DBL Desferrioxamine Mesylate for Injection BP
Brand Information
| Brand name | DBL Desferrioxamine Mesylate for Injection BP |
| Active ingredient | Desferrioxamine mesilate |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the DBL Desferrioxamine Mesylate for Injection BP.
Summary CMI
DBL™ Desferrioxamine Mesylate for Injection BP
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about being given this medicine, speak to your doctor or nurse.
1. Why am I being treated with DBL Desferrioxamine Mesylate for Injection BP?
DBL Desferrioxamine Mesylate for Injection BP contains the active ingredient desferrioxamine mesilate. It is used to remove excess iron from the body, after poisoning with iron-containing medicines or in certain patients with anaemia who receive many blood transfusions. For more information, see Section 1. Why am I being treated with DBL Desferrioxamine Mesylate for Injection BP? in the full CMI.
2. What should I know before treatment with DBL Desferrioxamine Mesylate for BP?
You should not be started on treatment if you have ever had an allergic reaction to desferrioxamine mesilate, or if tests show that you don't have enough iron stores in your body.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before treatment with DBL Desferrioxamine Mesylate for Injection BP? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with DBL Desferrioxamine Mesylate for Injection BP and affect how it works. A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How is DBL Desferrioxamine Mesylate for Injection BP given?
Your doctor will decide what dose you will receive and the best way for it to be given. It must only be given by a doctor or nurse (in hospital) or other trained person (at home). More instructions can be found in Section 4. How is DBL Desferrioxamine Mesylate for Injection BP given? in the full CMI.
5. What should I know while I am being treated with DBL Desferrioxamine Mesylate for Injection BP?
| Things you should do |
|
| Driving or using machines |
|
| Drinking alcohol |
|
For more information, see Section 5. What should I know while I am being treated with DBL Desferrioxamine Mesylate for Injection BP? in the full CMI.
6. Are there any side effects?
Light-headedness/dizziness, irregular heartbeat, pain/swelling/blisters at injection site, hearing problems, wee or poo colour changes, skin rash/itchiness/redness/flushing, numbness/tingling/coldness in hands, feet, arms or legs, aching joints/muscles, sight problems, nausea/vomiting, diarrhoea, stomach/abdominal cramps, difficulty urinating/weeing, bone pain, muscle cramps, headache, infection (fever, chills, sore throat, mouth ulcers), unexplained/easy bruising, nose/gum bleeds, prolonged bleeding, sudden swelling of skin, eyes, lips, throat, chest pain, breathing issues, confusion/dizziness, blueish skin colour, fatigue, seizures. Also, for patients on dialysis: personality changes, paralysis of part/all body, stiff neck, abnormal speech/eye movements.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
1. Why am I being treated with DBL Desferrioxamine Mesylate for Injection BP?
DBL Desferrioxamine Mesylate for Injection BP contains the active ingredient desferrioxamine mesilate.
DBL Desferrioxamine Mesylate for Injection BP is used to remove excess iron from the body, thereby reducing damage that excess iron may cause.
This may be necessary after poisoning with iron containing medicines or in certain patients with anaemia who receive many blood transfusions.
Desferrioxamine mesilate works by binding with the iron in the bloodstream. The bound compound can then be removed from the body.
Desferrioxamine mesilate may be used in adults and in children.
2. What should I know before I am given DBL Desferrioxamine Mesylate for Injection BP?
Warnings
You must not be given DBL Desferrioxamine Mesylate for Injection BP if:
- you are allergic to desferrioxamine mesilate.
Symptoms of an allergic reaction may include:
- shortness of breath, wheezing or difficulty breathing
- swelling of the face, lips, tongue or other parts of the body
- rash, itching or hives on the skin.
Always check the ingredients to make sure you can use this medicine.
- you do not have any excess iron stores. Your doctor will give you tests to confirm your iron levels.
Treatment with DBL Desferrioxamine Mesylate for Injection BP may affect growth in children 3 years of age and under. Talk to your doctor regarding risks and benefits of treatment in this age group and any checks that should be done to monitor weight and height.
If you are not sure whether you should be given DBL Desferrioxamine Mesylate for Injection BP, talk to your doctor, nurse or pharmacist.
Check with your doctor if you:
- have or have had any other medical conditions, especially the following:
- problems with urination, eg. kidney infection
- kidney disease eg. you are receiving dialysis
- sight or hearing problems
- any heart conditions
- the blood condition "thalassaemia"
- signs of infection, such as fever, chills, stomach pain and/or sore throat
- hyperparathyroidism (a condition resulting in excess calcium in the blood and problems with the bones) - take any medicines for any other condition.
Tell your doctor if are about to have any scans or x-rays. Your doctor may recommend that you stop or delay your treatment with DBL Desferrioxamine Mesylate for Injection BP, as it has the potential to interfere with certain scans.
If you are going to be given desferrioxamine mesilate for a prolonged period, you should have sight and hearing tests done before you start your treatment, and also a test to confirm your blood iron levels before treatment begins.
If your doctor has told you that aluminium has affected your nerves, you may be given the medicine clonazepam before you are given DBL Desferrioxamine Mesylate for Injection BP.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor if you are pregnant or intend to become pregnant.
DBL Desferrioxamine Mesylate for Injection BP is not recommended during pregnancy, especially during the first three months, unless you and your doctor have discussed the risks and benefits involved.
DBL Desferrioxamine Mesylate for Injection BP may affect your developing baby if you are given it during pregnancy. If it is necessary for you to be given this medicine, your doctor can help you decide whether you should be given it during pregnancy.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
It is not known whether DBL Desferrioxamine Mesylate for Injection BP passes into breast milk; therefore, there is a possibility that the breastfed baby may be affected.
If there is a need to consider using this medicine while you are breastfeeding, your doctor will discuss with you the benefits and risks of you being given it.
3. What if I am taking other medicines?
Tell your doctor, nurse or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with DBL Desferrioxamine Mesylate for Injection BP and affect how it works. These include:
- prochlorperazine; a medicine used for nausea
- any phenothiazines; medicines used to correct chemical imbalance in the brain and mental illness
- methyldopa; a medicine used to treat high blood pressure
- vitamin C (ascorbic acid)
- erythropoietin (used to treat anaemia)
- gallium-67; an injection given when having some nuclear medicine scans.
These medicines may be affected by DBL Desferrioxamine Mesylate for Injection BP or may affect how well it works. You may need different amounts of your medicine, or you may need to take/use different medicines. Your doctor or pharmacist will advise you.
Your doctor and pharmacist may have more information on medicines to be careful with or avoid while you are being given this medicine.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect DBL Desferrioxamine Mesylate for Injection BP.
4. How is DBL Desferrioxamine Mesylate for Injection BP given?
How much is given
Your doctor will decide what dose you will receive. This depends on your condition and other factors, such as your health and weight.
How it is given
DBL Desferrioxamine Mesylate for Injection BP must be dissolved into a solution using Water for Injections and then may be given as an injection into a muscle, under the skin or as a slow injection into a vein. It may also be given as a slow infusion (eg. as a ‘drip’) into a vein or under the skin.
If you are on peritoneal dialysis, DBL Desferrioxamine Mesylate for Injection BP may be administered as part of your dialysis fluid.
It must only be given by a doctor or nurse or another trained person.
DBL Desferrioxamine Mesylate for Injection BP is sometimes used for home infusions. If it is to be used at home, you and your carers must be trained in its safe and appropriate use before you can be given the medicine at home.
While DBL Desferrioxamine Mesylate for Injection BP should be used immediately after being dissolved into a solution, if necessary, it can be stored in a refrigerator between 2°C - 8°C for no longer than 24 hours.
How many injections will you need
Your doctor will decide how long you should continue to be treated with DBL Desferrioxamine Mesylate for Injection BP.
If you are given too much DBL Desferrioxamine Mesylate for Injection BP
As DBL Desferrioxamine Mesylate for Injection BP is given to you under the supervision of a doctor, it is very unlikely that you will receive too much.
However, if you think that you have been given too much DBL Desferrioxamine Mesylate for Injection BP and/or if you experience severe side effects, you should immediately:
- contact your doctor or nurse if you are already in hospital, or
- phone the Poisons Information Centre
(by calling 13 11 26), or - go to the Emergency Department at your nearest hospital, especially if you are receiving ongoing treatment at home.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know while I am being treated with DBL Desferrioxamine Mesylate for Injection BP?
Things you should do
Remind any doctor, nurse, pharmacist or dentist you visit that you are being treated with DBL Desferrioxamine Mesylate for Injection BP.
If you are about to be started on any new medicine, remind your doctor and pharmacist that you are being treated with this medicine.
If you become pregnant while being treated with DBL Desferrioxamine Mesylate for Injection BP, tell your doctor or pharmacist immediately.
If you are being treated with DBL Desferrioxamine Mesylate for Injection BP for a prolonged period, you should have tests to assess the amount of iron in your urine every few weeks, as advised by your doctor. Sight and hearing tests should also be repeated at three-month intervals.
If DBL Desferrioxamine Mesylate for Injection BP is given to children, it is recommended that three-monthly checks on body weight and height are done by a doctor or nurse.
Call your doctor straight away if you:
- experience visual or hearing disturbances, seizures, breathing difficulties, flushing of the skin, hives or itchy rash or feel dizzy or lightheaded.
- have symptoms of an infection where you start to feel feverish with a sore throat or stomach pains, or general discomfort or develop shortness of breath; or experience chills, fever, have pain in your back, side or groin area, feel nauseous or vomit, and have cloudy, dark, bloody or bad smelling urine, or frequent painful urination.
This is because people who have iron or aluminium overload are more vulnerable to certain types of infection.
If you get an infection, your doctor may want you to do some tests and give you some medicines to treat the infection. Your doctor may also have you stop being treated with DBL Desferrioxamine Mesylate for Injection BP until any infections clear up.
Things you should not do
Do not stop taking this medicine or change the dosage without consulting with your doctor.
Driving or using machines
Avoid driving or using any machines or tools until you know how DBL Desferrioxamine Mesylate for Injection BP affects you.
DBL Desferrioxamine Mesylate for Injection BP may cause dizziness, light-headedness and sight or hearing disturbances in some people.
Make sure you know how you react to this medicine and do not drive a car, operate machinery, or do anything else that could be dangerous.
Drinking alcohol
No information available.
Looking after your medicine
DBL Desferrioxamine Mesylate for Injection BP will usually be stored in the pharmacy or on the ward.
If you are going to be treated at home, store DBL Desferrioxamine Mesylate for Injection BP below 25°C. It is important to keep it in the carton until use, as it must be protected from light.
Store it in a cool dry place away from moisture, heat, or sunlight; for example, do not store it:
- in the bathroom or near a sink, or
- in the car or on windowsills.
Do not use this medicine after the expiry date, or if the packaging is torn or shows signs of tampering.
Keep it where young children cannot reach it.
Getting rid of any unwanted medicine
If you no longer need to be given this medicine or it is out of date, take it to any pharmacy for safe disposal.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Side effects
| Side effects | What to do |
| Speak to your doctor or nurse if you have any of these side effects and they worry you. |
| Side effects | What to do |
| Tell your doctor or nurse straight away, or go to the Emergency Department at your nearest hospital if you notice any of these side effects. These may be more serious side effects. You may need urgent medical attention. |
Tell your doctor, nurse or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side-effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/safety/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop treatment with any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What DBL Desferrioxamine Mesylate for Injection BP contains
| Active ingredient (main ingredient) | Desferrioxamine mesilate |
| Other ingredients | There are no other ingredients |
DBL Desferrioxamine Mesylate for Injection BP does not contain lactose, sucrose, gluten, tartrazine or any other azo dyes.
You should not be given this medicine if you are allergic to desferrioxamine mesilate.
What DBL Desferrioxamine Mesylate for Injection BP looks like
DBL Desferrioxamine Mesylate for Injection BP is a white to cream coloured powder.
DBL Desferrioxamine Mesylate for Injection BP is available in 2 strengths:
- 500 mg/vial (AUST R 53942)
- 2 g/vial (AUST R 73173)
Who distributes DBL Desferrioxamine Mesylate for Injection BP
Pfizer Australia Pty Ltd
Sydney NSW
Toll Free Number: 1800 675 229
www.pfizermedicalinformation.com.au
This leaflet was prepared in August 2025.
™ Trademark
Brand Information
| Brand name | DBL Desferrioxamine Mesylate for Injection BP |
| Active ingredient | Desferrioxamine mesilate |
| Schedule | S4 |
MIMS Revision Date: 01 May 2023
1 Name of Medicine
Desferrioxamine mesilate.
2 Qualitative and Quantitative Composition
Each vial of DBL Desferrioxamine Mesylate for Injection BP contains 500 mg or 2 g desferrioxamine mesilate.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Powder for injection.
DBL Desferrioxamine Mesylate for Injection BP is a sterile white to cream coloured powder or lyophilised plug for reconstitution. When reconstituted with water for injections a clear solution with a pH of 4.0 - 6.0 is produced.
4 Clinical Particulars
4.1 Therapeutic Indications
Chronic iron overload. Desferrioxamine mesilate is used to promote iron excretion in patients with iron overload as a result of multiple blood transfusions frequently used in the treatment of some chronic anaemias and thalassaemia. Long-term therapy with desferrioxamine mesilate slows accumulation of hepatic iron and retards or eliminates progression of hepatic fibrosis.
Patients under the age of 3 years with small degree of iron overload have relatively poor iron mobilisation with desferrioxamine mesilate. The drug is not normally given to such patients unless significant iron mobilisation of 1 mg or more of iron per day can be demonstrated.
Desferrioxamine mesilate is not indicated for the treatment of primary haemochromatosis as phlebotomy is the method of choice for removing excess iron in this disorder.
Acute iron poisoning. Desferrioxamine mesilate is an adjunct to, and not a substitute for, standard measures used in treating acute iron poisoning, which may include induction of emesis, gastric lavage, suction and maintenance of a clear airway, control of shock with intravenous fluids, blood, oxygen and vasopressor and correction of acidosis.
4.2 Dose and Method of Administration
Desferrioxamine mesilate may be administered intramuscularly, or via intravenous or subcutaneous infusion. When administered subcutaneously the needle should not be inserted too close to the dermis.
The presence of iron overload, preferably quantified, should be established before initiating therapy with desferrioxamine mesilate.
Chronic iron overload. In young patients with chronic iron overload the main aim of chelation therapy is to attain an iron balance and to prevent haemosiderosis. In older patients with chronic iron overload, the main aim of chelation therapy is a negative iron balance in order to slowly reduce the increased iron stores and to prevent the toxic effects of iron.
Dosage. The dosage schedule for children should be individually titrated according to the extent of iron overload. In children, the earliest age at which therapy with desferrioxamine mesilate should be undertaken is 2 to 3 years. The minimum effective dose is not known, so an initial trial of chelation therapy should be performed. To assess the response to chelation therapy, 24 hour urinary iron excretion should be monitored daily initially and the response to increasing doses of desferrioxamine mesilate established, starting with 0.5 g daily and increasing the dose until urine iron excretion reaches a plateau.
The lowest effective dose resulting in a negative iron balance should be used. In most patients daily doses of 20 to 40 mg/kg bodyweight are adequate. Higher doses should be administered only if the benefit for the patient outweighs the risk of unwanted effects associated with repeated high daily doses. Maximum doses of 80 mg/kg/day should not be exceeded. If ferritin values fall below 1000 nanogram/mL, the risk of desferrioxamine mesilate toxicity increases; it is important to monitor these patients particularly carefully and perhaps to consider lowering the total weekly dose.
Whichever route of administration is chosen, the maintenance dose selected will depend on the individual patient's iron excretion rate.
Growth retardation may result from iron overload or excessive desferrioxamine mesilate doses. If chelation is started before 3 years of age, growth must be monitored carefully and the mean daily dose should not exceed 40mg/kg (see Section 4.4 Special Warnings and Precautions for Use).
Monitoring therapy. Once the maintenance dosage has been established, urinary iron excretion rates should be assessed at intervals of a few weeks. The expected rate of excretion of iron is 10 to 20 mg/day. The patient's total iron stores can be estimated by accurate recording of the amount of iron received through transfusions, supplemented by serum ferritin determination. Iron balance can be calculated based on the amount of iron excreted in the urine; negative iron balance is considered to be achieved when the total amount of iron excreted in the urine, plus a further 50% (approximate mean iron excretion in the stools), exceeds the total iron received from blood transfusions. Chelation therapy is considered satisfactory when serum ferritin levels are close to normal values (< 300 microgram/L).
Infusion. Intravenous infusions are usually more effective than subcutaneous infusions, but slow subcutaneous administration by means of a portable, lightweight infusion pump over a period of 8 to 12 hours is regarded as effective and convenient for ambulant patients. In some patients it is possible to achieve a further increase in iron excretion by infusing the same daily dose over a 24 hour period. Desferrioxamine mesilate is not formulated to support subcutaneous bolus injection.
Patients and nurses should be warned against accelerating intravenous infusions, as an intravenous bolus of desferrioxamine mesilate may lead to flushing, hypotension and circulatory collapse (see Section 4.4 Special Warnings and Precautions for Use). Heavily iron loaded patients should receive infusions five to seven times a week as protection against iron toxicity. However, if the iron load is low, infusions may be given three to five times a week.
Intramuscular. Desferrioxamine mesilate may be injected intramuscularly, though this method is less effective than subcutaneous infusion. The maximum locally tolerated dose by intramuscular injection lies in the range 0.5 to 1.5 g. The volume of solution should be not less than 3 mL for each gram of desferrioxamine mesilate (i.e. reconstitute each 500 mg vial of DBL Desferrioxamine Mesylate for Injection BP with not less than 1.5 mL of water for injections).
Note. Ascorbic acid (approximately 200 mg daily) may be given as an adjuvant after about six months of regular chelation therapy with desferrioxamine mesilate. Ascorbic acid in doses of 150 to 250 mg daily enhances urinary iron excretion, but very high doses have been suspected of giving rise to cardiac complications or ocular toxicity (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Acute iron poisoning. Desferrioxamine mesilate is an adjunct to standard measures generally used in treating acute iron poisoning. These may include gastric lavage, induction of emesis, control of shock and correction of acidosis.
Iron levels. Plasma or serum iron should be measured three to four hours postingestion in the case of any iron preparation. Levels taken after four hours may underestimate toxicity because the subject iron may have either been distributed into tissues or be bound to ferritin. In the case of slow release or enteric coated tablets, levels should be repeated at six to eight hours as absorption may be erratic.
As a lesser priority iron binding capacity may usually be measured. Blood for plasma/ serum iron measurement should be taken before chelation therapy is commenced. The following quantities are recommended: plasma/ serum iron > 0.5 mL of blood in serum or heparinised tube (plasma from heparinised blood allows more rapid analysis); total iron binding > 2 mL of blood in serum or heparinised tube.
Iron level treatment. < 62 micromol/L for general support only; 62 to 90 micromol/L for brief chelation therapy; 90 to 180 micromol/L for vigorous support and chelation; > 189 micromol/L for vigorous support and chelation therapy, and possible exchange transfusion or haemodialysis.
Indications for chelation therapy. Desferrioxamine mesilate should be used if serum iron > 62 micromol/L or the patient has severe symptoms and serum iron is not yet available.
The endpoint of desferrioxamine therapy is indicated by the disappearance of reddish-brown coloured urine. In patients in whom reddish-brown coloured urine does not develop, the endpoint for chelation therapy occurs when serum iron concentration falls to less than 54 micromol/L (300 microgram/100 mL).
To eliminate iron that has already been absorbed, desferrioxamine mesilate should be given either intramuscularly or, preferably, intravenously. The dosage and route of administration should be adapted to the severity of the poisoning, preferably by reference to the serum iron concentrations and total iron binding capacity, which should be monitored regularly. Facilities for monitoring serum iron should be available round the clock. In addition, the total amount of iron ingested and remaining in the gastrointestinal tract should be taken into account.
If the patient is normotensive, desferrioxamine mesilate may be given in a single intramuscular dose: 2 g for an adult and 1 g for a child. However, intravenous infusion is preferable since the rate of administration can be controlled and adapted to the patient's condition.
If the patient is hypotensive, the intravenous route is recommended. The maximum rate for intravenous administration is 15 mg/kg/hour and is reduced after four to six hours so that the total intravenous dose in general does not exceed 80 mg/kg/24 hours. However, in an adult patient with severe iron poisoning, an infusion of desferrioxamine mesilate 37.1 g over 52 hours has been tolerated without apparent unwanted effects.
Therapy should be continued until the serum iron concentrations are less than the total iron binding capacity. The effectiveness of treatment is dependent on an adequate output of urine in order to ensure that the iron complex ferrioxamine is excreted from the body. If oliguria or anuria develop, peritoneal dialysis or haemodialysis may become necessary to remove ferrioxamine.
It should be noted that the serum iron level may rise sharply when the iron is released from the tissues.
Desferrioxamine test. This test is based on the principle that in normal subjects desferrioxamine mesilate is incapable of raising iron excretion above a certain limit.
Normal renal function. Desferrioxamine mesilate 500 mg should be injected intramuscularly. The urine should then be collected for a period of six hours and its iron content determined. An excretion of 1 to 1.5 mg (18 to 27 micromol) during this six hour period is suggestive of iron overload; values of more than 1.5 mg (27 micromol) can be regarded as definitely pathological. The test yields reliable results only in cases where renal function is normal.
Renal failure. In patients with terminal renal failure receiving haemodialysis, serum iron values should be determined before and after the administration of desferrioxamine mesilate 500 mg intramuscularly or intravenously. A continuous increase in serum iron during the following hours is suggestive of overload.
Dosage adjustment. Treatment in patients with terminal renal failure. The iron complex is dialysable. In patients with renal failure, its elimination can be increased by dialysis. Administration of desferrioxamine mesilate may precipitate aluminium toxicity in patients on dialysis.
In patients on maintenance haemodialysis or haemofiltration, desferrioxamine mesilate doses between 1 and 4 g per week have proven effective.
Method of administration. Preparation and administration of solution. For parenteral administration, DBL Desferrioxamine Mesylate for Injection BP should be reconstituted with water for injections (5 mL for the 500 mg vial and 20 mL for the 2 gram vial) to produce an approximate 10% solution (see below). However for IM administration, each 500 mg vial of DBL Desferrioxamine Mesylate for Injection BP may be reconstituted with not less than 1.5 mL of water for injections. The drug should be completely dissolved to produce a clear solution before use. DBL Desferrioxamine Mesylate for Injection BP 500 mg vials reconstituted with 5 mL will yield desferrioxamine mesilate concentrations of 93.5 mg/mL. (The displacement volume of DBL Desferrioxamine Mesylate for Injection BP is approximately 7% when reconstituted with 5 mL of Water for Injections).
For intravenous infusion, further dilution may be performed with 0.9% sodium chloride intravenous infusion, 5% glucose intravenous infusion or Ringer's lactate intravenous infusion at a concentration of 1 to 8 mg/mL, although these should not be used as solvents for the dry substance. For subcutaneous administration, the reconstituted solution may be given undiluted.
Dissolved desferrioxamine mesilate can also be added to the dialysis fluid and given intraperitoneally to patients on chronic ambulatory peritoneal dialysis or continuous cycling peritoneal dialysis.
Desferrioxamine is sometimes used for home infusions. If home use is to be instituted, it is important that patients and families be fully instructed on the safe and appropriate technique of administration.
4.3 Contraindications
DBL Desferrioxamine Mesylate for Injection BP is contraindicated in patients with a known hypersensitivity to desferrioxamine (except where desensitisation proves possible) and in patients with an absence of excess iron stores.
4.4 Special Warnings and Precautions for Use
Flushing of the skin, urticaria, hypotension and shock have been reported when desferrioxamine mesilate was administered by rapid intravenous injection. Therefore, DBL Desferrioxamine Mesylate for Injection BP should be given intramuscularly or by slow subcutaneous or slow intravenous infusion. The maximum rate for intravenous infusion should not exceed 15 mg/kg/hour.
Injection site reactions have been reported following subcutaneous, intravenous and intramuscular administration of desferrioxamine.
Acute fatal pulmonary injury has been reported in patients receiving high dose continuous intravenous infusions of desferrioxamine. The cases were clinically manifested as acute adult respiratory distress syndrome (ARDS), with respiratory failure, hypoxia, pulmonary oedema, low pulmonary compliance and pulmonary capillary wedge pressures below 18 mmHg. The respiratory distress developed 32 to 72 hours after commencing the infusion. Therefore caution should be taken in patients receiving high dose continuous intravenous infusions of desferrioxamine.
Acute respiratory distress syndrome has been described following treatment with excessively high IV doses of desferrioxamine in patients with acute iron intoxication, and also in thalassaemic patients. The recommended daily doses should therefore not be exceeded.
It has been reported that iron overload disorder may cause the patient to have an increased susceptibility to infectious diseases. In some cases the use of desferrioxamine has promoted the development of infections, notably with micro-organisms that are iron dependent such as Yersinia enterocolitica, Yersinia pseudotuberculosis, Pneumocystis carinii and Staphylococcus aureus. If a patient, while undergoing treatment with desferrioxamine mesilate, develops pyrexia accompanied by acute enteritis/ enterocolitis, diffuse abdominal pain or pharyngitis, the treatment should be discontinued, appropriate bacteriological tests performed, and suitable antibiotic therapy instituted immediately. Desferrioxamine mesilate treatment may be recommenced once the infection resolves.
Rare reports of severe fungal infections (e.g. cases of mucormycosis or infection with Pneumocystis carinii or Rhizopus) have been documented in patients undergoing haemodialysis while receiving desferrioxamine mesilate, some with fatal outcome. Although a causal relationship with the medicine has not been firmly established, the known suppressant effect of desferrioxamine mesilate on lymphocytes may have been a contributing factor. If any characteristic signs or symptoms occur desferrioxamine mesilate treatment should be discontinued, mycological tests carried out and appropriate treatment immediately instituted. Mucormycosis has been reported to occur in dialysis patients not receiving desferrioxamine mesilate, thus no causal link with the use of the medicinal product has been established.
Visual and auditory disturbances have been reported when desferrioxamine mesilate has been administered over prolonged periods of time, particularly when the doses used were higher than those recommended or in patients with low ferritin levels. Patients with renal failure who are receiving maintenance dialysis and have low ferritin levels may be particularly prone to adverse reactions, visual symptoms having been reported after single doses of desferrioxamine.
The visual disturbances observed have been blurring of vision, cataracts after prolonged desferrioxamine therapy for chronic iron storage disease, decreased visual acuity including visual loss, impaired peripheral, colour and night vision and retinal pigmentary abnormalities. The auditory abnormalities reported have been tinnitus and hearing loss including high frequency sensorineural hearing loss, and occasionally deafness. In most cases, both ocular and auditory disturbances were reversible upon immediate cessation of treatment.
Ophthalmological and audiological tests should therefore be carried out before starting treatment with desferrioxamine mesilate, as well as at intervals of about three months during the treatment. By keeping the ratio of the mean daily dose (mg/kg of desferrioxamine) divided by the serum ferritin (micrograms/litre) below 0.025, the risk of audiometric abnormalities may be reduced in thalassaemia patients. A detailed ophthalmological assessment is recommended (visual field measurements, funduscopy, colour vision testing using pseudoisochromatic plates and the Farnsworth D-15 colour test, slit lamp investigation, visual evoked potential studies).
If disturbances of vision and/or hearing occur, the treatment with desferrioxamine mesilate should be discontinued, in order to improve the chances that the disturbances of vision and/or hearing will prove completely reversible. If treatment with desferrioxamine mesilate is later resumed with a reduced dosage, it should be done under close ophthalmological and/or audiological control and with due regard to the risk-benefit ratio.
Since desferrioxamine therapy may cause neurological effects such as dizziness, in addition to visual impairment, patients should take caution if driving a motor vehicle after treatment with desferrioxamine.
Used alone desferrioxamine mesilate may exacerbate neurological impairment in patients with aluminium-related encephalopathy. This deterioration (manifest as seizures) is probably related to an acute increase in brain aluminium secondary to elevated circulating levels. Pre-treatment with clonazepam has been shown to afford protection against such impairment.
The drug should not be given at concentrations higher than a 10% solution in water for injection as this increases the risk of local reactions by the subcutaneous route. When given intramuscularly, each gram of desferrioxamine mesilate should be made up in a volume of not less than 3 mL (see Section 4.2 Dose and Method of Administration).
Urinary excretion of parenterally administered iron has been reported to exacerbate latent pyelonephritis, this may also occur with desferrioxamine therapy. Desferrioxamine should be used with caution in patients with pyelonephritis.
Desferrioxamine mesilate has some neurotoxic effects which may be due to its ability to chelate copper or zinc. It has a suppressant effect on lymphocytes.
Excretion of the ferrioxamine complex may be associated with a reddish brown discolouration of the urine.
The use of inappropriately high doses of desferrioxamine mesilate in patients with low ferritin levels or young children (< 3 years at commencement of treatment) has also been associated with growth retardation.
Growth retardation, if associated with excessive doses of desferrioxamine mesilate, must be distinguished from growth retardation from iron overload. Growth retardation from desferrioxamine mesilate use is rare if the dose is kept below 40 mg/kg; if growth retardation has been associated with doses above this value, then reduction of the dose may result in return in growth velocity, however, predicted adult height is not attained.
Use in renal impairment. Caution is recommended in patients with severe renal failure as approximately 50% or more of the ferrioxamine formed is excreted via the kidneys. The iron complex is dialysable and its elimination can be increased by dialysis in patients with renal failure.
In patients undergoing haemodialysis who are not overloaded with iron, plasma concentrations of aluminium may rise in response to administration of desferrioxamine mesilate.
Use in the elderly. Clinical studies of desferrioxamine mesilate did not include sufficient numbers of subjects aged 65 years and over to determine whether they respond differently compared to younger subjects. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting the greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or other drug therapy.
Pediatric use. Growth should be monitored regularly in children receiving long term treatment with desferrioxamine mesilate, since impairment of growth has been documented in such children.
Three monthly checks on body weight and height are recommended in children.
Effects on laboratory tests. Blood creatinine increased.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Concurrent administration of desferrioxamine mesilate with a single dose of prochlorperazine, a phenothiazine derivative, has lead to a loss of consciousness for 48 to 72 hours, possibly because this combination of medicines removes essential iron from the nervous system. Therefore desferrioxamine mesilate and phenothiazine derivatives should not be used concomitantly.
The neuro-ophthalmic toxicity of desferrioxamine mesilate may also be potentiated by concurrent use of phenothiazines or methyldopa.
Gallium-67 imaging results may be distorted because of the rapid urinary excretion of desferrioxamine-bound radiolabel. Discontinuation of desferrioxamine mesilate 48 hours prior to scintigraphy is advised.
Vitamin C (ascorbic acid) given orally in doses of 150 to 250 mg per day improves the chelating action of desferrioxamine and increases the amount of iron excreted. However, concurrent use may cause enhancement of tissue iron toxicity, especially in the heart causing cardiac decompensation. Therefore, this regimen should be used with caution in older patients and patients with cardiac problems. The need for ascorbic acid supplementation should be completely documented by measurements of iron excretion before and after supplements, and the oral dose of ascorbic acid should be given an hour or two after the desferrioxamine infusion has been initiated when adequate concentrations of desferrioxamine have been achieved.
Ascorbic acid should not be administered until treatment with desferrioxamine mesilate has been in progress for more than a week. Monitoring of cardiac function is indicated during such combined therapy. Bilateral cataracts have also been documented in a patient on long-term combined therapy with ascorbic acid and desferrioxamine.
There is evidence that aluminium intoxication causes reduced erythropoiesis. In dialysed patients with aluminium and/or iron overload treated with desferrioxamine mesilate and erythropoietin, some dosage adjustment of the latter may be necessary. Regular monitoring of iron stores should also be carried out.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. Desferrioxamine mesilate is teratogenic in animal experiments (see Use in pregnancy).
Use in pregnancy. (Category B3)
Studies in animals have shown evidence of an increased occurrence of fetal damage, the significance of which is considered uncertain in humans.
In teratogenicity studies, desferrioxamine mesilate in daily doses up to 4.5 times the maximum human daily dose appeared to cause delayed ossification in mice and skeletal anomalies in rabbits. No adverse effects were observed in similar studies in rats. There are no adequate or well controlled studies in pregnant women. For this reason, desferrioxamine mesilate should not be administered to pregnant women (especially during the first three months of pregnancy) or to women who may become pregnant unless the potential benefits outweigh the potential risks to the fetus.
Use in lactation. It is not known whether desferrioxamine mesilate is excreted in human breast milk. Because many medicines are excreted in human milk and because of the potential for serious adverse drug effects due to desferrioxamine mesilate occurring in breastfed infants, a decision should be made either to discontinue breastfeeding or the drug, taking into account the importance of the medicine to the mother.
4.7 Effects on Ability to Drive and Use Machines
Desferrioxamine mesilate has a major influence on the ability to drive and use machines in patients experiencing CNS effects such as dizziness or impaired vision/hearing. Patients should be warned against driving or operating machinery.
4.8 Adverse Effects (Undesirable Effects)
Frequency estimate: Very common (> 1/10); common (> 1/100 to < 1/10); uncommon (> 1/1,000 to < 1/100); rare (> 1/10,000 to < 1/1,000); very rare (< 1/10,000) including isolated reports, not known (cannot be estimated from the available data).
The following adverse effects have been observed:
Many of these reactions may occur as manifestations of iron overload.
Vascular disorders. Hypotension, shock.
Cardiac disorders. Tachycardia, arrhythmia.
Respiratory, thoracic and mediastinal disorders. A pulmonary syndrome of a moderate to life-threatening nature has been reported. The patients had tachypnoea, hypoxaemia, a diffuse interstitial pattern on the chest X-ray and restrictive pulmonary dysfunction. In addition, cases of acute adult respiratory distress syndrome (ARDS), with respiratory failure, hypoxia, pulmonary oedema, low pulmonary compliance, and pulmonary arterial wedge pressures below 18 mmHg have been reported (see Section 4.4 Special Warnings and Precautions for Use).
Uncommon: asthma.
Very rare: adult respiratory distress syndrome (with dyspnoea, cyanosis and lung infiltration); following excessively high intravenous doses of desferrioxamine mesilate.
Immune system disorders. Hypersensitivity reactions occasionally occur. Rash, pyrexia and oedema and anaphylactic shock have been encountered.
Rare: anaphylactic/anaphylactoid reactions with or without shock, angioedema including laryngeal oedema.
Nervous system disorders. Headache, nervous system order (dizziness, seizure), reversible aphasia, peripheral sensory neuropathy and paraesthesia (see Section 4.4 Special Warnings and Precautions for Use).
Isolated cases: precipitation of toxic encephalopathy.
Eye disorders. Visual impairment including acute visual neurotoxicity, lenticular opacities and irreversible blindness.
Rare: vision blurred, visual acuity reduced, blindness, impairment of colour vision, night blindness, visual field defect, retinopathy (pigmentary degeneration of the retina), optic neuritis, cataract, corneal opacity, chromatopsia.
Ear and labyrinth disorders. Auditory disturbances included acute auditory neurotoxicity and irreversible loss of hearing.
Uncommon: tinnitus; hearing loss (including high frequency sensorineural hearing loss), deafness neurosensory.
Musculoskeletal and connective tissue. Bone dysplasia, characterised by circumferential metaphyseal osseous defects, sharp zones of provisional calcification and widened growth plates, and flattening of the thoracic and lumbar vertebral bodies has been reported in children receiving desferrioxamine for thalassaemia. Growth impairment especially in children.
Very common: arthralgia/myalgia.
Common: growth retardation and bone changes (e.g. metaphyseal dysplasia) are common in chelated patients given doses of 60 mg/kg especially those who begin iron chelation in the first three years of life. If doses are kept to 40 mg/kg or below, the risk is considerably reduced.
Rare: Muscle spasms and bone pain have also been reported in isolated cases.
Metabolism and nutrition disorders. Hypocalcaemia (transient), hyperparathyroidism, iron deficiency.
Blood and lymphatic system disorders. Thrombocytopenia, leukopenia, eosinophilia, aplastic anaemia and one case of fatal pancytopenia attributed to the use of desferrioxamine has been reported. Inhibition of DNA synthesis in T and B lymphocytes.
Gastrointestinal disorders. Nausea, vomiting, abdominal pain, faeces discoloured, diarrhoea.
Hepatobiliary disorders. Hepatic impairment.
Renal and urinary disorders. Renal failure, aggravation of pyelonephritis, renal tubular disorder.
Dysuria, urine colour change to orange-rose or 'vin rose colour'.
Infections and infestations. Infections caused by Yersinia enterocolitica, Yersinia pseudotuberculosis, Pneumocystis carinii, Staphylococcus aureus, Rhizopus and cases of mucormycosis may develop in patients receiving desferrioxamine (see Section 4.4 Special Warnings and Precautions for Use).
General disorders and administration site conditions. Rapid intravenous injection may be followed by localised irritation and pain, swelling and induration, pruritus, erythema and urticaria. Occasionally accompanied by pyrexia, chills and malaise (see Section 4.4 Special Warnings and Precautions for Use).
Subcutaneous administration of desferrioxamine may cause local irritation of the skin at infusion sites especially when administered in concentrations greater than 10% or doses higher than those recommended. The addition of 1 to 2 mg hydrocortisone to the desferrioxamine solution and/or dilution with additional water for injections may alleviate this problem.
Pyrexia. Uncommon: blisters and local oedema at the injection site.
Other. In some patients treated for aluminium intoxication, generalised tonic-clonic seizures, hallucination and delusion, toxic encephalopathy and hyperparathyroid bone disease have been reported on isolated occasions.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
Signs and symptoms. Tachycardia, hypotension and gastrointestinal symptoms have occasionally been reported in patients who received above average doses of desferrioxamine mesilate. Accidental administration of desferrioxamine mesilate by the intravenous route may be associated with acute but transient blindness, aphasia, agitation, headache, nausea, bradycardia, acute kidney injury and hypotension.
Acute respiratory distress syndrome has been described following treatment with excessively high IV doses of desferrioxamine in patients with acute iron intoxication, and also in thalassaemic patients.
Treatment. There is no specific antidote for desferrioxamine mesilate overdose. Signs and symptoms of overdosage may be eliminated by reducing the dosage. Desferrioxamine is dialysable. Appropriate supportive therapy should be instituted.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Desferrioxamine mesilate is a chelating agent that forms a stable complex by binding the three hydroxamic groups of the molecule to ferric ions and to a lesser degree with aluminium, copper, zinc and calcium ions. Desferrioxamine mesilate readily chelates iron from ferritin and haemosiderin but not readily from transferrin (siderophillin). However, iron recently cleared from plasma is not accessible, and iron deposits in the lungs are not removed.
Ferrioxamine, the resulting octahedral iron complex, is formed in many tissues, but mainly in plasma. This complex is stable, water soluble, and readily excreted by the kidneys. Theoretically, 1 g of desferrioxamine mesilate is capable of sequestering 85 mg of iron (in the ferric form) i.e. on a 1:1 molar basis, however, the rare complex formation appears to be pH dependent and is most rapid at acid pH. Desferrioxamine mesilate does not remove iron from haemoglobin or other haemin containing substances in the body, such as myoglobin and iron containing enzymes (i.e. cytochrome, catalases and perioxidases).
Treatment with desferrioxamine mesilate can facilitate excretion of 10 to 50 mg of iron per day from patients with iron overload. A transfusion of 500 mL whole blood provides 250 mg of iron to the body. There is a nonlinear relationship between dose of desferrioxamine mesilate and iron excreted, with reducing efficiency at higher doses.
Desferrioxamine mesilate causes the release of histamines resulting in acute hypotensive episodes following rapid intravenous administration.
Clinical trials. No data available.
5.2 Pharmacokinetic Properties
Absorption. Desferrioxamine mesilate is poorly absorbed from the gastrointestinal tract after oral administration; therefore parenteral administration is required. It is rapidly absorbed by the intramuscular and subcutaneous routes.
Distribution. Less than 10% is bound to serum proteins.
Following a single intravenous injection of desferrioxamine (10 mg/kg) in healthy subjects and in patients with transfusion induced iron overload, plasma concentrations of between 80 and 130 micromol/L were recorded after 3 minutes. These concentrations declined rapidly with a half-life of 5 to 10 minutes, and thereafter declined more slowly. The short half-life is due not only to distribution, metabolic transformation and excretion of the active substance, but also to formation of the iron complex ferrioxamine (which commences within a few minutes and proceeds to an extent which depends on the individual's iron status).
Following continuous subcutaneous or intravenous infusion of desferrioxamine (100 mg/kg in 24 mL sterile water at a rate of 1 mL/hour), the plasma concentration of desferrioxamine and ferrioxamine in healthy subjects rose to a plateau after 12 hours, i.e. to a maximum level of 20 micromol/L for desferrioxamine and 2.75 micromol/L for ferrioxamine. The corresponding values in patients were 8.3 micromol/L for desferrioxamine and 12.9 micromol/L for ferrioxamine.
Metabolism. In healthy subjects, elimination following intramuscular injection was biphasic, with first phase half-life of 1 hour for desferrioxamine and second phase half-life was 6.1 hours. Patients with haemochromatosis showed a single phase of decline with a half-life of 5.6 hours.
Excretion. Desferrioxamine is readily metabolised and/or excreted uncombined with iron by the kidneys, hence the need to maintain a constant blood level for optimal iron excretion. Within 12 hours after the intravenous administration of desferrioxamine to 20 volunteers, about 33.1% of the dose was excreted in the urine (the bulk of it in the first 3 hours) in the form of desferrioxamine and ferrioxamine, and the remainder in the form of metabolites. The corresponding figure in a patient with haemochromatosis was 60.5% of the dose. In patients with haemochromatosis, the increase in iron excretion occurring in response to desferrioxamine was approximately as high in the faeces as in the urine.
5.3 Preclinical Safety Data
Genotoxicity. No evidence of mutagenic potential has been observed in vitro.
Carcinogenicity. Long term carcinogenicity studies in animals have not been performed with desferrioxamine mesilate.
6 Pharmaceutical Particulars
6.1 List of Excipients
None.
6.2 Incompatibilities
Cloudiness or precipitation may result when desferrioxamine mesilate solutions are mixed with injectable solutions containing heparin.
0.9% Sodium chloride intravenous infusion should not be used as a solvent to reconstitute DBL Desferrioxamine Mesylate for Injection BP since it produces a hypertonic solution. However, 0.9% sodium chloride intravenous infusion may be employed, after reconstitution with water for injections, for further dilution.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C. Protect from light.
To reduce the risk of microbiological contamination, use as soon as practicable after reconstitution. If storage is necessary, hold at 2-8°C for not more than 24 hours.
6.5 Nature and Contents of Container
The powder for injections are supplied in glass vials with a bromobutyl rubber closure and aluminium seal with plastic flip-off top. DBL Desferrioxamine Mesylate for Injection BP is available as follows:
Strength and pack. 500 mg: 10 x 500 mg vials.
2 gram: 1 x 2 gram vial.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Desferrioxamine mesilate is a white to cream powder.
Chemical structure.
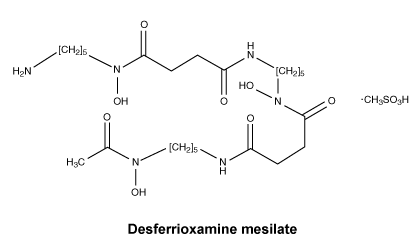
Molecular weight: 656.8.
CAS number. 138-14-7.
7 Medicine Schedule (Poisons Standard)
S4 - Prescription Only Medicine.
Date of Revision
09 January 2023
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.