Calquence Tablets
Brand Information
| Brand name | Calquence Tablets |
| Active ingredient | Acalabrutinib |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Calquence Tablets.
Summary CMI
CALQUENCE® Tablets
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using CALQUENCE tablets?
CALQUENCE tablets contain the active ingredient acalabrutinib maleate monohydrate. CALQUENCE tablets are used to treat Mantle Cell Lymphoma (MCL) and Chronic Lymphocytic Leukaemia (CLL)/Small Lymphocytic Lymphoma (SLL).
For more information, see Section 1. Why am I using CALQUENCE tablets? in the full CMI.
2. What should I know before I use CALQUENCE tablets?
Do not use if you have ever had an allergic reaction to CALQUENCE or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I use CALQUENCE tablets? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with CALQUENCE tablets and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use CALQUENCE tablets?
- The usual dose is one 100 mg tablet twice a day. Doses should be taken about 12 hours apart.
- Swallow the tablet whole with water. Do not chew, crush, dissolve, or divide the tablets.
More instructions can be found in Section 4. How do I use CALQUENCE tablets? in the full CMI.
5. What should I know while using CALQUENCE?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using CALQUENCE tablets? in the full CMI.
6. Are there any side effects?
All medicines can have side effects. Sometimes they are serious, most of the time they are not. You may need medical attention if you get some of the side effects. Tell your doctor, nurse or pharmacist if you notice any of the following and they worry you: fever, chills, headache, nausea, vomiting, dizziness, stomach pain, diarrhoea, constipation, rash, bruising, bleeding, fatigue, muscle and bone pain, joint pain, new cancers. Tell your doctor, nurse or pharmacist as soon as possible if you notice any of the following: signs or symptoms of serious bleeding, infection or heart problems.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
1. Why am I using CALQUENCE?
CALQUENCE tablets contain the active ingredient acalabrutinib maleate monohydrate.
CALQUENCE belongs to a group of anti-cancer medicines called Bruton tyrosine kinase (BTK) inhibitors. BTK is a protein in the body that helps cancer cells to grow.
CALQUENCE works by blocking BTK which may help to reduce the number of cancer cells and may slow the spread of the cancer.
CALQUENCE tablets are used to treat:
Mantle Cell Lymphoma (MCL), a type of blood cancer that affects the lymph nodes (lymph glands). It is used in:
- patients who are not intending to have a stem cell transplant procedure and have not been previously treated.
- or in patients who have had at least one other treatment for their cancer.
Chronic Lymphocytic Leukaemia (CLL)/Small Lymphocytic Lymphoma (SLL), a type of blood cancer that affects lymphocytes (a certain type of white blood cell) and the lymph nodes. It is used in:
- patients who have not had any previous treatment for their cancer, CALQUENCE can be used alone, or in combination with other anti-cancer medicines.
- patients who have had at least one previous treatment for their cancer.
If using CALQUENCE in combination, it is important that you also read the Consumer Medicine Information (CMI) for the specific anti-cancer medicines you may be receiving. If you have any questions about these medicines, ask your doctor.
2. What should I know before I use CALQUENCE?
Do not use CALQUENCE tablets if:
- you are pregnant or intend to become pregnant
- you are breastfeeding
- you are allergic to acalabrutinib, or any of the ingredients listed at the end of this leaflet.
Some of the symptoms of an allergic reaction may include:
shortness of breath; wheezing or difficulty breathing; swelling of the face, lips, tongue or other parts of the body; rash, itching or hives on the skin.
There is not enough information to recommend the use of this medicine for children or adolescents under the age of 18 years.
Check with your doctor if you:
- have allergies to any other medicines, foods, preservatives or dyes
- have any other medical conditions such as:
- any unusual bruising or bleeding, or you have any bleeding disorders
- infections (bacterial, viral and/or fungal)
- any liver problems
- a liver infection (Hepatitis B), so that your doctor can look out for signs of reactivation of this infection, such as fever, chills, weakness, confusion, vomiting and jaundice (yellowing of the skin or eyeballs)
- have or have had heart rhythm problems (such as atrial fibrillation)
- any other medical conditions - take any medicines for any other condition
- have recently undergone surgery or are planning any surgery or medical or dental procedures.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor if you are pregnant or intend to become pregnant.
CALQUENCE tablets may harm your unborn baby.
You should not take CALQUENCE tablets if you are pregnant and you should not get pregnant while you are taking CALQUENCE tablets. Use effective contraception (such as condoms) during treatment with CALQUENCE tablets and for at least one week after your final dose of CALQUENCE tablets.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
You should not breastfeed during treatment with CALQUENCE tablets.
It is not known if CALQUENCE tablets pass into your breast milk. Do not breast-feed during treatment with CALQUENCE tablets and for at least 2 weeks after your final dose of CALQUENCE tablets.
3. What if I am taking other medicines?
Tell your doctor, nurse or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with CALQUENCE tablets and affect how it works.
- Medicines used to control heart rhythm disturbances (e.g. amiodarone, diltiazem, verapamil)
- Antibiotics used to treat bacterial infections (e.g. clarithromycin, erythromycin, telithromycin, ciprofloxacin, rifampin)
- Medicines to treat fungal infections (e.g. fluconazole, posaconazole, ketoconazole, itraconazole, voriconazole)
- Medicines used to treat HIV infection (e.g. ritonavir, cobicistat, indinavir, nelfinavir, saquinavir, amprenavir, atazanavir, darunavir/ritonavir or fosamprenavir)
- Medicines used to treat hepatitis C infection (e.g. telaprevir)
- Medicines used to prevent seizures or to treat epilepsy (e.g. carbamazepine, phenytoin)
- St. John's wort - a herbal medicine used to treat depression
- Methotrexate, a medicine used to treat other cancers or to treat immune disorders such as rheumatoid arthritis or psoriasis.
- Medicines used to control blood sugar in patients with diabetes (eg. metformin)
CALQUENCE tablets may make you bleed more easily. This means you should tell your doctor if you take other medicines that increase your risk of bleeding. These include:
- Medicines used to treat pain and inflammatory conditions (e.g. aspirin and non-steroidal anti-inflammatory [NSAIDS] such as ibuprofen)
- Medicines used to prevent blood clots, such as antiplatelet therapy or blood thinners (e.g. aspirin, warfarin).
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect CALQUENCE tablets.
4. How do I use CALQUENCE tablets?
Your doctor has prescribed CALQUENCE film-coated tablets for you. Please note CALQUENCE is also available as a 100 mg capsule and should not be interchanged with CALQUENCE film-coated tablets.
How much to take
- The usual dose is one 100 mg tablet twice a day.
Follow the instructions provided and use CALQUENCE tablets until your doctor tells you to stop. Check with your doctor, nurse or pharmacist if you are not sure.
The instructions may differ from the information contained in this leaflet.
When to take CALQUENCE tablets
- CALQUENCE tablets should be taken about 12 hours apart.
- Take your medicine at about the same time each day.
Taking it at the same time each day will have the best effect. It will also help you remember when to take it.
You can check when you last took a tablet of CALQUENCE tablets by looking at the sun and moon symbols on the blister pack. There is a sun (for the morning) and a moon (for the evening). This will tell you whether you have taken the dose.
It is important that you tell your doctor that you are taking any of the medicines mentioned in the ‘Taking other medicines section’, as you may need to:
- avoid taking certain medicines including certain medicines used to treat fungal infections
- take your medicine at a different time to CALQUENCE tablets
- Temporarily decrease your dose of CALQUENCE depending on which other medicine.
How to take / use CALQUENCE tablets
- Swallow the tablet whole with water. Do not chew, dissolve, divide, or crush the tablets.
- You can take CALQUENCE with or without food.
If you forget to use CALQUENCE tablets
CALQUENCE tablets should be used regularly at the same time each day.
If you miss a dose by more than 3 hours, skip the dose you missed and take your next dose when you are meant to.
Do not take a double dose to make up for the dose you missed.
If you take too much CALQUENCE tablets
If you think that you have used too much CALQUENCE tablets, you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know while using CALQUENCE tablets?
Things you should do
- You should be careful to protect yourself from the sun.
- If you are about to be started on any new medicine, remind your doctor, nurse and pharmacist that you are taking CALQUENCE tablets.
- If you are going to have surgery, tell the surgeon or anaesthetist that you are taking this medicine.
- If you are about to have any blood tests, tell your doctor and nurse that you are taking this medicine.
- Keep all of your doctor's appointments so that your progress can be checked.
Call your doctor straight away if you:
- become pregnant while taking this medicine,
Remind any doctor, nurse, dentist or pharmacist you visit that you are using CALQUENCE tablets.
Things you should not do
- Do not stop using this medicine or change the dose without checking with your doctor.
- Do not give this medicine to anyone else, even if they have the same condition as you.
- Do not take it after the expiry date printed on the pack or if the packaging is torn or shows signs of tampering. If it has expired or is damaged, return it to your pharmacist for disposal
Driving or using machines
Be careful before you drive or use any machines or tools until you know how CALQUENCE tablets affects you.
CALQUENCE may cause dizziness, weakness or tiredness in some people.
Food and drink
You can take CALQUENCE tablets with or without food.
Looking after your medicine
Store it in a cool dry place where the temperature stays below 30°C. Keep CALQUENCE tablets away from moisture, heat or sunlight; for example, do not store it:
- in the bathroom or near a sink, or
- in the car or on windowsills.
Keep it where young children cannot reach it.
Getting rid of any unwanted medicine
If you no longer need to use this medicine or it is out of date, take it to any pharmacy for safe disposal.
Do not use this medicine after the expiry date.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
Bleeding
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
Bleeding
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Like other cancer medicines, new cancers such as skin cancers have been known to occur in patients taking CALQUENCE tablets.
Some side effects can also be found when your doctor or nurse does regular blood tests. These include:
- decreased number of white blood cells (neutropenia).
- decreased number of red blood cells (anaemia).
- decreased number of platelets which are cells that help your blood to clot (thrombocytopenia).
- Increased level of liver enzymes (aspartate aminotransferase and alanine aminotransferase).
- condition called tumour lysis syndrome (TLS), when there are unusual levels of chemicals in the blood caused by the fast breakdown of cancer cells have happened during treatment of cancer and sometimes even without treatment. Signs of TLS are changes in kidney function, abnormal heartbeat, or seizures.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What CALQUENCE tablets contain
| Active ingredient (main ingredient) | acalabrutinib maleate monohydrate |
| Other ingredients (inactive ingredients) | mannitol microcrystalline cellulose hyprolose sodium stearylfumarate hypromellose copovidone titanium dioxide macrogol 3350 medium chain triglycerides iron oxide yellow iron oxide red |
Do not take this medicine if you are allergic to any of these ingredients.
This medicine does not contain lactose, sucrose, gluten, tartrazine or any other azo dyes.
What CALQUENCE looks like
The CALQUENCE 100 mg film-coated tablet is an orange, 7.5 x 13 mm, oval, biconvex tablet, debossed with ‘ACA 100’ on one side and plain on the reverse (Aust R 377410).
CALQUENCE tablets is supplied in a carton containing 7 blister strips, each containing 8 tablets (a total of 56 tablets in a carton).
Who distributes CALQUENCE tablets
AstraZeneca Pty Ltd
ABN 54 009 682 311
66 Talavera Road
MACQUARIE PARK NSW 2113
Telephone: 1800 805 342
This leaflet was prepared in March 2026.
CALQUENCE is a registered trademark of the AstraZeneca group of companies.
© AstraZeneca 2026
VV-RIM-04944888 v 5.0
Brand Information
| Brand name | Calquence Tablets |
| Active ingredient | Acalabrutinib |
| Schedule | S4 |
MIMS Revision Date: 01 May 2026
1 Name of Medicine
Acalabrutinib maleate monohydrate.
2 Qualitative and Quantitative Composition
Each film-coated tablet contains acalabrutinib maleate monohydrate equivalent to 100 mg of acalabrutinib.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
The Calquence 100 mg film-coated tablet is an orange, 7.5 x 13 mm, oval, biconvex tablet, debossed with 'ACA 100' on one side and plain on the reverse.
4 Clinical Particulars
4.1 Therapeutic Indications
Mantle cell lymphoma (MCL). Calquence as monotherapy is indicated for the treatment of patients with mantle cell lymphoma (MCL) who have received at least one prior therapy.
Calquence in combination with bendamustine and rituximab (BR) is indicated for the treatment of adult patients with previously untreated mantle cell lymphoma (MCL) who are not eligible for autologous haematopoietic stem cell transplantation.
Chronic lymphocytic leukaemia (CLL) / small lymphocytic lymphoma (SLL). Calquence as monotherapy is indicated for the treatment of patients with chronic lymphocytic leukaemia (CLL)/small lymphocytic lymphoma (SLL) who have received at least one prior therapy.
Calquence as monotherapy or in combination with obinutuzumab is indicated for the treatment of patients with previously untreated chronic lymphocytic leukaemia (CLL)/small lymphocytic lymphoma (SLL). For details of the combination regimens, see Section 5.1 Pharmacodynamic Properties, Clinical trials.
Calquence in combination with venetoclax with or without obinutuzumab is indicated for the treatment of patients with previously untreated chronic lymphocytic leukaemia (CLL)/small lymphocytic lymphoma (SLL). For details of the combination regimens, see Section 5.1 Pharmacodynamic Properties, Clinical trials.
4.2 Dose and Method of Administration
Treatment with Calquence should be initiated and supervised by a physician experienced in the use of anticancer therapies.
Recommended dosage (18 years and above). Mantle cell lymphoma (MCL). The recommended dose of Calquence in monotherapy or in combination with other medicines is 100 mg (1 tablet) twice daily. For the combination regimens, refer to the product information of each of the medicine for dosing information. For details of the combination regimens, see Section 5.1 Pharmacodynamic Properties, Clinical trials.
Chronic lymphocytic leukaemia (CLL). The recommended dose of Calquence for the treatment of CLL is 100 mg (1 tablet) twice daily, either as monotherapy or in combination. Refer to the product information of each of the combination medicines for recommended dosing information (for details of the combination regimen, see Section 5.1 Pharmacodynamic Properties, Clinical trials).
Calquence doses should be separated by approximately 12 hours.
Treatment with Calquence monotherapy or in combination with obzinutumab should continue until disease progression or unacceptable toxicity.
Treatment with Calquence in combination with venetoclax with or without obinutuzumab should continue until disease progression, unacceptable toxicity or completion of 14 cycles of treatment (each cycle is 28 days).
Missed dose. If a patient misses a dose of Calquence by more than 3 hours, they should take the next dose at its regularly scheduled time. Extra tablets of Calquence should not be taken to make up for a missed dose.
Dose adjustments. Adverse reactions. Recommended dose modifications for adverse reactions are provided in Table 1 (for patients receiving Calquence monotherapy, and Calquence in combination with obinutuzumab or in combination with venetoclax with or without obinutuzumab) and Table 2 (for patients receiving Calquence in combination with bendamustine and rituximab). Refer to the product information of each medicine used in combination with Calquence for additional information regarding management of toxicities.
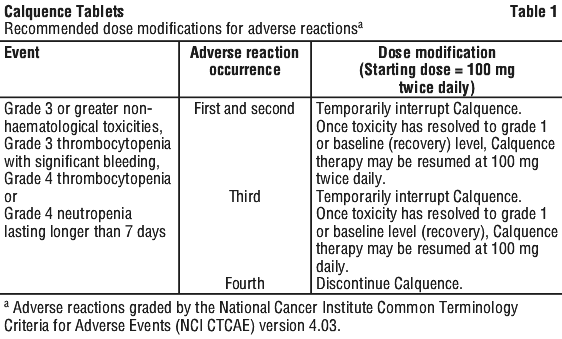
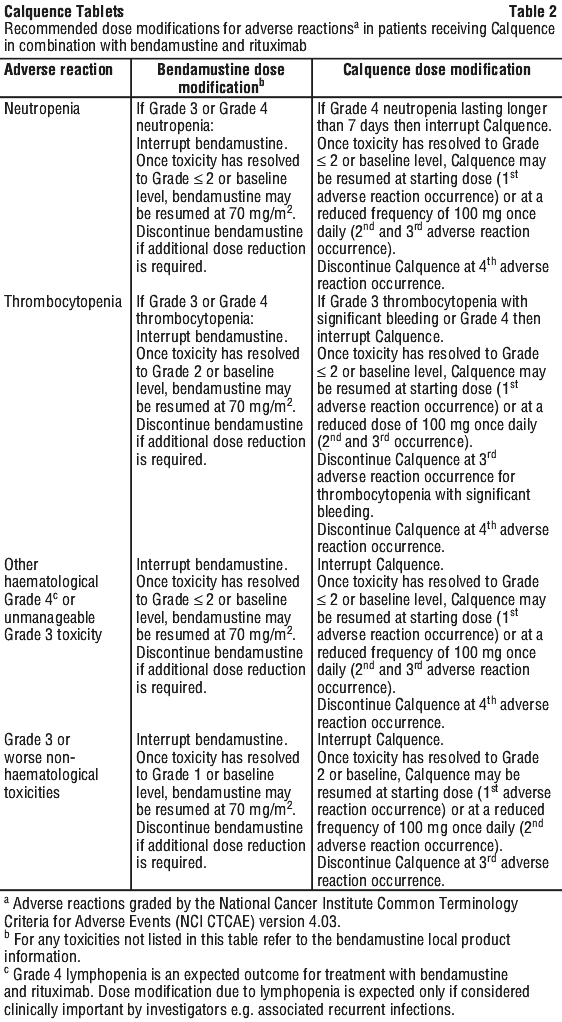

Hepatic impairment. No dose adjustment is recommended in patients with mild or moderate hepatic impairment (Child-Pugh A, Child-Pugh B, or total bilirubin between 1.5-3 times the upper limit of normal [ULN] and any AST). It is not recommended to administer Calquence in patients with severe hepatic impairment (Child-Pugh C or total bilirubin > 3 times ULN and any AST) (see Section 5.2 Pharmacokinetic Properties).
Severe cardiac disease. Patients with severe cardiovascular disease were excluded from Calquence clinical studies.
Elderly patients. No dose adjustment is necessary based on age (see Section 5.2 Pharmacokinetic Properties).
Paediatric patients. The safety and efficacy of Calquence in children and adolescents aged less than 18 years have not been established.
Method of administration. Calquence should be swallowed whole with water at approximately the same time each day. Calquence can be taken with or without food. The tablet should not be chewed, crushed, dissolved, or divided.
4.3 Contraindications
None.
4.4 Special Warnings and Precautions for Use
Haemorrhage. Serious haemorrhagic events, including fatal events, have occurred in the combined safety database of 1478 patients with haematological malignancies treated with Calquence monotherapy. Major haemorrhage (Grade 3 or higher bleeding events, serious, or any central nervous system events) occurred in 5.5% of patients, with fatalities occurring in 0.1% of patients. Overall, bleeding events including bruising and petechiae of any grade occurred in 46.1% of patients with haematological malignancies.
The mechanism for the bleeding events is not well understood. Use of antithrombotic agents concomitantly with Calquence may increase the risk of haemorrhage. In Calquence clinical trials, 3% of patients taking Calquence without antithrombotic agents experienced major haemorrhage. The addition of antithrombotic agents increased the percentage to 4.3%. Consider the risks and benefits of antithrombotic agents when co-administered with Calquence. Patients should be monitored for signs of bleeding. Consider the benefit-risk of withholding Calquence for 3-7 days pre- and post-surgery depending upon the type of surgery and the risk of bleeding.
Infection. Serious infections (bacterial, viral or fungal), including fatal events have occurred in the combined safety database of 1478 patients with haematological malignancies treated with Calquence monotherapy.
Grade 3 or higher infections occurred in 26.4% of these patients. The most frequently reported Grade 3 or higher infection was pneumonia. Infections due to hepatitis B virus (HBV) reactivation, aspergillosis, and progressive multifocal leukoencephalopathy (PML) have occurred. Serious and/or fatal COVID-19 infection has occurred, particularly when Calquence is used in combination with venetoclax with, or without, obinutuzumab. Appropriate monitoring and prophylaxis, as indicated, together with careful patient selection taking into account the risk of infection, are essential to optimise the benefit-risk profile of Calquence.
Consider prophylaxis for opportunistic infections in line with standard of care. Monitor patients for signs and symptoms of infection and treat as medically appropriate.
Cytopenias. In the combined safety database of 1478 patients with haematological malignancies, patients treated with Calquence monotherapy commonly experienced Grade 3 or higher cytopenias, including neutropenia (17.5%), anaemia (9.5%) and thrombocytopenia (6.2%). Monitor complete blood counts as medically appropriate during treatment.
Second primary malignancies. Second primary malignancies, including non-skin cancers, occurred in 17.6% of patients with haematological malignancies treated with Calquence monotherapy in the combined safety database of 1478 patients. The most frequent second primary malignancy was skin cancer, which occurred in 9.9% of patients. Monitor patients for the appearance of skin cancers. Advise protection from sun exposure.
Atrial fibrillation and flutter. In the combined safety database of 1478 patients with haematological malignancies treated with Calquence monotherapy, atrial fibrillation and atrial flutter of any grade occurred in 7.4% of patients and Grade 3 or higher occurred in 2.3% of patients. Monitor for symptoms (e.g. palpitations, dizziness, syncope, chest pain, dyspnoea) of atrial fibrillation and atrial flutter and obtain an ECG as appropriate.
Use in the elderly. Of the 1478 patients in clinical trials of Calquence monotherapy, 42% were ≥ 65 years of age and less than 75 years of age, and 20.6% were 75 years of age or older. No clinically relevant differences in safety or efficacy were observed between patients ≥ 65 years and younger.
Paediatric use. The safety and efficacy of Calquence in children and adolescents aged less than 18 years have not been established.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Interactions with CYP3A inhibitors and inducers. The clinical impact and prevention or management of interactions with CYP3A inhibitors or inducers are provided in Table 4. Also see Section 4.2 Dose and Method of Administration; Section 5.2 Pharmacokinetic Properties.
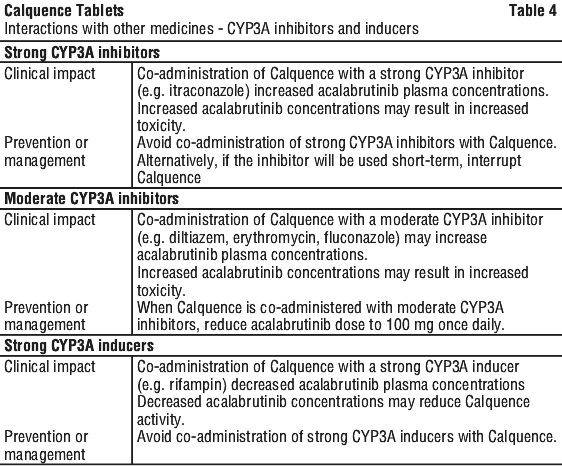
Effects of acalabrutinib and its active metabolite, ACP-5862, on drug transport systems. Acalabrutinib may increase exposure to co-administered BCRP substrates (e.g. methotrexate) by inhibition of intestinal BCRP.
ACP-5862 may increase exposure to co-administered MATE1 substrates (e.g. metformin) by inhibition of MATE1.
In vitro, acalabrutinib and ACP-5862 are substrates of P-glycoprotein (P-gp) and breast cancer resistance protein (BCRP). Acalabrutinib is not a substrate of renal uptake transporters OAT1, OAT3, and OCT2, or hepatic transporters OATP1B1 and OATP1B3. ACP-5862 is not a substrate of OATP1B1 or OATP1B3. Acalabrutinib and ACP-5862 do not inhibit P-gp, OAT1, OAT3, OCT2, OATP1B1, OATP1B3 and MATE2-K at clinically relevant concentrations.
Effect of food on acalabrutinib. In healthy subjects, administration of a single 100 mg dose of acalabrutinib tablet with a high fat, high calorie meal (approximately 918 calories, 59 grams carbohydrate, 59 grams fat, and 39 grams protein) did not affect the mean AUC as compared to dosing under fasted conditions. Resulting Cmax decreased by 54% and Tmax was delayed 1-2 hours.
Gastric acid reducing medications. Acalabrutinib tablets can be co-administered with gastric acid reducing agents (proton pump inhibitors, H2-receptor antagonists, antacids).
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. No effects on fertility were observed in male or female rats at exposures 10- or 9-times the clinical exposure (based on AUC) at the recommended dose, respectively.
Use in pregnancy. (Category C)
No clinical data are available, but based on findings in animals (see below), Calquence can cause fetal harm and dystocia if administered during pregnancy. Test for pregnancy prior to initiating treatment with Calquence, and advise patients of the potential risk to a fetus. Patients who could become pregnant should use highly effective contraception (such as condoms) during treatment with acalabrutinib and for one week following the last dose.
In an embryofetal study in pregnant rabbits, decreased fetal body weight and delayed skeletal ossification were observed at exposure levels that produced maternal toxicity, which were 2.4 times greater than the clinical exposure (based on AUC) at the recommended dose.
No effects on embryofetal development and survival were observed in one study in pregnant rats, at exposures approximately 9 times greater than the clinical exposure (based on AUC) at the recommended dose. In another study in pregnant rats, underdeveloped renal papilla was observed in F1 generation offspring at doses resulting in maternal exposures approximately 5 times greater than the clinical exposure (based on AUC) at the recommended dose. In two rat reproductive studies, dystocia (prolonged/difficult labour) and mortality of offspring were observed at exposures > 2.3 times greater than the clinical exposure (based on AUC) at the recommended dose. The presence of acalabrutinib and its active metabolite were confirmed in foetal rat plasma. Acalabrutinib and its active metabolite were present in the milk of lactating rats.
Use in lactation. No data are available regarding the presence of acalabrutinib or its active metabolite in human milk, its effects on the breastfed child, or on milk production. Acalabrutinib and its active metabolite were present in the milk of lactating rats. Due to the potential for adverse reactions in a breastfed child from Calquence, advise patients not to breastfeed while taking Calquence and for at least 2 weeks after the final dose.
4.7 Effects on Ability to Drive and Use Machines
Calquence has no or negligible influence on the ability to drive and use machines. However, during treatment with acalabrutinib fatigue and dizziness have been reported and patients who experience these symptoms should observe caution when driving or using machines.
4.8 Adverse Effects (Undesirable Effects)
Summary of the safety profile. Calquence monotherapy. Across 11 studies, 1478 patients with haematological malignancies have received Calquence as monotherapy at the recommended dose (100 mg twice daily; approximately every 12 hours). The median and mean duration of treatment was 38 months. The most commonly reported (≥ 20%) adverse drug reactions of any grade were infection, diarrhoea, headache, musculoskeletal pain, bruising, cough, arthralgia, fatigue, nausea, leukopenia (mostly neutropenia) and rash. The most commonly reported (≥ 5%) Grade 3 or worse adverse drug reactions were infection, leukopenia, neutropenia, anaemia, second primary malignancy, and thrombocytopenia. Dose reductions due to adverse events were reported in 5.9% of patients (most frequently due to hepatitis B reactivation, sepsis, or diarrhoea). Discontinuation due to adverse events were reported in 14.6% of patients (most frequently due to pneumonia, thrombocytopenia, or diarrhoea).
Calquence in combination regimens. The safety profile of acalabrutinib when used in combination with other therapies is described specifically for each combination regimen under the relevant clinical trial heading below.
Clinical trials experience. As clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trials of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice.
Safety data from clinical trials in mantle cell lymphoma (MCL). ECHO (acalabrutinib+BR in previously untreated MCL not eligible for transplant). The safety of Calquence in combination with bendamustine and rituximab was evaluated in 297 patients with previously untreated MCL in ECHO (see Section 5.1 Pharmacodynamic Properties, Clinical trials). The trial enrolled patients at least 65 years of age with no intention for transplant, with total bilirubin ≤ 1.5 x ULN, AST or ALT ≤ 2.5 x ULN, and estimated creatinine clearance of > 50 mL/min.
The median duration of treatment with Calquence was 28.6 (range: 0.1 to 80) months. A total of 171 (58%) patients were treated with Calquence for ˃ 24 months and 122 (41%) patients were treated for ˃ 36 months.
Serious adverse reactions occurred in 69% of patients who received Calquence. Serious adverse reactions reported in ≥ 2% of patients were COVID-19 (20%), pneumonia (9%), second primary malignancy (7%), pyrexia (5.7%), rash (3.4%), febrile neutropenia (3.4%), atrial fibrillation (3.0%), sepsis (2.7%) and anaemia (2.4%).
Fatal adverse reactions that occurred within 30 days of the last study treatment were reported in 12% of patients who received Calquence plus BR including COVID-19 (6%), pneumonia (1.0%), second primary malignancy (0.7%), sepsis (0.3%), and pneumonitis (0.3%).
Dose interruption, reduction, and discontinuation due to any adverse reaction were reported in 74%, 10% and 43% of patients, respectively. Adverse reactions that resulted in dosage modification in > 10% included infections, cytopenias, rashes, and gastrointestinal toxicity. Adverse reactions which resulted in permanent discontinuation of Calquence in ≥ 4% of patients included COVID-19 and neutropenia.
Table 5 and Table 6 present summaries of the most common adverse reactions and laboratory abnormalities observed in patients with MCL who received Calquence in the ECHO study.
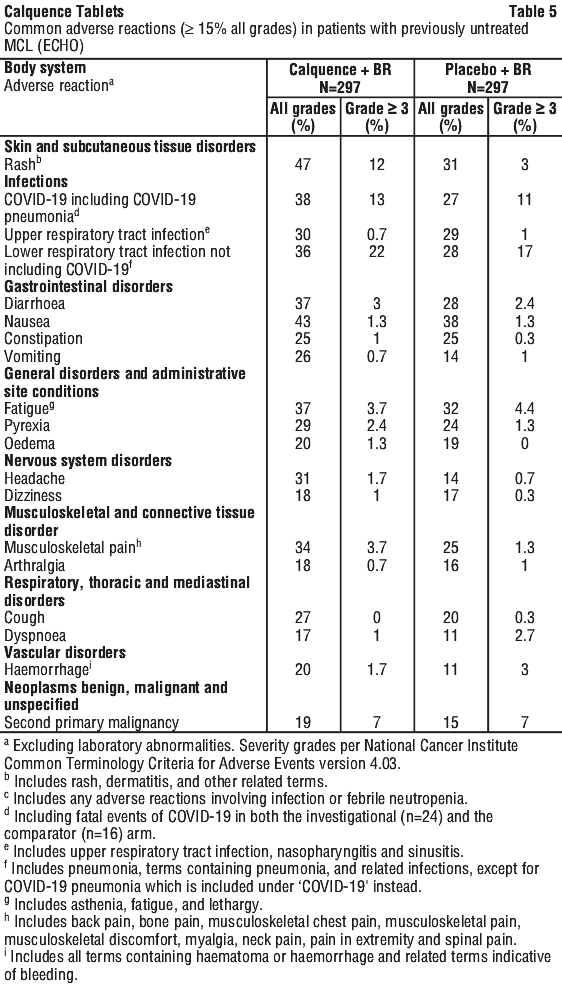
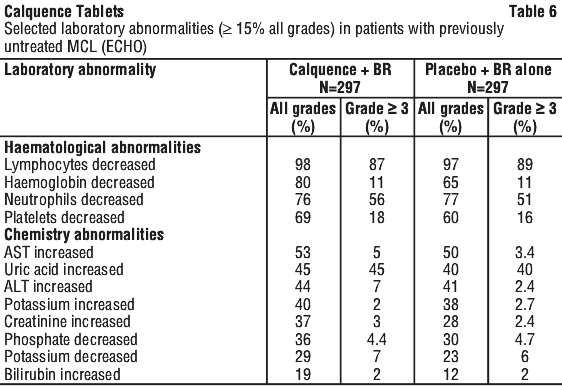
The most common adverse reactions (≥ 20%) of any grade were anaemia, thrombocytopenia, headache, neutropenia, diarrhoea, fatigue, myalgia, and bruising. Grade 1 severity for the non-haematologic, most common events were as follows: headache (25%), diarrhoea (16%), fatigue (20%), myalgia (15%), and bruising (19%). The most common Grade ≥ 3 non-haematological adverse reaction (reported in at least 2% of patients) was diarrhoea.
Dose reductions and discontinuation due to any adverse reaction were reported in 1.6% and 6.5% of patients, respectively.
Table 7 and Table 8 present the frequency category of adverse reactions observed in patients with MCL treated with Calquence.
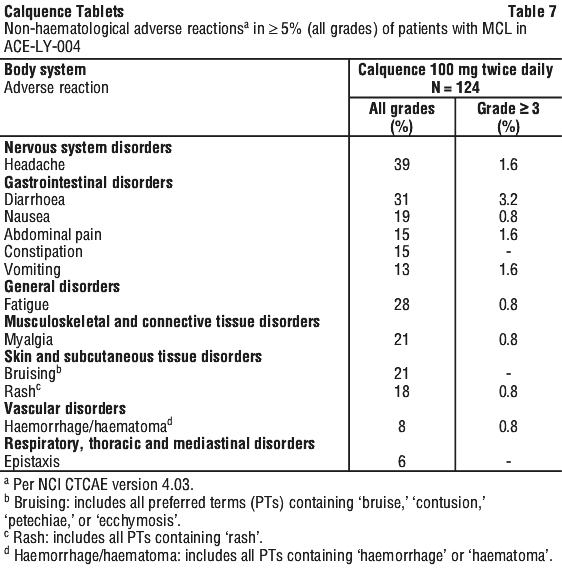
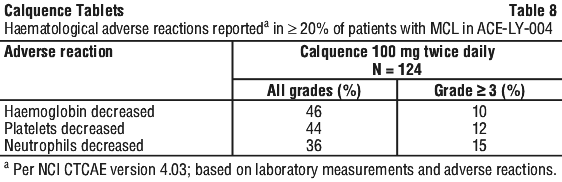
Safety data from clinical trials in chronic lymphocytic leukaemia (CLL). The safety data described below reflect exposure to Calquence (100 mg twice daily) in two randomised controlled clinical trials (AMPLIFY, ELEVATE-TN and ASCEND) in patients with CLL (see Section 5.1 Pharmacodynamic Properties, Clinical trials).
The most common adverse reactions (≥ 20%) of any grade were infection, neutropenia, anaemia, thrombocytopenia, headache, diarrhoea, musculoskeletal pain, bruising, and nausea. The most commonly reported Grade ≥ 3 adverse reactions were infection, neutropenia, and anaemia.
AMPLIFY (acalabrutinib+venetoclax+/-obinutuzumab in previously untreated CLL). The safety of Calquence in patients with previously untreated CLL has been studied in a 3-arm, randomised, multicentre, open-label Phase 3 trial (AMPLIFY). Calquence plus venetoclax, Calquence plus venetoclax and obinutuzumab, or Investigator's choice of chemoimmunotherapy, either FCR (fludarabine plus cyclophosphamide plus rituximab) or BR (bendamustine plus rituximab) were administered to 867 patients with previously untreated CLL (see Section 5.1 Pharmacodynamic Properties, Clinical trials). See Table 10.
The adverse reactions described in Table 9 reflect exposure to Calquence in the Calquence plus venetoclax and Calquence plus venetoclax with obinutuzumab arms with a median duration of exposure of 12.9 months in patients with previously untreated CLL. The tabulated adverse reactions were reported in ≥ 5% of patients in either Calquence-containing treatment arm and are considered at least possibly related to study drug. See Table 9.
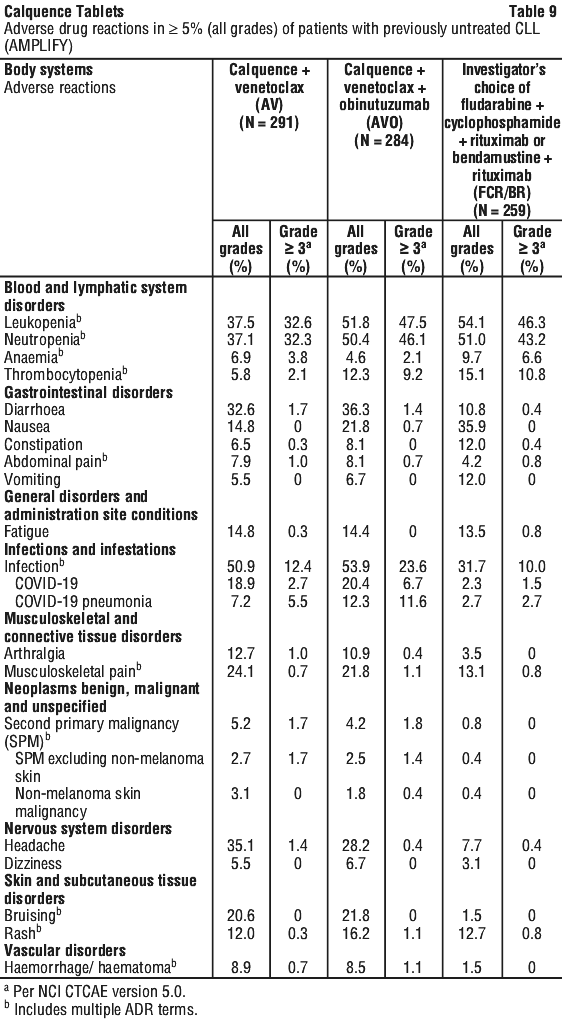
Cardiac disorders: atrial fibrillation/flutter.*
General disorders and administration site conditions: asthenia.
Metabolism and nutrition disorders: tumour lysis syndrome.
Respiratory, thoracic and mediastinal disorders: epistaxis.
* Includes multiple ADR terms.
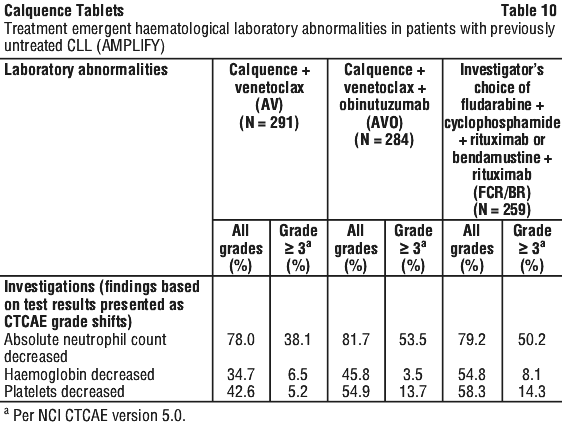
Of the 284 patients treated with Calquence in combination with venetoclax and obinutuzumab, severe (Grade ≥ 3) infections were reported in 23.6% of the patients (most frequently reported COVID-19 or COVID-19 pneumonia). Fatal infections occurred in 5.6% of patients (most frequently reported COVID-19 or COVID-19 pneumonia).
Deaths from COVID-19 in the full analysis set during treatment emergent as well as follow-up periods were reported for 10 (3.4%) patients in the AV arm, 25 (8.7%) in the AVO arm and 21 (7.2%) in the FCR/BR arm.
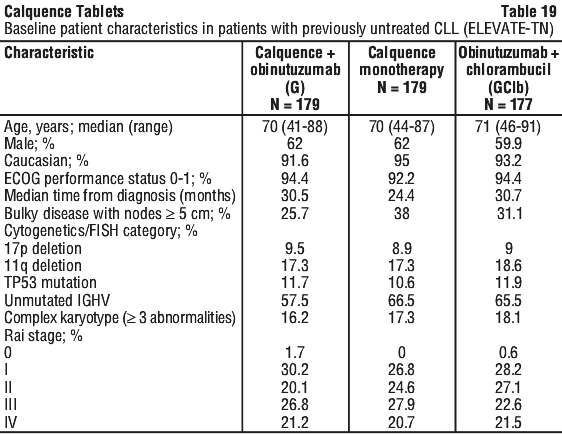
ELEVATE-TN (acalabrutinib+/-obinutuzumab vs chlorambucil+obinutuzumab in previously untreated CLL). The safety of Calquence plus obinutuzumab (Calquence+G), Calquence monotherapy, and obinutuzumab plus chlorambucil (GClb) was evaluated in a randomised, multicentre, open-label, Phase 3 study, in 526 patients with previously untreated CLL. Details of the study treatment are described in Section 5.1 Pharmacodynamic Properties, Clinical trials.
In the Calquence+G arm, adverse events led to regimen discontinuation in 11% of patients and a dose reduction of Calquence in 8% of patients. In the Calquence monotherapy arm, adverse events led to discontinuation in 9% and dose reduction in 3% of patients. In the GClb arm, adverse events led to regimen discontinuation in 14% of patients and a dose reduction of chlorambucil in 28% of patients. There were no dose reductions for obinutuzumab.
The adverse reactions described in Table 11 and Table 12 reflect exposure to Calquence in the Calquence+G and Calquence monotherapy arms with a median duration of exposure of 27.7 months in patients with previously untreated CLL. The median duration of exposure in the GClb arm was 5.6 months.
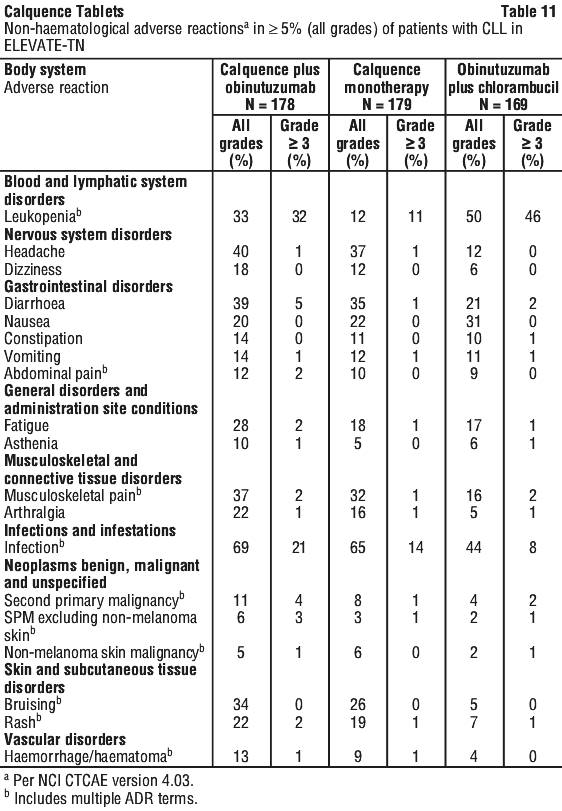
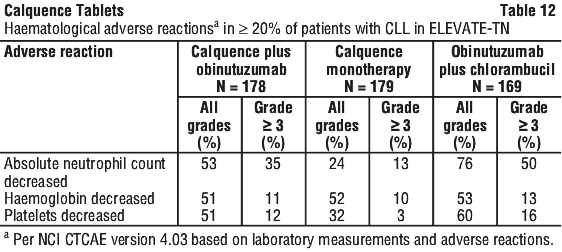
Atrial fibrillation/atrial flutter in ELEVATE-TN. Atrial fibrillation/atrial flutter was reported in patients treated with Calquence+G and Calquence monotherapy with an incidence of 3% and 4%, respectively, including 1% with ≥ Grade 3 atrial fibrillation/atrial flutter in the Calquence+G arm. No patients experienced ≥ Grade 3 atrial fibrillation/atrial flutter in the Calquence monotherapy arm.
Infusion related reaction in ELEVATE-TN. Infusion related reaction was reported in 14% and 40% of patients in the Calquence+G and GClb arms, respectively.
ASCEND (acalabrutinib monotherapy in relapsed/refractory CLL after at least one prior therapy). The safety of Calquence versus investigator's choice of either idelalisib plus rituximab or bendamustine plus rituximab was evaluated in a randomised, multicentre, open-label, Phase 3 study, in 307 patients with relapsed or refractory CLL. Details of the study treatment are described in Section 5.1 Pharmacodynamic Properties, Clinical trials.
In the Calquence arm, adverse events led to discontinuation in 10% and dose reduction in 3% of patients. In patients receiving idelalisib plus rituximab, adverse events led to regimen discontinuation in 9% of patients and a dose reduction of idelalisib in 24%. In patients receiving bendamustine plus rituximab, adverse events led to regimen discontinuation in 9% of patients and a dose reduction of bendamustine in 14% of patients. There were no dose reductions of rituximab.
The adverse reactions described in Table 13 and Table 14 reflect exposure to Calquence with a median duration of 15.7 months, exposure to idelalisib with a median duration of 11.5 months, exposure to rituximab with a median duration of 5.5 months, and exposure to bendamustine and a median duration of 5.6 months in patients with relapsed or refractory CLL.
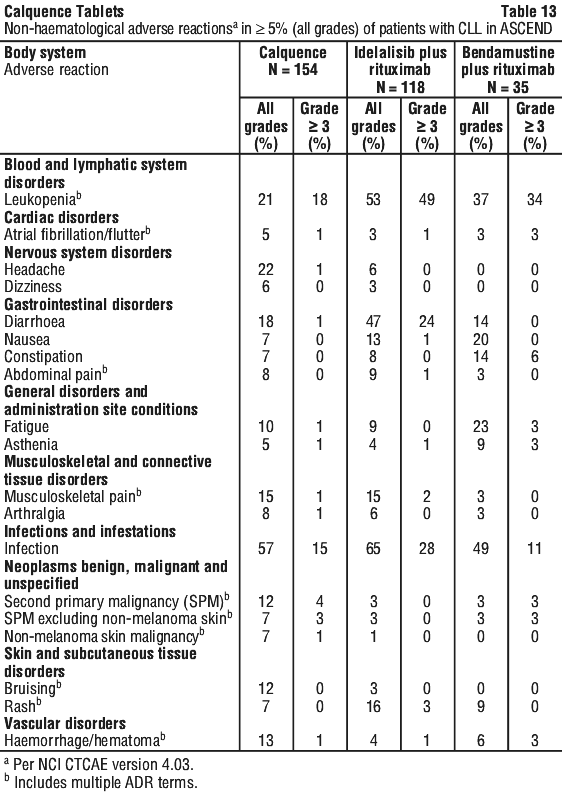
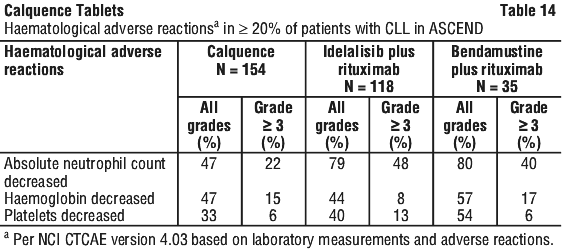
Post-marketing experience. The following adverse reactions have been identified during post-approval use of Calquence. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Vascular disorders. Hypertension.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
There is no specific treatment for acalabrutinib overdose and symptoms of overdose have not been established. In the event of an overdose, patients must be closely monitored for signs or symptoms of adverse reactions and appropriate symptomatic treatment instituted.
For information on the management of overdose, contact the Poison Information Centre on 131126 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Acalabrutinib is a small-molecule inhibitor of Bruton's tyrosine kinase (BTK). Acalabrutinib and its active metabolite, ACP-5862, form a covalent bond with a cysteine residue in the BTK active site, leading to inhibition of BTK enzymatic activity. BTK is a signalling molecule of the B-cell antigen receptor (BCR) and cytokine receptor pathways. In B-cells, BTK signalling results in activation of pathways necessary for B-cell proliferation, trafficking, chemotaxis, and adhesion. In nonclinical studies, acalabrutinib inhibited BTK-mediated activation of downstream signalling proteins CD86 and CD69 and inhibited malignant B-cell proliferation and tumour growth in mouse xenograft models.
Pharmacodynamics. In patients with B-cell malignancies dosed with 100 mg twice daily, median steady state BTK occupancy of ≥ 95% in peripheral blood was maintained over 12 hours, resulting in inactivation of BTK throughout the recommended dosing interval.
Cardiac electrophysiology. The effect of acalabrutinib on the QTc interval was evaluated in a randomised, double-blind, double-dummy, placebo- and positive-controlled, 4-way crossover thorough QTc study in 48 healthy adult subjects. Administration of a single dose of acalabrutinib that is the 4-fold maximum recommended single dose did not prolong the QTc interval to any clinically relevant extent (i.e. ≥ 10 ms).
Clinical trials. Mantle cell lymphoma (MCL). Patients with previously untreated MCL - ECHO. The safety and efficacy of Calquence in patients with previously untreated MCL was evaluated in ECHO, a randomised, double-blind, placebo controlled, multicentre phase 3 study. ECHO enrolled 598 patients who were at least 65 years of age and had no intention to undergo autologous haematopoietic stem cell transplant. The study excluded patients with total bilirubin > 1.5 x upper limit of normal (ULN), AST or ALT > 2.5 x ULN, or estimated creatinine clearance of ≤ 50 mL/min. Randomisation was stratified by geographic region and simplified Mantle Cell Lymphoma International Prognostic Index (MIPI) score. The study enrolled patients during the COVID-19 pandemic.
Patients were randomised in a 1:1 ratio to receive either Calquence plus bendamustine and rituximab (Calquence + BR) or placebo + BR. Treatment in both arms was continued until disease progression or unacceptable toxicity, and was administered in 28-day cycles as follows:
Induction (maximum 6 cycles):
Calquence 100 mg (or matching placebo) orally twice daily, every day of the cycle.
Bendamustine 90 mg/m2 administered IV over 30 minutes on Days 1 and 2 of each cycle.
Rituximab 375 mg/m2 administered IV on Day 1 of each cycle.
Maintenance - for patients remaining in response (PR or CR) after induction:
Calquence 100 mg (or matching placebo) orally twice daily, every day of the cycle
Rituximab 375 mg/m2 administered IV on Day 1 of every other cycle; ceased after a maximum of 12 additional doses of rituximab (up to Cycle 30).
After discontinuation of rituximab, patients continued Calquence 100 mg (or matching placebo) as monotherapy, taken orally twice daily until disease progression or unacceptable toxicity.
Crossover to Calquence monotherapy was permitted for patients in the placebo plus BR arm at disease progression.
The median age was 71 years (range 65-86), 71% were male, 78% were Caucasian, and 93% had an ECOG performance status of 0-1. The simplified MIPI score was low (0-3) in 33%, intermediate (4-5) in 43% and high (6-11) in 24% of patients. A total of 38% of patients had tumour bulk ≥ 5 cm and 86% had Ann Arbor stage IV disease. Most (80%) had classic MCL histology, whilst 7.7% had blastoid and 5.5% had pleomorphic forms. A total of 48% patients had Ki-67 score of ≥ 30%. The baseline characteristics were similar between both treatment arms.
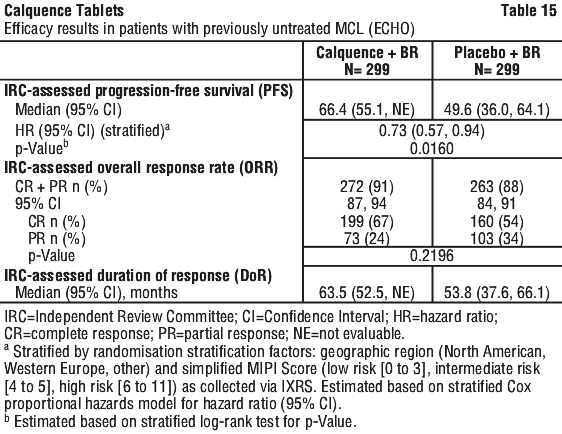
The primary endpoint was progression-free survival (PFS) as assessed by an Independent Review Committee (IRC) per Lugano Classification for NHL in subjects with previously untreated MCL. Additional efficacy endpoints were Investigator-assessed (INV) PFS, INV and IRC assessed overall response rate (ORR), IRC and INV assessed duration of response (DOR) and overall survival (OS).
Efficacy results are presented in Table 15 and Figure 1. At this prespecified interim analysis, the median follow-up for PFS was 49.8 months in both arms. Median OS had not been reached in any arm with a total of 203 deaths: 97 (32.4%) in the Calquence + BR arm, 106 (35.5%) in the Placebo + BR arm.
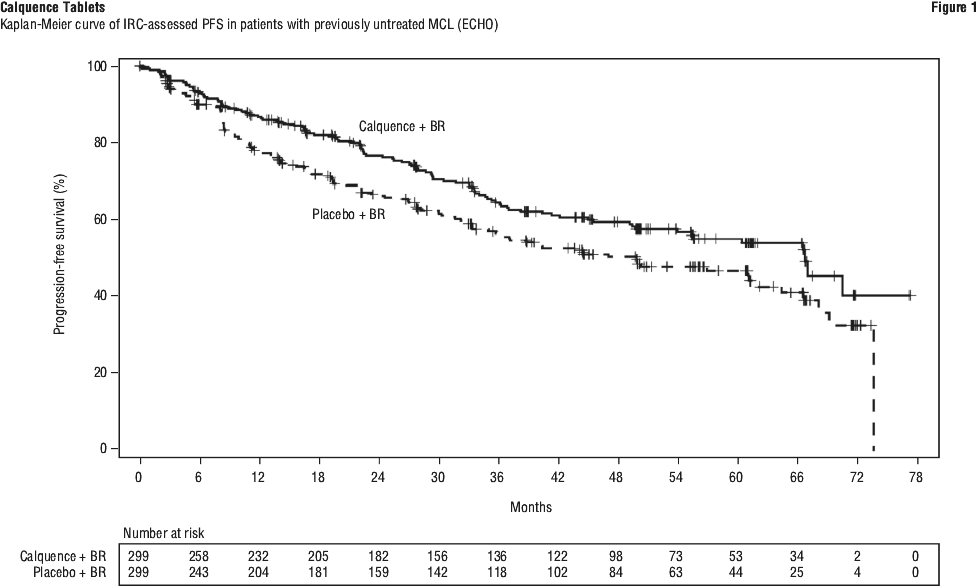
The median age was 68 (range 42 to 90) years, 80% were male and 74% were Caucasian. At baseline, 93% of patients had an ECOG performance status of 0 or 1. The median time since diagnosis was 46 months and the median number of prior treatments was 2 (range 1 to 5), including 17.7% with prior stem cell transplant. The most common prior regimens were CHOP-based (52%) and ARA-C (34%). At baseline, 37% of patients had at least one tumour with a longest diameter ≥ 5 cm, 73% had extra nodal involvement including 51% with bone marrow involvement. The simplified MIPI score (which includes age, ECOG score, and baseline lactate dehydrogenase and white cell count) was intermediate in 44% and high in 17% of patients. The median dose intensity was 98.5%.
Efficacy results are presented in Table 16 for the primary analysis, and at a 54-month final analysis (median follow-up 38.1 months).
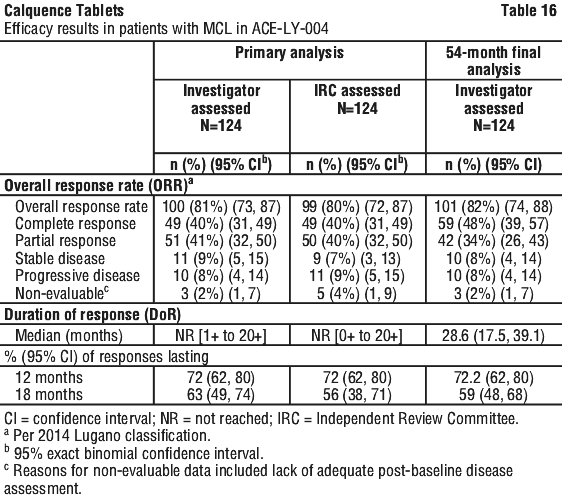
Chronic lymphocytic leukaemia (CLL). Patients with previously untreated CLL - fixed duration therapy - AMPLIFY. The safety and efficacy of Calquence in combination with venetoclax with or without obinutuzumab in previously untreated CLL was evaluated in a randomised, multicentre, open-label Phase 3 study (AMPLIFY) of 867 patients. Patients received Calquence plus venetoclax, Calquence plus venetoclax and obinutuzumab, or Investigator's choice of chemoimmunotherapy, either FCR (fludarabine plus cyclophosphamide plus rituximab) or BR (bendamustine plus rituximab).
Patients were randomised in a 1:1:1 ratio into 3 arms to receive:
Calquence plus venetoclax (AV): Calquence 100 mg was administered twice daily starting on Cycle 1 Day 1 for a total of 14 cycles or until disease progression or unacceptable toxicity. On Cycle 3 Day 1 patients started the venetoclax 5 week dose titration schedule, starting at 20 mg and increasing weekly to 50 mg, 100 mg, 200 mg and finally 400 mg once daily. Venetoclax was administered for a total of 12 cycles. Each cycle was 28 days.
Calquence plus venetoclax plus obinutuzumab (AVO): Calquence 100 mg was administered twice daily starting on Cycle 1 Day 1 for a total of 14 cycles or until disease progression or unacceptable toxicity. On Cycle 3 Day 1 patients started the venetoclax 5 week dose titration schedule, starting at 20 mg and increasing weekly to 50 mg, 100 mg, 200 mg and finally 400 mg once daily. Venetoclax was administered for a total of 12 cycles. Obinutuzumab 1000 mg was administered on Days 1 and 2 (100 mg on Day 1 and 900 mg on Day 2), 8 and 15 of Cycle 2 followed by 1000 mg on Day 1 of Cycles 3-7. Each cycle was 28 days.
Investigator's choice of chemoimmunotherapy (FCR/BR):
Fludarabine plus cyclophosphamide plus rituximab (FCR): Fludarabine (25 mg/m2) and cyclophosphamide (250 mg/m2) were administered on Days 1 3 up to a maximum of 6 cycles. Rituximab was administered at a dose of 375 mg/m2 on Day 1 Cycle 1 and 500 mg/m2 on Day 1 of Cycles 2 up to 6. Each cycle was 28 days.
Bendamustine plus rituximab (BR): Bendamustine 90 mg/m2 was administered on Days 1 and 2 up to maximum of 6 cycles. Rituximab was administered at a dose of 375 mg/m2 on Day 1 Cycle 1 and 500 mg/m2 on Day 1 of Cycles 2 up to 6. Each cycle was 28 days.
Patients were stratified by age (> 65 years or ≤ 65 years), IGHV mutational status (mutated versus unmutated), Rai stage (high risk [≥ 3] versus non-high risk) and geographic region (North America and Western Europe versus other). Table 17 summarises the baseline demographics and disease characteristics of the study population.
AMPLIFY included patients previously untreated for CLL without del(17p) or TP53 mutation that were 18 years of age and older. The trial also allowed patients to receive antithrombotic agents other than warfarin or equivalent vitamin K antagonists. The study enrolled patients during the COVID-19 pandemic.
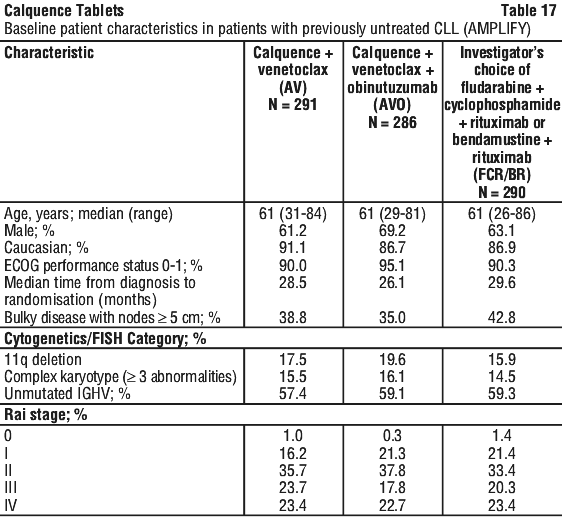
With a median follow-up of 41.3 months, IRC-assessed PFS indicated a 35% statistically significant reduction in risk of disease progression or death in patients treated with AV compared to FCR/BR. The secondary endpoint median for Investigator-assessed PFS was not reached.
With a median follow-up of 42.0 months, IRC-assessed PFS indicated a 58% statistically significant reduction in risk of disease progression or death in patients treated with AVO compared to FCR/BR. The secondary endpoint median for Investigator-assessed PFS was not reached.
Efficacy results are presented in Table 18. The Kaplan-Meier curve for IRC-PFS is shown in Figure 2.
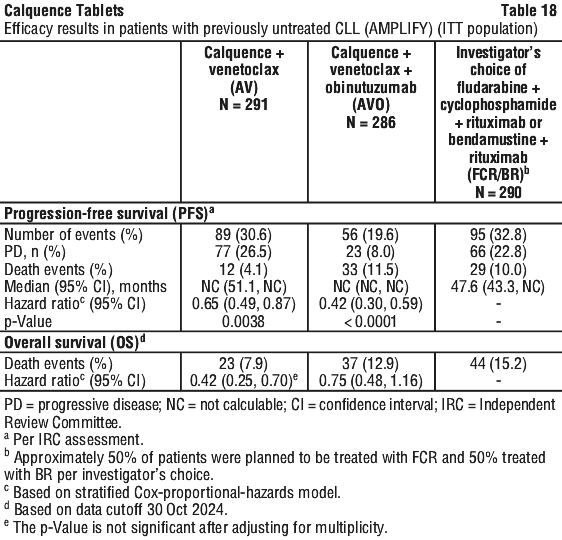
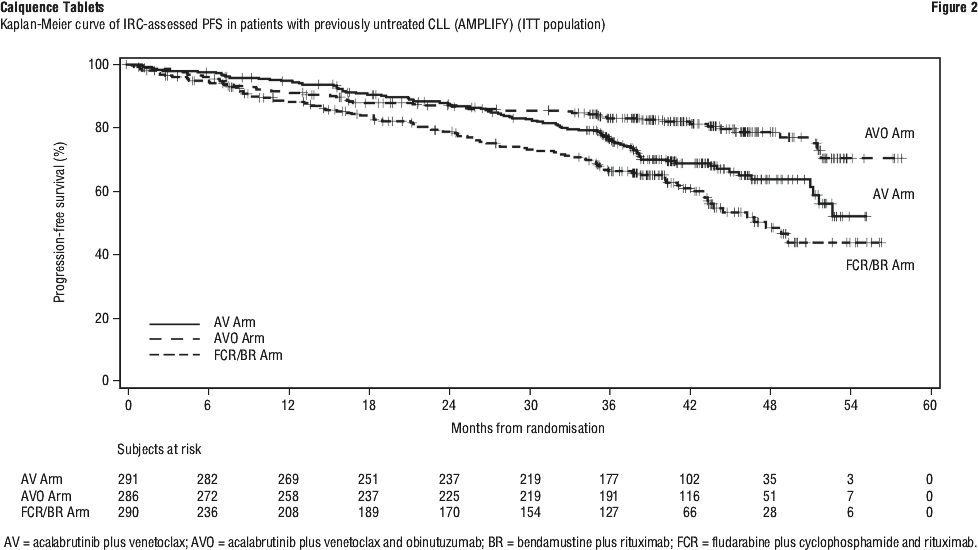
As shown in Figure 3 at the time of the interim analysis (approximately 10% OS maturity), a total of 18 (6.2%) and 42 deaths (14.5%) were observed in Arm A (AV) and C (FCR/BR), respectively. OS HR was 0.33 (95% CI: 0.18-0.56; nominal p < 0.0001). Additionally, at approximately 14% OS maturity, a total of 37 (12.9%) deaths were observed in Arm B (AVO). OS HR compared to Arm C was 0.76 (95% CI: 0.49-1.18, nominal p = 0.2224).
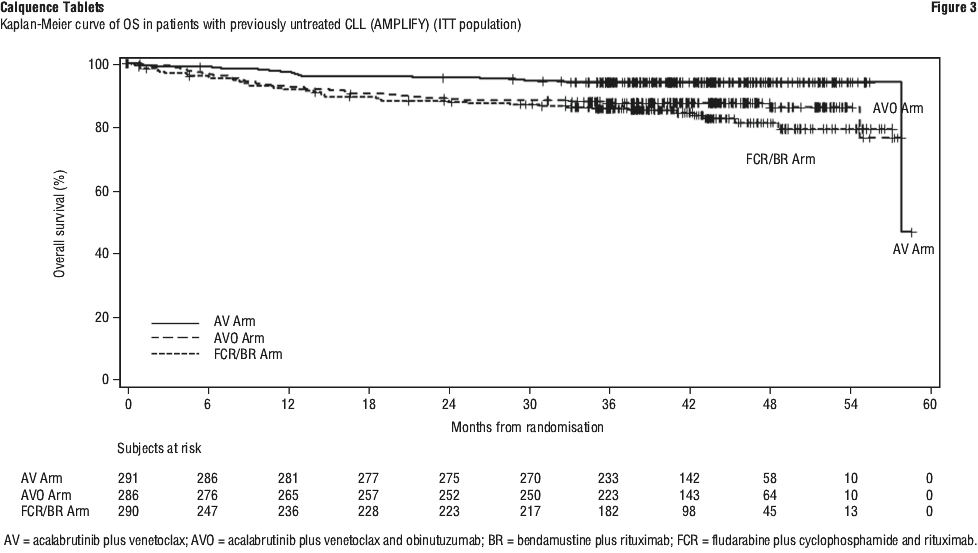
Patients were randomised in a 1:1:1 ratio into 3 arms to receive:
Calquence plus obinutuzumab (Calquence+G): Calquence 100 mg was administered twice daily starting on Cycle 1 Day 1 until disease progression or unacceptable toxicity. Obinutuzumab was administered starting on Cycle 2 Day 1 for a maximum of 6 treatment cycles. Obinutuzumab 1000 mg was administered on Days 1 and 2 (100 mg on Day 1 and 900 mg on Day 2), 8 and 15 of Cycle 2 followed by 1000 mg on Day 1 of Cycles 3 up to 7. Each cycle was 28 days.
Calquence monotherapy: Calquence 100 mg was administered twice daily until disease progression or unacceptable toxicity.
Obinutuzumab plus chlorambucil (GClb): obinutuzumab and chlorambucil were administered for a maximum of 6 treatment cycles. Obinutuzumab 1000 mg was administered on Days 1 and 2 (100 mg on Day 1 and 900 mg on Day 2), 8 and 15 of Cycle 1 followed by 1000 mg on Day 1 of Cycles 2 up to 6. Chlorambucil 0.5 mg/kg was administered on Days 1 and 15 of Cycles 1 up to 6. Each cycle was 28 days.
Patients were stratified by 17p deletion mutation status (presence versus absence), ECOG performance status (0 or 1 versus 2) and geographic region (North America and Western Europe versus Other). After confirmed disease progression, 45 patients randomised on the GClb arm crossed over to Calquence monotherapy. Table 19 summarises the baseline demographics and disease characteristics of the study population.
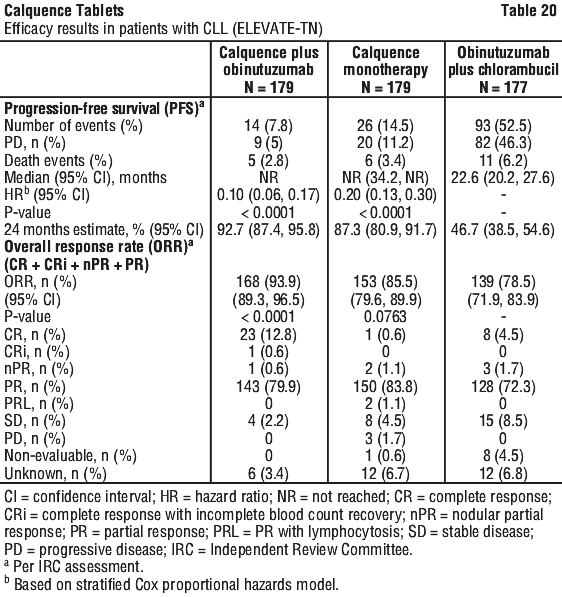
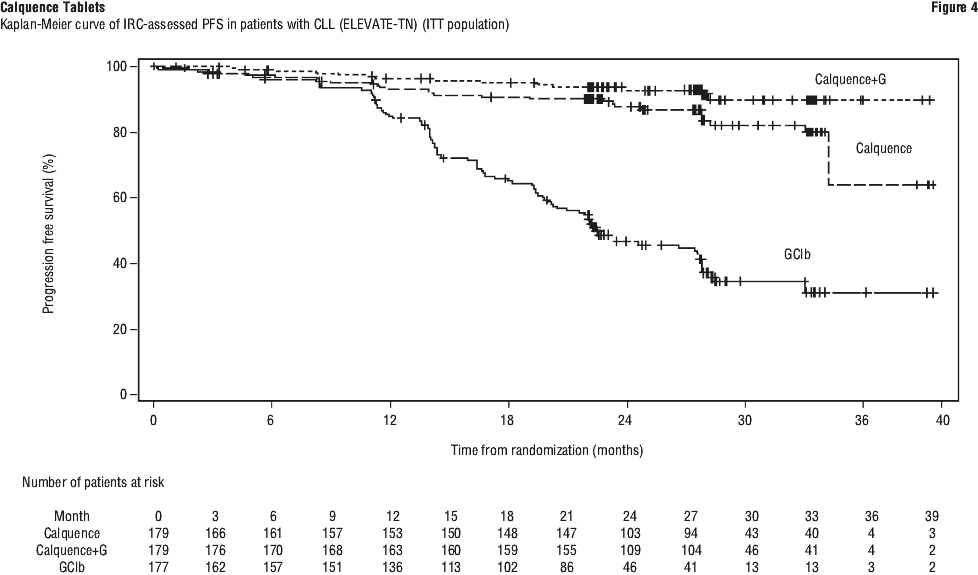
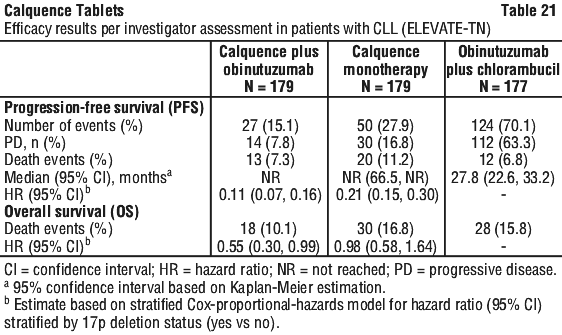
With long term data, the median follow-up was 58.2 months for Calquence+G arm, 58.1 months for Calquence arm and 58.2 months for the GClb arm. The median investigator-assessed PFS for Calquence+G and Calquence monotherapy was not reached; and was 27.8 months in GClb arm. At the time of most recent data cut off, a total of 72 patients (40.7%) originally randomised to the GClb arm crossed over to Calquence monotherapy. The median overall survival had not been reached in any arm with a total of 76 deaths: 18 (10.1%) in the Calquence+G arm, 30 (16.8%) in the Calquence monotherapy arm, and 28 (15.8%) in the GClb arm. The time to next treatment was prolonged for Calquence+G arm (HR=0.14 [95% CI: 0.09, 0.21]) and Calquence only arm (HR=0.27 [95% CI: 0.19, 0.38]) compared to GClb arm. See Table 21 and Figure 5.
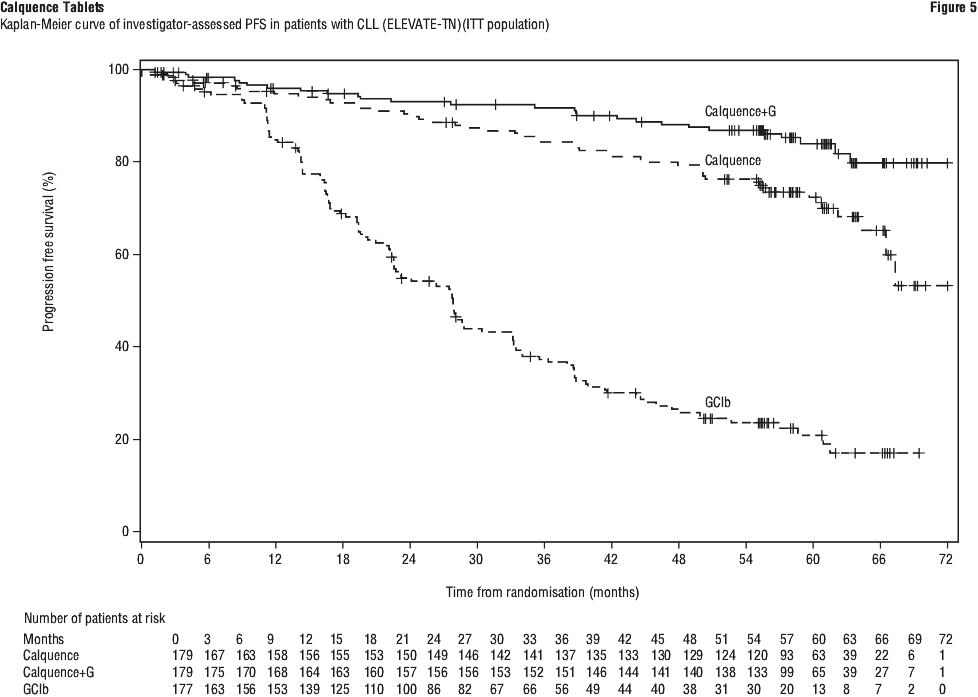
Patients were randomised 1:1 to receive either:
Calquence 100 mg twice daily until disease progression or unacceptable toxicity, or
Investigator's choice: idelalisib 150 mg twice daily until disease progression or unacceptable toxicity in combination with ≤ 8 infusions of rituximab (375 mg/m2/500 mg/m2) on Day 1 of each 28-day cycle for up to 6 cycles.
Bendamustine 70 mg/m2 (Day 1 and 2 of each 28-day cycle) in combination with rituximab (375 mg/m2/500 mg/m2) on Day 1 of each 28-day cycle for up to 6 cycles.
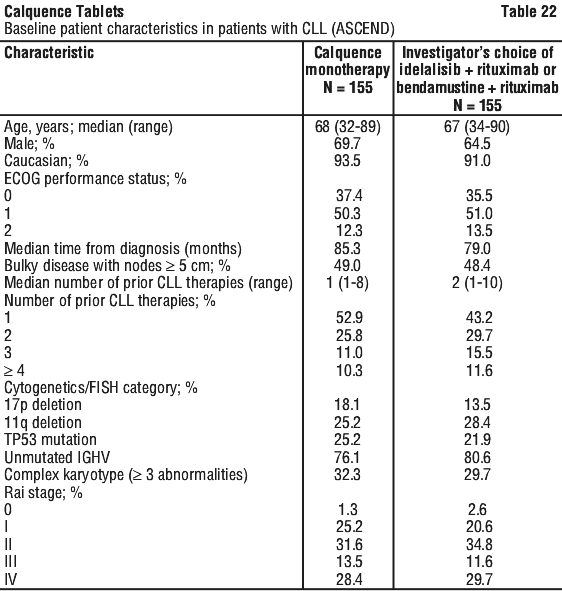
Patients were stratified by 17p deletion mutation status (presence versus absence), ECOG performance status (0 or 1 versus 2) and number of prior therapies (1 to 3 versus ≥ 4). After confirmed disease progression, 35 patients randomised on investigator's choice of either idelalisib plus rituximab or bendamustine plus rituximab crossed over to Calquence. Table 22 summarises the baseline demographics and disease characteristics of the study population.

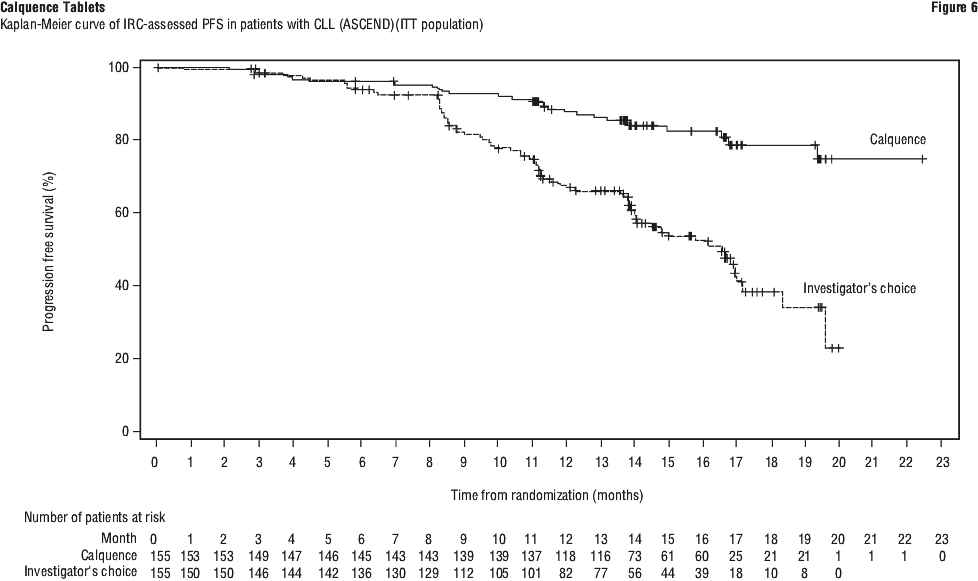
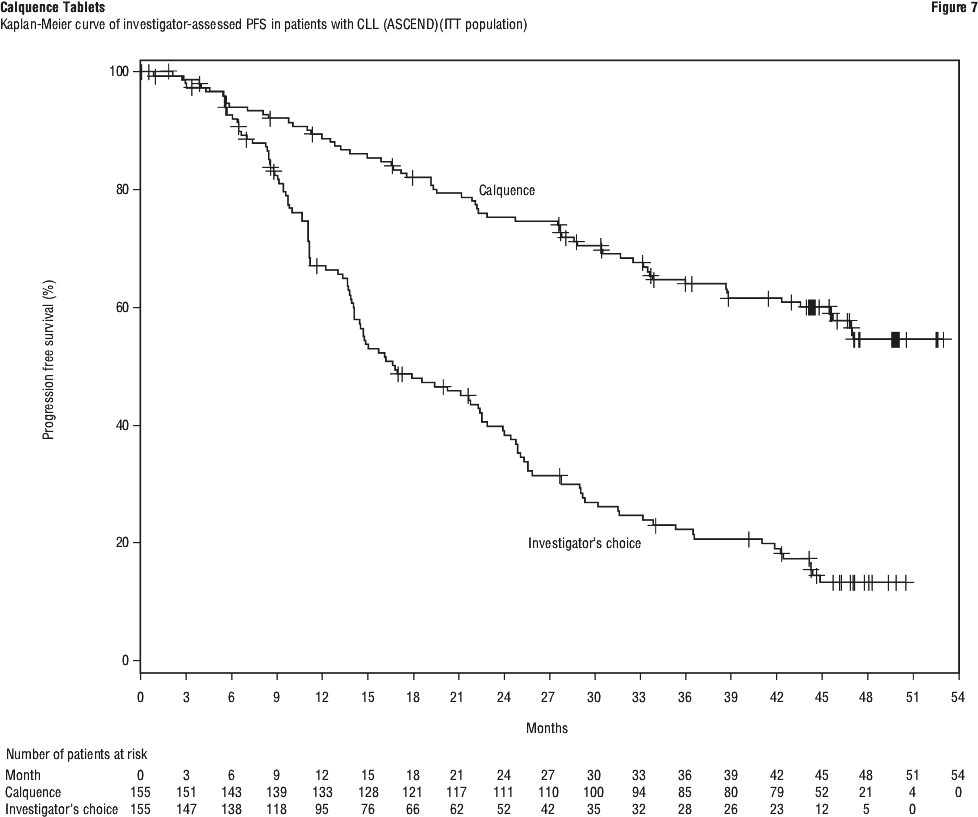
At the time of final analysis, median overall survival had not been reached in any arm with a total of 95 deaths: 41 (26.5%) in the Calquence monotherapy arm and 54 (34.8%) in the IR/BR arm. See Table 24 and Figure 7.
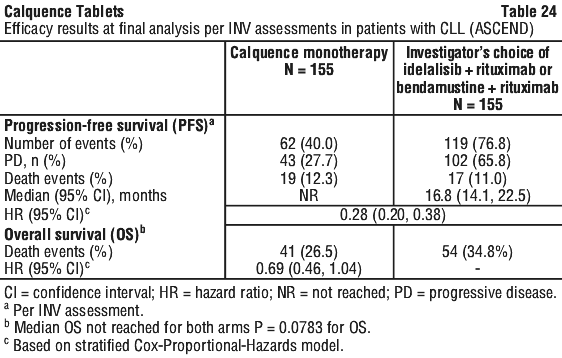
5.2 Pharmacokinetic Properties
The pharmacokinetics (PK) of acalabrutinib and its active metabolite, ACP-5862 were studied in healthy subjects and patients with B-cell malignancies. Acalabrutinib exhibits dose-proportionality, and both acalabrutinib and ACP-5862 exhibit almost linear PK across a dose range of 75 to 250 mg (0.75 to 2.5 times the approved recommended single dose). Population PK modelling suggests that the PK of acalabrutinib and ACP-5862 does not differ significantly in patients with different B-cell malignancies. At the recommended dose of 100 mg twice daily in patients with B-cell malignancies (including MCL and CLL), the geometric mean steady state daily area under the plasma drug concentration over time curve (AUC24h) and maximum plasma concentration (Cmax) of acalabrutinib were 1893 nanogram.h/mL and 466 nanogram/mL, respectively, and for ACP-5862 were 4091 nanogram.h/mL and 420 nanogram/mL, respectively.
Calquence tablets and Calquence capsules have been demonstrated to be bioequivalent. Geometric mean PK exposures (Cmax and AUClast or AUCinf) of acalabrutinib and ACP-5862 were similar (< 4% difference) between the tablet and capsule, with the 90% confidence intervals for geometric mean ratios within the pre-defined bioequivalence margin of 80% and 125%.
Absorption. The median (min-max) time to peak plasma concentrations (Tmax) was 0.5 (0.2, 3.0) hours for acalabrutinib, and 0.75 (0.5, 4.0) hours for ACP-5862, following administration of acalabrutinib tablet. The absolute bioavailability of Calquence was 25% following oral administration of acalabrutinib capsule.
Distribution. Reversible binding to human plasma protein was 97.5% for acalabrutinib and 98.6% for ACP-5862. The in vitro mean blood-to-plasma ratio was 0.8 for acalabrutinib and 0.7 for ACP-5862. The mean steady state volume of distribution (Vss) was approximately 34 L for acalabrutinib.
Metabolism. In vitro, acalabrutinib is predominantly metabolised by CYP3A enzymes, and to a minor extent by glutathione conjugation and amide hydrolysis. ACP-5862 was identified as the major metabolite in plasma with a geometric mean exposure (AUC) that was approximately 2- to 3-fold higher than the exposure of acalabrutinib. ACP-5862 is approximately 50% less potent than acalabrutinib with regard to BTK inhibition.
Acalabrutinib may inhibit intestinal BCRP substrates (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions), while ACP-5862 may inhibit MATE1 (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions) at clinically relevant concentrations. Acalabrutinib does not inhibit MATE1, while ACP-5862 does not inhibit BCRP at clinically relevant concentrations.
Excretion. Following a single oral dose of 100 mg acalabrutinib tablet, the median terminal elimination half-life (t1/2) of acalabrutinib was 1.3 (range: 0.8 to 9.0) hours. The median t1/2 of the active metabolite, ACP-5862, was 7.3 hours (range: 2.5 to 10.1) hours.
The mean apparent oral clearance (CL/F) was 70 L/hr for acalabrutinib and 13 L/hr for ACP-5862, with similar PK between patients and healthy subjects, based on population PK analysis.
Following administration of a single 100 mg radiolabelled [14C]-acalabrutinib dose in healthy subjects, 84% of the dose was recovered in the faeces and 12% of the dose was recovered in the urine, with less than 2% of the dose excreted as unchanged acalabrutinib in urine and faeces.
Specific populations. Age, race, and body weight. Age (32 to 90 years), sex, race (Caucasian, African American), and body weight (40 to 149 kg) did not have clinically meaningful effects on the PK of acalabrutinib and its active metabolite, ACP-5862, based on population PK analysis.
Renal impairment. Acalabrutinib undergoes minimal renal elimination. Based on population PK analysis, no clinically relevant PK difference was observed in 543 patients with mild or moderate renal impairment (eGFR ≥ 30 mL/min/1.73 m2, as estimated by MDRD (modification of diet in renal disease equation)). Acalabrutinib PK has not been evaluated in patients with severe renal impairment (eGFR < 29 mL/min/1.73 m2, MDRD) or renal impairment requiring dialysis.
Hepatic impairment. Acalabrutinib is metabolised in the liver. In hepatic impairment studies, compared to subjects with normal liver function (n = 6), acalabrutinib exposure (AUC) was increased by 1.9-fold, 1.5-fold, and 5.3-fold in subjects with mild (n = 6) (Child-Pugh A), moderate (n = 6) (Child-Pugh B) and severe (n = 8) (Child-Pugh C) hepatic impairment, respectively. Based on a population PK analysis, no clinically relevant PK difference was observed in subjects with mild (n = 79) or moderate (n = 6) hepatic impairment (total bilirubin between 1.5 to 3 times the upper limit of normal [ULN] and any AST) relative to subjects with normal (n = 651) hepatic function (total bilirubin and AST within ULN).
Drug interaction studies. Effect of CYP3A inhibitors on acalabrutinib. Co-administration with a strong CYP3A inhibitor (200 mg itraconazole once daily for 5 days) increased the acalabrutinib Cmax by 3.9-fold and AUC by 5.1-fold in healthy subjects.
Physiologically based pharmacokinetic (PBPK) simulations with acalabrutinib and moderate CYP3A inhibitors (erythromycin, fluconazole, diltiazem) showed that co-administration increased acalabrutinib Cmax and AUC increased by 2- to almost 3-fold (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Effect of CYP3A inducers on acalabrutinib. Co-administration with a strong CYP3A inducer (600 mg rifampin once daily for 9 days) decreased acalabrutinib Cmax by 68% and AUC by 77% in healthy subjects (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Gastric acid reducing medicines. Co-administration of acalabrutinib tablet with a proton pump inhibitor (20 mg rabeprazole, twice daily for 3 days) increased AUC by 17% (up to 31% increase, based on upper limit of 90% confidence interval) and decreased Cmax by 24% (up to 45% decrease, based on lower limit of 90% confidence interval), with a delay in Tmax (up to 1 hour, approximately).
5.3 Preclinical Safety Data
Genotoxicity. Acalabrutinib was not mutagenic in an in vitro bacterial reverse mutation (AMES) assay or clastogenic in an in vitro human lymphocyte chromosomal aberration assay or in an in vivo rat bone marrow micronucleus assay.
Carcinogenicity. Carcinogenicity studies have not been conducted with acalabrutinib.
6 Pharmaceutical Particulars
6.1 List of Excipients
Tablet core. Mannitol, microcrystalline cellulose, hyprolose, and sodium stearylfumarate.
Tablet coating. Hypromellose, copovidone, titanium dioxide, macrogol 3350, medium chain triglycerides, iron oxide yellow, iron oxide red.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 30°C.
6.5 Nature and Contents of Container
Polyamide-aluminium-polyvinylchloride/aluminium blisters. Cartons of 56 tablets.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Acalabrutinib maleate monohydrate is a white to pale brown powder with pH-dependent solubility. It is freely soluble in water at pH values below 3 and practically insoluble at pH values above 6.
Chemical structure. The chemical name is 4-{8-Amino-3-[(2S)-1-(but-2-ynoyl)pyrrolidin-2-yl]imidazo[1,5-a]pyrazin-1-yl}-N-(pyridin-2-yl)benzamide (2Z)-2-butenedioic acid hydrate (1:1:1).
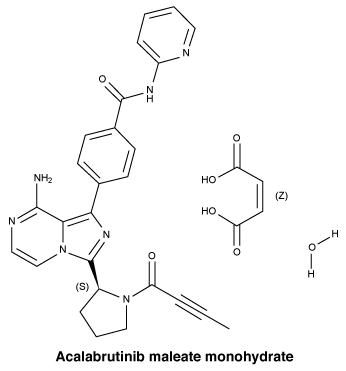
Molecular weight: 599.59.
CAS number. CAS 2641500-53-8.
7 Medicine Schedule (Poisons Standard)
Prescription only medicine (Schedule 4).
Date of First Approval
13 October 2022
Date of Revision
11 March 2026
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.