Diacomit
Brand Information
| Brand name | Diacomit |
| Active ingredient | Stiripentol |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Diacomit.
Summary CMI
DIACOMIT®
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
▼ This medicine is new or being used differently. Please report side effects. See the full CMI for further details.
1. Why is my child taking DIACOMIT?
DIACOMIT contains the active ingredient stiripentol. DIACOMIT is an antiepileptic medicine. It is taken together with other antiepileptic medicines to treat a form of epilepsy called severe myoclonic epilepsy in infancy (Dravet syndrome), which affects infants and children.
For more information, see Section 1. Why is my child taking DIACOMIT? in the full CMI.
2. What should I know before my child takes DIACOMIT?
Your child must not take DIACOMIT if they have ever had an allergic reaction to stiripentol or any of the ingredients listed at the end of the CMI, or if they have ever had attacks of delirium (confused, excited, restless and/or have hallucinations).
Talk to your doctor if your child has any other medical conditions, takes any other medicines, is pregnant or could become pregnant or is breastfeeding.
For more information, see Section 2. What should I know before my child takes DIACOMIT? in the full CMI.
3. What if my child is taking other medicines?
Some medicines may interfere with DIACOMIT and affect how it works or increase the chance of side effects.
A list of these medicines is in Section 3. What if my child is taking other medicines? in the full CMI.
4. How do I give my child DIACOMIT?
The dose of DIACOMIT to give to your child is worked out by their doctor, based on your child's body weight.
It will be gradually increased over several weeks. The recommended dose is 50 mg per kg of body weight per day, split into 2 or 3 doses and taken during meals.
More instructions can be found in Section 4. How do I give my child DIACOMIT? in the full CMI.
5. What should I know while my child is taking DIACOMIT?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines | Your child should not ride bicycles, climb trees or play on playground equipment while taking DIACOMIT until they know how it affects them. DIACOMIT may make your child feel sleepy, dizzy or uncoordinated. |
| Looking after your medicine | Store DIACOMIT below 25°C in the original package in order to protect from light. |
For more information, see Section 5. What should I know while my child is taking DIACOMIT? in the full CMI.
6. Are there any side effects?
Common side effects include lack of appetite, feeling or being sick, weight loss, problems with movement and muscle strength, problems sleeping, feeling sleepy, mood changes. Serious side effects include hypersensitivity (allergic) reactions (such as rash, itching, hives on the skin; swollen face, tongue, throat or other parts of the body; shortness of breath, wheezing or problem breathing); suicidal thoughts and actions. For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
▼ This medicine is subject to additional monitoring. This will allow quick identification of new safety information. You can help by reporting any side effects you may get. You can report side effects to your doctor, or directly at www.tga.gov.au/reporting-problems.
DIACOMIT®
Active ingredient: stiripentol
Consumer Medicine Information (CMI)
This leaflet provides important information about using DIACOMIT. You should also speak to your child's doctor or the pharmacist if you would like further information or if you have any concerns or questions about using DIACOMIT.
Where to find information in this leaflet:
1. Why is my child taking DIACOMIT?
2. What should I know before my child takes DIACOMIT?
3. What if my child is taking other medicines?
4. How do I give my child DIACOMIT?
5. What should I know while my child is taking DIACOMIT?
6. Are there any side effects?
7. Product details
1. Why is my child taking DIACOMIT?
DIACOMIT contains the active ingredient stiripentol. DIACOMIT is an antiepileptic medicine.
DIACOMIT is used to treat a form of epilepsy called severe myoclonic epilepsy in infancy (Dravet syndrome), which affects infants and children. It should always be taken together with other prescribed antiepileptic medicines under the direction of a doctor.
2. What should I know before my child takes DIACOMIT?
Warnings
Your child must not take DIACOMIT if:
- they are allergic to stiripentol, or any of the ingredients listed at the end of this leaflet
- they have ever had attacks of delirium (where they become confused, excited, restless and/or have hallucinations)
Always check the ingredients to make sure your child can take this medicine.
Check with your doctor if your child:
- has any other medical conditions such as kidney or liver problems
- takes any medicine for any other condition
- has a condition called phenylketonuria (a genetic disorder) if they are taking the Powder for Suspension.
This medicine contains a source of phenylalanine which may be harmful for people with phenylketonuria, a rare genetic disorder where the body can't break down protein properly - has an intolerance to aspartame or some sugars if they are taking the Powder for Suspension
- is on a sodium-controlled diet. The capsules contain 0.16 mg sodium per 250 mg capsule and 0.32 mg sodium per 500 mg capsule. The Powder for Suspension contains 0.11 mg sodium per 250 mg sachet and 0.22 mg sodium per 500 mg sachet
During treatment, your child may be at risk of developing certain side effects. It is important you understand these DIACOMIT risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your child's doctor if your child is pregnant or could become pregnant. During pregnancy, effective antiepileptic treatment should NOT be stopped.
Talk to your child's doctor if your child is breastfeeding or intends to breastfeed. Breastfeeding is not recommended during treatment with this medicine.
3. What if my child is taking other medicines?
Tell your doctor or pharmacist if your child is taking any other medicines, including any medicines, vitamins or supplements bought without a prescription from your pharmacy, supermarket or health food shop.
Some medicines and DIACOMIT may interact with each other and affect how they work. These include:
- cisapride (used to treat symptoms of night time heartburn)
- pimozide (used to treat the symptoms of Tourette's syndrome e.g. vocal outbursts and uncontrolled, repeated movements of the body)
- ergotamine (used to treat migraine)
- dihydroergotamine (used to relieve the signs and symptoms of decreased mental capacity due to the aging process)
- halofantrine (an antimalarial treatment)
- quinidine (used to treat abnormal heart rhythms)
- bepridil (used to control chest pain)
- cyclosporine, tacrolimus, sirolimus (all three used to prevent rejections of liver, kidney and heart transplants)
- statins (simvastatin and atorvastatin, both used to reduce the amount of cholesterol in blood)
- antiepileptic medicines containing phenobarbital, primidone, phenytoin, carbamazepine, diazepam
- Medicines containing:
- midazolam or triazolam (medicines used to reduce anxiety and sleeplessness – in combination with DIACOMIT they may make your child very sleepy);
- chlorpromazine (used for mental illness such as psychosis) ;
- caffeine (this substance helps restore mental alertness) or theophylline (this substance is used in case of asthma). The combination with DIACOMIT should be avoided as it may increase their blood levels, leading to digestive disorders, racing heart and insomnia - Medicines metabolized by certain liver enzymes including:
- citalopram (used in the treatment of depressive episodes)
- omeprazole (used in case of gastric ulcer);
- HIV protease inhibitors (used in the treatment of HIV)
- astemizole, chlorpheniramine (antihistamines)
- calcium channel blockers (used in the treatment of angina or troubles of heart rhythm)
- oral contraceptives
- propranolol, carvedilol, timolol (used in the treatment of high blood pressure)
- fluoxetine, paroxetine, sertraline, imipramine, clomipramine (antidepressants)
- haloperidol (antipsychotics)
- codeine, dextromethorphan, tramadol (used in the treatment of pain)
- fluoxetine, paroxetine, sertraline, imipramine, clomipramine, citalopram
- pimozide, haloperidol, chlorpromazine
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements your child is taking and if these affect DIACOMIT.
4. How do I give my child DIACOMIT?
How much to give
- It is important that your child takes this medicine as directed by the doctor.
- Your child's doctor will tell you how much you should give them, when and how often. The dose of DIACOMIT to give to your child is worked out by their doctor, based on your child's age, weight and condition, generally 50 mg per kg bodyweight and per day.
- The dose will be gradually increased over several weeks.
- Follow the instructions provided and give DIACOMIT to your child until your doctor says they can stop taking it. Stopping DIACOMIT must be done gradually over about a month to avoid seizures coming back.
- The dose of other medication that your child is taking may be reduced when they start taking DIACOMIT. Follow the doctor's instructions carefully for these medicines also.
- Your child's doctor will monitor your child closely if they switch between taking the capsules and taking the powder for oral suspension (or the other way around), as the two forms of medicine are not identical.
When to take DIACOMIT
DIACOMIT should be given in divided doses, two or three times a day, e.g. morning and night, or morning, noon and night.
How to take DIACOMIT
The capsules should be swallowed whole with a glass of water during a meal. The capsules should not be chewed.
The powder should be mixed in a glass of water and taken straight away during a meal.
Your child must not take DIACOMIT on an empty stomach.
Your child must NOT take it with dairy products, fizzy drinks, fruit juice or food and drinks that contain caffeine, or theophylline (e.g. chocolate).
If your child vomits within the first few minutes of taking DIACOMIT, they should have a new dose, as no medicine would have been absorbed into the body.
If your child vomits more than one hour after taking the medicine then there is no need for them to have a replacement dose.
If you forget to give DIACOMIT to your child
DIACOMIT should be used regularly at the same time each day. If your child misses a dose at the usual time, they should have it as soon as you or they remember.
If it is almost time for the next dose, however, your child should skip the missed dose and take the next dose when they are meant to.
Your child should not have a double dose to make up for the dose they missed.
If your child takes too much DIACOMIT
If you think that your child has used too much DIACOMIT, they may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre by calling 13 11 26, or
- contact your child's doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know while my child is taking DIACOMIT?
Things you should do
- Tell your child's doctor or pharmacist if you think that the effect of this medicine is too strong or too weak or if your child has any side effects. The dose of DIACOMIT and the other medicines they are taking will be adjusted by the doctor according to your child's condition.
- Make sure your child keeps any appointments with the doctor or to have any blood tests. Your child's doctor will monitor liver function and blood count before starting DIACOMIT and every six months after that. They will also monitor your child's growth rate routinely.
- Remind any doctor, dentist or pharmacist your child visits that you are using DIACOMIT.
Call your doctor straight away or take your child to hospital if:
Your child has suicidal thoughts or actions. Antiepileptic drugs may cause suicidal thoughts or actions.
All mentions of suicidal thoughts or actions must be taken seriously. Families and caregivers of children and adolescents who are taking this medicine should be especially watchful for any changing behaviour.
Things you should not do
- Do not stop giving this medicine to your child suddenly. Stopping suddenly may make the seizures come back.
- Do not give DIACOMIT to anyone else, even if they have the same symptoms as your child.
Driving or using machines
Your child should not ride bicycles, climb trees or play on playground equipment until you know how DIACOMIT affects them.
DIACOMIT may make your child feel sleepy, dizzy or uncoordinated.
Looking after your medicine
- Store DIACOMIT below 25°C.
- Keep DIACOMIT in the original package in order to protect it from light.
Follow the instructions on the carton on how to take care of your medicine properly.
Store it in a cool dry place away from moisture, heat or sunlight; for example, do not store it:
- in the bathroom or near a sink, or
- in the car or on window sills
Keep it where young children cannot reach it.
A locked cupboard at least one-and-a-half metres above the ground is a good place to store medicines.
Getting rid of any unwanted medicine
If you no longer need to take this medicine or it is out of date, take it to any pharmacy for safe disposal.
Do not take this medicine after the expiry date.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
Blood
| Speak to your child's doctor if they have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
Hypersensitivity (allergic) reaction* may include:
All mentions of suicidal thoughts or actions must be taken seriously. Families and caregivers of children and adolescents who are taking this medicine should be especially watchful for any changing behaviour | Call your child's doctor straight away or take your child to hospital if you notice any of these serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making your child feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What DIACOMIT contains
| Active ingredient (main ingredient) | Stiripentol |
| Other ingredients (inactive ingredients) | 250 mg Capsule povidone
The printing ink contains
povidone
The printing ink contains
aspartame |
Do not take this medicine if you are allergic to any of these ingredients.
What DIACOMIT looks like
Capsule
Each capsule contains 250 mg or 500 mg of stiripentol.
The DIACOMIT 250 mg capsules are pink with a capsule shell that is imprinted with “Diacomit 250 mg”.
The DIACOMIT 500 mg capsules are white with a capsule shell that is imprinted with “Diacomit 500 mg”.
The 250 mg and 500 mg capsules are supplied in plastic bottles containing 60 capsules in cardboard cartons.
Powder for Oral suspension
Each sachet contains 250 mg or 500 mg of stiripentol.
The DIACOMIT 250 mg and 500 mg sachet of powder for oral suspension contains pale pink powder.
The sachets are supplied in boxes of 60 sachets.
Not all strengths or pack sizes may be available.
ARTG Numbers:
250 mg capsules: Aust R 280985
500 mg capsules: Aust R 281294
250 mg powder for oral suspension: Aust R 281460
500 mg powder for oral suspension: Aust R 281461
Who distributes DIACOMIT
DIACOMIT is supplied in Australia by:
Chiesi Australia Pty Ltd
Level 7, Suite 1, 500 Bourke Street,
Melbourne, VIC 3000
Australia
® Registered trade mark.
This leaflet was prepared in November 2025
Brand Information
| Brand name | Diacomit |
| Active ingredient | Stiripentol |
| Schedule | S4 |
▼ This medicinal product is subject to additional monitoring in Australia. This will allow quick identification of new safety information. Healthcare professionals are asked to report any suspected adverse events at www.tga.gov.au/reporting-problems.
MIMS Revision Date: 01 October 2025
1 Name of Medicine
Diacomit (stiripentol).
2 Qualitative and Quantitative Composition
Stiripentol 250 mg and 500 mg capsule.
Stiripentol 250 mg and 500 mg powder for oral suspension.
Each capsule contains either 250 mg or 500 mg stiripentol as the active ingredient.
Each sachet contains either 250 mg or 500 mg stiripentol as the active ingredient.
Excipients with a known effect in powders for oral suspensions. Aspartame and sugars.
Capsules contain no excipients with a known effect.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
250 mg capsule appears as an opaque pink capsule of size 2 with self-locking closure, imprinted with "Diacomit 250 mg".
Diacomit 500 mg capsule appears as a white capsule of size 0 with self-locking closure, imprinted with "Diacomit 500 mg".
Diacomit 250 mg and 500 mg powder for oral suspension is a pale pink powder filled in a single dose sachet.
4 Clinical Particulars
4.1 Therapeutic Indications
Diacomit is indicated for adjunctive treatment of generalised tonic-clonic and clonic seizures associated with severe myoclonic epilepsy in infancy (SMEI, also known as Dravet syndrome) in patients whose seizures are not adequately controlled with a benzodiazepine (usually clobazam) and valproate.
4.2 Dose and Method of Administration
Dosage. Prescriptions and treatment should be initiated by neurologists experienced in the diagnosis and management of epilepsy, with continuation of patient management by general paediatricians and practitioners when the initiating neurologist is unavailable.
General. The dose of stiripentol is calculated on a mg/kg body weight basis.
It is recommended to split the daily dose in two or three daily intakes (totalling the daily recommended dose per kg and per day). The initiation of adjunctive therapy with stiripentol should be undertaken gradually using upwards dose escalation to reach the recommended dose of 50 mg/kg/day.
Stiripentol dosage escalation should be gradual, starting with 20 mg/kg/day for 1 week, then 30 mg/kg/day for 1 week. Further dosage escalation is age dependent:
children less than 6 years should receive an additional 20 mg/kg/day in the third week, thus achieving the recommended dose of 50 mg/kg/day in three weeks;
children from 6 to less than 12 years should receive an additional 10 mg/kg/day each week, thus achieving the recommended dose of 50 mg/kg/day in four weeks;
children and adolescents 12 years and older should receive an additional 5 mg/kg/day each week until the optimum dose is reached based on clinical judgment.
The recommended dose of 50 mg/kg/day is based on the available clinical study findings and was the only dose of Diacomit evaluated in the pivotal studies (see Section 5.1 Pharmacodynamic Properties, Clinical trials).
There are no clinical study data to support the clinical safety of stiripentol administered at daily doses greater than 50 mg/kg/day.
There are no clinical study data to support the use of stiripentol as monotherapy in Dravet syndrome.
Dose adjustments of other antiepileptics used in combination with stiripentol. Despite the absence of comprehensive pharmacology data on potential drug interactions, the following advice regarding modification of the dose and dosage schedules of other anti-epileptic medicinal products administered in conjunction with stiripentol is provided based on clinical experience.
Clobazam. In the pivotal studies, when the use of stiripentol was initiated, the daily dose of clobazam was 0.5 mg/kg/day usually administered in divided doses, twice daily. In the event of clinical signs of adverse reactions or overdose of clobazam (i.e. drowsiness, hypotonia, and irritability in young children), this daily dose was reduced by 25% every week.
Approximately two to three fold increases in clobazam and five fold increases in norclobazam plasma levels respectively have been reported with co-administration of stiripentol in children with Dravet syndrome.
Valproate. The potential for metabolic interaction between stiripentol and valproate is considered modest and thus, no modification of valproate dosage should be needed when stiripentol is added, except for clinical safety reasons. In the pivotal studies in the event of gastrointestinal adverse reactions such as loss of appetite, loss of weight, the daily dose of valproate was reduced by around 30% every week.
Effect of formulation. The sachet formulation (Cmax = 7.32 microgram/mL) has a slightly higher Cmax than the capsules (Cmax = 5.99 microgram/mL) and thus the formulations are not bioequivalent. It is recommended that if a switch of formulations is required this is done under clinical supervision, in case of problems with tolerability (see Section 5 Pharmacological Properties).
Renal and hepatic impairment. Stiripentol is not recommended for use in patients with impaired hepatic and/or renal function (see Section 4.4 Special Warnings and Precautions for Use).
Method of administration. The capsule should be swallowed whole with a glass of water during a meal.
The powder should be mixed in a glass of water and should be taken immediately after mixing during a meal.
Stiripentol must always be taken with food as it degrades rapidly in an acidic environment (e.g. exposure to gastric acid in an empty stomach).
Diacomit should not be taken with milk or dairy products (yoghurt, soft cream cheese, etc.), carbonated drinks, fruit juice or food and drinks that contain caffeine or theophylline.
Drug discontinuation. Antiepileptic drugs, including Diacomit, should be withdrawn gradually to minimise the potential for seizures or increased seizure frequency. In clinical trials in children with Dravet syndrome, dosages were gradually reduced over a period lasting at least one month.
In situation where rapid withdrawal of Diacomit is medically required, appropriate monitoring is recommended.
4.3 Contraindications
Hypersensitivity to the active substance or to any of the excipients.
A past history of psychoses in the form of episodes of delirium.
4.4 Special Warnings and Precautions for Use
Identified precautions. The pivotal clinical evaluation of Diacomit was in children of 3 years of age and over with SMEI. Children under 3 years of age and adults were not studied in the pivotal trials therefore efficacy and safety for those populations were not established in the pivotal trials.
Drug interactions. Carbamazepine, phenytoin and phenobarbital. Carbamazepine, phenytoin, and phenobarbital should generally not be used in conjunction with stiripentol in the management of Dravet syndrome.
Phenytoin and phenobarbital can significantly decrease the serum concentration of stiripentol. Stiripentol can significantly increase the serum concentration of carbamazepine, phenytoin, and phenobarbital. Furthermore, there is evidence that these drugs have the potential to worsen seizure activity in patients with Dravet syndrome, even though these drugs may have a role in a subset of patients with Dravet syndrome.
It is recommended that carbamazepine, phenytoin, and phenobarbital be used in conjunction with stiripentol only under expert supervision with appropriate monitoring.
Clobazam and valproate. The daily dosage of clobazam and/or valproate should be reduced according to the onset of side effects whilst on stiripentol therapy (see Section 4.2 Dose and Method of Administration).
Substances interfering with CYP enzymes. Stiripentol is an inhibitor of the enzymes CYP1A2, CYP2C8, CYP2C19, CYP3A4, CYP2C9 and CYP2D6 and may markedly increase the plasma concentrations of substances metabolised by these enzymes and increase the risk of adverse reactions (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions). In vitro data also suggest that STP induces the activity of CYP1A2 and CYP2B/3A, but the clinical relevance of this is uncertain. In vitro studies suggested that stiripentol phase 1 metabolism is catalysed by CYP1A2, CYP2C9, CYP2C19 and CYP3A4/5 and possibly other enzymes. Caution is advised when combining stiripentol with other substances that inhibit or induce one or more of these enzymes.
Blood count. Neutropenia may be associated with the administration of stiripentol, clobazam and valproate. Blood counts should be assessed prior to starting treatment with stiripentol. Unless otherwise clinically indicated, blood counts should be checked every 6 months.
Neurologic/psychiatric. Patients should be monitored for somnolence and drowsiness, particularly when stiripentol is used concomitantly with other central nervous depressant. An adjustment of the dosage of concomitant clobazam or other anti-epileptic dugs could be considered. Patients (or their parents or carers) should be advised to not operate machinery or drive.
Movement disorders including ataxia, hypotonia, tremor, hyperkinesia, dysarthria and equilibrium disorders have been reported in patients treated with Diacomit for Dravet syndrome.
Suicidal ideation and behaviour. Suicidal ideation and behaviour have been reported in patients treated with antiepileptic agents in several indications.
All patients treated with antiepileptic drugs, irrespective of indication, should be monitored for signs of suicidal ideation and behaviour and appropriate treatment should be considered. Patients (or their parents or carers) should be advised to seek medical advice should signs of suicidal ideation or behaviour emerge.
Use in hepatic impairment. Liver function. In patients newly prescribed stiripentol, raised γGT (notably when combined with valproate) are observed with a common frequency, whilst abnormal liver function tests (increases in AST and/or ALT) are also reported with a rare frequency. Liver function (γGT, AST and ALT levels) should therefore be assessed prior to starting treatment with stiripentol and, unless otherwise clinically indicated, should be checked every 6 months.
Stiripentol is primarily metabolised by the liver and primarily excreted by the kidney.
In the absence of specific clinical data in patients with impaired hepatic or renal function, stiripentol is not recommended for use in patients with impaired hepatic and/or renal function.
Use in renal impairment. Stiripentol is primarily metabolised by the liver and primarily excreted by the kidney.
In the absence of specific clinical data in patients with impaired hepatic or renal function, stiripentol is not recommended for use in patients with impaired hepatic and/or renal function.
Use in the elderly. No data are available.
Paediatric use. Growth rate of children. Due to the frequency of gastrointestinal adverse reactions to treatment with stiripentol and valproate (anorexia, loss of appetite, nausea, vomiting), the growth rate of children under this combination of treatment should be carefully monitored.
Effects on laboratory tests. In the event of an abnormal blood count or liver function test finding, the clinical decision for continuing use or adjusting the dose of stiripentol in conjunction with adjusting the doses of clobazam and valproate needs to be made on an individual patient basis taking into consideration the potential clinical benefits and risks.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Stiripentol is subject to non-linear pharmacokinetics (see Section 5 Pharmacological Properties).
Potential medicinal product interactions affecting stiripentol. The influence of other antiepileptic medicinal products on stiripentol pharmacokinetics is not well established.
The impact of macrolides and azole antifungal agents, that are known to be inhibitors of CYP3A4 and substrates of the same enzyme, on stiripentol metabolism is not known. Likewise, the effect of stiripentol on their metabolism is not known.
In vitro studies suggested that stiripentol phase 1 metabolism is catalysed by CYP1A2, CYP2C19 and CYP3A4 and possibly other enzymes. Caution is advised when combining stiripentol with other substances that inhibit or induce one or more of these enzymes.
Effect of stiripentol on cytochrome P450 enzymes. Many of these interactions have been partially confirmed by in vitro studies and in clinical trials. The increase in steady state levels with the combined use of stiripentol, valproate, and clobazam is similar in adults and children, though inter-individual variability is marked.
At therapeutic concentrations, stiripentol significantly inhibits several CYP450 isoenzymes: for example, CYP2C19, CYP1A2, CYP2C8, CYP2D6, CYP2C9 and CYP3A4. As a result, pharmacokinetic interactions of metabolic origin with other medicines may be expected. These interactions may result in increased systemic levels of these active substances that may lead to enhanced pharmacological effects and to an increase in adverse reactions. In vitro data also suggest that stiripentol induces the activity of CYP1A2 and CYP2B/3A, but the clinical relevance of this is uncertain.
Caution must be exercised if clinical circumstances require combining stiripentol with substances metabolised by CYP2C19 (e.g. citalopram, omeprazole) or CYP3A4 (e.g. HIV protease inhibitors, antihistamines such as astemizole and chlorpheniramine, calcium channel blockers, statins, oral contraceptives, codeine) due to the increased risk of adverse reactions (see further in this section for antiepileptic medicines). Monitoring of plasma concentrations or adverse reactions is recommended. A dose adjustment may be necessary.
Co-administration with CYP3A4 substrates with a narrow therapeutic index should be avoided due to the markedly increased risk of severe adverse reactions.
Data on the potential for inhibition of CYP1A2 are limited, and therefore, interactions with theophylline and caffeine cannot be excluded because of the increased plasma levels of theophylline and caffeine which may occur via inhibition of their hepatic metabolism, potentially leading to toxicity. Use in combination with stiripentol is not recommended. This warning is not only restricted to medicinal products but also to a considerable number of foods and nutritional products aimed at children, such as cola drinks, which contain significant quantities of caffeine or chocolate, which contains trace amounts of theophylline.
As stiripentol inhibited CYP2D6 in vitro at concentrations that are achieved clinically in plasma, substances that are metabolised by this isoenzyme like: beta-blockers (propranolol, carvedilol, timolol), antidepressants (fluoxetine, paroxetine, sertraline, imipramine, clomipramine), antipsychotics (haloperidol), analgesics (codeine, dextromethorphan, tramadol) may be subject to metabolic interactions with stiripentol. A dose-adjustment may be necessary for substances metabolised by CYP2D6 and that are individually dose titrated.
Effect of stiripentol on GABA receptor site. Stiripentol is a positive allosteric modulator of the GABAA receptor. There is a potential for it to act synergistically with other allosteric modulators at the same site (e.g. benzodiazepines, non-benzodiazepines, barbiturates, bromides or neuroactive steroids) to enhance GABAergic neurotransmission.
Potential for stiripentol to interact with other medicinal products. In the absence of available clinical data, caution should be taken with the following clinically relevant interactions with stiripentol, see Table 1 and Table 2.
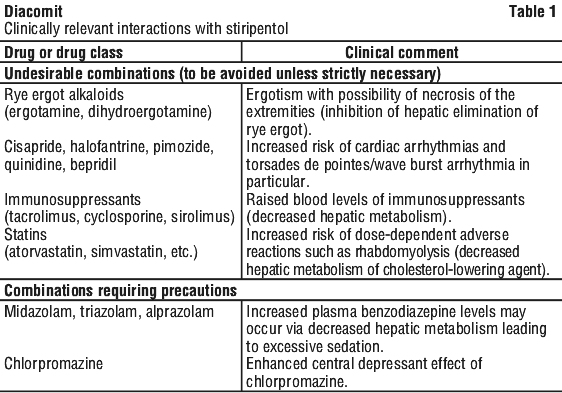

4.6 Fertility, Pregnancy and Lactation
Effects on fertility. There were no effects on fertility in male and female rats following oral administration of STP at doses up to 800 mg/kg/day (equivalent to about 3-fold the MRHD, based on body surface area). As no human clinical data are available, the potential risk for humans is unknown.
Use in pregnancy. (Category B3)
Risk related to epilepsy and antiepileptic medicinal products in general. It has been shown that in the offspring of women with epilepsy, the prevalence of malformations is two to three times greater than reported in the general population. Although other factors, e.g. the epilepsy, can contribute, available evidence suggests that this increase, to a large extent, is caused by the treatment. In the treated population, an increase in malformations has been noted with polytherapy.
However, effective anti-epileptic therapy should not be interrupted during pregnancy, since the aggravation of the illness may be detrimental to both the mother and the foetus.
Risk related to stiripentol. No data on exposed pregnancies are available. Stiripentol and/or its metabolites cross the placenta in rats. There was no evidence of teratogenicity in mice or rabbits treated with STP during the period of organogenesis at oral doses up to 800 mg/kg/day, which is about 2-fold (mice) and 6-fold (rabbits) the MRHD, based on body surface area. Increased numbers of resorptions were reported in mouse embryofetal development studies at doses of ≥ 200 mg/kg/day (0.4 times the MRHD based on BSA), and also in the rabbit embryofetal development study at a dose of 800 mg/kg/day (6 times the MRHD based on BSA). Rats treated with oral STP from early or late gestation to weaning showed maternotoxicity and reduced pup survival and reflex development at 800 mg/kg/day (equivalent to about 3-fold the mg/m2 MRHD); the no-effect dose was 200 mg/kg/day.
In view of the indication, administration of stiripentol during pregnancy and in women of childbearing potential would not be expected. The clinical decision for use of stiripentol in pregnancy needs to be made on an individual patient basis taking into consideration the potential clinical benefits and risks. Caution should be exercised when prescribing to pregnant women and use of efficient methods of contraception is advisable.
Use in lactation. It is not expected that Dravet syndrome affected women will conceive and have children. However, as there are no human studies on the excretion of stiripentol in breast milk, and given that stiripentol passes freely from plasma into milk in the goat, breast feeding is not recommended while on treatment with stiripentol. In the unlikely event that stiripentol therapy is maintained while breast feeding, the breast fed infant should be carefully monitored for potential adverse effects.
4.7 Effects on Ability to Drive and Use Machines
Patients with Dravet syndrome would not be expected to drive or operate machinery due to the nature of the underlying disease and the effects of long term administration of anticonvulsant medicines.
Stiripentol may cause dizziness and ataxia that may affect ability to drive and use machines and patients should not drive or use machinery whilst on stiripentol therapy.
4.8 Adverse Effects (Undesirable Effects)
Summary of the safety profile. Clinical trial experience. Two prospective, randomised, 8-week treatment, double-blind, placebo-controlled trials were conducted in Dravet syndrome patients (STICLO France and STICLO Italy). In both trials, stiripentol was added on to treatment with valproate and clobazam. The dose of stiripentol was 50 mg/kg/day.
Table 3 lists the adverse events that were reported during the studies. No patient died during these double-blind, placebo-controlled studies.
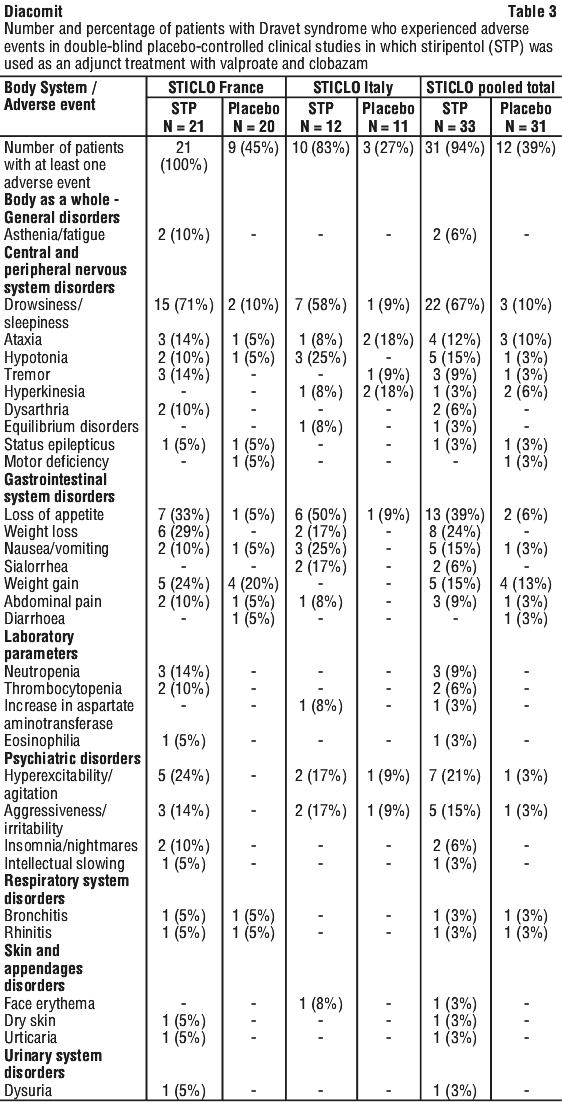
Adverse effects encountered most often are as follows: very common (≥ 1/10), common (≥ 1/100 to < 1/10), uncommon (≥ 1/1,000 to < 1/100), rare (≥ 1/10,000 to < 1/1,000), very rare (< 1/10,000), not known (cannot be estimated from the available data). Within each frequency grouping, adverse effects are presented in order of decreasing severity. These data are presented in Table 4.
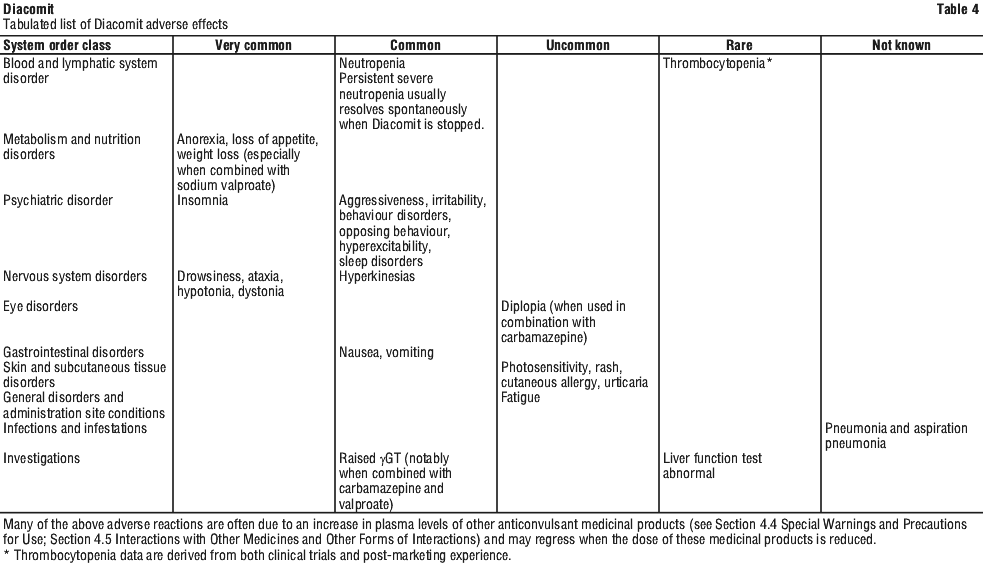
In two double-blind, placebo-controlled trials in Dravet syndrome patients, gastrointestinal adverse events most often reported in patients receiving stiripentol were loss of appetite in 39% of the treated patients and loss of weight in 24% of the treated patients.
Nausea and vomiting. Nausea and vomiting are common adverse effects.
In 2 double-blind, placebo-controlled trials in Dravet syndrome patients, nausea and vomiting were observed in 15% of the treated patients.
Due to the frequency of gastrointestinal adverse reactions to treatment with stiripentol and valproate (anorexia, loss of appetite, nausea, vomiting), the growth rate of children under this combination of treatment should be carefully monitored.
Abnormal liver function tests. Raised γGT (notably when combined with carbamazepine and valproate) is a common adverse effect.
Liver function should be assessed prior to starting treatment with stiripentol. Unless otherwise clinically indicated, liver function should be checked every 6 months. As the drug is metabolised mainly by the liver, stiripentol is not recommended for use in patients with impaired hepatic function.
Central nervous system adverse events. Drowsiness, ataxia, hypotonia, dystonia and insomnia are very common adverse effects.
In 2 double-blind, placebo-controlled trials in Dravet syndrome patients, drowsiness/sleepiness were observed in 67% of the treated patients, hyperexcitability/agitation in 21% of treated patients, aggressiveness/irritability in 15% of treated patients, hypotonia in 15% of the treated patients, and ataxia in 12% of the treated patients.
Patients should be monitored for somnolence and drowsiness, particularly when stiripentol is used concomitantly with other central nervous depressant. An adjustment of the dosage of concomitant clobazam or other anti-epileptic drugs could be considered. Patients should be advised to not operate machinery or drive.
Thrombocytopenia and neutropenia. Neutropenia is a common adverse effect. Thrombocytopenia is a rare adverse effect.
In 2 double-blind, placebo-controlled trials in Dravet syndrome patients, neutropenia was observed in 9% of the treated patients and thrombocytopenia in 6% of the treated patients.
Blood counts should be assessed prior to starting treatment with stiripentol. Unless otherwise clinically indicated, blood counts should be checked every 6 months.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
Data on clinical overdose are not available. Treatment is supportive (symptomatic measures in intensive care units).
For information on the management of overdose, contact the Poison Information Centre on 131126 (Australia) or the New Zealand Poisons Centre on 0800 POISON or 0800 764 766.
5 Pharmacological Properties
Pharmacology data are mainly based on four clinical pharmacokinetics studies in healthy adult volunteers, one population pharmacokinetics study in children with Dravet syndrome, three efficacy studies in the target population that generated supportive pharmacokinetics data and studies from the clinical literature.
5.1 Pharmacodynamic Properties
Mechanism of action. The mechanism of antiepileptic activity of stiripentol is based on the potentiation of the GABAergic transmissions in the CNS. In vitro, stiripentol has been shown to directly enhance GABAA receptor-mediated transmission by acting both post-synaptically at a neuronal site coupled to the GABAA receptor and pre-synaptically to increase GABA release from nerve terminals. In rodent models, stiripentol appears to increase brain levels of GABA. This could occur by inhibition of synaptosomal uptake of GABA and/or inhibition of GABA transaminase. Stiripentol has been shown to enhance GABAA receptor-mediated transmission in the immature rat hippocampus and increase the mean open-duration (but not the open-frequency) of GABAA receptor chloride channels.
Stiripentol also potentiates the efficacy of clobazam and other anticonvulsants, as a result of the pharmacokinetic interactions (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions). This effect of stiripentol is mainly based on metabolic inhibition of several isoenzymes, in particular CYP450 3A4 and 2C19, involved in the hepatic metabolism of other anti-epileptic medicines.
Clinical trials. The efficacy of stiripentol, as an add-on therapy to optimised treatment with valproate and clobazam in patients presenting with Dravet syndrome has been demonstrated in two randomised, double-blind, placebo-controlled clinical trials. These trials, designated STICLO France and STICLO Italy, involved 41 (age range: 3.0-20.7) and 23 patients (age range: 3.5-18.9) respectively. Both studies were conducted according to similar design to evaluate the responder rate to treatment, where the responder was defined as a patient who achieved ≥ 50% decrease in the frequency of generalised clonic or tonic-clonic seizures during the double-blind treatment period compared to baseline (i.e. placebo run-in).
Eligible patients were included initially in a 1-month baseline period during which they continued to receive their optimised antiepileptic treatment. Following this 1-month baseline, patients were randomly allocated to receive either stiripentol (50 mg/kg/day) or placebo added on to their antiepileptic treatment. The frequency of generalised clonic or tonic-clonic seizures during the trial was recorded by the patients and or their caregivers, using a diary. Patients were treated double-blind for 2 months.
Results of each clinical trial are presented separately as well as pooled. Several criteria allow to pool the results of STICLO France and STICLO Italy. The data poolability from the two STICLO trials was assessed statistically and results indicated that the data were poolable using the demographic and primary endpoints data.
In study STICLO France, total of 41 patients were enrolled; 21 were randomised to receive stiripentol and 20 were randomised to receive placebo. One patient in the stiripentol group was excluded. For study STICLO Italy, 23 patients were enrolled; 12 were randomised to STP, and 11 to placebo. All were judged to be evaluable. A summary of the baseline demographic data is provided in Table 5.

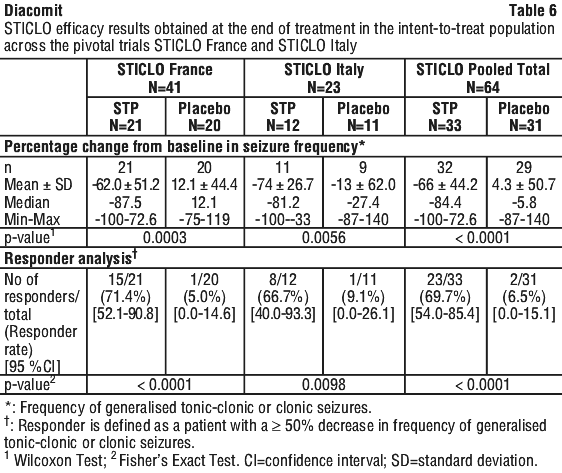
When efficacy results of both STICLO trials were pooled, 23 of 33 (69.7%) patients on stiripentol versus 2 of 31 (6.5%) patients on placebo met the criterion for response (p < 0.0001). Mean percent reduction in seizure frequency was 66% in the pooled STP group versus an increase of 4% in the pooled placebo groups (p < 0.0001).
5.2 Pharmacokinetic Properties
Studies in children of various ages showed that the pharmacokinetic behaviour of stiripentol is influenced by age and body weight. Stiripentol should be adjusted accordingly by reducing the daily dose as body weight and age increase.
Absorption. Stiripentol is quickly absorbed. The Tmax times were 2.42 hours for single doses of stiripentol 500 mg and 1,000 mg and 2.96 hours for 2,000 mg. According to Michaelis‐Menten kinetics there is some evidence for non‐linearity regarding stiripentol absorption. Following the oral administration of 500 mg, 1,000 mg and 2,000 mg of stiripentol in healthy volunteers the following data were determined, see Table 7.
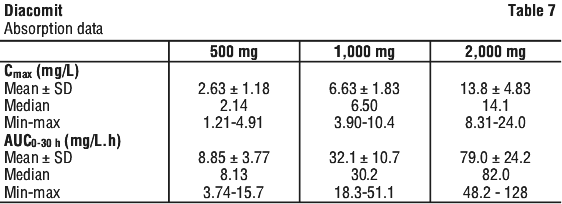
Distribution. Stiripentol binds extensively to circulating plasma proteins (about 99% at clinical plasma concentrations).
In a population pharmacokinetic study conducted in Dravet syndrome patients at steady state receiving the combination valproate + clobazam + stiripentol, the apparent volume of stiripentol distribution according to weight was as follows (see Table 8).
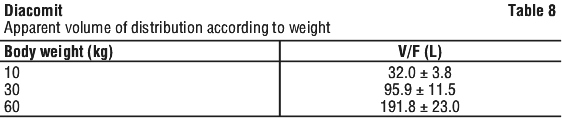
Stiripentol undergoes extensive first-pass metabolism in the liver with CYP1A2, CYP2C19 and CYP3A4 being the main isozymes involved in stiripentol metabolism. Stiripentol is mainly metabolised by glucuronidation and oxidative cleavage.
Stiripentol is supplied as a racemic mixture, and after administration R-enantiomer is the predominant enantiomer, but glucuronidation appears to favour the S-enantiomer.
Elimination of a single dose was mainly (73%) via the kidney after extensive metabolisation (13 different metabolites) by the liver (Cytochrome P 450).
Excretion. Stiripentol is primarily excreted by the kidney.
Systemic exposure to stiripentol increases markedly compared to dose proportionality. In healthy adults, plasma clearance decreases markedly at high doses; it falls from approximately 40 L/kg/day at the dose of 600 mg/day to about 8 L/kg/day at the dose of 2,400 mg. Clearance is decreased after repeated administration of stiripentol, probably due to inhibition of the cytochrome P450 isoenzymes responsible for its metabolism. The half-life of elimination was in the range of 4.5 hours to 13 hours, increasing with dose.
Similarly, in a population pharmacokinetic study conducted in Dravet syndrome patients at steady state receiving the combination valproate + clobazam + stiripentol, the apparent volume of stiripentol distribution according to weight was as follows (see Table 9).

5.3 Preclinical Safety Data
Genotoxicity. There was no evidence for genotoxic potential in in vitro assays for gene mutation or unscheduled DNA synthesis. A positive in vitro chromosomal aberration assay in Chinese Hamster Ovary cells (observed at the highest concentration) was not confirmed in a similar assay with human lymphocytes or in a mouse micronucleus test in vivo. The genotoxic potential of STP is considered to be low.
Carcinogenicity. There was no evidence of carcinogenicity in rats following oral administration of STP for 2 years at doses up to 800 mg/kg/day. This dose is approximately 3-4 times the MRHD based on body surface area, and systemic exposure (plasma AUC) was about 4-fold the estimated exposure in adults at the MRHD. In mice treated orally for 78 weeks, there was an increase in the incidence of hepatic adenomas and carcinomas at doses of 200 or 600 mg/kg/day. These doses are about 0.5 to 2-fold the MRHD based on body surface area, and plasma exposure was about 2-fold the paediatric Cmax; the no-effect dose was 60 mg/kg/day. In view of the lack of genotoxicity of STP and the known susceptibility of the mouse liver to tumour formation in response to hepatic enzyme induction, this finding is not considered to indicate a risk of tumorigenicity in patients.
6 Pharmaceutical Particulars
6.1 List of Excipients
Capsules. Povidone, sodium starch glycolate type A, magnesium stearate, gelatin, titanium dioxide, erythrosine (Diacomit 250 mg only), indigo carmine (Diacomit 250 mg only).
Printing Ink: Shellac, iron oxide black.
Powder for oral suspension. Aspartame, spray-dried liquid glucose, povidone, sodium starch glycolate type A, erythrosine, titanium dioxide, carmellose hyetellose, Arome Polv tutti frutti 25 H 245.
6.2 Incompatibilities
See Section 4.5 Interactions with Other Medicines and Other Forms of Interactions.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C. Store in original container to protect from light.
6.5 Nature and Contents of Container
Diacomit 250 mg and 500 mg capsules are supplied in high density polyethylene bottles with tamper-evident seal and child-resistant polypropylene screw cap. Each bottle contains 60 capsules.
Diacomit 250 mg and 500 mg powder for oral suspension are packaged in paper/aluminium/high density polyethylene film sachet. The sachets are supplied in boxes of 60 sachets.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
Stiripentol is a white to pale yellow crystalline powder, practically insoluble in water at 25°C, sparingly soluble in chloroform and soluble in acetone, ethanol, ether, acetonitrile and dichloromethane.
Chemical structure.
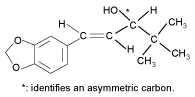
Molecular formula: C14H18O3.
Relative molecular mass: 234.3 g/mol.
Stiripentol is obtained as a racemate.
7 Medicine Schedule (Poisons Standard)
Schedule 4.
Date of First Approval
13 September 2019
Date of Revision
25 August 2025
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.