Bactrim DS Tablets and Bactrim Oral Suspension
Brand Information
| Brand name | Bactrim DS Tablets and Bactrim Oral Suspension |
| Active ingredient | Trimethoprim + Sulfamethoxazole |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Bactrim DS Tablets and Bactrim Oral Suspension.
Summary CMI
Bactrim® DS Tablets
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using Bactrim DS Tablets?
Bactrim DS Tablets contains the active ingredient sulfamethoxazole and trimethoprim, also known as co-trimoxazole. Bactrim DS Tablets is used to treat bacterial infections in different parts of the body.
For more information, see Section 1. Why am I using Bactrim DS Tablets? in the full CMI.
2. What should I know before I use Bactrim DS Tablets?
Do not use if you have ever had an allergic reaction to Bactrim DS Tablets or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I use Bactrim DS Tablets? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with Bactrim DS Tablets and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use Bactrim DS Tablets?
- Take Bactrim DS Tablets exactly as your doctor has prescribed. The dose and length of time you have to take Bactrim DS Tablets will depend on the type of infection you have. For adults and children over 12 years, the usual dose is one tablet twice per day.
- Swallow Bactrim DS Tablets whole (or halve if necessary) with a glass of water after a meal.
More instructions can be found in Section 4. How do I use Bactrim DS Tablets? in the full CMI.
5. What should I know while using Bactrim DS Tablets?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Drinking alcohol |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using Bactrim DS Tablets? in the full CMI.
6. Are there any side effects?
Common side effects include nausea, vomiting, diarrhoea, abdominal (gut) or stomach discomfort.
Serious side effects include any form of skin rash, jaundice, persistent diarrhoea, severe fever, sore throat, lumps in neck, severe persistent headache, discolouration of urine, renal stones or swelling of face and throat.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
Bactrim® DS Tablets pronounced BACK-TRIM
Active ingredient(s): sulfamethoxazole and trimethoprim
Consumer Medicine Information (CMI)
This leaflet provides important information about using Bactrim DS Tablets. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using Bactrim DS Tablets.
Where to find information in this leaflet:
1. Why am I using Bactrim DS Tablets?
2. What should I know before I use Bactrim DS Tablets?
3. What if I am taking other medicines?
4. How do I use Bactrim DS Tablets?
5. What should I know while using Bactrim DS Tablets?
6. Are there any side effects?
7. Product details
1. Why am I using Bactrim DS Tablets?
Bactrim DS Tablets contains the active ingredient sulfamethoxazole and trimethoprim, also known as co-trimoxazole. Bactrim DS Tablets belongs to a group of medicines called antibiotics. There are many different types of medicines used to treat bacterial infections. Sulfamethoxazole in Bactrim DS Tablets belongs to a group of medicines known as sulfonamides. Trimethoprim belongs to a group of medicines known as the benzylpyrimidines.
Bactrim DS Tablets is used to treat bacterial infections in different parts of the body. It works by stopping the growth of the bacteria causing the infection.
2. What should I know before I use Bactrim DS Tablets?
Warnings
Do not use Bactrim DS Tablets if:
- you are allergic to sulfamethoxazole, trimethoprim, any other sulfonamide, or any of the ingredients listed at the end of this leaflet.
Some of the symptoms of an allergic reaction to Bactrim DS Tablets may include shortness of breath, wheezing or difficulty breathing; swelling of the face, lips, tongue which may cause difficulty in swallowing or breathing; skin rash, itching or hives, peeling of the skin. - you have severe liver or kidney disease, any blood disorder or megaloblastic anaemia.
- the child you are treating is less than 6 weeks of age.
- you have streptococcal pharyngitis
- you are taking dofetilide, a medicine used to treat irregular heartbeats.
- the package is torn or shows signs of tampering.
- the expiry date (EXP) printed on the pack has passed.
Always check the ingredients to make sure you can use this medicine.
Check with your doctor if you:
- have an allergic reaction to any diuretic (fluid) tablet or medicines for diabetes or overactive thyroid. This may increase your chances of an allergic reaction to Bactrim DS Tablets.
- have any type of blood disorder (including porphyria and glucose-6-phosphate dehydrogenase deficiency)
- have kidney or liver disease
- have a hereditary disorder called phenylketonuria
- have epilepsy (fits or convulsions)
- have asthma
- have allergic disorders
- have rheumatoid arthritis
- have urinary obstruction
- have folic acid deficiency
- have an allergy to any other medicines, foods, dyes or preservatives.
- take any medicines for any other condition
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor if you are pregnant or intend to become pregnant.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
Geriatric use
People over 65 years are more at risk of severe side effects when taking Bactrim DS Tablets. The risk is greater if you have kidney or liver disease or are taking some types of other medicines, such as diuretics.
Use in People with HIV infection
People with HIV infection have been reported to get more side effects while being treated with Bactrim DS Tablets than people without HIV.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with Bactrim DS Tablets and affect how it works.
- medicines used to treat diabetes such as repaglinide, rosiglitazone, pioglitazone, glibenclamide, gliclazide, glipizide, chlorpropamide and tolbutamide
- fluid Tablets (diuretics)
- phenytoin, a medicine for epilepsy
- pyrimethamine, a medicine for malaria
- other medicines used to treat infections such as rifampicin, dapsone and polymyxin
- zidovudine, a medicine to treat HIV infection
- cyclosporin, a medicine used to treat organ transplant patients
- warfarin, acenocoumarol, phenprocoumon, medicines used to thin the blood
- medicines used to treat certain heart conditions such as digoxin and amiodarone
- amantadine, a medicine used to treat influenza virus and Parkinson's Disease
- memantine, a medicine used to treat Parkinson's Disease
- urinary acidifiers (for kidney conditions)
- oral contraceptives (“The Pill”)
- sulfinpyrazone, a medicine used to treat gout
- salicylates, medicines to treat conditions such as psoriasis or warts
- medicines used to treat cancer such as paclitaxel, mercaptopurine and methotrexate
- clozapine, a medicine used to treat schizophrenia
- medicines used to treat overactive thyroid conditions
- medicines used to treat depression such as imipramine, clomipramine, amitriptyline, dothiepin, doxepin, nortriptyline and trimipramine
- immunosuppressant medicines such as azathioprine and methotrexate
- medicines used to treat high blood pressure as well as a variety of heart and kidney conditions such as captopril, enalapril, lisinopril, fosinopril, perindopril, quinapril, ramipril, trandolapril valsartan, telmisartan, irbesartan, candesartan, eprosartan, losartan, dofetilide and olmesartan.
These medicines may be affected by Bactrim DS Tablets or may affect how well it works. You may need to use different amounts of your medicine, or you may need to take different medicines. Your doctor will advise you.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect Bactrim DS Tablets.
4. How do I use Bactrim DS Tablets?
How much to take
- Take Bactrim DS Tablets exactly as your doctor has prescribed.
- Your doctor will tell you how much Bactrim DS Tablets to take each day.
- The dose and length of time you have to take Bactrim DS Tablets will depend on the type of infection you have.
- For adults and children over 12 years, the usual dose of Bactrim DS Tablets is one tablet twice per day.
- Follow the instructions provided when Bactrim DS Tablets was prescribed, including the number of days it should be taken.
How to take Bactrim DS Tablets
- Bactrim DS Tablets should be swallowed with a glass of water after a meal.
If you forget to take Bactrim DS Tablets
Bactrim DS Tablets should be used regularly at the same time each day.
If you miss your dose at the usual time, if it is almost time for your next dose, skip the dose you missed and take your next dose when you are meant to.
Do not try to make up for the dose that you missed by taking more than one dose at a time.
If you are not sure what to do, contact your doctor or pharmacist.
If you use too much Bactrim DS Tablets
If you think that you have used too much Bactrim DS Tablets, you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning. You may need urgent medical attention.
If you take too much Bactrim DS Tablets, you may feel sick or vomit, feel dizzy, depressed or confused or have a headache. You may also feel drowsy or become unconscious.
5. What should I know while using Bactrim DS Tablets?
Things you should do
Tell all doctors, dentists and pharmacists who are treating you that you are taking Bactrim DS Tablets.
Tell your doctor if, for any reason, you have not taken your medicine exactly as prescribed. Otherwise, your doctor may think that it was not effective and change your treatment unnecessarily.
Tell your doctor if you feel the Tablets is not helping your condition.
Drink plenty of fluids while you are taking Bactrim DS Tablets. This will help to flush the medicine through your system.
If you are taking Bactrim DS Tablets for a long time, visit your doctor regularly so your progress can be checked. Your doctor may ask you to have regular tests to check your kidneys, liver or blood.
Tell your doctor you are taking Bactrim DS Tablets if you have to have any blood tests. Bactrim DS Tablets may affect the results of some blood tests.
Call your doctor straight away if you:
- become pregnant while taking Bactrim DS Tablets.
- feel the Tablets is not helping your condition.
- get severe diarrhoea, even if it occurs several weeks after stopping Bactrim DS Tablets.
DO NOT take any diarrhoea medicine without first checking with your doctor. Diarrhoea medicines may make your diarrhoea worse or make it last longer.
Remind any doctor, dentist or pharmacist as appropriate you visit that you are using taking Bactrim DS Tablets.
Things you should not do
- Do not stop using this medicine suddenly or change the dose without first checking with your doctor.
- Do not let yourself run out of medicine over the weekend or on holidays.
- Do not give your medicine to anyone else, even if they have the same condition as you.
- Do not take Bactrim DS Tablets to treat any other complaints unless your doctor tells you to.
- Do not take any other medicines whether they require a prescription or not without first telling your doctor or consulting with a pharmacist.
Things to be careful of
Sometimes use of this medicine allows other bacteria and fungi which are not sensitive to Bactrim DS Tablets to grow. If other infections such as thrush occur while you are taking Bactrim DS Tablets, tell your doctor.
If you are going outdoors, wear protective clothing or use a SPF 15+ sunscreen. Your skin may burn more easily while you are taking Bactrim DS Tablets.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how Bactrim DS Tablets affects you.
Drinking alcohol
Tell your doctor if you drink alcohol.
Looking after your medicine
- Keep your Bactrim DS Tablets in the blister pack until it is time to take them. If you take the Tablets out of the blister pack before it is time to take them, they may not keep well.
- Keep Bactrim DS Tablets in a cool dry place where the temperature stays below 30°C.
Follow the instructions in the carton on how to take care of your medicine properly.
Store it in a cool dry place away from moisture, heat or sunlight; for example, do not store it:
- in the bathroom or near a sink, or
- in the car or on window sills.
Keep it where young children cannot reach it.
Getting rid of any unwanted medicine
If you no longer need to use this medicine or it is out of date, take it to any pharmacy for safe disposal.
Do not use this medicine after the expiry date.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
| Speak to your doctor if you have any of these less serious side effects and they worry you. Your doctor will need to treat the thrush infection separately. |
Serious side effects
Call the emergency department immediately if you experience multiple symptoms such as fever, very low blood pressure, increased heart rate or confusion after taking this drug as it may be a sign of shock.
| Serious side effects | What to do |
| Call your doctor straight away or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Other rare side effects
| Other rare side effects | What to do |
| Contact your doctor as soon as possible if you have any of these rare side effects |
Very rarely, people have died from complications due to certain severe skin, liver or blood reactions. Elderly people, people with liver or kidney disease and people taking certain other medicines are more at risk of these severe reactions.
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What Bactrim DS Tablets contains
| Active ingredient (main ingredient) |
|
| Other ingredients (inactive ingredients) |
|
| Potential allergens | NA |
Bactrim DS Tablets are gluten free and lactose free.
Do not take this medicine if you are allergic to any of these ingredients.
What Bactrim DS Tablets look like
Bactrim DS Tablets are white to almost white, oblong, with a breakline on one side and "BACTRIM 800 + 160" on the other side. The Tablets have a breakline so that they can be broken in half if needed.
They are supplied in blister pack of 10 Tablets with AUST R 162563.
Who distributes Bactrim DS Tablets
Echo Therapeutics Pty Ltd
ABN 92628 298 699
Sydney, Australia
www.echotherapeutics.com.au
Medical enquiries: 1300 838 428
This leaflet was prepared in December 2025.
Brand Information
| Brand name | Bactrim DS Tablets and Bactrim Oral Suspension |
| Active ingredient | Trimethoprim + Sulfamethoxazole |
| Schedule | S4 |
MIMS Revision Date: 01 February 2026
1 Name of Medicine
Sulfamethoxazole/ trimethoprim.
2 Qualitative and Quantitative Composition
The tablets contain 800 mg sulfamethoxazole and 160 mg trimethoprim.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Bactrim DS tablets are oblong, biconvex, white to almost white, scored on one side and marked "BACTRIM 800 + 160" on the other side.
4 Clinical Particulars
4.1 Therapeutic Indications
Upper and lower respiratory tract infections, renal and urinary tract infections, genital tract infections, gastrointestinal tract infections, skin and wound infections, septicaemias and other infections caused by sensitive organisms.
4.2 Dose and Method of Administration
Dosage. In acute infections Bactrim should be given for at least five days or until the patient has been symptom-free for two days.
Adults and children over 12 years of age. Standard dosage. One Bactrim DS (double strength) tablet morning and evening after meals.
Minimum dosage. Half a Bactrim DS (double strength) tablet twice daily (see below).
Maximum dosage (for particularly severe infections). One and a half Bactrim DS (double strength) tablets twice daily.
The recommended dose for patients with documented Pneumocystis jirovecii pneumonitis is 20 mg/kg trimethoprim and 100 mg/kg sulfamethoxazole/24 hours given in equally divided doses every six hours for 14 days.
Special populations. Renal impairment. The following dosage regimens are based on published information for the administration of Bactrim DS tablets to patients with reduced kidney function (see Table 1).
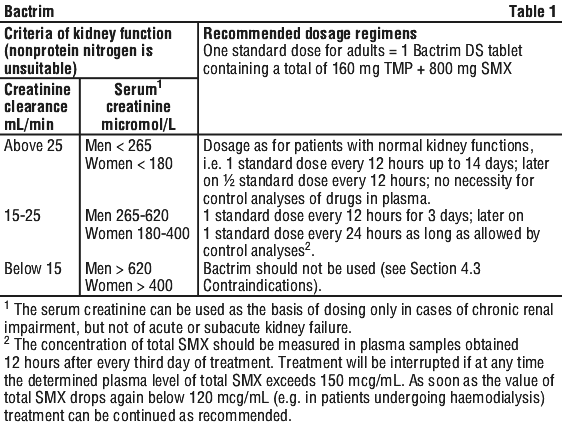
4.3 Contraindications
Bactrim is contraindicated in patients showing marked liver parenchymal damage, blood dyscrasias, megaloblastic bone marrow or severe renal insufficiency, characterised by creatinine clearance < 15 mL/min (see Section 4.2 Dose and Method of Administration).
Bactrim should not be given to patients with a history of hypersensitivity to the active ingredients or the excipients, or other sulfonamides.
Bactrim should not be used in the treatment of streptococcal pharyngitis. Clinical studies have documented that patients with group A β-haemolytic (Sp) streptococcal tonsillopharyngitis have a greater incidence of bacteriologic failure when treated with Bactrim than to those patients treated with penicillin, as evidenced by failure to eradicate this organism from the tonsillopharyngeal area.
Bactrim must not be given in combination with dofetilide (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Bactrim must not be given to premature babies, nor during the first six weeks of life because of the risk of producing kernicterus.
4.4 Special Warnings and Precautions for Use
Use in treatment of Pneumocystis jirovecii pneumonitis in patients with acquired immunodeficiency syndrome (AIDS). Because of their unique immune dysfunction, AIDS patients may not tolerate or respond to Bactrim in the same manner as non-AIDS patients. The incidence of side effects, particularly rash, fever and leucopenia, with Bactrim therapy in AIDS patients who are being treated for Pneumocystis jirovecii pneumonia has been reported to be greatly increased compared with the incidence normally associated with the use of Bactrim in non-AIDS patients.
Use in glucose-6-phosphate dehydrogenase deficiency. In glucose-6-phosphate dehydrogenase deficient individuals, haemolysis may occur. This may be dose related. Bactrim should not be given to patients with a glucose-6-phosphate dehydrogenase deficiency unless absolutely essential, and then only in minimal doses.
Pseudomembranous colitis. The use of Bactrim can lead in very rare instances to the development of severe colitis as a result of colonisation with C. difficile, a toxin producing organism. The colitis, which may or may not be accompanied by the formation of a pseudomembrane in the colon, can be fatal. If significant diarrhoea occurs (this may, however, begin up to several weeks after the cessation of antibiotic therapy), Bactrim should be discontinued. This may be sufficient treatment in the early stages although cholestyramine orally may help by binding the toxin in the colonic lumen. However, in moderate to severe cases appropriate therapy with a suitable oral antibacterial agent effective against C. difficile should be considered.
Drugs which delay peristalsis, e.g. opiates and diphenoxylate with atropine (Lomotil), may prolong and/or worsen the condition and should not be used.
Fluids, electrolytes and protein replacement therapy should be provided when indicated.
Even if an organism is sensitive to trimethoprim, if it is not sensitive to sulfamethoxazole the combination should not be used, to avoid unnecessary exposure to the potential side effects of the sulfonamide component.
Serious adverse reactions. Fatalities, although rare, have occurred due to severe reactions including Stevens-Johnson syndrome, toxic epidermal necrolysis, drug rash with eosinophilia and systemic symptoms (DRESS), acute generalized exanthematous pustulosis (AGEP), fulminant hepatic necrosis, agranulocytosis, aplastic anaemia and other blood dyscrasias.
Circulatory shock. Circulatory shock with fever, severe hypotension, elevated heart rate and confusion requiring intravenous fluid resuscitation and vasopressors has occurred within minutes to hours of rechallenge with sulfamethoxazole/trimethoprim in patients with history of recent (days to weeks) exposure to sulfamethoxazole/trimethoprim.
Hypersensitivity and allergic reactions. Bactrim should be discontinued if a skin rash appears. Clinical signs such as rash, sore throat, fever, arthralgia, cough, shortness of breath, pallor, purpura or jaundice may be early indications of serious reactions.
An adequate urinary output should be maintained at all times. Evidence of crystalluria in vivo is rare, although sulfonamide crystals have been noted in cooled urine from treated patients. In patients suffering from malnutrition, this risk may be increased.
As with other sulfonamide preparations, critical appraisal of benefit versus risk should be made in patients with liver damage, renal damage, urinary obstruction, blood dyscrasias, allergies or bronchial asthma.
Pulmonary infiltrates reported in the context of eosinophilic or allergic alveolitis may manifest through symptoms such as cough or shortness of breath. Should such symptoms appear or unexpectedly worsen, the patient should be re-evaluated and discontinuation of Bactrim therapy considered.
Haemophagocytic lymphohistiocytosis (HLH). Cases of HLH have been reported very rarely in patients treated with sulfamethoxazole/trimethoprim. HLH is a life-threatening syndrome of pathologic immune activation characterised by clinical signs and symptoms of an excessive systemic inflammation (e.g. fever, hepatosplenomegaly, hypertriglyceridaemia, hypofibrinogenaemia, high serum ferritin, cytopenias and haemophagocytosis). Patients who develop early manifestations of pathologic immune activation should be evaluated immediately. If diagnosis of HLH is established, sulfamethoxazole/trimethoprim treatment should be discontinued.
Long-term treatment. If Bactrim is given over a prolonged period, regular blood counts are required. If a significant reduction in count of any formed blood element is noted, Bactrim should be discontinued.
As with all drugs containing sulfonamides, caution is advisable in patients with porphyria or thyroid dysfunction.
Patients who are 'slow acetylators' may be more prone to idiosyncratic reactions to sulfonamides.
Electrolyte abnormalities. Close monitoring of serum potassium and renal function is warranted in patients receiving high dose Bactrim, as used in patients with Pneumocystis jirovecii pneumonia, or in patients receiving standard dose Bactrim with underlying disorders of potassium metabolism or renal insufficiency, or who are receiving drugs which induce hyperkalaemia (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions). Severe and symptomatic hyponatremia can occur in patients receiving Bactrim, particularly for the treatment of P. jirovecii pneumonia. Evaluation for hyponatremia and appropriate correction is necessary in symptomatic patients to prevent life threatening complications.
Sulfonamides, including Bactrim, may induce diuresis, particularly in patients with oedema of cardiac origin.
Cross sensitivity is known to occur among sulfonamides (see Section 4.3 Contraindications).
Except under careful supervision, Bactrim should not be given to patients with serious haematological disorders. Bactrim has been given to patients receiving cytotoxic therapy.
Because of possible interference with folate metabolism, regular blood counts are advisable in patients on long-term therapy, in those who are predisposed to folate deficiency (i.e. the elderly, chronic alcoholics and rheumatoid arthritics), in malabsorption syndromes, malnutrition states, or during the treatment of epilepsy with anticonvulsant drugs such as phenytoin, primidone or barbiturates. Changes indicative of folic acid impairment have, in certain specific situations, been reversed by folinic acid therapy.
Urine analysis and renal function tests should be performed during long-term therapy, particularly in patients with reduced renal function.
The possibility of superinfection with a nonsensitive organism should be borne in mind.
Trimethoprim has been noted to impair phenylalanine metabolism in some patients.
Use in renal impairment. In patients with renal impairment, a reduced or less frequent dosage is recommended in order to avoid accumulation of trimethoprim in the blood. Nonionic diffusion is the main factor in the renal handling of trimethoprim, and as renal failure advances, trimethoprim excretion decreases. See the special dosage table for use in renal impairment. Patients with severe renal impairment who are receiving Bactrim should be closely monitored for symptoms and signs of toxicity such as nausea, vomiting and hyperkalemia. Bactrim should be given with caution to patients with impaired renal function and to those with underlying disorders such as: possible folate deficiency; hypoglycaemia; electrolyte abnormalities (hyperkalemia).
Patients on peritoneal dialysis. Peritoneal dialysis results in minimal clearance of administered trimethoprim and sulfamethoxazole. Use of trimethoprim and sulfamethoxazole in patients receiving peritoneal dialysis is not recommended.
Use in the elderly. The use of Bactrim in elderly patients carries an increased risk of severe adverse reactions. In rare instances fatalities have occurred. The risk of severe adverse reactions is particularly greater when complicating conditions exist, e.g. impaired kidney and/or liver function, or concomitant use of other drugs. Severe skin reactions, or generalised bone marrow suppression (see Section 4.8 Adverse Effects (Undesirable Effects)) or a specific decrease in platelets (with or without purpura) are the most frequently reported severe adverse reactions in elderly patients. In those concurrently receiving certain diuretics, primarily thiazides, an increased incidence of thrombocytopenia with purpura has been reported. Appropriate dosage adjustments should be made for patients with impaired kidney function (see Section 4.2 Dose and Method of Administration).
In view of the increased risk of severe adverse reactions in the elderly, consideration should be given to whether Bactrim is the antibacterial of choice in this age group.
Paediatric use. No data available.
Effects on laboratory tests. Two laboratory procedures, namely the Lactobacillus casei serum folate assay and the L. leishmanii serum vitamin B12 assay are affected by Bactrim.
Bactrim, specifically the trimethoprim component, can interfere with a serum methotrexate assay as determined by the competitive binding protein technique (CBPA) when a bacterial dihydrofolate reductase is used as the binding protein. No interference occurs, however, if methotrexate is measured by a radioimmunoassay (RIA).
The presence of trimethoprim and sulfamethoxazole may also interfere with the Jaffe alkaline picrate reaction assay for creatinine, resulting in overestimations of about 10% in the range of normal values.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Pharmacokinetic interactions. Trimethoprim is an inhibitor of the organic cation transporter 2 (OCT2), and a weak inhibitor of CYP2C8. Sulfamethoxazole is a weak inhibitor of CYP2C9.
Systemic exposure to drugs transported by OCT2 may increase when coadministered with Bactrim. Examples include dofetilide, amantadine, memantine and lamivudine. See Table 2.


4.6 Fertility, Pregnancy and Lactation
Effects on fertility. No data available.
Use in pregnancy. (Category C)
Sulfonamides may cause jaundice and haemolytic anaemia in the newborn. Sulfonamides may cause kernicterus in babies during the first month of life by displacing bilirubin from plasma albumin. Sulfonamides should therefore be avoided as far as possible during the last month of pregnancy (see Section 5.2 Pharmacokinetic Properties). Trimethoprim may interfere with folic acid metabolism and animal experiments have shown that administration of very high doses of trimethoprim during organ development may give rise to birth defects typical of folic acid antagonism. Two large observational studies have suggested a 2 to 3.5-fold increased risk of spontaneous abortion in women treated with trimethoprim alone and in combination with sulfamethoxazole during the first trimester compared to either no exposure to antibiotics or to exposure to penicillins. Bactrim should only be used during pregnancy if the potential benefit justifies the potential risk to the foetus. If Bactrim is used during pregnancy, or if the patient becomes pregnant while taking this drug, folic acid supplementation may be required. The patient should be appropriately counselled.
Use in lactation. Both trimethoprim and sulfamethoxazole are excreted in breast milk at concentrations comparable or somewhat lower than that in the blood. Although the quantity of Bactrim ingested by a breastfed infant is small, it is recommended that the possible risks should be balanced against the expected therapeutic effect (see Section 5.2 Pharmacokinetic Properties). Consideration should be made of the infant's age (see Section 4.3 Contraindications).
A folate supplement may be considered with prolonged high doses of Bactrim.
4.7 Effects on Ability to Drive and Use Machines
The effects of this medicine on a person's ability to drive and use machines were not assessed as part of its registration.
4.8 Adverse Effects (Undesirable Effects)
The most common adverse effects are gastrointestinal disturbances (nausea, vomiting, anorexia) and allergic skin reactions (such as rash (including maculopapular), pruritus and urticaria).
Fatalities associated with the administration of sulfonamides, although rare, have occurred due to severe reactions, including Stevens-Johnson syndrome, toxic epidermal necrolysis, agranulocytosis, aplastic anaemia, other blood dyscrasias, hypersensitivity of respiratory tract, acute and delayed lung injury, and circulatory shock (see Section 4.4 Special Warnings and Precautions for Use).
Haematologic. Agranulocytosis, aplastic anaemia, thrombocytopenia, leukopenia, neutropenia, haemolytic anaemia, autoimmune anaemia, megaloblastic anaemia, hypoprothrombinaemia, methaemoglobinaemia, eosinophilia, purpura, bone marrow depression, granulocytopenia and pancytopenia. Haematological changes have been observed particularly in the elderly. The great majority of these changes were mild, asymptomatic, and proved reversible on withdrawal of the drug which was, in some instances, necessary before therapy could be completed.
High doses of trimethoprim, as used in patients with Pneumocystis jirovecii pneumonia, induces progressive but reversible increase of serum potassium concentration in a substantial number of patients. Even treatment with recommended doses may cause hyperkalaemia when trimethoprim is administered to patients with underlying disorders of potassium metabolism, with renal insufficiency, or if drugs known to induce hyperkalaemia are given concomitantly. Cases of hyponatraemia have also been reported.
Allergic reactions. Skin and systemic reactions may occur. Stevens-Johnson syndrome, fixed drug reaction, morbilliform rash, erythema and toxic epidermal necrolysis (Lyell's syndrome) have been reported.
The following have been reported rarely: eosinophilic or allergic alveolitis, anaphylaxis, allergic myocarditis, exfoliative dermatitis, angioedema, erythema multiforme, drug fever, chills, drug rash with eosinophilia and systemic symptoms (DRESS), Henoch-Schonlein purpura, serum sickness-like syndrome, generalised allergic reactions, photosensitivity, conjunctival and scleral injection. In addition, polyarteritis nodosa and systemic lupus erythematosus have been reported.
Congenital disorders and pregnancy, puerperium and perinatal conditions. Spontaneous abortion.
Gastrointestinal. Hepatitis (including cholestatic jaundice and hepatic necrosis), elevation of serum transaminase and bilirubin, isolated cases of vanishing bile duct syndrome, pseudomembranous enterocolitis, pancreatitis, stomatitis, glossitis, nausea, emesis, abdominal pain, diarrhoea, anorexia, moniliasis. Jaundice has occurred rarely and has usually been mild and transient, frequently occurring in patients with a past history of infectious hepatitis.
General disorders and administration site conditions. Venous pain and phlebitis.
Genitourinary. Renal failure, impaired renal function, interstitial nephritis, BUN and serum creatinine elevation, toxic nephrosis with oliguria and anuria, and crystalluria. Cases of urolithiasis have been reported in patients treated with co-trimoxazole. Renal stones formed by N-acetylsulfamethoxazole crystals aggregation (either 100% or partial) have been described. A causal association is defined specifically for urolithiasis composed from Bactrim metabolites (either 100% or partial), when specific patient risk factors, like crystalluria or reduced urinary output, are met.
Neurologic. Aseptic meningitis, meningitis like symptoms, convulsions, neuropathy (including peripheral neuritis and paraesthesia), ataxia, vertigo, tinnitus, headache and uveitis, vasculitis cerebral.
Psychiatric. Hallucinations, depression, apathy, nervousness.
Endocrine. The sulfonamides bear certain chemical similarities to some goitrogens, diuretics (acetazolamide and the thiazides) and oral hypoglycaemic agents. Cross sensitivity may exist with these agents. Diuresis and hypoglycaemia have occurred rarely in patients receiving sulfonamides. Cases of hypoglycaemia in nondiabetic patients treated with Bactrim are seen rarely, usually occurring after a few days of therapy. Patients with renal dysfunction, liver disease, malnutrition, or those receiving high doses of Bactrim are particularly at risk.
Musculoskeletal. Arthralgia, myalgia and isolated cases of rhabdomyolysis.
Respiratory. Pulmonary infiltrates, pulmonary vasculitis.
Vascular disorders. Vasculitis, necrotizing vasculitis, granulomatosis with polyangiitis.
Miscellaneous. Weakness, fatigue, insomnia and fungal infections, such as candidiasis, retinal vasculitis.
Reporting of suspected adverse reactions. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
Acute. Symptoms. The amount of a single dose of Bactrim that is either associated with symptoms of overdosage or is likely to be life threatening has not been reported. Signs and symptoms of overdosage reported with sulfonamides include anorexia, colic, nausea, vomiting, dizziness, headache, drowsiness and unconsciousness. Pyrexia, haematuria and crystalluria may be noted. Blood dyscrasias and jaundice are potential late manifestations of overdosage.
Signs of acute overdosage with trimethoprim include nausea, vomiting, dizziness, headache, mental depression, confusion and bone marrow depression.
Treatment. Treatment of overdose should consist of general supportive measures.
General principles of treatment include the prevention of further absorption, forcing of oral fluids, and the administration of intravenous fluids if urine output is low and renal function is normal. Alkalinisation of the urine may aid the elimination of the sulfamethoxazole component of Bactrim but may decrease the elimination of the trimethoprim component. The patient should be monitored with blood counts and appropriate blood chemistries, including electrolytes. If a significant blood dyscrasia or jaundice occurs, specific therapy should be instituted for these complications. On cessation of therapy, calcium folinate 3 mg to 6 mg intramuscularly for five to seven days may be given to counteract the effects of trimethoprim on haematopoiesis.
Peritoneal dialysis is not effective and haemodialysis is only moderately effective in eliminating trimethoprim and sulfamethoxazole.
Chronic. Use of Bactrim at high doses and/or for extended periods of time may cause bone marrow depression manifested as thrombocytopenia, leukopenia and/or megaloblastic anaemia. Other blood dyscrasias may occur due to folinic acid deficiency. If signs of bone marrow depression occur, the patient should be given leucovorin 5 to 15 mg daily until normal haematopoiesis is restored.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Pharmacotherapeutic group: Combinations of sulfonamides and trimethoprim, incl. derivatives, ATC code: J01 EE01.
Mechanism of action. Sulfamethoxazole inhibits bacterial synthesis of dihydrofolic acid by competing with para-aminobenzoic acid. Trimethoprim blocks the production of tetrahydrofolic acid from dihydrofolic acid by binding to and reversibly inhibiting the required enzyme, dihydrofolate reductase. Thus, Bactrim blocks two consecutive steps in the biosynthesis of nucleic acids and proteins essential to bacteria.
Bactrim is effective against a wide range of Gram negative and Gram positive organisms, for example E. coli, Neisseria, Salmonella, Klebsiella-Enterobacter, Shigella, Vibrio cholerae, Bordetella pertussis, Streptococcus, Staphylococcus, Pneumococcus. Bactrim is usually active against the problem organisms Haemophilus influenzae and Proteus.
Bactrim is also active against the protozoan Pneumocystis jirovecii (see Section 4.2 Dose and Method of Administration). Bactrim is not active against Mycobacterium tuberculosis and Treponema pallidum. Pseudomonas aeruginosa is frequently insensitive. See Table 4.
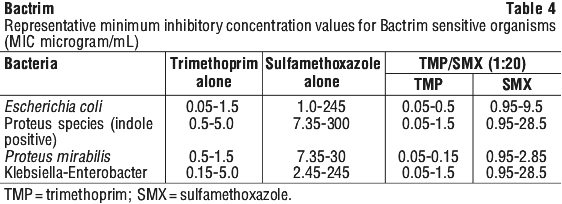
5.2 Pharmacokinetic Properties
Absorption. Bactrim is rapidly absorbed on oral administration, reaching peak blood levels after 1 to 4 hours, which correspond to those achieved when each component is given alone. Absorption is complete as reflected by the absolute oral bioavailability reaching 100% for both trimethoprim and sulfamethoxazole. The mean serum half-lives of trimethoprim and sulfamethoxazole are 10 hours, and 8-10 hours, respectively.
Distribution. The volume of distribution is approximately 1.6 L/kg for trimethoprim and approximately 0.26 L/kg for sulfamethoxazole, while the plasma protein binding reaches 37% for trimethoprim and 53% for sulfamethoxazole. The free forms of trimethoprim and sulfamethoxazole are considered to be the therapeutically active forms.
Studies in both animals and man have shown that diffusion of Bactrim into the tissue is good. Large amounts of trimethoprim and smaller amounts of sulfamethoxazole pass from the bloodstream into the interstitial fluid and other extravascular body fluids.
In humans, trimethoprim and sulfamethoxazole were detected in the foetal placenta, umbilical cord blood, amniotic fluid and foetal tissues (liver, lung), indicating placental transfer of both drugs (see Section 4.6 Fertility, Pregnancy and Lactation).
Metabolism. Around 30% of a trimethoprim dose is metabolised. The cytochrome P450 isoenzymes involved in the oxidative metabolism of trimethoprim have not been identified. The principal trimethoprim metabolites are 1 and 3-oxides and the 3' and 4'-hydroxy derivatives; some metabolites are active.
Around 80% of a sulfamethoxazole dose is metabolised in the liver, predominantly to the N4-acetyl derivative (~ 40% of the dose) and to a lesser extent by glucuronide conjugation. Sulfamethoxazole also undergoes oxidative metabolism. The first step of the oxidative pathway, which leads to the formation of the hydroxylamine derivative, is catalysed by CYP2C9. The metabolites are inactive.
Excretion. The elimination half-lives of the two components are very similar (a mean of 10 hours for trimethoprim and 11 hours for sulfamethoxazole).
Both substances, as well as their metabolites, are eliminated almost entirely by the kidneys through both glomerular filtration and tubular secretion, giving urine concentrations of both active substances considerably higher than the concentration in the blood. Around two thirds of the trimethoprim dose and one quarter of the sulfamethoxazole dose are excreted unchanged into the urine. The total plasma clearance of trimethoprim equals 1.9 mL/min/kg. The total plasma clearance of sulfamethoxazole equals 0.32 mL/min/kg. A small part of the substances is eliminated via the faeces.
Pharmacokinetics in special populations. Hepatic impairment. The pharmacokinetics of trimethoprim and sulfamethoxazole in patients with moderate or severe hepatic impairment are not significantly different from those observed in healthy subjects. (See Section 4.4 Special Warnings and Precautions for Use; Section 4.8 Adverse Effects (Undesirable Effects) for advice and experience of use in patients with impaired liver function.)
Patients with cystic fibrosis. The renal clearance of trimethoprim and the metabolic clearance of sulfamethoxazole are increased in patients with cystic fibrosis. Consequently, the total plasma clearance is increased and the elimination half-life is decreased for both drugs.
5.3 Preclinical Safety Data
Genotoxicity. No data available.
Carcinogenicity. No data available.
6 Pharmaceutical Particulars
6.1 List of Excipients
Povidone, docusate sodium, sodium starch glycollate, magnesium stearate.
6.2 Incompatibilities
Not applicable.
6.3 Shelf Life
5 years.
6.4 Special Precautions for Storage
Store below 30°C.
6.5 Nature and Contents of Container
Bactrim DS tablets are available in a PVC/Al blister pack of 10 tablets.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Chemical structure.
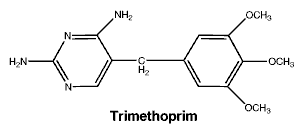
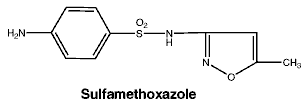
The chemical name for sulfamethoxazole is 3-(4-aminobenzenesulfonamido)-5-methylisoxazole having a molecular weight of 253.28 and a pKa 5.9. The chemical name for trimethoprim is 2,4-diamino-5-(3,4,5-trimethoxybenzyl) pyrimidine having a molecular weight of 290.3 and a pKa 7.3.
Sulfamethoxazole is a white to off-white powder and is virtually insoluble in water at 20°C. Trimethoprim is a white to cream-coloured powder that has an aqueous solubility of 300 mg/L at 20°C.
CAS number. Sulfamethoxazole: 723-46-6 and trimethoprim: 738-70-5.
7 Medicine Schedule (Poisons Standard)
Schedule 4 - Prescription medicine.
Date of First Approval
18 August 2005
Date of Revision
19 December 2025
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.