Crinone
Brand Information
| Brand name | Crinone |
| Active ingredient | Progesterone |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Crinone.
Summary CMI
CRINONE®
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using CRINONE?
CRINONE contains the active ingredient progesterone. CRINONE is used in IVF and ART, where luteal phase support is indicated.
For more information, see Section 1. Why am I using CRINONE? in the full CMI.
2. What should I know before I use CRINONE?
Do not use if you have ever had an allergic reaction to CRINONE or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I use CRINONE? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with CRINONE and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use CRINONE?
- CRINONE is applied directly from the applicator deep into the vagina.
- The applicator is designed to deliver a pre-measured dose of progesterone gel. Your doctor will tell you how much CRINONE to use and when to start treatment.
More instructions can be found in Section 4. How do I use CRINONE? in the full CMI.
5. What should I know while using CRINONE?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using CRINONE? in the full CMI.
6. Are there any side effects?
All medicines can have side effects. Sometimes they are serious, most of the time they are not. Tell your doctor if you experience any side effects. Most common side effects include cramps, abdominal pain, perineal pain (around the genitals and the back passage), constipation, nausea, headache, breast pain, breast enlargement, feelings of severe sadness and unworthiness, decreased sexual drive, sleepiness, feeling emotional and passing urine at night.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
CRINONE®
Active ingredient: progesterone
Consumer Medicine Information (CMI)
This leaflet provides important information about using CRINONE. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using CRINONE.
Where to find information in this leaflet:
1. Why am I using CRINONE?
2. What should I know before I use CRINONE?
3. What if I am taking other medicines?
4. How do I use CRINONE?
5. What should I know while using CRINONE?
6. Are there any side effects?
7. Product details
1. Why am I using CRINONE?
CRINONE contains the active ingredient progesterone.
Progesterone is a hormone that is produced by the ovaries during the second half of the menstrual cycle.
It is an essential hormone for preparing the uterus (womb) for pregnancy and on-going support of pregnancy.
CRINONE is used in IVF and ART, where luteal phase support is indicated.
2. What should I know before I use CRINONE?
Warnings
Do not use CRINONE if:
- you have ever had an allergic reaction to progesterone or to any of the ingredients listed at the end of this leaflet
Always check the ingredients to make sure you can use this medicine. - you have cancer of the breast and genital organs
- you have porphyria
- you have abnormal vaginal bleeding that has not been diagnosed, or is due to a recent or current missed abortion or miscarriage
- you have or have ever had blood clots or stroke
- you have liver disease or abnormal laboratory results
Check with your doctor if you:
- have any other medical conditions (i.e. depression, migraine, epilepsy, asthma, heart, kidney or liver disease)
- take any medicines for any other condition
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
CRINONE is used to support embryo implantation and maintain pregnancies through its use as part of ART treatment.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
Do not use CRINONE if you are breastfeeding.
Talk to your doctor about any concerns you may have before undergoing treatment or before you start using CRINONE.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Do not use Crinone at the same time as other vaginal preparations.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect CRINONE.
4. How do I use CRINONE?
How much to use
- The amount of CRINONE used depends on the condition being treated.
- Your doctor may prescribe one applicator of CRINONE either daily or twice daily and will advise you when to start treatment. If pregnancy occurs treatment may continue for up to 12 weeks or as directed by your doctor.
- Follow the instructions provided and use CRINONE until your doctor tells you to stop.
When to use CRINONE
- CRINONE should be used at the same time each day.
- If used twice a day, one applicator of CRINONE should be used in the morning and the other at night.
How to use CRINONE
- CRINONE is applied directly from the applicator deep into the vagina to provide a prolonged release of a natural progesterone.
- The applicator is designed to deliver a pre-measured dose of progesterone gel.
- A small amount of gel will be left in the applicator after usage. Do not be concerned because you will still be receiving the required dose.
- Follow all instructions given to you by your doctor or nurse carefully. Follow these steps:
- Wash your hands well with soap and water.
- Remove the applicator from the sealed wrapper.
- DO NOT REMOVE THE TWIST-OFF TAB AT THIS TIME.
- Hold the applicator by the thick end. Shake down several times like a thermometer to ensure that the contents are at the thin end.
- The plastic ball in the thin end helps the gel to move down to the tip of the applicator. The ball also helps to control the release of the gel. The applicator is designed so that the ball cannot exit it.
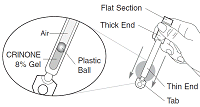
- Hold the applicator by the flat section of the thick end. Twist off the tab at the thin end of the applicator and discard it. DO NOT squeeze the thick end while twisting off the tab. This may release gel.
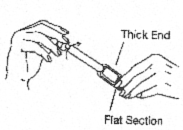
- Carefully insert the applicator into the vagina while you are in a sitting position or when lying on your back with the knees bent. Gently insert the thin end of the applicator well into the vagina.
- Squeeze the thick end of the applicator firmly to push the gel into the vagina. Remove the applicator and discard into a waste container. There may be some gel left in the applicator. Do not worry; you will still be receiving the correct dose.
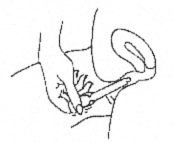
CRINONE coats the vaginal lining to provide a prolonged release of progesterone.
If you forget to use CRINONE
CRINONE should be used regularly at the same time each day. If you miss your dose at the usual time, use it as soon as you remember and then continue the same schedule as before.
Do not use more than the recommended daily dose.
If you use too much CRINONE
If you think that you have used too much CRINONE, you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26 in Australia or 0800 764 766 in New Zealand), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know while using CRINONE?
Things you should do
See your doctor regularly and keep all your doctor's appointments so your progress can be checked.
If you are about to be started on any new medicine, tell your doctor or pharmacist that you are using CRINONE.
Remind any doctor, dentist or pharmacist you visit that you are using CRINONE.
Things you should not do
- Do not stop using this medicine suddenly without telling your doctor.
- Do not change the dose unless your doctor tells you to.
- Do not give this medicine to anyone else, even if they have the same condition as you.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how CRINONE affects you.
CRINONE can make some people feel drowsy and sleepy.
If you have any of these symptoms, do not drive, operate machinery or do anything else that could be dangerous.
Looking after your medicine
- Store CRINONE below 25°C.
- Each applicator must be used once only. Use new applicator for each treatment.
Store it in a cool dry place away from moisture, heat or sunlight; for example, do not store it:
- in the bathroom or near a sink, or
- in the car or on window sills.
Keep it where young children cannot reach it.
Getting rid of any unwanted medicine
If you no longer need to use this medicine or it is out of date, take it to any pharmacy for safe disposal.
Do not use this medicine after the expiry date.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Side effects
| Side effects | What to do |
Gastrointestinal system related:
| Speak to your doctor if you have any of these side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
Allergic reactions:
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems.
In New Zealand, you can report side effects to Medsafe online at pophealth.my.site.com/carmreportnz/s/. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What CRINONE contains
| Active ingredient (main ingredient) | Progesterone |
| Other ingredients (inactive ingredients) | Hydrogenated palm glycerides Glycerol Carbomer 974P Sorbic acid Polycarbophil Sodium hydroxide Purified water Light liquid paraffin |
Do not take this medicine if you are allergic to any of these ingredients.
What CRINONE looks like
CRINONE is a soft, white to off-white gel. It is supplied in an applicator with a twist-off top. The applicator contains a plastic ball. Each applicator is sealed in a wrapper and contains a single dose of CRINONE.
Each applicator contains 1.45 g of gel and delivers a constant dose of 1.125 g of CRINONE gel containing 90 mg (8% gel) of progesterone.
CRINONE is available in boxes containing 6, 15 or 18 applicators*.
* Not all pack sizes may be available.
Australian Registration Number: AUST R 83166
Who distributes CRINONE
CRINONE is supplied in Australia by:
Merck Healthcare Pty Ltd
Suite 1, Level 1, Building B
11 Talavera Road
Macquarie Park NSW 2113
E-mail: medinfo.australia@merckgroup.com
Phone: 1800 633 463
CRINONE is supplied in New Zealand by:
Healthcare Logistics
58 Richard Pearse Drive
Airport Oaks
Auckland
E-mail: medinfo.australia@merckgroup.com
Phone: 0800 426 252
This leaflet was prepared in August 2025.
Brand Information
| Brand name | Crinone |
| Active ingredient | Progesterone |
| Schedule | S4 |
MIMS Revision Date: 01 December 2021
1 Name of Medicine
Progesterone.
2 Qualitative and Quantitative Composition
Each applicator contains 1.45 g of gel and delivers a constant dose of 1.125 g of Crinone gel containing 90 mg (8% gel) of progesterone.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Prolonged release vaginal gel with polyethylene applicator. Crinone vaginal gel has the appearance of a soft, white to off white gel.
4 Clinical Particulars
4.1 Therapeutic Indications
Crinone is used in IVF and ART, where luteal phase support is indicated.
4.2 Dose and Method of Administration
Reproductive failure and in vitro fertilisation treatment. Crinone is given at a dose of 90 mg. Crinone treatment is started within 4 days, preferably 2 days, after hCG (human chorionic gonadotropin) administration. One application of 90 mg (1.125 g, 8% gel) should be given vaginally daily or twice daily. Most women will respond to 90 mg given daily. However, some women may need 90 mg twice daily. If pregnancy occurs treatment may continue for up to 10 to 12 weeks.
Instructions for use/ handling. Crinone is administered vaginally. Remove the applicator from the sealed wrapper.
Do not remove the twist-off cap at this stage.
1. Grip the applicator firmly by the thick end. Shake down like a thermometer to ensure that the contents are at the thin end.
2. Twist off the tab and discard.
3. The applicator may be inserted into the vagina while the patient is in a sitting position or when lying on their back with knees bent. Gently insert the thin end of applicator well into the vagina.
4. Press the thick end of the applicator firmly to deposit gel. Remove the applicator and discard in a waste container.
Crinone coats the vaginal mucosa to provide prolonged release of progesterone.
4.3 Contraindications
1. Known or suspected malignancy of the breast or genital organs.
2. Missed abortion.
3. Undiagnosed uterine bleeding.
4. Liver dysfunction or disease.
5. Known hypersensitivity to any of the components of the Crinone formulation.
6. Known or suspected progesterone dependent neoplasia.
7. Active thrombophlebitis or thromboembolic disorders, cerebral apoplexy, or a history of hormone associated thrombophlebitis or thromboembolic disorders.
8. Acute porphyria.
4.4 Special Warnings and Precautions for Use
The physician should be alert to the earliest manifestations of thrombotic disorders (thrombophlebitis, cerebrovascular disorders, pulmonary embolism and retinal thrombosis). Should any of these occur or be suspected, the drug should be discontinued immediately. Patients who have risk factors for thrombotic disorders should be kept under careful observation.
Treatment should be discontinued if the results of liver function tests become abnormal or if cholestatic jaundice appears.
Progesterone and progestins have been used to prevent miscarriage in women with a history of recurrent spontaneous pregnancy losses. No adequate evidence is available to show that they are effective for this purpose.
The pre-treatment physical examination should include particular attention to the breasts and pelvic organs, and a Papanicolaou smear should be obtained.
As progestogens may cause some degree of fluid retention, a woman who has any condition that might be influenced by this factor (such as epilepsy, asthma, migraine, and cardiac or renal dysfunction) requires careful observation.
In cases of breakthrough bleeding, as with all cases of irregular vaginal bleeding, diagnostic measures may be indicated to assess whether organic disease is present.
Patients with a history of depression should be carefully observed and Crinone discontinued if the depression recurs to a serious degree.
Progestogens may worsen the manifestations of pre-existing porphyria. Therefore the use of Crinone in such patients is not recommended.
The pathologist should be advised of progestogen therapy when relevant specimens are submitted because of the influence of progestogens on the structure and pathology of organs such as the endometrium.
Crinone should not be used concurrently with other vaginal therapy (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Use in the elderly. No data available.
Paediatric use. Crinone should not be used in children.
Effects on laboratory tests. There is no evidence that Crinone has any effects on laboratory tests other than endometrial histology tests.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Although no interactions with other drugs have been reported, Crinone is not recommended for use concurrently with other vaginal preparations.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. See Section 4.1 Therapeutic Indications.
Use in pregnancy. (Category A)
Crinone has been used to successfully support embryo implantation and maintain pregnancies through its use as part of ART treatment regimens.
Use in lactation. Do not use during lactation. Detectable amounts of progestogens have been identified in the milk of mothers receiving them. The effect of this on the nursing infant has not been determined.
4.7 Effects on Ability to Drive and Use Machines
Drivers and users of machines are warned that risk of somnolence may occur. Special care should be taken if it is essential that patients drive or operate machinery while undergoing treatment with Crinone.
4.8 Adverse Effects (Undesirable Effects)
Adverse reactions are listed according to System Organ Class (SOC) in MedDRA. The corresponding category for each adverse reaction is based on the CIOMS III convention and is defined as follows:
Very Common: ≥ 1/10; Common: ≥ 1/100 to < 1/10; Uncommon: ≥ 1/1,000 to < 1/100; Rare ≥ 1/10,000 to < 1/1,000; Very Rare < 1/10,000; Not known: cannot be estimated from available data.
Clinical trials experience. In a study of 63 women with ovarian failure undergoing a donor oocyte transfer procedure receiving Crinone twice daily, treatment-emergent adverse events occurring in ≥ 5% of the women is shown below.
Body as a whole. Very common: cramps.
Common: bloating, pain.
Central and peripheral nervous system. Very common: headache.
Common: dizziness.
Gastro-intestinal. Common: nausea.
Reproductive, female. Very common: breast pain.
Common: genital moniliasis, vaginal discharge.
Skin and appendages. Common: genital pruritus.
In the second study of 139 women using Crinone once daily for luteal support while undergoing IVF procedure, treatment-emergent adverse events reported in ≥ 5% of women are shown below.
Body as a whole. Very common: abdominal pain, perineal pain.
Central and peripheral nervous system. Very common: headache.
Gastro-intestinal. Very common: constipation, nausea.
Common: diarrhoea, vomiting.
Reproductive, female. Very common: breast enlargement.
Common: dyspareunia.
Musculo-skeletal. Common: arthralgia.
Psychiatric. Very common: depression, decreased libido, nervousness and somnolence.
Urinary system. Very common: nocturia.
Post-market experience. Immune system disorders. Frequency not known: hypersensitivity reactions usually manifesting as skin rash.
Reproductive system and breast disorders. Frequency not known: intermenstrual bleeding (spotting).
General disorders and administration site conditions. Frequency not known: vaginal irritation and other mild application site reactions.
For adverse reactions identified during post-marketing surveillance, quantification of frequency has not been attempted, but most likely uncommon to very rare.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems in Australia, or at nzphvc.otago.ac.nz/reporting/ in New Zealand.
4.9 Overdose
There have been no reports of overdosage with Crinone. Acute overdosage is unlikely with this product due to the concentration-dependent, rate-limited absorption of progesterone by the vaginal epithelium and the prolonged release characteristics of the formulation. However, in case of overdosage, discontinue Crinone and treat the patient symptomatically.
For information on the management of overdose, contact the Poisons Information Centre on 131 126 (Australia) or 0800 764 766 (New Zealand).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Progesterone is a naturally occurring steroid that is secreted by the ovary, placenta and adrenal gland. In the presence of adequate oestrogen, progesterone transforms a proliferative endometrium into a secretory endometrium. Progesterone is essential for the development of decidual tissue, and the effect of progesterone on the differentiation of glandular epithelia and stroma has been extensively studied. Progesterone is necessary to increase endometrial receptivity for implantation of an embryo. Once an embryo is implanted, progesterone acts to maintain the pregnancy. Normal or near normal endometrial responses to exogenous oestrogen and progesterone have been noted in functionally agonadal women through the sixth decade of life. Progesterone administration decreases the circulatory levels of gonadotropins.
Clinical trials. In clinical studies of patients (n=99) with either partial or premature ovarian failure who were candidates to receive a donor oocyte transfer as an Assisted Reproductive Technology (ART) procedure were randomised to receive either Crinone twice daily or intramuscular progesterone 100 mg daily. The study was divided into three phases. The first phase of the study consisted of a test Pilot Cycle to ensure that the administration of transdermal estradiol and progesterone would adequately prime the endometrium to receive the donor egg. The second phase was the Donor Egg Cycle during which a fertilized oocyte was implanted. Crinone was administered beginning the evening of Day 14 of the Pilot and Donor Egg cycles. Subjects with partial ovarian function also underwent a Pre-Pilot Cycle and a Pre-Donor Egg Cycle during which time they were administered only leuprolide acetate to suppress remaining ovarian function. The Pre-Pilot Cycle, Pilot Cycle, Pre-Donor Egg Cycle, and Donor Egg Cycle each lasted approximately 34 days. The third phase of the study consisted of a 10-week treatment period to maintain a pregnancy until placental autonomy was achieved.
Sixty-one women received Crinone as part of the Pilot Cycle to determine their endometrial response. Of the 55 evaluable endometrial biopsies in the Crinone group performed on Day 25-27, all were histologically "in-phase" consistent with luteal phase biopsy specimens of menstruating women at comparable time intervals. Fifty-four women who received Crinone and had an histologically "in-phase" biopsy received a donor oocyte transfer. Among these 54 Crinone-treated women, clinical pregnancies (assessed about week 10 after transfer by clinical examination), occurred in 26 women (48%). In these 54 women, 17 women (31%) delivered a total of 25 newborns, seven women (13%) had spontaneous abortions and two women (4%) had elective abortions.
In a second study, Crinone was used in luteal phase support of women with tubal or idiopathic infertility due to endometriosis and normal ovulatory cycles, undergoing in vitro fertilisation (IVF) procedures. All women received a GnRH (gonadotropin-releasing hormone) analog to suppress endogenous progesterone, human menopausal gonadotropin and human chorionic gonadotropin. In this multi-center, open labelled study 139 women (aged 22-38 years) received Crinone once daily beginning within 24 hours of embryo transfer and continuing through 30 days post-transfer. Clinical pregnancies assessed at Day 90 post-transfer were seen in 36 (26%) of women. Thirty-two women (23%) delivered newborns and four women (3%) had spontaneous abortions.
Use of Crinone for Pre-Menstrual Tension (PMT) and Hormone Replacement Therapy (HRT) is not supported by the information provided in this product label.
5.2 Pharmacokinetic Properties
Limited pharmacokinetic data are available for Crinone, however studies have been conducted and the pharmacokinetic parameters from these studies can be seen in Tables 1 and 2.
Absorption. The bioavailability of progesterone in Crinone was determined relative to progesterone administered intramuscularly, orally and vaginally.
In one single dose parallel group study, 18 healthy, postmenopausal women received single doses of either 90 mg progesterone vaginally in Crinone 8% or, 100 mg progesterone orally in a capsule, or 100 mg progesterone vaginally in a capsule. The pharmacokinetic parameters are shown in Table 1.
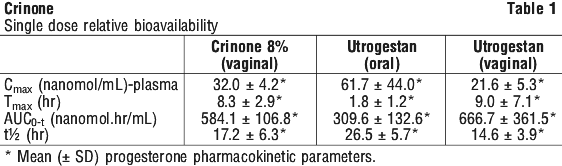
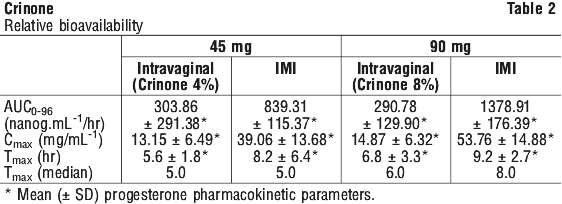
Distribution. Progesterone is extensively bound to serum proteins (≈96-99%), primarily to serum albumin and corticosteroid binding globulin.
Metabolism. The major urinary metabolite of progesterone is 5β-pregnan- 3α,20α-diol glucuronide which is present in plasma in the conjugated form only. Plasma metabolites also include 5β-pregnan-3α-ol-20-one (5β-pregnenolone) and 5α-pregnan-3α-ol- 20-one (5α-pregnenolone) which may be associated with sedation and hypnosis.
Excretion. Progesterone undergoes both biliary and renal elimination. Following an injection of labelled progesterone, 50-60% of the excretion of progesterone metabolites occurs via the kidneys and approximately 10% via the bile and faeces. Overall recovery of labelled material accounts for 70% of an administered dose, with the remainder of the dose not characterised with respect to elimination. Only a small portion of unchanged progesterone is excreted in the bile.
5.3 Preclinical Safety Data
The effect of Crinone on fertility has not been evaluated in animals.
Genotoxicity. No studies to determine the genotoxic potential of Crinone have been performed.
Carcinogenicity. No studies to determine the carcinogenic potential of Crinone have been performed. Progesterone has been shown to induce and/or promote mammary, uterine, ovarian, endometrial, cervical and vaginal tumours in experimental animals. The clinical relevance of these findings is unknown.
6 Pharmaceutical Particulars
6.1 List of Excipients
Glycerol, light liquid paraffin, hydrogenated palm glycerides, carbomer 974P, polycarbophil, sorbic acid, sodium hydroxide and purified water.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
Information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG) in Australia or on Medsafe Product Detail in New Zealand. The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
The product must be stored below 25°C.
6.5 Nature and Contents of Container
Crinone is supplied as single use, one piece, disposable, white polyethylene vaginal applicators with a twist off top in packs of 6, 15 and 18*.
Each applicator is individually wrapped and sealed in a foil over wrap.
* Not all pack sizes may be available.
6.6 Special Precautions for Disposal
Any unused medicine or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
Crinone (progesterone gel) is a bioadhesive vaginal gel which contains micronised progesterone in a diluted emulsion system, which is contained in single use, one piece polyethylene vaginal applicators.
Crinone is administered vaginally from a pre-filled applicator and is designed to provide a prolonged release of a natural progesterone into the vagina from a polycarbophil based gel.
The delivery system of Crinone is based on a vaginal moisturising formulation and provides sustained topical application of progesterone into the vagina. The Crinone delivery system is an emulsion that consists of lipophilic (lipid) and hydrophilic (aqueous) phases. The aqueous phase contains polycarbophil, a polymer that swells in the presence of water. Overall, it has a slightly negative ionic charge which produces temporary adhesion to the cell surface of the vaginal epithelium. The majority of progesterone is suspended and stored in the lipid phase while a small portion is dissolved in the aqueous phase. Absorption of progesterone occurs from the aqueous phase, which is then replenished from the lipid phase that acts as a reservoir.
Chemical structure. Natural progesterone is a hormone secreted by the corpus luteum. Progesterone is the prototype of the hormone class known as progestogens. It is chemically described as pregn-4-ene-3, 20-dione and is practically insoluble in water and soluble in most organic solvents including alcohol. Progesterone has the following chemical structure:
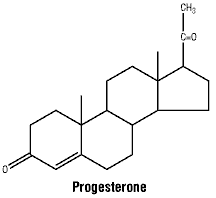
CAS number. 57-83-0.
7 Medicine Schedule (Poisons Standard)
S4 (Prescription Only Medicine).
Date of First Approval
25 September 2002
Date of Revision
02 November 2021
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.