Estro-Pess Pessary
Brand Information
| Brand name | Estro-Pess Pessary |
| Active ingredient | Estradiol |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Estro-Pess Pessary.
Summary CMI
ESTRO-PESS pessary
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using ESTRO-PESS?
ESTRO-PESS contains the active ingredient estradiol (as hemihydrate). ESTRO-PESS is a local hormone replacement therapy (HRT) used to treat a condition called atrophic vaginitis.
For more information, see Section 1. Why am I using ESTRO-PESS? in the full CMI.
2. What should I know before I use ESTRO-PESS?
Do not use if you have ever had an allergic reaction to ESTRO-PESS or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I use ESTRO-PESS? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with ESTRO-PESS and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use ESTRO-PESS?
- The usual dose of ESTRO-PESS is 1 pessary each day for the first two weeks, then one pessary twice a week.
- The ESTRO-PESS pessary should be inserted into your vagina using the applicator (see the diagrams included in the ‘Directions for Use’ section of this leaflet).
More instructions can be found in Section 4. How do I use ESTRO-PESS? in the full CMI.
5. What should I know while using ESTRO-PESS?
| Things you should expect |
|
| Things you should do |
|
| Things you should not do |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using ESTRO-PESS? in the full CMI.
6. Are there any side effects?
Common side effects of ESTRO-PESS include headaches, abdominal pain, and vaginal bleeding, discharge, or discomfort. If you notice any of these common side effects, speak to your doctor. In rarer cases, a serious side effect may occur. These involve severe pain or swelling in your legs, or sudden chest pain and difficulty breathing, yellowing of the skin and eyes (jaundice), and a migraine-like headache (with no prior history of migraines). More serious side effects are listed in Section 6. Are there any side effects?. If you notice any of these serious side effects, call your doctor straight away or go to the Emergency Department at your nearest hospital, as you may need urgent medical attention. Taking HRT is associated with an increased risk of certain cancers, and cardiovascular disease (e.g. heart disease, stroke, blood clots).
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
ESTRO-PESS pessary
Active ingredient: estradiol (as hemihydrate)
Consumer Medicine Information (CMI)
This leaflet provides important information about using ESTRO-PESS.
You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using ESTRO-PESS.
Where to find information in this leaflet:
1. Why am I using ESTRO-PESS?
2. What should I know before I use ESTRO-PESS?
3. What if I am taking other medicines?
4. How do I use ESTRO-PESS?
5. What should I know while using ESTRO-PESS?
6. Are there any side effects?
7. Product details
1. Why am I using ESTRO-PESS?
ESTRO-PESS contains the active ingredient estradiol (as estradiol hemihydrate). The estradiol in ESTRO-PESS is identical to the estradiol produced in the ovaries of women and is classified as a natural estrogen.
ESTRO-PESS is a local hormone replacement therapy (HRT) used to treat a condition called atrophic vaginitis. The symptoms include dryness and irritation in the vagina and pain during sexual intercourse. Atrophic vaginitis is caused by a loss of the female sex hormone, estrogen, which occurs around the menopause. When placed in the vagina, ESTRO-PESS gradually releases estradiol. This may relieve discomfort in the vagina.
Ask your doctor if you have any questions about why ESTRO-PESS has been prescribed for you.
Your doctor may have prescribed ESTRO-PESS for another reason.
2. What should I know before I use ESTRO-PESS?
Warnings
Do not use ESTRO-PESS if:
- you have, you are suspected of having, or you have had breast cancer.
- you have, you are suspected of having, or you have had cancer which is sensitive to estrogens, such as cancer of the lining of the womb (endometrium).
- you have any unexplained vaginal bleeding.
- you have excessive thickening of the lining of the womb (endometrial hyperplasia) that is not being treated.
- you have or have ever had a blood clot in a vein (thrombosis), such as in the legs (deep venous thrombosis) or the lungs (pulmonary embolism)
- you have a blood clotting disorder (such as protein C, protein S or antithrombin deficiency).
- you have or have previously had a disease caused by blood clots in the arteries, such as a heart attack, stroke or angina.
- you have or have had a liver disease, and your liver function tests have not returned to normal.
- you have a rare blood problem called ‘porphyria’, which is passed down in families.
- you are pregnant or suspect you may be pregnant.
- you are breast-feeding.
- you are allergic to estradiol, or any of the ingredients listed at the end of this leaflet.
Symptoms of an allergic reaction may include shortness of breath, wheezing or difficulty in breathing; swelling of the face, lips, tongue, or any other parts of the body; rash, itching or hives on the skin. - the expiry date printed on the pack has passed.
- the packaging is torn or shows signs of tampering.
ESTRO-PESS should not be used in children or by males.
Stop using this medicine and consult your doctor immediately if any of the above conditions appear for the first time while using ESTRO-PESS.
Medical history and regular check-ups
The use of HRT carries risks which need to be considered when deciding whether to start taking it, or whether to carry on taking it.
Before you start or restart HRT, your doctor will ask about your own and your family's medical history. Your doctor may decide to perform a physical examination. This may include an examination of your breasts and/or an internal examination.
Once you've started on ESTRO-PESS, you should see your doctor for regular check-ups (3-6 months after starting ESTRO-PESS, and at least once a year thereafter).
Go for regular breast screening as recommended by your doctor.
There is only limited experience of treating women older than 65 years with ESTRO-PESS.
Vaginal infections should be treated before ESTRO-PESS are used.
Check with your doctor if you:
- have or have had any of the following health conditions:
- asthma
- epilepsy
- diabetes
- gallstones
- high blood pressure
- migraines or severe headaches
- a liver disorder, such as a benign liver tumour
- growth of womb lining outside your womb (endometriosis) or a history of excessive growth of the womb lining (endometrial hyperplasia)
- a disease affecting the eardrum and hearing (otosclerosis)
- a disease of the immune system that affects many organs of the body (systemic lupus erythematosus, SLE)
- increased risk of getting an estrogen-sensitive cancer (such as having a mother, sister or grandmother who has had breast cancer)
- increased risk of developing blood clots (see ‘Blood clots in a vein (thrombosis)’)
- fibroids inside your womb
- a very high level of fat in your blood (triglycerides)
- fluid retention due to cardiac or kidney problems.
Stop using ESTRO-PESS and see a doctor immediately if you experience any unexplained vaginal bleeding, or persistent or recurrent vaginal bleeding.
Pregnancy and breastfeeding
Talk to your doctor if you are pregnant, plan to be pregnant or if you are breastfeeding.
Risks associated with HRT
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
The following risks apply to HRT medicines in general, which circulate in the blood. It is not known how these risks apply to locally administered treatments such as ESTRO-PESS.
HRT and cancer
Excessive thickening of the lining of the womb (endometrial hyperplasia) and cancer of the lining of the womb (endometrial cancer)
Taking estrogen-only HRT tablets for a long time can increase the risk of developing cancer of the womb lining, the endometrium. It is uncertain whether long term (more than one year) or repeated use of local vaginally administered estrogen products possess a similar risk.
If you get breakthrough bleeding or spotting, it's usually nothing to worry about, but you should make an appointment to see your doctor. It could be a sign that your endometrium has become thicker.
Compare:
In women who still have a womb and who are not taking HRT, on average, 5 in 1,000 will be diagnosed with endometrial cancer between the ages of 50 and 65.
For women aged 50 to 65 who still have a womb and who take estrogen-only HRT, between 10 and 60 women in 1,000 will be diagnosed with endometrial cancer (i.e. between 5 and 55 extra cases), depending on the dose and for how long it is taken.
Breast cancer:
Evidence suggests that taking combined estrogen-progestagen and possibly also estrogen-only HRT increases the risk of breast cancer. The extra risk depends on how long you take HRT. The additional risk becomes clear within a few years. However, it returns to normal within a few years (at most 5) after stopping treatment.
For women who have had their womb removed and who are using estrogen-only HRT for 5 years, little or no increase in breast cancer risk is shown.
Compare:
Women aged 50 to 79 who are not taking HRT, on average, 9 to 17 in 1,000 will be diagnosed with breast cancer over a 5-year period. For women aged 50 to 79 who are taking estrogen-progestagen HRT over 5 years, there will be 13 to 23 cases in 1,000 users (i.e. an extra 4 to 6 cases).
Regularly check your breasts. See your doctor if you notice any changes such as:
- dimpling of the skin
- changes in the nipple
- any lumps you can see or feel dimpling of the skin.
Additionally, you are advised to join mammography screening programs when offered to you. For mammogram screening, it is important that you inform the nurse/healthcare professional who is taking the x-ray that you use HRT, as this medication may increase the density of your breasts which may affect the outcome of the mammogram. Where the density of the breast is increased, mammography may not detect all lumps.
Ovarian cancer:
Ovarian cancer is rare, much rarer than breast cancer. The use of estrogen-only or combined estrogen-progestagen HRT has been associated with a slightly increased risk of ovarian cancer.
Compare:
The risk of ovarian cancer varies with age. For example, in women aged 50 to 54 who are not taking HRT, about 2 women in 2,000 will be diagnosed with ovarian cancer over a 5-year period. For women who have been taking HRT for 5 years, there will be about 3 cases per 2,000 users (i.e. about 1 extra case).
Effect of HRT on the heart and circulation
Blood clots in a vein (thrombosis):
The risk of blood clots in the veins is about 1.3- to 3-times higher in HRT users than in non-users, especially during the first year of taking it.
Blood clots can be serious, and if one travels to the lungs, it can cause chest pain, breathlessness, fainting or even death.
You are more likely to get a blood clot in your veins as you get older and if any of the following applies to you.
Inform your doctor if any of these situations applies to you:
- you are unable to walk for a long time because of major surgery, injury or illness
- you are seriously overweight (BMI >30 kg/m²)
- you have any blood clotting problem that needs long-term treatment with a medicine used to prevent blood clots
- if any of your close relatives has ever had a blood clot in the leg, lung or another organ
- you have systemic lupus erythematosus (SLE)
- you have cancer.
If you notice signs of a blood clot stop using HRT and see a doctor immediately.
Compare:
Looking at women in their 50s who are not taking HRT, on average, over a 5-year period, 4 to 7 in 1,000 would be expected to get a blood clot in a vein.
For women in their 50s who have been taking estrogen-progestagen HRT for over 5 years, there will be 9 to 12 cases in 1,000 users (i.e. 5 extra cases).
For women in their 50s who have had their womb removed and have been taking estrogen-only HRT for over 5 years, there will be 5 to 8 cases in 1,000 users (i.e. 1 extra case).
Heart disease (heart attack):
There is no evidence that HRT will prevent a heart attack.
Women over the age of 60 years who use estrogen-progestagen HRT are slightly more likely to develop heart disease than those not taking any HRT.
For women who have had their womb removed and are taking estrogen-only therapy, there is no increased risk of developing a heart disease.
Stroke:
The risk of getting stroke is about 1.5-times higher in HRT users than in non-users. The number of extra cases of stroke due to use of HRT will increase with age.
Compare:
Looking at women in their 50s who are not taking HRT, on average, 8 in 1,000 would be expected to have a stroke over a 5-year period. For women in their 50s who are taking HRT, there will be 11 cases in 1,000 users, over 5 years (i.e. 3 extra cases).
Other conditions
HRT will not prevent memory loss. There is some evidence of a higher risk of memory loss in women who start using HRT after the age of 65.
Speak to your doctor for advice.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect ESTRO-PESS.
ESTRO-PESS contains a very small amount of hormone which should not interact with other medicines you are using.
4. How do I use ESTRO-PESS?
ESTRO-PESS is suitable for women who have had their womb removed (have had a hysterectomy) as well as for those who have not.
How much to use
The usual dose of ESTRO-PESS is 1 pessary each day for the first two weeks, then one pessary twice a week (allowing three to four days between doses).
When to use ESTRO-PESS
- You can start treatment with ESTRO-PESS on any convenient day.
- Your doctor will tell you for how long you should use ESTRO-PESS.
How to use it
- The ESTRO-PESS pessary is inserted into your vagina using the applicator (see the diagrams included in the ‘Directions for Use’ section of this leaflet).
- ESTRO-PESS treatment should not affect your normal hygiene routine or lifestyle.
If you forget to use ESTRO-PESS
If you forget to use ESTRO-PESS at the usual time, insert your pessary as soon as you remember.
Do not use a double dose to make up for the dose that you have missed.
If you use too much ESTRO-PESS
If you think that you have used too many pessaries, you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre (by calling 13 11 26), or
- contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
An overdose of this medicine may cause nausea and vomiting.
5. What should I know while using ESTRO-PESS?
- You can expect your symptoms to improve within a few weeks of starting ESTRO-PESS.
- ESTRO-PESS can be stopped at any time. You should discuss this with your doctor.
- ESTRO-PESS is not a contraceptive and will not prevent pregnancy.
Things you should do
- After starting ESTRO-PESS, you should see your doctor for regular check-ups (3-6 months after starting ESTRO-PESS, and at least once a year thereafter).
- Stop using ESTRO-PESS and see a doctor immediately if you become pregnant while using ESTRO-PESS.
Things you should not do
- Do not give this medicine to anyone else, even if their symptoms seem like yours.
- Do not use ESTRO-PESS to treat any other complaints unless your doctor tells you to.
- Do not change the way you use ESTRO-PESS, or change the dosage, without checking with your doctor.
- Do not swallow ESTRO-PESS.
This medicine is for vaginal use only.
Looking after your medicine
Keep ESTRO-PESS pessaries in the original carton protected from light.
Store this medicine in a cool dry place away from moisture or heat, where the temperature stays below 25°C.
For example, do not store it:
- in the refrigerator
- in the bathroom or near a sink, or
- in the car on a hot day.
Heat and dampness can destroy some medicines.
Keep it where young children cannot reach it.
Getting rid of any unwanted medicine
If you no longer need to use this medicine or it is out of date, take it to any pharmacy for safe disposal.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
| Speak to your doctor if you have any of these less serious, common side effects. |
Very rare side effects
| Serious side effects | What to do |
| Speak to your doctor if you have any of these very rare side effects. |
Reasons for immediate withdrawal
| Reasons for immediate withdrawal | What to do |
| Tell your doctor immediately. You may be told to stop using ESTRO-PESS if any of these conditions occur. |
Tell your doctor if you are not feeling well, find any side effect too uncomfortable or unacceptable or if any side effect becomes worse.
Cancer of the breast, ovaries or the lining of the womb, blood clots and stroke have been reported with some types of systemic hormone replacement therapy (“systemic” means to affect the body as a whole).
The following additional side effects have been reported to be associated with other types of estrogen treatment:
- heart attack or heart disease
- gall bladder disease
- various skin diseases and itching
- increase in size of uterine fibroids
- epilepsy
- libido disorder
- asthma
- probable dementia.
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What ESTRO-PESS contains
| Active ingredient (main ingredient) |
|
| Other ingredients (inactive ingredients) |
|
| Potential allergens |
|
Do not take this medicine if you are allergic to any of these ingredients.
What ESTRO-PESS looks like
ESTRO-PESS is a white, round, film coated tablet embossed with "E" one side and plain on the other side. The tablet is a modified release pessary designed for internal vaginal use. Available in blister packs of 18 pessaries with 6 reusable applicators.
Do not dispose of the applicators until all the tablets in the pack have been used.
Australian Registration number: AUST R 339050
Who distributes ESTRO-PESS
Aspen Pharmacare Australia Pty Ltd
34-36 Chandos St
St Leonards NSW 2065
Australia
This leaflet was revised in September 2025.
Directions for Use
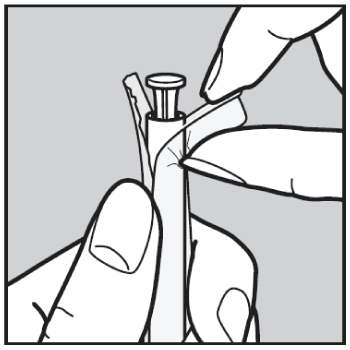
- Wash hands well. Take out the applicator. Open the end as shown in the picture.
- Pull the plunger out of the applicator until it comes to a stop.
Remove one vaginal tablet from the enclosed blister pack and insert into the applicator as follows:
Place the vaginal tablet firmly in the holder of the applicator end (wide end).
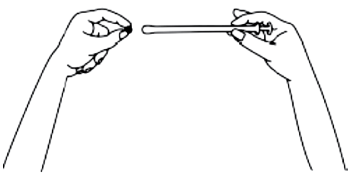
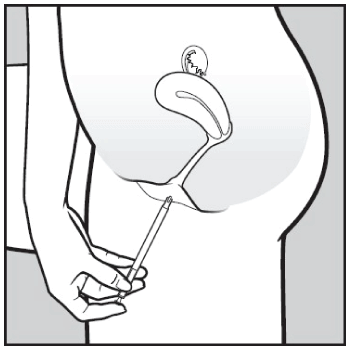
- Insert the applicator carefully into the vagina. Stop when you can feel some resistance (8-10 cm).
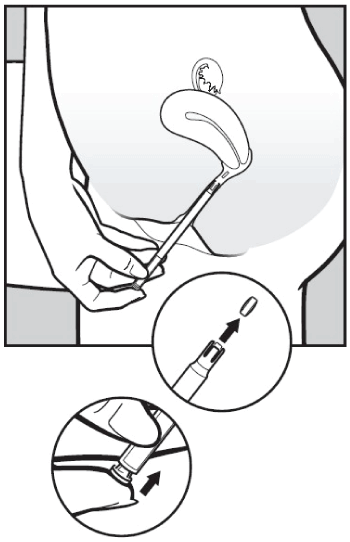
- To release the pessary, gently press the push button until you feel a click. The pessary will stick to the wall of the vagina straight away. It will not fall out if you stand up or walk.
- Take out the applicator and follow the washing instructions below.
After each use, clean the applicator as follows:
- Withdraw the plunger from the applicator.
- Clean both parts (tube and plunger) with mild soap and rinse with warm tap water for 5 seconds. Rinse the tube's inner and outer surface.
- If necessary, remove larger amounts of remaining water from both parts (tube and plunger) by shaking off the water.
- Air dry both parts (tube and plunger) on a clean surface (e.g. clean paper fleece)
- Introduce the plunger again in the applicator-tube for the next use of the applicator.
- The vaginal tablet applicator can be used for up to 24 times for one single patient. Remove the applicator when the pack is empty and dispose of as household waste. Do not use applicators that show obvious signs of damage.
Brand Information
| Brand name | Estro-Pess Pessary |
| Active ingredient | Estradiol |
| Schedule | S4 |
MIMS Revision Date: 01 May 2024
1 Name of Medicine
Estradiol.
2 Qualitative and Quantitative Composition
Each Estro-Pess pessary contains 10.3 microgram estradiol hemihydrate, equivalent to 10 microgram of estradiol.
Estro-Pess is an estrogen preparation for intravaginal application based on the active human estrogen estradiol. The Estro-Pess modified release pessary formulation is based on a hydrophilic cellulose-derived matrix which on contact with moisture hydrates and provides a controlled release of estradiol.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Modified release pessary. Each pessary is white, round, film coated tablet embossed with "E" one side and plain on the other side.
4 Clinical Particulars
4.1 Therapeutic Indications
Estro-Pess is indicated for the treatment of atrophic vaginitis due to estrogen deficiency in postmenopausal women.
Estro-Pess is not intended for children or males.
4.2 Dose and Method of Administration
Dosage. Estro-Pess may be used in women with or without an intact uterus.
Initial dose. 1 modified release pessary daily for 2 weeks.
Maintenance dose. 1 modified release pessary twice a week.
For initiation and continuation of treatment of postmenopausal symptoms, the lowest effective dose for the shortest duration (see Section 4.4 Special Warnings and Precautions for Use) should be used. Patient review should occur 3-6 months after treatment initiation. Reassessment of risks and benefits should occur no less frequently than annually.
Method of administration. Estro-Pess is administered deep intravaginally using the applicator(s) in the enclosed pack.
1. Open the blister pack and remove the applicator.
2. Pull the plunger out of the applicator until it comes to a stop. Press a vaginal tablet from the separate blister and place it firmly in the holder of the applicator end (wide end).
3. Insert the applicator carefully into the vagina. Stop when you can feel some resistance (8-10 cm).
4. To release the vaginal tablet, press the push-button until the end of the plunger. The tablet will stick to the wall of the vagina straight away. It will not fall out if you stand up or walk.
5. Immediately after each use, clean the applicator according to the cleaning procedure described below and in the packaging leaflet.
6. The applicator can be used for up to 24 times. Remove the applicator when the pack is empty and dispose of as household waste.
If a dose is forgotten, it should be taken as soon as the patient remembers. A double dose should be avoided.
After each use clean the applicator as follows. 1. Withdraw the plunger from the applicator.
2. Clean both parts (tube and plunger) with mild soap and rinse with warm tap water for 5 seconds. Rinse tubes inner and outer surface.
3. If necessary, remove larger amounts of remaining water from both parts (tube and plunger) by shaking-off the water.
4. Air dry both parts (tube and plunger) on a clean surface (e.g. clean paper fleece).
5. Introduce the plunger again in the applicator-tube for the next use of the applicator.
Directions for use. 1. Wash hands well. Take out the applicator. Open the end.
2. Pull the plunger out of the applicator until it comes to a stop.
3. Remove one vaginal tablet from the enclosed blister pack and insert into the applicator.
4. Place the vaginal tablet firmly in the holder of the applicator end (wide end).
5. Insert the applicator carefully into the vagina. Stop when you can feel some resistance (8-10 cm).
6. To release the pessary, gently press the push button until you feel a click. The pessary will stick to the wall of the vagina straight away. It will not fall out if you stand up or walk.
7. Take out the applicator and follow the washing instructions.
4.3 Contraindications
Known, suspected or past history of carcinoma of the breast.
Known, suspected or past history of estrogen dependent neoplasia, e.g. endometrial carcinoma or other hormone dependent tumour.
Abnormal genital bleeding of unknown aetiology.
Known or suspected pregnancy.
Untreated endometrial hyperplasia.
Previous or current venous thromboembolism (deep venous thrombosis, pulmonary embolism).
Known thrombophilic disorders (e.g. protein C, protein S, or antithrombin deficiency, see Section 4.4 Special Warnings and Precautions for Use).
Active or previous arterial thromboembolic disease (e.g. angina, myocardial infarction).
Acute liver disease, or a history of liver disease as long as liver function tests have failed to return to normal.
Porphyria.
Known hypersensitivity to the active substance or to any of the excipients.
4.4 Special Warnings and Precautions for Use
Hormone Replacement Therapy (HRT) should only be initiated for the short-term treatment of postmenopausal symptoms that adversely affect quality of life. In all cases, a careful appraisal of the risks and benefits should be undertaken.
Evidence regarding the risks associated with HRT in the treatment of premature menopause is limited.
Medical examination/follow-up. Before initiating or reinstituting therapy with Estro-Pess it is advisable to undertake a thorough examination to exclude any possibility of genital or mammary tumours. A complete personal and family medical history should be taken. Physical (including pelvic and breast) examination should be guided by this and by the contraindications and precautions for use. Vaginal infections should be treated before initiation of Estro-Pess therapy.
During treatment, periodic check-ups are recommended of a frequency and nature adapted to the individual woman, but no less frequently than annually. Women should be advised what changes in their breasts should be reported to their doctor or nurse. Investigations including appropriate imaging tools, e.g. mammography should be carried out in accordance with currently accepted screening practices, modified to the clinical needs of the individual.
Persistent or recurring vaginal bleeding should be investigated.
The pharmacokinetic profile of estradiol hemihydrate pessary shows that there is very low systemic absorption of estradiol during treatment (see Section 5.2 Pharmacokinetic Properties), however being an HRT product the following need to be considered, especially for long-term or repeated use of these products.
Conditions which need supervision. If any of the following conditions are present, have occurred previously, and/or have been aggravated during pregnancy or previous hormone treatment, the patient should be closely supervised. It should be taken into account that these conditions may recur or be aggravated during estrogen treatment. Patients with the following conditions should be monitored frequently and if any of the conditions worsen, Estro-Pess treatment should be withdrawn.
Leiomyoma (uterine fibroids) or endometriosis.
Liver disorders (e.g. liver adenoma).
Cholelithiasis.
Risk factors for estrogen dependent tumours, e.g. 1st degree heredity for breast cancer.
Risk factors for thromboembolic disorders (see below).
Haemoglobinopathies or sickle-cell anaemia.
Epilepsy.
Migraine or severe headache.
Diabetes mellitus with or without vascular involvement.
Asthma.
Cardiac dysfunction.
Hypertension.
Systemic lupus erythematosus (SLE).
A history of endometrial hyperplasia (see below).
Otosclerosis.
Reasons for immediate withdrawal of therapy. Therapy should be discontinued upon discovery of a contraindication and in the following situations.
Jaundice or deterioration in liver function.
Significant increase in blood pressure.
New onset of migraine type headache.
Pregnancy.
Venous thromboembolism. HRT is associated with a 1.3 to 3-fold risk of developing venous thromboembolism (VTE), i.e. deep vein thrombosis or pulmonary embolism. The occurrence of such an event is more likely in the first year of HRT than later (see Section 4.8 Adverse Effects (Undesirable Effects)).
Patients with known thrombophilic states have an increased risk of VTE and HRT may add to this risk. HRT is therefore contraindicated in these patients (see Section 4.3 Contraindications).
Generally recognised risk factors for VTE include use of estrogens, older age, major surgery, prolonged immobilisation, obesity (BMI > 30 kg/m2), pregnancy/postpartum period, systemic lupus erythematosus (SLE) and cancer. There is no consensus about the possible role of varicose veins in VTE.
A relationship between venous thromboembolism and low dose local vaginal estrogen therapy is uncertain.
As in all postoperative patients, prophylactic measures need to be considered to prevent VTE following surgery. If prolonged immobilisation is to follow elective surgery, temporarily stopping HRT 4 to 6 weeks earlier is recommended. Treatment should not be restarted until the woman is completely mobilised.
In women with no personal history of VTE but with a first degree relative with a history of thrombosis at a young age, screening may be offered after careful counselling regarding its limitations (only a proportion of thrombophilic defects are identified by screening).
If a thrombophilic defect is identified which segregates with thrombosis in family members or if the defect is 'severe' (e.g. antithrombin, protein S, or protein C deficiencies or a combination of defects), HRT is contraindicated.
Women already on chronic anticoagulant treatment require careful consideration of the benefit-risk of use of HRT.
If VTE develops after initiating therapy, the drug should be discontinued. Patients should be told to contact their doctors immediately when they are aware of a potential thromboembolic symptom (e.g. painful swelling of a leg, sudden pain in the chest, dyspnoea).
Coronary artery disease (CAD). There is no evidence from randomised controlled trials of protection against myocardial infarction in women with or without existing CAD who received combined estrogen-progestagen or estrogen only therapy.
Ischaemic stroke. Combined estrogen-progestagen and estrogen only therapy are associated with an up to 1.5-fold increase in risk of ischaemic stroke. The relative risk does not change with age or time since menopause. However, as the baseline risk of stroke is strongly age-dependent, the overall risk of stroke in women who use HRT increase with age (see Section 4.8 Adverse Effects (Undesirable Effects)).
A relationship between ischaemic stroke and low dose local vaginal estrogen therapy is uncertain.
Endometrial hyperplasia and carcinoma. Women with an intact uterus with abnormal bleeding of unknown aetiology or women with an intact uterus who have previously been treated with unopposed estrogens should be examined with special care in order to exclude hyperstimulation/malignancy of the endometrium before initiation of treatment with estradiol hemihydrate pessary.
There is some evidence that obesity and possibly hypertension or diabetes mellitus are predisposing factors to endometrial carcinoma. In view of this, special care should be taken in the presence of these conditions and also if a family history of endometrial carcinoma is present. Endometrial hyperplasia (atypical or adenomatous) often precedes endometrial cancer.
The risk of endometrial cancer after treatment with oral unopposed estrogens is dependent on both duration of treatment and on estrogen dose. In women with an intact uterus the risk of endometrial hyperplasia and carcinoma is increased when estrogens are administered alone for prolonged periods. The reported increase in endometrial cancer risk among systemic estrogen only users varies from 2 to 12-fold compared with non-users, depending on both duration of treatment and on estrogen dose. After stopping treatment, risk may remain elevated for at least 10 years.
Endometrial safety of long-term (more than one year) or repeated use of local vaginally administered estrogen is uncertain. Therefore, if repeated, treatment should be reviewed at least annually, with special consideration given to any symptoms of endometrial hyperplasia or carcinoma.
As a general rule, estrogen replacement therapy should not be prescribed for longer than one year without another physical, including gynaecological, examination being performed.
If bleeding or spotting appears at any time during therapy, the reason should be investigated, which may include endometrial biopsy to exclude endometrial malignancy.
The woman should be advised to contact her doctor in case bleeding or spotting occurs during treatment with Estro-Pess.
Unopposed estrogen stimulation may lead to premalignant or malignant transformation in the residual foci of endometriosis. Therefore caution is advised when using these products in women who have undergone hysterectomy because of endometriosis, especially if they are known to have residual endometriosis.
Breast cancer. Epidemiological evidence from a large meta-analysis suggests no increase in risk of breast cancer in women with no history of breast cancer taking low dose vaginally applied estrogens. It is unknown if low dose vaginal estrogens stimulate recurrence of breast cancer.
Ovarian cancer. Ovarian cancer is much rarer than breast cancer. Epidemiological evidence from a large meta-analysis suggests a slightly increased risk in women taking estrogen only or combined estrogen-progestogen HRT, which becomes apparent within 5 years of use and diminishes over time after stopping. Some other studies, including the WHI trial, suggest that use of combined HRTs may be associated with a similar or slightly smaller risk (see Section 4.8 Adverse Effects (Undesirable Effects)).
A relationship between ovarian cancer risk and low dose local vaginal estrogen therapy is uncertain.
Other conditions. Estrogens may cause fluid retention, and therefore patients with cardiac or renal dysfunction should be carefully observed.
Women with pre-existing hypertriglyceridaemia should be followed closely during estrogen replacement or hormone replacement therapy, since rare cases of large increases of plasma triglycerides leading to pancreatitis have been reported with estrogen therapy in this condition.
The relationship between pre-existing hypertriglyceridaemia and low dose local vaginal estrogen therapy is unknown.
Exogenous oestrogens may induce or exacerbate symptoms of hereditary and acquired angioedema.
Estrogens increase thyroid binding globulin (TBG), leading to increased circulating total thyroid hormone (as measured by protein-bound iodine (PBI)), T4 levels (by column or by radioimmunoassay) or T3 levels (by radioimmunoassay). T3 resin uptake is decreased, reflecting the elevated TBG. Free T4 and free T3 concentrations are unaltered. Other binding proteins may be elevated in serum, i.e. corticoid binding globulin (CBG), sex hormone-binding globulin (SHBG) leading to increased circulating corticosteroids and sex steroids, respectively. Free or biologically active hormone concentrations are unchanged. Other plasma proteins may be increased (angiotensinogen/renin substrate, alpha-1-antitrypsin, ceruloplasmin).
HRT does not improve cognitive function. There is some evidence from the WHI trial of increased risk of probable dementia in women who start using continuous combined or estrogen-only HRT after the age of 65.
Intravaginal applicator may cause minor local trauma, especially in women with serious vaginal atrophy.
Use in the elderly. The experience of treating women older than 65 years of age is limited.
Paediatric use. No data available.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Due to the local administration of the low dose of estradiol in Estro-Pess, interactions of clinical relevance are not expected.
However, the metabolism of estrogens may be increased by concomitant use of substances known to induce drug-metabolising enzymes, specifically cytochrome P450 enzymes, such as anticonvulsants (e.g. phenobarbital, phenytoin, carbamazepine) and anti-infectives (e.g. rifampicin, rifabutin, nevirapine, efavirenz).
Ritonavir and nelfinavir, although known as strong inhibitors, by contrast exhibit inducing properties when used concomitantly with steroid hormones. Herbal preparations containing St John's wort (Hypericum perforatum) may induce the metabolism of estrogens.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. No data available.
Use in pregnancy. (Category B3)
Estro-Pess is contraindicated during pregnancy. If pregnancy occurs during medication with Estro-Pess, treatment should be withdrawn immediately. In animal studies, maternal administration of high doses of estrogens has produced urogenital malformations in the offspring. The relevance of these animal findings for the clinical use of estradiol is uncertain, but is considered likely to be low.
Use in lactation. Estro-Pess is not indicated during lactation.
4.7 Effects on Ability to Drive and Use Machines
The effects of this medicine on a person's ability to drive and use machines were not assessed as part of its registration.
4.8 Adverse Effects (Undesirable Effects)
Clinical trial experience. More than 692 patients have been treated with estradiol hemihydrate pessaries in clinical trials, including over 456 patients treated up to 52 weeks. The most commonly reported adverse drug reactions were vulvovaginal mycotic infection and vulvovaginal pruritus.
If noted, estrogen related adverse events such as breast pain, peripheral oedema and postmenopausal bleeding were most likely to be present at the beginning of estradiol hemihydrate pessary treatment.
Adverse drug reactions which occurred with a higher frequency in the treated group as compared with the placebo group and which are possibly related to treatment, are presented in Table 1.
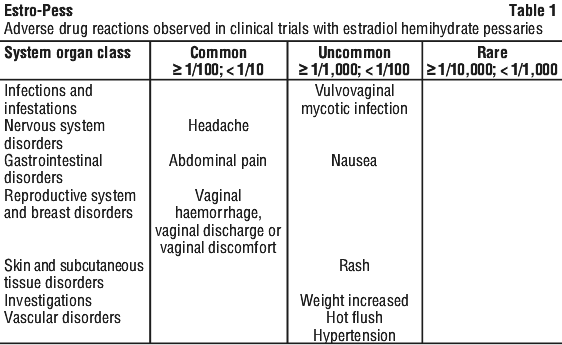
Postmarketing experience. In addition to the above mentioned adverse drug reactions, those presented below have been spontaneously reported for patients being treated with estradiol 25 microgram vaginal pessary, and are considered possibly related to treatment. The reporting rate of these spontaneous adverse drug reactions is very rare (< 1/10,000 patient years). Postmarketing experience is subject to underreporting especially with regard to trivial and well known adverse drug reactions. The presented frequencies should be interpreted in that light.
Neoplasms benign and malignant (including cysts and polyps). Breast cancer, endometrial cancer.
Immune system disorders. Generalised hypersensitivity reactions (e.g. anaphylactic reaction/shock).
Metabolism and nutrition disorders. Fluid retention.
Psychiatric disorders. Insomnia, depression.
Nervous system disorders. Migraine aggravated.
Vascular disorders. Deep venous thrombosis.
Gastrointestinal disorders. Diarrhoea.
Skin and subcutaneous tissue disorders. Urticaria, rash erythematous, rash NOS (not otherwise specified), rash pruritic.
Reproductive system and breast disorders. Endometrial hyperplasia, vaginal irritation, vaginal pain, vaginismus, vaginal ulceration, vulvovaginal pain1, pruritus genital.
General disorders and administration site conditions. Drug ineffective, application site reaction2, injury associated with device3.
Investigations. Weight increased, blood estrogen increased.
1 Including vulvovaginal burning sensation.
2 Local allergic reactions including vulvovaginal erythema, genital erythema, vulvovaginal rash, genital rash.
3 Minor local trauma caused by intravaginal applicator.
Other adverse reactions have been reported in association with estrogen treatment. Risk estimates have been drawn from systemic exposure and it is not known how these apply to local treatments.
Myocardial infarction, congestive heart disease.
Stroke.
Gall bladder disease.
Skin and subcutaneous disorders: chloasma, erythema multiforme, erythema nodosum, vascular purpura, pruritus, angioedema.
Endometrial cancer (see Section 4.4 Special Warnings and Precautions for Use), endometrial hyperplasia.
Increase in size of uterine fibroids.
Insomnia.
Epilepsy.
Libido disorder.
Deterioration of asthma.
Probable dementia (see Section 4.4 Special Warnings and Precautions for Use).
Endometrial cancer risk. Postmenopausal women with a uterus. The endometrial cancer risk is about 5 in every 1,000 women with a uterus not using HRT. In women with a uterus, use of systemic estrogen-only HRT is not recommended because it increases the risk of endometrial cancer (see Section 4.4 Special Warnings and Precautions for Use). Depending on the duration of systemic estrogen only use and estrogen dose, the increase in risk of endometrial cancer in epidemiology studies varied from between 5 and 55 extra cases diagnosed in every 1000 women between the ages of 50 and 65. Adding a progestogen to systemic estrogen-only therapy for at least 10 days per cycle can prevent this increased risk. In the Million Women Study the use of five years of combined (sequential or continuous) HRT did not increase risk of endometrial cancer (RR of 1.0 (0.8-1.2)). Please also see Section 4.4 Special Warnings and Precautions for Use.
Ovarian cancer. Risk estimates have been drawn from systemic exposure and it is not known how these apply to local treatments. Use of estrogen-only or combined estrogen-progestagen HRT has been associated with a slightly increased risk of having ovarian cancer diagnosed (see Section 4.4 Special Warnings and Precautions for Use).
A meta-analysis from 52 epidemiological studies reported an increased risk of ovarian cancer in women currently using HRT compared to women who have never used HRT (RR 1.43, 95% CI 1.31-1.56). For women aged 50 to 54 years taking 5 years of HRT, this results in about 1 extra case per 2,000 users. In women aged 50 to 54 who are not taking HRT, about 2 women in 2,000 will be diagnosed with ovarian cancer over a 5-year period.
Risk of venous thromboembolism. Risk estimates have been drawn from systemic exposure and it is not known how these apply to local treatments. HRT is associated with a 1.3 to 3-fold increased relative risk of developing venous thromboembolism (VTE), i.e. deep vein thrombosis or pulmonary embolism. The occurrence of such an event is more likely in the first year of using HRT (see Section 4.4 Special Warnings and Precautions for Use). Results of the WHI studies are presented in Table 2.

Risk of ischaemic stroke. Risk estimates have been drawn from systemic exposure and it is not known how these apply to local treatments. The use of estrogen only and estrogen-progestagen therapy is associated with an up to 1.5-fold increased relative risk of ischaemic stroke. The risk of haemorrhagic stroke is not increased during use of HRT. This relative risk is not dependent on age or on duration of use, but as the baseline risk is strongly age-dependent, the overall risk of stroke in women who use HRT will increase with age, see Section 4.4 Special Warnings and Precautions for Use. See Table 3.

4.9 Overdose
Estro-Pess is intended for intravaginal use only and the dose of estradiol is low. Treatment should be symptomatic. An overdose of estrogen may cause nausea and vomiting.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
During the climacteric the decline in endogenous estrogen production causes atrophic changes in the vaginal mucosa which may induce symptoms such as vaginal dryness, irritation and dyspareunia.
5.1 Pharmacodynamic Properties
Mechanism of action. Estradiol hemihydrate pessaries relieves the symptoms of atrophic vaginitis due to estrogen deficiency following the menopause. Estradiol hemihydrate pessaries therapy reverses the atrophic changes due to estrogen deficiency found in the affected postmenopausal vagina. The active ingredient, synthetic 17β-estradiol, is chemically and biologically identical to endogenous human estradiol.
Endogenous 17β-estradiol induces and maintains the primary and secondary female sexual characteristics. The biological effect of 17β-estradiol is carried out through a number of specific estrogen receptors. The steroid receptor complex is bound to the cell's DNA and induces synthesis of specific proteins.
Maturation of the vaginal epithelium is dependent upon estrogen. Estrogen increases the number of superficial and intermediate cells as compared to basal cells.
Estrogen keeps pH in the vagina down to around 4.5 which enhances normal bacterial flora, Lactobacillus doderlein predomination.
Clinical trials. Vag-2195 was a 12-month double-blind, randomised, parallel group, placebo-controlled multicenter study was conducted to evaluate the efficacy and safety of estradiol hemihydrate pessaries in the treatment of postmenopausal symptoms of vaginal atrophy. Subjects were predominantly Caucasian (92.9%) and had a mean age of 57.6 years, BMI of 25 kg/m2, and were on average 8.1 years from last menses. The primary efficacy endpoints were the mean change from baseline to week 12 in: 1) Vaginal Maturation Index (parabasal and superficial cells) and Value; 2) vaginal pH; and 3) the moderate to severe symptom that was identified by the subject as being most bothersome. Vaginal Maturation Index (MI) was expressed as percentages of parabasal, intermediate, and superficial cells. The Vaginal Maturation Value (MV) was calculated using: MV = 0 x % parabasal cells + 0.5 x % intermediate cells + 1.0 x % superficial cells. Vaginal pH was recorded within four intervals (< 5, 5-5.49, 5.5-6.49, and > 6.49). These observations were graded on a 4-point scale (no atrophy=0, mild=1, moderate=2, or severe=3 respectively).
After 12 weeks of treatment with estradiol hemihydrate pessary, significant improvements from baseline and versus placebo were demonstrated for the three primary endpoints. Cytologically, a shift towards normalisation in the proportion of parabasal, intermediate, and superficial cells was apparent after Week 2 and sustained through the Week 52 evaluation point (p < 0.001).
Parabasal cells. The mean change from baseline to Week 12 (LOCF) for estradiol hemihydrate pessary was -37.0% compared to -9.3% for the placebo group (p < 0.001).
Superficial cells. At baseline, the proportion of superficial cells was < 5%. After 2 weeks of daily administration with estradiol hemihydrate pessary, superficial cells comprised approximately 27% of the total cell count, which was statistically significant compared to placebo treatment (p < 0.001). The mean change from baseline to Week 12 (LOCF) was 13.2% compared to 3.8% for placebo (p < 0.001).
Intermediate cells. The mean change from baseline to Week 12 (LOCF) was approximately 24% (p < 0.001, compared to placebo).
Maturation Value (MV) at Week 12 (LOCF) was 35.9 for placebo and 55.5 for estradiol hemihydrate pessary. The mean change in MV from baseline to Week 12 (LOCF) was 6.5 for placebo and 25.0 for estradiol hemihydrate pessary p < 0.001. A statistically significant treatment effect was apparent after 2 weeks of study drug administration. The mean change from baseline to Week 2 in MV was 8.3 for placebo and 31.6 for estradiol hemihydrate pessary (p < 0.001). These effects were sustained at Week 52 (LOCF): the mean change from baseline for the placebo-treatment group was 5.9 and for estradiol hemihydrate pessary treated subjects was 24.5, p < 0.001.
Vaginal pH. Within 2 weeks of treatment with estradiol hemihydrate pessary, the vaginal pH grade was significantly improved versus placebo (p < 0.001), which was sustained at the Week 12 (LOCF) (p < 0.001) and Week 52 (LOCF) (p < 0.001). See Table 4.

5.2 Pharmacokinetic Properties
The modified release pessary formulation of estradiol hemihydrate pessary is based on a hydrophilic cellulose derived matrix which hydrates on contact with moisture to give a controlled release of the soluble estradiol. Once the pessary is in place, it adheres to the vaginal mucosa. The polymer selected for the gel matrix hydrates quickly so that a gel layer is formed before the contents of the pessary begin to dissolve. Soluble estradiol is gradually released from the hydrophilic matrix.
Estrogen drug products are well absorbed through the skin, mucous membranes, and the gastrointestinal tract. The vaginal delivery of estrogens circumvents first-pass metabolism. After treatment with estradiol hemihydrate pessary, marginal elevations of plasma estradiol and its metabolites have been observed. This indicates that some absorption of estradiol occurs. Absorption is low as shown in the study described below.
A 12 week, single-centre randomised, open label, multiple dose, parallel-group trial was conducted to evaluate the extent of systemic absorption of estradiol from estradiol hemihydrate pessary. Subjects were randomised 1:1 to receive either 25 micrograms estradiol (E2) vaginal pessary or 10 micrograms E2 (estradiol hemihydrate pessary). Plasma levels of E2, estrone (E1) and estrone sulfate (E1S) were determined at Day-1 (predose), Day 1 (after 1st dosing), Day 14 (after 14 days of once-daily dosing), Day 82 (pre-dose after 10 weeks twice weekly treatment) and Day 83 (post-dose after 10 weeks twice-weekly treatment). The primary bioavailability endpoint of the clinical trial was AUC(0-24) for plasma E2 levels (see Table 5): this parameter indicated higher systemic estradiol levels for estradiol hemihydrate pessary as compared to baseline on treatment days 1, 14 and 83. However, average plasma E2 concentrations (Cave(0-24)) at all timepoints overall remained below 20 picogram/mL (below approx. 73.4 picomol/L) and therefore within the normal postmenopausal range. The data from day 82 indicate that in the long term, systemic estradiol levels do not accumulate during twice weekly maintenance therapy (see Table 5).
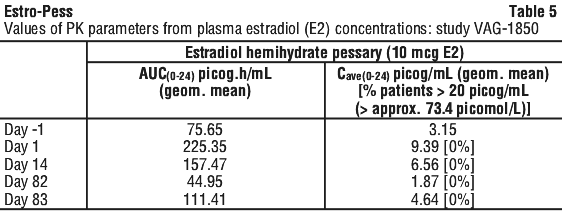
Estrogen metabolites are primarily excreted in the urine as glucuronides and sulfates.
5.3 Preclinical Safety Data
Genotoxicity. There is limited evidence available in the literature suggesting that estradiol may be weakly genotoxic. No evidence could be found for an increase in the rate of gene mutation in bacterial or mammalian cells, but there was some evidence for the induction of chromosomal aberrations and aneuploidy and an increased incidence of sister chromatid exchanges (indicative of DNA damage) in mammalian cells. None of these effects were induced by estradiol in human lymphocyte cultures. Importantly, there was no evidence of clastogenicity in rodent bone marrow micronucleus assays.
Carcinogenicity. Supra-physiological doses of estradiol have been associated with the induction of tumours in estrogen-dependent target organs in all rodent species tested. The relevance of these findings with respect to humans has not been established.
6 Pharmaceutical Particulars
6.1 List of Excipients
Pessary core. Hypromellose, lactose monohydrate, maize starch, magnesium stearate.
Film coating. Hypromellose, macrogol 6000.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C. Store in a dry place protected from light. Do not refrigerate.
6.5 Nature and Contents of Container
The Estro-Pess modified release pessaries are packed in PVC/PVDC/Aluminium blister packs.
The multi-use polyethylene/polypropylene applicators are packed separately in aluminium foil packs.
18 packs - 18 pessaries + 1 applicator.
18 packs - 18 pessaries + 6 applicators.
24 packs - 24 pessaries + 1 applicator.
24 packs - 24 pessaries + 6 applicators.
Not all pack sizes may be marketed.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking it to your local pharmacy.
6.7 Physicochemical Properties
Estradiol hemihydrate is a white or almost white crystalline powder which is practically insoluble in water and soluble in acetone.
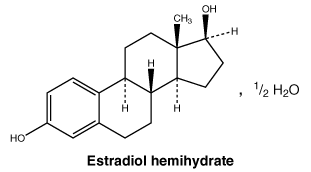
Chemical structure. Active ingredients: estradiol - chemical name: estra-1,3,5(10)-triene-3, 17β-diol (as hemihydrate). Estradiol hemihydrate has 5 chiral centres. The molecular formula is C18H24O2.½H2O.
Estradiol hemihydrate has a molecular weight of 281.39.
7 Medicine Schedule (Poisons Standard)
S4 Prescription Only Medicine.
Date of First Approval
30 March 2022
Date of Revision
07 March 2024
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.