Glucose 50%
Brand Information
| Brand name | Glucose 50% |
| Active ingredient | Glucose |
| Schedule | Unscheduled |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Glucose 50%.
Summary CMI
Glucose 50%
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why is this Glucose 50% being given?
Glucose 50% contains the active ingredient glucose (as anhydrous). Glucose 50% is used to treat low blood sugar levels. It may also be added to intravenous solutions as a source of calories for patients unable to consume food as well as used to treat pressure on the brain and spinal cord and/or swelling of the body caused from consuming to much alcohol.
For more information, see Section 1. Why is Glucose 50% being given? in the full CMI.
2. What should I know before Glucose 50% is given?
Do not use if you have ever had an allergic reaction to Glucose 50% or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before Glucose 50% is given? in the full CMI.
3. What if I am using other medicines?
Some medicines may interfere with Glucose 50% and affect how it works.
A list of these medicines is in Section 3. What if I am using other medicines? in the full CMI.
4. How is Glucose 50% given?
Your doctor will decide what dose of glucose you will receive and for how long you will receive it. This depends on your medical condition and other factors, such as your weight.
More instructions can be found in Section 4. How is Glucose 50% given? in the full CMI.
5. What should I know while using Glucose 50%?
| Things you should do |
|
| Looking after the medicine |
|
For more information, see Section 5. What should I know while using Glucose 50%? in the full CMI.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention. These include flushing causing redness over face and/or body. However, some side effects may require urgent medical attention. These include pain, burning or swelling at the site of injection, swelling of the hands, ankles or feet, symptoms caused by low levels of potassium, magnesium or phosphorus in the blood including drowsiness, loss of appetite, muscle twitching or trembling, nausea or vomiting, unusual tiredness or weakness, shortness of breath, wheezing or difficulty breathing, swelling of face lips tongue or other parts of the body, rash, itching or hives on the skin.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
Glucose 50%
Active ingredient: glucose (as anhydrous)
Consumer Medicine Information (CMI)
This leaflet provides important information about Glucose 50%. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using Glucose 50%.
Where to find information in this leaflet:
1. Why is Glucose 50% being given?
2. What should I know before Glucose 50% is given?
3. What if I am using other medicines?
4. How is Glucose 50% given?
5. What should I know while using Glucose 50%?
6. Are there any side effects?
7. Product details
1. Why is Glucose 50% being given?
Glucose 50% contains the active ingredient glucose (as anhydrous). Glucose 50% is a sugar which provides energy for the body.
Glucose 50% is used to treat low blood sugar levels. It may also be:
- added to intravenous solutions as a source of calories for patients unable to consume food.
- used to treat pressure on the brain and spinal cord and/or swelling of the body caused from consuming too much alcohol.
Ask your doctor if you have any questions about why Glucose 50% has been prescribed for you.
Your doctor may have prescribed it for another reason.
2. What should I know before Glucose 50% is given?
Warnings
You should not be given Glucose 50% if:
- you are allergic to glucose (as anhydrous) or any of the ingredients listed at the end of this leaflet.
Always check the ingredients to make sure you can use this medicine. - You have an allergy to:
- any medicine containing glucose
- any medicine listed at the end of this leaflet
- corn (maize) and corn products - You have of the following medical conditions:
- very high blood sugar levels
- difficulty digesting sugars
- unable to pass urine
- bleeding in the brain
- at risk of, or after a stroke
- dehydration - The solution is discoloured, cloudy, turbid, or a precipitate or particles are present.
This solution is normally a clear, colourless to faintly straw-coloured liquid. - If the solution causes a precipitate, discolouration or cloudiness to form when added to an intravenous (IV) solution.
- The medicine is after the expiry date printed on the pack, or if the packaging is torn or shows signs of tampering. If you are given this medicine after the expiry date has passed, it may not work as well.
- You are unsure whether you should be given this medicine talk to your doctor.
Check with your doctor if you:
- Have any allergies to any other medicines, foods, preservatives or dyes.
- Have or have had any of the following medical conditions:
- type II diabetes
- severe under-nutrition
- problems digesting carbohydrates or sugars
- vitamin B1 (thiamine) deficiency
- chronic alcoholism
- low levels of potassium, magnesium or phosphorous
- blood poisoning or serious infection
- recent IV (intravenous) infusion - Take any medicines for any other condition
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor if you are pregnant or intend to become pregnant.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
Your doctor can discuss with you the risks and benefits involved.
Children
- If your child is to be given Glucose 50% tell your doctor if the mother suffers from diabetes. Glucose 50% should be used with caution in infants with diabetic mothers.
3. What if I am using other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with Glucose 50% and affect how it works. These include:
- corticosteroids
- corticotrophin
These medicines may be affected by Glucose 50% or may affect how well it works. You may need to take different medicines. You may need different amounts of your medicine, or you may need to take different medicines.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect Glucose 50%.
4. How is Glucose 50% given?
How much to be given
- Glucose 50% must only be given by a doctor or nurse
It is usually diluted by adding to an intravenous (IV) solution and then injected into a vein.
It may also be directly injected slowly into a vein without being diluted for some medical conditions. - Your doctor will decide what dose of glucose you will receive and for how long you will receive it. This depends on your medical condition and other factors, such as your weight.
If too much Glucose 50% is given
Glucose 50% must only be given by a nurse or a doctor, so an overdose is not likely to occur.
Immediately contact your doctor if you notice the following symptoms of an overdose:
- mental confusion
- dehydration causing thirst or lack of urination
If you think too much Glucose 50% is used, you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know while using Glucose 50%?
Things you should do
If you are about to be started on any new medicine, remind your doctor and pharmacist that you have been given Glucose 50%.
If you are going to have surgery, tell the surgeon or anaesthetist that you have been given this medicine.
It may interfere with the results of some tests.
Remind any doctor, dentist or pharmacist you visit that you are using Glucose 50%.
If you are about to have any blood tests, tell your doctor that you have been given this medicine. It may interfere with the results of some tests.
Drinking alcohol
Tell your doctor if you drink alcohol.
Looking after your medicine
- Glucose 50% will be stored in the surgery, pharmacy, or ward of a hospital. The injection is kept in a cool dry place where the temperature stays below 25°C.
- Glucose 50% will be opened for use on you. It will be used only once and then it will be discarded.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Do not be alarmed by the following list of side effects. You may not experience any of them.
Side effects
| Less serious side effects | What to do |
Skin related:
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
Localized symptoms:
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Symptoms of allergic reactions
|
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Some side effects can only be found when your doctor does tests from time to time to check your progress.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What Glucose 50% contains
| Active ingredient (main ingredient) | Glucose monohydrate |
| Other ingredients (inactive ingredients) |
|
| Potential allergens | Glucose monohydrate |
Do not take this medicine if you are allergic to any of these ingredients.
This medicine does not contain lactose, sucrose, gluten, tartrazine or any other azo dyes or preservatives.
What Glucose 50% looks like
Glucose 50% is a clear, colourless to faintly straw-coloured solution in a clear glass vial.
Glucose 50% is available in 50 mL vials, packaged in a pack of 10 (AUST R 12420).
Who distributes Glucose 50%
Phebra Pty Ltd
17-19 Orion Road
Lane Cove West, NSW 2066
Australia
Telephone: 1800 720 020

This leaflet was prepared in August 2025.
Phebra and the Phi symbol are registered trademarks of Phebra Pty Ltd.
Brand Information
| Brand name | Glucose 50% |
| Active ingredient | Glucose |
| Schedule | Unscheduled |
MIMS Revision Date: 01 April 2021
1 Name of Medicine
Glucose monohydrate.
2 Qualitative and Quantitative Composition
Glucose 50% contains glucose monohydrate 27.5 g in 50 mL equivalent to glucose anhydrous 25 g per 50 mL (500 mg/mL or 50%) in water for injections.
Glucose 50% is strongly hypertonic. The solution has a pH range of 3.5 to 6.5.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Glucose 50% is a clear, colourless to faintly straw coloured, particle-free solution for intravenous infusion.
4 Clinical Particulars
4.1 Therapeutic Indications
Glucose 50% intravenous infusion is strongly hypertonic and may be used to reduce increased cerebrospinal pressure and/or oedema due to delirium tremens or acute alcoholic intoxication. It may also be used to treat severe hypoglycaemia due to an excess of insulin and to provide concentrated calories in total parenteral nutrition regimes.
4.2 Dose and Method of Administration
Glucose 50% intravenous infusion is strongly hypertonic and must be administered via the intravenous (IV) route only. Except in the emergency treatment of severe hypoglycaemia, Glucose 50% intravenous infusion should be appropriately diluted and administered via an IV catheter carefully placed in a large central vein.
For emergency treatment of hypoglycaemia, Glucose 50% intravenous infusion may be administered slowly (e.g. 3 mL/minute) via a small bore needle carefully placed in a large peripheral vein.
The dose of glucose is dependent on the age, weight and fluid, electrolyte, glucose and acid/ base balance of the patient. The rate of infusion should not exceed 0.5 g/kg/hr to avoid glycosuria.
Acute hypoglycaemia. Adults and children. 20-50 mL of Glucose 50% intravenous infusion administered by slow IV injection as an initial dose. The total dose will vary depending on the patient's response and blood glucose levels. Provision must be made to maintain the patient's blood glucose level after the initial response.
Neonates and infants. 1 mL/kg of Glucose 50%, then adjust as required. Due to the increased risk of phlebitis with glucose solutions over 10%, a central line should be considered.
4.3 Contraindications
Glucose 50% intravenous infusion is contraindicated in:
Diabetic coma while blood sugar levels are excessively high.
Glucose-galactose malabsorption syndrome.
Patients with anuria or intraspinal or intracranial haemorrhage and in dehydrated delirium tremens patients.
Patients at risk for ischaemic stroke. Use after an ischaemic stroke episode.
Patients with known allergy to corn (maize) and corn products.
4.4 Special Warnings and Precautions for Use
The use of hypertonic glucose solutions may result in dehydration, therefore, regular monitoring of the hydration status of the patient is recommended. It is important that hypertonic glucose solutions are administered slowly, because rapid administration may produce a local rise in the osmotic tension of the blood at the point of injection.
Intravenous administration of hypertonic glucose solutions may cause venous thrombosis, so it is important to employ proper techniques to avoid vein damage. It is recommended that the intravenous injection be given slowly, using a small bore needle and avoiding the walls of the vein if possible. The tourniquet should be removed as soon as venipuncture has occurred. Warming the arm and the solution to room temperature will help to avoid adverse sequelae.
Intravenous administration of glucose solutions, especially as infusions, may cause fluid overload with a resultant dilution of serum electrolytes and possible peripheral and pulmonary oedema. Prolonged therapy should be monitored for changes in fluid balance, electrolyte concentration and acid/ base balance.
Glucose solutions should be used with caution in patients with subclinical diabetes mellitus, severe undernutrition or with carbohydrate intolerance.
Hyperglycaemia and glycosuria may occur as a result of an over rapid rate of infusion or metabolic insufficiency. Blood and urine glucose should be monitored regularly.
Avoid use after an ischaemic stroke episode as, under this condition, the induced lactic acidosis aggravates the recovery of the damaged brain tissue. Thiamine diphosphate cocarboxylase is an essential coenzyme in carbohydrate metabolism, therefore, patients having thiamine deficiency should be treated cautiously with glucose injection. This is particularly important in patients who chronically abuse alcohol as this may precipitate an overt deficiency syndrome, e.g. Wernicke's encephalopathy.
Glucose solutions should not be infused concomitantly through the same IV set as blood, because agglomeration or haemolysis may occur.
Cautious use of glucose solutions is required in patients with thiamine deficiency, hypokalaemia, hypophosphataemia, hypomagnesaemia, haemodilution, sepsis and trauma.
Prolonged parenteral administration of glucose may affect insulin production. To avoid this it may be necessary to add insulin to the infusion. A review of a patient's oral hypoglycaemic or insulin requirements may be necessary. Additives may be incompatible with glucose. Do not administer such preparations unless the solution is clear. Do not store solutions containing additives unless compatibility has been proven. While some incompatibilities are readily observed, one must be aware that subtle physical, chemical and pharmacological incompatibilities can occur. The medical literature, the package insert and other available sources of information should be reviewed for a thorough understanding of possible incompatibility problems. In particular, the product information document of any added medication should be checked for any incompatibility with Glucose 50%.
Use in the elderly. No data available.
Paediatric use. Use with caution in infants of diabetic mothers.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Parenteral fluids, especially those containing sodium ions, should be administered with caution to patients receiving corticosteroids or corticotropin.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. No data available.
Use in pregnancy. Safety in pregnancy has not been established. Use only when clearly needed and potential benefits outweigh risk to the fetus.
Use in lactation. Safety in lactation has not been established. Use only when clearly needed and potential benefits outweigh risk to the baby.
4.7 Effects on Ability to Drive and Use Machines
The effects of this medicine on a person's ability to drive and use machines were not assessed as part of its registration.
4.8 Adverse Effects (Undesirable Effects)
Intravenous administration of hypertonic glucose solutions may cause local phlebitis or venous thrombosis and extravasation. If the solution is infused too rapidly, local pain and vein irritation may occur. A fever response and infection at the site of injection may also occur due to contamination of the solution or poor techniques of administration.
Hyperglycaemia and glycosuria may occur if glucose is administered at a rate greater than 0.5 g/kg/hr. Disruption of the fluid and acid/ base balance and dilution of electrolyte concentrations may occur during prolonged usage, resulting in oedema, hypokalaemia, hypomagnesaemia and hypophosphataemia (see Section 4.4 Special Warnings and Precautions for Use).
Vitamin B complex deficiency may occur with glucose administration.
High concentrations of glucose administered intravenously may induce an increased histamine release from blood cells resulting in anaphylactoid reactions. Anaphylactoid effects have been reported in two patients with both asthma and diabetes mellitus.
Rapid infusion of glucose 25-30 g over 3 minutes may occasionally cause a generalised flush. This subsides within 10 minutes.
Reporting suspected adverse reactions. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
Hyperglycaemia and glycosuria, if undetected, can lead to mental confusion, dehydration, hyperosmolar coma and death. Appropriate treatment may include decreasing the infusion rate of glucose and administration of insulin.
Fluid overload and biochemical imbalance resulting from overdosage with glucose solution should be treated with appropriate corrective therapy.
For information on the management of overdose, contact the Poisons Information Centre on 131126 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Glucose is a monosaccharide which provides the principal source of energy for the body. It is also involved in many additional areas of protein and fat metabolism. Glucose is stored in the body as fat and in the muscles and liver as glycogen. Glucose is rapidly metabolised from glycogen; it increases blood glucose concentrations and provides energy. However, when this supply is insufficient the body mobilises its fat stores to release energy. Glucose may also decrease body protein and nitrogen losses, promote glycogen deposition. Glucose is metabolised to carbon dioxide and water thus providing water for body hydration as well as calories.
Clinical trials. No data available.
5.2 Pharmacokinetic Properties
Distribution. Glucose is stored in the body as fat and in the muscles and liver as glycogen.
Metabolism. Glucose is metabolised to carbon dioxide and water, thus providing water for body hydration as well as calories.
Excretion. No data available.
5.3 Preclinical Safety Data
Genotoxicity. No data available.
Carcinogenicity. No data available.
6 Pharmaceutical Particulars
6.1 List of Excipients
Glucose 50% is a sterile solution of anhydrous glucose in water for injections, adjusted to pH 3.5-6.5 with sodium bicarbonate or hydrochloric acid.
6.2 Incompatibilities
See Section 4.4 Special Warnings and Precautions for Use; Section 4.5 Interactions with Other Medicines and Other Forms of Interactions.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the ARTG1. The expiry date can be found on the packaging.
1 AUST R 12420.
6.4 Special Precautions for Storage
Store below 25°C.
6.5 Nature and Contents of Container
It is presented in a 50 mL glass vial as a pack of 10.
Phebra product code INJ128.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
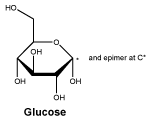
Chemical name: monohydrate of (+)-D-glucopyranose.
The molecular weight of the compound is 198.2. The molecular formula is C6H12O6.H2O.
Chemical structure.
7 Medicine Schedule (Poisons Standard)
Unscheduled.
Date of First Approval
13 August 1991
Date of Revision
05 February 2021
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.