APOHEALTH-Fluconazole-One
Brand Information
| Brand name | APOHEALTH-Fluconazole-One |
| Active ingredient | Fluconazole |
| Schedule | S3 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the APOHEALTH-Fluconazole-One.
Summary CMI
APOHEALTH Fluconazole One
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using APOHEALTH Fluconazole One?
APOHEALTH Fluconazole One contains the active ingredient Fluconazole. APOHEALTH Fluconazole One is used to treat a fungal infection known as vaginal thrush (vaginal candidiasis).
For more information, see Section 1. Why am I using APOHEALTH -Fluconazole One? in the full CMI.
2. What should I know before I use APOHEALTH Fluconazole One?
Do not use if you have ever had an allergic reaction to Fluconazole or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I use APOHEALTH Fluconazole One? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with APOHEALTH Fluconazole One and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use APOHEALTH Fluconazole One?
- APOHEALTH Fluconazole One should be taken as single dose of one capsule. The whole capsule is to be swallowed with one glass of water.
More instructions can be found in Section 4. How do I use APOHEALTH Fluconazole One? in the full CMI.
5. What should I know while using APOHEALTH Fluconazole One?
| Things you should do |
|
| Things you should not do |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using APOHEALTH Fluconazole One? in the full CMI.
6. Are there any side effects?
The common side effects include nausea, vomiting, stomach pain, indigestion, wind, diarrhoea, muscle or back pain and headache.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
APOHEALTH Fluconazole One
Active ingredient(s): Fluconazole
Consumer Medicine Information (CMI)
This leaflet provides important information about using APOHEALTH Fluconazole One. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using APOHEALTH Fluconazole One.
Where to find information in this leaflet:
1. Why am I using APOHEALTH Fluconazole One?
2. What should I know before I use APOHEALTH Fluconazole One?
3. What if I am taking other medicines?
4. How do I use APOHEALTH Fluconazole One?
5. What should I know while using APOHEALTH Fluconazole One?
6. Are there any side effects?
7. Product details
1. Why am I using APOHEALTH Fluconazole One?
APOHEALTH Fluconazole One contains the active ingredient Fluconazole. Fluconazole belongs to a group of medicines known as azole antifungals. These medicines work by preventing the growth of the fungi causing your infection.
APOHEALTH Fluconazole One is used to treat a fungal infection known as vaginal thrush (vaginal candidiasis).
What is vaginal thrush?
Vaginal thrush is a common name for vaginal candidiasis, an infection caused by a yeast-like fungus called Candida.
Candida is one of many organisms that live in the vagina. Your body's natural balance (immune system) normally keeps Candida under control, but when this natural balance is upset, Candida can multiply and can cause thrush symptoms.
Common symptoms of vaginal thrush include:
- itching, burning or soreness around the vagina
- cottage-cheese like discharge
- swelling or irritation of the infected area.
Things that may help you to avoid thrush in the future:
- wear cotton briefs, stockings and loose-fitting clothing rather than tight synthetic clothing
- wash regularly, but do not wash and dry yourself harshly
- avoid perfumed soaps, bath additives and vaginal deodorants.
Your doctor or pharmacist may have more information on things you can do to avoid thrush in the future.
Ask your doctor or pharmacist if you have any questions about why this medicine has been recommended for you. Your doctor or pharmacist may have recommended it for another reason.
There is no evidence that APOHEALTH Fluconazole One is addictive. “APOHEALTH Fluconazole One is a Pharmacist Only Medicine”. It is available without a doctor's prescription but your pharmacist's advice is required.
2. What should I know before I use APOHEALTH Fluconazole One?
Warnings
Do not use APOHEALTH Fluconazole One if:
- you are allergic to Fluconazole, or any of the ingredients listed at the end of this leaflet.
- Always check the ingredients to make sure you can use this medicine.
- Any other azole antifungals related to fluconazole such as miconazole (e.g. Daktarin), ketoconazole (e.g. Nizoral), clotrimazole (e.g. Canesten, Clonea) or itraconazole (e.g. Sporanox).
Some of the symptoms of an allergic reaction may include
- Shortness of breath
- Wheezing or breathing difficulty
- Swelling of the face, lips, tongue, throat, or other parts of the body
- Rash, itching or hives on the skin.
Do not use fluconazole if you are taking any of the following medicines:
- astemizole (a medicine used to treat allergy)
- cisapride (a medicine used to treat stomach problems)
- erythromycin (a medicine used to treat infections)
- pimozide (a medicine used to treat infections)
- quinidine (a medicine used to treat irregular heartbeat)
Check with your doctor or pharmacist if you:
- have allergies to any other medicines, food, dyes or preservatives
- take any medicines for any other condition
- have liver problems
- have kidney problems
- have heart problems
- have HIV infection or AIDS
- have diabetes
- have had thrush more than twice in the last six months
- are over 60 years of age
Tell your doctor or pharmacist if you:
- are experiencing any of the following: abnormal or irregular vaginal bleeding or blood stained discharge; foul smelling or unusual coloured discharge; vulval or vaginal sores, ulcers or blisters; lower abdominal pain or burning when passing urine; fever or chills
- are taking warfarin, as bleeding or bruising may occur
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Do not use fluconazole if you are pregnant, suspect you may be pregnant or if you may become pregnant during treatment. Fluconazole may affect your developing baby if you take it during pregnancy. Your pharmacist will discuss with you the risks and benefits involved.
Do not use this medicine if you are a female of childbearing age unless you are using adequate contraception.
Effective contraception should be taken during treatment and for about 1 week after the final dose.
Do not take this medicine if you are breast-feeding or intend to breastfeed.
Fluconazole may pass into breast milk and affect your baby.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines should not be taken with fluconazole.
These are listed under Section 2. What should I know before I use APOHEALTH Fluconazole One?
Some medicines and fluconazole may interfere with each other. These medicines and some others may be affected by fluconazole or may affect how well it works. You may need different amounts of your medicines, or you may need to take different medicines. These include:
- Amiodarone (used to treat irregular heartbeat)
- Some oral diabetes medication
- Some antibiotics such as rifampicin, rifabutin and azithromycin
- Some antiviral drugs used to treat HIV such as zidovudine and saquinavir
- Some antifungal drugs such as amphotericin B and voriconazole
- Some medicines used in problems with immune system, such as ciclosporin, tacrolimus, sirolimus, everolimus or tofacitinib
- cyclophosphamide, ibrutinib, Olaparib, vincristine, vinblastine (used to treat certain types of cancers)
- Vitamin A
- Antidepressants such as amitriptyline, nortriptyline
- predinsone (used to treat inflammation or suppress the immune system)
- lemborexant (used to treat insomnia or sleeping difficulties)
- Warfarin (used to stop blood clots).
- Phenytoin (used to treat epilepsy).
- carbamazepine (used in the treatment of epilepsy and bipolar disorder)
- Theophylline, used to treat asthma.
- Some opioid pain killers such as alfentanil, fentanyl and methadone
- Some benzodiazepines (used as sedatives or treat anxiety)
- Hydrochlorothiazide (used to treat fluid problems and high blood pressure)
- losartan (used for treating high blood pressure)
- calcium channel blockers such as nifedipine, amlodipine, felodipine and verapamil (used for relieving high blood pressure or irregular heart beat)
- statins such as simvastatin, Fluvastatin, atorvastatin (used to control high cholesterol levels)
- tolvaptan (used to treat low levels of sodium in your blood or for kidney problems)
- NSAIDS such as ibuprofen, naproxen, diclofenac and celecoxib
- lurasidone (used to manage schizophrenia)
- ivacaftor (used to manage cystic fibrosis)
- the contraceptive pill (birth control pill)
Talk to your doctor or pharmacist about the need for an additional method of contraception while taking fluconazole.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect APOHEALTH Fluconazole One.
4. How do I use APOHEALTH Fluconazole One?
How much to take / use
- Follow all directions given to you by your pharmacist carefully.
- They may differ to this information contained in this leaflet.
- Follow the instructions provided and use APOHEALTH Fluconazole One until your doctor tells you to stop.
When to take / use APOHEALTH Fluconazole One
- APOHEALTH Fluconazole One should be taken as single dose of one capsule.
- The whole capsule is to be swallowed with one glass of water.
- It does not matter whether you take this medicine with or without food.
If you forget to use APOHEALTH Fluconazole One
APOHEALTH Fluconazole One should be used regularly at the same time each day. If you miss your dose at the usual time, take immediately before the next dose.
If it is almost time for your next dose, skip the dose you missed and take your next dose when you are meant to.
Do not take a double dose to make up for the dose you missed.
If you use too much APOHEALTH Fluconazole One
If you think that you have used too much APOHEALTH Fluconazole One, you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know while using APOHEALTH Fluconazole One?
Things you should do
Call your doctor straight away if you:
- Are about to be started on any new medicine, remind your doctor or pharmacist that you have taken this medicine.
- Tell any other doctors, dentists and pharmacists who are treating you that you have taken this medicine.
- If you become pregnant while taking this medicine, tell your doctor immediately.
- If the symptoms of your infections do not improve after 03 days, or if they become worse, tell your doctor or pharmacist.
Remind any doctor, dentist, or pharmacist you visit that you are using APOHEALTH Fluconazole One.
Things you should not do
- Do not give this medicine to anyone else, even if they have the same condition as you.
- Do not take this medicine to treat any other complaint unless your doctor pr pharmacist tells you to do.
Things to be careful of
- Tell your doctor or pharmacist immediately if you develop rash soon after taking this medicine.
- People with HIV, AIDS or weak immune system may be prone to more serious side effects of the skin.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how APOHEALTH Fluconazole One affects you.
Fluconazole may cause occasional dizziness or seizures in some people.
Drinking alcohol
Tell your doctor if you drink alcohol.
No information on alcohol consumption with APOHEALTH Fluconazole One.
Looking after your medicine
- Keep your medicine in its pack until it is time to take it.
- If you take your medicine out of its pack it may not keep well.
Follow the instructions in the carton on how to take care of your medicine properly.
Store it in a cool dry place away from moisture, heat or sunlight; for example, do not store it:
- in the bathroom or near a sink, or
- in the car or on window sills.
Keep your medicine in a cool dry place where the temperature stays below 25°C.
Heat and dampness can destroy some medicines.
Keep it where young children cannot reach it.
A locked cupboard at least one-and -a half meters above the ground is a good place to store medicines.
Getting rid of any unwanted medicine
If you no longer need to use this medicine or it is out of date, take it to any pharmacy for safe disposal.
Do not use this medicine after the expiry date.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
Allergy or reaction related:
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
What APOHEALTH Fluconazole One contains
| Active ingredient (main ingredient) | Fluconazole |
| Other ingredients (inactive ingredients) | Lactose monohydrate Maize starch Colloidal anhydrous silica Purified talc Sodium lauryl sulphate Gelatin Titanium dioxide Paten blue V |
| Potential allergens | Contains sugars (as lactose) and sulfites |
This medicine does not contain gluten, sucrose, tartrazine, or any other azo dyes.
This medicine contains sugars (as lactose) and sulfites.
Do not take this medicine if you are allergic to any of these ingredients.
What APOHEALTH Fluconazole One looks like
APOHEALTH Fluconazole One is hard gelatin capsule of size “1” with sky blue body and cap (Aust R 152959).
Who distributes APOHEALTH Fluconazole One
Arrotex Pharmaceuticals Pty Ltd
15 – 17 Chapel Street
Cremorne VIC 3121
Australia
Web: www.arrotex.com.au
This leaflet was prepared in January 2026.
Brand Information
| Brand name | APOHEALTH-Fluconazole-One |
| Active ingredient | Fluconazole |
| Schedule | S3 |
MIMS Revision Date: 01 April 2026
1 Name of Medicine
Fluconazole.
2 Qualitative and Quantitative Composition
Each capsule contains 150 mg fluconazole, as its active ingredient.
Excipients with known effect. Each capsule contains sugars (as lactose) and sulfites.
For the full list of excipients see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Fluconazole is available as a hard gelatin capsule of size '1' with sky blue body and cap.
4 Clinical Particulars
4.1 Therapeutic Indications
Treatment of vaginal candidiasis.
4.2 Dose and Method of Administration
Fluconazole is intended for oral administration.
Adults. One capsule (150 mg fluconazole) should be administered as a single oral dose.
Use in renal impairment. Fluconazole is predominantly excreted in the urine as unchanged drug. No adjustments in single dose therapy are necessary in patients with minor or moderate renal impairment.
Children. Fluconazole is not recommended in children under 18 years of age except under medical advice.
4.3 Contraindications
Known sensitivity to fluconazole; to related azole compounds or to any of the excipients of this product.
Co-administration of terfenadine is contraindicated in patients receiving fluconazole at multiple doses of 400 mg/day or higher based upon results of a multiple dose interaction study.
Co-administration of other drugs known to prolong the QT interval and which are metabolised via the enzyme CYP3A4, such as cisapride, astemizole, erythromycin, pimozide and quinidine are contraindicated in patients receiving fluconazole (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
4.4 Special Warnings and Precautions for Use
Anaphylaxis. Anaphylaxis has been reported in rare instances.
Skin and subcutaneous tissue disorders. Patients have rarely developed exfoliative cutaneous reactions, such as Stevens-Johnson syndrome and toxic epidermal necrolysis, during treatment with fluconazole. Drug reaction with eosinophilia and systemic symptoms (DRESS) has been reported. AIDS patients are more prone to the development of serious cutaneous reactions to many drugs. If rash, which is attributable to fluconazole develops, fluconazole should not be used again. If patients with invasive/systemic fungal infections develop rashes, they should be monitored closely and fluconazole discontinued if bullous lesions or erythema multiforme develop (see Section 4.8 Adverse Effects (Undesirable Effects)).
QT interval prolongation. Some azoles, including fluconazole, have been associated with prolongation of the QT interval on the electrocardiogram. Fluconazole causes QT prolongation via the inhibition of the Rectifier Potassium Channel current (Ikr). The QT prolongation caused by other medicinal products (such as amiodarone) may be amplified via the inhibition of cytochrome P450 (CYP) 3A4 (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions). During post-marketing surveillance, there have been very rare cases of QT prolongation and torsades de pointes in patients taking fluconazole. These reports include seriously ill patients with multiple confounding risk factors, such as structural heart disease, electrolyte abnormalities and concomitant medications that may have been contributory. Patients with hypokalaemia and advanced cardiac failure are at an increased risk for the occurrence of life-threatening ventricular arrhythmias and torsades de pointes. Fluconazole should be administered with caution to patients with these potentially proarrhythmic conditions (see Section 4.8 Adverse Effects (Undesirable Effects)).
CYP2C9, CYP2C19 and CYP3A4 interactions. Fluconazole is a potent CYP2C9 and CYP2C19 inhibitor and a moderate CYP3A4 inhibitor. Fluconazole treated patients who are concomitantly treated with drugs with a narrow therapeutic window metabolised through CYP2C9, CYP2C19 and CYP3A4 should be monitored (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Monitoring of adrenal function. Adrenal insufficiency has been reported in patients receiving other azoles (e.g. ketoconazole).
Cases of adrenal insufficiency were reported in patients receiving fluconazole.
Candidiasis. Studies have shown an increasing prevalence of infections with Candida species other than C. albicans. These are often inherently resistant (e.g. C. krusei and C. auris) or show reduced susceptibility to fluconazole (C. glabrata). Such infections may require alternative antifungal therapy secondary to treatment failure. Therefore, prescribers are advised to take into account the prevalence of resistance in various Candida species to fluconazole (see Section 5.1 Pharmacodynamic Properties).
These capsules contain lactose and should not be given to patients with rare hereditary problems of galactose intolerance, Lapp lactase deficiency or glucose-galactose malabsorption.
Use in hepatic impairment. Fluconazole should be administered with caution to patients with liver dysfunction.
Fluconazole has been associated with rare cases of serious hepatic toxicity including fatalities, primarily in patients with serious underlying medical conditions. In cases of fluconazole-associated hepatotoxicity, no obvious relationship to total daily dose, duration of therapy, sex or age of patient has been observed.
Patients who develop abnormal liver function tests during fluconazole therapy should be monitored for the development of more severe liver injury. Fluconazole should not be used again if clinical signs and symptoms consistent with liver disease develop, that may be attributable to fluconazole (see Section 4.8 Adverse Effects (Undesirable Effects)).
Use in renal impairment. Fluconazole should be administered with caution to patients with renal dysfunction.
Use in the elderly. No adjustments in single dose therapy are necessary in elderly patients with minor to moderate renal impairment.
Paediatric use. Fluconazole is not recommended for use in children under 18 years of age except under medical advice.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Fluconazole is an inhibitor of the cytochrome P450 system, particularly the CYP2C and to a lesser extent, the CYP3A isoforms. Co-administration of fluconazole with some other drugs metabolised primarily by these P450 isoforms may result in altered plasma concentrations of these drugs that could change therapeutic effects and/or adverse event profiles.
Clinically or potentially significant drug interactions have been observed between fluconazole and the following agents: short acting benzodiazepines, cisapride, coumarin-type anticoagulants, ciclosporin, hydrochlorothiazide, oral hypoglycaemics, phenytoin, rifampicin, rifabutin, tacrolimus and theophylline. These are described in greater detail below. The relevance of the following drug interactions to single dose fluconazole is unknown. Patients on other medications should be advised to consult their doctor or pharmacist before starting fluconazole.
Effects of other medicinal products on fluconazole. The exposure to fluconazole is significantly increased by the concomitant administration of the following agent. Hydrochlorothiazide. Concomitant oral administration of fluconazole 100 mg and hydrochlorothiazide 50 mg for 10 days in normal volunteers resulted in an increase of 41% in Cmax and an increase of 43% in area under the curve (AUC) of fluconazole, compared to fluconazole given alone. Overall the plasma concentrations of fluconazole were approximately 3.26 to 6.52 micromol/L higher with concomitant diuretic. These changes are attributable to a mean net reduction of approximately 20% in renal clearance of fluconazole.
The exposure to fluconazole is significantly decreased by the concomitant administration of the following agent. Rifampicin. Administration of a single oral dose of fluconazole 200 mg after chronic rifampicin administration resulted in a 25% decrease in AUC and a 20% shorter half-life of fluconazole in normal volunteers. Depending on clinical circumstances, an increase of the dose of fluconazole should be considered when it is administered with rifampicin.
Minor or no significant pharmacokinetic interactions that require no dosage adjustment. Gastrointestinal drugs. In fasted normal volunteers, absorption of orally administered fluconazole does not appear to be affected by agents that increase gastric pH. Single dose administration of fluconazole 100 mg with cimetidine 400 mg resulted in a 13% reduction in AUC and 21% reduction in Cmax of fluconazole. Administration of an antacid containing aluminium and magnesium hydroxides immediately prior to a single dose of fluconazole 100 mg had no effect on the absorption or elimination of fluconazole.
Effects of fluconazole on other medicinal products. Fluconazole is a potent inhibitor of cytochrome P450 (CYP) isoenzyme 2C9 and a moderate inhibitor of CYP3A4. In addition to the observed/ documented interactions mentioned below, there is a risk of increased plasma concentration of other compounds metabolized by CYP2C9, CYP2C19 and CYP3A4 co-administered with fluconazole. Therefore caution should be exercised when using these combinations and the patients should be carefully monitored. The enzyme inhibiting effect of fluconazole persists 4-5 days after discontinuation of fluconazole treatment due to the long half-life of fluconazole.
Alfentanil. A study observed a reduction in clearance and distribution volume as well as prolongation of t1/2 of alfentanil following concomitant treatment with fluconazole. A possible mechanism of action is fluconazole's inhibition of CYP3A4. Dosage adjustment of alfentanil may be necessary.
Amitriptyline, nortriptyline. Fluconazole increases the effect of amitriptyline and nortriptyline. 5-Nortriptyline and/or S-amitriptyline may be measured at initiation of the combination therapy and after one week. Dosage of amitriptyline/ nortriptyline should be adjusted, if necessary.
Amphotericin B. Concurrent administration of fluconazole and amphotericin B in infected normal and immunosuppressed mice showed the following results: a small additive antifungal effect in systemic infection with C. albicans, no interaction in intracranial infection with Cryptococcus neoformans, and antagonism of the two drugs in systemic infection with A. fumigatus. The clinical significance of results obtained in these studies is unknown.
Concomitant use of the following agents with fluconazole is contraindicated. Cisapride. Fluconazole 200 mg daily increased the AUC and Cmax of cisapride (20 mg four times daily) both after a single dose (AUC increased 101% and Cmax increased 91%) and multiple doses (AUC increased 192% and Cmax increased 154%). A significant prolongation in QTc interval was recorded. Cardiac events including torsade de pointes have been reported in patients receiving fluconazole and cisapride concomitantly. In most of these cases, the patients appear to have been predisposed to arrhythmias or had serious underlying illness.
The co-administration of fluconazole and cisapride is contraindicated see Section 4.3 Contraindications).
Terfenadine. Because of the occurrence of serious cardiac dysrhythmias secondary to prolongation of the QTc interval in patients receiving azole antifungals in conjunction with terfenadine, interaction studies have been performed. One study at a 200 mg daily dose of fluconazole failed to demonstrate a prolongation in QTc interval. Another study at a 400 mg and 800 mg daily dose of fluconazole demonstrated that fluconazole taken in doses of 400 mg per day or greater significantly increases plasma levels of terfenadine when taken concomitantly. The combined use of fluconazole at doses of 400 mg or greater with terfenadine is contraindicated. The coadministration of fluconazole at doses lower than 400 mg per day with terfenadine should be carefully monitored. (See Section 4.3 Contraindications).
Astemizole. Concomitant administration of fluconazole with astemizole may decrease the clearance of astemizole. Resulting increased plasma concentrations of astemizole can lead to QT prolongation and rare occurrences of torsade de pointes. Coadministration of fluconazole and astemizole is contraindicated (see Section 4.3 Contraindications).
Pimozide. Although not studied in vitro or in vivo, concomitant administration of fluconazole with pimozide may result in inhibition of pimozide metabolism. Increased pimozide plasma concentrations can lead to QT prolongation and rare occurrences of torsade de pointes. Coadministration of fluconazole and pimozide is contraindicated (see Section 4.3 Contraindications).
Quinidine. Although not studied in vitro or in vivo, concomitant administration of fluconazole with quinidine may result in inhibition of quinidine metabolism. Use of quinidine has been associated with QT prolongation and rare occurrences of torsade de pointes.
Coadministration of fluconazole and quinidine is contraindicated.
Erythromycin. Concomitant use of fluconazole and erythromycin has the potential to increase the risk of cardiotoxicity (prolonged QT interval, torsade de pointes) and consequently sudden heart death. Coadministration of fluconazole and erythromycin is contraindicated (see Section 4.3 Contraindications).
Concomitant use that should be used with caution. Amiodarone. Concomitant administration of fluconazole with amiodarone may increase QT prolongation. Caution must be exercised if the concomitant use of fluconazole and amiodarone is necessary, notably with high-dose fluconazole (800 mg).
Lemborexant. Concomitant administration of fluconazole increased Lemborexant Cmax and AUC by approximately 1.6 and 4.2 - fold, respectively which is expected to increase risk of adverse reactions, such as somnolence. Avoid concomitant use of lemborexant.
Interaction of fluconazole with the following agents may result in increased exposure to these drugs. Careful monitoring and/or dosage adjustment should be considered.
Anticoagulants. Careful monitoring of prothrombin time in patients receiving fluconazole and indanedione anticoagulants is recommended.
Short-acting benzodiazepines. Studies in human subjects have reported changes in midazolam pharmacokinetics and clinical effects that are dependent on dosage and route of administration. Single doses of fluconazole 150 mg resulted in modest increases in midazolam concentrations and psychomotor effects following oral administration of 10 mg that may not be clinically significant. At doses used to treat systemic mycoses, fluconazole resulted in substantial increases in midazolam concentration and psychomotor effects following oral administration of midazolam 7.5 mg, but only modest increases that are not likely to be clinically significant following intravenous infusion of midazolam 0.05 mg/kg. This effect on midazolam appears to be more pronounced following oral administration of fluconazole than with fluconazole administered intravenously. There have been reports of sleepiness and disturbed consciousness in patients taking fluconazole for systemic mycoses and triazolam. However, in most of these cases the patients had serious underlying illnesses and/or concomitant therapies that could have contributed to the reported events and a true fluconazole-triazolam interaction has not been established. If concomitant benzodiazepine therapy is necessary in patients being treated with fluconazole, consideration should be given to decreasing the benzodiazepine dosage, and monitoring the patient's response.
Fluconazole increases the AUC of triazolam (single dose) by approximately 50%, Cmax with 20-32% and increases the half-life by 25-50% due to the inhibition of metabolism of triazolam. Dosage adjustments of triazolam may be necessary.
Calcium channel blockers. Certain dihydropyridine calcium channel antagonists (nifedipine, isradipine, amlodipine, verapamil and felodipine) are metabolised by CYP3A4. Fluconazole has the potential to increase the systemic exposure of the calcium channel antagonists. Frequent monitoring for adverse events is recommended.
Carbamazepine. Azole antifungals may raise carbamazepine plasma concentrations. Since high plasma concentrations of carbamazepine and/or carbamazepine-10, 11-epoxy may result in adverse effects (e.g. dizziness, drowsiness, ataxia, diplopia), the dosage of carbamazepine should be adjusted accordingly and/or plasma concentrations monitored when used concomitantly with fluconazole.
Celecoxib. During concomitant treatment with fluconazole (200 mg daily) and celecoxib (200 mg) the celecoxib Cmax and AUC increased by 68% and 134%, respectively. Half of the celecoxib dose may be necessary when combined with fluconazole.
Ciclosporin. Fluconazole significantly increases the concentration and AUC of ciclosporin. This combination may be used by reducing the dosage of ciclosporin depending on ciclosporin concentration.
Cyclophosphamide. Combination therapy with cyclophosphamide and fluconazole results in an increase in serum bilirubin and serum creatinine. The combination may be used while taking increased consideration to the risk of increased serum bilirubin and serum creatinine.
Everolimus. Although not studied in vivo or in vitro, fluconazole may increase serum concentrations of everolimus through inhibition of CYP3A4.
Fentanyl. One fatal case of possible fentanyl-fluconazole interaction was reported. The author judged that the patient died from fentanyl intoxication. Furthermore, in a randomised crossover study with twelve healthy volunteers it was shown that fluconazole delayed the elimination of fentanyl significantly. Elevated fentanyl concentration may lead to respiratory depression.
Halofantrine. Fluconazole can increase halofantrine plasma concentration due to an inhibitory effect on CYP3A4.
HMG-CoA reductase inhibitors. The risk of myopathy and rhabdomyolysis increases (dose-dependent) when fluconazole is coadministered with HMG-CoA reductase inhibitors metabolised through CYP3A4, such as atorvastatin and simvastatin, or through CYP2C9, such as fluvastatin (decreased hepatic metabolism of the statin). If concomitant therapy is necessary, the patient should be observed for symptoms of myopathy and rhabdomyolysis and creatinine kinase should be monitored. HMG-CoA reductase inhibitors should be discontinued if a marked increase in creatinine kinase is observed or myopathy/rhabdomyolysis is diagnosed or suspected. Lower doses of HMG-CoA reductase inhibitors may be necessary as instructed in the statins prescribing information.
Ibrutinib. Moderate inhibitors of CYP3A4 such as fluconazole increase plasma ibrutinib concentrations and may increase risk of toxicity. If the combination cannot be avoided, reduce the dose of ibrutinib as instructed in ibrutinib prescribing information and provide close clinical monitoring.
Ivacaftor (alone or combined with drugs in the same therapeutic class). Coadministration with ivacaftor, a cystic fibrosis transmembrane conductance regulator (CFTR) potentiator, increased ivacaftor exposure by 3-fold. A reduction of the ivacaftor (alone or combined) dose is necessary as instructed in the ivacaftor (alone or combined) prescribing information.
Losartan. Fluconazole inhibits the metabolism of losartan to its active metabolite (E-31 74) which is responsible for most of the angiotensin II receptor antagonism that occurs during treatment with losartan. Patients should have their blood pressure monitored continuously.
Lurasidone. Moderate inhibitors of CYP3A4 such as fluconazole may increase lurasidone plasma concentrations. If concomitant use cannot be avoided, reduce the dose of lurasidone as instructed in the lurasidone prescribing information.
Methadone. Fluconazole may enhance the serum concentration of methadone. Dosage adjustment of methadone may be necessary.
Nonsteroidal anti-inflammatory drugs (NSAIDs). Although not specifically studied, fluconazole has the potential to increase the systemic exposure of other NSAIDs that are metabolized by CYP2C9 (e.g. naproxen, lornoxicam, meloxicam, diclofenac). Frequent monitoring for adverse events and toxicity related to NSAIDs is recommended. Adjustment of dosage of NSAIDs may be needed.
Olaparib. Moderate inhibitors of CYP3A4 such as fluconazole increase olaparib plasma concentrations. Concomitant use is not recommended. If the combination cannot be avoided, reduce the dose of olaparib as instructed in the Lynparza (olaparib) Prescribing Information.
Oral hypoglycaemic agents. The effects of fluconazole on the pharmacokinetics of the sulfonylurea oral hypoglycaemic agents tolbutamide, glipizide and glibenclamide were examined in three placebo controlled crossover studies in normal volunteers. All subjects received the sulfonylurea alone and following treatment with fluconazole 100 mg as a single daily oral dose for seven days. Fluconazole administration resulted in significant increases in Cmax and AUC of the sulfonylurea. Several subjects in these three studies experienced symptoms consistent with hypoglycaemia. In the glibenclamide study, several volunteers required oral glucose treatment. As fluconazole is a potent inhibitor of CYP2C8 and CYP2C9, it may also interact with other sulfonylureas (e.g. glimepiride and gliclazide) and the thiazolidinediones (e.g. pioglitazone and rosiglitazone), which are metabolised by these enzymes.
When fluconazole and sulfonylureas or thiazolidinediones are coadministered, blood glucose concentrations should be monitored carefully, and the dose of sulfonylurea oral hypoglycaemic agent adjusted accordingly. The possibility of a hypoglycaemic episode should be borne in mind.
Phenytoin. Fluconazole inhibits the hepatic metabolism of phenytoin. With coadministration, serum phenytoin concentration levels should be monitored in order to avoid phenytoin toxicity.
Prednisone. There was a case report that a liver transplanted patient treated with prednisone developed acute adrenal cortex insufficiency when a three month therapy with fluconazole was discontinued. The discontinuation of fluconazole presumably caused an enhanced CYP3A4 activity which led to increased metabolism of prednisone. Patients on long-term treatment with fluconazole and prednisone should be carefully monitored for adrenal cortex insufficiency when fluconazole is discontinued. However such an event is unlikely to occur following a single dose of fluconazole.
Rifabutin. There have been reports that an interaction exists when fluconazole is administered concomitantly with rifabutin, leading to increased serum levels of rifabutin up to 80%. There have been reports of uveitis in patients whom fluconazole and rifabutin were co-administered. Patients receiving rifabutin and fluconazole concomitantly should be carefully monitored.
Saquinavir. Fluconazole increases the AUC of saquinavir and decreases clearance of saquinavir due to inhibition of saquinavir's hepatic metabolism by CYP3A4 and inhibition of P-glycoprotein. Dosage adjustment of saquinavir may be necessary.
Sirolimus. Fluconazole increases plasma concentrations of sirolimus presumably by inhibiting the metabolism of sirolimus via CYP3A4 and P-glycoprotein. This combination may be used with a dosage adjustment of sirolimus depending on the effect/ concentration measurements.
Sulfonylureas. Fluconazole has been shown to prolong the serum half-life of concomitantly administered oral sulfonylureas (e.g. chlorpropamide, glibenclamide, glipizide, tolbutamide) in healthy volunteers. Frequent monitoring of blood glucose and appropriate reduction of sulfonylurea dosage is recommended during coadministration.
Tacrolimus. Fluconazole may increase the serum concentrations of orally administered tacrolimus up to 5 times due to inhibition of tacrolimus metabolism through CYP3A4 in the intestines. No significant pharmacokinetic changes have been observed when tacrolimus is given intravenously. Increased tacrolimus levels have been associated with nephrotoxicity. Dosage of orally administered tacrolimus should be decreased depending on tacrolimus concentration. Patients receiving tacrolimus and fluconazole concomitantly should be carefully monitored.
Theophylline. In a placebo-controlled interaction study, the administration of fluconazole 200 mg for 14 days resulted in an 18% decrease in the mean plasma clearance of theophylline. Patients who are receiving high doses of theophylline or who are otherwise at increased risk of theophylline toxicity should be observed for signs of theophylline toxicity while receiving fluconazole and therapy modified appropriately if signs of toxicity develop.
Tofacitinib. Exposure is increased when tofacitinib is coadministered with medications that result in both moderate inhibition of CYP3A4 and potent inhibition of CYP2C19 (e.g. fluconazole). Dosage adjustment of tofacitinib may be necessary.
Tolvaptan. Exposure to tolvaptan is significantly increased (200% in AUC; 80% in Cmax) when tolvaptan, a CYP3A4 substrate, is co-administered with fluconazole, a moderate CYP3A4 inhibitor, with risk of significant increase in adverse effects particularly significant diuresis, dehydration and acute renal failure. In case of concomitant use, the tolvaptan dose should be reduced as instructed in the tolvaptan prescribing information and the patient should be frequently monitored for any adverse reactions associated with tolvaptan.
Vinca alkaloids. Although not studied, fluconazole may increase the plasma levels of the vinca alkaloids (e.g. vincristine and vinblastine) and lead to neurotoxicity, which is possibly due to an inhibitory effect on CYP3A4.
Vitamin A. Based on a case report in one patient receiving combination therapy with all-trans-retinoid acid (an acid form of vitamin A) and fluconazole, CNS related undesirable effects have developed in the form of pseudotumour cerebri, which disappeared after discontinuation of fluconazole treatment. This combination may be used but the incidence of CNS related undesirable effects should be borne in mind.
Warfarin. A single dose of warfarin 15 mg given to normal volunteers, following 14 days of orally administered fluconazole 200 mg resulted in a 12% increase in the prothrombin time response (area under the prothrombin time-time curve). One of 13 subjects experienced a two-fold increase in prothrombin time response. In postmarketing experience, as with other azole antifungals, bleeding events (bruising, epistaxis, gastrointestinal bleeding, haematuria and melaena) have been reported in association with increases in prothrombin time in patients receiving fluconazole concurrently with warfarin. Careful monitoring of prothrombin time in patients receiving fluconazole and coumarin-type anticoagulants is recommended.
Zidovudine. Fluconazole increases Cmax and AUC of zidovudine, respectively, due to decrease in oral zidovudine clearance. The half-life of zidovudine was likewise prolonged following combination therapy with fluconazole. Patients receiving this combination should be monitored for the development of zidovudine related adverse reactions. Dosage reduction of zidovudine may be considered.
Voriconazole (CYP2C9, CYP2C19 and CYP3A4 inhibitor). Concomitant administration of voriconazole and fluconazole at any dose is not recommended.
Minor or no significant pharmacokinetic interactions that require no dosage adjustment. Oral contraceptives. Oral contraceptives were administered as a single dose both before and after oral administration of fluconazole 50 mg once daily for ten days in ten healthy women. There was no significant difference in ethinyloestradiol or levonorgestrol AUC after the administration of fluconazole 50 mg. The mean increase in ethinyloestradiol AUC was 6% (range: -47 to 108%) and levonorgestrol AUC increased 17% (range: -33 to 141%).
In a second study, 25 normal females received daily doses of fluconazole 200 mg tablets or placebo for two ten-day periods. The treatment cycles were one month apart with all subjects receiving fluconazole during one cycle and placebo during the other. Single doses of an oral contraceptive tablet containing levonorgestrol and ethinyloestradiol were administered on the final treatment day (day 10) of both cycles. Following administration of fluconazole 200 mg, the mean percentage increase in AUC for levonorgestrol compared to placebo was 25% (range: -12 to 82%) and the mean percentage increase for ethinyloestradiol compared to placebo was 38% (range: -11 to 101%). Both of these increases were statistically significantly different from placebo.
In a third study, 21 healthy women received weekly doses of fluconazole 300 mg and single doses of ethinyloestradiol 35 microgram and norethindrone 0.5 mg. AUC of ethinyloestradiol was increased by 24% (range: 3 to 59%) and AUC of norethindrone was increased by 13% (range: -5 to 36%).
Multiple doses of fluconazole may increase exposure to hormone levels in women taking oral contraceptives and are unlikely to result in decreased efficacy of the oral contraceptive.
Two way interactions. Minor or no significant pharmacokinetic interactions that require no dosage adjustment. Azithromycin. An open label, randomised, three way crossover study in 18 healthy subjects assessed the effect of a single oral dose of azithromycin 1,200 mg on the pharmacokinetics of a single oral dose of fluconazole 800 mg as well as the effects of fluconazole on the pharmacokinetics of azithromycin. The estimated ratio of the mean AUC of fluconazole coadministered with azithromycin to fluconazole administered alone was 101%. The estimated ratio of the mean AUC of azithromycin coadministered with fluconazole to azithromycin administered alone was 107%. The estimated ratio of the mean Cmax of fluconazole coadministered with azithromycin to fluconazole administered alone was 104%. The estimated ratio of the mean Cmax of azithromycin coadministered with fluconazole to azithromycin administered alone was 82%. See Table 1.

4.6 Fertility, Pregnancy and Lactation
Effects on fertility. Fluconazole did not affect the fertility of male or female rats treated orally with daily doses of 5, 10 or 20 mg/kg or with parenteral doses of 5, 25 or 75 mg/kg, although the onset of parturition was slightly delayed at 20 mg/kg/p.o. In an intravenous perinatal study in rats at 5, 20 and 40 mg/kg, dystocia and prolongation of parturition were observed in a few dams at 20 mg/kg and 40 mg/kg, but not at 5 mg/kg. The disturbances in parturition were reflected by a slight increase in the number of stillborn pups and decrease of neonatal survival at these dose levels. The effects on parturition in rats are consistent with the species specific oestrogen lowering property produced by high doses of fluconazole. Such a hormone change has not been observed in women treated with fluconazole (see Section 5.1 Pharmacodynamic Properties).
Use in pregnancy. (Category D)
There have been reports of spontaneous abortion and congenital abnormalities in infants whose mothers were treated with 150 mg of fluconazole as a single or repeated dose in the first trimester.
In one large observational cohort study, first trimester exposure to oral fluconazole was associated with a small increased risk of musculoskeletal malformations, corresponding to approximately 1 additional case per 1000 women treated with cumulative doses ≤ 450 mg compared with women treated with topical azoles and to approximately 4 additional cases per 1000 women treated with cumulative doses over 450 mg. The adjusted relative risk was 1.29 (95% CI 1.05 to 1.58) for 150 mg oral fluconazole and 1.98 (95% CI 1.23 to 3.17) for doses over 450 mg fluconazole.
There are no adequate and well-controlled studies in pregnant women. There have been reports of multiple congenital abnormalities in infants whose mothers were being treated for 3 or more months with high dose (400-800 mg/day) fluconazole therapy for coccidiomycosis. The relationship between fluconazole use and these events is unclear. Adverse foetal effects have been seen in animals only at high dose levels associated with maternal toxicity. These findings are not considered relevant to fluconazole used at therapeutic doses.
Fluconazole should not be used in women who are pregnant or in women of childbearing potential, unless adequate contraception is employed. Effective contraceptive measures should continue throughout the treatment period and for approximately 1 week (5 to 6 half-lives) after the final dose.
Australian Categorisation Definition of Category D: Drugs, which have caused, are suspected to have caused or may be expected to cause, an increased incidence of human foetal malformations or irreversible damage. These drugs may also have adverse pharmacological effects. Accompanying texts should be consulted for further details.
Use in pregnancy should be avoided except in patients with severe or potentially life-threatening fungal infections in whom fluconazole may be used if the anticipated benefit outweighs the possible risk to the foetus.
Use in lactation. Fluconazole has been found in human breast milk at concentrations similar to plasma, hence its use in nursing mothers is not recommended.
4.7 Effects on Ability to Drive and Use Machines
When driving vehicles or operating machinery it should be taken into account that occasionally dizziness or seizures may occur.
4.8 Adverse Effects (Undesirable Effects)
Drug reaction with eosinophilia and systemic symptoms (DRESS) has been reported in association with fluconazole treatment (see Section 4.4 Special Warnings and Precautions for Use).
Fluconazole is generally well tolerated. See Table 2.

Cardiac disorders. Torsades de pointes (see Section 4.4 Special Warnings and Precautions for Use).
Gastrointestinal disorders. Dyspepsia, vomiting.
Nervous system disorders. Dizziness, seizures.
Immune system disorders. Anaphylaxis (including face oedema, angioedema, urticaria and pruritus).
Metabolism and nutrition disorders. Hypercholesterolaemia, hypertriglyceridaemia and hypokalaemia.
Hepatobiliary disorders. Hepatocellular necrosis, hepatic failure, hepatitis, jaundice.
Investigations. QT prolongation (see Section 4.4 Special Warnings and Precautions for Use).
Skin and subcutaneous tissue disorders. Alopecia, exfoliative skin disorders including Stevens-Johnson syndrome and toxic epidermal necrolysis, drug reaction with eosinophilia and systemic symptoms (DRESS).
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
Symptoms. The minimal lethal human dose has not been established. There have been plenty of reports of overdosage with fluconazole, and in one case, a 42-year old patient infected with human immunodeficiency virus developed hallucinations and exhibited paranoid behaviour after reportedly ingesting 8,200 mg of fluconazole. The patient was admitted to hospital and his condition resolved within 48 hours.
Signs and symptoms are likely to be an extension of those under Section 4.8 Adverse Effects (Undesirable Effects).
Treatment. There is no specific antidote. Treatment is symptomatic and supportive, including respiratory and cardiovascular function. Monitor for hypokalaemia and elevated liver enzymes; and obtain a full blood count to monitor for possible thrombocytopenia and agranulocytosis.
Fluconazole is largely excreted in the urine; forced volume diuresis would probably increase the elimination rate. A three hour haemodialysis session decreases plasma levels by approximately 50%.
Contact the Poisons Information Centre on 13 11 26 (Australia) for advice on the management of overdosage.
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Fluconazole is a member of the bis-triazole class of antifungal agents. Fluconazole is a highly selective inhibitor of fungal cytochrome P450 sterol C-14 alpha demethylation. Mammalian cell demethylation is much less sensitive to fluconazole inhibition. The subsequent loss of normal sterols correlates with the accumulation of 14 alpha-methyl sterols in fungi and may be responsible for the fungistatic activity of fluconazole. Fluconazole 50 mg daily, given up to 28 days has been shown not to affect corticosteroid levels or ACTH stimulated response in healthy female volunteers. Plasma oestradiol levels and urinary free cortisol levels were decreased with little effect on plasma testosterone levels. Interaction studies with antipyrine indicate that single or multiple doses of fluconazole 50 mg do not affect its metabolism.
Susceptibility in vitro. In vitro, fluconazole displays antifungal activity against clinically common Candida species (including C. albicans, C. parapsilosis, C. tropicalis). C. glabrata shows reduced susceptibility to fluconazole while C. krusei and C. auris are resistant to fluconazole. The minimum inhibitory concentrations (MICs) and epidemiological cut-off value (ECOFF) of fluconazole for C. guilliermondii are higher than for C. albicans.
Fluconazole also exhibits activity in vitro against Cryptococcus neoformans and Cryptococcus gattii as well as the endemic moulds Blastomyces dermatitidis, Coccidioides immitis, Histoplasma capsulatum and Paracoccidioides brasiliensis.
Pharmacokinetic/ pharmacodynamic relationship. In animal studies, there is a correlation between MIC values and efficacy against experimental mycoses due to Candida spp. In clinical studies, there is an almost 1:1 linear relationship between the AUC and the dose of fluconazole. There is also a direct though imperfect relationship between the AUC or dose and a successful clinical response of oral candidosis and to a lesser extent candidaemia to treatment. Similarly cure is less likely for infections caused by strains with a higher fluconazole MIC.
Mechanisms of resistance. Candida spp have developed a number of resistance mechanisms to azole antifungal agents. Fungal strains which have developed one or more of these resistance mechanisms are known to exhibit high MICs to fluconazole which impacts adversely efficacy in vivo and clinically.
In usually susceptible species of Candida, the most commonly encountered mechanism of resistance development involves the target enzymes of the azoles, which are responsible for the biosynthesis of ergosterol. Resistance may be caused by mutation, increased production of an enzyme, drug efflux mechanisms, or the development of compensatory pathways.
There have been reports of superinfection with Candida species other than C. albicans, which often have reduced susceptibility (C. glabrata) or resistance to fluconazole (e.g. C. krusei, C. auris). Such infections may require alternative antifungal therapy. The resistance mechanisms have not been completely elucidated in some intrinsically resistant (C. krusei) or emerging (C. auris) species of Candida.
Susceptibility testing breakpoints. Based on analyses of pharmacokinetic/pharmacodynamic (PK/PD) data, susceptibility in vitro and clinical response EUCAST-AFST (European Committee on Antimicrobial susceptibility Testing-subcommittee on Antifungal Susceptibility Testing) has determined breakpoints for fluconazole for Candida species (EUCAST Fluconazole rationale document (2020)-version 3; European Committee on Antimicrobial Susceptibility Testing, Antifungal Agents, Breakpoint tables for interpretation of MICs, Version 10.0, valid from 2020-02-04). These have been divided into non-species related breakpoints; which have been determined mainly on the basis of PK/PD data and are independent of MIC distributions of specific species, and species related breakpoints for those species most frequently associated with human infection. These breakpoints are given in Table 3:

Microbiology. Fluconazole administered orally or intravenously was active in a variety of animal models of fungal infections using standard laboratory strains of fungi. Fluconazole exhibits in vitro activity against Cryptococcus neoformans and Candida spp. Activity has been demonstrated in vivo in normal and immunocompromised animals against infections with Candida spp., including systemic candidiasis and in normal animals with C. neoformans, including intracranial infections. One case of cross-resistance of Candida to fluconazole in a patient (non-HIV) previously treated with ketoconazole has been reported. The efficacy of fluconazole in vivo is greater than would be apparent from in vitro testing against the above-mentioned fungi. Concurrent administration of fluconazole and amphotericin B in infected normal and immunocompromised mice showed antagonism of the two drugs in systemic infection with Aspergillus fumigatus. The clinical significance of results obtained in these studies is unknown.
Clinical trials. No data available.
5.2 Pharmacokinetic Properties
Absorption. Adults. The pharmacokinetic properties of fluconazole are similar following administration by the intravenous or oral routes.
In normal volunteers, the bioavailability of orally administered fluconazole is over 90% compared with intravenous administration. In fasted normal volunteers, peak plasma concentrations occur between 1 and 2 hours postdose with a terminal plasma elimination half-life of approximately 30 hours (range 20-50 hours). Plasma concentrations are proportional to dose and steady-state levels are reached within 5-10 days with oral doses of 50-400 mg once daily. Steady-state levels are approximately 2.5 times the levels achieved with single doses. Administration of loading dose (on day 1) of twice the usual daily dose enables plasma levels to approximate to 90% steady state levels by day 2.
Distribution. Adults. The apparent volume of distribution approximates to total body water. Plasma protein binding is low (11-12%).
Fluconazole has been found to achieve good penetration into all tissues and body fluids studied. See Table 4.
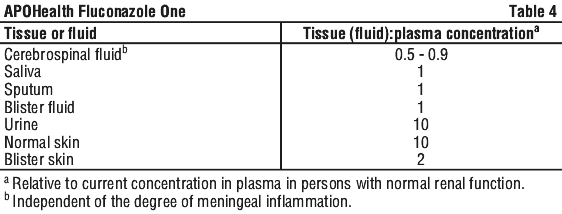
Children. There are differences in the pharmacokinetics of fluconazole between adults and children, with children, after the neonatal period, generally having a faster elimination rate and larger volume of distribution than adults.
5.3 Preclinical Safety Data
Genotoxicity. Fluconazole, with or without metabolic activation, was negative in tests for mutagenicity in 4 strains of Salmonella typhimurium and in the mouse lymphoma system. Cytogenetic studies in vivo and in vitro showed no evidence of chromosomal mutations.
Carcinogenicity. Fluconazole showed no evidence of carcinogenic potential in mice and rats treated orally for 24 months at doses of 2.5, 5 or 10 mg/kg/day (approximately 2-7 x recommended human dose). Male rats treated with 5 and 10 mg/kg/day had an increased incidence of hepatocellular adenomas.
6 Pharmaceutical Particulars
6.1 List of Excipients
In addition, each capsule contains the following inactive ingredients: lactose monohydrate, maize starch, colloidal anhydrous silica, purified talc, sodium lauryl sulfate, gelatin, titanium dioxide, patent blue V.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine, see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C.
6.5 Nature and Contents of Container
Each PVC/PE/PVDC/Aluminium blister pack contains one capsule. AUST R 152959.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Fluconazole is a white to off-white crystalline powder, which is sparingly soluble in water and saline.
Chemical structure. Chemical name: 2-(2,4-diflurophenyl)-1,3-bis(1H-1,2,4-triazol-1-yl)-2-propanol.
Structural formula:
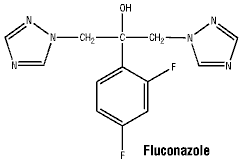
Molecular weight: 306.3.
CAS number. 86386-73-4.
7 Medicine Schedule (Poisons Standard)
S3 - Pharmacist Only Medicine.
Date of First Approval
04 June 2008
Date of Revision
29 January 2026
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.