Atrovent UDV
Brand Information
| Brand name | Atrovent UDV |
| Active ingredient | Ipratropium bromide |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Atrovent UDV.
Summary CMI
Atrovent® UDV
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using Atrovent UDV?
Atrovent Unit Dose Vial (UDV) contains the active ingredient ipratropium bromide monohydrate. Atrovent UDV is used to treat asthma, chronic obstructive bronchitis and people who have difficulty breathing during or after surgery using assisted ventilation. For more information, see Section 1. Why am I using Atrovent UDV? in the full CMI.
2. What should I know before I use Atrovent UDV?
Do not use if you have ever had an allergic reaction to ipratropium bromide monohydrate, atropine or any medicine like atropine or any of the ingredients listed at the end of the CMI. Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding. For more information, see Section 2. What should I know before I use Atrovent UDV? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with Atrovent UDV and affect how it works. A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use Atrovent UDV?
- Follow all directions given to you by your doctor or pharmacist carefully.
- Atrovent UDV is intended for inhalation with suitable nebulising equipment and must not be swallowed.
- You will find instructions on how to use Atrovent UDV at the end of this leaflet.
More instructions can be found in Section 4. How do I use Atrovent UDV? in the full CMI.
5. What should I know while using Atrovent UDV?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using Atrovent UDV? in the full CMI.
6. Are there any side effects?
Common but usually mild potential side effects include headaches, dizziness, dry or sore mouth, throat irritation, cough, nausea, vomiting and digestion related issues (e.g. constipation, diarrhoea, indigestion, reflux and wind). Serious potential side effects which require immediate medical attention include allergic reaction, difficulty in breathing, spasm of the muscles around the voice box, causing choking, heartbeat changes, eye irritation or vision changes and difficulty in passing urine. For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
Atrovent® UDV
Active ingredient(s): ipratropium bromide monohydrate
Consumer Medicine Information (CMI)
This leaflet provides important information about using Atrovent UDV. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using Atrovent UDV.
Where to find information in this leaflet:
1. Why am I using Atrovent UDV?
2. What should I know before I use Atrovent UDV?
3. What if I am taking other medicines?
4. How do I use Atrovent UDV?
5. What should I know while using Atrovent UDV?
6. Are there any side effects?
7. Product details
1. Why am I using Atrovent UDV?
Atrovent UDV contains the active ingredient ipratropium bromide monohydrate. It belongs to a group of medicines called anticholinergic bronchodilators.
Atrovent UDV opens up the air passages in people suffering from asthma, chronic bronchitis and difficulty breathing during or after surgery.
It begins to act quickly after use but may take up to 2 hours to give maximum benefit.
Ask your doctor if you have any questions about why Atrovent UDV has been prescribed for you. Your doctor may have prescribed Atrovent UDV for another reason.
There is no evidence that Atrovent UDV is addictive.
Atrovent UDV is available only with a doctor's prescription.
Atrovent UDV is used to treat:
- asthma
- chronic obstructive bronchitis
- people who have difficulty breathing during or after surgery using assisted ventilation.
Asthma is a lung condition where the lining of the lungs becomes inflamed (red and swollen), making it difficult to breathe. This may be due to an allergy to house dust mites, smoke or other irritants.
Chronic obstructive bronchitis is a lung condition that can cause difficulty in breathing, wheeziness and constant coughing.
2. What should I know before I use Atrovent UDV?
Warnings
When you must not use Atrovent UDV
Do not use Atrovent UDV if you have an allergy to:
- ipratropium bromide monohydrate
- similar medicines which contain atropine or medicines like atropine
- any of the ingredients listed at the end of this leaflet
- any other anticholinergic medicines.
Some of the symptoms of an allergic reaction may include:
- shortness of breath, wheezing or troubled breathing
- swelling of the face, lips, tongue or other parts of the body
- rash, itching or hives on the skin
Do not use Atrovent UDV after the expiry date printed on the pack or if the packaging is torn or shows signs of tampering.
If it has expired or is damaged, return it to your pharmacist for disposal.
If you are not sure whether you should start using Atrovent UDV, contact your doctor or pharmacist.
Before you start to use it:
Tell your doctor or pharmacist if you have allergies to any other medicines, foods, preservatives or dyes.
Tell your doctor or pharmacist if you have or have had any of the following medical conditions:
- glaucoma (high pressure in the eye)
- difficulty or pain when passing urine
- constipation
- cystic fibrosis
- hyperreactive airways
If you have not told your doctor or pharmacist about any of the above, tell them before you start using Atrovent UDV.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Tell your doctor or pharmacist if you are pregnant or intend to become pregnant.
Your doctor or pharmacist will discuss the possible risks and benefits of using Atrovent UDV during pregnancy.
Tell your doctor or pharmacist if you are breastfeeding or plan to breastfeed.
Your doctor or pharmacist will discuss the possible risks and benefits of using Atrovent UDV during breastfeeding.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines and Atrovent UDV may interfere with each other. These include:
- medicines used to treat heart problems such as adrenaline
- medicines used to treat asthma or a lung condition called chronic obstructive pulmonary disease (COPD) such as theophylline, salbutamol or tiotropium
- other nebuliser solutions such as disodium cromoglycate.
This is because some nebuliser solutions may not mix well with Atrovent UDV and may need to be nebulised separately.
You may need different amounts of your medicines, or you may need to take different medicines.
Your doctor may prescribe Atrovent UDV with other medicines that relax the air passages for additional symptom relief.
Check with your doctor or pharmacist before mixing other nebuliser solutions with Atrovent UDV. Some nebulised medicines may not mix well with Atrovent UDV and may need to be nebulised separately.
Your doctor and pharmacist have more information on medicines to be careful with or avoid while using Atrovent UDV.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect Atrovent UDV.
4. How do I use Atrovent UDV?
Follow all directions given to you by your doctor or pharmacist carefully. They may differ from the information contained in this leaflet.
You will find instructions on how to use Atrovent UDV at the end of this leaflet.
If you are not sure how to use a nebuliser mask, or do not understand the instructions on the box, ask your doctor or pharmacist for help.
Children should only use Atrovent 250 μg/1mL UDV on medical advice and with the help of an adult.
Fit the nebuliser mask to your or your child's nose and mouth before nebulising and inhaling Atrovent UDV to prevent the mist from contacting the eyes.
Should the mist contact the eyes, immediately flush your eyes with cold tap water for several minutes.
If you find it difficult to breathe in and use your nebulising mask at the same time, talk to your doctor or pharmacist. They may be able to recommend another method.
How much to use
The usual dose for adults and children is stated below:
Adults:
- 1 to 2 vials (250 μg to 500 μg) of Atrovent 250 μg/1mL UDV, or
- 1 vial of Atrovent Adult 500 μg/1mL UDV
diluted to 2-3 mL with normal saline and nebulised until the entire volume of solution is inhaled, 4 times daily.
Children:
- 1 vial of Atrovent 250 μg/1mL UDV, diluted to 2-3 mL with normal saline and nebulised until the entire volume of solution is inhaled, 4 times daily.
Depending on your condition and specific needs, your doctor may advise you to take a different dose.
Instructions for use
Atrovent UDV are intended for inhalation with suitable nebulising equipment and must not be swallowed or given by injection.
Diluted solutions should be freshly prepared before use.
At the end of inhalation, leftover solution from the nebuliser bowl should be discarded.
Take the following steps in using Atrovent UDV and if you have any problems, ask your doctor or pharmacist for assistance.
- Get your nebuliser ready by following the manufacturer's instructions and the advice of your doctor.
- Carefully tear a new vial from the strip. Never use one that has been opened already.
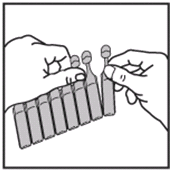
- Open the vial by twisting off the top, always taking care to hold it in an upright position.
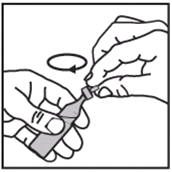
- Squeeze the contents of the vial into the nebuliser bowl. If dilution is necessary, this should be carried out using normal saline and as instructed by your doctor.
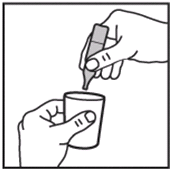
- Dilute with saline up to a final volume of 2-3 mL.
- Assemble the nebuliser and take the medicine or give it to your child as directed by your doctor.
- After nebulisation, follow the manufacturer's instructions about cleaning your nebuliser.
When to use Atrovent UDV
If your doctor has advised you to use Atrovent UDV regularly, then use your medicine at about the same time each day.
Using it at the same time each day will have the best effect. It will also help you remember when to use it.
If you forget to use Atrovent UDV
If it is almost time for your next dose, skip the dose you missed and have your next dose when you are meant to.
Otherwise, use it as soon as you remember, and then go back to using your medicine as you would normally.
Do not use a double dose to make up for the dose that you missed.
This may increase the chance of you getting an unwanted side effect.
If you are not sure what to do, ask your doctor or pharmacist.
If you have trouble remembering to use your medicine, ask your pharmacist for some hints.
How long to use it
Continue using Atrovent UDV for as long as your doctor tells you.
Atrovent UDV helps control your condition, but does not cure it. It is important to keep using it even if you feel well.
If you use too much Atrovent UDV
If you think that you have used too much Atrovent UDV, you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
Symptoms of an overdose may include:
- fast or irregular heartbeat
- dry mouth
- blurred vision
5. What should I know while using Atrovent UDV?
Things you should do
Stop using Atrovent UDV and tell your doctor immediately if you get sudden tightness of the chest, coughing, wheezing or breathlessness immediately after using Atrovent UDV.
These may be signs of a condition called bronchospasm.
If you have an Asthma Action Plan that you have agreed with your doctor, follow it closely at all times.
If you find that the usual dose of Atrovent UDV is not giving as much relief as before, or you need to use it more often, contact your doctor so that your condition can be checked. This is important to ensure your breathing problem is controlled properly.
Continue using Atrovent UDV for as long as your doctor or pharmacist tells you.
Visit your doctor regularly to check on your asthma condition.
Contact your doctor immediately if your breathing suddenly becomes more difficult after using Atrovent UDV.
This may be a sign of an allergic reaction.
Contact your doctor immediately if you experience irritation or a feeling of having something in the eye, or any disturbances with your sight (blurred vision, visual halos or coloured images) together with red eyes, during or after using Atrovent UDV.
This may mean that you have developed a serious eye condition called narrow-angle glaucoma. This can happen if the solution gets in your eyes.
Tell any other doctors, dentists, and pharmacists who are treating you that you are using Atrovent UDV.
Tell your doctor or pharmacist that you are using Atrovent UDV if you are about to start any new medicine.
Tell the surgeon or anesthetist that you are using Atrovent UDV if you plan to have surgery.
It may affect other medicines during surgery.
Tell your doctor or pharmacist immediately if you become pregnant while using Atrovent UDV.
Things you must not do
Do not take any other medicines for your breathing problems without checking with your doctor.
Do not give Atrovent UDV to anyone else, even if they have the same condition as you.
Do not use Atrovent UDV to treat any other complaints unless your doctor or pharmacist tells you to.
Do not stop using Atrovent UDV or lower the dosage, without checking with your doctor or pharmacist.
Do not allow the Atrovent UDV to enter the eyes.
Driving or using machines and other things to be careful of
Be careful before you drive or operating machinery until you know how Atrovent UDV affects you.
Atrovent UDV may cause dizziness and blurred vision in some people. If you have any of these symptoms, do not drive, operate machinery or do anything else that could be dangerous. Children should be careful when performing physical activities.
Looking after your medicine
Keep your Atrovent UDV in a cool, dry place where the temperature stays below 25°C and protect from light.
Do not store it:
- in the bathroom or near a sink, or
- in the car or on window sills.
Heat and dampness can destroy some medicines.
Keep it where young children cannot reach it.
A locked cupboard at least one-and-a-half meters above the ground is a good place to store medicines.
Getting rid of any unwanted medicine
If your doctor tells you to stop using Atrovent UDV or it has passed its expiry date, ask your pharmacist what to do with any medicine that is left over.
6. Are there any side effects?
Tell your doctor or pharmacist as soon as possible if you do not feel well while you are using Atrovent UDV.
This medicine helps most people with asthma or chronic obstructive bronchitis, but it may have unwanted side effects in a few people. All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
Do not be alarmed by the following list of possible side effects.
You may not experience any of them.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
If you get any side effects, do not stop using the Atrovent UDV without first talking to your doctor or pharmacist.
Less serious side effects
| Less serious side effects | What to do |
Brain and nerves:
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
Bladder:
| Call your doctor straight away, if you notice any of these serious side effects. |
Very serious side effects
| Very serious side effects | What to do |
Mouth, throat and airways:
| Call your doctor straight away or go to the Emergency Department at your nearest hospital, if you notice any of these very serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What Atrovent UDV contains
| Active ingredient (main ingredient) |
|
| Other ingredients (inactive ingredients) |
|
| Potential allergens | None |
Do not take this medicine if you are allergic to any of these ingredients.
Atrovent UDV does not contain lactose, sucrose, gluten, tartrazine or any other azo dyes.
What Atrovent UDV looks like
Atrovent UDV is a clear, colourless solution, supplied as Unit Dose Vials containing 1 mL of solution in packs of 30 vials arranged as 3 individually foil-wrapped strips of 10 unit dose vials, or 10 vials*.
* Not currently distributed in Australia.
Atrovent 250 μg/ 1mL UDV (AUST R 17909)
Each 1 mL of Atrovent 250 µg/1mL UDV contains 261 micrograms of ipratropium bromide monohydrate (equivalent to 250 micrograms of ipratropium bromide)
Atrovent Adult UDV 500 μg/ 1mL (AUST R 58203)
Each 1 mL of Atrovent Adult UDV contains 522 micrograms of ipratropium bromide monohydrate (equivalent to 500 micrograms of ipratropium bromide)
Who distributes Atrovent UDV
Atrovent UDV is supplied in Australia by:
Boehringer Ingelheim Pty Limited
ABN 52 000 452 308
Sydney NSW
www.boehringer-ingelheim.com.au
This leaflet was prepared in August 2025.
® Atrovent is a registered trademark of Boehringer Ingelheim
© Boehringer Ingelheim Pty Limited 2025
Brand Information
| Brand name | Atrovent UDV |
| Active ingredient | Ipratropium bromide |
| Schedule | S4 |
MIMS Revision Date: 01 February 2020
1 Name of Medicine
Ipratropium bromide monohydrate.
2 Qualitative and Quantitative Composition
Each 1 mL of Atrovent Inhalation Solution contains ipratropium bromide monohydrate 261 micrograms (equivalent to 250 micrograms ipratropium bromide).
Each 1 mL of Atrovent Unit Dose Vial (UDV) contains ipratropium bromide monohydrate 261 micrograms (equivalent to 250 micrograms ipratropium bromide).
Each 1 mL of Atrovent Adult Unit Dose Vials (UDV) contains ipratropium bromide monohydrate 522 micrograms (equivalent to 500 micrograms ipratropium bromide).
Excipients with known effect. Atrovent Inhalation Solution contains 0.1 mg benzalkonium chloride in each mL and disodium edetate.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Atrovent is an inhalation solution.
Atrovent Inhalation Solution. Clear, colourless or almost colourless liquid, free from suspended particles in multidose bottle. Contains benzalkonium chloride as the preservative.
Atrovent UDV. Preservative free, clear, colourless or almost colourless liquid, free from suspended particles.
Atrovent Adult UDV. Preservative free, clear, colourless or almost colourless liquid, free from suspended particles.
4 Clinical Particulars
4.1 Therapeutic Indications
Moderate asthmatic attacks; chronic forms of asthma; asthma in patients with diminished cardiac reserve; chronic obstructive bronchitis with bronchospasm; bronchospasm during or after surgery, use during assisted ventilation with a respirator.
Administration of Atrovent via a nebuliser is intended for those patients who cannot use a metered dose aerosol.
4.2 Dose and Method of Administration
Atrovent solution can be administered via a range of commercially available nebulising devices. Where wall oxygen is available, solutions are best administered at a flow rate of 6-8 litres per minute.
Dosage is dependent on the mode of inhalation and the quality of nebulisation. The duration of inhalation can be controlled by the dilution volume. It is advisable not to greatly exceed the recommended daily dose as this suggests additional therapeutic modalities may be needed.
Note. 20 drops from the dropper insert in the multidose bottle equal approximately 261 micrograms of ipratropium bromide monohydrate (equivalent to 250 micrograms ipratropium bromide).
The dosage should be adapted to the individual requirements of the patient; patients should also be kept under medical supervision during treatment. Unless otherwise prescribed, the following doses are recommended.
Adults. The recommended dose is 261-522 micrograms [equivalent to 250-500 micrograms ipratropium bromide], 4 times daily, diluted to 2-3 mL with normal saline, and nebulised until the entire volume of solution is consumed. Daily dose exceeding 2.088 mg (equivalent to 2 mg ipratropium bromide) in adults should be given under medical supervision.
In cases of moderate bronchospasm or with assisted ventilation, a dose in the lower range of 261 micrograms (equivalent to 250 micrograms ipratropium bromide) is recommended. In more severely distressed patients, 522 micrograms ipratropium bromide monohydrate (equivalent to 500 micrograms ipratropium bromide) has been shown to produce optimal bronchodilation.
Atrovent can be administered combined with an inhaled β2-agonist.
Children. The recommended dose is 261 micrograms (equivalent to 250 micrograms ipratropium bromide), 4 times daily, diluted to 2-3 mL with normal saline and nebulised until the entire volume of solution is consumed. Daily dose exceeding 1.044 mg (equivalent to 1 mg ipratropium bromide) in children ≤ 12 years of age should be given under medical supervision.
Atrovent can be administered combined with an inhaled β2-agonist.
It is advisable not to greatly exceed the recommended daily dose.
If therapy does not produce a significant improvement or if the patient's condition gets worse, medical advice must be sought in order to determine a new plan of treatment. In the case of acute or rapidly worsening dyspnoea (difficulty in breathing) a doctor should be consulted immediately.
4.3 Contraindications
Known hypersensitivity to atropine or its derivatives (such as the active substance ipratropium bromide), or to any of the other ingredients of Atrovent (see Section 6.1 List of Excipients).
4.4 Special Warnings and Precautions for Use
Atrovent Inhalation Solution contains 0.1 mg benzalkonium chloride in each mL.
Benzalkonium chloride may cause wheezing and breathing difficulties. Patients with asthma are at an increased risk for these adverse events.
Hypersensitivity. Immediate hypersensitivity reactions may occur after administration of Atrovent, as demonstrated by rare cases of urticaria, angio-oedema, rash, bronchospasm, oropharyngeal oedema and anaphylaxis.
Paradoxical bronchospasm. As with other inhaled medicines Atrovent may result in paradoxical bronchospasm that may be life threatening. If paradoxical bronchospasm occurs Atrovent should be discontinued immediately and substituted with an alternative therapy.
Anticholinergic effects. Like other drugs with anticholinergic activity, ipratropium bromide monohydrate should be avoided or used with caution in patients where atropine-like effects may precipitate or exacerbate a pre-existing clinical condition. Patients at particular risk are those with eyes with narrow iridocorneal angles as acute angle closure glaucoma may be precipitated, or patients with a tendency towards urinary retention or constipation.
Ocular complications. Atrovent should be used with caution in patients predisposed to narrow angle glaucoma.
There have been isolated reports of ocular complications (mydriasis, increased intraocular pressure, acute angle glaucoma, eye pain) as a result of direct eye contact of aerolised ipratropium bromide monohydrate, either alone or in combination with an adrenergic β2-agonist. Thus, patients must be instructed in the correct administration of Atrovent, and warned not to allow the solution or mist to enter the eyes. A nebuliser mask must be fitted properly during inhalation.
Patients who may be predisposed to glaucoma should be specifically warned to protect their eyes. Eye pain or discomfort, blurred vision, visual halos or coloured images, in association with red eyes from conjunctival congestion and corneal oedema, may be signs of acute angle closure glaucoma. Should any combination of these symptoms develop, treatment with miotic drops should be initiated and specialist advice sought immediately.
Renal and urinary effects. Atrovent should be used with caution in patients with pre-existing urinary outflow tract obstruction (e.g. prostatic hyperplasia or bladder neck obstruction).
Gastro-intestinal motility disturbances. Patients with cystic fibrosis may be more prone to gastrointestinal motility disturbances.
Local effects. Atrovent Inhalation Solution in the multidose bottle contains benzalkonium chloride and disodium edetate. When inhaled these agents may cause bronchospasm in sensitive patients with hyper-reactive airways. If the multidose nebulising solution is prescribed, it is suggested that patients be monitored for their FEV1, and if the FEV1 falls, therapy with the preservative free Unit Dose Vials or Metered Dose Aerosol should be used.
Use in the elderly. No data available.
Paediatric use. Paediatric patients can use Atrovent inhalation at the recommended dose.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
The chronic co-administration of Atrovent inhalation with other anticholinergic drugs has not been studied. Therefore, the chronic co-administration of Atrovent with other anticholinergic drugs is not recommended.
Beta-Adrenergics and xanthine preparations may intensify the bronchodilatory effect.
The risk of acute glaucoma in patients with a history of narrow angle glaucoma (see Section 4.4 Special Warnings and Precautions for Use) may be increased when nebulised ipratropium bromide monohydrate and beta-mimetics are administered simultaneously.
Physical compatibility. Atrovent Inhalation Solutions and disodium cromoglycate inhalation solutions that contain the preservative benzalkonium chloride should not be administered simultaneously in the same nebuliser as precipitation may occur.
Atrovent UDVs and disodium cromoglycate inhalation solutions should not be administered simultaneously in the same nebuliser.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. Clinical data on fertility are not available for ipratropium bromide monohydrate.
Use in pregnancy. (Category B1)
Care is recommended during pregnancy, particularly in the first trimester. The safety of Atrovent during pregnancy has not been established. The benefits of using Atrovent when pregnancy is confirmed or suspected must be weighed against possible hazards to the foetus. Studies in rats, mice and rabbits showed no embryo-toxic nor teratogenic effects.
Use in lactation. No specific studies are available to determine the excretion of ipratropium bromide in human breast milk. Although lipid insoluble quaternary cations pass into breast milk, it is unlikely that ipratropium bromide would reach the infant to an important extent, especially when administered by inhalation. However, as many drugs are excreted into breast milk, caution should be exercised when Atrovent is administered to breastfeeding mothers.
4.7 Effects on Ability to Drive and Use Machines
No studies on the effects on the ability to drive and use machines have been performed. However, patients should be advised that they may experience undesirable effects such as dizziness, accommodation disorder, mydriasis and blurred vision during treatment with Atrovent. Therefore, caution should be recommended when driving a car or operating machinery. If patients experience the above mentioned side effects they should avoid potentially hazardous tasks such as driving or operating machinery.
4.8 Adverse Effects (Undesirable Effects)
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
Many of the listed undesirable effects can be assigned to the anticholinergic properties of Atrovent. As with all inhalation therapy Atrovent may show symptoms of local irritation.
The most frequent side effects reported in clinical trials were headache, dizziness, throat irritation, cough, gastrointestinal disorders (including constipation, diarrhoea, gastrointestinal motility disorder, dry mouth, nausea, stomatitis, oedema mouth, and vomiting).
If the substance enters the eyes by inappropriate handling, mild and reversible disturbance of accommodation may occur. Other ocular complications have also been reported (see Section 4.4 Special Warnings and Precautions for Use). However, acute angle-closure glaucoma has been reported following direct eye contact.
Allergic-type reactions such as angio-oedema of the tongue, lips and face, may occur.
The following adverse reactions have been reported during use of Atrovent in clinical trials and during the post-marketing experience at the following frequency: very common (≥ 1/10); common (≥ 1/100, < 1/10); uncommon (≥ 1/1,000, < 1/100); rare (≥ 1/10,000, < 1/1,000); very rare (< 1/10,000). See Table 1.
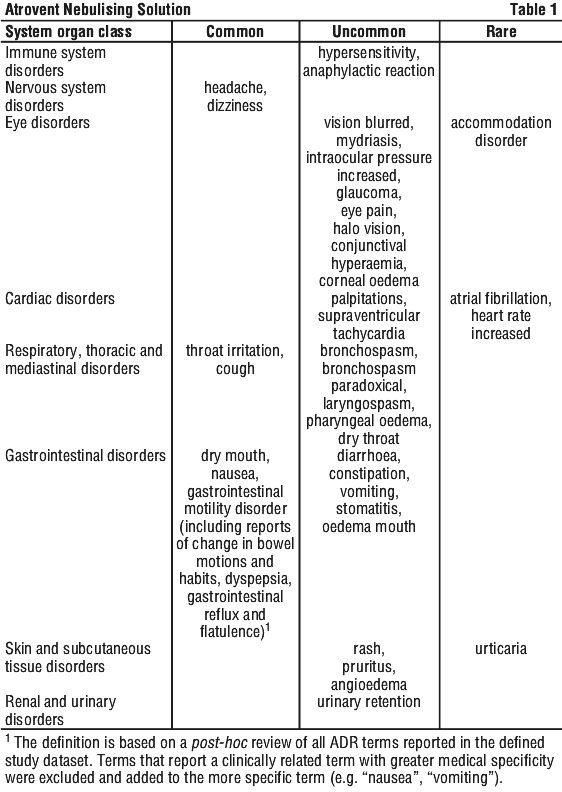
4.9 Overdose
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
No symptoms specific to overdosage have been encountered. In view of the wide therapeutic range and topical administration of Atrovent inhalation solutions, no serious anticholinergic symptoms are to be expected. Minor systemic manifestations of anticholinergic action, including dry mouth, visual accommodation disturbances and tachycardia may occur.
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Pharmacotherapeutic group: Anticholinergics.
ATC code: R03BB01.
Atrovent is an anticholinergic bronchodilator. It appears to inhibit vagally mediated reflexes by antagonising the action of acetylcholine, the transmitter agent released from the vagal nerve. Anticholinergics prevent the increase in intracellular calcium concentration caused by interaction of acetylcholine with the muscarinic receptor on bronchial smooth muscle. Bronchodilation following inhalation of Atrovent is primarily a local, site specific effect at the bronchial smooth muscle. Atrovent has no deleterious effect on airway mucous secretion or mucociliary clearance.
The time course of action of Atrovent also differs from the β2-agonists in that although the onset of bronchodilator response is seen within 3-5 minutes of administration, peak response is not reached until 1.5-2 hours after inhalation. The duration of significant bronchodilator action is up to 6 hours.
Atrovent may be used in combination with β2-agonists. There is evidence that in patients who respond to Atrovent, the concurrent administration of Atrovent and β2-agonists produces a greater relief of bronchospasm than either drug given alone.
Atrovent inhibits acetylcholine-induced bronchospasm and provides partial protection against histamine and allergen-induced bronchospasm.
Clinical trials. No data available.
5.2 Pharmacokinetic Properties
Absorption. Following inhalation, 10 to 30% of the dose (depending on the formulation and inhalation technique) is generally deposited in the lungs. The major part of the dose is swallowed and passes into the gastrointestinal tract. Due to the low gastrointestinal absorption of ipratropium bromide, the bioavailability of the portion of the dose swallowed accounts for approximately 2% of the dose. This fraction of the dose does not make a relevant contribution to the plasma concentrations of the active ingredient. The portion of the dose deposited in the lungs reaches the circulation rapidly (within minutes) and has nearly complete systemic availability.
From renal excretion data (0-24 hours), the total systemic bioavailability (pulmonary and gastrointestinal portions) of inhaled doses of ipratropium bromide was estimated to be in the range 7 to 28%. This is also a valid range for inhalation from Atrovent CFC-free because the kinetic results (renal excretion, AUC and Cmax) from the CFC-free and the CFC containing formulations are approximately comparable.
Distribution. Kinetic parameters describing the disposition of ipratropium bromide were calculated from plasma concentrations after intravenous administration. A rapid biphasic decline in plasma concentrations is observed. The volume of distribution (Vz) is 338 L (approximately 4.6 L/kg). The half-life of the terminal elimination phase is about 1.6 hours. The drug is less than 20% bound to plasma proteins. The ipratropium ion does not cross the blood-brain barrier, consistent with the ammonium structure of the molecule.
The main urinary metabolites bind poorly to the muscarinic receptor and have no activity.
Metabolism. The mean total clearance of the drug is 2.3 L/min. The major portion, approximately 60% of the systemically available dose, is eliminated by metabolic degradation, probably in the liver.
Excretion. Approximately 40% of the systemically available dose is cleared via urinary excretion, corresponding to an experimental renal clearance of 0.9 L/min. After oral dosing less than 1% of the dose is renally excreted, indicating an insignificant absorption of ipratropium bromide from the gastrointestinal tract.
In excretion balance studies, after intravenous administration of a radioactive dose, less than 10% of the drug-related radioactivity (including parent compound and all metabolites), are excreted via the biliary-faecal route. The dominant excretion of drug-related radioactivity occurs via the kidneys.
5.3 Preclinical Safety Data
Genotoxicity. Results of various mutagenicity studies (Ames test, mouse dominant lethal test, mouse micronucleus test and chromosome aberration of bone marrow in Chinese hamsters) were negative.
Carcinogenicity. Two-year oral carcinogenicity studies in rats and mice have revealed no carcinogenic potential at dietary doses up to 6 mg/kg/day for Atrovent.
6 Pharmaceutical Particulars
6.1 List of Excipients
Atrovent Inhalation Solution - multidose bottles and Atrovent UDVs contain sodium chloride, hydrochloric acid and purified water. The multidose solution also contains benzalkonium chloride as preservative and disodium edetate as stabiliser.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store the bottles at below 30°C. After opening the multidose bottle, the solution should be used as soon as possible and any unused solution should be discarded after 28 days.
Store the unopened Unit Dose Vials (UDV) at below 25°C. Protect from light. Diluted solutions should be freshly prepared before use and any solution remaining in the nebuliser, on completion of inhalation, should be discarded.
6.5 Nature and Contents of Container
Atrovent Inhalation Solution are available in glass bottles of 20 mL.
Atrovent UDV are available in LDPE vials; packs of 10* or 30 vials of 1 mL.
Atrovent Adult UDV are available in PE vials; packs of 10* or 30 vials of 1 mL.
* Not currently distributed in Australia.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Ipratropium bromide monohydrate is a synthetic quaternary ammonium compound, chemically related to atropine. The addition of an N-isopropyl group distinguishes the molecule from atropine and is responsible for a lower lipid solubility.
Ipratropium bromide monohydrate is a white or off-white crystalline substance. It is freely soluble in methanol, soluble in water and sparingly soluble in ethanol 96% (v/v).
The chemical name for ipratropium bromide (as monohydrate) is (1R,3r, 5S,8r)-3-[(RS)-(3-hydroxy-2-phenyl-propanoyl)-oxy]-8-methyl-8-(1-methylethyl)-8-azoniabicyclo[3.2.1]octane bromide monohydrate.
The molecular formula is C20H30NO3Br.H2O and the molecular weight is 430.4.
Chemical structure. Ipratropium bromide monohydrate has the following structural formula:
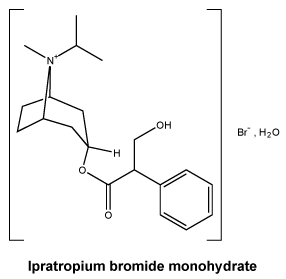
7 Medicine Schedule (Poisons Standard)
S4.
Date of Revision
28 November 2019
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.