Eikance 0.01%
Brand Information
| Brand name | Eikance 0.01% |
| Active ingredient | Atropine sulfate |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Eikance 0.01%.
Summary CMI
EIKANCE EYE DROPS
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
▼ This medicine is new or being used differently. Please report side effects. See the full CMI for further details.
1. Why am I using EIKANCE?
EIKANCE Eye Drops contain the active ingredient atropine sulfate monohydrate. They are used as a treatment for near sightedness when initiated in children aged from 4 to 14 years. The length of treatment is variable, and will be advised by your doctor.
For more information, see Section 1. Why am I using EIKANCE? in the full CMI.
2. What should I know before I use EIKANCE?
Do not use if you have ever had an allergic reaction to atropine or any of the ingredients of the Eye Drops listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, use any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I use EIKANCE? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with EIKANCE and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use EIKANCE?
- Use as directed by your Doctor. Do not use more than the number of drops he/she advises or use them more frequently than directed.
- Gently pull out the lower eyelid to form a sac. Allow one drop to fall into the sac without touching the eye with the dropper end of the container. To minimise absorption of the drug other than into the eye, close eyes and then apply gentle pressure to the tear duct for approximately one minute immediately after application.
More instructions can be found in Section 4. How do I use EIKANCE? in the full CMI.
5. What should I know while using EIKANCE?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using EIKANCE? in the full CMI.
6. Are there any side effects?
The most common side effects of EIKANCE Eye Drops are blurred vision, photophobia, allergy, sore, swollen, red and itchy eyes, headache and fatigue. For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
▼ This medicine is subject to additional monitoring. This will allow quick identification of new safety information. You can help by reporting any side effects you may get. You can report side effects to your doctor, or directly at www.tga.gov.au/reporting-problems.
EIKANCE EYE DROPS
Active ingredient: atropine sulfate (as atropine sulfate monohydrate)
Consumer Medicine Information (CMI)
This leaflet provides important information about using EIKANCE. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using EIKANCE.
Where to find information in this leaflet:
1. Why am I using EIKANCE?
2. What should I know before I use EIKANCE?
3. What if I am taking other medicines?
4. How do I use EIKANCE?
5. What should I know while using EIKANCE?
6. Are there any side effects?
7. Product details
1. Why am I using EIKANCE?
EIKANCE contains the active ingredient atropine sulfate monohydrate (atropine). EIKANCE is an eye drop preparation used to deliver atropine directly to the eye for local activity. It reduces the rate of unwanted changes in the eye which may slow the progression of near sightedness (myopia).
EIKANCE Eye Drops are used as a treatment to slow the progression of myopia in children aged from 4 to 14 years.
2. What should I know before I use EIKANCE?
Warnings
Do not use EIKANCE if:
- you are allergic to atropine, or any of the ingredients listed at the end of this leaflet.
- Always check the ingredients to make sure you can use this medicine.
- if you have angle closure glaucoma or a family history of glaucoma.
- the expiry date printed on the pack has passed. If you use it after the expiry date has passed, it may have no effect at all, or worse, there may be an entirely unexpected effect.
- if the packaging is torn or shows signs of tampering.
Check with your doctor if you:
- are allergic to any other medicines or any foods, dyes or preservatives.
- have glaucoma or a family history of glaucoma
- are wearing contact lenses
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor if you are pregnant or intend to become pregnant.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
EIKANCE, should not be used during pregnancy unless your doctor specifically tells you to.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with EIKANCE and affect how it works these include:
- Medicines to treat glaucoma
- Some medicines used to treat depression
- Some antihistamines
- Some medicines used to treat Parkinson's disease
- Some medicines used to treat mental illness
- Medicines used to treat muscle weakness
- Potassium citrate and potassium supplements
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect EIKANCE.
4. How do I use EIKANCE?
How much to use
- Gently pull out the lower eyelid to form a sac. Allow one drop to fall into the sac without touching the eye with the dropper end of the container.
- To minimise absorption of the drug other than into the eye, close eyes and then apply gentle pressure to the tear duct for approximately one minute immediately after application.
- Follow the instructions provided and use EIKANCE until your doctor tells you to stop.
- If you are wearing contact lenses, remove them before putting the drops in your eye.
- Wait 15 minutes before replacing your contact lenses.
When to use EIKANCE
- EIKANCE should be used as directed by your Doctor. Do not use more than the number of drops he/she advises or use them more frequently than directed.
- It is important to use EIKANCE exactly as directed.
- If you use less than you should, it may not work as well, and your medical condition may not improve.
- Using it more frequently than directed may not improve your condition any faster and may cause or increase side effects.
- If EIKANCE is stopped suddenly your vision may get worse. Discuss with your doctor before stopping EIKANCE.
EIKANCE eye drops should be administered as one drop to each eye at night
If you forget to use EIKANCE
If you miss your dose at the usual time use it as soon as you remember and then return to your normal dosing time.
If you have trouble remembering when to use EIKANCE Eye drops, ask your pharmacist for some hints.
If it is almost time for your next dose, skip the dose you missed and use your next dose when you are meant to.
Do not use a double dose to make up for the dose you missed.
If you use too much EIKANCE
While the risks associated with using too much EIKANCE is small, if you think that you have used too much, you may need urgent medical attention.
Signs associated with too much atropine use include:
- Dry or burning mouth
- Difficulty in swallowing or talking
- Hot, dry skin
- Difficulty in passing urine
You should immediately:
- phone the Poisons Information Centre
- (by calling 13 11 26), or
- contact your doctor, or
- go to the Emergency Department at your nearest hospital.
5. What should I know while using EIKANCE?
Things you should do
Call your doctor straight away if you:
- feel EIKANCE Eye Drops are not helping your child's condition.
- for any reason, you have not used the EIKANCE Eye Drops as prescribed. Otherwise, your doctor may think that it was not effective and change your treatment unnecessarily.
Always discuss with your doctor any problems or difficulties during or after using EIKANCE Eye Drops.
Remind any doctor, dentist or pharmacist you visit that your child is using EIKANCE.
When EIKANCE eye drops are first used, your child may experience greater sensitivity to sunlight. If this occurs, call your doctor. This effect usually decreases over time. The use of sunglasses or UV lenses in your glasses has been shown to help with this effect.
When using EIKANCE eye drops, your child may find it more difficult to focus for close work or when reading. If this occurs, call your doctor to discuss options to help you manage this issue.
If you find it more difficult to focus, be careful before you drive or use any machine or tools.
Things you should not do
- Do not give EIKANCE to anyone else even though their symptoms seem similar to yours.
- Do not use EIKANCE for other conditions unless your doctor tells you. EIKANCE Eye Drops have been prescribed for you for a specific condition. If you use it for another condition, it may not work or may make the condition worse.
- Do not give EIKANCE to children under the age of 4 years.
- Do not stop using EIKANCE suddenly. Discuss with your doctor if you plan to stop using this medicine.
Looking after your medicine
- A locked cupboard at least one and a half metres above the floor is a good place to store medicines.
- Keep EIKANCE in a cool, dry place where the temperature stays below 25°C and protect from light.
- Do not freeze or refrigerate.
Follow the instructions in the carton on how to take care of your medicine properly.
Store it in a cool dry place away from moisture, heat or sunlight; for example, do not store it:
- in the bathroom or near a sink, or
- in the car or on windowsills.
Keep it where young children cannot reach it.
When to discard your medicine
EIKANCE comes as single use containers. Discard any medicine left in the single use container after each dose administration.
Getting rid of any unwanted medicine
If you no longer need to use this medicine or it is out of date, take it to any pharmacy for safe disposal.
Do not use this medicine after the expiry date.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
Systemic absorption
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What EIKANCE contains
| Active ingredient (main ingredient) | Atropine sulfate monohydrate |
| Other ingredients (inactive ingredients) | Citric acid monohydrate, sodium chloride and purified water. Hydrochloride acid or sodium hydroxide is used to adjust pH. |
Do not use this medicine if you are allergic to any of these ingredients.
What EIKANCE Eye Drops look like
EIKANCE eye drops are a clear, colourless solution filled into transparent 0.3 mL single-dose containers.
Strips of 5 single-dose containers are packed in an aluminium laminated foil sachet.
EIKANCE eye drops are available in packs of 5, 30, 60 or 90 single-dose containers.
Not all pack sizes may be marketed.
EIKANCE 0.01%, AUST R 331960
EIKANCE 0.025%, AUST R 408371
EIKANCE 0.05%, AUST R 408372
Who distributes EIKANCE
Aspen Pharmacare Australia Pty Ltd
34-36 Chandos Street,
St Leonards NSW 2065
Australia
www.aspenpharma.com.au
Trademarks are owned by or licensed to the Aspen Group of companies.
© 2026 Aspen Group of companies or its licensor. All rights reserved
This leaflet was revised in March 2026.
Brand Information
| Brand name | Eikance 0.01% |
| Active ingredient | Atropine sulfate |
| Schedule | S4 |
▼ This medicinal product is subject to additional monitoring in Australia. This will allow quick identification of new safety information. Healthcare professionals are asked to report any suspected adverse events at www.tga.gov.au/reporting-problems.
MIMS Revision Date: 01 May 2026
1 Name of Medicine
Atropine sulfate.
2 Qualitative and Quantitative Composition
Eikance 0.05% eye drops is a preservative-free, sterile, ophthalmic solution containing 500 microgram of atropine sulfate in 1 mL of water (0.05%).
Eikance 0.025% eye drops is a preservative-free, sterile, ophthalmic solution containing 250 microgram of atropine sulfate in 1 mL of water (0.025%).
Eikance 0.01% eye drops is a preservative-free, sterile, ophthalmic solution containing 100 microgram of atropine sulfate in 1 mL of water (0.01%).
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Eikance eye drops are a clear, colourless solution, packed in transparent polyethylene single-dose containers, which are sealed in aluminium laminated foil sachets.
4 Clinical Particulars
4.1 Therapeutic Indications
Eikance 0.05%, 0.025% and 0.01% are indicated as a treatment to slow the progression of myopia when initiated in children aged from 4 to 14 years. Atropine treatment may be initiated in children when myopia progresses ≥ 0.5 D or axial length increase of 0.2 mm per year.
4.2 Dose and Method of Administration
Treatment should be supervised by an eyecare professional. It is recommended that at least 2 measurements at least 6 months apart are undertaken prior to initiation or dosage changes.
Eikance eye drops should be administered as one drop to each eye at night.
Instil one drop into the eye as required for treatment. To minimise the risk of systemic absorption, gentle pressure should be applied to the tear duct for one minute after application.
Each container is for single use and should be discarded after administration of the dose (see Section 6.5 Nature and Contents of Container).
While the lowest concentration of atropine eyedrops should always be used consistent with the targeted response, the following recommendations provide guidance on the selection of individualised initiation and maintenance treatment.
Initiation. Treatment should be initiated in children aged from 4 - 14 years.
Studies have demonstrated that the strongest predicator for higher concentrations of atropine is a faster rate of myopia progression. Age at presentation influences progression rate, with younger age contributing to faster progression. Other possible predictor includes female gender and thinner sub-foveal choroidal tissue. A family history of myopia may also be a relevant consideration.
Generally, the 0.05% concentration may be considered as the most appropriate initial treatment option in children with a higher risk of myopic progression. Older children at low risk of progression may be initially treated with 0.025% or 0.01% atropine.
Maintenance. Clinical studies have demonstrated that dose adjustments, both up and down, may be warranted over the course of treatment, based on response to treatment, and tolerability of treatment particularly once the child approaches puberty. For example, Hsieh 2022 found that a one-step dose reduction (e.g. 0.05% to 0.025%) was possible in children if risk categorisation was reduced and if the annualised SE progression was < 1.0 D.
Chuang 2021 increased the concentration of atropine by one step if SE progression was > 0.5 D at six months follow up. Similarly, the concentration could be reduced one step if progression was < 0.5 D, particularly in children approaching puberty.
Discontinuation. The mean age of myopia stabilization is around 15.6 years of age, and 95% of myopes stabilize by age of 24 years (Nemeth 2021). Loss of clinical effect, including a rebound increased rate of myopia progression, has been demonstrated if therapy is ceased prior to this time point. Discontinuation may be appropriate although possible myopia rebound should be considered during this progress (Yam 2022).
It may be appropriate to progressively reduce the dose over time, prior to cessation. It is currently not established if therapeutic effects are maintained if treatment is stopped after the age of stabilization. If there is evidence of myopia rebound, after stopping treatment, it is recommended that reinitiation of therapy is considered.
The maximum benefit of treatment may not be achieved with less than a 2 year continued administration period.
The duration of administration should be based on regular clinical assessment. The maximum duration of treatment in the clinical studies was 5 years.
4.3 Contraindications
Eikance eye drops are contraindicated in the presence of angle closure glaucoma or where angle closure glaucoma is suspected. If used in glaucoma susceptible patients, an estimation of the depth of the angle of the anterior chamber should be performed prior to the initiation of therapy.
Hypersensitivity to any of the ingredients of Eikance eye drops.
4.4 Special Warnings and Precautions for Use
Risk/benefit should be considered when the following medical problems exist:
Keratoconus. High concentrations of atropine may produce fixed dilated pupils.
Synechiae. High concentrations of atropine may increase the risk of adherence of the iris to lens.
Use in children. Atropine sulfate monohydrate should not be used in children who have previously had severe systemic reaction to atropine. An increased susceptibility to atropine has been reported in children with Down's syndrome, spastic paralysis, or brain damage; therefore, atropine should be used with great caution in these patients. No difference in myopia progression was observed in children with light and dark-coloured eyes when treated with atropine 0.01% eye drops. Limited clinical evidence is available for the long-term safety of atropine eye drops in children and adolescents. It is recommended that regular eye health clinical reviews are conducted if long term treatment is planned, including the monitoring of anterior segment development, IOP, retinal health and myopia progression.
Careful monitoring of anterior segment development should be considered in clinical application of topical atropine for prolonged periods in very young children.
Eikance eye drops should not be used in children less than 4 years of age.
Photophobia. In studies using low concentration atropine (≤ 0.05%), photophobia was dose related, particularly in the short term. The incidence of photophobia was much higher for all concentrations of atropine and placebo in the first two weeks of treatment compared to the incidence at the end of 12 months. After 12 months the overall incidence less than 10% for all low concentration atropine and similar to placebo.
If children experience photophobia or glare associated with atropine use, they may be offered polychromatic glasses or encouraged to wear sunglasses. In a clinical study, photophobia was resolved in 72% of the children reporting this effect by using photochromic lenses or sunglasses (see Section 4.8 Adverse Effects (Undesirable Effects)).
Poor visual acuity. Yam 2022 found distance best corrected visual acuity (BCVA) and near visual acuity (VA) in all atropine treatment groups who continued on treatment up to 36 months were not significantly different when compared to baseline. Only in the washout group however, was a significant decrease in BCVA and near VA noted following cessation of atropine (in Year 3) across all the atropine concentrations in comparison between baseline and 36 months. This is evident in a comparison of Table 5 and Supplementary Table 4 in Yam 2022.
The LAMP study series found that both near vision and mean distant best corrected visual acuity (BCVA) in 0.05%, 0.025% and 0.01% treatment groups were not affected significantly by any treatment (P = 0.25 and P = 0.82, respectively), with any changes associated with placebo no different to atropine treatment after the initial 12 month period. At 2 years, distance and near VA continued to be unaffected by atropine treatment.
However, both distant and near VA had significantly declined at the 36 month follow up period compared to the baseline values. All atropine concentrations demonstrated this change, with no difference between concentrations used. The clinical significance is uncertain.
If children experience poor visual acuity associated with atropine use, they may be prescribed progressive glasses. In a clinical study, poor near vision acuity was improved in 96% of children by the use of multifocal lenses (see Section 4.8 Adverse Effects (Undesirable Effects)).
Children treated with 0.05% atropine drops are more likely to require corrective spectacles and require reading materials with higher contrast compared to children with normal eyesight.
Rebound myopia upon discontinuation. Discontinuation of the atropine eye drops may lead to a rebound in myopia. In a clinical study, the rates of myopia progression after a 12 month washout for children administered atropine 0.05%, 0.025%, or 0.01% eye drops for 2 years was -0.68 ± 0.49 D, -0.57 ± 0.38 D, and -0.56 ± 0.40 D respectively (no significant differences in SE progression across concentration groups, P = 0.15). Axial elongation was greater for the higher concentration, with the respective AL elongations 0.33 ± 0.17 mm, 0.29 ± 0.14 mm and 0.29 ± 0.15 mm (P = 0.003). (See Section 4.8 Adverse Effects (Undesirable Effects)).
Use in the elderly. Eikance eye drops are not indicated for use in the elderly.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Anticholinergics. If significant systemic absorption of ophthalmic atropine occurs, concurrent use of other anticholinergics or medications with anticholinergic activity may result in potentiated anticholinergic effects.
Antiglaucoma agents. (Cholinergic, long acting, ophthalmic). Concurrent use with atropine may antagonise the anti-glaucoma and miotic actions of ophthalmic long acting cholinergic anti-glaucoma agents such as echothiophate. Concurrent use with atropine may also antagonise the anti-accommodative convergence effects of these medications when they are used for the treatment of strabismus. Although no studies are currently available evaluating low dose atropine eye drops in children with elevated IOP, there are some data to suggest that the use of low dose atropine drops may reduce the risk of glaucoma in myopic children.
Antimyasthenics, potassium citrate, potassium supplements. If significant systemic absorption of ophthalmic atropine occurs, concurrent use may increase the chance of toxicity and/or side effects of these systemic medications because of the anticholinergic induced slowing of gastrointestinal motility.
Carbachol, physostigmine or pilocarpine. Concurrent use with atropine may interfere with the antiglaucoma action of carbachol, physostigmine or pilocarpine. Also, concurrent use may counteract the mydriatic effect of atropine; this counteraction may be used to therapeutic advantage.
CNS depression-producing medications. If significant absorption of systemic atropine occurs, concurrent use of medications having CNS effects, such as antiemetic agents, phenothiazines, or barbiturates, may result in opisthotonos, convulsions, coma, and extrapyramidal symptoms.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. No data regarding effects on female fertility are available. Impairment of male fertility has been observed in rats treated with atropine at doses far higher than provided by Eikance therapy (≥ 62.5 mg/kg/day orally). This was mediated pharmacologically through inhibition of the contractile function of the vas deferens and seminal vesicle in emission; sperm production and motility were unaffected in treated rats.
Use in pregnancy. (Category A)
Atropine sulfate monohydrate may be systemically absorbed after ocular administration, however, significant effects on the fetus have not been reported.
Use in lactation. Systemically absorbed atropine sulfate monohydrate is distributed into breast milk in very small amounts. It may cause adverse effects, such as rapid pulse, fever, or dry skin, in nursing infants of mothers using ophthalmic atropine.
4.7 Effects on Ability to Drive and Use Machines
While the reported incidence of poor visual acuity associated with the use of low concentrations of atropine eye drops in clinical trials was very low, the possible effect on the ability to drive or use machinery should be evaluated, particularly at the commencement of treatment.
4.8 Adverse Effects (Undesirable Effects)
The following adverse reactions have been reported in association with atropine eyes drops:
Ophthalmic. Blurred vision, local irritation, follicular conjunctivitis, vascular congestion, oedema, exudate, contact dermatitis, eczematous dermatitis.
In clinical trials evaluating the safety of low concentrations of atropine eye drops when administered to myopic children treated for up to 3 years, the most common (≥ 1% and < 10%) reported adverse events were photophobia, blurred vision, poor visual acuity and allergy.
Systemic. Systemic atropine toxicity may be manifest as flushing and dryness of the skin, blurred vision, rapid and irregular pulse, fever, abdominal distension in infants, mental aberration and loss of neuromuscular coordination. Severe systemic reactions to atropine are characterised by hypotension with progressive respiratory depression. Higher concentrations of ophthalmic atropine have been associated with cardiac arrhythmias (e.g. atrial fibrillation). The reports occurred in older patients (aged > 75 years) or young children (6 to 10 years). In all cases the patients where using concentrations of atropine eye drops 1% or greater.
No systemic adverse events have been reported with low concentration atropine drops to date.
Adverse events associated with 0.01% to 1% atropine eye drops. In a meta-analysis by Gong 2017 of adverse events associated with atropine eye drop treatment of myopia in children, the overall incidence of adverse events reported in 2425 patients treated with concentrations ranging from 0.01% to 1% was relatively small (n = 308). The most common events were photophobia (25%), poor near visual acuity (7.5%) and allergy (2.9%). The remaining events occurred in less than 1% of subjects. These events increased with increasing concentrations of atropine eye drops. The incidence of photophobia was statistically significant, but highly variable and only moderately correlated with the dose of atropine (r = 0.56; P = 0.03). The incidence of poor visual acuity with 0.01% drops was 2.3%.
Yam 2018 found that at the 2 week visit, the percentage of participants reporting photophobia was 5.5% and 12.6%, respectively, in those allocated to 0.01% atropine drops and placebo, respectively. This difference was significant (P < 0.001). At the 12 month assessment point, the percentages had declined to 2.1% for atropine and 4.3% of placebo treated subjects. Change in accommodation amplitude (D) demonstrated a concentration dependent effect (P < 0.001), however, the change observed in the 0.01% group (-0.26 ± 3.04 D) was no different from the mean change seen with placebo (-0.32 ± 2.91 D; P = 0.89). The change in pupil size also demonstrated a concentration dependent effect for both photopic and mesopic measurements, however the change remained stable throughout the trial period.
Yam 2022 measured the change in pupil size following 36 months of continued treatment, as well as the change from year 2 to year 3.
Following three years of continued treatment, both the photopic and mesopic pupil size had returned to baseline levels. In addition, there was no statistically significant difference in pupil size for any of the three atropine concentrations administered. Other adverse events reported in clinical studies include local irritation, headache and fatigue.
Case reports of tachycardia, atrial fibrillation, cardiac rhythm disturbances, psychosis, confusional state, hallucinations, decrease in consciousness, exacerbation of seizures and bilateral pigment dispersion syndrome, in association with atropine eye drops have been recorded. In all cases the patients were using concentrations of atropine eye drops 1% or greater.
Long-term ocular toxicity of 0.01% to 1% atropine eye drops. The potential for longer term ocular toxicity associated with atropine treatment in myopia, in concentrations from 0.01% to 1%, has been evaluated in several clinical studies.
Luu 2005 and Chia 2013 found that atropine 1%, 0.5%, 0.1% or 0.01% eye drops when used for the treatment of myopia over 2 years, caused no significant retinal dysfunction.
Chua 2006 observed no optic disc, lenticular or macular changes in children treated with 1% atropine eye drops for 2 years. Similarly, Yen 1989 noted no ocular side effects associated with atropine 1% eye drop treatment in children treated for one year.
Wu 2012 found no association between either the cumulative dose or duration of atropine treatment and intraocular pressure (IOP) in children treated with 0.1 to 1% atropine drops for a mean 20.5 months. Chan 2017 studied children using atropine 0.25% drops for up to 70 months and observed no change in IOP, peripapillary RNFL thickness, areas of optic disc, cup or rim thickness or up to disc ratios.
Weng 2017 measured IOP using rebound tonometer in 44 myopic children under 0.15%, 0.3%, or 0.5% atropine treatment. The average IOP of the right eye by rebound tonometer was 17.4 ± 3 mmHg (range: 11-24 mmHg), and 17.1 ± 3 mmHg (range: 12-22 mmHg) by applanation tonometry.
Yam 2018 found that mean IOP was similar among all low concentration treatment groups (15.3 ± 2.10 mmHg in 0.05%, 15.8 ± 2.06 mmHg in 0.025%, and 15.4 ± 2.07 mmHg in 0.01% atropine groups, and 15.3 ± 2.09 mmHg in placebo group; P = 0.54).
Li 2020 concluded that 0.05%, 0.025% and 0.01% atropine eye drops administered over a 12 month period had no clinical effect on corneal or lens power.
Li 2022 observed that surrogate measures of optical quality did not change significantly after two weeks of treatment with 0.01% atropine eye drops but decreased after two weeks of treatment with 0.05% atropine eye drops.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
No cases of overdose associated with the use Eikance eye drops have been reported.
Following the administered single dose of 0.3 mg atropine sulfate by ocular instillation as a 1% solution to healthy volunteers, the mean maximum plasma concentration of the active isomer of atropine was between one third and one half of the concentration associated with cardiovascular effects.
Signs of overdosage are similar to those described as systemic effects (see Section 4.8 Adverse Effects (Undesirable Effects)). Treatment is symptomatic and supportive.
For systemic effects, 0.2 to 1 mg (0.2 mg in children) physostigmine should be administered intravenously, as a dilution containing 1 mg in 5 mL of normal saline. The solution should be injected over a period of not less than 2 minutes. Dosage may be repeated every 5 minutes up to a total dose of 2 mg in children and 6 mg in adults in each 30 minute period. Physostigmine is contraindicated in hypertensive reactions.
ECG monitoring is recommended during physostigmine administration.
Excitement may be controlled by diazepam or a short acting barbiturate.
It is recommended that 1 mg of atropine be available for immediate injection if the physostigmine causes bradycardia, convulsion, or bronchoconstriction.
Supportive therapy may require oxygen and assisted respiration; cool water baths for fever, especially in children; and catheterisation for urinary retention. In infants and small children, the body surface should be kept moist.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Atropine is a non-selective muscarinic receptor antagonist. It acts in the eye to block the action of acetylcholine, relaxing the cholinergically innervated sphincter muscle of the iris. This results in dilation of the pupil (mydriasis). The cholinergic stimulation of the accommodative ciliary muscle of the lens is also blocked. This results in paralysis of accommodation (cycloplegia).
The exact mode of action of atropine attributed to the suppression of the progression of myopia has not been fully elucidated. Muscarinic receptors are widely distributed in ocular tissues, with roles in ocular growth and development, as well as accommodation, recognised. Preclinical studies suggest that atropine acts via binding to the muscarinic receptors located on scleral fibroblasts and possibly in the retina, primarily the M1, M3 and M4 subtypes. This results in changes in the activity of cell signalling proteins and enzymes such as MEK-ERK-MAPK and transglutaminases, and possibly dopamine release, causing scleral remodelling or strengthening, leading to a reduction in axial length and vitreous chamber depth and consequently a suppression of myopia progression.
Clinical trials. Efficacy data submitted in support of low concentrations of atropine treatment to prevent or reduce the progression of myopia in children and adolescents was provided as published literature. The efficacy of low dose atropine eye drops is supported by an extensive range of publications, which document its use in the management of myopia in children and adolescents. Most studies were conducted in Asian children.
The individual publications use a range of atropine concentrations ranging from high dose 1% through to very low dose 0.01% drops. The individual studies evaluated not only the initial response to treatment, but in some cases, myopia rebound upon discontinuation, and response seen after re-introduction of treatment. This overview will focus of the key clinical studies relevant to the 0.05%, 0.025% and 0.01% formulation.
Chia 2012 (ATOM 2) is a randomised, double blind, three arm, active control, parallel group study which compared the rate of myopia progression in 400 children with myopia (mean refractive error -4.5 to -4.8 D) aged 6 to 12 years treated with 0.5%, 0.1% or 0.01% atropine eye drops for 2 years. The 0.01% strength was originally included as a non-active control as it was assumed to have minimal effect. Follow on studies by Chia 2014 reported the outcome of treatment discontinuation on myopia rebound, while Chia 2016 assessed the impact of re-introducing active treatment with very low dose atropine (0.01% drops). The total treatment period for the ATOM 2 series of studies was 5 years.
The final mean myopia progression over 2 years was -0.49 ± 0.60, -0.38 ± 0.60, and -0.30 ± 0.63 D in the atropine 0.01%, 0.1%, and 0.5% groups, respectively (P = 0.07), with a significant difference only between the 0.01% and 0.5% groups (p < 0.05). The percentage of children who recorded mild myopia progression at 2 years was 50% in the 0.01% group, 58% in the 0.1% group and 63% in the group treatment with 0.5% atropine drops. Mean change in AL at 2 years was 0.41 ± 0.32 mm for 0.01%, 0.28 ± 0.27 mm for 0.1% and 0.27 ± 0.25 mm for 0.5%.
Upon cessation of atropine treatment, a myopic rebound was observed by Chia 2014 in all 3 groups, however, the rebound was significantly greater (P < 0.001) in the 0.5% group (-0.87 ± 0.52 D) compared to the 0.1% (-0.68 ± 0.45 D) and 0.01% group (-0.28 ± 0.33 D). The increase was greatest over the first 8 months, slowing over the next 4 months. Similarly, there was a significant increase in AL (P < 0.0001) in the 0.5% group (0.35 mm) and 0.1% group (0.33 mm) compared to the 0.01% group (0.19 mm).
Chia 2016 demonstrated that fewer children in the 0.01% group (24%) required retreatment compared with children in the 0.1% (59%) and 0.5% group (68%). By year 5, overall progression of myopia was less in the 0.01% group (-1.38 ± 0.98 D) compared to with the 0.1% (-1.83 ± 1.16 D, P = 0.003) and 0.5% (-1.98 ± 1.10 D, P < 0.001). This was primarily due to fewer children in the 0.01% group progressing after treatment was stopped, and the rate of progression in the washout year in those who needed retreatment was also less in the 0.01% group compared to the 0.1 and 0.5% groups (-0.63, -0.94 and -1.09 D, respectively) (see Figure 1).
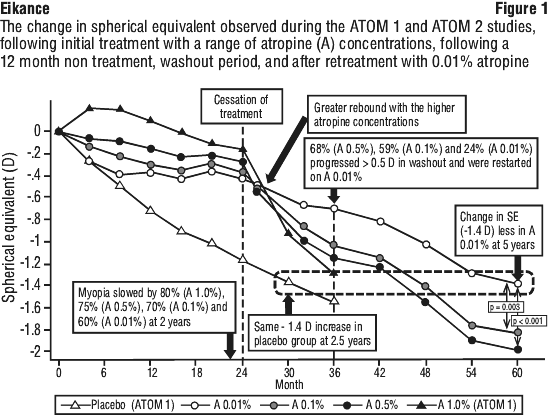
The final mean myopia progression at the end of 12 month's treatment was -0.27 ± 0.61, -0.46 ± 0.45, and -0.59 ± 0.61 D in the atropine 0.05%, 0.025%, and 0.01% groups, and -0.81 ± 0.53 D in the placebo group, respectively (P < 0.001). The difference between each group was also significant for each pair wise comparison. At 12 months, 69.6%, 51.6% and 43.8% of participants in the 0.05%, 0.025% and 0.01% treatment groups progressed by < 0.5 D, compared to 24.2% in the placebo group.
Similarly, the change in AL was larger in the placebo group (0.41 ± 0.22 mm) than in the 0.05% (0.20 ± 0.25 mm), 0.025% (0.29 ± 0.20 mm) and 0.01% (0.36 ± 0.29 mm) atropine groups (P < 0.001). The difference between placebo and 0.01% group was not significant, however, for all other pair wise comparisons between active treatment groups, the difference was statistically significant (P < 0.001). At the end of the initial 12 month period, the placebo group was crossed over to 0.05% atropine drops.
Compared with the first year, the second-year efficacy of 0.05% and 0.025% atropine remained similar (P > 0.1) but improved mildly in the 0.01% atropine group (P = 0.04). For the phase 1 placebo group, the myopia progression was reduced significantly after switching to 0.05% atropine (SE change, 0.18 D in second year vs. 0.82 D in first year [P < 0.001]; AL elongated 0.15 mm in second year vs 0.43 mm in first year [P < 0.001]). Accommodation loss and change in pupil size in all concentrations remained similar to the first-year results and were well tolerated. Visual acuity and vision-related quality of life remained unaffected.
In the third phase, children were randomised to either continue treatment with 0.05%, 0.025% and 0.01% atropine drops as allocated, or to discontinue treatment (washout). The results for the continuous treatment subgroups using the 0.05%, 0.025%, and 0.01 % atropine drops were -0.28 ± 0.42 D, -0.35 ± 0.37 D, and -0.38 ± 0.49 D (P = 0.65), and the respective AL elongations 0.17 ± 0.14 mm, 0.20 ± 0.15 mm, and 0.24 ± 0.18 mm (P = 0.19).
After treatment cessation during the third year, the SE progression and axial elongation for the washout subgroups followed concentration-dependent response, that is, faster progressions at higher concentrations.
In the washout groups, there were no significant differences in SE progression across concentration groups, with respective SE progressions of -0.68 ± 0.49 D, -0.57 ± 0.38 D, and -0.56 ± 0.40 D (P = 0.15), but a large axial elongation in higher concentration, with the respective AL elongations 0.33 ± 0.17 mm, 0.29 ± 0.14 mm and 0.29 ± 0.15 mm (P = 0.003) (see Table 1).
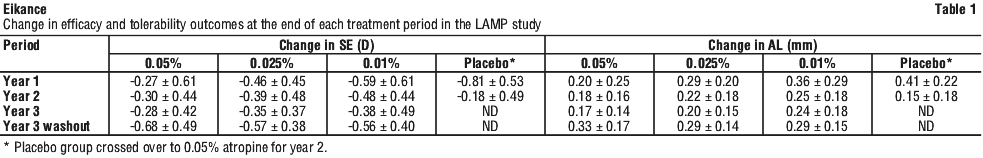
5.2 Pharmacokinetic Properties
Absorption. Atropine is readily absorbed from the gastrointestinal tract; it is also readily absorbed from mucous membranes, the eye, and to some extent through intact skin.
Following the instillation of 30 microlitres of 1% atropine sulfate ophthalmic solution (0.3 mg) into the lower cul-de-sac of one eye in young health volunteers, the average ocular bioavailability was estimated as 63.6 ± 28.6%. No cardiovascular changes were observed.
Distribution. It is rapidly cleared from the blood and is distributed throughout the body. It crosses the blood-brain barrier.
Metabolism. It is incompletely metabolised in the liver.
Excretion. It is excreted in the urine as unchanged drug and metabolites. A half-life of 4 hours has been reported.
5.3 Preclinical Safety Data
Genotoxicity. Available data are limited but indicate a lack of genotoxicity for atropine. Mutagenicity in bacteria and clastogenicity in vitro in human cells were not observed.
Carcinogenicity. No data available.
6 Pharmaceutical Particulars
6.1 List of Excipients
The product contains the following excipients: citric acid monohydrate, sodium chloride and purified water. Hydrochloric acid or sodium hydroxide is used to adjust pH.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging. Use within 3 months once the aluminium sachet is opened.
6.4 Special Precautions for Storage
Store below 25°C. Protect from light.
6.5 Nature and Contents of Container
Eikance eye drops are a clear, colourless solution filled into transparent low density polyethylene single-dose containers to a fill volume of 0.3 mL.
Strips of 5 single-dose containers are packed in an aluminium laminated foil sachet and available in 5#, 30, 60, and 90 packs*.
#The pack size of 5 ampoules is a stater pack.
*Not all pack sizes are marketed.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
Atropine sulfate monohydrate exists as odourless, colourless crystals or white crystalline powder. It effloresces in dry air. It is soluble in water (1 in 0.5), in boiling water (1 in 2.5), in alcohol (1 in 5), in glycerol (1 in 2.5), and is practically insoluble in chloroform and ether. A 2% solution in water has a pH of 4.5 to 6.2. Solutions may be sterilised by autoclave. Atropine sulfate monohydrate should be protected from light.
Chemical structure. Atropine sulfate monohydrate has the following chemical structure:
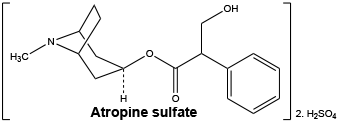
CAS number. CAS - 5908-99-6 [monohydrate].
7 Medicine Schedule (Poisons Standard)
Prescription Only Medicine: S4.
Date of First Approval
13 September 2021
Date of Revision
17 February 2026
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.