Co-Diovan
Brand Information
| Brand name | Co-Diovan |
| Active ingredient | Valsartan + Hydrochlorothiazide |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Co-Diovan.
Summary CMI
Co-Diovan® Film Coated Tablet
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using Co-Diovan?
Co-Diovan contains the active ingredients Valsartan and hydrochlorothiazide. Co-Diovan is used to treat high blood pressure. Symptoms include headache, fatigue, irregular heartbeat and vision problems.
For more information, see Section 1. Why am I using Co-Diovan? in the full CMI.
2. What should I know before I use Co-Diovan?
Do not use if you have ever had an allergic reaction to Co-Diovan or any of the ingredients listed at the end of the CMI. Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding. For more information, see Section 2. What should I know before I use Co-Diovan? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with Co-Diovan and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use Co-Diovan?
- Your doctor will advise you on the appropriate dose.
- Follow the instructions provided and use Co-Diovan until your doctor tells you to stop.
More instructions can be found in Section 4. How do I use Co-Diovan? in the full CMI.
5. What should I know while using Co-Diovan?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Drinking alcohol |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using Co-Diovan? in the full CMI.
6. Are there any side effects?
Common side effects include dizziness, headache, muscular weakness, joint pain, blurred vision, dry mouth, feeling sick, tiredness. For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
Co-Diovan® Film Coated Tablet
Active ingredients: Valsartan and hydrochlorothiazide
Consumer Medicine Information (CMI)
This leaflet provides important information about using Co-Diovan. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using Co-Diovan.
Where to find information in this leaflet:
1. Why am I using Co-Diovan?
2. What should I know before I use Co-Diovan?
3. What if I am taking other medicines?
4. How do I use Co-Diovan?
5. What should I know while using Co-Diovan?
6. Are there any side effects?
7. Product details
1. Why am I using Co-Diovan?
Co-Diovan contains the active ingredients Valsartan and Hydrochlorothiazide.
Co-Diovan is used to treat high blood pressure. Symptoms include headache, fatigue, irregular heartbeat and vision problems. Co-Diovan helps to reduce blood pressure in two ways:
Valsartan helps to lower your blood pressure by blocking the effect of angiotensin II. This is a substance which makes your blood vessels tighten, which raises your blood pressure. When Valsartan blocks it, your blood vessels become relaxed, making it easier for blood to flow and thus helping to lower your blood pressure.
Hydrochlorothiazide is a diuretic (water pill) type of medicine. It helps in reducing the amount of excess fluid in the body by increasing the amount of urine produced and thereby helps in lowering your blood pressure.
2. What should I know before I use Co-Diovan?
Warnings
Do not use Co-Diovan
- If you are allergic to Valsartan, Hydrochlorothiazide or other sulfonamide-derived medicines or any of the ingredients listed at the end of this leaflet. Always check the ingredients to make sure you can use this medicine. Symptoms of allergic reaction may include shortness of breath, difficulty breathing, swelling of the face, lips, tongue or other parts of the body, rash, hives.
- In pregnancy
- In children
- If you have severe liver diseases, symptoms such as and tiredness, itchy skin, and yellowing of the skin and eyes or intense itching, dark urine and light-colored stools.
- If you suffer from symptoms such as tiredness, weakness, little to no urine output or severe kidney problems.
- If you have following symptoms:
- Muscle weakness and muscle cramps, irregular heartbeat, weakness.
- Feeling sick, vomiting, headache, loss of energy
- Tiredness, pain in bone, headache
- Joint pain and swelling, redness and warmth around affected joints. - If you use a medicine called aliskiren.
Check with your doctor if you:
- have any other medical conditions.
- take any medicines for any other condition.
- are taking any medicines similar to Hydrochlorothiazide (diuretics).
- have severe heart failure.
- suffer from problems with your kidneys.
- have headache, muscle weakness, tiredness.
- have an allergy or symptoms such as wheezing, shortness of breath, coughing.
- have heart problems
- suffer from skin rashes (butterfly-shaped), tiredness, joint and muscle pain.
- have eye problems.
- suffer from non-melanoma skin cancer.
- have any breathing problems.
- suffer from mild to moderate liver diseases or any kidney problems.
- have high levels of cholesterol, triglycerides in your blood.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor if you are pregnant or intend to become pregnant.
Do not use Co-Diovan during pregnancy or if you are planning to become pregnant. It may affect your unborn baby.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
Do not use Co-Diovan during breastfeeding.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with Co-Diovan and affect how it works.
Tell your doctor if you take any of the following medicines:
- Medicines used to relieve pain, swelling e.g. non-steroidal anti-inflammatory drugs (NSAIDs), salicylic acid derivatives indomethacin including Selective Cyclooxegase-2 Inhibitors (COX-2 Inhibitors)
- Medicines used to treat high blood pressure and some other heart problems such as diuretic medicines, ACE-inhibitors, aliskiren and beta blockers
- Potassium supplements, potassium-sparing diuretics, or other drugs that may alter potassium levels e.g. heparin, trimethoprim containing medicines
- Antiretrovirals (ritonavir), antibiotics (rifamycins)
- Other antihypertensive drugs e.g. guanethidine, methyldopa, beta-blockers, vasodilators, calcium channel blockers, methyldopa.
- Diazoxide, drug used to treat low blood sugar level.
- Non-depolarising muscle relaxants (e.g. curare derivatives).
- Insulin and antidiabetic medicines
- Medicines used for treatment of heart problems and high blood pressure e.g. kaliuretic diuretics
- Carbenoxolone, medicine used for treatment of various stomach problems.
- Penicillin G, antibiotic used in treatment of bacterial infections
- Medicines used to treat irregular heart beats e.g. antiarrhythmics and digitalis glycosides
- Antidepressants, antipsychotics e.g. Lithium
- Antiepileptics e.g. carbamazepine
- Anticholinergic agents (e.g. atropine, biperiden, which are used to treat Parkinson's disease, relieve stomach cramps, spasms
- Pressor amines (e.g. noradrenaline)
- Medicines used to lower cholesterol e.g. cholestyramine or colestipol resins
- Tetracycline, a drug used to treat some infections
- Alcohol, anaesthetics and sedatives (sleeping tablets)
- Radioactive iodine, used as a medical tracer or diagnosis
- Cyclophosphamide, methotrexate, a drug used to treat arthritis and some cancers
- Medicines or supplements containing calcium
- Vitamin D
- Medicines used in organ transplants e.g. cyclosporin
- Steroid medicines such as cortisone, prednisone and ACTH
- Amphotericin, a drug used to treat fungal infections
- Medicines used to treat gout e.g. Allopurinol, probenacid or sulfinpyrazone
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect Co-Diovan.
4. How do I use Co-Diovan?
How much to take
- Your doctor will advise you on the appropriate dose.
- Follow the instructions provided and use Co-Diovan until your doctor tells you to stop.
- The usual dose is one tablet per day as advised by your doctor.
When to take Co-Diovan
- Co-Diovan should be taken at the same time each day.
- When you take the first dose from the pack of Co-Diovan, take the one marked with the correct day of the week (e.g. if it is Wednesday, take the dose from the section of the foil marked Wednesday).
How to take Co-Diovan
- Swallow the tablet with a full glass of water.
- Take Co-Diovan consistently with or without food
- If you feel that your stomach gets upset after taking Co-Diovan, always take it after a meal.
If you forget to use Co-Diovan
Co-Diovan should be used regularly at the same time each day. If you miss your dose at the usual time, take the dose as soon as you remember and then go back to taking it as you would normally.
If it is almost time for your next dose, skip the dose you missed and take your next dose when you are meant to.
Do not take a double dose to make up for the dose you missed.
If you use too much Co-Diovan
If you think that you have used too much Co-Diovan, you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know while using Co-Diovan?
Things you should do
- Check your skin for any new lesions and report any suspicious skin lesions to your doctor immediately.
- There may be a risk of developing non-melanoma skin cancer while on treatment with Co-Diovan.
- Avoid direct exposure to sunlight and UV rays, in case of exposure, use adequate protection to avoid the risk of skin cancer.
Call your doctor straight away if you:
- develop any signs of allergic reaction.
- become pregnant or intend to become pregnant or if you are breastfeeding.
- are going to have surgery, tell your doctor that you are taking Co-Diovan.
- notice symptoms such as increased sensitivity of the skin to sun. Symptoms of sunburn such as redness, itching, swelling, blistering which may occur more quickly than normal.
- have muscle weakness or cramps, tiredness.
- Remind any doctor, dentist, pharmacist or specialist you visit that you are using Co-Diovan.
Things you should not do
- Do not stop using this medicine suddenly.
- Do not give Co-Diovan to anyone else, even if they seem to have the same condition as you.
- Do not use Co-Diovan to treat any other complaints unless your doctor tells you to.
Lab tests:
- Your doctor may do a routine blood checkup, ECG during treatment with Co-Diovan.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how Co-Diovan affects you.
Co-Diovan may cause dizziness in some people. Precaution should be taken before driving or using any machines or tools.
Drinking alcohol
Tell your doctor if you drink alcohol.
Looking after your medicine
- Store below 30°C.
- Keep in the original package.
- Protect from moisture.
Follow the instructions in the carton on how to take care of your medicine properly.
Store it in a cool dry place away from moisture, heat or sunlight; for example, do not store it:
- in the bathroom or near a sink, or
- in the car or on window sills.
Keep it where young children cannot reach it.
Getting rid of any unwanted medicine
If you no longer need to use this medicine or it is out of date, take it to any pharmacy for safe disposal.
Do not use this medicine after the expiry date.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
General problems:
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
Respiratory problems:
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What Co-Diovan contains
| Active ingredient (main ingredient) | Valsartan and hydrochlorothiazide. |
| Other ingredients (inactive ingredients) | Co-Diovan 80/12.5: silica-colloidal anhydrous; crospovidone; hypromellose; magnesium stearate; cellulose-microcrystalline; macrogol 8000; talc-purified; titanium dioxide; iron oxide red; iron oxide yellow. Co-Diovan 160/12.5: silica-colloidal anhydrous; crospovidone; hypromellose; magnesium stearate; cellulose-microcrystalline; macrogol 8000; talc-purified; titanium dioxide; iron oxide red. Co-Diovan 160/25: silica-colloidal anhydrous; crospovidone; hypromellose; magnesium stearate; cellulose-microcrystalline; macrogol 4000; talc-purified; titanium dioxide, iron oxide red, iron oxide yellow, iron oxide black. Co-Diovan 320/12.5: silica-colloidal anhydrous; crospovidone; hypromellose; magnesium stearate; cellulose-microcrystalline; macrogol 4000; talc-purified; titanium dioxide, iron oxide red, iron oxide black. Co-Diovan 320/25: silica-colloidal anhydrous; crospovidone; hypromellose; magnesium stearate; cellulose-microcrystalline; macrogol 4000; talc-purified; titanium dioxide, iron oxide yellow. |
| Potential allergens | NA |
Do not take this medicine if you are allergic to any of these ingredients.
What Co-Diovan looks like
Co-Diovan 80/12.5: Ovaloid, non-divisible, film-coated tablets coloured light orange and imprinted with HGH on one side and CG on the other side. It is available in PA/Al/PVC/Al blister packs of 7, 14, 28, 30 and 56.
Co-Diovan 160/12.5: Ovaloid, non-divisible, film-coated tablets coloured dark red and imprinted with HHH on one side and CG on the other side. It is available in PA/Al/PVC/Al blister packs of 7, 14, 28, 30 and 56.
Co-Diovan 160/25: Ovaloid, non-divisible, film-coated tablets coloured brown-orange and imprinted with HXH on one side and NVR on the other side. It is available in PA/Al/PVC/Al blister packs of 7, 14, 28, 30 and 56.
Co-Diovan 320/12.5: Ovaloid, non-divisible, film-coated tablets coloured pink and imprinted with HIL on one side and NVR on the other side. It is available in PA/Al/PVC/Al blister packs of 7, 14, 28, 30 and 56.
Co-Diovan 320/25: Ovaloid, non-divisible, film-coated tablets coloured yellow and imprinted with CTI on one side and NVR on the other side. It is available in PA/Al/PVC/Al blister packs of 7, 14, 28, 30 and 56.
Not all strengths and pack sizes may be marketed.
Australian Registration Numbers
Co-Diovan 80/12.5 mg tablets AUST R 96740
Co-Diovan 160/12.5 mg tablets AUST R 96741
Co-Diovan 160/25 mg tablets AUST R 96742
Co-Diovan 320/12.5 mg tablets AUST R 135782
Co-Diovan 320/25 mg tablets AUST R 135812
Who distributes Co-Diovan
Co-Diovan is supplied in Australia by:
NOVARTIS Pharmaceuticals Australia Pty Limited
ABN 18 004 244 160
54 Waterloo Road North Ryde NSW 2113
Telephone: 1 800 671 203
®= Registered Trademark
This leaflet was prepared in October 2025
Internal code:
cod271022c_V2 based on PI cod271022i
Brand Information
| Brand name | Co-Diovan |
| Active ingredient | Valsartan + Hydrochlorothiazide |
| Schedule | S4 |
MIMS Revision Date: 01 December 2022
1 Name of Medicine
Valsartan/hydrochlorothiazide.
2 Qualitative and Quantitative Composition
Valsartan [N-Pentanoyl-N-[2'-(1H-tetrazol-5-yl)biphenyl-4ylmethyl]-L-valine] is a fine white powder soluble in methanol, neutral and basic aqueous solutions, and very slightly soluble in solutions with pH < 7.
Hydrochlorothiazide [6-chloro-3,4-dihydro-2H-1,2,4-benzothiadiazine-7-sulfonamide-1,1-dioxide] is structurally related to the thiazide group of diuretics. It is a white or almost white powder. Hydrochlorothiazide is very slightly soluble in water and freely soluble in dimethylsulfoxide.
Co-Diovan 80/12.5 contains valsartan 80 mg and hydrochlorothiazide 12.5 mg; Co-Diovan 160/12.5 contains valsartan 160 mg and hydrochlorothiazide 12.5 mg; Co-Diovan 160/25 contains valsartan 160 mg and hydrochlorothiazide 25 mg; Co-Diovan 320/12.5 contains valsartan 320 mg and hydrochlorothiazide 12.5 mg; Co-Diovan 320/25 contains valsartan 320 mg and hydrochlorothiazide 25 mg.
Co-Diovan is available in five strengths: Co-Diovan 80/12.5, Co-Diovan 160/12.5, Co-Diovan 160/25, Co-Diovan 320/12.5 and Co-Diovan 320/25.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Co-Diovan 80/12.5: Ovaloid, non-divisible, film-coated tablets coloured light orange and imprinted with HGH on one side and CG on the other side.
Co-Diovan 160/12.5: Ovaloid, non-divisible, film-coated tablets coloured dark red and imprinted with HHH on one side and CG on the other side.
Co-Diovan 160/25: Ovaloid, non-divisible, film-coated tablets coloured brown-orange and imprinted with HXH on one side and NVR on the other side.
Co-Diovan 320/12.5: Ovaloid, non-divisible, film-coated tablets coloured pink and imprinted with HIL on one side and NVR on the other side.
Co-Diovan 320/25: Ovaloid, non-divisible, film-coated tablets coloured yellow and imprinted with CTI on one side and NVR on the other side.
Co-Diovan tablets cannot be divided into equal doses.
4 Clinical Particulars
4.1 Therapeutic Indications
Co-Diovan is indicated for the treatment of hypertension. Treatment should not be initiated with these combinations.
4.2 Dose and Method of Administration
The recommended dose of Co-Diovan is one tablet per day. When clinically appropriate either Co-Diovan 80/12.5, 160/12.5 or 320/12.5 may be used.
Co-Diovan 160/12.5 mg may be administered in patients whose blood pressure is not adequately controlled after 4 weeks of treatment by valsartan 160 mg monotherapy. Treatment with Co-Diovan 160/25 mg is limited to those patients who do not show adequate blood pressure reduction with Co-Diovan 160/12.5 mg after at least 4 weeks of treatment.
Co-Diovan 320/12.5 mg may be administered in patients whose blood pressure is not adequately controlled after 4 weeks of treatment by valsartan 320 mg monotherapy. Treatment with Co-Diovan 320/25 mg is limited to those patients with more severe hypertension who do not show adequate blood pressure reduction with Co-Diovan 320/12.5 mg after at least 4 weeks of treatment.
Co-Diovan should be administered consistently with or without food (see Section 5.2 Pharmacokinetic Properties).
Renal or hepatic impairment. No dosage adjustment is required for patients with mild to moderate renal impairment (creatinine clearance > 30 mL/min). In patients with mild to moderate hepatic impairment without cholestasis the daily dose of valsartan should not exceed 80 mg (see Section 4.4 Special Warnings and Precautions for Use).
Patients with severe renal or hepatic impairment, biliary cirrhosis or cholestasis must not take Co-Diovan (see Section 4.3 Contraindications).
4.3 Contraindications
Hypersensitivity to valsartan, hydrochlorothiazide, other sulfonamide-derived medicinal products or to any of the excipients of Co-Diovan; pregnancy; severe hepatic impairment; biliary cirrhosis and cholestasis; anuria; severe renal impairment (creatinine clearance < 30 mL/min); refractory hypokalaemia, hyponatraemia, hypercalcaemia, and symptomatic hyperuricaemia; concomitant use with aliskiren in patients with type 2 diabetes mellitus (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
4.4 Special Warnings and Precautions for Use
Serum electrolyte changes. Concomitant use with potassium supplements, potassium-sparing diuretics, salt substitutes containing potassium, or other drugs that may increase potassium levels (heparin, trimethoprim containing medicines etc.) should be used with caution. Thiazide diuretics can precipitate new onset hypokalaemia or exacerbate pre-existing hypokalaemia. Thiazide diuretics should be administered with caution in patients with conditions involving enhanced potassium loss, for example salt losing nephropathies and prerenal (cardiogenic) impairment of kidney function. If hypokalaemia is accompanied by clinical signs (e.g. muscular weakness, paresis, or ECG alterations), Co-Diovan should be discontinued. Correction of hypokalaemia and any coexisting hypomagnesaemia is recommended prior to the initiation of thiazides. Potassium and magnesium serum concentrations should be checked periodically. All patients receiving thiazide diuretics should be monitored for imbalances in electrolytes, particularly potassium.
Regular monitoring of serum sodium concentrations is recommended. Treatment with thiazide diuretics, including hydrochlorothiazide, has been associated with hyponatraemia and hypochloraemic alkalosis. Hyponatraemia, accompanied by neurological symptoms (nausea, progressive disorientation, apathy) has been observed in isolated cases. Thiazides, including hydrochlorothiazide, increase the urinary excretion of magnesium, which may result in hypomagnesaemia. Calcium excretion is decreased by thiazide diuretics. This may result in hypercalcaemia.
Periodic determination of serum electrolytes should be performed at appropriate intervals.
Sodium and/or volume depleted patients. In severely sodium-depleted and/or volume-depleted patients, such as those receiving high doses of diuretics, symptomatic hypotension may occur in rare cases after initiation of therapy with Co-Diovan. Sodium and/or volume depletion should be corrected before starting treatment with Co-Diovan.
If hypotension occurs, the patient should be placed in the supine position and, if necessary, given an intravenous infusion of normal saline. Treatment can be continued once the blood pressure has stabilised.
Patients with severe chronic heart failure or other conditions with stimulation of the renin-angiotensin-aldosterone-system. In patients whose renal function may depend on the activity of the renin-angiotensin aldosterone system (e.g. patients with severe heart failure), treatment with angiotensin converting enzyme inhibitors has been associated with oliguria and/or progressive azotaemia and in rare cases with acute renal failure. The use of Co-Diovan in patients with severe heart failure has not been established. Hence it cannot be excluded that because of the inhibition of the renin-angiotensin aldosterone system the use of Co-Diovan may as well be associated with impairment of the renal function. Co-Diovan should not be used in these patients.
Renal artery stenosis. There is an increased risk of severe hypotension and renal insufficiency when patients with unilateral or bilateral renal artery stenosis or stenosis to a solitary kidney are treated with agents that affect the renin angiotensin aldosterone system. Co-Diovan should be used with caution, since blood urea and serum creatinine may increase in such patients.
Primary hyperaldosteronism. Patients with primary hyperaldosteronism will not generally respond to antihypertensive drugs acting through the renin angiotensin aldosterone system therefore use of Co-Diovan in these patients is not recommended.
Aortic and mitral valve stenosis, hypertrophic obstructive cardiomyopathy. As with all other vasodilators, special caution is indicated when using Co-Diovan in patients with haemodynamically relevant aortic or mitral stenosis, or hypertrophic obstructive cardiomyopathy (HOCM).
Angioedema. Angioedema, including swelling of the larynx and glottis, causing airway obstruction and/or swelling of the face, lips, pharynx and/or tongue has been reported in patients treated with valsartan; some of these patients previously experienced angioedema with other drugs including ACE inhibitors. Co-Diovan should be immediately discontinued in patients who develop angioedema, and should not be readministered.
Dual blockade of the renin-angiotensin system (RAS). Caution is required while coadministering angiotensin receptor antagonists (ARBs), including valsartan, with other agents blocking the RAS such as ACE inhibitors or aliskiren (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Systemic lupus erythematosus. Thiazide diuretics, including hydrochlorothiazide, have been reported to exacerbate or activate systemic lupus erythematosus.
Other metabolic disturbances. Thiazide diuretics, including hydrochlorothiazide, may alter glucose tolerance and raise serum levels of cholesterol, triglycerides and uric acid. Like other diuretics, hydrochlorothiazide, may raise the serum uric acid level due to reduced clearance of uric acid and may cause or exacerbate hyperuricaemia and precipitate gout in susceptible patients.
Thiazides decrease urinary calcium excretion and may cause mild elevation of serum calcium in the absence of known disorders of calcium metabolism. Since hydrochlorothiazide can increase serum calcium concentrations, it should be used with caution in patients with hypercalcaemia. Marked hypercalcaemia unresponsive to thiazide withdrawal or ≥ 12 mg/dL may be evidence of an underlying thiazide independent hypercalcaemic process.
Pathological changes in the parathyroid gland of patients with hypercalcaemia and hypophosphataemia have been observed in a few patients on prolonged thiazide therapy. If hypercalcaemia occurs, further diagnostic clarification is necessary.
Choroidal effusion, acute myopia and secondary angle-closure glaucoma. Hydrochlorothiazide, a sulfonamide, has been associated with an idiosyncratic reaction resulting in choroidal effusion with visual field defect, acute transient myopia and acute angle-closure glaucoma. Symptoms include acute onset of decreased visual acuity or ocular pain and typically occur within hours to week of a drug initiation. Untreated acute angle-closure glaucoma can lead to permanent vision loss.
The primary treatment is to discontinue hydrochlorothiazide as rapidly as possible. Prompt medical or surgical treatment may need to be considered if the intraocular pressure remains uncontrolled. Risk factors for developing acute angle-closure glaucoma may include a history of sulfonamide or penicillin allergy.
Photosensitivity. Cases of photosensitivity reactions have been reported with thiazide diuretics. If photosensitivity reaction occurs during treatment, it is recommended to stop the treatment. If readministration of the diuretic is deemed necessary, it is recommended to protect exposed areas to the sun or to artificial UVA.
General. Hypersensitivity reactions to hydrochlorothiazide are more likely in patients with allergy and asthma.
Non-melanoma skin cancer. An increased risk of non-melanoma skin cancer [basal cell carcinoma (BCC) and squamous cell carcinoma (SCC)] with increasing cumulative dose of hydrochlorothiazide exposure has been observed in two epidemiological studies based on the Danish National Cancer Registry. The risk for non-melanoma skin cancer appears to increase with long-term use (see Section 5.1 Pharmacodynamic Properties). Photosensitizing actions of hydrochlorothiazide could act as a possible mechanism for non-melanoma skin cancer.
Patients taking hydrochlorothiazide should be informed of the risk of non-melanoma skin cancer and advised to regularly check their skin for any new lesions and promptly report any suspicious skin lesions. Possible preventive measures such as limited exposure to sunlight and UV rays and, in case of exposure, adequate protection should be advised to the patients in order to minimize the risk of skin cancer. Suspicious skin lesions should be promptly examined, potentially including histological examination of biopsies. The use of hydrochlorothiazide may also need to be reconsidered in patients who have previously experienced non-melanoma skin cancer (see Section 4.8 Adverse Effects (Undesirable Effects)).
Acute respiratory toxicity. Very rare severe cases of acute respiratory toxicity, including acute respiratory distress syndrome (ARDS) have been reported after taking hydrochlorothiazide. Pulmonary oedema typically develops within minutes to hours after hydrochlorothiazide intake. At the onset, symptoms include dyspnoea, fever, pulmonary deterioration and hypotension. If diagnosis of ARDS is suspected, Co-Diovan should be withdrawn and appropriate treatment given. Hydrochlorothiazide should not be administered to patients who previously experienced ARDS following hydrochlorothiazide intake.
Use in hepatic impairment. In patients with mild to moderate hepatic impairment without cholestasis Co-Diovan should be used with caution (see Section 5.2 Pharmacokinetic Properties, Pharmacokinetics in patients with hepatic impairment). Patients with severe hepatic impairment, biliary cirrhosis or cholestasis should not take Co-Diovan (see Section 4.3 Contraindications).
Thiazides, like other diuretics, may precipitate electrolyte imbalance, hepatic encephalopathy and hepato-renal syndrome when used to treat cirrhotic ascites.
Use in renal impairment. Renal function has a marked effect on the kinetics of hydrochlorothiazide (see Section 5.2 Pharmacokinetic Properties, Pharmacokinetics in patients with renal impairment). Thiazide diuretics may precipitate azotaemia in patients with chronic kidney disease. Co-Diovan should be used with caution in patients with moderate renal impairment (creatinine clearance > 30 mL/min). Periodic checks of serum potassium, creatinine and uric acid levels are advisable.
Patients with severe renal impairment (creatinine clearance < 30 mL/min) should not take Co-Diovan (see Section 4.3 Contraindications).
Use in the elderly. See Section 4.5 Interactions with Other Medicines and Other Forms of Interactions; Section 5.2 Pharmacokinetic Properties.
Paediatric use. The safety and efficacy of Co-Diovan have not been established in children.
Effects on laboratory tests. See Section 4.4 Special Warnings and Precautions for Use, Serum electrolyte changes, Other metabolic disturbances.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Valsartan-hydrochlorothiazide. The following drug interactions may occur due to both components (valsartan and/or hydrochlorothiazide) of Co-Diovan:
Lithium. Reversible increases in serum lithium concentrations and toxicity have been reported during concomitant administration of lithium with ACE inhibitors, angiotensin II receptor antagonists or thiazides. Since renal clearance of lithium is reduced by thiazides, the risk of lithium toxicity may presumably be increased further with Co-Diovan. Therefore, careful monitoring of serum lithium concentrations is recommended during concomitant use.
Valsartan. In monotherapy with valsartan, no drug interactions of clinical significance have been found with the following drugs: cimetidine, warfarin, frusemide, digoxin, atenolol, indomethacin, hydrochlorothiazide, amlodipine, glibenclamide.
As valsartan is not metabolised to a significant extent, clinically relevant drug-drug interactions in the form of metabolic induction or inhibition of the cytochrome P450 system are not expected with valsartan. Although valsartan is highly bound to plasma proteins, in vitro studies have not shown any interaction at this level with a range of molecules which are also highly protein-bound, such as diclofenac, frusemide, and warfarin.
Combination use of ACE inhibitors or angiotensin receptor antagonist, thiazide diuretics and anti-inflammatory drugs (NSAIDs or COX-2 inhibitors). When angiotensin II antagonists are administered simultaneously with NSAIDs, attenuation of the antihypertensive effect may occur.
Furthermore, the use of an ACE inhibiting drug (ACE inhibitors) or angiotensin receptor antagonist, a thiazide diuretic (including hydrochlorothiazide), and an anti-inflammatory drug (NSAID or COX-2 inhibitor) at the same time increases the risk of renal impairment. Concomitant use of angiotensin II antagonists and NSAIDs in patients who are elderly, volume-depleted (including those on diuretic therapy) or have compromised renal function may lead to an increased risk of worsening renal function, including possible acute renal failure. This includes use in fixed combination products containing more than one class of drug. Combined use of these medications should be accompanied by increased monitoring of serum creatinine, particularly when initiating or modifying treatment.
Dual blockade of the renin angiotensin system (RAS) with ARBs, ACEIs or aliskiren. The concomitant use of ARBs, including valsartan, with other agents acting on the RAS is associated with an increased incidence of hypotension, hyperkalaemia, and changes in renal function compared to monotherapy. It is recommended to monitor blood pressure, renal function and electrolytes in patients on Co-Diovan and other agents that affect the RAS (see Section 4.4 Special Warnings and Precautions for Use).
The concomitant use of ARBs including valsartan, or ACEIs, with aliskiren is contraindicated in patients with type 2 diabetes mellitus (see Section 4.3 Contraindications).
Potassium. Concomitant use with potassium supplements, potassium-sparing diuretics, salt substitutes containing potassium or other drugs that may alter potassium levels (heparin, trimethoprim containing medicines etc.) should be used with caution and with frequent monitoring of potassium (see Section 4.4 Special Warnings and Precautions for Use, Serum electrolyte changes).
Hepatic transporters. Coadministration with inhibitors of the hepatic uptake transporter OATP1B1 (such as rifampicin, cyclosporin) or hepatic efflux transporter MRP2 (e.g. ritonavir) may increase the systemic exposure to valsartan.
Hydrochlorothiazide. Other diuretics and antihypertensive agents. The antihypertensive effect may be increased with concomitant use of other antihypertensive drugs (e.g. guanethidine, methyldopa, beta-blockers, vasodilators, calcium channel blockers). The thiazide component of Co-Diovan may enhance the hyperglycemic effect of beta-blockers and diazoxide.
Drugs used during surgery. Thiazides, including hydrochlorothiazide, potentiate the action of non-depolarising muscle relaxants (e.g. curare derivatives).
Non-steroidal anti-inflammatory drugs. Concomitant administration of NSAIDs (e.g. salicylic acid derivatives indomethacin) including selective cyclooxygenase-2 inhibitors (COX-2 inhibitors) may weaken the diuretic and antihypertensive activity of the thiazide component of Co-Diovan. Concurrent hypovolaemia may induce acute renal failure. In patients who are elderly, volume-depleted (including those on diuretic therapy), or have compromised renal function, concomitant use of angiotensin II antagonists and NSAIDs may lead to an increased risk of worsening of renal function. Therefore, monitoring of renal function is recommended when initiating or modifying the treatment in patients on valsartan who are taking NSAIDs concomitantly.
Antidiabetic agents. Thiazide diuretics, including hydrochlorothiazide, may increase blood glucose. It may prove necessary to readjust the dosage of insulin and of oral antidiabetic agents.
Digitalis glycosides. Thiazide-induced hypokalaemia or hypomagnesaemia may occur as unwanted effects, favouring the onset of digitalis-induced cardiac arrhythmias.
Hypokalaemic agents. The hypokalaemic effect of diuretics may be increased by concomitant administration of kaliuretic diuretics, amphotericin, carbenoxolone, penicillin G, salicylic acid derivatives or antiarrhythmics. If these medicinal products are to be prescribed with the hydrochlorothiazide-valsartan combination, monitoring of potassium plasma levels is advised. These medicinal products may potentiate the effect of hydrochlorothiazide on serum potassium (see Section 4.4 Special Warnings and Precautions for Use, Serum electrolyte changes).
Medicinal products affected by serum potassium disturbances. Periodic monitoring of serum potassium and ECG is recommended when Co-Diovan is administered with medicinal products affected by serum potassium disturbances (e.g. digitalis glycosides, antiarrhythmics) and the torsades de pointes inducing medicinal products (which include some antiarrhythmics), hypokalaemia being a predisposing factor to torsades de pointes.
Medicinal products affecting serum sodium level. The hyponatraemic effect of diuretics may be intensified by concomitant administration of drugs such as antidepressants, antipsychotics, antiepileptics, etc. Caution is advised in long-term administration of these drugs.
Allopurinol. Coadministration of thiazide diuretics (including hydrochlorothiazide) may increase the incidence of hypersensitivity reactions to allopurinol.
Anticholinergic agents. The bioavailability of thiazide-type diuretics may be increased by anticholinergic agents (e.g. atropine, biperiden), apparently due to a decrease in gastrointestinal motility and the stomach emptying rate. Conversely, prokinetic drugs such as cisapride may decrease the bioavailability of thiazide-type diuretics.
Pressor amines. The effect of pressor amines (e.g. noradrenaline) may be decreased.
Cholestyramine and colestipol resins. Single doses of cholestyramine or colestipol resins reduced the absorption of hydrochlorothiazide by up to 85 and 43 percent, respectively.
Corticosteroids, ACTH. Electrolyte depletion, particularly hypokalaemia, may be increased.
Treatments for gout. Coadministration of thiazide diuretics, including hydrochlorothiazide, may increase the incidence of hypersensitivity reactions to allopurinol. Thiazides may also increase serum uric acid levels, and the dose of uricosuric agents such as probenecid or sulfinpyrazone may need to be increased.
Tetracyclines. Concomitant administration of tetracyclines and thiazide diuretics increases the risk for tetracycline induced increase in urea. This interaction is probably not applicable to doxycycline.
Alcohol, anaesthetics and sedatives. Potentiation of orthostatic hypotension may occur.
Iodine contrast media. In case of diuretic-induced dehydration, there is an increased risk of acute renal failure, especially with high doses of the iodine product. Patients should be rehydrated before the administration.
Other interactions. Coadministration of thiazide diuretics, including hydrochlorothiazide, may increase the risk of adverse effects caused by amantadine, and may reduce the renal excretion of cytotoxic drugs (e.g. cyclophosphamide, methotrexate) and potentiate their myelosuppressive effects.
There have been reports in the literature of haemolytic anaemia occurring with concomitant use of hydrochlorothiazide and methyldopa.
Administration of thiazide diuretics, including hydrochlorothiazide, with vitamin D or with calcium salts may potentiate the rise in serum calcium.
Concomitant treatment with cyclosporin may increase the risk of hyperuricaemia and gout-type complications.
Patients receiving hydrochlorothiazide concomitantly with carbamazepine may develop hyponatremia. Such patients should therefore be advised about the possibility of hyponatremic reactions, and should be monitored accordingly.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. The effects of valsartan and hydrochlorothiazide in combination and hydrochlorothiazide alone on fertility have not been investigated.
Fertility of male and female rats was not affected at oral doses of valsartan up to 200 mg/kg/day, with plasma concentrations approximately 2 times the concentrations achieved in humans (based on AUC) at the maximum recommended dose.
Use in pregnancy. (Category D)
Co-Diovan should not be used during pregnancy (see Section 4.3 Contraindications) or in women planning to become pregnant. Physicians prescribing any agents acting on the RAAS should counsel women of childbearing potential about the potential risk of these agents during pregnancy. If pregnancy is detected during therapy, Co-Diovan should be discontinued as soon as possible.
Drugs that act on the renin-angiotensin-aldosterone system (RAAS) can cause fetal and neonatal morbidity and death when administered to pregnant women. Several dozen cases have been reported in the world literature in patients who were taking angiotensin converting enzyme inhibitors (a specific class of drugs acting on the RAAS).
Due to the mechanism of action of angiotensin II antagonists, a risk to the fetus cannot be excluded. The use of drugs that act directly on the renin-angiotensin-aldosterone system (RAAS) during the second and third trimesters of pregnancy has been associated with fetal and neonatal injury, including hypotension, neonatal skull hypoplasia, anuria, reversible or irreversible renal failure and death. In addition, in retrospective data, first trimester use of ACE inhibitors has been associated with a potential risk of birth defects. Intrauterine exposure to thiazide diuretics, including hydrochlorothiazide, is associated with fetal or neonatal thrombocytopenia, and may be associated with other adverse reactions that have occurred in adults. There have been reports of spontaneous abortion, oligohydramnios and newborn renal dysfunction when pregnant women have inadvertently taken valsartan. In case of accidental exposure to ARB therapy, appropriate foetal monitoring should be considered. Infants whose mothers have taken ARB therapy should be closely observed for hypotension.
There was no evidence of teratogenicity in mice, rats and rabbits dosed with the valsartan/hydrochlorothiazide combination during organogenesis at up to 600/187.5, 200/62.5 and 100/3.125 mg/kg/day PO, respectively. Fetotoxicity was observed in association with maternal toxicity in rats and rabbits at valsartan/hydrochlorothiazide doses of 200/62.5 mg/kg/day and 100/3.125 mg/kg/day. Decreased fetal weights, absent renal papillae and delayed ossification were observed in rats and increased late resorptions in rabbits.
No teratogenic effects were observed when valsartan alone was administered orally to mice and rats at a dose of 600 mg/kg/day and to rabbits at a dose of 10 mg/kg/day during the period of organogenesis. However, foetal losses were observed at the highest dose level in rabbits, and foetal weight was reduced at 600 mg/kg/day in rats and at 5 mg/kg/day in rabbits.
Administration of 600 mg/kg/day valsartan to rats prior to parturition and during lactation caused a decrease in birth weight, a reduction in postnatal growth and survival, and a slight delay in physical development of the offspring. A reduction of red blood cell parameters and evidence of changes in renal haemodynamics were observed at 200-600 mg/kg/day.
Use in lactation. It is not known whether valsartan is excreted in human milk. Valsartan was excreted in the milk of lactating rats. Hydrochlorothiazide crosses the placenta and is excreted in human milk. Thus, it is not advisable to use Co-Diovan in breastfeeding mothers.
There are no studies with the valsartan/hydrochlorothiazide combination in lactating animals. A peri/postnatal study in rats with valsartan showed reductions in postnatal growth and survival, and a slight delay in physical development of the offspring when valsartan was administered to rats prior to parturition and during lactation at 600 mg/kg/day. No effects were observed at 200 mg/kg/day.
4.7 Effects on Ability to Drive and Use Machines
When driving vehicles or operating machinery, it should be taken into account that occasionally dizziness may occur during treatment of hypertension.
4.8 Adverse Effects (Undesirable Effects)
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
Co-Diovan has been evaluated for safety in more than 5,700 patients. Adverse experiences have generally been mild and transient in nature.
The following table of adverse experiences is based on five controlled trials involving a total of 7,616 patients (study protocols 201, 301, 19, C2301 and C2302). Of the 7,616 patients receiving valsartan in combination with hydrochlorothiazide, 4,372 received one of the marketed doses. All adverse experiences showing an incidence of 1% or more in the Co-Diovan group are included in Table 1, irrespective of their causal association with the study drug.
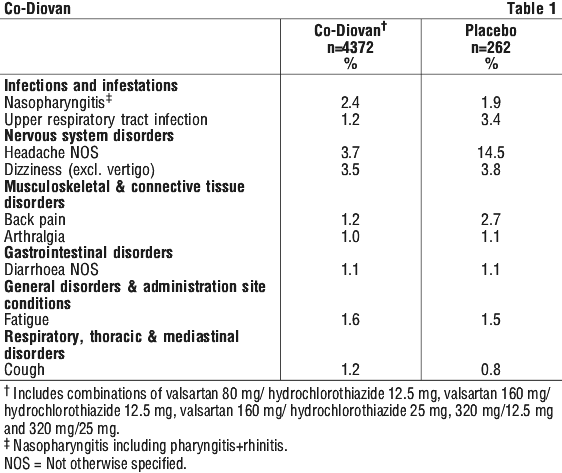
Postmarketing data. Very rare cases of angioedema, rash, pruritus, and other hypersensitivity/allergic reactions including serum sickness, and vasculitis have been reported. Very rare cases of impaired renal function, and myalgia have also been reported. Several cases of hydrochlorothiazide-induced pulmonary oedema with granulocytic infiltration and IgG deposition in alveolar membranes have been reported. Noncardiogenic pulmonary oedema may be an immunologically mediated rare idiosyncratic reaction to hydrochlorothiazide. Very rare cases of thrombocytopenia have been reported.
Laboratory findings. A greater than 20% decrease in serum potassium was observed in 3.7% of patients receiving Co-Diovan as compared to placebo (3.1%) (see Section 4.4 Special Warnings and Precautions for Use, Serum electrolyte changes).
Elevations in creatinine and blood urea nitrogen (BUN) occurred in 1.9% and 14.7%, respectively, of patients taking Co-Diovan and 0.4% and 6.3%, respectively, given placebo in controlled clinical trials.
Neutropenia was observed in 0.1% of patients treated with Co-Diovan versus 0.4% of patients treated with placebo.
Additional information on the individual components. Valsartan. Other adverse experiences that occurred in controlled clinical trials of patients treated with valsartan (> 0.2% of valsartan patients) are listed below. It cannot be determined whether these events were causally related to valsartan.
Blood and lymphatic system. Decrease in haemoglobin, decrease in haematocrit.
Body as a whole. Oedema, allergic reactions and asthenia.
Cardiovascular. Palpitations.
Dermatologic. Pruritus and rash.
Gastrointestinal. Abdominal pain, constipation, diarrhoea, dry mouth, dyspepsia and flatulence.
Infections and infestations. Viral infections, pharyngitis, sinusitis, upper respiratory tract infection.
Metabolism and nutrition. Increase of serum potassium.
Musculoskeletal. Back pain, muscle cramps, arthralgia and myalgia.
Neurologic and psychiatric. Anxiety, insomnia, paraesthesia and somnolence, neuralgia, libido decrease.
Respiratory. Dyspnoea.
Special senses. Vertigo.
Urogenital. Impotence.
Other reported events seen less frequently in clinical trials included other hypersensitivity reactions including serum sickness, vasculitis, thrombocytopenia, acute renal failure, chest pain, syncope, anorexia, vomiting, dizziness, headache, nausea, rhinitis and angioedema.
During the postmarketing period of valsartan there have been reports of dermatitis bullous, elevated liver enzymes and very rare reports of hepatitis. There have also been very rare cases of bleeding. Rare cases of rhabdomyolysis have been reported in patients receiving angiotensin II receptor blockers.
Hydrochlorothiazide. Hydrochlorothiazide has been extensively prescribed for many years, frequently in higher doses than those contained in Co-Diovan. The following adverse reactions have been reported in patients treated with thiazide diuretics alone, including hydrochlorothiazide.
Very common. Mainly at higher doses, hypokalaemia, blood lipids increased.
Common. Hyponatraemia, hypomagnesaemia, hyperuricaemia, urticaria and other forms of rash, loss of appetite, mild nausea and vomiting, postural hypotension, which may be aggravated by alcohol, anaesthetics or sedatives, impotence, electrolyte and metabolic disorders (see Section 4.4 Special Warnings and Precautions for Use).
Rare. Hypercalcaemia, hyperglycaemia, glycosuria and worsening of diabetic metabolic state, photosensitisation, abdominal distress, constipation, diarrhoea and gastrointestinal discomfort, intrahepatic cholestasis or jaundice, cardiac arrhythmias, headache, dizziness or lightheadedness, sleep disturbances, depression, paraesthesia, disturbances of vision and thrombocytopenia, sometimes with purpura.
Very rare. Hypochloraemic alkalosis, necrotising vasculitis and toxic epidermal necrolysis, cutaneous lupus erythematosus-like reactions, reactivation of cutaneous lupus erythematosus, pancreatitis, leukopenia, agranulocytosis, bone marrow depression, haemolytic anaemia, hypersensitivity reactions, respiratory distress including pneumonitis and pulmonary oedema. Acute respiratory distress syndrome (see Section 4.4 Special Warnings and Precautions for Use).
Adverse drug reactions from postmarketing experiences. The following adverse drug reactions have been identified based on postmarketing experiences. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequencies. Therefore the frequency assigned is 'not known'.
Frequency not known. Acute renal failure, renal disorder, aplastic anemia, erythema multiforme, pyrexia, muscle spasm, asthenia, acute angle-closure glaucoma.
With hydrochlorothiazide. Frequency not known. Non-melanoma skin cancer (Basal cell carcinoma and Squamous cell carcinoma). Based on available data from epidemiological studies, cumulative dose dependent association between hydrochlorothiazide and non-melanoma skin cancer has been observed (see Section 4.4 Special Warnings and Precautions for Use; Section 5.1 Pharmacodynamic Properties).
Eye disorders. Choroidal effusion, acute myopia (frequency not known). Cases of choroidal effusion with visual field defect have been reported after the use of thiazide diuretics.
4.9 Overdose
Overdose with valsartan may result in marked hypotension, which could lead to depressed level of consciousness, circulatory collapse and/or shock. In addition, the following signs and symptoms may occur due to an overdose of the hydrochlorothiazide component: dizziness, nausea, somnolence, hypovolaemia, hypotension and electrolyte disturbances associated with cardiac arrhythmias and muscle spasms.
If the ingestion is recent, a sufficient amount of activated charcoal should be administered. Otherwise, the usual treatment would be intravenous infusion of normal saline solution.
Valsartan cannot be eliminated by means of haemodialysis because it is strongly bound to plasma proteins. The degree to which hydrochlorothiazide is removed by haemodialysis has not been established.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. The active hormone of the renin-angiotensin-aldosterone system (RAAS) is angiotensin II, which is formed from angiotensin I through angiotensin converting enzyme (ACE). Angiotensin II binds to specific receptors located in the cell membranes of various tissues. It has a wide variety of physiological effects, including in particular both direct and indirect involvement in the regulation of blood pressure. As a potent vasoconstrictor, angiotensin II exerts a direct pressor response. In addition, it promotes sodium retention and stimulation of aldosterone secretion.
Valsartan is an orally active, potent and specific angiotensin II (Ang II) receptor antagonist. It acts selectively on the AT1 receptor subtype, which is responsible for the known actions of angiotensin II. The AT2 receptor subtype has not been definitely shown to be associated with cardiovascular homeostasis. The increased plasma levels of Ang II following AT1 receptor blockade with valsartan may stimulate the unblocked AT2 receptor. This may counteract the effect of blocking the AT1 receptor. Valsartan does not exhibit any partial agonist activity at the AT1 receptor and about a 20,000-fold greater affinity for the AT1 receptor than for the AT2 receptor.
Valsartan does not inhibit ACE, also known as kininase II, which converts Ang I to Ang II and degrades bradykinin. Since there is no effect on ACE and no potentiation of bradykinin or substance P, angiotensin II antagonists are unlikely to be associated with cough. In clinical trials where valsartan was compared with an ACE inhibitor, the incidence of dry cough was significantly (P < 0.05) less in patients treated with valsartan than in those treated with an ACE inhibitor (2.4% versus 7.9%, respectively). In a clinical trial of patients with a history of dry cough during ACE inhibitor therapy, 19.5% of trial subjects receiving valsartan and 19.0% of those receiving a thiazide diuretic experienced cough, compared to 68.9% of those treated with an ACE inhibitor (P < 0.05). Valsartan does not bind to or block other hormone receptors or ion channels known to be important in cardiovascular regulation.
Administration of valsartan to patients with hypertension results in reduction of blood pressure without affecting pulse rate.
In most patients, after administration of a single oral dose, onset of antihypertensive activity occurs within 2 hours, and the peak reduction of blood pressure is achieved within 4-6 hours. The antihypertensive effect persists over 24 hours after administration. During repeated administration, the maximum reduction in blood pressure with any dose is generally attained within 2-4 weeks and is sustained during long-term therapy. When valsartan is combined with hydrochlorothiazide, a significant additional reduction in blood pressure is achieved.
Abrupt withdrawal of Diovan has not been associated with rebound hypertension or other adverse clinical events.
In multiple dose studies in hypertensive patients valsartan had no notable effects on total cholesterol, fasting triglycerides or fasting serum glucose. Valsartan has no uricosuric effect.
The site of action of thiazide diuretics is primarily in the renal distal convoluted tubule. It has been shown that there is a high affinity receptor in the renal cortex with the primary binding site for the thiazide diuretic action and inhibition of NaCl transport in the distal convoluted tubule. The mode of action of thiazides is through inhibition of the Na+Cl- symporter which affects mechanisms of electrolyte reabsorption. Inhibition of the Na+Cl- symporter directly increases excretion of sodium and chloride in approximately equivalent amounts. It also indirectly reduces plasma volume, with consequent increases in plasma renin activity, aldosterone secretion and urinary potassium loss, and decreases in serum potassium. The renin-aldosterone link is mediated by angiotensin II, so coadministration of an angiotensin II receptor antagonist tends to reverse the potassium loss associated with these diuretics.
Clinical trials. The combination of valsartan and hydrochlorothiazide in once daily doses ranging from 80/12.5 mg to 160/25 mg was studied in three controlled studies (19, 301 and 201) and two uncontrolled studies (11E and 31E) in patients with hypertension.
Study 19 evaluated the effect of valsartan monotherapy (80 mg and 160 mg) and valsartan 80 mg in combination with 12.5 mg or 25 mg hydrochlorothiazide. A total of 708 patients whose hypertension remained inadequately controlled after 4 weeks of treatment with valsartan 80 mg were randomised to one of four treatments for an 8-week period. Valsartan 80 mg combined with either 12.5 mg or 25 mg hydrochlorothiazide produced a greater blood pressure lowering effect than increasing the dose of valsartan to 160 mg. The additional diastolic blood pressure reduction with valsartan 80 mg/hydrochlorothiazide 12.5 mg was a statistically (p = 0.002) and clinically (3.2 mmHg) significant improvement over 80 mg valsartan.
Study 301 was a placebo controlled, randomised, double-blind study to evaluate the efficacy, safety and tolerability of once daily dosing of 25 mg or 12.5 mg hydrochlorothiazide in combination with valsartan 80 mg or 160 mg in hypertensive patients. In this study, 871 patients were randomised into one of nine treatment groups for an 8-week period. The primary efficacy variable was the mean change from baseline in trough sitting diastolic blood pressure (MSDBP). Secondary efficacy variables were mean change from baseline in trough sitting systolic blood pressure (MSSBP) and response rates, defined as the proportion of patients with SDBP < 90 mmHg at endpoint or a drop ≥ 10 mmHg from baseline.
The decrease in blood pressure with the combination of valsartan 160 mg with either 12.5 or 25 mg hydrochlorothiazide was clinically and statistically significantly greater than placebo or monotherapy with valsartan 160 mg or the corresponding dose of hydrochlorothiazide alone. A positive dose response in MSDBP, and in MSSBP was observed when either hydrochlorothiazide dose was combined with valsartan 80 mg or 160 mg. Table 2 summarises the additional blood pressure reduction seen with Co-Diovan compared to monotherapy and placebo.
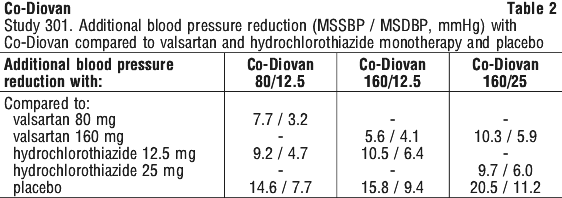
The addition of 12.5 mg hydrochlorothiazide to valsartan 160 mg resulted in additional lowering of systolic BP of 3.74 mmHg and diastolic BP of 1.65 mmHg compared to valsartan alone. The addition of 25 mg hydrochlorothiazide to valsartan 160 mg resulted in an additional lowering of 5.92 mmHg systolic BP and 3.16 mmHg diastolic BP compared to valsartan alone.
The main objective for the extension studies 11E and 31E was to obtain long-term tolerability, safety and efficacy data in adult patients with hypertension treated with valsartan and hydrochlorothiazide. Patients whose blood pressure was inadequately controlled in the extension phase of these studies could have hydrochlorothiazide 12.5 or 25 mg in addition to valsartan therapy. More than 350 patients were treated with hydrochlorothiazide in combination with valsartan for a period of one to three years.
These studies demonstrated that long-term treatment with valsartan in combination with hydrochlorothiazide was efficacious in lowering blood pressure and maintained significant antihypertensive effect in patients with hypertension, with no evidence of development of tolerance. These studies also demonstrated that long-term combination treatment was safe and well tolerated.
The combination of valsartan and hydrochlorothiazide in once daily doses of 320/12.5 mg and 320/25 mg has been shown to be efficacious in the treatment of patients with essential hypertension in a large placebo-controlled study C2301; and in the treatment of patients with essential hypertension not adequately controlled with valsartan 320 mg monotherapy in an active controlled study C2302.
Study C2301 was a multicenter, double-blind, randomized, placebo-controlled, multifactorial, 8-arm parallel design study comparing the efficacy and safety of the combination therapy of valsartan/hydrochlorothiazide (320/12.5 mg, 320/25 mg, 160/12.5 mg) to their respective monotherapies, valsartan (160 mg, 320 mg), hydrochlorothiazide (12.5 mg, 25 mg) or to placebo once daily for 8 weeks in patients with essential hypertension (MSDBP ≥ 95 mmHg and < 110 mmHg). The first week post-randomization was a forced titration period for patients randomized to the valsartan/hydrochlorothiazide 320/12.5 and 320/25 mg treatment groups. During this period, patients randomized to the valsartan/hydrochlorothiazide 320/12.5 and 320/25 mg treatment groups received valsartan/hydrochlorothiazide 160/12.5 mg, while patients randomized to the remaining six treatment groups received their respective final doses. From the second post-randomization week through the end of the study (week 8), all treatment groups received their final dose giving a minimum of 7 weeks on each of the final doses. A total of 1652 patients were enrolled into the single-blind period of the study and 1346 patients were randomized into the double-blind treatment phase. A total of 1329 patients were included in the primary efficacy population (ITT) and 1161 patients completed the study.
In patients with essential hypertension, global assessment of MSDBP and MSSBP reductions at endpoint shows that both monotherapy treatments contribute to the overall effect of the combination treatment on blood pressure reduction (p < 0.0001 for both valsartan and hydrochlorothiazide).
Statistically significant greater reductions in both MSDBP and MSSBP were observed for both valsartan/hydrochlorothiazide 320/12.5 mg and valsartan/hydrochlorothiazide 320/25 mg compared with placebo and each of the respective monotherapy doses (p < 0.0001 for all comparisons).
These results with both valsartan 320 mg/hydrochlorothiazide combinations were clinically relevant with minimum differences in MSDBP of at least 8.0 mmHg compared to placebo and at least 3.6 mmHg compared to their respective monotherapies. Similarly, the results in MSSBP were clinically relevant with minimum differences of at least 15.8 mmHg compared to placebo and at least 8.0 mmHg compared to their respective monotherapies. These results were valid across age, race and gender subgroups.
Dose-dependent hypokalaemia occurred in controlled clinical studies with valsartan + hydrochlorothiazide. Hypokalaemia occurred more frequently in patients given 25 mg hydrochlorothiazide than in those given 12.5 mg hydrochlorothiazide.
Dose-dependent orthostatic reactions were reported in < 1% of patients given a combination of valsartan + hydrochlorothiazide. A dose-dependent increase in the frequency of 'dizziness' was reported in patients treated with doses ranging from valsartan 80 mg + hydrochlorothiazide 12.5 mg to valsartan 160 mg + hydrochlorothiazide 25 mg. In a non-controlled study in which Co-Diovan 160 mg/25 mg was given for 4 weeks to patients who had not been adequately treated with valsartan 160 mg and hydrochlorothiazide 12.5 mg, total cholesterol rose from 209 to 220 mg/dL.
Beneficial effects of valsartan in combination with hydrochlorothiazide on cardiovascular mortality and morbidity are currently unknown. See Table 3.
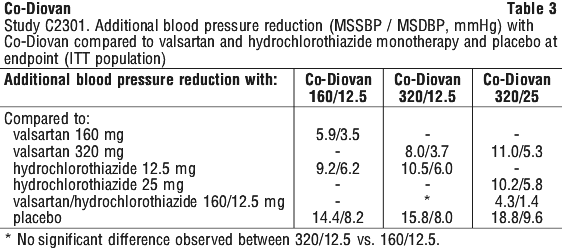
In patients whose blood pressure was not adequately controlled with valsartan monotherapy, all treatments produced reductions in MSDBP and MSSBP from baseline to endpoint. The reduction in MSDBP and MSSBP at endpoint was statistically significantly greater for the valsartan/hydrochlorothiazide 320/12.5 mg and 320/25 mg combinations than for valsartan 320 mg monotherapy (p < 0.0001).
The reductions in BP at endpoint with both valsartan/hydrochlorothiazide combinations were clinically relevant compared to valsartan monotherapy with minimum differences in MSDBP of at least 3.9 mmHg and minimum differences in MSSBP of at least 7.5 mmHg. These results were valid across age and gender subgroups.
Diastolic response rates were 74.9% in the valsartan/hydrochlorothiazide 320/25 mg and 68.8% in the valsartan/hydrochlorothiazide 320/12.5 mg groups. Both combination doses show clinically and statistically greater diastolic response rates than the valsartan monotherapy (52.7%). Similarly, diastolic control rates were significantly greater with valsartan/hydrochlorothiazide 320/25 mg and 320/12.5 mg than with valsartan monotherapy (70.6%, 65.3% and 49.8%, respectively).
These efficacy results demonstrate that patients not adequately controlled with valsartan 320 mg benefit from clinically relevant additional BP reductions when treated with the valsartan/hydrochlorothiazide combinations.
No specific studies were performed to assess the efficacy of Co-Diovan in patients inadequately controlled on hydrochlorothiazide alone, or to determine in direct comparison the difference between Co-Diovan 160/25 mg and 320/25 mg.
Non-melanoma skin cancer. Based on available data from epidemiological studies, cumulative dose-dependent association between hydrochlorothiazide and non-melanoma skin cancer has been observed. One study included a population comprised of 71,553 cases of BCC and of 8,629 cases of SCC matched to 1,430,883 and 172,462 population controls, respectively. High hydrochlorothiazide use (≥ 50,000 mg cumulative) was associated with an adjusted OR of 1.29 (95% CI: 1.23-1.35) for BCC and 3.98 (95% CI: 3.68-4.31) for SCC. A clear cumulative dose response relationship was observed for both BCC and SCC. Another study showed a possible association between lip cancer (SCC) and exposure to hydrochlorothiazide: 633 cases of lip-cancer were matched with 63,067 population controls, using a risk-set sampling strategy. A clear cumulative dose-response relationship was demonstrated with an adjusted OR 2.1 (95% CI: 1.7-2.6) increasing to OR 3.9 (3.0-4.9) for high use (~25,000 mg) and OR 7.7 (5.7-10.5) for the highest cumulative dose (~100,000 mg). For example: A 100,000 mg cumulative dose corresponds to more than 10 years' daily use with a defined daily dose of 25 mg (see Section 4.4 Special Warnings and Precautions for Use; Section 4.8 Adverse Effects (Undesirable Effects)).
5.2 Pharmacokinetic Properties
Valsartan. Peak plasma concentrations are reached 2 to 4 hours after dosing. The amount absorbed varies widely. Mean absolute bioavailability is 23% and the bioavailability relative to an oral solution is 59%.
The pharmacokinetics of valsartan are linear over the dose range 80 - 320 mg. There is no change in the kinetics of valsartan on repeated administration and little accumulation when dosed once daily. Plasma concentrations are similar in males and females.
When valsartan is given with food, the area under the plasma concentration-time curve (AUC) of valsartan is reduced by 48% although, from about 8 h postdosing, plasma valsartan concentrations are similar for the fed and fasted group.
Valsartan is highly bound to serum protein (94-97%), mainly serum albumin. Steady-state volume of distribution is low (about 17 L) indicating that valsartan does not distribute into tissues extensively.
Valsartan does not undergo extensive biotransformation. Only approximately 25% of absorbed drug is metabolised. The primary metabolite is valeryl 4-hydroxy valsartan, which is pharmacologically inactive. The enzyme(s) responsible for valsartan metabolism have not been identified.
Valsartan shows biexponential decay kinetics with a t½α of about 1 hour and a t½β of about 9.5 hours. After oral dosing, 83% of the dose is excreted in the faeces and 13% in the urine, mainly as unchanged compound. Following intravenous administration, renal clearance of valsartan accounts for about 30% of total plasma clearance. Plasma clearance is relatively slow (about 2 L/h) when compared with hepatic blood flow (about 30 L/h).
Hydrochlorothiazide. The absorption of hydrochlorothiazide after an oral dose is rapid (Tmax about 2 hours), with similar absorption characteristics for both suspension and tablet formulations. Absolute bioavailability of hydrochlorothiazide is 60-80% after oral administration.
The increase in mean AUC is linear and dose proportional in the therapeutic range. There is no change in the kinetics of hydrochlorothiazide on repeated administration, and accumulation is minimal when administered once daily.
The distribution and elimination kinetics have generally been described by a biexponential decay function, with a terminal half-life of 6-15 hours. Greater than 95% of the absorbed dose is excreted as unchanged compound in the urine.
Valsartan/hydrochlorothiazide. The systemic availability of hydrochlorothiazide is reduced by about 30% when coadministered with valsartan. Coadministration of hydrochlorothiazide decreased peak concentrations of valsartan by 13% and systemic exposure to valsartan by 17%. This observed interaction has no impact on the combined use of valsartan and hydrochlorothiazide, since controlled clinical trials have shown a clear antihypertensive effect, greater than that obtained with either drug administered alone or placebo.
Pharmacokinetics in the elderly. Exposure (measured by AUC) to valsartan is higher by 70% and the half-life is longer by 35% in the elderly compared to younger patients.
Limited data suggest that the systemic clearance of hydrochlorothiazide is reduced in both healthy and hypertensive elderly subjects compared to young healthy volunteers. No dosage adjustment of Co-Diovan is necessary in elderly patients.
Pharmacokinetics in children. The pharmacokinetics of Co-Diovan have not been investigated in children.
Pharmacokinetics in patients with renal impairment. As expected for a compound where renal clearance accounts for only 30% of total plasma clearance, there is no apparent correlation between renal function (measured by creatinine clearance) and systemic exposure to valsartan (measured by AUC) in patients with different degrees of renal failure. A trial in 5 normotensive patients undergoing haemodialysis demonstrated that complete loss of renal function does not lead to a gross increase in the exposure to valsartan and does not have a major impact on the kinetics of valsartan. This study also confirmed that valsartan is not removed from the plasma by haemodialysis.
Renal clearance of hydrochlorothiazide is composed of passive filtration and active secretion into the renal tubule. As expected for a compound which is cleared almost exclusively via the kidneys, renal function has a marked effect on the kinetics of hydrochlorothiazide (see Section 4.3 Contraindications; Section 4.4 Special Warnings and Precautions for Use).
In patients with severe renal impairment (creatinine clearance < 30 mL/min) and patients undergoing dialysis, no data are available for Co-Diovan (see Section 4.3 Contraindications).
Pharmacokinetics in patients with hepatic impairment. About 70% of the absorbed valsartan dose is excreted in the bile, mainly as unchanged compound. The AUC with valsartan has been observed to approximately double in patients with mild or moderate hepatic impairment including patients with biliary obstructive disorders (see Section 4.4 Special Warnings and Precautions for Use, Use in hepatic impairment). There are no data available on the use of valsartan in patients with severe hepatic dysfunction (see Section 4.3 Contraindications).
Hepatic disease does not significantly affect the pharmacokinetics of hydrochlorothiazide.
5.3 Preclinical Safety Data
The combination valsartan/hydrochlorothiazide was not tested for mutagenicity, clastogenicity, or carcinogenicity.
Genotoxicity. Valsartan. Genetic toxicology studies showed that valsartan does not cause gene mutation in bacteria or mammalian cells, nor does it induce chromosomal damage in vitro or in vivo.
Hydrochlorothiazide. Hydrochlorothiazide did not induce gene mutation in bacteria or chromosome damage in mammalian cells in several in vitro and in vivo assays. However positive results were obtained in a mammalian cell assay for gene mutation (mouse lymphoma cell assay) and in two other tests (sister chromatid exchange assay in Chinese hamster ovary cells and nondisjunction assay in Aspergillus nidulans). Hydrochlorothiazide enhanced the UVA-induced formation of pyrimidine dimers in vitro and in the skin of mice following oral treatment. It is therefore concluded that there is no relevant mutagenic potential in vivo, although hydrochlorothiazide could enhance the genotoxic effects of UVA light.
Carcinogenicity. Valsartan. In animal studies there was no clear evidence of carcinogenic activity when valsartan was administered in the diet to male and female mice at doses up to 160 mg/kg/day for two years, but systemic exposure (plasma AUC value) at this dose level was lower than that achieved in humans. There was no clear evidence of carcinogenic activity in male or female rats at up to 200 mg/kg/day with plasma concentrations approximately 3 times the concentrations achieved in humans (based on AUC) at the maximum recommended dose (320/25 mg).
Hydrochlorothiazide. Two-year feeding studies in mice and rats showed no evidence of carcinogenic potential in female mice at doses up to approximately 600 mg/kg/day, or in male and female rats at doses up to approximately 100 mg/kg/day. However, there was equivocal evidence for hepatocarcinogenicity in male mice treated with hydrochlorothiazide alone at approximately 600 mg/kg/day.
6 Pharmaceutical Particulars
6.1 List of Excipients
Co-Diovan 80/12.5: silica-colloidal anhydrous; crospovidone; hypromellose; magnesium stearate; cellulose-microcrystalline; macrogol 8000; talc-purified; titanium dioxide; iron oxide red; iron oxide yellow.
Co-Diovan 160/12.5: silica-colloidal anhydrous; crospovidone; hypromellose; magnesium stearate; cellulose-microcrystalline; macrogol 8000; talc-purified; titanium dioxide; iron oxide red.
Co-Diovan 160/25: silica-colloidal anhydrous; crospovidone; hypromellose; magnesium stearate; cellulose-microcrystalline; macrogol 4000; talc-purified; titanium dioxide, iron oxide red, iron oxide yellow, iron oxide black.
Co-Diovan 320/12.5: silica-colloidal anhydrous; crospovidone; hypromellose; magnesium stearate; cellulose-microcrystalline; macrogol 4000; talc-purified; titanium dioxide, iron oxide red, iron oxide black.
Co-Diovan 320/25: silica-colloidal anhydrous; crospovidone; hypromellose; magnesium stearate; cellulose-microcrystalline; macrogol 4000; talc-purified; titanium dioxide, iron oxide yellow.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Keep in the original package. Protect from moisture. Store below 30°C.
6.5 Nature and Contents of Container
Co-Diovan 80/12.5: PA/Al/PVC/Al blister packs of 7, 14, 28, 30 and 56.
Co-Diovan 160/12.5: PA/Al/PVC/Al blister packs of 7, 14, 28, 30 and 56.
Co-Diovan 160/25: PA/Al/PVC/Al blister packs of 7, 14, 28, 30 and 56.
Co-Diovan 320/12.5: PA/Al/PVC/Al blister packs of 7, 14, 28, 30 and 56.
Co-Diovan 320/25: PA/Al/PVC/Al blister packs of 7, 14, 28, 30 and 56.
Not all strengths and pack sizes may be marketed.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Active ingredients: Valsartan, hydrochlorothiazide.
Chemical structure. Valsartan.
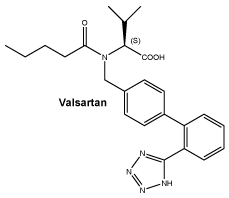
Molecular formula: C24H29N5O3.
Molecular weight: 435.5.
Chemical structure. Hydrochlorothiazide.
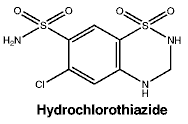
Molecular formula: C7H8ClN3O4S2.
Molecular weight: 297.72.
7 Medicine Schedule (Poisons Standard)
Schedule 4 - Prescription Only Medicine.
Date of First Approval
31 May 2005
Date of Revision
27 October 2022
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.