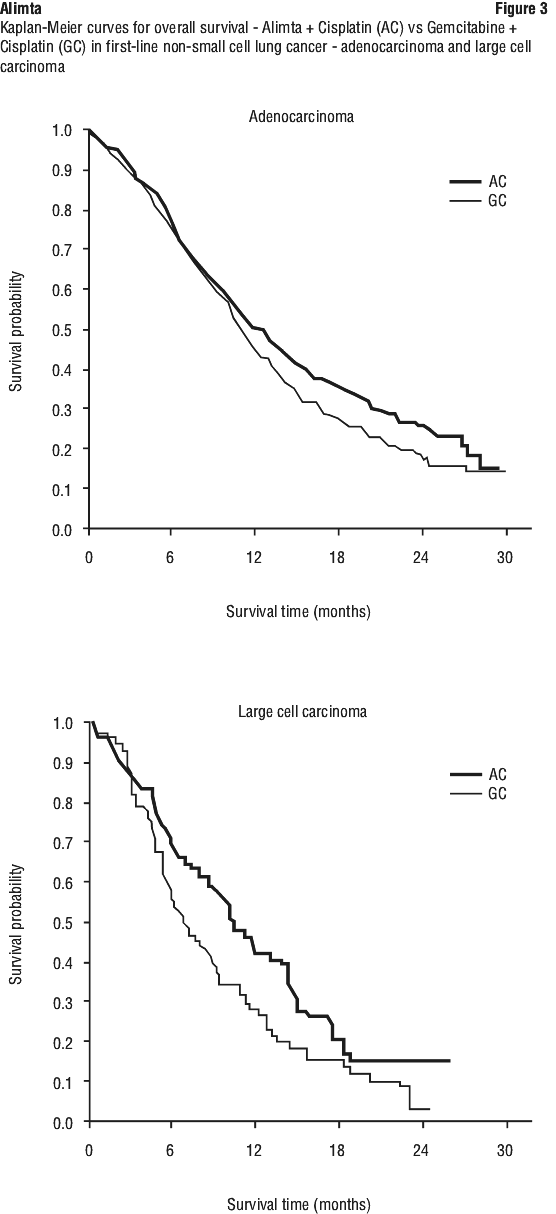
There were no clinically relevant differences observed for the safety profile of Alimta plus cisplatin within the histology subgroups.
A multicentre, randomised, double blind, placebo controlled phase 3 study (JMEN), compared the efficacy and safety of maintenance treatment with Alimta plus best supportive care (BSC) (n = 441) with that of placebo plus BSC (n = 222) in patients with locally advanced (stage IIIB) or metastatic (stage IV) non-small cell lung cancer (NSCLC) who did not progress after 4 cycles of first line doublet therapy. All patients included in this study had an ECOG performance status 0 or 1. Patients received maintenance treatment until disease progression. Efficacy and safety were measured from the time of randomisation after completion of first line (induction) therapy. Patients received a median of 5 cycles of maintenance treatment with Alimta and 3.5 cycles of placebo. A total of 213 patients (48.3%) completed ≥ 6 cycles and a total of 103 patients (23.4%) completed ≥ 10 cycles of treatment with Alimta.
In the overall study population, Alimta was statistically superior to placebo in terms of overall survival (OS) (median 13.4 months versus 10.6 months, HR = 0.79 (95% CI: 0.65-0.95), p-value = 0.012) and PFS (median 4.0 months versus 2.0 months, HR = 0.60 (95% CI: 0.49-0.73), p-value < 0.00001). Consistent with previous Alimta studies, a difference in treatment outcomes was observed according to histologic classification. For the indicated population i.e. patients with NSCLC other than predominantly squamous cell histology, Alimta was superior to placebo for OS (median 15.5 months versus 10.3 months, HR = 0.70 (95% CI: 0.56-0.88)) and PFS (median 4.4 months versus 1.8 months, HR = 0.47 (95% CI: 0.37-0.60)).
The PFS and OS results in patients with squamous cell histology suggested no advantage for Alimta over placebo.
There were no clinically relevant differences observed for the safety profile of Alimta within the histology subgroups. See Figure 4.
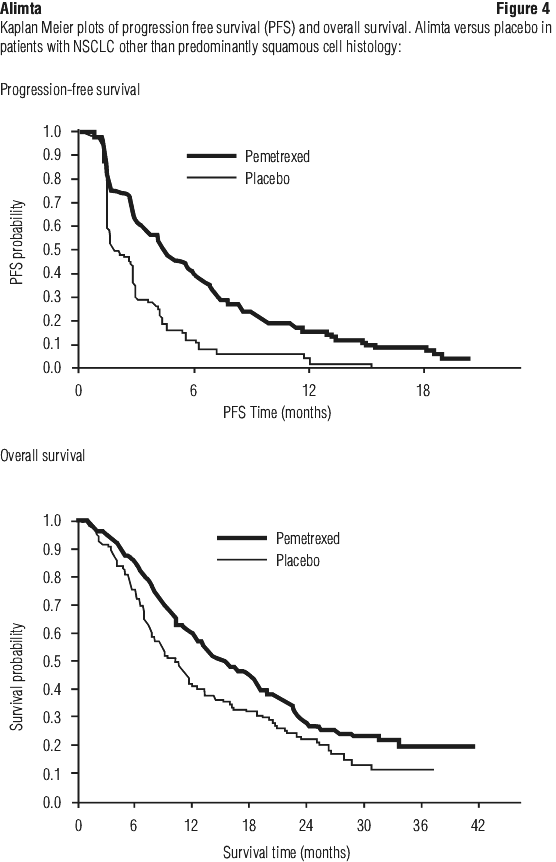
Independent review of the imaging of 472 of the 539 randomised patients showed that the study met its primary endpoint (PFS) and showed a statistically significant improvement in PFS in the Alimta arm over the placebo arm, median of 3.9 months and 2.6 months respectively (hazard ratio = 0.64, 95% CI = 0.51-0.81, p = 0.0002). The independent review of patient scans showed consistent results to the findings of the investigator assessment of PFS. In addition, for randomised patients, as measured from the start of Alimta plus cisplatin first line induction treatment, the median investigator assessed PFS was 6.9 months for the Alimta arm and 5.6 months for the placebo arm (hazard ratio = 0.59, 95% CI = 0.47-0.74).
Following Alimta plus cisplatin induction (4 cycles), treatment with Alimta was statistically superior to placebo for OS (median 13.9 months versus 11.0 months, hazard ratio = 0.78, 95% CI = 0.64-0.96, p = 0.0195). At the time of final survival analysis, 28.7% of patients were alive or lost to follow up on the Alimta arm versus 21.7% on the placebo arm. The relative treatment effect of Alimta was internally consistent across subgroups (including disease stage, induction response, ECOG PS, smoking status, gender, histology and age) and similar to that observed in the unadjusted OS and PFS analyses. The 1 year and 2 year survival rates for patients on Alimta were 58% and 32% respectively, compared to 45% and 21% for patients on placebo. From the start of Alimta plus cisplatin first line induction treatment, the median OS of patients was 16.9 months for the Alimta arm and 14.0 months for the placebo arm (hazard ratio = 0.78, 95% CI = 0.64-0.96). The percentage of patients that received postdiscontinuation chemotherapy was 64.3% for Alimta and 71.7% for placebo. See Figure 5.
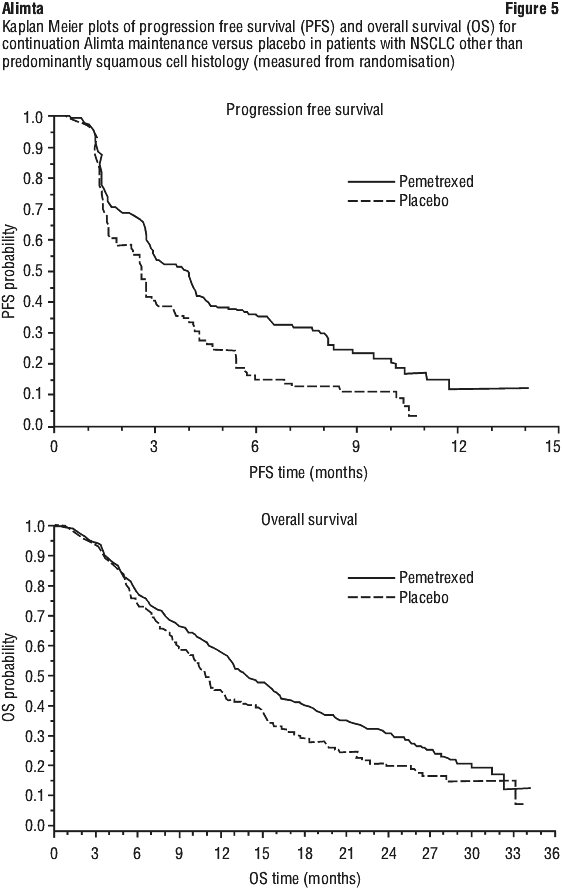
A multicentre, randomised, open label phase 3 study of Alimta versus docetaxel (with treatment until progression) in patients with locally advanced or metastatic NSCLC after prior chemotherapy has shown median survival times of 8.3 months for patients treated with Alimta (intent to treat population n = 283) and 7.9 months for patients treated with docetaxel (ITT n = 288) which is not statistically significantly different. These data, as outlined in Table 11, indicate comparable efficacy between pemetrexed and docetaxel.
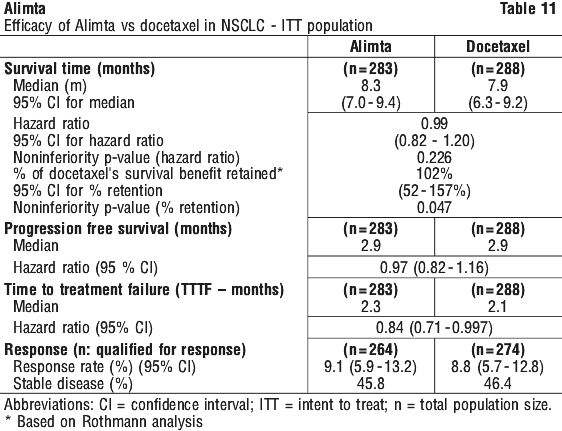
An analysis of the impact of NSCLC histology on overall survival was in favor of Alimta versus docetaxel for other than predominantly squamous histology (n = 399, 9.3 versus 8.0 months, adjusted HR = 0.78; 95% CI = 0.61-1.00, p = 0.047) and was in favor of docetaxel for squamous cell carcinoma histology (n = 172, 6.2 versus 7.4 months, adjusted HR = 1.56; 95% CI = 1.08-2.26, p = 0.018). There were no clinically relevant differences observed for the safety profile of Alimta within the histology subgroups.
5.2 Pharmacokinetic Properties
Absorption. Alimta is for intravenous administration only.
Distribution. Alimta has a steady-state volume of distribution of 16.1 litres. In vitro studies indicate that Alimta is approximately 81% bound to plasma proteins. Binding is not affected by degree of renal impairment.
Metabolism. Alimta undergoes limited hepatic metabolism.
Excretion. Alimta is primarily eliminated in the urine with up to 70% to 90% of the dose recovered unchanged within the first 24 hours following administration. Total plasma clearance of Alimta is 92 mL/min, and the elimination half-life from plasma is 3.5 hours in patients with normal renal function.
Special populations. Analyses to evaluate the pharmacokinetics of Alimta in special populations included 287 patients with a variety of advanced tumor types from 10 single agent phase 2 studies, 70 patients from the phase 3 malignant pleural mesothelioma EMPHACIS trial, and 47 patients from a phase 1 renal study.
Elderly. No effect of age on the pharmacokinetics of Alimta was observed over a range of 26 to 80 years.
Hepatic insufficiency. No effect of AST (SGOT), ALT (SGPT) or total bilirubin on the pharmacokinetics of Alimta was observed. However, specific studies of hepatically impaired patients have not been conducted (see Section 4.4 Special Warnings and Precautions for Use).
Renal insufficiency. Pharmacokinetic analyses included 127 patients with reduced renal function. Total plasma clearance and renal clearance of Alimta decrease as renal function decreases. On average, patients with creatinine clearance of 45 mL/min will have a 56% increase in Alimta total systemic exposure (AUC) relative to patients with creatinine clearance of 90 mL/min (see Section 4.4 Special Warnings and Precautions for Use; Section 4.2 Dose and Method of Administration).
5.3 Preclinical Safety Data
Genotoxicity. Pemetrexed has been shown to be clastogenic in the in vivo micronucleus assay in the mouse, but was negative in the in vitro chromosome aberration test in Chinese hamster ovary cells. Pemetrexed was negative in assays for gene mutation (bacteria and mammalian cells in vitro).
Carcinogenicity. Studies to assess the carcinogenic potential of pemetrexed have not been conducted.
6 Pharmaceutical Particulars
6.1 List of Excipients
Each 500 mg vial of Alimta contains 500 mg of mannitol. Hydrochloric acid and/or sodium hydroxide may have been added to adjust pH.
Each 100 mg vial of Alimta contains 106.4 mg of mannitol. Hydrochloric acid and/or sodium hydroxide may have been added to adjust pH.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C. Alimta is not light sensitive.
6.5 Nature and Contents of Container
Alimta, pemetrexed disodium for injection is available in sterile single use vials containing 100 mg or 500 mg pemetrexed (pack size 1 vial).
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Chemical structure. The active ingredient in Alimta powder for injection is pemetrexed disodium. Pemetrexed disodium has the chemical name l-glutamic acid, N-[4-[2-(2-amino-4,7-dihydro-4- oxo-1H-pyrrolo [2,3-d]pyrimidin-5-yl) ethyl]benzoyl]-, disodium salt, heptahydrate. It has an empirical formula of C20H19N5O6.2Na.7H2O and a molecular weight of 597.49. Pemetrexed disodium is a white to almost white solid. The structural formula is as follows:
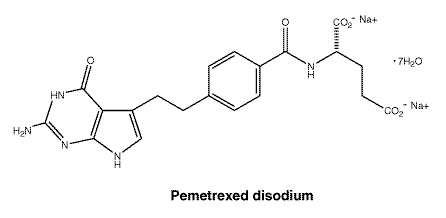
7 Medicine Schedule (Poisons Standard)
S4 - Prescription only Medicine.
Date of First Approval
30 June 2004
Date of Revision
06 August 2025
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.