Imuran Tablets
Brand Information
| Brand name | Imuran Tablets |
| Active ingredient | Azathioprine |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Imuran Tablets.
Summary CMI
IMURAN tablets
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using IMURAN?
IMURAN contains the active ingredient azathioprine. It is used to help prevent the rejection of transplanted organs, or to treat other diseases called autoimmune diseases where your immune system is reacting against your own body.
For more information, see Section 1. Why am I using IMURAN? in the full CMI.
2. What should I know before I take IMURAN?
Do not use if you have ever had an allergic reaction to azathioprine, 6-mercaptopurine or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I take IMURAN? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with IMURAN and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use IMURAN?
- The dose of IMURAN varies from patient to patient. Your doctor will tell you how much to take.
- Take IMURAN tablets at least 1 hour before or 3 hours after food or milk.
More instructions can be found in Section 4. How do I use IMURAN? in the full CMI.
5. What should I know while taking IMURAN?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while taking IMURAN? in the full CMI.
6. Are there any side effects?
Tell your doctor immediately if you experience any side effects while taking IMURAN. Side effects may include any infection or fever; unexpected bruising or bleeding, black tarry stools or blood in urine or stools; new marks on skin or any change to marks that may have been there previously; headache, stiff neck and extreme sensitivity to bright light; nausea and vomiting; tiredness, dizziness or generally unwell; irregular heartbeat; sores in the mouth and on the lips; feeling of ants creeping in or under the skin; changes in sense of smell or taste; or reactivation of hepatitis B. More serious side effects of IMURAN include an allergic-type reaction; muscle weakness, with or without a skin rash; muscle pain or stiffness; severe joint pain; kidney problems; feeling faint especially when standing up; severe abdominal pain; diarrhoea; yellowing of the skin/eyes; and serious skin reactions such as blistering or peeling.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
IMURAN tablets
Active ingredient: azathioprine
Consumer Medicine Information (CMI)
This leaflet provides important information about using IMURAN tablets.
You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using IMURAN.
Where to find information in this leaflet:
1. Why am I using IMURAN?
2. What should I know before I take IMURAN?
3. What if I am taking other medicines?
4. How do I use IMURAN?
5. What should I know while taking IMURAN?
6. Are there any side effects?
7. Product details
1. Why am I using IMURAN?
IMURAN contains the active ingredient azathioprine. It belongs to a group of medicines called immunosuppressants.
IMURAN is used to help prevent the rejection of a transplanted organ such as a kidney, liver or heart. It works by suppressing the body's immune defence system.
IMURAN can also be used to treat other diseases called autoimmune diseases where your immune system is reacting against your own body. These may include:
- severe rheumatoid arthritis
- systemic lupus erythematosus
- chronic active hepatitis
- certain skin, muscle, and blood diseases.
IMURAN is usually taken in combination with other medicines such as corticosteroids or other immunosuppressive drugs.
Ask your doctor if you have any questions about why IMURAN has been prescribed for you.
Your doctor may have prescribed it for another purpose.
There is no evidence that it is addictive.
2. What should I know before I take IMURAN?
Warnings
Do not take IMURAN if:
- you are allergic to azathioprine, 6-mercaptopurine (Puri-Nethol, a medicine which is similar to IMURAN) or any of the ingredients listed at the end of this leaflet.
- Symptoms of an allergic reaction may include shortness of breath, wheezing or difficulty in breathing; swelling of the face, lips, tongue, or any other parts of the body; rash, itching or hives on the skin. - you have any of the following:
- rheumatoid arthritis that has been previously treated with some other medicines, such as chlorambucil, melphalan or cyclophosphamide. - the expiry date printed on the pack has passed.
- the packaging is torn or shows signs of tampering.
Check with your doctor if you:
- have or have had any other medical conditions, especially the following:
- liver or kidney disease
- a condition where your body produces too little of a natural chemical called thiopurine methyltransferase (TPMT)
- Lesch-Nyhan syndrome
- chickenpox or shingles
- hepatitis B. - have recently been vaccinated or immunized or plan to do so.
- IMURAN may affect the way the vaccine works or your reaction to the vaccine. - take any medicines for any other condition.
- have had any allergy to any other medicines, or any other substances, such as foods, preservatives, or dyes.
- have any upcoming dental procedures.
- Dental work, whenever possible, should be completed before you start taking IMURAN or delayed until your blood cell counts are normal.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Do not take IMURAN if you are pregnant, may be pregnant, plan to become pregnant or intending to father a child.
IMURAN may cause birth defects if either the male or female is taking it at the time of conception. You or your partner should take adequate contraceptive precautions while you are taking IMURAN.
Do not take IMURAN if you are breastfeeding unless you and your doctor have discussed the risks and benefits involved.
It is not recommended for use while breastfeeding as it may cause serious side effects to your baby.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with IMURAN and affect how it works. These include:
- penicillamine, used mainly in the treatment of rheumatoid arthritis
- captopril, used mainly to treat high blood pressure and heart failure
- cimetidine, used to treat stomach ulcers and indigestion
- indomethacin, used as a painkiller and anti-inflammatory
- co-trimoxazole, used to treat infections
- allopurinol, oxipurinol or thiopurinol, used mainly to treat gout
- tubocurarine, succinylcholine, used during anaesthesia
- frusemide, may be used to reduce swelling caused by excess fluid
- warfarin, used to prevent blood clots
- mesalazine, olsalazine or sulfasalazine, used mainly to treat ulcerative colitis
- phenytoin, phenobarbital, rifampicin, ketoconazole, erythromycin
- methotrexate, used in the treatment of cancer.
- ribavirin, used to treat a type of respiratory infection.
These medicines may be affected by IMURAN or may affect how well it works. You may need to take different amounts of your medicine, or you may need to take different medicines.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect IMURAN.
4. How do I use IMURAN?
How much to take
Your doctor will tell you how much IMURAN to take.
The dose will depend on the condition being treated, your bodyweight and how you respond to the medicine. Your initial dose will be maintained or adjusted until a satisfactory response is noted.
From time to time, while you are taking IMURAN, your doctor will want you to have a blood test. This is to check your blood cell count and to change your dose if necessary.
When to take it
Take IMURAN tablets at least 1 hour before or 3 hours after food or milk.
How to take it
Swallow IMURAN tablets whole with a glass of water.
Do not break, chew or crush the tablets.
How long to take it
Patients with a transplant will need to take IMURAN tablets continuously to reduce the risk of organ rejection.
For other conditions, your doctor will discuss with you how long you need to take this medicine. It could take some weeks or months for it to take full effect.
If you forget to use it
If it is almost time for your next dose, skip the dose you missed and take your next dose when you are meant to. Otherwise, take it as soon as you remember, then go back to taking it as you would normally.
Do not take a double dose to make up for the dose that you missed.
If you take too much IMURAN
If you think that you have taken too many IMURAN tablets, you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know while taking IMURAN?
Things you should do
- Take IMURAN exactly as your doctor has prescribed.
- Visit your doctor regularly, so they can make sure that IMURAN is working properly and to check for any unwanted side-effects.
Your doctor may order regular blood tests while you are taking this medicine to check how it affects you. The frequency of your blood tests will usually decrease the longer you continue to take IMURAN. - Tell any other doctor, dentist or pharmacist who is treating you that you are taking IMURAN, especially if you are about to be started on any new medicines.
- Tell your doctor if you have recently been vaccinated or immunized or plan to do so.
IMURAN may affect the way some vaccines work or your reaction to the vaccine. - Tell your doctor if you become pregnant, are trying to become pregnant or planning to father a child.
- If you must have an operation, tell your surgeon and anaesthetist that you are taking IMURAN.
- Tell your doctor immediately if you notice new moles, changes in existing moles, any lumps on your body or you feel unwell.
Immunosuppressant drugs, like IMURAN, lower the body's immune defence system. There may be an increased risk of developing infections or tumours, including skin cancer, whilst taking this medicine.
Protect yourself from the sun while you are taking IMURAN.
If you go out in the sun, wear a hat, protective clothing and use sunscreen. - Avoid contact with anyone suffering from chickenpox or shingles.
Infection with chickenpox or shingles can become severe in patients taking drugs such as IMURAN.
Things you should not do
- Do not stop taking IMURAN or change the dose without first checking with your doctor.
- Do not take this medicine to treat any other complaints unless your doctor has instructed you to do so.
- Do not give this medicine to anyone else, even if their symptoms seem like yours.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how IMURAN affects you.
Looking after your medicine
Keep IMURAN tablets in the pack until it is time to take them.
Store it in a cool dry place, away from moisture, heat, or light where the temperature stays below 30°C.
For example, do not store it:
- in the bathroom or near a sink, or
- in the car or on window sills.
Keep it where young children cannot reach it.
Getting rid of any unwanted medicine
If you no longer need to use this medicine or it is out of date, take it to any pharmacy for safe disposal.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
| Tell your doctor immediately if you notice any of these side effects |
Serious side effects
| Serious side effects | What to do |
Reported particularly in organ transplant patients:
| Call your doctor or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
IMURAN could cause your hepatitis B to become active again.
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What IMURAN contains
IMURAN tablets are available in two strengths: 25 mg or 50 mg.
| Active ingredient (main ingredient) |
|
| Other ingredients (inactive ingredients) |
In addition, the 25 mg tablets contain:
|
| Potential allergens |
|
Do not take this medicine if you are allergic to any of these ingredients.
What IMURAN looks like
- IMURAN 25 mg are an orange, film-coated, round, biconvex, unscored and branded “IM 2” tablet. Available in blister packs of 100 tablets.
- IMURAN 50 mg are a yellow, film-coated, round, biconvex, scored and branded “IM 5” tablet. Available in blister packs of 100 tablets.
Australian Registration Numbers:
25 mg tablet: AUST R 31393
50 mg tablet: AUST R 31398
Who distributes IMURAN
Aspen Pharmacare Australia Pty Ltd
34-36 Chandos St
St Leonards NSW 2065
Australia
This leaflet was revised in August 2025.
Brand Information
| Brand name | Imuran Tablets |
| Active ingredient | Azathioprine |
| Schedule | S4 |
MIMS Revision Date: 01 March 2025
1 Name of Medicine
Imuran tablets contain azathioprine.
2 Qualitative and Quantitative Composition
Imuran is available in film-coated tablets.
Imuran film-coated tablets contain either 25 mg or 50 mg of the active azathioprine.
Excipients with known effect. Sugars as lactose.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
25 mg. Orange, round, biconvex film-coated tablets, unscored and branded IM 2.
50 mg tablet. Yellow tablet, film-coated, round, biconvex, scored and branded IM 5.
4 Clinical Particulars
4.1 Therapeutic Indications
Imuran is used as an immunosuppressant antimetabolite either alone, or more commonly, in combination with other agents (usually corticosteroids) and procedures which influence the immune response. Therapeutic effect may be evident only after weeks or months and can include a steroid-sparing effect, thereby reducing the toxicity associated with high dosage and prolonged usage of corticosteroids.
Imuran, in combination with corticosteroids and/or other immunosuppressive agents and procedures, is indicated in the management of patients receiving organ transplants.
Imuran, either alone or more usually in combination with corticosteroids and/or other procedures, has been used with clinical benefit (which may include reduction of dosage or discontinuation of corticosteroids) in a proportion of patients suffering from the following: severe rheumatoid arthritis; systemic lupus erythematosus; dermatomyositis/polymyositis; autoimmune chronic active hepatitis; pemphigus vulgaris; polyarteritis nodosa; autoimmune haemolytic anaemia; chronic refractory idiopathic thrombocytopenic purpura.
4.2 Dose and Method of Administration
Tablets. Imuran tablets should be administered at least 1 hour before or 3 hours after food or milk.
Tablets. Specialist medical literature should be consulted for guidance as to clinical experience in particular conditions.
Dosage in transplantation - adults and children. Depending on the immunosuppressive regimen adopted, a loading dose of up to 5 mg/kg bodyweight/day is usually given.
Maintenance dosage may range from 1 to 4 mg/kg bodyweight/day orally and must be adjusted according to clinical requirements and haematological tolerance.
Evidence indicates that Imuran therapy should be maintained indefinitely, even if only low doses are necessary, because of risk of graft rejection.
Dosage in other conditions - adults and children. In general, the initial dose should be approximately 1.0 mg/kg/day (50 to 100 mg) gradually increasing in increments of 0.5 mg/kg/day over several weeks, if necessary up to a maximum dose of 2.5 mg/kg/day.
When therapeutic response is evident, consideration should be given to reducing the maintenance dosage to the lowest level compatible with maintenance of that response. If no improvement occurs in the patient's condition within three months, consideration should be given to withdrawing Imuran.
The maintenance dosage required may range from less than 1 mg/kg bodyweight/day to 3 mg/kg bodyweight/day, depending on the clinical condition being treated and the individual patient response, including haematological tolerance.
Use in the elderly (see Section 4.8, Haematopoiesis). The rapid in vivo cleavage of the azathioprine molecule followed by tissue fixation makes it impossible to relate plasma drug levels to toxicity. There are no specific data as to the tolerance of Imuran in elderly patients. It is recommended that the dosages used are at the lower end of the range given for adults and children.
Particular care should be taken to monitor haematological response and to reduce the maintenance dosage to the minimum required for clinical response.
Renal/hepatic impairment. See Section 4.4 Special Warnings and Precautions for Use.
4.3 Contraindications
Imuran is contraindicated in patients known to be hypersensitive to azathioprine or any other component of the preparation. Hypersensitivity to 6-mercaptopurine (6-MP) should alert the prescriber to probable hypersensitivity to Imuran.
Patients with rheumatoid arthritis previously treated with alkylating agents (cyclophosphamide, chlorambucil, melphalan or others) may have a prohibitive risk of neoplasia if treated with Imuran.
Imuran therapy should not be initiated in patients who may be pregnant, who are likely to become pregnant in the near future, or who are known to be pregnant (see Section 4.4 Special Warnings and Precautions for Use).
4.4 Special Warnings and Precautions for Use
Co-administration of ribavirin and azathioprine is not advised. Ribavirin may reduce efficacy and increase toxicity of azathioprine.
Cytomegalovirus (CMV) disease (see Section 4.8 Adverse Effects (Undesirable Effects)). Cytomegalovirus (CMV) viraemia resulting in severe pneumonitis and associated haemophagocytic syndrome manifesting in patients with inflammatory bowel disease has been reported in the literature.
Caution should be exercised and specialist literature consulted when determining the risks of CMV reactivation and lBD deterioration.
Monitoring. There are potential hazards to the use of Imuran. It should be prescribed only if the patient can be adequately monitored for toxic effects throughout the duration of therapy.
Azathioprine is hepatotoxic and liver function tests should be routinely monitored during treatment (see Section 4.8 Adverse Effects (Undesirable Effects)). More frequent monitoring may be advisable in those with pre-existing liver disease or receiving other potentially hepatotoxic therapy. The patient should be instructed to discontinue azathioprine immediately if jaundice becomes apparent.
Particular care should be taken to monitor haematological response and to reduce the maintenance dosage to the minimum required for clinical response.
During the first eight weeks of therapy, complete blood counts, including platelets, must be performed weekly or more frequently if high dosage is used or if severe renal and/or hepatic disorder is present. The blood count frequency may be reduced later in therapy, but it is recommended that complete blood counts are repeated at intervals of not longer than one month or more frequently if dosage alterations or other changes to therapy are made. Delayed haematological suppression may occur.
Prompt reduction in dosage or temporary withdrawal of the drug may be necessary if there is a rapid fall in, or persistently low, leucocyte count or other evidence of bone marrow depression.
Patients receiving Imuran should be instructed to report immediately if there is any evidence of infection, unexpected bruising or bleeding, black tarry stools and blood in the urine or stools, or other manifestations of bone-marrow depression. Bone marrow suppression is reversible if azathioprine is withdrawn early enough.
TPMT testing. There are individuals with an inherited deficiency of the enzyme thiopurine methyltransferase (TPMT) who may be unusually sensitive to the myelosuppressive effect of azathioprine and prone to developing rapid bone marrow depression following the initiation of treatment with Imuran. There have been fatal cases of myelosuppression in patients with low or absent TPMT activity treated with thiopurines. This problem could be exacerbated by coadministration with drugs that inhibit TPMT, such as olsalazine, mesalazine or sulfasalazine. Also, a possible association between decreased TPMT activity and secondary leukaemias and myelodysplasia has been reported in individuals receiving 6-mercaptopurine (the active metabolite of azathioprine) in combination with other cytotoxics (see Section 4.8 Adverse Effects (Undesirable Effects)).
Patients should be tested for TPMT activity before starting Imuran. TPMT testing cannot substitute for complete blood count monitoring in patients receiving Imuran. TPMT genotyping can be used to identify patients with absent or reduced TPMT activity. Patients with low or absent TPMT activity (homozygous for non-functional alleles) are at an increased risk of developing severe, life-threatening myelotoxicity from Imuran if conventional doses are given. Alternative therapies may be considered for patients who have low or absent TPMT activity. Imuran should be administered with caution to patients having one non-functional allele (heterozygous) who are at risk for reduced TPMT activity that may lead to toxicity if conventional doses are given. Dosage reduction is recommended in patients with reduced TPMT activity. The dosage of azathioprine may need to be reduced when this agent is combined with other drugs whose primary or secondary toxicity is myelosuppression.
TPMT testing is widely available through pathology laboratories and genetic testing services.
NUDT15 testing. Patients with inherited mutated NUDT15 gene are at increased risk for severe thiopurine toxicity, such as early leukopenia and alopecia, from conventional doses of thiopurine therapy and generally require substantial dose reduction. The precise mechanism of NUDT 15-associated thiopurine-related toxicity is not understood. Patients of Asian ethnicity are particularly at risk, due to the increased frequency of the mutation in this population. The optimal starting dose for heterozygous or homozygous deficient patients has not been established. Close monitoring of blood count is necessary.
Genotypic and phenotypic testing of NUDT15 variants should be considered before initiating thiopurine therapy in all patients (including paediatric patients) to reduce the risk of thiopurine-related severe leukocytopenia and alopecia, especially in Asian populations.
Renal and/or hepatic impairment. It is impossible to relate plasma levels of azathioprine or 6-mercaptopurine to therapeutic efficacy or toxicity. Conversion of 6-thioinosinic acid to 6-thiouric acid by xanthine oxidase is not dependent on intact hepatic and/or renal function. Nevertheless, it is recommended that the dosages used are at the lower end of the normal range and that haematological response is carefully monitored. Dosage should be further reduced if haematological toxicity occurs.
Caution is necessary during the administration of Imuran to patients with hepatic dysfunction, and regular complete blood counts and liver function tests should be undertaken. In such patients the metabolism of Imuran may be impaired, and the dosage of Imuran further reduced if hepatic or haematological toxicity occurs.
Lesch-Nyhan syndrome. Limited evidence suggests that Imuran is not beneficial to patients with hypoxanthine-guanine-phosphoribosyltransferase deficiency (Lesch-Nyhan syndrome). Therefore, given the abnormal metabolism in these patients, it is not prudent to recommend that these patients should receive Imuran.
Carcinogenicity. Patients receiving immunosuppressive therapy, including azathioprine, are at an increased risk of developing lymphoproliferative disorders and other malignancies, notably skin cancers (melanoma and non-melanoma), sarcomas (Kaposi's and non-Kaposi's) and uterine cervical cancer in situ. The increased risk appears to be related to the degree and duration of immunosuppression. It has been reported that discontinuation of immunosuppression may provide partial regression of the lymphoproliferative disorder. A treatment regimen containing multiple immunosuppressants (including thiopurines) should therefore be used with caution as this could lead to lymphoproliferative disorders, some with reported fatalities. A combination of multiple immunosuppressants, given concomitantly increases the risk of Epstein-Barr virus (EBV)-associated lymphoproliferative disorders.
Varicella zoster virus infection (see Section 4.8 Adverse Effects (Undesirable Effects)). Immunisation using a live organism vaccine has the potential to cause infection in immunocompromised hosts. Therefore, immunisations with live organism vaccines are not recommended.
Infection with varicella zoster virus (VZV; chickenpox and herpes zoster) may become severe during the administration of immunosuppressants. Caution should be exercised especially with respect to the following:
Before starting the administration of immunosuppressants, the prescriber should check to see if the patient has a history of VZV. Serologic testing may be useful in determining previous exposure. Patients who have no history of exposure should avoid contact with individuals with chickenpox or herpes zoster. If the patient is exposed to VZV, special care must be taken to avoid patients developing chickenpox or herpes zoster, and passive immunisation with varicella-zoster immunoglobulin (VZIG) may be considered.
If the patient is infected with VZV, appropriate measures should be taken, which may include antiviral therapy and supportive care.
Progressive multifocal leukoencephalopathy (PML). PML, an opportunistic infection caused by the JC virus (a type of human polyomavirus) has been reported in patients receiving azathioprine with other immunosuppressive agents. Immunosuppressive therapy should be withheld at the first sign or symptoms suggestive of PML and appropriate evaluation undertaken to establish a diagnosis (see Section 4.8 Adverse Effects (Undesirable Effects)).
Hepatitis B (see Section 4.8 Adverse Effects (Undesirable Effects)). Hepatitis B carriers (defined as patients positive for hepatitis B surface antigen [HBsAg] for more than six months), or patients with documented past HBV infection, who receive immunosuppressive drugs are at risk of reactivation of HBV replication, with asymptomatic increases in serum HBV DNA and ALT levels. Specialist medical literature should be consulted for guidance including prophylactic therapy with oral anti-HBV agents.
Macrophage activation syndrome. Macrophage activation syndrome (MAS) is a known, life-threatening disorder that may develop in patients with autoimmune conditions, in particular with inflammatory bowel disease (IBD) and there could potentially be an increased susceptibility for developing the condition with the use of azathioprine. If MAS occurs, or is suspected, evaluation and treatment should be started as early as possible, and treatment with azathioprine should be discontinued. Physicians should be attentive to symptoms of infection such as EBV and cytomegalovirus (CMV), as these are known triggers for MAS.
Metabolism and nutrition disorders. Administration of purine analogues (azathioprine, mercaptopurine and thioguanine) may interfere with the niacin pathway, potentially leading to nicotinic acid deficiency/pellagra. A few cases have been reported with the use of azathioprine, especially in patients with IBD (Crohn's disease, colitis ulcerative); therefore, health care professionals should be aware of this condition and provide appropriate medical care if pellagra occurs (such as niacin/nicotinamide supplementation).
Other precautions. Imuran should be used with caution in hypersplenism.
Withdrawal of Imuran should be gradual and performed under close supervision.
Dental work, whenever possible, should be completed prior to initiation of Imuran therapy or deferred until blood counts are normal.
Hypersensitivity. Patients suspected to have previously presented a hypersensitivity reaction to 6-mercaptopurine should not be recommended to use its pro-drug azathioprine, and vice-versa, unless the patient has been confirmed as hypersensitive to the culprit drug with allergological tests, and tested negative for the other.
Use in the elderly. See Section 4.2 Dose and Method of Administration.
Paediatric use. See Section 4.2 Dose and Method of Administration.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Allopurinol/oxipurinol/thiopurinol and other xanthine oxidase inhibitors. Xanthine oxidase activity is inhibited by allopurinol, oxipurinol and thiopurinol which results in reduced conversion of biologically active 6-thioinosinic acid to biologically inactive 6-thiouric acid. When allopurinol, oxipurinol and/or thiopurinol are given concomitantly with 6-mercaptopurine (6-MP) or azathioprine, the dose of 6-MP and azathioprine should be reduced to one quarter of the original dose. For example, an azathioprine dose of 100 mg should be reduced to 25 mg when used concomitantly with allopurinol.
Other xanthine oxidase inhibitors, such as febuxostat my decrease the metabolism of azathioprine. Concomitant administration is not recommended as data are insufficient to determine an adequate dose reduction.
Neuromuscular blocking agents. Imuran can potentiate the neuromuscular blockade produced by depolarising agents such as succinylcholine and reduce the blockade produced by non-depolarising agents such as tubocurarine.
Anticoagulants. Inhibition of the anticoagulant effect of warfarin and acenocoumarol has been reported when co-administered with azathioprine. Therefore, higher doses of the anticoagulant may be needed. It is recommended that coagulation tests are closely monitored when anticoagulants are concurrently administered with azathioprine.
Cytostatic/myelosuppressive agents. Imuran should be used with caution in patients receiving, or who have recently received, other bone marrow suppressive agents.
Where possible, concomitant administration of cytostatic drugs, or drugs which may have a myelosuppressive effect, such as penicillamine, should be avoided. There are conflicting clinical reports of interactions, resulting in serious haematological abnormalities, between Imuran and co-trimoxazole.
There have been case reports suggesting that haematological abnormalities may develop due to the concomitant administration of azathioprine and ACE inhibitors.
It has been suggested that cimetidine and indomethacin may have myelosuppressive effects which may be enhanced by concomitant administration of Imuran.
Aminosalicylates. As there is in vitro and in vivo evidence that aminosalicylate derivatives (e.g. olsalazine, mesalazine or sulfasalazine) inhibit the TPMT enzyme, they should be administered with caution to patients receiving concurrent Imuran therapy (see Section 4.4 Special Warnings and Precautions for Use).
Methotrexate. When azathioprine is administered concomitantly with high dose methotrexate, the dose should be adjusted to maintain a suitable white blood cell count.
Vaccines. The immunosuppressive activity of Imuran could result in an atypical and potentially deleterious response to live vaccines and so the administration of live vaccines to patients receiving Imuran therapy is contraindicated on theoretical grounds.
A diminished response to killed vaccines is likely and such a response to hepatitis B vaccine has been observed among patients treated with a combination of azathioprine and corticosteroids.
A small clinical study has indicated that standard therapeutic doses of azathioprine do not deleteriously affect the response to polyvalent pneumococcal vaccine, as assessed on the basis of mean anti-capsular specific antibody concentration.
Ribavirin. Ribavirin inhibits the enzyme, inosine monophosphate dehydrogenase (IMPDH), leading to a lower production of the active 6-thioguanine nucleotides. Severe myelosuppression has been reported following concomitant administration of azathioprine and ribavirin; therefore co-administration is not advised.
Infliximab. An interaction has been observed between azathioprine and infliximab. Patients receiving ongoing azathioprine experienced increase in 6-TGN (6-thioguanine nucleotide, an active metabolite of azathioprine) levels and a decrease in the mean leukocyte count following infliximab infusion.
Miscellaneous. Frusemide has been shown to impair the metabolism of azathioprine by human hepatic tissue in vitro. The clinical significance is unknown.
Drugs known to induce (phenytoin, phenobarbital, rifampicin) or inhibit (ketoconazole, erythromycin) hepatic microsomal enzymes may alter the clearance of Imuran.
Coadministration of Imuran and captopril may result in increased susceptibility to leucopenia.
4.6 Fertility, Pregnancy and Lactation
Use in pregnancy. (Category D)
The decision to maintain or discontinue Imuran during pregnancy, or to terminate the pregnancy, depends on the condition under treatment in which the maternal wellbeing has to be weighed against possible risks to the foetus. As a general rule, Imuran therapy should not be initiated in patients known to be pregnant.
Cholestasis of pregnancy has occasionally been reported in association with azathioprine therapy. If cholestasis of pregnancy occurs, case by case assessment is necessary considering the risk-benefit profile of the drug.
As with all cytotoxic chemotherapy, adequate contraceptive precautions should be advised when either partner is receiving Imuran.
There have been reports of premature birth and low birth weight following maternal exposure to azathioprine, particularly in combination with corticosteroids. There have also been reports of spontaneous abortion following either maternal or paternal exposure.
Imuran and/or its metabolites have been found in low concentrations in foetal blood and amniotic fluid.
The rare possibility of neonatal leucopenia and/or thrombocytopenia which may not be clinically evident appears to be preventable by reducing maternal dosage of Imuran if, at 32 weeks' gestation, the maternal leucocyte count is at or below 8.6 x 109 per litre. The possibility of neonatal immunosuppression is a serious and potentially fatal complication. Extra care in haematological monitoring is advised during pregnancy.
Teratogenicity. Studies in pregnant rats, mice and rabbits using azathioprine in dosages from 5-15 mg/kg bodyweight/day over the period of organogenesis have shown varying degrees of foetal abnormalities. Teratogenicity was evident in rabbits at 10 mg/kg bodyweight/day.
Epidemiological evidence in man indicates that the frequency of occurrence of congenital abnormalities in the offspring of maternal transplant recipients is similar to that in the general population.
As with all cytotoxic chemotherapy, adequate contraceptive precautions should be advised when either partner is receiving Imuran.
Use in lactation. 6-Mercaptopurine has been identified in the colostrum and breast-milk of women receiving azathioprine treatment. Nursing mothers should be advised to consult their physician, since use by nursing mothers is not recommended because of possible adverse effects on the infant.
Effects on fertility. Relief of chronic progressive renal failure by renal transplantation involving the use of Imuran has been accompanied by increased fertility in both male and female transplant recipients.
4.7 Effects on Ability to Drive and Use Machines
No specific studies have been conducted to assess the direct effect of Imuran on the ability to drive and use machines. However, adverse effects of Imuran include dizziness which could affect the ability to drive or use machines. See Section 4.8 Adverse Effects (Undesirable Effects).
4.8 Adverse Effects (Undesirable Effects)
Hypersensitivity reactions. Several different clinical syndromes, which appear to be of an idiosyncratic hypersensitivity nature, have been described occasionally. They include general malaise, headache, dizziness, nausea, vomiting, diarrhoea, fever, rigors, exanthema, rash, vasculitis, myalgia, muscular pains, arthralgia, hypotension, disturbed liver function, cholestatic jaundice, pancreatitis, cardiac dysrhythmia, and renal dysfunction. In many cases, rechallenge has confirmed an association with Imuran.
Additional adverse reactions of low frequency have been reported. These include skin rashes (approximately 2%), steatorrhoea, negative nitrogen balance, Stevens-Johnson syndrome and toxic epidermal necrolysis (all less than 1%).
It has been suggested that the imidazole side chain gives rise to hypersensitivity, whereas the 6-mercaptopurine (6-MP) molecule gives rise to cholestasis. Immediate withdrawal of azathioprine and supportive circulatory measures has led to recovery in the majority of cases. Other marked underlying pathology has contributed to the very rare deaths reported.
Imuran should be permanently withdrawn after any such clinical syndrome.
Neoplasms benign, malignant and unspecified (including cysts and polyps). The risk of developing lymphomas and other malignancies, notably skin cancers is increased in patients who receive immunosuppressive drugs, particularly in transplant recipients receiving aggressive treatment and such therapy should be maintained at the lowest effective levels. The increased risk of developing lymphomas in immunosuppressed rheumatoid arthritis patients compared with the general population appears to be related at least in part to the disease itself.
There have been rare reports of acute myeloid leukaemia and myelodysplasia (some in association with chromosomal abnormalities).
Rare: neoplasms including lymphoproliferative disorders, skin cancers (melanomas and non-melanomas), sarcomas (Kaposi's and non-Kaposi's) and uterine cervical cancer in situ (see Section 4.4 Special Warnings and Precautions for Use).
Haematopoiesis. Imuran may be associated with a dose-related, generally reversible, depression of bone marrow function, most frequently expressed as leucopenia, but also sometimes as anaemia and thrombocytopenia and rarely as agranulocytosis, pancytopenia and aplastic anaemia. These occur particularly in patients predisposed to myelotoxicity, such as those with TPMT deficiency and renal or hepatic insufficiency and in patients failing to reduce the dose of Imuran when receiving concurrent allopurinol therapy.
Therapeutic use of Imuran is associated with a reversible, dose-related reduction in numbers of circulating total white cells, granulocytes and lymphocytes together with increases in mean corpuscular volume and red cell haemoglobin content. Megaloblastic bone marrow changes have been observed, but severe megaloblastic anaemia and erythroid hypoplasia are rare.
Imuran may produce thrombocytopenia which is dose-related and may be delayed.
Alopecia. Hair loss has been described in 50% of renal transplant recipients receiving Imuran and corticosteroids, but does not appear to be a major problem when Imuran is used for other indications. It is reversible in over 80% of cases despite continuing immunosuppression.
Susceptibility to infection. Patients receiving Imuran alone or in combination with other immunosuppressants, particularly corticosteroids, have shown increased susceptibility to viral, fungal and bacterial infections, including severe or atypical infection and reactivation with VZV, hepatitis B, Cytomegalovirus (CMV) and other infectious agents. Viral, fungal and bacterial infections are very common in transplant patients receiving azathioprine in combination with other immunosuppressants.
Very rare cases of JC virus associated PML have been reported following the use of azathioprine in combination with other immunosuppressants (see Section 4.4 Special Warnings and Precautions for Use).
Gastrointestinal reactions. Nausea, vomiting and gastrointestinal discomfort may occur during the first few months of Imuran therapy. These effects are usually reduced by dosage adjustment and by administering the tablets in divided doses and/or after meals.
Serious complications, including colitis, diverticulitis and bowel perforation, have been described in transplant recipients and appear to relate to high dosage of corticosteroids rather than to Imuran per se.
Severe diarrhoea, recurring on rechallenge, has been reported in patients treated with Imuran for inflammatory bowel disease. The possibility that exacerbation of symptoms might be drug-related should be borne in mind when treating such patients.
Pancreatitis has been reported in a small percentage of patients on Imuran therapy, particularly in renal transplant patients and those diagnosed as having inflammatory bowel disease. There are difficulties in relating the pancreatitis to the administration of one particular drug, although rechallenge has confirmed an association with Imuran on occasions.
Pulmonary reactions. Reversible pneumonitis has been described very rarely.
Hepatotoxicity. Cholestasis and deterioration of liver function have occasionally been reported in association with Imuran therapy and are usually reversible on withdrawal of therapy. This may be associated with symptoms of a hypersensitivity reaction (see Hypersensitivity reactions).
Hepatotoxicity may manifest by elevation of serum alkaline phosphatase, bilirubin and/or serum transaminases and is generally reversible after interruption of Imuran. Periodic measurement of serum transaminases, alkaline phosphatase and bilirubin is indicated for early detection of hepatotoxicity. Hepatotoxicity has been uncommon (less than 1%) in rheumatoid arthritis patients.
Rare, but life threatening hepatic damage associated with chronic administration of azathioprine has been described, primarily in transplant patients. Histological findings include sinusoidal dilation, peliosis hepatis, veno-occlusive disease and nodular regenerative hyperplasia. In some cases withdrawal of azathioprine has resulted in either a temporary or permanent improvement in liver histology and symptoms. Imuran should be permanently withdrawn in patients with hepatic veno-occlusive disease.
Also, in patients using azathioprine for long term especially for IBD, treating physicians should consider nodular regenerative hyperplasia in their differential diagnosis when patients develop clinical manifestations of non-cirrhotic portal hypertension like gastric oesophageal varices, splenomegaly, ascites and thrombocytopenia. Hence, it is advised that such patients should be monitored for these signs to avoid further complications.
Immune system disorders. Erythema nodosum.
Other adverse effects. Other adverse reactions include sores in the mouth and on the lips, meningitis, formication, acute febrile neutrophilic dermatosis (Sweet's syndrome), exacerbation of myasthenia gravis and dermatomyositis and alterations in the senses of smell or taste.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
Signs. Unexplained infection, ulceration of the throat, bruising and bleeding are the main signs of overdosage with Imuran and result from bone marrow depression which may be maximal after 9-14 days. These signs are more likely to be manifest following chronic overdosage, rather than after a single acute overdose. Occasional reports describe ingestion of from 0.5 - 7.5 g Imuran on a single occasion with apparent uneventful recovery.
Treatment. Treatment is symptomatic and has included gastric lavage. If overdosage occurs the blood picture and hepatic function in particular should be monitored. Azathioprine is dialysable but the procedure is of doubtful value since azathioprine is rapidly metabolised with entry of metabolites into tissue cells.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Suppression of the immune responses.
Azathioprine is an imidazole derivative of 6-mercaptopurine (6-MP). It is rapidly broken down in vivo into 6-MP and a methylnitroimidazole moiety. The 6-MP readily crosses cell membranes and is converted intracellularly into a number of purine thioanalogues, which include the main active nucleotide, thioinosinic acid. The rate of conversion varies from one person to another. Nucleotides do not traverse cell membranes and therefore do not circulate in body fluids. Irrespective of whether it is given directly or is derived in vivo from azathioprine, 6-MP is eliminated mainly as the inactive oxidised metabolite thiouric acid. This oxidation is brought about by xanthine oxidase, an enzyme which is inhibited by allopurinol. The activity of the methylnitroimidazole moiety has not been defined clearly. However, in several systems it appears to modify the activity of azathioprine as compared with that of 6-MP. Determinations of plasma concentrations of azathioprine or 6-MP have no prognostic value as regards effectiveness or toxicity of these compounds.
While the precise modes of action remain to be elucidated, some suggested mechanisms include:
1. the release of 6-MP which acts as a purine antimetabolite;
2. the possible blockade of -SH groups by alkylation;
3. the inhibition of many pathways in nucleic acid biosynthesis, hence preventing proliferation of cells involved in determination and amplification of the immune response;
4. damage to deoxyribonucleic acid (DNA) through incorporation of purine thio-analogues.
Because of these mechanisms, the therapeutic effect of Imuran may be evident only after several weeks or months of treatment.
Imuran tablets appear to be well absorbed from the upper gastrointestinal tract. Studies in mice with 35S-azathioprine showed no unusually large concentration in any particular tissue, but there was very little 35S found in the brain.
Clinical trials. No data available.
5.2 Pharmacokinetic Properties
No data available.
5.3 Preclinical Safety Data
Genotoxicity. Chromosomal abnormalities, which can occur independently of the influence of Imuran, have been demonstrated in both male and female transplant recipients.
Chromosomal abnormalities which disappear in time have been demonstrated in offspring of transplant recipients. Except in extremely rare cases, no overt physical evidence of abnormality has been observed in these offspring.
Azathioprine and long-wave ultraviolet light have been shown to have a synergistic clastogenic effect in patients treated with azathioprine for a range of disorders.
Carcinogenicity. See Section 4.4 Special Warnings and Precautions for Use.
Patients receiving immunosuppressive therapy are at an increased risk of developing lymphomas and other malignancies, notably skin cancers. The risk appears to be related to the intensity and duration of immunosuppression rather than to the use of any specific agent.
Patients receiving multiple immunosuppressive agents may be at risk of over-immunosuppression, therefore such therapy should be maintained at the lowest effective level. As is usual for patients with increased risk for skin cancer, exposure to sunlight and UV light should be limited by wearing protective clothing and using a sunscreen with a high protection factor.
Renal transplant recipients in some geographical areas are at greater risk of skin cancers than those in other areas.
Other neoplasms reportedly associated with Imuran include carcinoma of the urinary bladder and adenocarcinoma of the lung (see Section 4.4 Special Warnings and Precautions for Use; Section 4.8 Adverse Effects (Undesirable Effects)).
6 Pharmaceutical Particulars
6.1 List of Excipients
Imuran film coated tablets contain the excipients hypromellose, lactose monohydrate, macrogol 400, magnesium stearate, maize starch, pregelatinised maize starch and stearic acid. The 25 mg tablets also contain iron oxide red, iron oxide yellow, Opadry complete film coating system 06B230003 Orange (ARTG PI No 110486) and titanium dioxide.
6.2 Incompatibilities
No data available.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Tablets. Store below 30°C. Protect from light.
6.5 Nature and Contents of Container
Tablets. PVC/Al blister packs of 100 tablets.
6.6 Special Precautions for Disposal
Tablets. Film-coated Imuran tablets should not be divided. Provided that the film coating is intact, there is no risk in handling film-coated Imuran tablets.
6.7 Physicochemical Properties
Azathioprine is a pale yellow powder, practically insoluble in water and in alcohol. It is soluble in dilute solutions of alkali hydroxides and sparingly soluble in dilute mineral acids.
The chemical name for azathioprine is 6-[(1-methyl-4-nitro-1H-imidazol-5-yl) sulfanyl]-7H-purine.
Chemical structure.
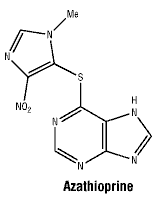
CAS number. 446-86-6.
7 Medicine Schedule (Poisons Standard)
S4 (Prescription only medicine).
Date of First Approval
30 June 2003
Date of Revision
14 January 2025
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.