Cafnea Injection and Cafnea Oral Solution
Brand Information
| Brand name | Cafnea Injection and Cafnea Oral Solution |
| Active ingredient | Caffeine citrate |
| Schedule | Unscheduled |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Cafnea Injection and Cafnea Oral Solution.
Summary CMI
Cafnea® Injection and
Cafnea® Oral Solution
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why is Cafnea Injection or Cafnea Oral Solution being given?
Cafnea Injection and Cafnea Oral Solution contains the active ingredient caffeine citrate. Cafnea Injection and Cafnea Oral Solution are used to help improve the breathing of premature infants suffering from apnoea of prematurity who have been born between 28 and less than 33 weeks gestation. For more information, see Section 1. Why is Cafnea Injection or Cafnea Oral Solution being given? in the full CMI.
2. What should I know before Cafnea Injection or Cafnea Oral Solution is given?
Your baby should not be given Cafnea Injection or Cafnea Oral Solution if they have ever had an allergic reaction to caffeine or citrate or any of the ingredients listed at the end of the CMI. For more information, see Section 2. What should I know before Cafnea Injection or Cafnea Oral Solution is given? in the full CMI.
3. What if I am using other medicines?
Some medicines may interfere with Cafnea Injection or Cafnea Oral Solution and affect how it works.
A list of these medicines is in Section 3. What if I am using other medicines? in the full CMI.
4. How is Cafnea Injection or Cafnea Oral Solution given?
- Cafnea Injection or Cafnea Oral solution must only be given by a doctor or nurse.
- Cafnea Injection is infused into a vein slowly using a syringe infusion pump.
- Cafnea Oral Solution is given in a measured dose by mouth through a dropper or feeding tube.
More instructions can be found in Section 4. How is Cafnea Injection or Cafnea Oral Solution given? in the full CMI.
5. What should I know while using Cafnea Injection or Cafnea Oral Solution?
| Things you should do |
|
| Things you should not do |
|
| Looking after the medicine |
|
For more information, see Section 5. What should I know while using Cafnea Injection or Cafnea Oral Solution? in the full CMI.
6. Are there any side effects?
The serious side effects include irritability, jitteriness, restlessness, fast heartbeat, stomach upset or vomiting, reflux, passing large amounts of urine, excessive thirst, dry mouth and skin, sweating, weakness, dizziness, trembling, flushing or paleness, symptoms of necrotising enterocolitis a serious stomach condition which include lack of energy, severe vomiting, stomach/abdominal bloating (distension) and bloody stools. For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
Cafnea® Injection and
Cafnea® Oral Solution
Active ingredient: caffeine citrate
Consumer Medicine Information (CMI)
This leaflet provides important information about using Cafnea Injection and Cafnea Oral Solution. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using Cafnea Injection and Cafnea Oral Solution.
Where to find information in this leaflet:
1. Why is Cafnea Injection or Cafnea Oral Solution being given?
2. What should I know before Cafnea Injection or Cafnea Oral Solution is given?
3. What if I am using other medicines?
4. How is Cafnea Injection or Cafnea Oral Solution given?
5. What should I know while using Cafnea Injection or Cafnea Oral Solution?
6. Are there any side effects?
7. Product details
1. Why is Cafnea Injection or Cafnea Oral Solution being given?
Cafnea Injection and Cafnea Oral Solution contain the active ingredient caffeine citrate.
Cafnea Injection and Cafnea Oral Solution are used to help improve the breathing of premature infants suffering from apnoea of prematurity who have been born between 28 and less than 33 weeks gestation.
Apnoea of prematurity is a condition where a baby stops breathing for short periods of time.
Cafnea Injection and Cafnea Oral Solution work by stimulating breathing in premature babies.
Ask your doctor if you have any questions about why Cafnea Injection or Cafnea Oral Solution has been prescribed for your baby.
Your doctor may have prescribed it for another reason.
2. What should I know before Cafnea Injection or Cafnea Oral Solution is given?
Warnings
You should not be given Cafnea Injection or Cafnea Oral Solution if:
- you are allergic to caffeine or citrate, or any other similar medicine.
- Always check the ingredients to make sure you can use this medicine.
Your baby should not be given Cafnea Injection or Cafnea Oral Solution if the solution is discoloured, cloudy, turbid, or a precipitate or particles are present. The solutions are normally clear, and colourless.
Your baby should not be given either medicine if, when mixed with another solution it causes the solution, to become discoloured, cloudy, turbid, precipitate or form particles.
The solutions are normally clear, and colourless.
The doctor or nurse will check to ensure the medicine is not past its expiry date and has not been tampered with.
If you are not sure whether your baby should be given either medicine talk to your doctor.
Check with your doctor if:
- your baby has allergies to any other medicines, foods, preservatives, or dyes.
- your baby's breathing problems are caused by other medical conditions. If the breathing problems are caused by another medical condition. Cafnea Injection or Cafnea Oral Solution may not be used until the other condition is treated.
- your baby has any of the following medical conditions:
- seizure disorders
- heart problems
- kidney problems
- liver problems.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
3. What if I am using other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines can be passed onto your baby through the placenta before birth or in breast milk.
Some medicines may interfere with Cafnea Injection and Cafnea Oral Solution. These include:
- methylxanthines such as theophylline and aminophylline, medicines used to control asthma
- antibiotics used to treat bacterial infections such as ciprofloxacin, enoxacin, norfloxacin
- any medicine containing caffeine
- medicines used to treat heart problems such as Mexiletine and Verapamil
- Cimetidine a medicine used to treat reflux and ulcers
- Fluvoxamine a medicine used to treat depression
- Idrocilamide a medicine used to relax muscle
- Methoxsalen a medicine used to treat skin problems
- Tiabendazole used to treat certain worm infections
- Artemisinin a medicine used to treat malaria
- medicines used to treat fungal infections such as Fluconazole and Terbinafine
- Phenytoin a medicine used to treat epilepsy
- benzodiazepines a group of medicines used as a sedative or to treat anxiety
- Clozapine a medicine used to treat schizophrenia.
These medicines may be affected by Cafnea Injection and Cafnea Oral Solution or may affect how well they work.
Your doctor and pharmacist have more information on medicines to be careful with or avoid while your baby is being given Cafnea Injection or Cafnea Oral Solution.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect Cafnea Injection or Cafnea Oral Solution.
4. How is Cafnea Injection or Cafnea Oral Solution given?
How much to be given
- Your doctor will decide what dose of Cafnea Injection or Cafnea Oral solution your baby will receive and for how long they will receive it. This depends on their medical condition and other factors, such as weight.
- It will also depend on what medicines and fluids the mother has consumed prior to delivery as these may have crossed the placenta and been passed onto the baby.
How is Cafnea Injection or Cafnea Oral Solution given
- Cafnea Injection or Cafnea Oral Solution must only be given by a doctor or nurse.
- Cafnea Injection is usually infused into a vein slowly using a syringe infusion pump.
- Cafnea Oral Solution is usually given in a measured dose by mouth through a dropper or feeding tube.
If too much Cafnea Injection or Cafnea Oral Solution is given
Both Cafnea Injection and Cafnea Oral Solution must only be given by a doctor or nurse, so an overdose is not likely to occur.
Contact your doctor or nurse immediately if you notice any symptoms of an overdose in your baby:
- jitteriness
- loss in weight
- fever
- irritability, sleeplessness
- poor feeding
- rapid shallow breathing, difficulty breathing
- muscle spasms or contractions including tremors in the hands or feet and arching of the back
- muscle spasm in which the head and the heels are bent backward and the body bowed forward
- muscle stiffness causing poor control of movement
- unusual jaw and lip movement
- vomiting
- passing large amounts of urine
- excessive thirst, dry mouth and skin
- seizures, fits or convulsions
- increased heart rate
- stomach bloating
- pain or redness at the injection site.
If you think that your baby had too much Cafnea Injection or Cafnea Oral Solution, your baby may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know while using Cafnea Injection or Cafnea Oral Solution?
Your doctor may do tests on your baby from time to time to make sure the medicine is working and to prevent unwanted side effects.
Looking after your medicine
Cafnea Injection and Cafnea Oral Solution will be stored in the surgery, pharmacy or ward of a hospital in a cool dry place where the temperature stays below 30°C.
Cafnea Injection or Cafnea Oral Solution will be opened for use on your baby. It will be used only once and then it will be discarded. It will never be stored after it is opened or used for more than one baby.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Tell your doctor or nurse as soon as possible if your baby does not appear well while receiving Cafnea Injection or Cafnea Oral Solution.
Do not be alarmed by the following list of side effects. Your baby may not experience any of them.
Serious side effects
| Serious side effects | What to do |
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor or nurse if you notice anything that is making your baby feel unwell.
Other side effects not listed above may also occur in some babies.
Some side effects can only be found when your doctor does tests from time to time to check your baby's progress.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What Cafnea Injection and Cafnea Oral Solution contains
| Active ingredient (main ingredient) | caffeine |
| Other ingredients (inactive ingredients) | citric acid monohydrate sodium citrate dihydrate water for injections |
These medicines do not contain lactose, sucrose, gluten, tartrazine or any other azo dyes, alcohol or preservatives.
Do not take this medicine if you are allergic to any of these ingredients.
What Cafnea Injection and Cafnea Oral Solution looks like
Cafnea Injection and Cafnea Oral Solution are clear, colourless solutions in a clear glass vial with a grey rubber stopper, aluminum seal and a plastic top.
Cafnea Injection
Cafnea Injection contains caffeine citrate 40 mg in 2 mL (equivalent to 20 mg of caffeine) is presented in 2 mL clear vial available as pack of 10 vials (AUST R 153873).
Cafnea Oral Solution
Cafnea Oral Solution contains caffeine citrate 25 mg in 5 mL (equivalent to 12.5 mg of caffeine) is available in 7 mL clear vial available as pack of 10 vials (AUST R 153874).
Who distributes Cafnea Injection and Cafnea Oral Solution
Cafnea Injection and Cafnea Oral solution is made and supplied in Australia by:
Phebra Pty Ltd
17-19 Orion Road
Lane Cove West, NSW 2066
Australia
Telephone: 1800 720 020

This leaflet was prepared in December 2025.
Cafnea, Phebra and the Phi symbol are registered trademarks of Phebra Pty Ltd.
Brand Information
| Brand name | Cafnea Injection and Cafnea Oral Solution |
| Active ingredient | Caffeine citrate |
| Schedule | Unscheduled |
MIMS Revision Date: 01 June 2021
1 Name of Medicine
Caffeine citrate.
2 Qualitative and Quantitative Composition
Cafnea Injection contains 20 mg/mL caffeine citrate (equivalent to 10 mg/mL of caffeine base).
Cafnea Oral Solution contains 5 mg/mL caffeine citrate (equivalent to 2.5 mg/mL of caffeine base).
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Both Cafnea Injection (caffeine citrate injection 40 mg/2 mL) and Cafnea Oral Solution (caffeine citrate oral solution 25 mg/5 mL) are clear, colourless, preservative free sterile solutions adjusted to a pH of 4.2 - 5.2.
4 Clinical Particulars
4.1 Therapeutic Indications
Cafnea Injection and Cafnea Oral Solution are indicated for the short-term treatment of apnoea of prematurity (AOP) in infants of gestational age 28 to less than 33 weeks.
4.2 Dose and Method of Administration
Cafnea Injection and Cafnea Oral Solution are intended to be used in neonatal specialist units. The product is for single use in one patient only. Discard any residue.
Note. A prior check should be made to ensure that no other methylxanthine (e.g. theophylline and aminophylline) is being administered.
Baseline serum levels of caffeine should be measured if mothers have consumed caffeine containing fluids prior to delivery, since caffeine readily crosses the placenta.
The dose expressed as caffeine base is half the dose when expressed as caffeine citrate (e.g. 20 mg of caffeine citrate is equivalent to 10 mg of caffeine base).
Loading dose. Caffeine citrate 20 mg/kg bodyweight intravenously using a syringe infusion pump over 30 minutes.
Maintenance dose. Caffeine citrate 5 mg/kg once a day until apnoea ceases or until treatment is considered to be no longer required. The maintenance dose can be increased to a maximum of 10 mg/kg caffeine citrate once a day if apnoea persists. The maintenance dose should be adjusted weekly for changes in bodyweight. If symptoms suggestive of caffeine induced toxicity are observed such as tachycardia, tachypnoea, jitteriness, tremors and unexplained seizures and vomiting, the dose of caffeine citrate can be reduced or withheld. The dose of caffeine citrate can be withheld or reduced for other clinical reasons.
Maintenance dose can be administered either intravenously (over 10 minutes) using Cafnea Injection or orally using Cafnea Oral Solution once the infant is tolerating full enteral feeds. Maintenance dose begins 24 hours after loading dose.
Compatibility. Cafnea Injection and Cafnea Oral Solution are compatible with 0.9% sodium chloride solution.
4.3 Contraindications
Cafnea Injection and Cafnea Oral Solution are contraindicated in patients who have demonstrated hypersensitivity to caffeine or citrate.
4.4 Special Warnings and Precautions for Use
Prior to treatment it is essential that other causes of apnoea (e.g. CNS disorders, primary lung disease, anaemia, sepsis, metabolic disturbances, cardiovascular abnormalities, or obstructive apnoea) be ruled out or treated prior to initiation of caffeine citrate therapy.
Caffeine is a CNS stimulant and in cases of caffeine overdose, seizures have been reported. Cafnea Injection and Cafnea Oral Solution should be used with caution in infants with seizure disorders.
Clinical trials have indicated that necrotising enterocolitis may develop in neonates under treatment. Patients should be carefully monitored for the development of necrotising enterocolitis.
Cardiovascular effects. Cafnea Injection and Cafnea Oral Solution should be used with caution in infants with cardiovascular disease since caffeine has been shown to increase heart rate, left ventricular output, and stroke volume.
Gastro-oesophageal disease. Cafnea Injection and Cafnea Oral Solution may relax the lower oesophageal sphincter and increase the gastric acid excretion leading to increased episodes of gastro-oesophageal reflux in neonates.
Use in hepatic impairment. Cafnea Injection and Cafnea Oral Solution should be administered with caution in infants with impaired hepatic function. In such cases, serum caffeine should be monitored and dose administration should be adjusted to avoid potential toxicity.
Use in renal impairment. Cafnea Injection and Cafnea Oral Solution should be administered with caution in infants with impaired renal function. In such cases, serum caffeine should be monitored and dose administration should be adjusted to avoid potential toxicity.
Use in the elderly. Cafnea is not applicable to this indication. See Section 4.1 Therapeutic Indications.
Paediatric use. Cafnea is indicated for use in pre-term infants of gestational age 28 to less than 33 weeks. See Section 4.1 Therapeutic Indications; Section 5.1, Clinical trials.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
There is little data on drug interactions with caffeine in preterm neonates. However, CYP1A2 is the major enzyme responsible for caffeine metabolism and there is potential for interactions between caffeine and drugs that are substrates for this enzyme, or inhibit or reduce it. Studies in adults show that co-administration of mexiletine, cimetidine, fluvoxamine, oral idrocilamide, oral methoxsalen and 5-methoxypsoralen, enoxacin, tiabendazole, artemisinin, fluconazole and terbinafine, verapamil may decrease caffeine elimination. Co-administration of phenytoin may increase caffeine elimination. Caffeine antagonises the effects of benzodiazepines. Caffeine increases the levels of both endogenous and orally administered melatonin as well as clozapine. Caffeine may cause a reduction in the bioavailability of fluvoxamine.
Caffeine elimination half-life has been reported to be increased and clearance decreased by concomitant administration of antibacterials such as ciprofloxacin, enoxacin and pipemidic acid, lomefloxacin, norfloxacin and ofloxacin.
Other methylxanthines (theophylline, aminophylline) should not be used concomitantly.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. Studies in animals are limited but suggest that neonatal exposure to caffeine does not pose a hazard to later fertility.
Use in pregnancy. Not applicable.
Use in lactation. Not applicable. If mothers are drinking caffeine containing fluids, this should be taken into consideration when determining the dose for the neonate.
4.7 Effects on Ability to Drive and Use Machines
The effects of this medicine on a person's ability to drive and use machines were not assessed as part of its registration.
4.8 Adverse Effects (Undesirable Effects)
Necrotising enterocolitis is a common event in preterm infants and must be investigated whether or not the infant is receiving caffeine. See Table 1.
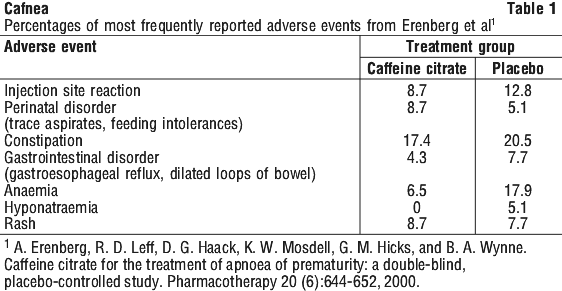
CNS stimulation: i.e. irritability, restlessness, jitteriness.
Cardiovascular effects: tachycardia, increased left ventricular output and increased stroke volume.
Gastrointestinal effects: i.e. increased gastric aspirate, gastrointestinal intolerance.
Alterations in serum glucose: hypoglycaemia and hyperglycaemia.
Renal effects: increased urine flow rate, increased creatinine clearance and increased sodium and calcium excretion.
Adverse effects observed in the Schmidt et al2,3 controlled clinical trials have included tachycardia, tachypnoea, jitteriness, tremors, unexplained seizures and vomiting. Caffeine reduced weight gain temporarily.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
Up to three times the usual dose has been given without noticeable side effects except an increase in jitteriness and a loss in weight which returns to normal following cessation of therapy. Higher doses may result in fever, irritability, poor feeding, insomnia, tachypnoea, jitteriness, fine tremor of the extremities, hypertonia, opisthotonos, tonic-clonic movements, nonpurposeful jaw and lip movements, vomiting, hyperglycaemia, elevated blood urea nitrogen, and elevated total leukocyte concentration, seizures, neurological sequelae, tachycardia, respiratory distress, heart failure, gastric distention and acidosis.
Treatment of overdose. Treatment of caffeine overdose is primarily symptomatic and supportive. Caffeine levels have been shown to decrease after exchange transfusions. Convulsions may be treated with intravenous administration of diazepam or a barbiturate such as pentobarbital sodium.
Treatment of withdrawal. Caffeine withdrawal. No withdrawal symptoms have been reported following short-term therapy (less than three weeks).
For information on the management of overdose, contact the Poison Information Centre on 131126 (Australia).
5 Pharmacological Properties
Note. The pharmacology, dosage regimens and clinical descriptions apply only to preterm infants with apnoea.
Caffeine is a methylxanthine and is structurally related to other methylxanthines such as theophylline.
5.1 Pharmacodynamic Properties
Mechanism of action. Caffeine is a centrally acting respiratory stimulant. It increases respiratory rate (breaths/minute) significantly in premature infants and significantly reduces the number of short and prolonged attacks of apnoea. There is evidence that caffeine has a direct effect on the myocardium. In ventilator dependent preterm infants, caffeine has been shown to reduce pulmonary resistance and increase lung compliance with a concomitant reduction in the requirement for inspired oxygen.
The following pharmacodynamic effects of caffeine were found in preterm infants with apnoea.
Caffeine increases heart rate.
Caffeine increased respiratory rate in some studies but not others.
Mean arterial blood pressure, TcPO2, TcPCO2 are unchanged.
Blood flow volumes in the coeliac artery and superior mesenteric artery, LVO, PCO2, do not change significantly.
Caffeine increases cerebral blood flow in some studies but not in others.
Clinical trials. Efficacy study. The randomised double blinded placebo controlled trial by Erenberg et al1 evaluated the efficacy and safety of caffeine citrate for the treatment of AOP. The study included a total of 87 preterm infants of 28-32 weeks post-conceptional age. Infants randomised to caffeine received a loading dose of 20 mg/kg caffeine citrate IV. A daily maintenance dose of caffeine citrate 5 mg/kg was administered by IV or orally for 10 days.
The primary efficacy end point was at least a 50% reduction in apnoeic episodes from baseline events and elimination of apnoea. Caffeine citrate was significantly more effective than placebo in reducing apnoeic episodes by at least 50% in 6 days (p < 0.05). The percentage of patients with 50% reduction in apnoeic episodes was 68.9% active treatment vs 43.2% placebo (p = 0.02). Caffeine citrate was also significantly better at eliminating apnoea in 5 days (p < 0.05). The percentage of patients with elimination of apnoeic episodes was 24.4% active treatment vs 0% placebo (p = 0.005).
Safety study. The long term safety study by Schmidt et al2,3 was a large multinational study involving 2006 randomised preterm infants with birth weights of 500 to 1250 g in which caffeine was compared to placebo for the short and long term safety of caffeine treatment for apnoea of prematurity (AOP), the prevention of AOP or to facilitate extubation. Treated infants received an intravenous loading dose of 20 mg/kg of caffeine citrate followed by a daily maintenance dose of 5 mg/kg IV or orally. If apnoea persisted, the daily maintenance dose could be increased to a maximum of 10 mg/kg. Maintenance dose was adjusted weekly for changes in body weight. See Table 2.
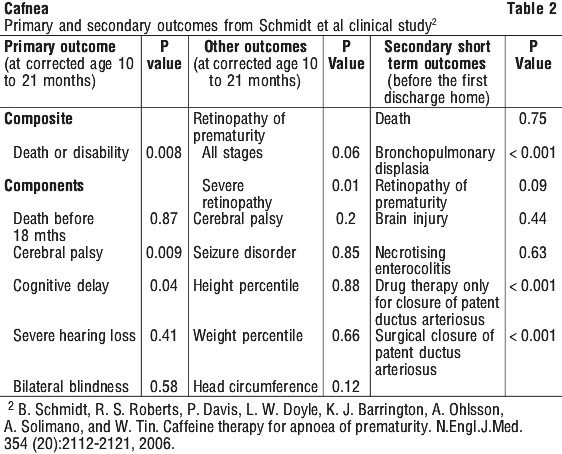
5.2 Pharmacokinetic Properties
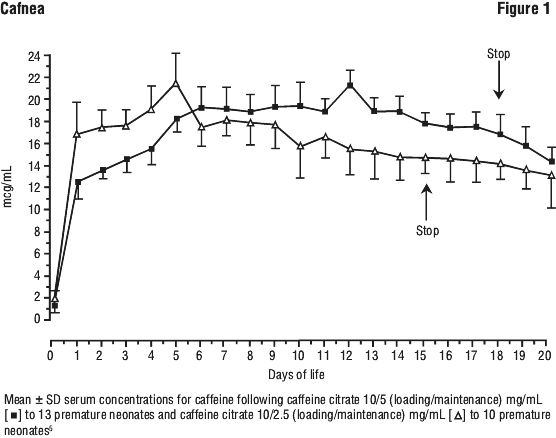
Absorption. Following an oral dose of caffeine citrate solution, the time to reach peak concentration ranges from 30 minutes to 2 hours. Absorption following oral administration is complete. Feeding does not affect the rate or extent of oral caffeine absorption in premature infants. Following an intravenous (IV) loading dose of 20 mg/kg of caffeine citrate, the mean peak plasma level for caffeine is 12 mg/L. Following a single 10 mg/kg IV infusion of caffeine citrate, the mean ± SD serum concentration of caffeine was 14.5 ± 1.4 micrograms/mL at 10 minutes, 11.3 ± 0.1 micrograms/mL at 24 hours and 6.1 micrograms/mL at 72 hours. After a loading dose of 10 mg/kg of caffeine citrate and maintenance dose of either 5 mg/kg/day orally or 10 mg/kg/day orally, serum concentrations reached steady state at about 5 days with higher concentrations being observed with the 5 mg/kg maintenance regimen4 (see Figure 1). Following maintenance doses of caffeine citrate 5 mg/kg, caffeine plasma levels range from 5 to 15 mg/L.
Distribution. Caffeine is distributed rapidly in infants with a volume of distribution, V = 0.8 to 0.9 L/kg.
Metabolism. Caffeine is poorly metabolised in preterm infants. The primary metabolites of caffeine are paraxanthines (main metabolite), theobromine, and theophylline. Interconversion between caffeine and theophylline has been observed in premature infants and approximately 3% to 8% of administered caffeine is expected to be converted to theophylline.
Caffeine is metabolised in the liver by cytochrome P450 enzymes, primarily by CYP1A2. This enzyme catalyses N1, N3, and N7-demethylation of caffeine. In addition, CYP2E1 also catalyses N1 and N7-demethylation, while CYP3A catalyses 8-hydroxylation. The N3 and N7 metabolic pathways are not mature until a postnatal age of about 4 months and explain the long half-life and low clearance in infants younger than this age.
Special groups. Neonates of Asian background tolerated an IV loading dose of 20 mg/kg caffeine citrate with a maintenance dose of 5 mg/kg/day caffeine citrate IV. A higher maintenance dose resulted in an increase of hyperglycaemia and tachycardia6.
Other studies have found no effect of gender or race on volume of distribution of caffeine. Hepatic impairment as measured by serum creatinine or serum urea levels did not influence volume of distribution.
5.3 Preclinical Safety Data
Genotoxicity. Assays for bacterial and mammalian mutagenicity in vitro, and for clastogenicity in vitro and in vivo generally show negative results for caffeine. Positive responses have been observed in some tests, but these studies use extreme concentrations, lethal doses or nonvalidated methods. Cafnea is not considered to pose a genotoxic hazard to patients.
Carcinogenicity. In a small number of animal studies, caffeine did not show carcinogenicity or tumorigenicity. In a two year carcinogenicity study conducted in rats, caffeine (administered as base) did not increase tumour incidence at oral doses up to 102 mg/kg/day in males and 170 mg/kg/day in females. Systemic exposure in animals at these doses is estimated to be 2-6 times higher than that in neonates at the recommended maintenance dose of 5 mg/kg/day caffeine citrate.
6 Pharmaceutical Particulars
6.1 List of Excipients
Cafnea Injection contains the excipients citric acid monohydrate and sodium citrate dihydrate in water for injections. The injection contains no preservatives.
Cafnea Oral Solution contains the excipients citric acid monohydrate and sodium citrate dihydrate in water for injections. The solution contains no preservatives.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG*). The expiry date can be found on the packaging.
*AUST R 153873 (injection); AUST R 153874 (oral solution).
6.4 Special Precautions for Storage
The product is for single use in one patient only. Discard any residue. Store below 30°C.
6.5 Nature and Contents of Container
Cafnea Injection: 40 mg caffeine citrate (equivalent to 20 mg caffeine) per 2 mL injection presented in a 2 mL clear vial available as a pack of 10 vials.
Phebra product code - INJ101.
Cafnea Oral Solution: 25 mg caffeine citrate (equivalent to 12.5 mg caffeine) per 5 mL of sterile solution presented in a 7 mL clear vial available as a pack of 10 vials.
Phebra product code - SOL026.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Caffeine citrate. The molecular weight of the compound is 386.3.
The molecular formula is C8H10N4O2,C6H8O7.
Chemical structure. Chemical structure of caffeine citrate:
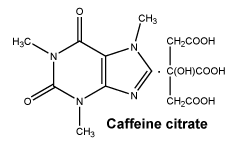
The molecular weight of caffeine is 194.2.
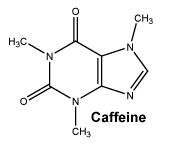
The chemical name for caffeine is 1,3,7-trimethyl-3,7-dihydro-1H-purine-2,6-dione.
The molecular formula is C8H10N4O2.
Chemical structure. Chemical structure of caffeine:
7 Medicine Schedule (Poisons Standard)
Not scheduled.
Date of First Approval
17 March 2010
Date of Revision
03 May 2021
Summary Table of Changes

References
1 A. Erenberg, R. D. Leff, D. G. Haack, K. W. Mosdell, G. M. Hicks, and B. A. Wynne. Caffeine citrate for the treatment of apnoea of prematurity: a double-blind, placebo-controlled study. Pharmacotherapy 20 (6):644-652, 2000.
2 B. Schmidt, R. S. Roberts, P. Davis, L. W. Doyle, K. J. Barrington, A. Ohlsson, A. Solimano, and W. Tin. Caffeine therapy for apnoea of prematurity. N.Engl.J.Med. 354 (20):2112-2121, 2006.
3 B. Schmidt, R. S Roberts, P. Davis, L. W Doyle, K. J Barrington, A. Ohlsson, A. Solimano, W. Tin. Long-term effects of caffeine therapy for apnoea of prematurity. N Engl J Med. 357 (19):1893-902, 2007.
4 M. P. De Carolis, C. Romagnoli, U. Muzii, G. Tortorolo, M. Chiarotti, Giovanni N. De, and A. Carnevale. Pharmacokinetic aspects of caffeine in premature infants. Dev. Pharmacol.Ther. 16 (3):117-122, 1991.
5 C. Romagnoli, M. P. De Carolis, U. Muzii, E. Zecca, G. Tortorolo, M. Chiarotti, Giovanni N. De, and A. Carnevale. Effectiveness and side effects of two different doses of caffeine in preventing apnoea in premature infants. Ther.Drug Monit. 14 (1):14-19, 1992.
6 H. S. Lee, Y. M. Khoo, Y. Chirino-Barcelo, K. L. Tan, and D. Ong. Caffeine in apnoeic Asian neonates: a sparse data analysis. Br.J.Clin.Pharmacol. 54 (1):31-37, 2002.
Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.