Havrix 1440 and Havrix Junior
Brand Information
| Brand name | Havrix 1440 and Havrix Junior |
| Active ingredient | Hepatitis A vaccine |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Havrix 1440 and Havrix Junior.
Summary CMI
HAVRIX 1440 and HAVRIX Junior
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about receiving this vaccine, speak to your doctor, nurse or pharmacist.
1. Why am I being given HAVRIX?
HAVRIX is used to prevent hepatitis A infection. In this leaflet, HAVRIX refers to the use of both HAVRIX 1440 for adults, and HAVRIX Junior for children. HAVRIX contains inactivated hepatitis A virus.
For more information, see Section 1. Why am I being given HAVRIX? in the full CMI.
2. What should I know before I am given HAVRIX?
Do not receive this vaccine if you/your child has ever had an allergic reaction to HAVRIX or any of the ingredients listed at the end of the CMI.
You should not be given HAVRIX if you have/your child has a severe infection with a high temperature. A minor infection such as a cold should not be a problem, but talk to your doctor or nurse about this before being vaccinated.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I am given HAVRIX? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with HAVRIX and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How is HAVRIX given?
- HAVRIX will be injected into the upper arm muscle in adults and older children, and into the thigh muscle in infants. For some people with bleeding problems, the dose may need to be given under the skin (subcutaneously).
- HAVRIX is generally given as a single dose on an elected date. If travelling overseas, HAVRIX should be given at least 2 weeks before departure. After one dose of HAVRIX, protection from hepatitis A lasts for at least 1 year. A second booster dose, given 6 to 12 months after the first dose, gives longer term protection.
More instructions can be found in Section 4. How is HAVRIX given? in the full CMI.
5. What should I know when being given HAVRIX?
| Things you should do |
|
| Driving or using machines |
|
| Looking after your vaccine |
|
For more information, see Section 5. What should I know when being given HAVRIX? in the full CMI.
6. Are there any side effects?
Side effects which have been reported include redness, swelling, a hard lump, soreness, bruising or itching around the injection site, headache, irritability, drowsiness, diarrhoea, vomiting, loss of appetite, stiff joints, aching muscles, headache, tiredness, fever, and feeling generally unwell.
As with all vaccines given by injection there is a very small risk of serious allergic reaction. For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
1. Why am I being given HAVRIX?
HAVRIX contains inactivated hepatitis A virus.
HAVRIX is a vaccine used to prevent hepatitis A infection.
The vaccine works by causing the body to produce its own protection (antibodies) against this disease.
HAVRIX cannot give you hepatitis A when you receive it as the virus in the vaccine has been killed.
Hepatitis A is an infectious disease, which can affect the liver. This disease is caused by the hepatitis A virus.
The hepatitis A virus can be passed from person to person in food and drink, or by swimming in water contaminated by sewage. Symptoms of hepatitis A begin 3 to 6 weeks after coming into contact with the virus. These consist of nausea (feeling sick), fever and aches and pains. After a few days the whites of eyes and skin may become yellowish (jaundice). The severity and type of symptoms can vary. Young children may not develop jaundice. Most people recover completely but the illness is usually severe enough to keep people off work for about a month.
Hepatitis A is very common in many parts of the world, and the risk of infection is greatest in those areas where hygiene and sanitation are poor. Such areas include Asia, India, Africa, Central and South America, the Pacific Islands, the Middle East, and the Mediterranean basin. HAVRIX is recommended for all travellers to these areas, including people in the armed forces.
Hepatitis A occurs in Australia, but is not common. Some groups of people however, are at risk of exposure to the disease and should be vaccinated. Vaccination is recommended for:
- healthcare workers
- day-care centre staff
- staff and residents of homes for the intellectually disabled
- sewage workers
- food handlers
- abusers of injectable drugs
- homosexual men
- people in contact with an infected person
- and people with some types of liver or blood disorders.
There is no specific treatment for hepatitis A. Therefore, vaccination is the best way to protect against infection in the longer term.
HAVRIX will not protect against hepatitis caused by other agents or viruses (such as hepatitis B, hepatitis C or hepatitis E). If a person is already infected with the hepatitis A virus at the time of vaccination, HAVRIX may not prevent the disease in these people.
2. What should I know before I am given HAVRIX?
Warnings
You should not be given HAVRIX if:
- you/your child are allergic to HAVRIX, or any of the ingredients listed at the end of this leaflet. Signs of an allergic reaction may include itchy skin rash, shortness of breath and swelling of the face or tongue. Always check the ingredients to make sure you can use this vaccine
- you have/your child has had HAVRIX before and became unwell. Tell your doctor or nurse before the first dose is given
- you have/your child has a severe infection with a high temperature. A minor infection such as a cold should not be a problem, but talk to your doctor or nurse about this before being vaccinated.
Check with your doctor if you/your child:
- has any other medical conditions such as:
- a bleeding disorder, or
- an immune deficiency condition (e.g. are HIV positive) - take any medicines for any other condition
- you have/your child has allergies to any other medicines or substances, such as dyes, foods or preservatives
- has fainted with a previous injection. Fainting can occur following, or even before, any needle injection.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor if you are pregnant or intend to become pregnant.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
Your doctor or nurse can discuss with you the risks and benefits involved.
Children
HAVRIX Junior is recommended for use in children 2 to 15 years of age.
HAVRIX is not recommended in children under 2 years of age, as information on use is limited.
Elderly
Information on use of HAVRIX in the elderly is limited.
3. What if I am taking other medicines?
Tell your doctor, nurse or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with HAVRIX and affect how it works such as:
- steroids, ciclosporin – medicines used to suppress the immune system.
Having other vaccines
Tell your doctor, nurse or pharmacist if you/your child have received another vaccine recently.
Some vaccines may be affected by other vaccines.
HAVRIX can be given at the same time as other vaccines including: hepatitis B, typhoid, yellow fever, cholera (injectable) and tetanus.
It can also be given at the same time as human immunoglobulin. HAVRIX will always be given separately from other injections.
Check with your doctor, nurse or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect HAVRIX.
4. How is HAVRIX given?
The doctor or nurse will give HAVRIX as an injection.
If you have any concerns about how this vaccine is to be given, talk to your doctor, nurse or pharmacist.
How it is given
- For adults and children aged 16 years and over: HAVRIX 1440 is given as a 1 mL injection into the upper arm muscle.
- For adolescents and children aged 2 to 15 years: HAVRIX Junior is given as a 0.5 mL injection into the upper arm muscle in older children and into the thigh muscle in infants.
- For some people with bleeding problems, the dose may need to be given under the skin (subcutaneously).
The vaccine should never be given into a vein (intravenously).
When it is given
- HAVRIX is generally given as a single dose on an elected date.
- If travelling overseas, HAVRIX should be given at least 2 weeks before departure.
- After one dose of HAVRIX, protection from hepatitis A lasts for at least 1 year. A second booster dose, given 6 to 12 months after the first dose, gives longer term protection. It is predicted that protection could last for 20 years. Your doctor will advise on the need for booster dosing.
If there is a risk of hepatitis A infection occurring before immunity develops, human immunoglobulin may need to be given at the same time as HAVRIX.
If a dose is missed
If a scheduled dose is missed, talk to your doctor or nurse and arrange another visit as soon as possible.
If you/your child are given too much HAVRIX
If you think that you/you child has been given too much HAVRIX, you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know when being given HAVRIX?
Things you must do
Keep your visits with the doctor or clinic. It is important that HAVRIX doses are given at the correct times. This will ensure the best effect of the vaccine in protecting you/your child against hepatitis A.
Remind any doctor, nurse or pharmacist you visit that you have/your child has been given HAVRIX.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how HAVRIX affects you.
HAVRIX may cause dizziness or lightheadedness in some people.
Looking after your vaccine
HAVRIX is usually stored at the doctor's clinic or surgery, or at the pharmacy.
If you need to store HAVRIX:
- store in the refrigerator between 2°C and 8°C
- THE PACK SHOULD NEVER BE FROZEN. FREEZING DESTROYS THE VACCINE
- store in the original pack.
Follow the instructions in the carton on how to take care of your vaccine properly.
Keep it where young children cannot reach it.
Getting rid of any unwanted vaccine
If you no longer need to use this vaccine or it is out of date, take it to any pharmacy for safe disposal.
Do not use this vaccine after the expiry date.
6. Are there any side effects?
All vaccines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
Nervous system disorders:
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
| Immune system disorders and allergic reactions: As with all vaccines given by injection there is a very small risk of serious allergic reaction.
Allergy to HAVRIX is rare. Any such severe reactions will usually occur within the first few hours of vaccination. | Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor, nurse or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this vaccine.
Always make sure you speak to your doctor, nurse or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This vaccine is only available with a doctor's prescription.
What HAVRIX contains
| Active ingredient (main ingredient) | Inactivated hepatitis A virus |
| Other ingredients (inactive ingredients) |
|
You should not be given this vaccine if you are allergic to any of these ingredients.
HAVRIX does not contain human blood or blood products, or any other substances of human origin.
The manufacture of this vaccine includes exposure to bovine derived materials. No evidence exists that any case of vCJD (considered to be the human form of bovine spongiform encephalopathy) has resulted from the administration of any vaccine product.
What HAVRIX looks like
HAVRIX is a turbid liquid suspension in a glass pre-filled syringe. Upon storage, a fine white deposit with a clear colourless supernatant may be observed.
HAVRIX 1440 - 1 mL of suspension in a pre-filled syringe (AUST R 147331)
HAVRIX Junior - 0.5 mL of suspension in a pre-filled syringe (AUST R 147335)
Who distributes HAVRIX
GlaxoSmithKline Australia Pty Ltd
Level 4, 436 Johnston Street,
Abbotsford, Victoria, 3067
Phone: 1800 033 109
www.gsk.com.au
Trade marks are owned by or licensed to the GSK group of companies.
©2025 GSK group of companies or its licensor.
This leaflet was prepared on 05 August 2025.
Version 6.0
Brand Information
| Brand name | Havrix 1440 and Havrix Junior |
| Active ingredient | Hepatitis A vaccine |
| Schedule | S4 |
MIMS Revision Date: 01 September 2023
1 Name of Medicine
Inactivated hepatitis A virus vaccine.
2 Qualitative and Quantitative Composition
Havrix, hepatitis A vaccine, is a sterile suspension containing formaldehyde - inactivated hepatitis A virus (HM 175 hepatitis A virus strain) adsorbed onto aluminium hydroxide hydrate.
The virus is propagated in MRC5 human diploid cells. Before viral extraction, the cells are extensively washed to remove culture medium constituents. A virus suspension is then obtained by lysis of the cells followed by purification using ultrafiltration techniques and gel chromatography. The virus is then inactivated with formalin. Residual formaldehyde in the vaccine should be not more than 0.01%.
One dose (1.0 mL) of Havrix 1440 Adult contains: hepatitis A virus (inactivated)1,2 1440 ELISA units.
1Produced on human diploid (MRC-5) cells, 2adsorbed on aluminium hydroxide hydrate.
Total: 0.50 milligrams Al3+.
One dose (0.5 mL) of Havrix 720 Junior contains: hepatitis A virus (inactivated)1,2 720 ELISA units.
1Produced on human diploid (MRC-5) cells, 2adsorbed on aluminium hydroxide hydrate.
Total: 0.25 milligrams Al3+.
The manufacture of this product includes exposure to bovine derived materials. No evidence exists that any case of vCJD (considered to be the human form of bovine spongiform encephalopathy) has resulted from the administration of any vaccine product.
Havrix meets the World Health Organization requirements for biological substances.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Suspension for injection.
Turbid liquid suspension. Upon storage, a fine white deposit with a clear colourless supernatant can be observed.
4 Clinical Particulars
4.1 Therapeutic Indications
Havrix is indicated for active immunisation against hepatitis A virus (HAV) infection in susceptible subjects at risk of exposure to HAV. Havrix Junior is indicated in subjects aged 2 to 15 years and Havrix 1440 is indicated in subjects aged 16 years and older.
In areas of low prevalence of hepatitis A, immunisation with Havrix is particularly recommended in the following subjects.
Travellers: persons travelling to areas of intermediate or high endemicity for hepatitis A. These areas include Africa, Asia, India, the Pacific Islands, the Mediterranean basin, the Middle East, Central and South America.
Armed forces: armed forces personnel who travel to higher endemicity areas or to areas where hygiene is poor, have an increased risk of HAV infection.
Persons for whom hepatitis A is an occupational hazard or for whom there is an increased risk of transmission. These include: employees in daycare centres, particularly in situations where children have not been toilet trained; teachers and other close contacts of the intellectually disabled; staff and residents of residential facilities for the intellectually disabled; health workers and teachers in remote Aboriginal and Torres Strait Islander communities; nursing staff and other healthcare workers in contact with patients in paediatric wards, infectious diseases wards, emergency rooms and intensive care units; sewerage workers; food handlers, since food hygiene procedures and food processing methods are not always adequate to protect from contamination from food handlers.
Homosexual men: increased incidence of hepatitis A infection among homosexual males suggests that the disease may be sexually transmitted in this group.
Contacts of infected persons: since virus shedding from infected persons may occur for a prolonged period, active immunisation of close contacts is recommended. The use of vaccine in outbreak control has been shown to be more effective than the use of immunoglobulin.
Specific population groups known to have a higher incidence of hepatitis A: e.g. Australian Aboriginals, recognised community-wide HAV epidemics.
Individuals with chronic liver disease and recipients of liver transplants, as hepatitis A infections is likely to be more severe in these groups. Many injecting drug users will have pre-existing liver disease from hepatitis B or hepatitis C infection.
Recipients of blood products, such as factor VIII e.g. haemophiliacs.
Havrix will not prevent hepatitis infection caused by other agents such as hepatitis B virus, hepatitis C virus, hepatitis D virus, hepatitis E or other pathogens known to infect the liver.
4.2 Dose and Method of Administration
Havrix is administered by intramuscular injection. The vaccine should never be administered intravenously.
Each dose consists of ready-to-use sterile suspension. The vaccine should be inspected visually for any foreign particulate matter and/or variation of physical aspect prior to administration. Before use of Havrix, the syringe should be well shaken to obtain a slight opaque white suspension. Discard if the contents of the syringe appear otherwise.
Instructions for the pre-filled syringe. Hold the syringe by the barrel, not by the plunger.
Unscrew the syringe cap by twisting it anticlockwise.
To attach the needle, connect the hub to the Luer lock adaptor and rotate a quarter turn clockwise until you feel it lock.
Do not pull the syringe plunger out of the barrel. If it happens, do not administer the vaccine.
The pre-filled syringe is for use in a single patient only. Any unused product or waste material should be disposed of in accordance with local requirements.
Adults (16 years and older). A single dose of Havrix 1440 (1 mL) is used for primary immunisation.
To prolong the protective effect, a single booster dose of Havrix 1440 is recommended at any time between 6 and 12 months after the primary dose. Long-term persistence of serum antibodies after vaccination with Havrix is under evaluation. Data available after five years show persistence of antibodies which is consistent with a projected 20 years persistence (based on mathematical calculations). Further measurement of antibody titres are needed to confirm these mathematical projections.
Children and adolescents (aged 2 years up to and including 15 years). A single dose of Havrix Junior (0.5 mL) is used for primary immunisation.
To prolong the protective effect, a single booster dose of Havrix Junior is recommended at any time between 6 and 12 months after the primary dose. The exact duration of this protection subsequent to the booster dose is unknown.
Havrix should be injected intramuscularly into the deltoid region of the upper arm in adults and older children or the antero-lateral aspect of the thigh in infants. The vaccine should not be administered intramuscularly in the gluteal region or subcutaneously/ intradermally since administration by these routes may result in a less than optimal anti-HAV antibody response.
4.3 Contraindications
Havrix should not be administered to subjects with known hypersensitivity to any component of the vaccine, or to subjects having shown signs of hypersensitivity after previous Havrix administration.
As with other vaccines, the administration of Havrix should be postponed in subjects with severe febrile illness. The presence of a minor infection, however is not a contraindication.
4.4 Special Warnings and Precautions for Use
Havrix should never be administered intravenously.
As with all injectable vaccines, appropriate medical treatment and supervision should always be readily available in case of anaphylactic reactions following the administration of the vaccine.
Syncope (fainting) can occur following, or even before, any vaccination as a psychogenic response to the needle injection. It is important that procedures are in place to avoid injury from faints.
The antibody response to Havrix may be impaired in subjects whose immune system is compromised by either disease or drugs.
Havrix should be administered with caution to subjects with thrombocytopenia or a bleeding disorder since bleeding may occur following an intramuscular administration to these subjects.
It is possible that the subjects may be in the incubation period of hepatitis A infection at the time of immunisation. It is not known whether Havrix will prevent hepatitis A in such cases.
Use in the elderly. Clinical experience with Havrix 1440 in the elderly is also limited.
Paediatric use. See Section 4.4 Special Warnings and Precautions for Use.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
No data are available concerning concomitant administration of ISG with Havrix 1440 or Havrix Junior. Clinical experience with Havrix 720 ELISA suggests that the concomitant administration of ISG with the first dose of Havrix does not influence the seroconversion rate, but may result in a relatively lower anti-HAV antibody titre than when the primary course of vaccine is given alone. Havrix and ISG should be administered at separate injection sites.
Since Havrix is an inactivated vaccine its concomitant use with other inactivated vaccines is unlikely to result in interference with immune response. Havrix can be given concomitantly with any of the following vaccines: typhoid, yellow fever, cholera (injectable), tetanus, or with monovalent and combination vaccines comprised of measles, mumps, rubella and varicella.
Clinical experience of the concomitant administration of Havrix 720 ELISA units and the recombinant hepatitis B virus vaccine (Engerix-B) suggests no interference in the respective immune responses to each of the antigens. When given concomitantly, Havrix and Engerix-B should be administered in separate syringes at separate sites.
If another vaccine needs to be administered concurrently, the vaccines must be administered using separate syringes at separate sites.
Havrix must not be mixed with other vaccines.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. No data available.
Use in pregnancy. (Category B2)
Adequate human data on use during pregnancy and adequate animal reproduction studies are not available. Although there is no convincing evidence of risk to the foetus from immunisation of pregnant women using inactivated virus vaccines, Havrix should be used during pregnancy only when clearly needed.
Use in lactation. Adequate human data on use during lactation and adequate animal reproduction studies are not available. Havrix should therefore be used with caution in breastfeeding women.
4.7 Effects on Ability to Drive and Use Machines
The vaccine is unlikely to produce an effect on the ability to drive and use machines.
4.8 Adverse Effects (Undesirable Effects)
Clinical trials. Solicited and unsolicited events occurring during clinical trials are listed below. The safety profile presented below is based on data from more than 5300 subjects. Events are listed within body systems and categorised by frequency according to the following definitions:
Very common: ≥ 1/10; Common: ≥ 1/100 to < 1/10; Uncommon: ≥ 1/1,000 to < 1/100; Rare: ≥ 1/10,000 to < 1/1,000; Very rare: < 1/10,000.
Local reactions at injection site. Very common: soreness, redness.
Common: induration, swelling.
Body as a whole. Very common: headache, fatigue.
Common: fever (> 37.5°C), malaise.
Uncommon: influenza-like illness.
Rare: chills.
Dermatologic. Uncommon: rash.
Rare: pruritus.
Respiratory. Uncommon: pharyngitis, other upper respiratory tract infections, rhinitis.
Gastrointestinal. Common: nausea, diarrhoea, vomiting, appetite lost.
Uncommon: abdominal pain.
Musculoskeletal. Uncommon: myalgia, musculoskeletal stiffness.
Haematologic. Rare: lymphadenopathy.
Central nervous system. Very common: irritability.
Common: drowsiness.
Uncommon: dizziness.
Rare: hypoaesthesia, paraesthesia.
When ISG was given concurrently with Havrix 720 ELISA units, the incidence but not severity of the adverse events were higher, this being largely due to more reports of local adverse events.
Postmarketing data. Since marketing of the product, elevations of serum liver enzymes (usually transient) have been reported rarely. However a causal relationship with the vaccine has not been established. Neurological manifestations occurring in temporal association have been reported extremely rarely with the vaccine and include transverse myelitis, Guillain-Barre syndrome and neuralgic amyotrophy. No causal relationship has been established.
Very rarely, allergic reactions including anaphylactic reactions, and convulsions have been reported.
Anaphylaxis and mimicking serum sickness, vasculitis, angioneurotic oedema, urticaria, erythema multiforme, arthralgia have also been reported.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
Cases of overdose have been reported during post-marketing surveillance. Adverse events reported following overdosage were similar to those reported with normal vaccine administration.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Havrix confers immunity against hepatitis A virus (HAV) infection by inducing the production of specific anti-HAV antibodies in normal healthy individuals.
The mean titre of anti-HAV antibodies induced by Havrix is higher than that observed after passive immunisation using specific HAV immune serum globulins (ISG). Vaccine-induced anti-HAV antibodies have been shown to be qualitatively indistinguishable from those of the specific HAV ISG.
A booster dose may be administered at any time between 6 and 12 months after the primary dose, to induce a rise in antibody titres. Long-term persistence of serum antibodies has been predicted using mathematical modelling of data obtained after vaccination of adults (17-40 years age) with Havrix 1440.
Data available after 17 years allows prediction that at least 95% and 90% of subjects will remain seropositive (≥ 15 mIU/mL) 30 and 40 years after vaccination, respectively (see Table 1).
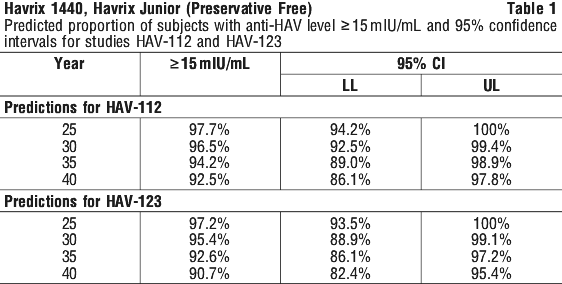
Immunogenicity in children. In clinical studies involving subjects 2 to 19 years of age (N = 314), specific humoral antibodies against HAV were elicited in 93% of vaccinees after 15 days and in approximately 99% of vaccinees 1 month after the administration of a single dose of Havrix Junior. The GMTs 1 month after the initial dose ranged from 194 to 305 IU/L. One month following the booster dose at month 6, all subjects were seropositive with GMTs ranging from 2495 to 3644 IU/L.
In one additional study in which the booster dose was delayed until 1 year following the initial dose, 95.2% of all subjects were seropositive just prior to administration of the booster dose. One month later, all subjects were seropositive with GMTs of 2657 IU/L.
Protective efficacy. Protective efficacy with Havrix has been demonstrated in a double-blind, randomized controlled study in school children (age 1 to 16 years) in Thailand who were at high risk of HAV infection. A total of 40,119 children were randomized to be vaccinated with either Havrix 360 ELISA units or Engerix-B at 0, 1, 12 months. 19,037 children received a primary course (0, 1 months) of Havrix and 19,120 children received a primary course (0, 1 months) of Engerix-B. 38,157 children entered surveillance at day 138 and were observed for an additional 8 months. Using the protocol-defined endpoint (≥ 2 days absence from school, ALT level > 45 IU/mL, and a positive result in the HAVAB-M test), 32 cases of clinical hepatitis A occurred in the control group; in the Havrix group, two cases were identified. These two cases were mild both in terms of biochemical and clinical indices of hepatitis A disease. Thus the calculated efficacy rate for prevention of clinical hepatitis A was 94% (95% confidence intervals 74% to 99%).
In outbreak investigations occurring in the trial, 26 clinical cases of hepatitis A (of a total of 34 occurring in the trial) occurred. No cases occurred in Havrix vaccinees.
Using additional virological and serological analyses post hoc, the efficacy of Havrix was confirmed. Up to three additional cases of very mild clinical illness may have occurred in vaccinees. Using available testing, these illnesses could neither be proven nor disproven to have been caused by HAV. By including these as cases, the calculated efficacy rate for prevention of clinical hepatitis A would be 84% (95% confidence intervals 60% to 94%).
The benefit of post-exposure vaccination has been studied in an animal model. Primates exposed to the virulent heterologous hepatitis A strain were vaccinated with either a single dose of 360 or 1440 ELISA unit vaccine 2 days after exposure. Only partial protection was observed in the animals vaccinated with the lower dose, with three of four animals developing hepatitis A. Post-exposure vaccination with 1440 ELISA units provided complete protection against disease and HAV transmission, although 2 of the four animals had evidence of infection.
Impact of mass vaccination on disease incidence. A reduction in the incidence of hepatitis A was observed in two countries where a two-dose Havrix immunization program was implemented for children in their second year of life. The two countries had intermediate A hepatitis virus endemicity before the program:
In Israel, two retrospective database studies showed 88% and 95% reduction in hepatitis A incidence in the general population 5 and 8 years after the implementation of the vaccination program, respectively. Data from national surveillance also showed a 95% reduction in hepatitis A incidence as compared to the pre-vaccination period.
In Panama, a retrospective database study showed a 90% reduction in reported hepatitis A incidence in the vaccinated population, and 87% in the general population, 3 years after implementation of the vaccination programme. In paediatric hospitals in Panama City, confirmed acute hepatitis A cases were no longer diagnosed 4 years after implementation of the vaccination programme.
The observed reductions in hepatitis A incidence in the general population (vaccinated and non-vaccinated) in both countries demonstrate herd immunity.
5.2 Pharmacokinetic Properties
Not relevant to vaccines.
5.3 Preclinical Safety Data
Genotoxicity. No data available.
Carcinogenicity. No data available.
6 Pharmaceutical Particulars
6.1 List of Excipients
The vaccine preparation contains aluminium hydroxide hydrate, aluminium (Havrix Junior only), neomycin sulphate (trace amounts), polysorbate 20 and amino acid supplement in a phosphate buffered saline solution, dibasic sodium phosphate heptahydrate, monobasic potassium phosphate, sodium chloride, potassium chloride and water for injections.
6.2 Incompatibilities
See Section 4.5 Interactions with Other Medicines and Other Forms of Interactions.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Havrix must be stored at +2°C to +8°C. Do not freeze, discard if vaccine has been frozen.
The shelf life of Havrix is three years from the date of manufacture at temperatures of +2°C to +8°C.
Stability. Stability data indicate that Havrix is stable at temperatures up to 25°C for 3 days. These data are intended to guide healthcare professionals in case of temporary exposure to such temperatures, and are not recommendations for storage.
6.5 Nature and Contents of Container
Havrix 1440. 1 mL of suspension in a pre-filled syringe (type I glass) with a plunger stopper (butyl rubber) and with a rubber tip cap.
Havrix Junior. 0.5 mL of suspension in a pre-filled syringe (type I glass) with a plunger stopper (butyl rubber) and with a rubber tip cap.
The tip cap and rubber plunger stopper of the pre-filled syringe are not made with natural rubber latex.
Not all presentations and pack sizes may be marketed in Australia.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Not relevant to vaccines.
7 Medicine Schedule (Poisons Standard)
Schedule 4 - Prescription Only Medicine.
Date of First Approval
22 December 2009
Date of Revision
19 July 2023
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.