Cefoxitin Juno
Brand Information
| Brand name | Cefoxitin Juno |
| Active ingredient | Cefoxitin |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Cefoxitin Juno.
Summary CMI
CEFOXITIN JUNO
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using CEFOXITIN JUNO?
CEFOXITIN JUNO contains the active ingredient Cefoxitin sodium. CEFOXITIN JUNO is used to is used to treat a wide range of infections caused by bacteria.
For more information, see Section 1. Why am I using CEFOXITIN JUNO? in the full CMI.
2. What should I know before I use CEFOXITIN JUNO?
Do not use if you have ever had an allergic reaction to medicines containing cephalosporins or penicillins or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I use CEFOXITIN JUNO? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with CEFOXITIN JUNO and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use CEFOXITIN JUNO?
CEFOXITIN JUNO will always be prepared and given to you by a doctor or another healthcare professional. CEFOXITIN JUNO will be injected deep into muscle tissue or into a vein. When it is injected into a vein it may be given directly or through a 'drip'.
More instructions can be found in Section 4. How do I use CEFOXITIN JUNO? in the full CMI.
5. What should I know while using CEFOXITIN JUNO?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
For more information, see Section 5. What should I know while using CEFOXITIN JUNO? in the full CMI.
6. Are there any side effects?
Like other medicines, CEFOXITIN JUNO may have unwanted side effects in some people. Sometimes they are serious, most of the time they are not. You may need medical attention if you get some of the side effects.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
CEFOXITIN JUNO
Active ingredient: cefoxitin (as sodium)
Consumer Medicine Information (CMI)
This leaflet provides important information about using CEFOXITIN JUNO. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using CEFOXITIN JUNO.
Where to find information in this leaflet:
1. Why am I using CEFOXITIN JUNO?
2. What should I know before I use CEFOXITIN JUNO?
3. What if I am taking other medicines?
4. How do I use CEFOXITIN JUNO?
5. What should I know while using CEFOXITIN JUNO?
6. Are there any side effects?
7. Product details
1. Why am I using CEFOXITIN JUNO?
CEFOXITIN JUNO contains the active ingredient cefoxitin sodium. CEFOXITIN JUNO is an antibiotic that belongs to a group of medicines called cephalosporins.
CEFOXITIN JUNO is used to treat many different types of infections caused by bacteria. It works by killing the bacteria responsible for your infection. It may be given with other antibiotics.
2. What should I know before I use CEFOXITIN JUNO?
Do not use CEFOXITIN JUNO if:
- you are allergic to cefoxitin sodium, or any other cephalosporin antibiotics, or any of the other ingredients of this medicine.
- you have ever had a severe allergic (hypersensitive) reaction (e.g., severe skin peeling; swelling of the face, hands, feet, lips, tongue or throat; or difficulty swallowing or breathing) to any other type of beta-lactam antibiotic (penicillins, monobactams and carbapenems).
Tell your doctor if you:
- have any other medical conditions
- kidney disease
- liver disease
- central nervous system disorders - take any medicines for any other condition
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor if you are pregnant or intend to become pregnant.
Like most cephalosporin medicines, cefoxitin is not recommended for use during pregnancy. If there is a need to consider cefoxitin during your pregnancy, your doctor or pharmacist will discuss with you the benefits and risks of using it.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
Like most cephalosporin medicines, cefoxitin is not recommended while you are breast-feeding. If there is a need to consider cefoxitin while you are breast feeding, your doctor or pharmacist will discuss the possible risks and benefits of using it.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines and CEFOXITIN JUNO may interfere with each other. These include:
- warfarin or phenindione (medicines used to stop blood clots)
- frusemide (a medicine used to reduce fluid or blood pressure)
- gentamicin (a medicine used to treat severe infections)
- probenicid, a medicine used to treat gout.
Talk to your doctor about the need for an additional method of contraception while being given cefoxitin.
Some antibiotics may decrease the effectiveness of some birth control pills, although this has not been shown with cefoxitin.
These medicines may be affected by CEFOXITIN JUNO or may affect how well it works. You may need different amounts of your medicines, or you may need to take different medicines.
Your doctor and pharmacist have more information on medicines to be careful with or avoid while taking this medicine.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect CEFOXITIN JUNO.
4. How do I use CEFOXITIN JUNO?
How much to take / use
CEFOXITIN JUNO will always be prepared and given to you by a doctor or another healthcare professional.
Depending on the severity and type of infection, your weight, your age and how well your kidneys are working, your doctor will determine a suitable dosage.
How it is given
CEFOXITIN JUNO should be administered for as long as recommended by your doctor.
If you are given too much CEFOXITIN JUNO
As your dose of CEFOXITIN JUNO will be determined and administered by a medical specialist, the chance of receiving an overdose is most unlikely. However, if an overdose should be given, your specialist will give the appropriate treatment.
If you use too much CEFOXITIN JUNO
If you think that you have used too much CEFOXITIN JUNO, you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know while using CEFOXITIN JUNO?
Things you should do
If you are about to be started on any new medicine, remind your doctor and pharmacist that you are being given CEFOXITIN JUNO.
Tell any other doctors, dentists and pharmacists who treat you that you are being given this medicine.
It may interfere with the results of some tests.
If you are about to have any blood or urine tests, tell your doctor that you are being given this medicine.
If you become pregnant while taking this medicine, tell your doctor immediately.
Tell your doctor if the symptoms of your infection do not improve within a few days, or if they become worse.
Tell your doctor if you have any types of allergies to penicillin antibiotics. You may have an increased chance of being allergic to Cefoxitin if you are allergic to penicillins.
Tell your doctor if you have had an allergic reaction to lignocaine. In this case Cefoxitin should not be mixed with lignocaine and given to you. Sometimes Cefoxitin Juno is mixed with lignocaine hydrochloride so that the injection into the muscle is less painful.
Inform your doctor straight away if you do not feel well while you are being treated with CEFOXITIN JUNO.
This medicine helps most people with infections, but it may have unwanted side effects in a few people. All medicines can have side effects. Sometimes they are serious, most of the time they are not. You may need medical attention if you get some of the side effects.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how CEFOXITIN JUNO affects you.
CEFOXITIN JUNO may have a major influence on the ability to drive and use machines due to the possible occurrence of encephalopathy.
Certain side effects, such as dizziness and convulsions, have been reported with cefoxitin, which may affect some patient's ability to drive and use machines.
Looking after your medicine
CEFOXITIN JUNO will be stored in the pharmacy or on the ward.
Before opening:
Store in the original package at a temperature below 25°C. Protect from light.
After reconstitution:
To reduce microbiological hazard, use as soon as practicable after reconstitution/preparation. If storage is necessary, hold at 2-8°C for not more than 24 hours.
This medicine is for single use only. Any unused solution should be discarded.
Do not store CEFOXITIN JUNO or any other medicine in the bathroom or near a sink. Do not leave it on a window sill or in the car.
Heat and dampness can destroy some medicines.
Keep it where young children cannot reach it.
A locked cupboard at least one-and-a-half meters above the ground is a good place to store medicines.
Keep it where young children cannot reach it.
Getting rid of any unwanted medicine
If your doctor tells you to stop using this medicine or the expiry date has passed, ask your pharmacist what to do with any medicine that is left over.
Do not use this medicine after the expiry date.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Treatment with Cefoxitin, particularly in elderly patients with serious kidney or nervous system problems may rarely cause brain or nervous system disorders.
If you get severe diarrhoea, tell your doctor immediately. Do this even if it occurs several weeks after cefoxitin has been stopped. Do not take any diarrhoea medicine without first checking with your doctor.
Diarrhoea may mean that you have a serious condition affecting your bowel. You may need urgent medical care.
If you get a sore, white mouth or tongue while you are being treated with, or soon after stopping treatment with Cefoxitin, tell your doctor. Also tell your doctor if you get vaginal itching or discharge.
This may mean you have fungal infection called thrush. Sometimes the use of this medicine allows fungi to grow and the above symptoms to occur. Cefoxitin does not work against fungi.
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What CEFOXITIN JUNO contains
| Active ingredient (main ingredient) | Cefoxitin (as sodium) |
| Other ingredients (inactive ingredients) | NA |
| Potential allergens | Cefoxitin (as sodium) |
Do not take this medicine if you are allergic to any of these ingredients.
What CEFOXITIN JUNO looks like
CEFOXITIN JUNO is a powder for injection and is a white to slightly yellow sterile powder.
CEFOXITIN JUNO is available in packs of 5 or 10 vails in two different strengths:
CEFOXITIN JUNO 1 g/vial Aust R 50310.
CEFOXITIN JUNO 2 g/vial Aust R 50311.*
*Not marketed
Who distributes CEFOXITIN JUNO
Juno Pharmaceuticals Pty Ltd
15 – 17 Chapel Street,
Cremorne,
VIC 3121
www.junopharm.com.au
This leaflet was prepared in September 2025.
Brand Information
| Brand name | Cefoxitin Juno |
| Active ingredient | Cefoxitin |
| Schedule | S4 |
MIMS Revision Date: 01 November 2025
1 Name of Medicine
Cefoxitin sodium.
2 Qualitative and Quantitative Composition
Each gram of cefoxitin sodium contains approximately 51.2 mg (2.2 mEq) of sodium. The pH of 10% w/v cefoxitin sodium in Water for Injections is 4.2 to 7.0. Each vial contains cefoxitin sodium equivalent to 1 g or 2 g of cefoxitin.
3 Pharmaceutical Form
Cefoxitin Juno powder for injection is a white to slightly yellow sterile powder of cefoxitin sodium for intravenous and intramuscular administration following reconstitution.
4 Clinical Particulars
4.1 Therapeutic Indications
Cefoxitin (as sodium) powder for injection is indicated for the treatment of the following infections when due to susceptible organisms (see Section 5.1 Pharmacodynamic Properties, Microbiology) peritonitis and other intra-abdominal and intra-pelvic infections, female genital tract infections, septicaemia, endocarditis, urinary tract infections, respiratory tract infections, bone and joint infections, skin and skin structure infections.
Cefoxitin (as sodium) powder for injection has a high degree of stability against beta-lactamase and is therefore effective against beta-lactamase producing organisms resistant to penicillins or cephalosporins. It can also be used in mixed infections provided that the organisms are sensitive to it.
Cefoxitin (as sodium) powder for injection can be used as adjunctive therapy in the surgical treatment of infections including abscesses, infection complicating hollow viscus perforations, cutaneous infections and infections of serous surfaces whether caused by aerobes, mixed aerobes and anaerobes, or anaerobes.
Cefoxitin (as sodium) powder for injection is also indicated for the prevention of postoperative infections associated with certain surgical procedures of the gastrointestinal, biliary and genital tracts.
4.2 Dose and Method of Administration
Treatment. Cefoxitin Juno powder for injection may be administered intravenously or intramuscularly (see reconstitution directions for each route below). Dosage and route of administration are determined by severity of infection, susceptibility of the causative organisms, and condition of the patient.
Therapy may be started while awaiting the results of susceptibility testing.
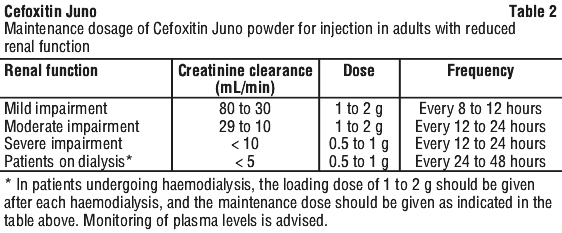
Adults. The usual adult dosage is 1 g or 2 g of cefoxitin sodium every 8 hours (see Tables 1 and 2). In adults with renal insufficiency, an initial loading dose of 1 g to 2 g may be given. After a loading dose, the recommendations for maintenance dosage may be used as a guide.
In severe infections, the total daily dosage should not exceed 12 g per day.

Neonates, infants and children. Neonates. 0 to 1 week of age, 20 to 40 mg/kg every 12 hours. 1 to 4 weeks of age, 20 to 40 mg/kg every 8 hours.
Dosage for premature infants not yet established.
Infants (1 to 3 months). 20 to 40 mg/kg every 6 hours or every 8 hours.
Children (over 3 months). 20 to 40 mg/kg every 6 hours or every 8 hours.
Cefoxitin sodium is not recommended for the therapy of meningitis. If meningitis is suspected, an appropriate antibiotic should be used.
In children with renal insufficiency, the dosage frequency should be reduced as indicated for adults.
Prophylaxis. For prophylactic use, the following doses are recommended:
Adults. 2 g administered intramuscularly approximately 1 hour before initial incision or intravenously just prior to surgery; then 2 g repeated twice at 6 hourly intervals.
Neonates, infants and children. There are no paediatric data on the prophylactic use of cefoxitin sodium. However, in view of its human efficacy and safety in this age group, the following doses are proposed - in the case of infants and children 30 to 40 mg/kg doses may be given at the times designated above. However, in neonates 30 to 40 mg/kg doses may be given approximately 1 hour before initial incision and one further dose may be given after 8-12 hours.
Caesarean section patients. The first dose of 2.0 g is administered intravenously as soon as the umbilical cord has been clamped. The second and third doses should be given as 2.0 g intravenously or intramuscularly 4 hours and 8 hours after the first dose.
Administration. Intravenous administration. Warning for neonates. Solutions containing preservatives should not be used for injection or for flushing catheters in treating neonates. Benzyl alcohol as a preservative in Bacteriostatic Water for Injections has been associated with toxicity in neonates. Data are unavailable on the toxicity of other preservatives in this age group. Therefore, any diluent used with Cefoxitin Juno powder for injection in the treatment of neonates should be free of any preservative.
Reconstitution. Reconstitute Cefoxitin Juno powder for injection with Sterile Water for Injections - 1 g is soluble in 2 mL. Although cefoxitin sodium is very soluble, for intravenous use it is preferable to add 10 mL of Sterile Water for Injections to the 1 g vial or 10 mL to 20 mL to the 2 g vial. Shake to dissolve and then withdraw entire contents of the vial into a syringe.
For direct intravenous injection, cefoxitin sodium may be slowly injected into the vein over a period of 3 to 5 minutes or may be given through the tubing when the patient is receiving compatible parenteral solutions.
Alternatively, an intermittent intravenous infusion of cefoxitin sodium may be employed when large amounts of fluid are to be given. However, during infusion of the solution containing cefoxitin sodium, it may be advisable temporarily to discontinue administration of any other infusion solution at the same site (by using an appropriate IV infusion set).
A solution of cefoxitin sodium may also be given by continuous intravenous infusion (see Compatibility information).
Intramuscular administration. Reconstitute Cefoxitin Juno powder for injection 1 g with 2 mL of 0.5% or 1% lignocaine hydrochloride (without adrenaline) solution. Some patients may be hypersensitive to lignocaine (see Section 4.8 Adverse Effects (Undesirable Effects)). If lignocaine cannot be used, Cefoxitin Juno powder for injection may be reconstituted with 2 mL of Sterile Water for Injections. The 2 g vial may be reconstituted with 4 mL of diluent for intramuscular use. Cefoxitin sodium is given by deep injection into a large muscle mass. Avoid injection into a blood vessel.
Preparation of solution. Table 3 is provided for convenience in reconstituting Cefoxitin Juno for injection for both intravenous and intramuscular administration.

Compatibility information. The compatibility and stability of cefoxitin sodium in solution with the following series of frequently used intravenous infusion fluids and injectable additives have been established: Sodium Chloride Intravenous Infusion 0.9%, Glucose Intravenous Infusion 5% or 10%, Glucose 5% with Sodium Chloride Intravenous Infusion 0.9%, Lactated Ringers Injection, Glucose 5% in Lactated Ringers Injection, Invert sugar 5% or 10% in water, Heparin 100 units/mL in Glucose 5% or Sodium Chloride Intravenous Infusion.
Cefoxitin Juno powder for injection reconstituted to a concentration of 95 mg/mL or 400 mg/mL with Water for Injections, or Water for Injections preserved with benzyl alcohol, or Sodium Chloride Intravenous Infusion 0.9%, or Glucose Intravenous Infusion 5% strength or 10% strength should be used immediately after preparation. Any unused portion should be discarded.
The reconstituted solutions maintain satisfactory chemical potency for 6 hours at 30°C and for 96 hours at 2 to 8°C.
More dilute solutions of cefoxitin 1 mg/mL or 40 mg/mL in Water for Injections, or Sodium Chloride Intravenous Infusion 0.9%, or Glucose Intravenous Infusion 5% strength or 10% strength, or Glucose 5% strength with Sodium Chloride Intravenous Infusion 0.9%, or Glucose 5% strength in Lactated Ringers Injection, or Lactated Ringers Injection, or Invert Sugar 5% strength or 10% strength in Water for Injections, or Heparin 100 units/mL in Glucose Intravenous Infusion 5% strength or Sodium Chloride Intravenous Infusion 0.9% should be used immediately after preparation. Any unused portion should be discarded.
The reconstituted solutions retain adequate potency for up to 6 hours when stored at 30°C and for at least 36 hours when stored at 2 to 8°C.
4.3 Contraindications
Cefoxitin (as sodium) powder for injection is contraindicated in persons who have shown hypersensitivity to cefoxitin and the cephalosporin group of antibiotics.
Its use in patients with a history of hypersensitivity to penicillin requires great care (see Section 4.4 Special Warnings and Precautions for Use). Cefoxitin (as sodium) powder for injection is contraindicated in patients who have had a major allergic reaction to penicillin (anaphylaxis, angioneurotic oedema or urticaria).
Lignocaine hydrochloride should not be used as a diluent for intramuscular injection in patients who are hypersensitive to lignocaine.
4.4 Special Warnings and Precautions for Use
Severe cutaneous adverse reactions. Severe cutaneous adverse reactions (SCAR), such as Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), drug reaction with eosinophilia and systemic symptoms (DRESS), and acute generalised exanthematous pustulosis (AGEP) have been reported in patients taking beta-lactam antibiotics. When SCAR is suspected, cefoxitin should be discontinued immediately and an alternative treatment should be considered.
Hypersensitivity reaction (allergic/anaphylaxis). There is some clinical and laboratory evidence of partial cross-allergenicity between cephamycins and the other beta-lactam antibiotics, penicillins and cephalosporins. Severe reactions (including anaphylaxis) have been reported with most beta lactam antibiotics.
Before therapy with cefoxitin (as sodium) powder for injection, careful inquiry should be made concerning previous hypersensitivity reactions to beta-lactam antibiotics. Cefoxitin (as sodium) powder for injection should be given cautiously to penicillin allergic patients. If an allergic reaction occurs, the drug should be discontinued (see Section 4.3 Contraindications). Serious hypersensitivity reactions may require adrenaline (epinephrine) and other emergency measures.
Any patient who has demonstrated some form of allergy, particularly to drugs, should receive antibiotics cautiously.
Neurotoxicity. There have been reports of neurotoxicity associated with cephalosporin treatment. Symptoms of neurotoxicity include encephalopathy, seizures and/or myoclonus. Risk factors for developing neurotoxicity with cephalosporin treatment include being elderly, renal impairment, central nervous system disorders and intravenous administration. Withdrawal of the medicine should be considered if there are signs of neurotoxicity.
Neonates. Solutions containing preservatives should not be used for injection or for flushing catheters in treating neonates. Benzyl alcohol as a preservative in Bacteriostatic Water for Injections has been associated with toxicity in neonates. Data are unavailable on the toxicity of other preservatives in this age group. Therefore, any diluent used with Cefoxitin Juno powder for injection in the treatment of neonates should be free of any preservative.
Concentrations of cefoxitin sodium in the CSF are considerably lower than in the plasma. Its use in the treatment of meningitis and brain abscess is therefore not advised.
Superinfection with non-susceptible organisms, including fungi, may occur and requires appropriate therapy.
Cefoxitin sodium appears to have little nephrotoxic potential in man at the usual doses. Patients whose clinical condition requires high doses, especially when potentially nephrotoxic drugs (e.g. aminoglycoside antibiotics) are administered concurrently, should be carefully monitored for renal function. Increased nephrotoxicity has been reported following concomitant administration of cephalosporins and aminoglycoside antibiotics.
Repeated use of lignocaine hydrochloride as a diluent for intramuscular use should be avoided in patients with severe liver disease or decreased hepatic blood flow, due to the possibility of lignocaine toxicity (resulting from decreased metabolism and accumulation).
Clostridium difficile associated diarrhoea (CDAD). Clostridium difficile associated diarrhoea (CDAD) has been reported with nearly all antibacterial agents, including cefoxitin injection and may range in severity from mild diarrhoea to fatal colitis. Treatment with antibacterial agents alters the normal flora of the colon leading to overgrowth of C. difficile.
Antibiotic associated pseudomembranous colitis has been reported with many antibiotics including cefoxitin sodium. Toxin produced by Clostridium difficile, appears to be the primary cause. Hypertoxin producing strains of C. difficile cause increased morbidity and mortality, as these infections can be refractory to antimicrobial therapy and may require colectomy. CDAD must be considered in all patients who present with diarrhoea following antibiotic use. It is important to consider this diagnosis in patients who develop diarrhoea or colitis in association with antibiotic use (this may occur up to several weeks - usually over two months after cessation of antibiotic therapy). Mild cases usually respond to drug discontinuation alone. However, in moderate to severe cases appropriate therapy with a suitable oral antibacterial agent effective against Clostridium difficile should be considered. Fluids, electrolytes and protein replacement should be provided when indicated. Drugs which delay peristalsis e.g. opiates and diphenoxylate with atropine (Lomotil) may prolong and/or worsen the condition and should not be used.
Antibiotics should be prescribed with care for patients with a history of gastrointestinal disease, especially ulcerative colitis, regional enteritis, or antibiotic associated colitis.
Use in renal impairment. This drug is known to be substantially excreted by the kidney, and the risk of toxic reactions to this drug may be greater in patients with impaired renal function. The total daily dosage should be reduced when cefoxitin (as sodium) powder for injection is administered to patients with transient or persistent reduction of urinary output due to renal impairment, because high and prolonged serum concentrations can occur in such individuals (see Section 4.2 Dose and Method of Administration).
Use in the elderly. Elderly patients are more likely to have decreased renal function, care should be taken in dose selection and it may be useful to monitor renal function.
Paediatric use. In children with renal insufficiency, the dosage frequency should be reduced as indicated for adults (see Section 4.2 Dose and Method of Administration).
Effect on laboratory tests. A false-positive reaction to glucose in the urine may occur with reducing substances but not with the use of specific glucose oxidase methods.
Using the Jaffe Technique, falsely high creatinine values in serum may occur if cefoxitin sodium serum concentrations exceed 100 microgram/mL. Serum samples from patients treated with cefoxitin sodium should not be analysed for creatinine if withdrawn within two hours of drug administration.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Cephalosporins have affected the stability of anticoagulant control of patients treated with phenindione and warfarin during one trial.
Concurrent treatment with nephrotoxic drugs such as gentamicin and frusemide may result in increased nephrotoxicity (see Section 4.4 Special Warnings and Precautions for Use).
Concomitant administration of oral probenecid competitively inhibits tubular secretion resulting in higher and more prolonged serum concentrations of cefoxitin.
High concentrations of cefoxitin in the urine may interfere with measurement of 17-hydroxy-corticosteroids by the Porter-Silber reaction, and produce false increases of modest degree in the levels reported.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. No data available.
Use in pregnancy. (Category B1)
Category B1: This category specifies drugs which have been taken by only a limited number of pregnant women and women of childbearing age, without an increase in the frequency of malformations or other direct or indirect harmful effects on the human foetus having been observed.
Studies in animals have not shown evidence of an increased occurrence of foetal damage. Cefoxitin (as sodium) powder for injection should not however be used in women of childbearing potential unless, in the judgement of the treating clinician, its use is deemed essential to the welfare of the patient and the expected benefits outweigh potential risks.
Use in lactation. Cefoxitin sodium is excreted in human milk. If possible, alternative arrangements should be made to feed the infant.
4.7 Effects on Ability to Drive and Use Machines
Cefoxitin has a major influence on the ability to drive and use machines especially because of the possible occurrence of encephalopathy.
4.8 Adverse Effects (Undesirable Effects)
Cefoxitin sodium is generally well tolerated. Adverse effects occurred in 8.5% of cases, were usually mild and transient, and rarely required cessation of treatment.
Skin and other subcutaneous tissue disorders. Severe cutaneous adverse reactions, including Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), drug reaction with eosinophilia and systemic symptoms (DRESS), and acute generalised exanthematous pustulosis (AGEP) have been reported in beta-lactam antibiotics (see Section 4.4 Special Warnings and Precautions for Use).
Local reactions. Thrombophlebitis or phlebitis has occurred in 2.5% of cases following intravenous administration. Another 1.7% of cases reported pain in the infused vein and vein induration, erythema or exudates. Pain, induration and tenderness following intramuscular injections have been reported. Pain was often severe in cases where cefoxitin (as sodium) powder for injection had been dissolved in Water for Injections instead of 0.5% lignocaine hydrochloride (see Section 4.2 Dose and Method of Administration).
Allergic. Skin rashes, e.g. maculopapular rash and urticaria, occurred in 1.7% of cases. Other adverse effects included pruritus, eosinophilia, fever and, rarely, other allergic reactions, including anaphylaxis which in rare cases has led to death.
Gastrointestinal. Nausea, vomiting and diarrhoea have been reported rarely (see Section 4.4 Special Warnings and Precautions for Use).
Cardiovascular. Hypotension.
Blood. Eosinophilia, leukopenia, agranulocytosis, granulocytopenia, neutropenia, thrombocytopenia, haemolytic anaemia and bone marrow depression have been reported. Some individuals, particularly those with azotaemia, may develop positive direct Coombs tests during therapy with cefoxitin sodium.
Liver function. Transient elevations in AST, ALT, serum LDH, and serum alkaline phosphatase have been reported. Jaundice has occurred.
Renal and urinary disorders. Elevations in serum creatinine and/or blood urea nitrogen levels have been observed. As with the cephalosporins, acute renal failure has been reported rarely. The role of cefoxitin sodium in changes in renal function tests is difficult to assess, since factors predisposing to prerenal azotaemia or to impaired renal function usually have been present.
In addition to the adverse reactions listed above which have been observed in patients treated with cefoxitin, the following adverse reactions and altered laboratory test results have been reported for cephalosporins class antibiotics:
Urticaria, erythema multiforme, Stevens-Johnson syndrome, serum sickness-like reactions, abdominal pain, colitis, renal dysfunction, toxic nephropathy, false positive test for urinary glucose, hepatic dysfunction including cholestasis, elevated bilirubin, aplastic anaemia, haemorrhage, prolonged prothrombin time, pancytopenia, agranulocytosis, superinfection, vaginitis including vaginitis candidiasis.
Musculoskeletal and connective tissue disorders. Exacerbation of myasthenia gravis.
Several cephalosporins have been implicated in triggering seizures, particularly in patients with renal impairment when the dosage was not reduced (see Section 4.2 Dose and Method of Administration). If seizures associated with drug therapy occur, the drug should be discontinued. Anticonvulsant therapy can be given if clinically indicated.
Post-marketing experience. Nervous system disorders. Seizures, encephalopathy, myoclonus - frequency not known.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
Expected effects would be those described (see Section 4.8 Adverse Effects (Undesirable Effects)); namely, allergic, gastrointestinal, blood, liver function and kidney.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Cefoxitin is a bactericidal antibiotic which acts by inhibiting bacterial cell wall synthesis. Due to the presence of a 7-α methoxy group in the β-lactam ring, it exhibits a high degree of stability in the presence of beta-lactamases.
Microbiology. Cefoxitin is active against the following microorganisms in vitro:
Aerobic bacteria. 1. Gram-positive cocci including Staphylococci (including coagulase-positive, coagulase-negative and penicillinase producing strains), Group A beta-haemolytic streptococci (Streptococcus pyogenes), Group B beta-haemolytic streptococci (Streptococcus agalactiae) and Streptococcus pneumoniae (Diplococcus pneumoniae). Other streptococci (most strains of enterococci, e.g. Streptococcus faecalis) are resistant.
2. Gram-negative cocci including Neisseria gonorrhoeae (including penicillinase-producing strains) and Neisseria meningitidis.
3. Gram-negative rods (facultative anaerobes) including Escherichia coli, Klebsiella pneumoniae, Klebsiella spp, Proteus mirabilis, Proteus (indole-positive), Proteus vulgaris, Providencia rettgeri, Morganella morganii, Serratia marcescens, Providencia spp, Salmonella and Shigella spp.
Anaerobic bacteria. 1. Gram-positive cocci including Peptococcus spp, Peptostreptococcus spp and Microaerophilic streptococcus.
2. Gram-positive rods including Clostridium perfringens, Clostridium spp, Eubacterium spp and Propionibacterium acnes.
3. Gram-negative cocci including Veillonella spp.
4. Gram-negative rods including Bacteroides fragilis, Bacteroides melaninogenicus, Bacteroides spp (including both penicillin-susceptible and penicillin-resistant strains) and Fusobacterium spp.
Cefoxitin sodium is not active against pseudomonas spp, most strains of enterococci and many strains of Enterobacter cloacae. Methicillin-resistant staphylococci are almost uniformly resistant to cefoxitin sodium.
Susceptibility testing. For fast growing aerobic organisms, quantitative methods that require measurements of zone diameters give the most precise estimates of antibiotic susceptibility. One such procedure (Kirby-Bauer) has been recommended for use with discs to test susceptibility to cefoxitin. Interpretation involves correlation of the diameters obtained in the disc test with minimal inhibitory concentration (MIC) values for cefoxitin sodium.
Reports from the laboratory giving results of the standardized single disc susceptibility test using a 30 microgram cefoxitin disc should be interpreted according to the following criteria:
Organisms producing zones of 18 mm or greater are considered susceptible indicating that the tested organism is likely to respond to therapy.
Organisms of intermediate susceptibility produce zones of 15 to 17 mm indicating that the tested organism would be susceptible if high dosage is used or if the infection is confined to tissues and fluids (e.g. urine) in which high antibiotic levels are attained.
Resistant organisms produce zones of 14 mm or less indicating that other therapy should be selected.
The cefoxitin disc should be used for testing cefoxitin susceptibility.
Cefoxitin sodium has been shown by in vitro tests to have activity against certain strains of Enterobacteriaceae found resistant when tested with the cephalosporin class disc. For this reason, the cefoxitin disc should not be used for testing susceptibility to cephalosporins, and cephalosporin discs should not be used for testing susceptibility to cefoxitin sodium.
Dilution methods, preferably the agar plate dilution procedure, are most accurate for susceptibility testing of obligate anaerobes. A bacterial isolate may be considered susceptible if the MIC value for cefoxitin sodium is not more than 16 microgram/mL. Organisms are considered resistant if the MIC is greater than 32 microgram/mL.
Clinical trials. No data available.
5.2 Pharmacokinetic Properties
Cefoxitin sodium administered by the parenteral route is excreted virtually unchanged by the kidneys. The mean terminal serum half life is approximately one hour and co-administration of probenecid will slow tubular excretion and increase and prolong blood levels. Although cefoxitin sodium will penetrate into the CSF, concentrations are considerably lower than in the plasma.
Following intravenous administration, the peak serum concentration of cefoxitin sodium following 1 g infused intravenously over 3 minutes was 110.5 microgram/mL, when infused over 30 minutes was 72 microgram/mL, and when infused over 120 minutes was 25 microgram/mL. Following 2 g infused intravenously over 3 minutes, the peak serum concentration was 221 microgram/mL. The serum half life was approximately 50 minutes, falling to less than 1 microgram/mL at 4 hours.
In a number of studies using 0.5 g, 1 g, or 2 g intravenous doses of cefoxitin sodium, mean total urinary recovery ranged from 77% to 99% of the dose administered.
Following intramuscular administration, injections of 1 g of cefoxitin sodium in 0.5% lignocaine hydrochloride solution produced a peak serum concentration of approximately 30 microgram/mL at 30 minutes, falling to approximately 3.2 microgram/mL at 3 hours. Approximately 85% of an intramuscular dose is excreted by the kidneys in the first six hours resulting in high urine levels; for example, greater than 3000 microgram/mL between one and two hours after a 1 g dose. When cefoxitin (as sodium) powder for injection was reconstituted with 0.5% or 1% of lignocaine hydrochloride for intramuscular use, the local anaesthetic was found to have no effect on the absorption or elimination.
5.3 Preclinical Safety Data
Genotoxicity. No data available.
Carcinogenicity. No data available.
6 Pharmaceutical Particulars
6.1 List of Excipients
No excipients.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C. Protect from light.
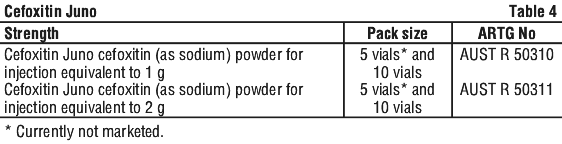
6.5 Nature and Contents of Container
See Table 4.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
Chemical structure.
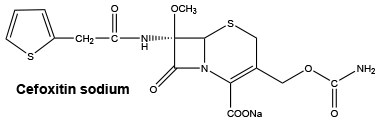
Molecular formula: C16H16N3NaO7S2.
Molecular weight: 449.4.
CAS number. Chemical Abstracts Service (CAS) registry number: 33564-30-6.
7 Medicine Schedule (Poisons Standard)
S4-Prescription Only Medicine.
Date of First Approval
14 September 1994
Date of Revision
29 September 2025
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.