Extraneal
Brand Information
| Brand name | Extraneal |
| Active ingredient | Calcium chloride dihydrate + Icodextrin + Magnesium chloride hexahydrate + Sodium lactate + Sodium chloride |
| Schedule | Unscheduled |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Extraneal.
Summary CMI
EXTRANEAL
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using EXTRANEAL?
EXTRANEAL contains the active ingredients icodextrin, sodium chloride, sodium lactate, calcium chloride dihydrate and magnesium chloride hexahydrate. EXTRANEAL Peritoneal dialysis solution is an alternative fluid to be used in chronic kidney failure patients being treated on peritoneal dialysis. For more information, see Section 1. Why am I using EXTRANEAL? in the full CMI.
2. What should I know before I use EXTRANEAL?
Do not use EXTRANEAL if you have ever had an allergic reaction to EXTRANEAL or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding. For more information, see Section 2. What should I know before I use EXTRANEAL? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with EXTRANEAL and affect how it works. A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use EXTRANEAL?
- Follow all directions given to you by your doctor or nurse or pharmacist carefully.
- EXTRANEAL solutions are intended for use via PD catheter only. Aseptic techniques must be maintained during the bag connection in order to reduce the risk of infection.
- Do not use EXTRANEAL if the solution is discoloured, cloudy, contains particulate matter or shows evidence of leakage or if seals are not intact.
- EXTRANEAL bags should be used only once and any unused solution remaining must be discarded.
More instructions can be found in Section 4. How do I use EXTRANEAL? in the full CMI.
5. What should I know while using EXTRANEAL?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using EXTRANEAL? in the full CMI.
6. Are there any side effects?
You may experience side effects such as hernia, abdominal pain, bleeding, peritonitis, infection around the catheter and catheter blockage and electrolyte imbalances as part of peritoneal dialysis treatment.
For more information, including full list of possible side effects and what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
EXTRANEAL
Active ingredient(s): Icodextrin, sodium chloride, sodium lactate, calcium chloride dihydrate and magnesium chloride hexahydrate
Consumer Medicine Information (CMI)
This leaflet provides important information about using EXTRANEAL. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using EXTRANEAL.
Where to find information in this leaflet:
1. Why am I using EXTRANEAL?
2. What should I know before I use EXTRANEAL?
3. What if I am taking other medicines?
4. How do I use EXTRANEAL?
5. What should I know while using EXTRANEAL?
6. Are there any side effects?
7. Product details
1. Why am I using EXTRANEAL?
EXTRANEAL contains the active ingredients icodextrin, sodium chloride, sodium lactate, calcium chloride dihydrate and magnesium chloride hexahydrate. EXTRANEAL is a solution for peritoneal dialysis.
EXTRANEAL Peritoneal dialysis solution is an alternative fluid to be used in chronic kidney failure patients being treated on peritoneal dialysis.
2. What should I know before I use EXTRANEAL?
Warnings
Do not use EXTRANEAL if:
- the expiry date on the pack has passed.
- the solution is discoloured, cloudy, contains particulate matter or shows evidence of leakage, or if seals are not intact.
- you are allergic to icodextrin, sodium chloride, sodium lactate, calcium chloride dihydrate and magnesium chloride hexahydrate, or any of the ingredients listed at the end of this leaflet. Always check the ingredients to make sure you can use this medicine.
- you have a known allergy to starch based polymers (e.g., corn starch) and/or Icodextrin.
- you have known maltose or isomaltose intolerance or patients with glycogen storage disease.
- you have a disorder of metabolism known as lactic acidosis.
- you have any issues that prevents effective dialysis or increase the likelihood of the infection.
- you have any changes in peritoneal function.
Warning for incorrect blood glucose level:
The active ingredient in EXTRANEAL can interfere with the way you measure your blood glucose. This may result in higher than true blood glucose levels being reported by your monitor. Check with your blood glucose device/monitor manufacturer to see if it is safe to be used when you are on EXTRANEAL.
EXTRANEAL PD solution is not recommended in children.
Check with your doctor if you:
- have injury or surgery or congenital anomalies (birth defects) related to abdominal wall or cavity
- a history of abdominal operations with fibrous adhesions (scar tissue)
- faecal fistula (a passageway from your stomach or bowel to the skin
- intra-abdominal tumours
- open wounds
- hernia
- Peritonitis
- abdominal wall infection
- have severe abdominal pain, abdominal distension, or vomiting. This can be a sign of encapsulating peritoneal sclerosis, a complication of the peritoneal dialysis therapy that can be fatal
- inflammatory bowel diseases (Crohn's disease, ulcerative colitis, diverticulitis)
- large polycystic kidneys
- colostomy or ileostomy
- frequent episodes of diverticulitis
- you have a lung disease (especially pneumonia)
- aortic graft replacement
- take any medicines for any other condition
On rare occasions, some people may have severe reactions to EXTRANEAL PD solution. This appears as a severe skin reaction with blistering and peeling of the skin. It can also appear as a swelling of the skin and redness. Occasionally there is also swelling of the blood vessels. If any of these symptoms appear contact your doctor immediately.
It is important to keep a record of your fluid levels to avoid overhydration or underhydration. Your doctor will monitor your weight to ensure that you are using the right fluid volumes.
Your doctor will monitor your electrolytes levels (particularly bicarbonate, potassium, magnesium, and calcium) and blood profile, as well as other indicators of your health to ensure they are in safe ranges. It is important to carefully monitor the levels of potassium in your blood if you are being treated with heart medications called cardiac glycosides.
EXTRANEAL PD solution does not contain potassium. In patients with normal or low potassium levels, your doctor may consider adding potassium to the dialysis solution to prevent the occurrence of very low potassium levels.
You may also need to take a magnesium supplement to keep your magnesium level in the safe range.
Peritoneal dialysis can lead to a loss of proteins, amino acids, water-soluble vitamins and other medicines. An adequate diet or nutritional supplements may be recommended in order to avoid deficiency states. Some changes in your medicine may be needed.
If you have diabetes requiring insulin, carefully monitor your insulin requirements during and following dialysis with glucose-containing solutions.
The drained fluid should be inspected for the presence of fibrin or cloudiness, which may indicate the presence of peritonitis.
Aseptic techniques must be maintained during the bag connection in order to reduce the risk of infection. Improper clamping or priming sequence may result in infusion of air into the peritoneal cavity, which may result in abdominal pain and/or peritonitis. If you experience peritonitis, your doctor may prescribe antibiotics.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor if you are pregnant or intend to become pregnant.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Because peritoneal dialysis may influence the effects of medicines, your doctor may need to change their dosages, especially those:
- for heart failure, such as digoxin. Your doctor will check the level of potassium, calcium, and magnesium in your blood and, if necessary, will take appropriate measures.
Peritoneal dialysis can lead to a loss of proteins, amino acids, water-soluble vitamins and other medicines. An adequate diet or nutritional supplements may be recommended in order to avoid deficiency states. Some changes in your medicine may be needed.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect EXTRANEAL.
4. How do I use EXTRANEAL?
How much to use
Your doctor will determine the method, duration and frequency of use and the required volume of solution and time in the peritoneal cavity (dwell time).
You must follow the procedures and instructions given by your doctor or nurse every time you do peritoneal dialysis. Contact your doctor if you are having problems or are unsure about any of the techniques.
Adults: Single exchange in each 24 hour-period, as part of a Continuous Ambulatory Peritoneal Dialysis (CAPD) or Automated Peritoneal Dialysis (APD) regimen.
Elderly: As for adults.
Children: Not recommended for use in children (less than 18 years).
EXTRANEAL PD solution is recommended for use during the longest dwell period; that is in CAPD usually overnight and in APD for the long daytime dwell.
When to use EXTRANEAL
EXTRANEAL should be used, as prescribed by your doctor.
You must follow the procedures and instructions given by your doctor or nurse every time you do peritoneal dialysis. Contact your doctor if you are having problems or are unsure about any of the techniques or your prescription.
How to use EXTRANEAL for PD
EXTRANEAL PD solution is intended for intraperitoneal administration only. Not for intravenous administration.
Aseptic technique should be observed throughout the procedure.
To reduce discomfort on administration, the solution may be warmed to a temperature of 37°C prior to use. This should be done using dry heat ideally with a warming cabinet. Do not heat EXTRANEAL in water or in a microwave. Do not use EXTRANEAL if the solution is discoloured, cloudy, contains particulate matter or shows evidence of leakage, or if seals are not intact.
The drained fluid should be inspected for the presence of fibrin or cloudiness, which may indicate the presence of peritonitis.
EXTRANEAL bags should be used once, and any unused portion of the solution must be discarded.
If you forget to use EXTRANEAL
EXTRANEAL should be used, as prescribed by your doctor.
If you forget to do an exchange or have used too little solution, contact your doctor for guidance.
If you use too much EXTRANEAL
Overdose by over infusion of a EXTRANEAL Solutions into the peritoneal cavity is characterised by abdominal pain and abdominal stretching and shortness of breath.
If you allow too much solution to flow into the peritoneal cavity, the excess can easily be drained into the empty bag. However, overdose can result in too much body fluid and electrolyte imbalance. In this case, please consult your doctor.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know while using EXTRANEAL?
Things you should do
Follow the procedures and instructions from your nurse or doctor on how to carry out peritoneal dialysis with EXTRANEAL every time you do it.
EXTRANEAL dialysis solutions should be used, as prescribed by your doctor.
Body weight, blood sugar, potassium, calcium, magnesium, bicarbonate, blood protein and blood profile, as well as other indicators of your health should be monitored regularly by your doctor.
Warning for incorrect blood glucose level:
The active ingredient in EXTRANEAL can interfere with the way you measure your blood glucose. This may result in higher than true blood glucose levels being reported by your monitor. Check with your blood glucose device/monitor manufacturer to see it is safe to be used when you are on EXTRANEAL.
Call your doctor straight away if you:
- Do not feel well or develop any unwanted side effects (see section 6. Are there any side effects?). Seek medical attention immediately.
Remind any doctor, surgeon, anaesthetist, dentist, pharmacist, or nurse you visit that you are using EXTRANEAL.
Things you should not do
- Do not use EXTRANEAL for intravenous administration.
- Do not heat EXTRANEAL in water or in a microwave.
- Do not stop using EXTRANEAL without letting your doctor know.
Driving or using machines
Patients on peritoneal dialysis may experience undesirable effects, which could affect the ability to drive or use machines.
Looking after your medicine
- Store below 30°C.
- Do not use after the expiry date on the bag.
Keep it where young children cannot reach it.
Follow the instructions in the carton on how to take care of your medicine properly.
When to discard your medicine
EXTRANEAL bag should be used once, and any unused portion of the solution must be discarded.
Getting rid of any unwanted medicine
If you no longer need to use this medicine or it is out of date, take it to any pharmacy for safe disposal.
Do not use this medicine after the expiry date.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
Peritoneal dialysis procedure related disorders
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
Peritoneal dialysis procedure related disorders
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What EXTRANEAL contains
| Active ingredient (main ingredient) | Icodextrin, sodium chloride, sodium lactate, calcium chloride dihydrate, magnesium chloride hexahydrate |
| Other ingredients (inactive ingredients) | hydrochloric acid, sodium hydroxide, water for injections |
Do not take this medicine if you are allergic to any of these ingredients.
What EXTRANEAL looks like
EXTRANEAL is clear peritoneal dialysis solution. EXTRANEAL solutions are available in pack sizes of 1500 mL, 2000 mL, 2500 mL, and 3000 mL.
- Standard single bag: flexible PVC container in 1500 mL, 2000 mL, 2500 mL and 3000 mL volumes. AUST R 91344.
- Twin Bag: flexible PVC container in 1500 mL, 2000 mL, 2500 mL and 3000 mL volumes. A drainage bag is attached. AUST R 91430.
Not all pack sizes are marketed.
Who distributes EXTRANEAL
VANTIVE Pty Ltd
1 Baxter Drive
OLD TOONGABBIE NSW 2146 AUSTRALIA
This leaflet was prepared in December 2025.
Brand Information
| Brand name | Extraneal |
| Active ingredient | Calcium chloride dihydrate + Icodextrin + Magnesium chloride hexahydrate + Sodium lactate + Sodium chloride |
| Schedule | Unscheduled |
MIMS Revision Date: 01 December 2024
1 Name of Medicine
Icodextrin, sodium chloride, sodium lactate, calcium chloride dihydrate and magnesium chloride hexahydrate.
2 Qualitative and Quantitative Composition
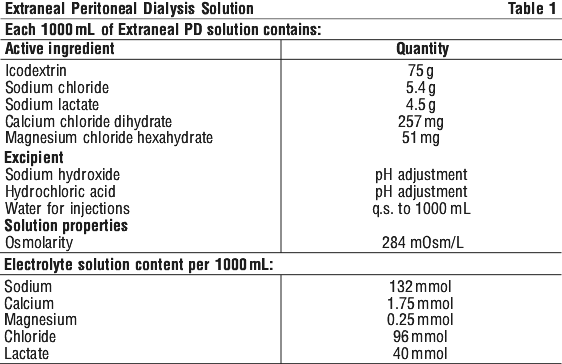
Extraneal PD solution contains icodextrin as the active ingredient at a concentration of 7.5% w/v in an electrolyte solution. Icodextrin is an α(1-4) linked glucose polymer which contains 5-10% α(1-6) links. It is produced by the hydrolysis of starch and fractionated by membrane separation technology to produce material with the desired molecular weight distribution (85% w/w within the molecular weight range 1,640-45,000).
Extraneal PD solution is presented in a flexible PVC bag and is sterile, nonpyrogenic and contains no bacteriostatic or antimicrobial agents or added buffers (see Table 1).
3 Pharmaceutical Form
Dialysis solution.
4 Clinical Particulars
4.1 Therapeutic Indications
Extraneal PD solution is indicated for use as an alternative osmotic agent in dialysis solutions for the long dwell exchange in patients treated with peritoneal dialysis.
4.2 Dose and Method of Administration
Dosage. Adults. By intraperitoneal administration limited to a single exchange in each 24 hour period, as part of a continuous ambulatory peritoneal dialysis (CAPD) or automated peritoneal dialysis (APD) regimen.
Elderly. As for adults.
Children. Not recommended for use in children (less than 18 years).
Administration. Extraneal PD solution is recommended for use during the longest dwell period that is in CAPD usually overnight and in APD for the long daytime dwell.
Extraneal PD solution is intended for intraperitoneal administration only. Not for intravenous administration.
Single use only. Any unused portion of dialysate should be discarded.
The mode of therapy, frequency of treatment, exchange volume, duration or dwell and length of dialysis should be initiated and supervised by the physician.
Aseptic technique should be observed throughout the procedure.
Do not administer if the solution is discoloured, cloudy, contains particulate matter or shows evidence of leakage, or if seals are not intact.
To reduce discomfort on administration, the solution may be warmed to a temperature of 37°C prior to use. This should be done using dry heat ideally with a warming cabinet. The bags should not be immersed in water nor should they be microwaved in order to warm.
The volume to be instilled should be given over a period of approximately 10 to 20 minutes at a rate which the patients finds comfortable.
For adult patients of normal body size the instilled volume should not exceed 2.0 L. If the instilled volume causes discomfort due to abdominal tension the instilled volume should be reduced.
The recommended dwell time is between 6 and 12 hours in CAPD and 14-16 hours in APD.
Drainage of the fluid is by gravity at a rate comfortable for the patient. The drained fluid should be inspected for the presence of fibrin or cloudiness, which may indicate the presence of infection or aseptic peritonitis (see Section 4.8 Adverse Effects (Undesirable Effects)).
4.3 Contraindications
Extraneal PD solution should not be used in patients with a known allergy to starch based polymers (e.g. corn starch) and/or icodextrin, in patients with maltose or isomaltose intolerance or patients with glycogen storage disease.
Extraneal PD solution is also contraindicated in patients with:
a history of abdominal surgery in the month preceding commencement of therapy or in patients with abdominal fistulae, tumours, open wounds, hernias or other conditions which compromise the integrity of the abdominal wall, abdominal surface or intra-abdominal cavity;
pre-existing severe lactic acidosis;
uncorrectable mechanical defects that prevent effective PD or increase the risk of infection;
documented loss of peritoneal function or extensive adhesions that compromise peritoneal function.
4.4 Special Warnings and Precautions for Use
Warning: dangerous drug-device interaction. Only use glucose specific monitors and test strips to measure blood glucose levels in patients using Extraneal PD solution. Blood glucose monitoring devices using GDH-PQQ, GDO or GDH-FAD based methods may not be used. The manufacturer(s) of the monitor and test strips should be contacted to determine if icodextrin or maltose causes interference or falsely elevated glucose results. Use of GDH-PQQ, GDO-or GDH-FAD based glucose monitors and test strips has resulted in falsely elevated glucose readings (due to the presence of maltose) and has led patients or health care providers to withhold treatment of hypoglycaemia or to administer insulin inappropriately. Both of these situations have resulted in unrecognised hypoglycaemia, which has led to loss of consciousness, coma, permanent neurological damage and death. Plasma levels of Extraneal PD solution and its metabolites return to baseline within approximately 14 days following cessation of Extraneal PD solution administration. Therefore falsely elevated glucose levels may be measured up to two weeks following cessation of Extraneal PD solution therapy when GDH-PQQ, GDO-or GDH-FAD based blood glucose monitors and test strips are used.
Because GDH-PQQ, GDO or GDH-FAD based blood glucose monitors may be used in hospital settings, it is important that the health care providers of all peritoneal dialysis patients using Extraneal PD solution carefully review the product information of the blood glucose testing system, including that of test strips, to determine if the system is appropriate for use with Extraneal PD solution.
To avoid improper insulin administration, educate all patients on Extraneal PD solution therapy to alert health care providers of this interaction whenever they are admitted to the hospital.
The manufacturer(s) of the monitor and test strips should be contacted to determine if icodextrin or maltose causes interference or falsely elevated glucose.
Encapsulating peritoneal sclerosis (EPS) is considered to be a known, rare complication of peritoneal dialysis therapy. EPS has been reported in patients using peritoneal dialysis solutions including Extraneal PD solution. Fatal outcomes of EPS have been reported with Extraneal PD solution.
If peritonitis occurs, the choice and dosage of antibiotics should be based upon the results of identification and sensitivity studies of the isolated organism(s) when possible. Prior to identification of the involved organism(s), broad spectrum antibiotics may be indicated.
Solutions containing glucose should be used with caution in patients with a known allergy to corn or corn products. Hypersensitivity reactions such as those due to a corn starch allergy, including anaphylactic/ anaphylactoid reactions, may occur. Stop the infusion immediately and drain the solution from the peritoneal cavity if any signs or symptoms of a suspected hypersensitivity reaction develop. Appropriate therapeutic countermeasures must be instituted as clinically indicated.
Rarely, serious hypersensitivity reactions to Extraneal PD solution have been reported such as toxic epidermal necrolysis, angioedema, serum sickness, erythema multiforme and vasculitis. If a serious reaction is suspected, discontinue Extraneal PD solution and institute appropriate treatment as clinically indicated.
Patients with severe lactic acidosis should not be treated with lactate based peritoneal dialysis solutions (see Section 4.3 Contraindications). It is recommended that patients with conditions known to increase the risk of lactic acidosis (e.g. severe hypotension or sepsis that can be associated with acute renal failure, inborn errors of metabolism, treatment with drugs such as metformin and nucleoside/ nucleotide reverse transcriptase inhibitors (NRTIs)) must be monitored for occurrence of lactic acidosis before the start of treatment and during treatment with lactate based peritoneal dialysis solutions.
When prescribing the solution to be used for an individual patient, consideration should be given to the potential interaction between the dialysis treatment and therapy directed at other existing illnesses. Serum potassium levels should be monitored carefully in patients treated with cardiac glycosides. For example, rapid potassium removal may create arrhythmias in cardiac patients using digitalis or similar drugs; digitalis toxicity may be masked by hyperkalaemia, hypermagnesaemia, or hypocalcaemia. Correction of electrolytes by dialysis may precipitate signs and symptoms of digitalis excess. Conversely, toxicity may occur at suboptimal dosages of digitalis if potassium is low or calcium high.
Use with caution in the following circumstances. Extraneal PD solution associated skin reactions, including rash and pruritus, are generally mild or moderate in severity. Occasionally, these rashes have been associated with exfoliation. In the event of this occurring, and depending on the severity, Extraneal PD solution should be withdrawn at least temporarily.
Peritoneal dialysis should be done with caution in patients with: 1) abdominal conditions, including disruption of the peritoneal membrane and diaphragm by surgery, from congenital anomalies or trauma until healing is complete, abdominal tumours, abdominal wall infection, hernias, faecal fistula, colostomy or ileostomy, frequent episodes of diverticulitis, inflammatory or ischemic bowel disease, large polycystic kidneys, or other conditions that compromise the integrity of the abdominal wall, abdominal surface, or intra-abdominal cavity; and 2) other conditions including recent aortic graft replacement and severe pulmonary disease.
As with other peritoneal dialysis fluids, Extraneal PD solution should be used with caution, after careful evaluation of its potential risks and benefits, in patients with conditions which preclude normal nutrition, with impaired respiratory function or potassium deficiency.
Patients should be carefully monitored to avoid over and under hydration. An accurate fluid balance record should be kept and the patient's bodyweight monitored.
Overinfusion of an Extraneal PD solution volume into the peritoneal cavity may be characterized by abdominal distension, feeling of fullness and/or shortness of breath.
Treatment of Extraneal PD solution overinfusion is to release the Extraneal PD solution from the peritoneal cavity by drainage of the Extraneal PD solution volume contained within the peritoneal cavity.
Blood chemistry, haematology and plasma osmolality should be monitored at regular intervals.
Protein, amino acids, water soluble vitamins and other medicines may be lost during peritoneal dialysis and may require replacement.
In patients with hypercalcaemia, particularly in those on low calcium peritoneal dialysis solutions, consideration should be given to the fact that Extraneal PD solution is not provided in a low calcium electrolyte solution.
Potassium is omitted from Extraneal PD solution due to the risk of hyperkalaemia. In situations in which there is a normal serum potassium level or hypokalaemia, the addition of potassium chloride (up to a concentration of 4 mEq/L) may be indicated to prevent severe hypokalaemia and should be made after careful evaluation of serum and total body potassium, only under the direction of a physician.
Fluid, haematology, blood chemistry, and electrolyte concentrations should be monitored periodically, including magnesium and bicarbonate. If serum magnesium levels are low, oral magnesium supplements or peritoneal dialysis solutions containing higher magnesium concentrations may be used.
Decreases in serum sodium and chloride have been observed in patients using Extraneal PD solution.
Solutions that are discoloured, cloudy, contain particulate matter, or show evidence of leakage should not be used.
The drained fluid should be inspected for the presence of fibrin or cloudiness, which may indicate the presence of peritonitis.
In diabetic patients, blood glucose levels should be regularly monitored, and the dosage of insulin or other treatment for hyperglycaemia should be adjusted following initiation of treatment with Extraneal PD solution.
Blood glucose measurement must be done with a glucose specific method to prevent maltose interference. Glucose dehydrogenase based methods or glucose dye oxidoreductase based methods should not be used.
It is recommended that reference is made to the relevant section of the glucose test kit product leaflet to ascertain that interference while using icodextrin based dialysis therapy is not described (see Section 4.4 Special Warnings and Precautions for Use, Effects on laboratory tests).
Aseptic technique should be employed throughout the peritoneal dialysis procedure. If peritonitis occurs, the choice and dosage of antibiotics should be based upon the results of culture and sensitivity of the isolated organisms. Prior to identification of involved organisms, broad spectrum antibiotics may be indicated.
To reduce discomfort on administration, the solution may be warmed in the over pouch to a temperature of 37°C prior to use. This should be done using dry heat, ideally within a warming cabinet. The bags should not be immersed in water nor should they be microwaved in order to warm due to the potential for patient injury or discomfort.
Treatment should be initiated and monitored under the supervision of a physician knowledgeable in the management of patients with renal failure.
Pregnancy should be excluded prior to therapy with Extraneal PD solution. A reliable method of contraception should be used by women of reproductive age, should they require long-term treatment with Extraneal PD solution.
Extraneal PD solution is intended for intraperitoneal administration only. Not for intravenous injection.
This therapy is not recommended in patients with known allergy to starch based polymers or an icodextrin intolerance.
Extraneal PD solution should not be used if there is a history of abdominal surgery in the month preceding commencement of therapy or if the patient is suffering from any of the following conditions affecting their abdomen: tumours, open wounds or hernias.
Use in renal impairment. Extraneal PD solution is not recommended in patients with acute renal failure.
Extraneal PD solution should not be used when acute renal failure has been diagnosed.
Use in the elderly. See Section 4.2 Dose and Method of Administration for recommended dosage.
Paediatric use. Safety and effectiveness in paediatric patients have not been established.
Extraneal PD solution is not recommended in children.
Effects on laboratory tests. The safety and efficacy of Extraneal PD solution was established via laboratory tests conducted on a patient study of over 200 individuals. A study of the results shows that icodextrin use produced a greater ultrafiltration volume compared to weak 1.36% glucose and was as effective as the stronger (3.86%) glucose. The mean overnight ultrafiltration was 3.5 times greater than 1.36% glucose at 8 hours and 5.5 times greater at 12 hours. No significant difference was observed at 8 or 12 hours comparing icodextrin to 3.86% glucose.
Extending the dwell time from 8 to 12 hours tended to reduce net ultrafiltration with glucose 1.36% but increase it with icodextrin. In addition 9-41% of patients on glucose (1.36 and 3.86%) experienced reabsorption of peritoneal dialysis fluid.
A subgroup analysis of diabetic patients showed that overall diabetic control and insulin requirements were not different in the icodextrin and glucose groups.
An increase in volume of ultrafiltrate after an 8 hour overnight dwell was seen in all patients when going from 1.36% glucose to icodextrin.
Decreases in serum sodium and chloride have been observed in patients using Extraneal PD solution. The mean change in serum sodium from baseline to the last study visit was -2.8 mmol/L for patients on Extraneal PD solution and -0.3 mmol/L for patients on control solution. Four Extraneal PD solution patients and two control patients developed serum sodium < 125 mmol/L. The mean change in serum chloride from baseline to last study visit was -2.0 mmol/L for Extraneal PD solution patients and +0.6 mmol/L for control patients. The declines in serum sodium and chloride may be related to dilution resulting from the presence of icodextrin metabolites in plasma. Although these decreases have been small and clinically unimportant, monitoring of the patient's serum electrolyte levels as part of routine blood chemistry testing is recommended.
An increase in mean serum alkaline phosphatase has been observed in clinical studies of ESRD patients receiving Extraneal PD solution. No associated increases in liver function tests were observed. Serum alkaline phosphatase levels did not show evidence of progressive increase over a 12 month study period. Levels returned to normal approximately two weeks after discontinuation of Extraneal PD solution.
There were individual cases where increased alkaline phosphatase was associated with elevated AST (SGOT), but neither elevation was considered causally related to treatment.
An apparent decrease in serum amylase activity has been observed in patients using Extraneal PD solution.
Blood glucose measurement must be done with a glucose specific method to prevent maltose interference with test results. Since falsely elevated glucose levels have been observed with blood glucose monitoring devices and test strips that use GDH PQQ-based methods or GDO based methods, GDH PQQ based methods should not be used to measure glucose levels in patients administered Extraneal PD solution. Also, the use of some glucose monitors and test strips using GDH-FAD methodology has resulted in falsely elevated glucose readings due to the presence of maltose. (See Section 4.4 Special Warnings and Precautions for Use.)
4.5 Interactions with Other Medicines and Other Forms of Interactions
No interaction studies have been conducted with Extraneal PD solution. The blood concentrations of dialyzable drugs may be reduced by dialysis.
Corrective therapy should be instituted if necessary. In patients using cardiac glycosides, plasma levels of potassium and calcium and magnesium must be carefully checked. In the event of abnormal levels, appropriate actions should be taken.
Minimum inhibitory concentration (MIC). No formal clinical drug interaction studies with antibiotics were conducted. In vitro studies with Extraneal PD solution and the following antibiotics have demonstrated no effects with regard to MIC: vancomycin, cefazolin, ampicillin, ampicillin/ flucoxacillin, ceftazidime, gentamicin and amphotericin. However, aminoglycosides should not be mixed with penicillins due to chemical incompatibility.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. Potential effects on male and female fertility are unknown.
Use in pregnancy. (Category B2)
Extraneal PD solution is not recommended during pregnancy.
The potential effects of Extraneal PD solution on reproduction have not been adequately studied in animals. There are no adequate data from the use of Extraneal PD solution in pregnant women.
Women of childbearing potential should be treated with Extraneal PD solution only when adequate contraceptive precautions have been taken.
Physicians should carefully consider the potential risks and benefits for each specific patient before prescribing Extraneal PD solution.
Use in lactation. Extraneal PD solution is not recommended during lactation.
There are no available data from animal studies on the effects of icodextrin administered during lactation. It is not known whether icodextrin and/or its metabolites are excreted into human milk. Because many drugs are excreted into human milk and because of the potential of adverse effects on the infants, Extraneal PD solution should not be used in breastfeeding women.
4.7 Effects on Ability to Drive and Use Machines
Patients on peritoneal dialysis may experience undesirable effects, which could affect the ability to drive or use machines.
4.8 Adverse Effects (Undesirable Effects)
Blood glucose management with Extraneal PD solution must be done with a glucose specific method to avoid interference resulting in unrecognised hypoglycaemia. If nonspecific glucose test methods (GDH-PQQ and glucose dye oxidoreductase based methods) are used, loss of consciousness, neurological damage and death may occur. This is a result of falsely high blood glucose readings due to the interaction between icodextrin and its byproducts and glucometers that use glucose dehydrogenase pyrroloquinolinequinone (GDH-PQQ) or glucose dye oxidoreductase based methods for measuring blood glucose.
A listing of adverse events reported in clinical studies, regardless of causality, occurring in > 5% of patients and more common on Extraneal PD solution, is presented in Table 2.
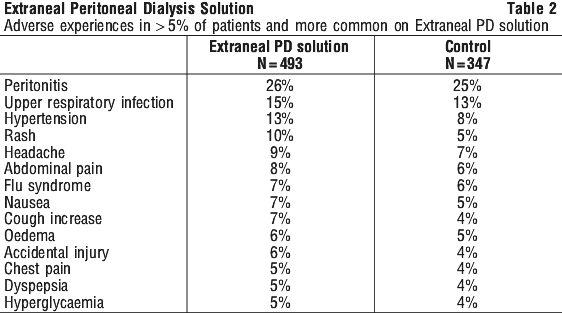
Adverse reactions on Extraneal PD solution also include anorexia/ loss of appetite, blood volume decreased, constipation, muscle cramps, dehydration, disequilibrium syndrome, hypovolaemia, serum osmolality increased, ultrafiltration increased, urine volume decreased, weight increased and weight decreased.
Additional adverse events occurring at an incidence of < 5% and that may or may not have been related to Extraneal PD solution include: pain on infusion, abdominal enlargement, cloudy effluent, bloody effluent, ultrafiltration decrease, postural hypotension, heart failure, hyponatraemia, hypochloraemia, hypercalcaemia, hypoglycaemia, alkaline phosphatase increase, SGPT increase, SGOT increase, cramping, confusion, lung oedema, facial oedema, exfoliative dermatitis, eczema, vesicobullous rash, maculopapular rash, erythema multiforme, serum amylase decrease, catheter blockage, disturbed vision, electrolyte imbalance, fatigue, fluid imbalance.
All reported events are included except those already listed in Table 1, those not plausibly associated with Extraneal PD solution, and those that were associated with the condition being treated or related to the dialysis procedure.
Other adverse events reported with Extraneal PD solution include. Furuncle, leucocytosis, eosiniphilia, parathyroid disorder, hypomagnesaemia, anxiety, abnormal thinking, nervousness, hyperkinesia, paraesthesia, ageusia, tinnitus, tachycardia, hiccups, lung disorder, intestinal obstruction, gastrointestinal disorder, gastric ulcer, gastritis, dry mouth, flatulence, nail disorder, dry skin, skin discolouration, neck pain, renal pain, bone pain, muscle spasm, skin ulcer, psoriasis, dermatitis bullous, urticaria and myalgia.
Other undesirable effects of peritoneal dialysis related to the procedure and/or the solution. The following undesirable effects are often reported spontaneously and in the literature.
Those which are related to the procedure include peritonitis (septic or aseptic), with or without abdominal pain, cloudy effluent and sometimes fever; bleeding, catheter blockage, infection around the catheter (signs of inflammation: redness and secretion), hypervolaemia, hypovolaemia, hypertension, hypotension, dehydration, oedema, constipation, hernia of the abdominal cavity, ileus, loss of appetite, dyspepsia, nausea and vomiting, dizziness, fatigue, headache, shoulder pain, pruritus, muscle cramps, disturbed vision, dyspnoea/ shortness of breath, fluid imbalance, pain and abnormal laboratory test results.
Those which are generally related to peritoneal dialysis solutions are seen less frequently than those related to the procedure and include electrolyte disturbances (e.g. hypokalaemia, hypocalcaemia and hypercalcaemia), fainting, muscle cramping, respiratory symptoms associated with shortness of breath and weakness, anorexia/ loss of appetite, asthenia, catheter blockage, constipation, disturbed vision, disequilibrium syndrome, dyspnoea/ shortness of breath, oedema, cloudy effluent, exfoliative dermatitis, fatigue, fluid imbalance, hypertension, hypervolaemia, exit site infection, abdominal pain, peritonitis, aseptic peritonitis and rash.
In addition there have been common reports of skin reactions in patients treated with icodextrin, including rash and pruritus. Occasionally, these rashes have been associated with exfoliation. The incidence of rash considered to be related to treatment in pooled data from all clinical studies was 5.5% for Extraneal PD solution treated patients compared with 1.7% in patients treated with dextrose solutions.
Post-marketing surveillance. Postmarketing surveillance data worldwide show that there have been serious hypoglycaemic reactions associated with the use of Extraneal PD solution and nonglucose specific measuring devices. These reactions have resulted in death (2 cases to May 2005) and hypoglycaemic coma with neurological sequelae (2 cases to May 2005), and other hypoglycaemic events from which the patients recovered.
To avoid these events, a glucose specific blood glucose monitor must be used (see Section 4.4 Special Warnings and Precautions for Use).
In addition to the adverse reactions noted in clinical trials, the following adverse reactions have been reported in the postmarketing setting, listed by system organ class (SOC), then by preferred MedDRA term in order of severity.
Infections and infestations. Fungal peritonitis, peritonitis bacterial, catheter site infection, catheter related infection.
Blood and lymphatic system disorders. Thrombocytopenia, leukopenia.
Immune system disorders. Vasculitis, serum sickness, hypersensitivity.
Metabolism and nutrition disorders. Shock, hypoglycaemia, fluid overload, fluid imbalance.
Nervous system disorders. Hypoglycaemic coma, burning sensation.
Eye disorders. Vision blurred.
Respiratory, thoracic, and mediastinal disorders. Bronchospasm, stridor.
Gastrointestinal disorders. Encapsulating peritoneal sclerosis, aseptic peritonitis*, peritoneal cloudy effluent, ileus, ascites, inguinal hernia, abdominal discomfort.
Skin and subcutaneous disorders. Toxic epidermal necrolysis, erythema multiforme, angioedema, urticaria generalized, toxic skin eruption, swelling face, periorbital edema, exfoliative rash, skin exfoliation, prurigo, rash (including macular, papular, erythematous, exfoliative), dermatitis (including allergic and contact), drug eruption, erythema, onychomadesis, skin chapped, blister.
Musculoskeletal, connective tissue disorders. Arthralgia, back pain, musculoskeletal pain.
Reproductive system and breast disorders. Penile edema, scrotal edema.
General disorders and administrative site conditions. Discomfort, pyrexia, chills, malaise, drug effect decreased, drug ineffective, catheter site erythema, catheter site inflammation, infusion related reaction (including infusion site pain, instillation site pain).
Injury, poisoning and procedural complications. Device interaction.
* Lower level term.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
No data is available on the effects of overdosage. However, continuous administration of more than one bag of Extraneal PD solution in 24 hours would increase plasma levels of carbohydrate metabolites and maltose. The effects of such an increase are unknown but an increase in plasma osmolality may occur. The treatment could be managed by icodextrin free peritoneal dialysis or haemodialysis.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Icodextrin is a starch derived glucose polymer which acts as an osmotic agent when administered intraperitoneally for continuous ambulatory peritoneal dialysis. A 7.5% solution is approximately iso-osmolar to serum but produces sustained ultrafiltration over a period up to 12 hours in CAPD. The volume of ultrafiltrate produced is comparable to that with 3.86% glucose when used in CAPD. Blood glucose and insulin levels remain unaffected.
Clinical trials. Extraneal PD solution has demonstrated efficacy, as a peritoneal dialysis solution in clinical trials of approximately 400 patients studied with endstage renal disease (ESRD). In active-controlled trials of one to six months in duration, Extraneal PD solution used once daily for the long dwell in either CAPD or APD therapy resulted in higher net ultrafiltration compared with 1.5% and 2.5% dextrose solutions, and higher creatinine and urea nitrogen clearances when compared to 2.5% dextrose. Net ultrafiltration was similar to 4.25% dextrose. There is no information on how creatinine and urea nitrogen clearances on Extraneal PD solution compared with 4.25% dextrose. Effects were generally similar in CAPD and APD. These studies were conducted in male and female patients > 18 years of age. Survival analysis was not included in these protocols. Ultrafiltration (UF) was the primary efficacy endpoint for all three of the pivotal studies. The studies only evaluated the effects of Extraneal PD solution on ultrafiltration for the long dwell; the effects on 24 hour ultrafiltration are unknown. See Table 3.

5.2 Pharmacokinetic Properties
In a single dose pharmacokinetic study using Extraneal PD solution (n = 13), a median of 40% (60 g) of the instilled icodextrin was absorbed from the peritoneal solution during a 12 hour dwell. Plasma levels of icodextrin rose during the dwell and declined after the dwell was drained. Peak plasma levels of icodextrin plus its metabolites (median Cpeak 2.2 g/L) were observed at the end of the long dwell exchange (median Tmax = 13 hours). Plasma levels return to baseline values within 7 days following cessation of icodextrin administration.
At steady state, the mean plasma level of icodextrin plus its metabolites was about 5 g/L. In multidose studies, steady-state levels of icodextrin were achieved within one week.
Icodextrin is metabolized by alpha-amylase into oligosaccharides with a lower degree of polymerization (DP), including maltose (DP2), maltotriose (DP3), maltotetraose (DP4), and higher molecular weight species. In a single dose study, DP2, DP3 and DP4 showed a progressive rise in plasma concentrations with a profile similar to that for total icodextrin, with peak values reached by the end of the dwell and declining thereafter. Only very small increases in blood levels of larger polymers were observed. Steady-state plasma levels of icodextrin metabolites were achieved within one week and stable plasma levels were observed during long-term administration. Steady-state plasma levels of 1.8 mg/mL have been measured for oligomers of glucose units greater than 9 (G9) and there is a rise in serum maltose (G2) to 1.1 mg/mL but there is no significant change in serum osmolality. The long-term effects of raised plasma levels of maltose and glucose polymer are unknown.
Some degree of metabolism of icodextrin occurs intraperitoneally with a progressive rise in the concentration of the smaller polymers in the dialysate during the 12 hour dwell. These fragments are cleared by peritoneal dialysis.
Icodextrin undergoes renal elimination in direct proportion to the level of residual renal function. Diffusion of the smaller icodextrin metabolites from plasma into the peritoneal cavity is also possible after systematic absorption and metabolism of icodextrin.
5.3 Preclinical Safety Data
Genotoxicity. Icodextrin was not mutagenic in a bacterial gene mutation assay, and was not clastogenic in V79 Chinese hamster lung cells in vitro or in mouse bone marrow cells in vivo.
Carcinogenicity. Long-term carcinogenicity studies of icodextrin have not been done.
6 Pharmaceutical Particulars
6.1 List of Excipients
Sodium hydroxide and hydrochloric acid (pH adjustment), water for injections.
6.2 Incompatibilities
See Section 4.5 Interactions with Other Medicines and Other Forms of Interactions.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 30°C. Do not administer unless the solution is clear and the bag undamaged. Shelf Life is 2 years.
6.5 Nature and Contents of Container
Standard single bag: flexible PVC container in 1500 mL, 2000 mL, 2500 mL and 3000 mL volumes. AUST R 91344.
Twin Bag: flexible PVC container in 1500 mL, 2000 mL, 2500 mL and 3000 mL volumes. A drainage bag is attached. AUST R 91430.
Not all pack sizes are marketed.
Package size. 1500 mL, 2000 mL, 2500 mL and 3000 mL.
6.6 Special Precautions for Disposal
Any unused product or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
Chemical structure. Icodextrin.
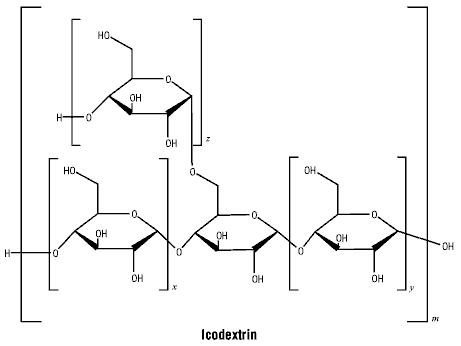
Molecular Weight: 231.08.
Sodium chloride. Molecular formula: NaCl.
Molecular Weight: 58.44.
Appearance: colourless or white crystal.
Solubility: freely soluble in water.
Sodium lactate. Molecular formula: NaC3H5O3.
Molecular Weight: 112.06.
Calcium chloride dihydrate. Molecular formula: CaCl2.2H2O.
Molecular Weight: 147.01.
Appearance: a white crystalline powder.
Solubility: hygroscopic, freely soluble in water.
Magnesium chloride hexahydrate. Molecular formula: MgCl2.6H2O.
Molecular Weight: 203.31.
Appearance: white or colourless crystalline solid.
Solubility: very soluble in water.
CAS number. Icodextrin. CAS No.: 37376-15-5.
Sodium chloride. CAS No.: 7647-14-5.
Sodium lactate. CAS No.: 72-17-3.
Calcium chloride dihydrate. CAS No.: 10035-04-8.
Magnesium chloride hexahydrate. CAS No.: 7791-18-6.
7 Medicine Schedule (Poisons Standard)
Not scheduled.
Date of First Approval
17 October 2002
Date of Revision
11 October 2024
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.