Gliolan
Brand Information
| Brand name | Gliolan |
| Active ingredient | Aminolevulinic acid hydrochloride |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Gliolan.
Summary CMI
GLIOLAN®
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using GLIOLAN?
GLIOLAN contains the active ingredient aminolevulinic acid hydrochloride (ALA HCl). GLIOLAN is used for the visualisation of certain brain tumours (called glioblastoma multiforme) during tumour surgery.
For more information, see Section 1. Why am I using GLIOLAN? in the full CMI.
2. What should I know before I use GLIOLAN?
Do not use if you have ever had an allergic reaction to aminolevulinic acid hydrochloride (ALA HCl).
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I use GLIOLAN? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with GLIOLAN and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use GLIOLAN?
- The usual dose is 20 mg GLIOLAN per kilogram body weight.
- GLIOLAN is given once only on the day of surgery, 2-4 hours before start of anaesthesia.
More instructions can be found in Section 4. How do I use GLIOLAN? in the full CMI.
5. What should I know while using GLIOLAN?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
For more information, see Section 5. What should I know while using GLIOLAN? in the full CMI.
6. Are there any side effects?
Side effects listed are due to the medicine and/or the surgery. The most common side effects include anemia, thrombocytopenia, leukocytosis, neurological disorders, blood clots that may obstruct blood vessels (thromboembolism), vomiting, nausea and increase in liver enzymes. Serious side effects can include nervous system related disorders, thromboembolism and blood clots that may move to the lungs (pulmonary embolism).
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
GLIOLAN®
Active ingredient(s): aminolevulinic acid hydrochloride (ALA HCl)
Consumer Medicine Information (CMI)
This leaflet provides important information about using GLIOLAN. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using GLIOLAN.
Where to find information in this leaflet:
1. Why am I using GLIOLAN?
2. What should I know before I use GLIOLAN?
3. What if I am taking other medicines?
4. How do I use GLIOLAN?
5. What should I know while using GLIOLAN?
6. Are there any side effects?
7. Product details
1. Why am I using GLIOLAN?
GLIOLAN contains the active ingredient aminolevulinic acid hydrochloride (ALA HCl).
GLIOLAN is used for the visualisation of certain brain tumours (called glioblastoma multiforme) during tumour surgery.
ALA HCl accumulates preferably in tumour cells where it is transformed into another similar substance. If the tumour is then exposed to blue light this new substance emits a red-violet light, which helps the surgeon to better see what is normal tissue and what is tumour tissue. This helps the surgeon to remove the tumour while sparing healthy tissue.
2. What should I know before I use GLIOLAN?
Warnings
Do not use GLIOLAN if:
- You are allergic to aminolevulinic acid hydrochloride or porphyrins (such as heme the pigment in red blood cells).
- You have, or may have, acute or chronic types of porphyria. Porphyria is a rare blood pigment disorder. This disorder can be inherited or acquired during your lifetime.
Always check the ingredients to make sure you can use this medicine.
Check with your doctor if you:
- Have any other medical conditions
- Take any medicines for any other condition
- Have heart disease. This medicine should be used with caution because the blood pressure may be decreased
- Have liver or kidney disease. This medicine should be used with caution as there is limited information on its use in patients with poor liver or kidney function
- Have or have had allergies to any other medicines, foods, preservatives or dyes
- Are a child or adolescent.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor if you are pregnant or intend to become pregnant. GLIOLAN must not be used during pregnancy. It may affect your developing baby if you take it during pregnancy.
Talk to your doctor if you are breastfeeding or intend to breastfeed. It is not known whether this medicine enters breast milk. Breastfeeding mothers should not breastfeed for 24 hours after treatment with this medicine. Your doctor can discuss with you the risks and benefits involved.
GLIOLAN with food and drink
- You should not drink or eat for at least 6 hours before starting anaesthesia.
- This medicine is generally used once only, 2-4 hours before anaesthesia for surgery.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with GLIOLAN and affect how it works, particularly medicines that may cause skin problems, such as sunburn, when the skin comes under strong light. These include:
- Some types of antibiotics such as tetracyclines, sulfonamides and fluoroquinolones
- Hypericin extracts used to treat mild forms of depression. One case of severe sunburn lasting for 5 days has been reported in a patient after having taken this medicine and a hypericin extract.
You should not take any such products for up to 2 weeks after you have taken GLIOLAN.
- Any medicines known to harm the liver within 24 hours of having taken GLIOLAN
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect GLIOLAN.
4. How do I use GLIOLAN?
This medicine is a powder that must be mixed with drinking water before use.
This will be done for you by a pharmacist or a nurse.
How much to take
- The usual dose is 20 mg GLIOLAN per kilogram body weight. The pharmacist or nurse will calculate the exact dose you need.
When and how to take GLIOLAN
- You have to drink the prepared solution 2-4 hours before start of anaesthesia.
- The solution has a sour taste when taken orally.
- If the anaesthesia/surgery is delayed by some hours, additional doses of this medicine must not be given.
- If the surgery is postponed by more than 12 hours, surgery should be re-scheduled for the next day or later. If the surgery is delayed by a day or more another dose of this medicine can be taken 2-4 hours before anaesthesia.
If you forget to use GLIOLAN
GLIOLAN is given once only on the day of surgery, 2-4 hours before start of anaesthesia.
If you have forgotten to take this medicine during this time period, it is not advisable to take it just before start of anaesthesia. In this case, anaesthesia and surgery must be postponed for at least 2 hours, if possible.
If you use too much GLIOLAN
If you have taken more GLIOLAN than you should, your doctor will decide on any necessary measures to avoid any problems, including sufficient protection from strong light (for example direct sunlight).
Symptoms of an overdose may include skin rash and problems breathing.
If you think that you have used too much GLIOLAN, you may need urgent medical attention.
You should immediately:
- If in Australia: phone the Poisons Information Centre
(by calling 13 11 26)
If in New Zealand phone the Centre for Adverse reaction monitoring (by calling 03 479 7185), or - Contact your doctor, or
- Go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know while using GLIOLAN?
Things you must do
- If you are about to be started on any new medicine, remind your doctor and pharmacist that you have recently taken, or due to be given GLIOLAN.
- If you are going to have surgery, tell the surgeon or anaesthetist about all other medicines you have taken at least in the 4 weeks before your surgery.
- If you are required to have any blood tests after your surgery, tell your doctor that you have taken this medicine. It may interfere with the results of some tests.
Remind any doctor, dentist or pharmacist you visit that you have recently taken, or due to be given GLIOLAN.
Things to be careful of
Light exposure
- Protect your eyes and skin from strong light (for example direct sunlight or brightly focused indoor light) for 24 hours after administration of this medicine.
Things you must not do
- Do not take GLIOLAN to treat any other complaints unless your doctor tells you to.
- Do not give your medicine to anyone else, even if they have the same condition as you.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how GLIOLAN affects you.
This medicine is not expected to affect your ability to drive a car or operate machinery.
Looking after your medicine
GLIOLAN will be stored in the pharmacy or in the ward. The medicine is kept in its original packaging where the temperature stays below 25°C protected from light.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Some of the side effects listed are due to the medicine, anaesthesia and/or the surgery, or a combination of these.
Less serious side effects
| Less serious side effects | What to do |
General or affecting different parts of the body:
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
| Nervous system related: Neurological disorders which may include
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects in Australia to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems
If you are located in New Zealand, contact Medsafe at pophealth.my.site.com/carmreportnz/s/. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What GLIOLAN contains
| Active ingredient (main ingredient) | Aminolevulinic acid hydrochloride |
| Other ingredients (inactive ingredients) | None |
This medicine does not contain lactose, sucrose, gluten, tartrazine or any other azo dyes.
Do not take this medicine if you are allergic to any of this ingredient.
What GLIOLAN looks like
GLIOLAN is a powder for oral solution. It is a white to off-white cake powder stored in a glass vial (Aust R 202549).
When the powder is dissolved in water the solution is a clear and colourless to slightly yellowish fluid.
GLIOLAN is provided in a glass vial and presented in packs of 1, 2 and 10 vials. Not all pack sizes may be marketed.
Who distributes GLIOLAN
In Australia
Specialised Therapeutics Glio Pty Ltd
Level 2, 17 Cotham Road
Kew, Victoria 3101
Ph: 1300 798 820
www.stbiopharma.com
In New Zealand:
Specialised Therapeutics Limited
Level 1, The Lane,
Botany Town Centre
588 Chapel Road, East Tamaki, Auckland 2013, New Zealand
Tel: +64 9801 0299
This leaflet was prepared in November 2025.
Brand Information
| Brand name | Gliolan |
| Active ingredient | Aminolevulinic acid hydrochloride |
| Schedule | S4 |
MIMS Revision Date: 01 December 2025
1 Name of Medicine
Aminolevulinic acid hydrochloride 30 mg/mL powder for oral solution.
2 Qualitative and Quantitative Composition
One vial contains 1.5 g of aminolevulinic acid hydrochloride (ALA HCl), equivalent to 1.17 g of aminolevulinic acid.
One mL of reconstituted solution contains 30 mg of aminolevulinic acid hydrochloride (ALA HCl), equivalent to 23.4 mg of aminolevulinic acid.
Excipient(s) with known effect. For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Gliolan is supplied in a vial as a powder for oral solution.
The powder is a white to off-white cake.
4 Clinical Particulars
4.1 Therapeutic Indications
Gliolan is indicated in adult patients for visualisation of malignant tissue during surgery for malignant gliomas that are glioblastoma multiforme (GBM) on preoperative imaging, and who are intended for resection of the tumour.
4.2 Dose and Method of Administration
Gliolan should only be used by experienced neurosurgeons conversant with surgery of malignant gliomas and in-depth knowledge of functional brain anatomy who have completed a training course in fluorescence-guided surgery.
Dose. The recommended dose is 20 mg aminolevulinic acid hydrochloride per kilogram body weight.
Special populations. Elderly. There are no special instructions for use in elderly patients with regular organ function.
Renal or hepatic impairment. No trials have been performed in patients with clinically relevant hepatic or renal impairment. Therefore, Gliolan should be used with caution in such patients.
Paediatric population. The safety and efficacy of ALA in children and adolescents aged 0 to 18 years has not yet been established. No data are available.
Method of administration. The solution should be administered orally three hours (range 2-4 hours) before anaesthesia. Use of ALA under conditions other than the ones used in the clinical trials entail an undetermined risk.
If the surgery is postponed by more than 12 hours, surgery should be re-scheduled for the next day or later. Another dose of this medicine can be taken 2 - 4 hours before anaesthesia.
For instructions on reconstitution of the medicine before administration, see Section 6.6 Special Precautions for Disposal.
4.3 Contraindications
Hypersensitivity to ALA or porphyrins or to any of the excipients listed in Section 6.1 List of Excipients.
Acute or chronic types of porphyria.
Pregnancy (see Section 4.6 Fertility, Pregnancy and Lactation; Section 5.3 Preclinical Safety Data for further information).
4.4 Special Warnings and Precautions for Use
Gliolan should only be used by experienced neurosurgeons conversant with surgery of malignant gliomas and in-depth knowledge of functional brain anatomy who have completed a training course in fluorescence-guided surgery.
ALA-induced fluorescence of brain tissue does not provide information about the tissue's underlying neurological function. Therefore, resection of fluorescing tissue should be weighed up carefully against the neurological function of fluorescing tissue.
Special care must be taken in patients with a tumour in the immediate vicinity of an important neurological function and pre-existing focal deficits (e.g. aphasia, vision disturbances and paresis etc.) that do not improve on corticosteroid treatment. Fluorescence-guided resection in these patients has been found to impose a higher risk of critical neurological deficits. A safe distance to eloquent cortical areas and subcortical structures of at least 1 cm should be maintained independent of the degree of fluorescence.
In all patients with a tumour in the vicinity of an important neurological function, either pre- or intraoperative measures should be used to localise that function relative to the tumour in order to maintain safety distances.
False negative and false positive results may occur with the use of 5-ALA for intraoperative visualisation of malignant glioma. Non-fluorescing tissue in the surgical field does not rule out the presence of tumour in patients with glioma. On the other hand, fluorescence may be seen in areas of abnormal brain tissue (such as reactive astrocytes, atypical cells), necrotic tissue, inflammation, infections (such as fungal or bacterial infections and abscesses), CNS lymphoma or metastases from other tumour types.
After administration of Gliolan, exposure of eyes and skin to strong light sources (e.g. operating illumination, direct sunlight or brightly focused indoor light) should be avoided for 24 hours.
Co-administration with other potentially phototoxic substances (e.g. tetracyclines, sulfonamides, fluoroquinolones, hypericin extracts) should be avoided (see Section 5.3 Preclinical Safety Data).
Within 24 hours after administration, other potentially hepatotoxic medicinal products should be avoided. In patients with pre-existing cardiovascular disease, Gliolan should be used with caution since literature reports have shown decreased systolic and diastolic blood pressures, pulmonary artery systolic and diastolic pressure as well as pulmonary vascular resistance.
Use in the elderly. See Section 4.2 Dose and Method of Administration, Special populations.
Paediatric use. See Section 4.2 Dose and Method of Administration, Special populations.
Effects on laboratory tests. See Section 4.8 Adverse Effects (Undesirable Effects).
4.5 Interactions with Other Medicines and Other Forms of Interactions
Patients should not be exposed to any photosensitising agent up to 2 weeks after administration of Gliolan.
In the absence of compatibility studies, Gliolan must not be mixed with other medicinal products, see Section 6.6 Special Precautions for Disposal.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. There are no data available regarding the influence of Gliolan on fertility.
Use in pregnancy. (Category C)
There are no or limited amount of data from the use of Gliolan in pregnant woman. Some limited animal studies suggest an embryotoxic activity of ALA plus light exposure (see Section 5.3 Preclinical Safety Data). Therefore, Gliolan should not be used during pregnancy.
Use in lactation. It is unknown whether ALA or its metabolite protoporphyrin IX (PPIX) is excreted in human breast milk. The excretion of ALA or PPIX in milk has not been studied in animals. Breast-feeding should be interrupted for 24 hours after treatment with Gliolan.
4.7 Effects on Ability to Drive and Use Machines
Not relevant, as the surgical procedure itself will have an influence on the ability to drive and use machines.
4.8 Adverse Effects (Undesirable Effects)
Summary of the safety profile. Adverse reactions observed after the use of Gliolan for fluorescence-guided glioma resection are divided into the following two categories:
immediate reactions occurring after oral administration of the medicinal product before anaesthesia (= active substance-specific side effects);
combined effects of ALA, anaesthesia, and tumour resection (= procedure-specific side effects).
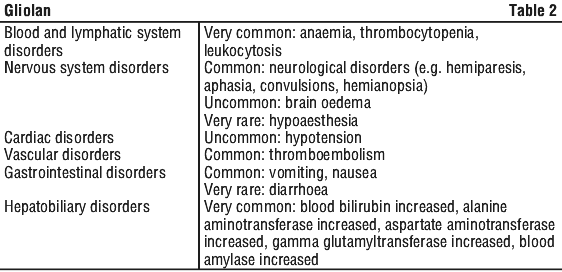
Side effects of concern were photosensitivity as substance-related effect; neurological disorders (e.g. convulsions, hemiparesis, and aphasia); pulmonary embolism that were more frequent in patients receiving ALA and surgery; and anaemia, thrombocytopenia and leukocytosis seen with equal frequency after surgery, with and without ALA. Further frequently observed side effects are vomiting, nausea and increase of blood bilirubin, alanine aminotransferase, aspartate aminotransferase, gamma glutamyltransferase and blood amylase.
Tabulated summary of adverse reactions. Very common (≥ 1/10). Common (≥ 1/100 to < 1/10). Uncommon (≥ 1/1,000 to < 1/100). Rare (≥ 1/10,000 to < 1/1,000). Very rare (< 1/10,000). Not known (cannot be estimated from the available data).
Substance specific side effects. See Table 1.

In another single-centre trial, 21 patients with malignant glioma received 0.2, 2, or 20 mg/kg body weight ALA HCl followed by fluorescence-guided tumour resection. The only adverse reaction reported in this trial was one case of mild sunburn occurring in a patient treated with the highest dose.
In a single-arm trial including 36 patients with malignant glioma, drug reactions were reported in four patients (mild diarrhoea in one patient: moderate hypesthesia in another patient: moderate chills in another patient, and arterial hypotension 30 minutes after application of ALA in another patient). All patients received the medicinal product in a dose of 20 mg/kg body weight and underwent fluorescence-guided resection. Follow-up time was 28 days.
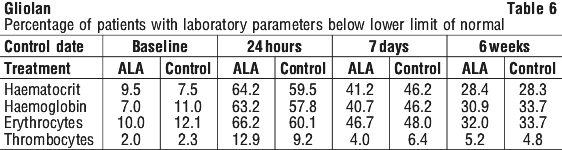
In a comparative, unblinded phase III trial (MC-ALS.3/GLI), 201 patients with malignant gliomas received ALA HCl in a dose of 20 mg/kg body weight and 176 of these patients underwent fluorescence-guided resection with subsequent radiotherapy. 173 patients received standard resection without administration of the medicinal product and subsequent radiotherapy. Follow-up time comprised at least 180 days after administration. At least possibly related adverse reactions were reported in 2/201 (1.0%) patients: mild vomiting 48 hours after trial surgery, and mild photosensitivity 48 hours after study surgery. In patients undergoing fluorescence-guided resection, the incidence of pulmonary embolism was significantly increased (7.4% cf 1.2%, p=0.006). However, the median time of onset of pulmonary embolism after study surgery was 35 days (range 1-150 days). Another patient accidentally received an overdose of the medicinal product (3000 mg instead of 1580 mg). Respiratory insufficiency, which was reported in this patient, was managed by adaptation of ventilation and resolved completely. A more pronounced transient increase of liver enzymes without clinical symptoms was observed in the ALA treated patients. Peak values occurred between 7 and 14 days after administration. Increased levels of amylase, total bilirubin, and leukocytes, but decreased levels of thrombocytes and erythrocytes were observed, however differences between treatment groups were not statistically significant.
Table 3 shows adverse events reported with a frequency of > 1% of patients in this trial.
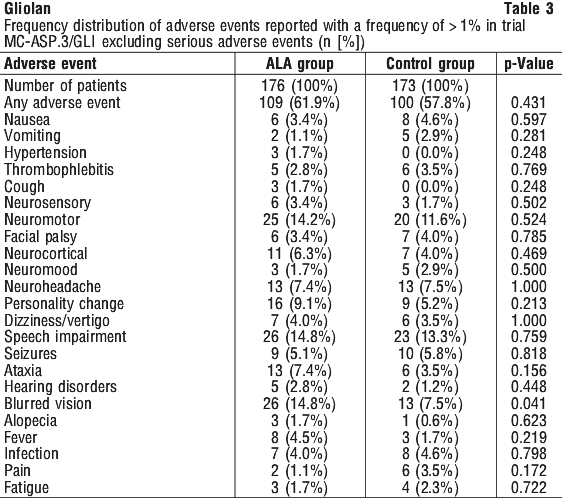
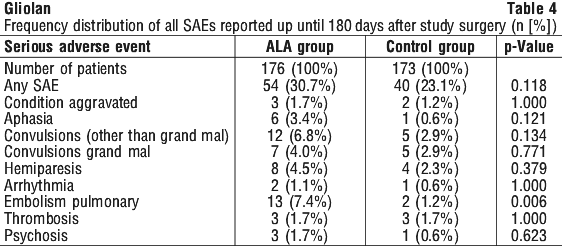
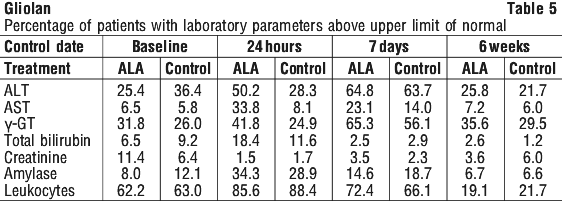
4.9 Overdose
Within a clinical trial, a 63-year old patient with known cardiovascular disease was accidentally given an overdose of ALA HCl (3000 mg instead of 1580 mg). During surgery he developed respiratory insufficiency, which was managed by adaptation of ventilation. After surgery the patient also displayed facial erythema. It was stated that the patient had been exposed to more light than permitted for the trial. Respiratory insufficiency and erythema completely resolved.
In the event of overdose, supportive measures should be provided as necessary, including sufficient protection from strong light sources (e.g. direct sunlight).
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26.
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Pharmacotherapeutic group: Antineoplastic agents, sensitisers used in photodynamic therapy, ATC code: L01XD04.
Mechanism of action. Aminolevulinic acid (ALA) is a natural biochemical precursor of heme that is metabolised in a series of enzymatic reactions to fluorescent porphyrins, particularly PPIX. ALA synthesis is regulated by an intracellular pool of free heme via a negative feedback mechanism. Administration of excess exogenous ALA avoids the negative feedback control, and accumulation of PPIX occurs in target tissue. In the presence of visible light, fluorescence of PPIX (photodynamic effect) in certain target tissues can be used for photodynamic diagnosis.
Pharmacodynamic effects. Systemic administration of ALA results in an overload of the cellular porphyrin metabolism and accumulation of PPIX in various epithelia and cancer tissues. Malignant glioma tissue (WHO-grade III and IV, e.g. glioblastoma, gliosarcoma or anaplastic astrocytoma) has also been demonstrated to synthesise and accumulate porphyrins in response to ALA administration. The concentration of PPIX is significantly lower in white matter than in cortex and tumour. Tissue surrounding the tumour and normal brain may also be affected. However, ALA induced PPIX formation is significantly higher in malignant tissue than in normal brain.
In contrast, in low-grade tumours (WHO-grade I and II, e.g. oligodendroglioma) no fluorescence could be observed after application of the active substance. Medulloblastoma or brain metastases revealed inconsistent results or no fluorescence.
The phenomenon of PPIX accumulation in WHO-grade III and IV malignant gliomas may be explained by higher ALA uptake into the tumour tissue or an altered pattern of expression or activity of enzymes (e.g. ferrochelatase) involved in haemoglobin biosynthesis in tumour cells.
Explanations for higher ALA uptake include a disrupted blood-brain barrier, increased neo-vascularisation, and the overexpression of membrane transporters in glioma tissue.
After excitation with blue light (lambda = 400-410 nanometre), PPIX is strongly fluorescent (peak at lambda = 635 nanometre) and can be visualised after appropriate modifications to a standard neurosurgical microscope.
Fluorescence emission can be classified as intense (solid) red fluorescence (corresponds to vital, solid tumour tissue) and vague pink fluorescence (corresponds to infiltrating tumour cells), whereas normal brain tissue lacking enhanced PPIX levels reflects the violet-blue light and appears blue.
Clinical trials. In a phase I/II trial including 21 patients, a dose-efficacy relationship between the dose levels and the extent and quality of fluorescence in the tumour core was detected: higher doses of ALA enhanced the fluorescence quality and the fluorescence extent of the tumour core compared to demarcation of the tumour core under standard white illumination in a monotone, non-falling fashion. The highest dose (20 mg/kg body weight) was determined to be the most efficient.
A positive predictive value of tissue fluorescence of 84.8% (90% CI: 70.7%-93.8%) was found. This value was defined as the percentage of patients with positive tumour cell identification in all biopsies taken from areas of weak and strong fluorescence. The positive predictive value of strong fluorescence was higher (100.0%; 90% CI: 91.1%-100.0%) than of weak fluorescence (83.3%; 90% CI: 68.1%-93.2%). Results were based on a phase II trial including 33 patients receiving ALA HCl in a dose of 20 mg/kg body weight.
The resulting fluorescence was used as an intraoperative marker for malignant glioma tissue with the aim of improving the surgical resection of these tumours.
In a phase III trial with 349 patients with suspected malignant glioma amenable to complete resection of contrast-enhancing tumour were randomised to fluorescence-guided resection after administration of 20 mg/kg body weight ALA HCl or conventional resection under white light. Contrast-enhancing tumour was resected in 64% of patients in the experimental group compared to 38% in the control-group (p < 0.0001).
At the visit six months after tumour resection, 20.5% of ALA treated patients and 11% of patients who underwent standard surgery were alive at the six-month visit without progression. The difference was statistically significant using the chi-square test (p=0.015). No significant increase in overall survival has been observed in this trial, however, it was not powered to detect such a difference.
5.2 Pharmacokinetic Properties
General characteristics. Gliolan shows good solubility in aqueous solutions. After ingestion, ALA itself is not fluorescent but is taken up by tumour tissue (see Section 5.1 Pharmacodynamic Properties) and is intracellularly metabolised to fluorescent porphyrins, predominantly PPIX.
Absorption. ALA as drinking solution is rapidly and completely absorbed and peak plasma levels of ALA are reached 0.5-2 hours after oral administration of 20 mg/kg body weight. The median (range) Cmax value was 20.8 (11.6 - 27.7) mg/L in normal subjects and 8.2 (7.4 - 9.7) mg/L in patients. The reason for the difference has not been established. Plasma levels return to baseline values 24 hours after administration of an oral dose of 20 mg/kg body weight. The influence of food has not been investigated because Gliolan is generally given on empty stomach prior to induction of anaesthesia.
Distribution and metabolism. ALA is preferentially taken up by the liver, kidney, endothelials and skin as well as by malignant gliomas (WHO-grade III and IV) and metabolised to fluorescent PPIX. Four hours after oral administration of 20 mg/kg body weight ALA HCl, the maximum PPIX plasma level is reached. PPIX plasma levels rapidly decline during the subsequent 20 hours and are not detectable anymore 48 hours after administration. At the recommended oral dose of 20 mg/kg body weight, tumour to normal brain fluorescence ratios are usually high and offer lucid contrast for visual perception of tumour tissue under violet-blue light for at least 9 hours.
Besides tumour tissue, faint fluorescence of the choroid plexus was reported. ALA is also taken up and metabolised to PPIX by other tissues, e.g. liver, kidneys or skin (see Section 4.4 Special Warnings and Precautions for Use). Plasma protein binding of ALA is unknown.
Excretion. ALA is eliminated quickly with a terminal half-life of 1-3 hours. The shorter half-life was seen in normal subjects and the longer half-life in patients. Approximately 30% of an orally administered dose of 20 mg/kg body weight is excreted unchanged in urine within 12 hours.
Linearity/nonlinearity. By regression analysis, the AUC0-inf of ALA plasma levels versus dose was linear over the dose range (0.2, 2, and 20 mg/kg) studied (R2 = 0.9998). Dose proportionality was not found for the active metabolite, PPIX, within 12 hours in normal patients.
Renal or hepatic impairment. Pharmacokinetics of ALA in patients with renal or liver impairment has not been investigated.
5.3 Preclinical Safety Data
Standard safety pharmacology experiments were performed under light protection in the mouse, rat and dog. ALA administration does not influence the function of the gastro-intestinal and central nervous system. A slight increase in saluresis cannot be excluded.
Single administration of high doses of ALA to mice or rats leads to unspecific findings of intolerance without macroscopic abnormalities or signs of delayed toxicity. Repeat-dose toxicity studies performed in rats and dogs demonstrate dose-dependent adverse reactions affecting changes in bile duct histology (non-reversible within a 14 day recovery period), transient increase in transaminases, LDH, total bilirubin, total cholesterin, creatinine, urea and vomiting (only in dogs). Signs of systemic toxicity (cardiovascular and respiratory parameters) occurred at higher doses in the anaesthetised dog: at 45 mg/kg body weight intravenously a slight decrease in peripheral arterial blood pressure and systolic left ventricular pressure was recorded. Five minutes after administration, the baseline values had been reached again. The cardiovascular effects seen are considered to be related to the intravenous route of administration.
Phototoxicity observed after ALA treatment in vitro and in vivo is obviously closely related to dose- and time-dependent induction of PPIX synthesis in the irradiated cells or tissues. Destruction of sebaceous cells, focal epidermal necrosis with a transient acute inflammation and diffuse reactive changes in the keratinocytes as well as transient secondary oedema and inflammation of dermis are observed. Light exposed skin recovered completely except for a persistent reduction in the number of hair follicles. Accordingly, general light protective measures of eyes and skin are recommended for at least 24 hours after administration of Gliolan.
Although pivotal studies on the reproductive and developmental behaviour of ALA have not been performed, it can be concluded that ALA induced porphyrin synthesis may lead to embryotoxic activity in mouse, rat and chick embryos only under the condition of direct concomitant light exposure. Gliolan should, therefore, not be administered to pregnant women. Excessive single dose treatment of rats with ALA reversibly impaired male fertility for two weeks after dosing.
Genotoxicity. The majority of genotoxicity studies performed in the dark do not reveal a genotoxic potential of ALA. The compound potentially induces photogenotoxicity after subsequent irradiation or light exposure, which is obviously related to the induction of porphyrin synthesis.
Carcinogenicity. Long-term in vivo carcinogenicity studies have not been conducted. However, considering the therapeutic indication, a single oral treatment with ALA might not be related to any serious potential carcinogenic risk.
6 Pharmaceutical Particulars
6.1 List of Excipients
None.
6.2 Incompatibilities
In the absence of compatibility studies, Gliolan must not be mixed with other medicines except those mentioned in Section 6.6 Special Precautions for Disposal.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date of the unopened vial can be found on the packaging.
6.4 Special Precautions for Storage
Store the vials in original cartons below 25°C. Protect from light.
Storage conditions after reconstitution. The reconstituted solution is physically-chemically stable for 24 hours at 25°C. Use within 4 hours of reconstitution.
6.5 Nature and Contents of Container
Clear type I 50 mL glass vial with butyl rubber stopper and secured with aluminium 'push tear-off' cap. Contains 1.5 g powder for reconstitution in 50 mL of drinking water.
Pack sizes. 1, 2 and 10 vials of powder in a carton.
Not all pack sizes may be marketed.
6.6 Special Precautions for Disposal
Reconstitution. The oral solution is prepared by dissolving the amount of powder of one vial in 50 mL of drinking water. The reconstituted solution is a clear and colourless to slightly yellowish fluid.
In the absence of compatibility studies, Gliolan must not be mixed with other medicinal products.
Disposal. Any unused product or waste material should be disposed of in accordance with local requirements. Gliolan is for single use only and any content remaining after first use must be discarded.
6.7 Physicochemical Properties
Chemical structure. Chemical Formula: C5H9NO3.HCl.
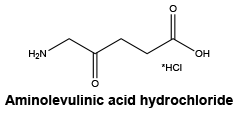
Molecular Weight: 167.59 g/mol. Freely soluble in water. pKa1: 3.90. pKa2: 8.05. The reconstituted solution has a pH of approximately 2.2 - 2.8.
7 Medicine Schedule (Poisons Standard)
Australia: S4.
Date of First Approval
07 November 2013
Date of Revision
13 October 2025
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.