BrinzoQuin Eye Drops 1.0%
Brand Information
| Brand name | BrinzoQuin Eye Drops 1.0% |
| Active ingredient | Brinzolamide |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the BrinzoQuin Eye Drops 1.0%.
Summary CMI
BrinzoQuin®
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using BrinzoQuin?
BrinzoQuin contains the active ingredient Brinzolamide. BrinzoQuin is used to treat certain types of eye conditions such as high pressure inside your eye and open angle glaucoma (an eye condition caused by fluid buildup that damages the optic nerve).
For more information, see Section 1. Why am I using BrinzoQuin? in the full CMI.
2. What should I know before I use BrinzoQuin?
Do not use if you have ever had an allergic reaction to BrinzoQuin or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I use BrinzoQuin? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with BrinzoQuin and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use BrinzoQuin?
- Follow the instructions provided by your doctor carefully.
- Put one drop of BrinzoQuin in the conjunctival sac of the affected eye(s) twice daily.
More instructions can be found in Section 4. How do I use BrinzoQuin? in the full CMI.
5. What should I know while using BrinzoQuin?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using BrinzoQuin? in the full CMI.
6. Are there any side effects?
Common side effects include eye pain, dry eye, itchy eye(s), eye irritation, vision problems, increased sensitivity to light, dizziness, blurred vision, feeling that something is in your eye(s), itchy eye(s).
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
1. Why am I using BrinzoQuin?
BrinzoQuin contains the active ingredient Brinzolamide. It belongs to a class of medicines called Carbonic anhydrase inhibitors.
BrinzoQuin is used to treat certain types of eye conditions such as high pressure inside your eye and open angle glaucoma (an eye condition caused by fluid buildup that damages the optic nerve).
BrinzoQuin helps in reducing eye pressure within the eye by reducing the production of fluid.
2. What should I know before I use BrinzoQuin?
Warnings
Do not use BrinzoQuin:
- If you are allergic to Brinzolamide, sulfonamides or any of the ingredients listed at the end of this leaflet. Always check the ingredients to make sure you can use this medicine. Symptoms of allergic reaction may include shortness of breath, difficulty breathing, swelling of the face, lips, tongue or other parts of the body, rash, hives.
- If you have severe kidney disease.
- If you have symptoms such as headache, lack of energy, vomiting and feeling sick.
- in children
- after the expiry date printed on the pack or if the seal around the pack is broken or shows signs of tampering.
Check with your doctor if you:
- have any other types of Glaucoma
- use carbonic anhydrase inhibitor medicines e.g. Acetazolamide
- take any medicines for any other condition
- suffer from any liver, kidney problems
- have any skin rash, problems with your skin
- have any problems with your cornea.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor if you are pregnant or intend to become pregnant.
Your doctor will advise you regarding the possible risks and benefits of using BrinzoQuin during pregnancy.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
Your doctor will advise you regarding the possible risks and benefits of using BrinzoQuin during breastfeeding.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with BrinzoQuin and affect how it works.
Tell your doctor if you use any of the following medicines:
- Nonsteroidal anti-inflammatory drugs (NSAIDs) eg Ibuprofen, Aspirin or high dose of salicylates
- Oral carbonic anhydrase inhibitors such as acetazolamide
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect BrinzoQuin.
4. How do I use BrinzoQuin?
How much to use
- Follow the instructions provided and use BrinzoQuin until your doctor tells you to stop.
- Put one drop of BrinzoQuin in the conjunctival sac of the affected eye(s) twice daily.
- If you are being changed from one eye drop to another, follow your doctor's instructions carefully as to when to stop the old drops and when to start the new drops.
When to use BrinzoQuin
- BrinzoQuin should be used at about the same time every day unless your doctor tells you otherwise.
How to use BrinzoQuin
- Sitting or a lying down position might make the process simpler.
- Remove contact lenses if you are wearing them before using the eye drops.
- Shake the bottle well prior to use.
Follow the steps below to use BrinzoQuin:
- Wash your hands thoroughly with soap and water.
- Before using a bottle for the first time, break the safety seal around the neck area and throw the loose plastic ring away.
- Remove the cap from the bottle.
- After the cap is removed, if the tamper evident snap collar is loose, it should be removed before using the product.
- Mix the contents of the bottle by inverting 5 to 10 times.
- Hold the bottle upside down in one hand between your thumb and middle finger (refer diagram 1).
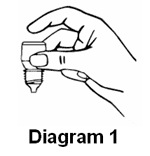
- Tilt your head back, gently pull down the lower eyelid of your eye to form a pouch/pocket.
- Place the tip of the bottle close to your eye. Do not touch the tip to your eye as this may cause injury to the eye.
- Do not touch the dropper tip to eyelid or surrounding areas or any surface to avoid contamination of the dropper tip and solution.
- Release one drop into the pouch/pocket formed between your eye and eyelid by gently tapping or pressing the base of the bottle with your forefinger (refer diagrams 2 and 3).
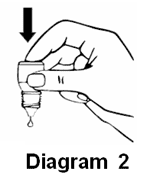
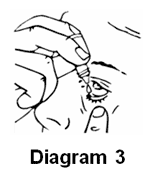
- Gently close your eye(s) for 2 minutes. Do not blink or rub your eye(s).
- When your eye is closed, place your index finger against the inside corner of your eye and press against your nose for about two minutes. This will help to prevent the medicine from draining through the tear duct to the nose and throat, from where it can be absorbed into other parts of your body and may result in less side effects.
- This will also help to prevent the unpleasant taste sensation that some people experience while using these eye drops.
- If necessary, repeat the above steps for the other eye.
- You may feel initial discomfort or a slight burning sensation in the eye shortly after using BrinzoQuin. If it continues, or is uncomfortable, contact your doctor or pharmacist.
- If you want to use any other eye drops wait at least 5 minutes after using BrinzoQuin. Eye ointments should be used last.
- It is normal for a small amount of eye drops to spill onto your cheek since your eyelids can only hold less than one drop at a time. Wipe away any spillage with a tissue.
- Replace the cap on the bottle and close it tightly.
- Always keep the bottle tightly closed when not in use.
- Wash your hands again with soap and water to remove any residue.
- Wait for 15 minutes before putting in your contact lenses.
- Discard BrinzoQuin eye drops 4 weeks after opening it.
If you forget to use BrinzoQuin
BrinzoQuin should be used regularly at the same time each day. If you miss your dose at the usual time, use the drops as soon as you remember and then go back to using them as told by your doctor.
If it is almost time for your next dose, skip the dose you missed and take your next dose when you are meant to.
Do not take a double dose to make up for the dose you missed.
If you use too much BrinzoQuin
If you think that you have used too much BrinzoQuin, you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
If you accidentally use several BrinzoQuin Eye Drops in your eyes, immediately wash your eyes with warm tap water.
5. What should I know while using BrinzoQuin?
Things you should do
- Do not put BrinzoQuin into your eye(s) while wearing contact lenses.
- Remove the soft contact lenses before using BrinzoQuin. Benzalkonium chloride, one of the ingredients may cause eye irritation and is known to discolour soft contact lenses.
- Put your lenses back in 15 minutes after using the eye drops.
Call your doctor straight away if you:
- develop any signs of allergic reaction.
- become pregnant, plan to become pregnant or if you are breast feeding while using BrinzoQuin.
- have severe kidney diseases.
- develop a skin rash, hives or other skin problems while on treatment with BrinzoQuin.
Remind any doctor, dentist, pharmacist or specialist you visit that you are using BrinzoQuin.
Things you should not do
- Do not stop using this medicine suddenly.
- Do not use BrinzoQuin in children.
- Do not give BrinzoQuin to anyone else, even if they seem to have the same condition as you.
- Do not touch the dropper tip to any surface.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how BrinzoQuin affects you.
BrinzoQuin may cause temporary blurred vision or other visual problems in some people.
If blurred vision occurs when you use BrinzoQuin, wait until your vision clears before driving or using machinery.
BrinzoQuin may also cause nervous system problems in some people. Be careful as it may affect your ability to drive or use machines.
Looking after your medicine
- Store below 25°C.
- Do not freeze.
Follow the instructions in the carton on how to take care of your medicine properly.
Store it in a cool dry place away from moisture, heat or sunlight; for example, do not store it:
- in the bathroom or near a sink, or
- in the car or on window sills.
Keep it where young children cannot reach it.
When to discard your medicine
Discard BrinzoQuin 4 weeks after opening.
Getting rid of any unwanted medicine
If you no longer need to use this medicine or it is out of date, take it to any pharmacy for safe disposal.
Do not use this medicine after the expiry date.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
Eye Problems:
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
Eye problems:
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What BrinzoQuin contains
| Active ingredient (main ingredient) | Brinzolamide |
| Other ingredients (inactive ingredients) | Mannitol, carbomer 974P, sodium chloride, tyloxapol, disodium edetate, sodium hydroxide and/or hydrochloric acid (for pH adjustment), purified water and benzalkonium chloride. |
| Potential allergens | NA |
Do not take this medicine if you are allergic to any of these ingredients.
What BrinzoQuin looks like
BrinzoQuin Eye Drops 1.0% is a white to off-white, uniform suspension which is available in LDPE bottle dispenser. Pack sizes: 1 x 5 mL and 1 x 10 mL.
Not all pack sizes may be marketed.
Australian registration number
AUST R No. 99179
Who distributes BrinzoQuin
BrinzoQuin is supplied in Australia by:
Novartis Pharmaceuticals Australia Pty Limited
ABN 18 004 244 160
54 Waterloo Road
Macquarie Park NSW 2113
Telephone: 1-800-671-203
Web site: www.novartis.com.au
® Registered Trademark
© Novartis Pharmaceuticals Australia Pty Limited 2022
This leaflet was prepared in August 2025.
Internal document code:
brq091123c_V2 based on PI brq091123i
Brand Information
| Brand name | BrinzoQuin Eye Drops 1.0% |
| Active ingredient | Brinzolamide |
| Schedule | S4 |
MIMS Revision Date: 01 January 2024
1 Name of Medicine
Brinzolamide.
2 Qualitative and Quantitative Composition
The eye drops suspension contains 10 mg/mL (1%) brinzolamide and also 0.1 mg/1 mL benzalkonium chloride as a preservative.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Eye drops.
BrinzoQuin is a white to off-white, uniform suspension.
4 Clinical Particulars
4.1 Therapeutic Indications
BrinzoQuin Eye Drops 1.0% are indicated to decrease intraocular pressure in: ocular hypertension, open-angle glaucoma.
4.2 Dose and Method of Administration
The recommended dosage is one drop of BrinzoQuin in the conjunctival sac of the affected eye(s) twice daily.
When substituting for another ophthalmic anti-glaucoma agent with BrinzoQuin, the other agent should be discontinued and BrinzoQuin should be started on the following day.
Concomitant therapy. BrinzoQuin has been used concomitantly with other agents e.g. travoprost, latanoprost, timolol (see Section 5.1 Pharmacodynamic Properties, Clinical trials). In case of concomitant therapy with more than one topical ophthalmic medicinal product being used, the eye drops must be administered with an interval of at least five minutes. Eye ointments should be administered last.
Method of administration. For ocular use. Patients should be instructed to shake the bottle well prior to use.
To avoid contamination, the dropper tip should not touch any surface. The dropper tip should also not come into contact with the eye as this may cause injury to the eye. Patients should be instructed to keep the bottle tightly closed when not in use.
Instillation of eye drops may cause initial discomfort (see Section 4.8 Adverse Effects (Undesirable Effects)).
Nasolacrimal occlusion and closing the eyelid for two minutes, after instillation is recommended. This may result in a decrease in systemic side effects and an increase in local activity.
Patients must be instructed to remove soft contact lenses prior to application of BrinzoQuin and to wait fifteen minutes after instillation of the dose before reinsertion.
4.3 Contraindications
BrinzoQuin is contraindicated in patients with a known hypersensitivity to brinzolamide, sulfonamides or any of the excipients in the product (see Section 6.1 List of Excipients).
BrinzoQuin is also contraindicated in patients with severe renal impairment and in patients with hyperchloraemic acidosis.
4.4 Special Warnings and Precautions for Use
Not for injection or oral ingestion.
The management of patients with acute angle-closure glaucoma requires therapeutic interventions in addition to ocular hypotensive agents. BrinzoQuin has not been studied in patients with acute angle-closure glaucoma.
Brinzolamide is a sulfonamide and, although administered topically, is absorbed systemically. The same types of adverse reactions or hypersensitivity that are attributable to sulfonamides may, therefore, occur with topical administration. Hypersensitivity reactions reported with sulfonamide derivatives, including Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN), can occur in patients receiving BrinzoQuin. At the time of prescription, patient should be advised of the signs and symptoms and monitored closely for skin reactions. BrinzoQuin should be discontinued immediately if signs of serious reactions or hypersensitivity occur.
There is a potential for an additive effect on the known systemic effects of carbonic anhydrase inhibition in patients receiving an oral carbonic anhydrase inhibitor and BrinzoQuin. The concomitant administration of BrinzoQuin and oral carbonic anhydrase inhibitors has not been studied and is not recommended.
Acid-base disturbances have been reported with oral carbonic anhydrase inhibitors. BrinzoQuin should be used with caution in patients with risk of renal impairment because of the possible risk of metabolic acidosis.
The possible role of brinzolamide on corneal endothelial function has not been investigated in patients with compromised corneas (particularly in patients with low endothelial cell count). Carbonic anhydrase inhibitors may affect corneal hydration, which may lead to a corneal decompensation and oedema. Careful monitoring of patients with compromised corneas, such as patients with diabetes mellitus or corneal dystrophies, is recommended.
BrinzoQuin contains benzalkonium chloride which may cause eye irritation and is known to discolour soft contact lenses. Avoid contact with soft contact lenses. Patients must be instructed to remove contact lenses prior to application of BrinzoQuin and wait at least 15 minutes before reinsertion.
Contact lenses. If patients continue to wear soft (hydrophilic) contact lenses while under treatment with BrinzoQuin, they should remove their lens(es) prior to instilling BrinzoQuin in the affected eye(s) and should not insert their lens(es) until 15 minutes after instillation of the eye drops.
Use in hepatic impairment. BrinzoQuin has not been studied in patients with hepatic impairment. Caution should, therefore, be exercised if a decision is made to commence therapy with BrinzoQuin in such patients.
Use in renal impairment. BrinzoQuin has not been studied in patients with severe renal impairment (CrCl < 30 mL/min) or in patients with hyperchloraemic acidosis. Brinzolamide and its main metabolite are predominantly excreted by the kidney; BrinzoQuin is, therefore, contraindicated in such patients (see Section 4.3 Contraindications).
Use in the elderly. In clinical studies conducted with brinzolamide 1.0%, the probability of having an adverse reaction was independent of age. No differences in patients experiencing adverse reactions were noted when patients less than 65 years of age were compared to patients greater than 65 years of age. There are no modifications to the recommended dosing regimen for elderly patients.
Paediatric use. The safety and effectiveness of BrinzoQuin in paediatric patients have not been established.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Specific drug interaction studies have not been performed with BrinzoQuin. In clinical studies, however, brinzolamide 1.0% were used concomitantly with the following medications without evidence of adverse interactions: timolol maleate eye drops, systemic medications including ACE inhibitors, calcium-channel blockers, diuretics, non-steroidal anti-inflammatory drugs including aspirin, and hormones (e.g. oestrogen, insulin, thyroxine).
Association between BrinzoQuin and miotics or adrenergic agonists has not been fully evaluated during adjunctive glaucoma therapy.
Brinzolamide is a carbonic anhydrase inhibitor and, although administered topically, is absorbed systemically. In clinical studies, brinzolamide was not associated with acid-base disturbances. These disturbances have, however, been reported with oral carbonic anhydrase inhibitors and have, in some instances, resulted in drug interactions (e.g. nonsteroidal anti-inflammatory drugs (NSAIDs) and toxicity associated with high-dose salicylate therapy). The potential for such drug interactions should, therefore, be considered in patients receiving BrinzoQuin.
There is potential for an additive effect on the known systemic effects of carbonic anhydrase inhibition in patients receiving an oral carbonic anhydrase inhibitor and BrinzoQuin. The concomitant administration of BrinzoQuin and oral carbonic anhydrase inhibitors is not recommended.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. A fertility and early embryonic study, in which male and female rats were dosed by oral gavage with brinzolamide at doses up to 18 mg/kg/day, showed no effects on fertility or reproductive capacity. Studies have not been performed to evaluate the effect of topical ocular administration of brinzolamide on human fertility.
Use in pregnancy. (Category B3)
Studies in animals with brinzolamide have shown reproductive toxicity following systemic administration. Radioactivity was found to cross the placenta and was present in the foetal tissues and blood following oral administration of 14C-brinzolamide to pregnant rats.
Developmental toxicity studies in rabbits at oral doses up to 6 mg/kg/day brinzolamide produced maternal toxicity at 6 mg/kg/day and a significant increase in the number of foetal variations, such as accessory skull bones; at 1 and 6 mg/kg/day the incidence was only slightly higher than seen historically. In rats, statistically significant decreased bodyweights of foetuses from dams receiving oral doses of 18 mg/kg/day during gestation were proportional to the reduced maternal weight gain, with no statistically significant effects on organ or tissue development. No treatment-related malformations were seen.
No studies of the use of ophthalmic brinzolamide have been conducted in pregnant women. BrinzoQuin should be used during pregnancy only if the potential benefit justifies the potential risk to the foetus.
Use in lactation. Studies in animals have shown that following oral administration brinzolamide is excreted in breast milk. Following oral administration of 14C-brinzolamide to lactating rats, radioactivity was found in milk at concentrations below those in the blood and plasma. Decreases in pup bodyweights were observed at 15 mg/kg/day in a pre- and postnatal study in which rats were given brinzolamide by oral gavage at doses up to 15 mg/kg/day.
It is not known whether brinzolamide is transferred into human milk following topical ocular administration. Because many drugs are excreted in human milk and because of the potential for serious adverse reactions in nursing infants from brinzolamide, a decision should be made whether to discontinue nursing or to discontinue the drug, taking into account the importance of the drug to the mother.
The developmental and health benefits of breast-feeding should be considered along with the mother's clinical need for BrinzoQuin and any potential adverse effects on the breast-fed child from BrinzoQuin.
4.7 Effects on Ability to Drive and Use Machines
As with other ophthalmic medications, patients should be advised to exercise caution if they experience transient blurred vision or other visual disturbances following instillation of eye drops; patients should wait until their vision clears before driving or using machinery.
Additionally, nervous system disorders have been reported with the use of the product which may affect the ability to drive or use machines (see Section 4.8 Adverse Effects (Undesirable Effects)).
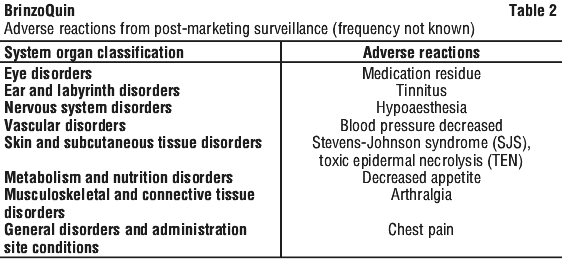
4.8 Adverse Effects (Undesirable Effects)
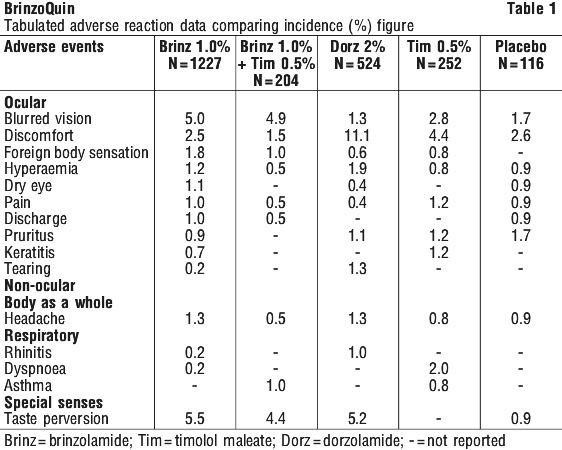
In well-controlled clinical studies, undesirable effects related to brinzolamide 1.0% were non-serious, generally mild to moderate, and usually did not lead to discontinuation of therapy. Tabulated adverse reaction data (considered to be possibly, probably or definitely related to treatment), providing comparisons to placebo and other active comparators (to an incidence 1% or greater), which have been generated from all clinical studies with brinzolamide 1.0%, are provided in Table 1.
Uncommon ophthalmic events (incidence < 1% and ≥ 0.1%) not detailed in Table 1 included blepharitis, conjunctivitis, lid margin crusting, sticky sensation, eye fatigue, abnormal vision, keratopathy, keratoconjunctivitis, corneal staining, eye disorder, photophobia, diplopia, meibomitis, vision changes, irritation, glare and lid disorder.
Uncommon non-ocular events (incidence < 1% and ≥ 0.1%) not detailed in Table 1 included:
Body as a whole. Chest pain, asthenia and pain.
Digestive. Dry mouth, nausea, dyspepsia, diarrhoea, gastrointestinal disturbance.
Nervous. Paraesthesia, depression, dizziness, dream abnormality, hypertonia, agitation, amnesia, depersonalisation, nervousness.
Respiratory. Dyspnoea, pharyngitis, bronchitis, dry nose, epistaxis.
Skin and appendages. Dermatitis, alopecia, urticaria, pruritus.
Special senses. Tinnitus.
Urogenital. Kidney pain, impotence.
Eye disorders. Common (≥ 1% to < 10%): vision blurred, eye irritation, eye pain, dry eye, eye discharge, ocular discomfort, ocular hyperaemia.
Uncommon (≥ 0.1% to < 1%): corneal erosion, punctate keratitis, keratitis, conjunctivitis, conjunctivitis allergic, blepharitis, visual acuity reduced, photophobia, asthenopia, periorbital oedema, eye pruritus, lacrimation increased, eyelid margin crusting.
Rare (≥ 0.01% to < 0.1%): corneal oedema, diplopia, reduced visual acuity, photopsia, hypoaesthesia eye, periorbital oedema.
Psychiatric disorders. Uncommon (≥ 0.1% to < 1%): depression.
Rare (≥ 0.01% to < 0.1%): insomnia.
Nervous system disorders. Common (≥ 1% to < 10%): headache, dysgeusia.
Uncommon (≥ 0.1% to < 1%): dizziness, paresthesia.
Rare (≥ 0.01% to < 0.1%): memory impairment, somnolence.
Cardiac disorders. Rare (≥ 0.01% to < 0.1%): angina pectoris, heart rate irregular.
Respiratory, thoracic and mediastinal disorders. Uncommon (≥ 0.1% to < 1%): dyspnoea, epistaxis, rhinorrhoea, oropharyngeal pain, upper airway cough syndrome, throat irritation.
Rare (≥ 0.01% to < 0.1%): bronchial hyperreactivity, upper respiratory tract congestion, sinus congestion, nasal congestion, cough, nasal dryness.
Gastrointestinal disorders. Uncommon (≥ 0.1% to < 1%): nausea, diarrhoea, dyspepsia, abdominal discomfort, dry mouth.
Skin and subcutaneous tissue disorders. Uncommon (≥ 0.1% to < 1%): rash.
Rare (≥ 0.01% to < 0.1%): urticaria, alopecia, pruritus generalised.
General disorders and administration site conditions. Uncommon (≥ 0.1% to < 1%): fatigue, irritability.
Rare (≥ 0.01% to < 0.1%): feeling jittery, asthenia.
See Table 2.
4.9 Overdose
No information on systemic overdosage is available in humans. Treatment should be symptomatic and supportive. Electrolyte imbalance, development of an acidotic state, and possible nervous system effects may occur. Serum electrolyte levels (particularly potassium) and blood pH levels should be monitored.
A topical overdose of BrinzoQuin may be flushed from the eyes with warm tap water.
In Australia, contact Poisons Information Centre on 13 11 26 for advice on management.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Brinzolamide is a carbonic anhydrase inhibitor. When instilled in the eye, BrinzoQuin has the action of reducing elevated intraocular pressure, whether or not accompanied by glaucoma.
Glaucoma is defined as an optic neuropathy resulting in optic nerve head damage and visual field loss. The pathogenesis of glaucoma is multi-factorial, however, the primary risk factors are considered to be sustained elevated intraocular pressure and poor ocular perfusion. The ocular hypotensive action of brinzolamide is mediated through inhibition of carbonic anhydrase in the ciliary processes of the eye which decreases aqueous humour secretion, presumably by slowing the formation of bicarbonate ions with subsequent reduction in sodium and fluid transport.
Carbonic anhydrase is an enzyme found in many tissues of the body, including the eye. Carbonic anhydrase catalyses the reversible reaction involving the hydration of carbon dioxide and the dehydration of carbonic acid. In humans, carbonic anhydrase exists as a number of isoenzymes, the most active being CA-II, found primarily in red blood cells (RBCs), but also in other tissues. Brinzolamide is an inhibitor of carbonic anhydrase II (CA-II), which is the predominant iso-enzyme in the eye, with an in vitro IC50 of 3.2 nanoM and a Ki of 0.13 nanoM against CA-II. Brinzolamide has also been shown to have a low affinity for 34 receptors or second messenger systems, indicating selectivity for CA-II.
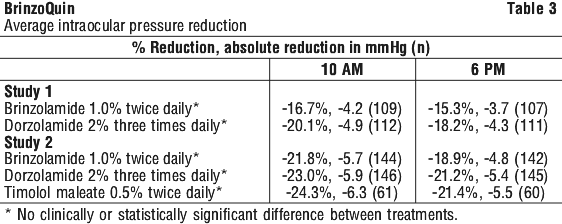
Clinical trials. In two randomised, double-masked studies of 3 month duration, monotherapy with brinzolamide eye drops 1.0% produced a significant reduction in intraocular pressure when dosed twice daily; this intraocular pressure reduction was equivalent to that of dorzolamide 2% dosed three times daily (see Table 3). No additional clinically or statistically significant benefit was evident following administration of brinzolamide eye drops three times daily.
Thirty volunteers with a diagnosis of asthma or chronic obstructive pulmonary disease were enrolled in a masked, cross-over design study to compare the acute effects of brinzolamide 1.0% versus timolol maleate 0.5% on pulmonary function as measured by forced expiratory volume in one second (FEV1). Within 15 minutes of the instillation of a single drop of timolol maleate 0.5%, statistically significant decreases in mean FEV1 were observed (compared to both baseline and brinzolamide 1.0%); these continued for up to 3 hours following instillation. No effect was observed on FEV1 following the instillation of brinzolamide 1.0%.
Two masked, well-controlled studies, each of one-week duration, were designed to compare the comfort of brinzolamide 1.0% twice daily to dorzolamide eye drops 2.0% three times daily. Each of these studies indicated that a significantly greater (p < 0.001) percentage of patients experienced no discomfort following repeated instillation of brinzolamide 1.0%, as shown in Table 4.

One 12-week, double-masked, randomised study in which 215 patients with ocular hypertension or primary open-angle glaucoma were enrolled, was conducted. A total of 201 patients were randomised and 192 were included in the per protocol analysis. The primary objective of the study was to compare the efficacy and safety of brinzolamide 1% and timolol 0.5%, each administered twice daily when added to travoprost 0.004% administered once daily in the evening. Patients who were considered inadequately controlled on monotherapy (travoprost, latanoprost or bimatoprost) were eligible to be enrolled in this study. The primary endpoint was mean diurnal IOP.
There was no statistically significant difference in mean diurnal IOP at 12 weeks between the treatment groups (18.1 mmHg vs 18.1 mmHg in the brinzolamide and timolol groups, respectively). The mean reductions in diurnal IOP were 3.4 mmHg and 3.2 mmHg for the brinzolamide and timolol groups, respectively. Overall, the efficacy of brinzolamide 1%, as concomitant therapy, was comparable to concomitant therapy with timolol 0.5%. There was a higher incidence of local adverse effects (conjunctival hyperaemia, burning or foreign body sensation) with brinzolamide than with timolol; however, the differences were not statistically significant.
A second, open-label 12-week study was conducted in 82 patients with open-angle glaucoma or ocular hypertension. A total of 79 patients were evaluable for the intent-to-treat analysis. Patients, requiring additional IOP-lowering from a baseline of travoprost eye drops, received brinzolamide 1% concomitantly. The primary efficacy endpoint was the mean reduction in IOP at 12 weeks.
There was a mean reduction of 3.9 mmHg after 4 weeks and 4.2 mmHg after 12 weeks. Overall, 43 patients (60.6%) had an IOP below 18 mmHg at the conclusion of the study.
Additional studies have been published concerning IOP control (Tsukamoto et al. J. Ocular Pharmacol. Ther. 21: 170-173, 2005, Tsukamoto et al. J. Ocular Pharmacol. Ther. 21: 395-399, 2005). These studies suggest that brinzolamide might be added to dual therapy (latanoprost plus beta-blocker) or substituted for dorzolamide in triple therapy.
When used twice daily, adjunctively to timolol maleate 0.5% for 3 months, brinzolamide 1.0% provided an additional intraocular pressure lowering effect. This was equivalent to dorzolamide 2% dosed twice daily adjunctively to timolol maleate 0.5% (see Table 5). No additional clinically or statistically significant benefit was evident following administration of brinzolamide 1.0% three times daily.

5.2 Pharmacokinetic Properties
Following topical ocular administration, brinzolamide is absorbed into the systemic circulation. Due to its high affinity for carbonic anhydrase II (CA-II), brinzolamide distributes extensively into the red blood cells (RBCs) and exhibits a long half-life in whole blood (approximately 111 days). In humans, the metabolite N-desethyl brinzolamide is formed, which also binds to CA and accumulates in RBCs. This metabolite binds mainly to CA-I in the presence of brinzolamide. In plasma, both parent brinzolamide and N-desethyl brinzolamide concentrations are low and generally below assay quantitation limits (< 10 nanogram/mL). Binding to plasma proteins is not extensive (approximately 60%). Brinzolamide is eliminated predominantly in the urine as unchanged drug. N-desethyl brinzolamide is also found in the urine along with lower concentrations of the N-desmethoxypropyl and O-desmethyl metabolites.
An oral pharmacokinetic study was conducted in which healthy volunteers received 1 mg capsules of brinzolamide twice daily for up to 32 weeks. This regimen provided a higher systemic exposure rate than topical ocular administration of brinzolamide dosed in both eyes three times daily, and simulated systemic drug and metabolite concentrations similar to those achieved with long-term topical dosing. RBC CA activity was measured to assess the degree of systemic CA inhibition.
Brinzolamide saturation of RBC CA-II was achieved within 4 weeks (RBC concentrations of approximately 20 microM). N-desethyl brinzolamide accumulated in RBCs to steady-state within 20-28 weeks reaching concentrations ranging from 6-30 microM. The inhibition of total RBC CA activity at steady state was approximately 70-75%, which is below that expected to adversely affect renal function or respiration in healthy subjects.
An oral pharmacokinetic study was conducted in which subjects with mild to moderate renal impairment (creatinine clearance of 30-60 mL/minute) received 1 mg capsules of brinzolamide twice daily for up to 54 weeks. By week 4 of treatment, parent drug RBC concentrations ranged from approximately 20 to 40 microM and showed little subsequent change. At steady state, parent drug and N-desethyl metabolite RBC concentrations ranged from 22.0 to 46.1 and 17.1 to 88.6 microM, respectively. Metabolite RBC concentrations, but not those of parent drug, showed a significant (p < 0.05) increase with decreasing creatinine clearance. Total RBC CA activity, but not CA-II activity, showed a significant decrease as creatinine clearance decreased. In spite of the greater inhibition of total CA activity in subjects showing the highest degree of renal impairment, all subjects showed < 90% total CA inhibition at steady state. This is below the 99% or greater inhibition associated with systemic adverse effects.
In a topical ocular study, patients with open-angle glaucoma or ocular hypertension received brinzolamide 1.0% either two or three times daily for up to 18 months. Steady-state concentrations of brinzolamide were reached for most subjects within 6-9 months, while steady state for the N-desmethyl metabolite was reached within 12 to 18 months. At steady state, brinzolamide RBC concentrations were similar to those found in the oral study, but levels of the N-desmethyl metabolite were lower. Carbonic anhydrase activity was approximately 40-70% of per-dose levels, indicating a degree of inhibition that was substantially lower than that observed orally and unlikely to elicit systemic side effects.
5.3 Preclinical Safety Data
Genotoxicity. Genotoxicity studies with brinzolamide did not demonstrate any mutagenic potential in one in vitro (Ames assay) or chromosomal damage in an in vivo assay (micronucleus formation). Brinzolamide did induce forward mutations in the mouse lymphoma assay in vitro, with, but not without metabolic activation. Brinzolamide was negative in a sister chromatid exchange assay in mice.
Carcinogenicity. A two year bioassay, in which rats were dosed by oral gavage at doses up to 8 mg/kg/day brinzolamide revealed no evidence of a carcinogenic effect. A similar study conducted in mice (0, 1, 3 and 10 mg/kg/day brinzolamide dosed by oral gavage) also showed that brinzolamide was non-carcinogenic. The mouse study did, however, reveal a statistically significant increase in urinary bladder tumours in female mice given 10 mg/kg/day orally for 24 months. Dose-related proliferative changes in the urinary bladder were observed in female mice at all dose levels and among males at 10 mg/kg/day. The elevated bladder tumour incidence was due to the increased incidence of a tumour considered to be unique to mice.
6 Pharmaceutical Particulars
6.1 List of Excipients
Mannitol, carbomer 974P, sodium chloride, tyloxapol, disodium edetate, sodium hydroxide and/or hydrochloric acid (for pH adjustment), purified water and benzalkonium chloride.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
Discard container 4 weeks after opening.
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C.
6.5 Nature and Contents of Container
BrinzoQuin Eye Drops 1.0% is available in LDPE bottle dispenser. Pack sizes: 1 x 5 mL and 1 x 10 mL.
Not all pack sizes may be marketed.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
Brinzolamide is presented as white to off-white crystals or powder.
Brinzolamide is very slightly soluble in water at neutral pH.
Chemical structure.
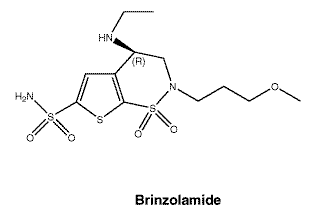
Empirical formula: C12H21N3O5S3.
Chemical name: (R)-4-(ethylamino)-3,4-dihydro- 2-(3-methoxypropyl)- 2H-thieno[3,2-e]-1,2-thiazine- 6-sulfonamide-1,1-dioxide.
CAS number. 138890-62-7.
7 Medicine Schedule (Poisons Standard)
Prescription Only Medicine (Schedule 4).
Date of First Approval
20 May 2004
Date of Revision
09 November 2023
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.