Maltofer Tablets, Syrup and Drops
Brand Information
| Brand name | Maltofer Tablets, Syrup and Drops |
| Active ingredient | Iron polymaltose complex |
| Schedule | S2 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Maltofer Tablets, Syrup and Drops.
Summary CMI
MALTOFER® tablets, syrup and drops
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using MALTOFER®
MALTOFER® contains the active ingredient iron as iron polymaltose, an iron carbohydrate compound. MALTOFER® is used to treat iron deficiency in adolescents and adults where the use of ferrous iron supplements is not tolerated, or otherwise inappropriate. MALTOFER® is also used for the prevention of iron deficiency in adults and adolescents at high risk where the use of ferrous iron supplements is not tolerated, or otherwise inappropriate.
For more information, see Section 1. Why am I using MALTOFER®? in the full CMI.
2. What should I know before I use MALTOFER®?
Do not use if you have ever had an allergic reaction to MALTOFER® or any of the ingredients listed at the end of the CMI.
Talk to your doctor or pharmacist if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I use MALTOFER®? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with MALTOFER® and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use MALTOFER®?
Always take MALTOFER® exactly as your medical practitioner or pharmacist has told you. You should check with your medical practitioner or pharmacist if you are not sure. More instructions can be found in Section 4. How do I use MALTOFER®? in the full CMI.
5. What should I know while using MALTOFER®?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Drinking alcohol |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using MALTOFER®? in the full CMI.
6. Are there any side effects?
Common side effects include discoloured stool, diarrhoea, nausea, indigestion, gut or stomach pain, discomfort or bloating and constipation.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
MALTOFER® tablets, syrup and drops
Active ingredient: iron as iron polymaltose
Consumer Medicine Information (CMI)
This leaflet provides important information about using MALTOFER®.
You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using MALTOFER®.
Where to find information in this leaflet:
1. Why am I using MALTOFER®?
2. What should I know before I use MALTOFER®?
3. What if I am taking other medicines?
4. How do I use MALTOFER®?
5. What should I know while using MALTOFER®?
6. Are there any side effects?
7. Product details
1. Why am I using MALTOFER®?
MALTOFER® contains the active ingredient iron as iron polymaltose, an iron carbohydrate compound. Iron is an essential element required for the oxygen-carrying capacity of haemoglobin (the red pigment in red blood cells) and of myoglobin (the red pigment in muscle tissue). Moreover, iron plays an important role in many other vital processes in the human body.
MALTOFER® is used for treatment of iron deficiency in adults and adolescents where the use of ferrous iron supplements is not tolerated or otherwise inappropriate.
MALTOFER® is used for the prevention of iron deficiency in adults and adolescents at high risk where the use of ferrous iron supplements is not tolerated, or otherwise inappropriate.
2. What should I know before I use MALTOFER®?
Warnings
Do not use MALTOFER®:
- if you are allergic to iron polymaltose, or any of the ingredients listed at the end of this leaflet.
Symptoms of an allergic reaction may include:
- rash, itching, hives on the skin
- shortness of breath
- wheezing or difficulty breathing
- swelling of the face, lips, tongue or other parts of the body - if you have anaemia not caused by iron deficiency
- if you have iron overload (too much iron in your body) or disturbances in utilisation of iron
- for children under the age of 12 years.
- if the expiry date printed on the pack has passed
- if the packaging is torn or shows signs of tampering.
Check with your doctor or pharmacist if you:
- you have or have had an infection or tumour
- you have or have had any other health problems
- take any medicines for any other condition.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor or pharmacist if you are pregnant or intend to become pregnant.
Talk to your doctor or pharmacist if you are breastfeeding or intend to breastfeed.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
The following medicines can affect the absorption of MALTOFER®:
- Injectable iron medicines. If you are treated with injectable iron medicines, you should not take MALTOFER® in addition to that therapy.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect MALTOFER®.
4. How do I use MALTOFER®?
How much to take
- Always take MALTOFER® exactly as your medical practitioner or pharmacist has told you. You should check with your medical practitioner or pharmacist if you are not sure.
- MALTOFER® tablets contain 100 mg iron and should not be divided to take lower doses than 100 mg iron. In cases where lower doses are required, MALTOFER® oral liquid forms (syrup or drops) should be used.
- Treatment of iron deficiency in adults and adolescents (children ≥ 12 years) where the use of ferrous iron supplements is not tolerated, or otherwise inappropriate, take 100 mg to 200 mg iron (1 to 2 tablets, 10-20 mL syrup, or 40-80 drops) daily preferably with food, or higher doses as directed by your medical practitioner.
- Prevention of iron deficiency in adults and adolescents (children ≥ 12 years) at high risk where the use of ferrous iron supplements is not tolerated, or otherwise inappropriate, take 100 mg iron (1 tablet, 10 mL syrup, or 40 drops) daily preferably with food, or higher doses as directed by your medical practitioner.
- You should consult your medical practitioner regularly to monitor your iron status (e.g. serum ferritin levels) during therapy. Follow the instructions provided with the medicine.
- Do not exceed the recommended dosage.
When to take MALTOFER®
Take MALTOFER® during or immediately after a meal.
The daily dose of MALTOFER® can be taken at once or divided into separate doses.
How to take MALTOFER®
- MALTOFER® tablets should be taken with a glass of water. MALTOFER® Tablets should be swallowed whole.
- MALTOFER® drops and syrup: liquid can be mixed with fruit and vegetable juices. Any discolouration of the mixture does not affect the taste of the juices or the effectiveness of MALTOFER®.
- To ensure accurate dosing of MALTOFER® drops, the bottle needs to be held upright. The drops should flow immediately. If this does not happen, tap the bottle gently until a drop forms. Do not shake the bottle.
How long to take MALTOFER®
- This is recommended by the medical practitioner and depends upon the degree of iron deficiency.
- Do not discontinue sooner than recommended as this may reduce the success of therapy.
If you forget to take it
Take the next dose at the usual time. Do not take a double dose to compensate for the forgotten dose.
If you have any further questions on the use of this product, ask your medical practitioner or pharmacist.
If you use too much MALTOFER®
If you think that you have used too much MALTOFER® you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(in Australia by calling 13 11 26 or in New Zealand by calling The National Poisons Centre 0800 POISON or 0800 764 766), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know while using MALTOFER®?
Things you should do
- Remind any doctor, dentist or pharmacist you visit that you are using MALTOFER®.
- Tell your medical practitioner if you become pregnant while taking MALTOFER®.
- Visit your medical practitioner regularly while you are on this therapy to monitor your iron status. If symptoms persist, consult your medical practitioner.
Things you should not do
- Do not stop taking MALTOFER® or change the dose without first checking with your medical practitioner or pharmacist.
- Do not give MALTOFER® to anyone else even if they have the same condition as you.
- Do not use MALTOFER® to treat other complaints unless your medical practitioner or pharmacist says to.
- Do not take any other medicines whether they require a prescription or not without first telling your medical practitioner or consulting a pharmacist.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how MALTOFER® affects you.
However, MALTOFER® has either no or negligible influence on your ability to drive a car or operate machinery.
Drinking alcohol
Tell your doctor or pharmacist if you drink alcohol.
Looking after your medicine
Keep MALTOFER® tablets, syrup or drops in a cool dry place where the temperature stays below 25°C.
Follow the instructions in the carton on how to take care of your medicine properly.
Store it in a cool dry place away from moisture, heat or sunlight.
For example, do not store it:
- in the bathroom or near a sink, or
- in the car or on window sills.
Keep it where young children cannot reach it.
Getting rid of any unwanted medicine
If you no longer need to use this medicine or it is out of date, take it to any pharmacy for safe disposal.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions.
Less serious side effects
| Less serious side effects | What to do |
Gastro-intestinal related:
| Speak to your doctor or pharmacist if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
Allergy related:
| Call your doctor immediately or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems or, in New Zealand, nzphvc.otago.ac.nz/reporting. By reporting side effects, you can help provide more information on the safety of this medicine.
7. Product details
This medicine is available over-the-counter without a doctor's prescription.
What MALTOFER® tablets contain
| Active ingredient (main ingredient) | Each tablet contains 100 mg iron as 370 mg iron polymaltose. |
| Other ingredients (inactive ingredients) |
|
What MALTOFER® syrup contains
| Active ingredient (main ingredient) | Each 10 mL dose contains 100 mg iron as 370 mg iron polymaltose. |
| Other ingredients (inactive ingredients) |
|
| Potential allergens |
|
MALTOFER® syrup contains sorbitol and sucrose/sugar. Patients with rare hereditary problems of fructose intolerance, glucose-galactose malabsorption or sucrase-isomaltase insufficiency should not take this medicine.
The maximum daily dose of MALTOFER® syrup contains 5.6 g of sorbitol. Products containing sorbitol may have a laxative effect or cause diarrhoea.
MALTOFER® syrup contains small amounts of ethanol/alcohol, 3.25 mg per mL.
What MALTOFER® drops contains
| Active ingredient (main ingredient) | Each 1 mL contains 50 mg iron as 185 mg iron polymaltose. |
| Other ingredients (inactive ingredients) |
|
| Potential allergens |
|
Do not take this medicine if you are allergic to any of these ingredients.
What MALTOFER® looks like
MALTOFER® tablets are reddish brown, round and biconvex. They are supplied in aluminum blister packs of 30 or 100 tablets.
MALTOFER® syrup is a dark brown solution in a 150 mL brown glass bottle closed with a child resistant tamperevident screw cap. A measuring cup for administration covers the screw cap.
(*) MALTOFER® drops is a dark brown solution in a 30 mL brown glass bottle with child resistant tamper-evident screw cap and inserted dropper applicator.
* Not marketed.
Australian Registration numbers:
MALTOFER® tablets: AUST R 229647
MALTOFER® syrup: AUST R 230643
MALTOFER® drops: AUST R 230644.
Who distributes MALTOFER®
Supplied in Australia by:
Aspen Pharmacare Australia Pty Ltd
34-36 Chandos St
St Leonards NSW 2065
Australia
Supplied in New Zealand by:
Pharmacy Retailing
(trading as Healthcare Logistics)
58 Richard Pearce Drive,
Airport Oaks, Mangere 2022
New Zealand
Tel: 0800 996 312
This leaflet was revised in October 2025.
Brand Information
| Brand name | Maltofer Tablets, Syrup and Drops |
| Active ingredient | Iron polymaltose complex |
| Schedule | S2 |
MIMS Revision Date: 01 April 2026
1 Name of Medicine
Iron polymaltose (AAN).
2 Qualitative and Quantitative Composition
Maltofer tablets contain 100 mg iron as iron polymaltose as the active ingredient.
Maltofer syrup, oral liquid contains 50 mg/5 mL iron as iron polymaltose as the active ingredient. The oral solution also contains methyl hydroxybenzoate, propyl hydroxybenzoate, sorbitol solution (70%) (non-crystallising), and sucrose.
Maltofer drops, oral liquid contains 50 mg/mL iron as iron polymaltose as the active ingredient. The oral liquid also contains sucrose, sodium methyl hydroxybenzoate and sodium propyl hydroxybenzoate.
For the full list of excipients see Section 6.1 List of Excipients.
Iron polymaltose is a polynuclear iron(III)-hydroxide core surrounded by polymaltose and has a molecular weight of about 55 kD. It is stable and highly water-soluble over a broad pH range, and, unlike simple iron(III)-oxide or iron(III)-hydroxide, does not precipitate even in an alkaline environment.
3 Pharmaceutical Form
Maltofer tablets are film-coated, reddish brown, round and biconvex tablets.
Maltofer syrup, oral liquid is a dark brown solution.
Maltofer drops, oral liquid is a dark brown solution.
4 Clinical Particulars
4.1 Therapeutic Indications
Treatment of iron deficiency in adults and adolescents where the use of ferrous iron supplements is not tolerated, or otherwise inappropriate.
Prevention of iron deficiency in adults and adolescents at high risk where the use of ferrous iron supplements is not tolerated, or otherwise inappropriate.
4.2 Dose and Method of Administration
The dosage and duration of treatment depend upon the extent of iron deficiency. The daily dose can be divided into separate doses or can be taken at once. Maltofer should be taken during or immediately after a meal.
Doses below 100 mg iron cannot be achieved with Maltofer tablets. In cases where lower doses are required, Maltofer oral liquids (syrup or drops) should be used.
Maltofer tablets should be swallowed whole. Do not chew film-coated Maltofer tablets.
Maltofer oral liquids can be mixed with fruit and vegetable juices. The slight discolouration of the mixture does not affect either the taste of the juices or the efficacy of Maltofer.
Treatment of iron deficiency in adults and adolescents (children ≥ 12 years). 100 mg to 200 mg iron (1 to 2 tablets, 10-20 mL syrup, or 40-80 drops) daily preferably with food, or higher doses as directed by a medical practitioner.
Prevention of iron deficiency in adults and adolescents (children ≥ 12 years) at high risk. 100 mg iron (1 tablet, 10 mL syrup, 40 drops) daily preferably with food, or higher doses as directed by a medical practitioner.
Regular monitoring of haematological parameters and iron store levels are recommended to assess the patient's response to treatment.
4.3 Contraindications
The use of Maltofer is contraindicated in the following cases.
Known hypersensitivity to iron polymaltose or to any of the excipients.
Iron overload (e.g. haemochromatosis, haemosiderosis).
Disturbances in iron utilisation (e.g. lead anaemia, sidero-achrestic anaemia, thalassaemia).
Anaemia not caused by iron deficiency (e.g. haemolytic anaemia or megaloblastic anaemia due to vitamin B12 deficiency).
4.4 Special Warnings and Precautions for Use
Iron deficiency anaemia. All other causes of anaemia should be considered and treated prior to initiating therapy with Maltofer.
Regular monitoring of the haematologic response is required during Maltofer therapy as a risk of iron overload and liver damage exists if too much Maltofer is ingested by haemachromatosis patients over a long period of time. Do not administer to patients with iron overload or haemochromatosis.
The following medicines can affect the absorption of Maltofer.
Injectable iron medicines. If the patient is treated with injectable iron medicines, Maltofer should not be taken in addition to that therapy.
Infections or tumour may cause anaemia. Since iron can be utilised only after correcting the primary disease, a benefit/ risk evaluation is advisable.
During the treatment with Maltofer there may be dark discolouration of the faeces (stool), however this is of no clinical relevance.
Maltofer syrup, oral liquid contains the excipients methyl hydroxybenzoate and propyl hydroxybenzoate which may cause allergic reactions (possibly delayed).
Maltofer syrup, oral liquid contains sorbitol and sucrose. Patients with rare hereditary problems of fructose intolerance, glucose-galactose malabsorption or sucrase-isomaltase insufficiency should not take this medicine.
Maltofer syrup, oral liquid contains small amounts of ethanol, 3.25 mg/mL.
Maltofer drops, oral liquid contains the excipients sodium methyl hydroxybenzoate and sodium propyl hydroxybenzoate which may cause allergic reactions (possibly delayed).
Maltofer drops, oral liquid contains sucrose. Patients with rare hereditary problems of fructose intolerance, glucose-galactose malabsorption or sucrase-isomaltase insufficiency should not take this medicine.
Laboratory tests. Regular monitoring of Hb levels and serum ferritin levels should be performed to assess the response to supplementation with Maltofer as deemed appropriate by the medical practitioner.
Use in hepatic impairment. No data available.
Use in renal impairment. Very limited data available.
Use in the elderly. Clinical experience with Maltofer in the elderly is limited. For use in elderly patients consult a medical practitioner.
Paediatric use. Maltofer has not been clearly shown to be effective in children < 12 years of age. The use of Maltofer in children < 12 years of age is not recommended.
Maltofer syrup contains ethanol.
Effects on laboratory tests. Maltofer can cause discoloured (black) stool. Discoloured (black) stool may visually mask gastrointestinal bleeding. However, the haemoccult test (selective for Hb) for the detection of occult blood is not impaired, and therefore there is no need to interrupt the therapy.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Concomitant administration of parenteral iron and Maltofer is not recommended since the absorption of oral iron would be reduced.
Interactions of iron polymaltose with tetracycline or aluminium hydroxide were investigated in 3 human studies (crossover design, 22 patients per study). No significant reduction in the absorption of tetracycline was observed. The plasma tetracycline concentration did not fall below the minimum inhibitory concentration level necessary for bacteriostasis. Iron absorption from iron polymaltose was not reduced by aluminium hydroxide or tetracycline. Iron polymaltose can therefore be administered at the same time as tetracycline or other phenolic compounds, as well as aluminium hydroxide.
Studies in rats with tetracycline, aluminium hydroxide, acetylsalicylate, sulphasalazine, calcium carbonate, calcium acetate and calcium phosphate in combination with vitamin D3, bromazepam, magnesium aspartate, D-penicillamine, methyldopa, paracetamol and auranofin have not shown any interactions with iron polymaltose.
Similarly, no interactions with food constituents such as phytic acid, oxalic acid, tannin, sodium alginate, choline and choline salts, vitamin A, vitamin D3 and vitamin E, soya oil and soya flour were observed in in vitro studies with iron polymaltose. These results suggest that iron polymaltose can be taken during or immediately after food intake.
The haemoccult test (selective for Hb) for the detection of occult blood is not impaired, and therefore there is no need to interrupt the therapy with iron polymaltose.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. Fertility studies of iron polymaltose in animals did not reveal any effects on fertility or early embryonic development.
Use in pregnancy. (Category A)
Australian categorization definition of Category A: Drugs which have been taken by a large number of pregnant women and women of childbearing age without any proven increase in the frequency of malformations or other direct or indirect harmful effects on the foetus having been observed.
As a precautionary measure, women of childbearing age, and women during pregnancy should only use Maltofer after consulting a medical doctor or pharmacist. A benefit/risk evaluation is advisable.
Use in lactation. Human breast milk naturally contains iron, which is bound to lactoferrin. The amount of iron passing from iron polymaltose to the mother's milk is unknown.
No effects of iron polymaltose on development or growth of offspring were observed in a pre/ postnatal toxicity study in rats, in which nursing dams were treated throughout the preweaning lactation period. Preliminary data from studies conducted in juvenile rats showed no treatment related adverse effect when immature rats were directly treated orally with iron polymaltose from shortly after birth up to sexual maturity.
As a precautionary measure, during lactation, Maltofer should only be used after consulting a medical practitioner. A benefit/risk evaluation is advisable.
4.7 Effects on Ability to Drive and Use Machines
The effects of this medicine on a person's ability to drive and use machines were not assessed as part of its registration.
4.8 Adverse Effects (Undesirable Effects)
Clinical trials (pre- and postauthorisation, including postauthorisation safety studies). The safety and tolerability of Maltofer has been evaluated in a meta-analysis of 24 publications or clinical study reports encompassing a total number of 1473 exposed patients.
The principal adverse drug reactions that have been reported in these trials occurred in 4 system organ classes (see Table 1).
Discoloured faeces are a well-known adverse drug reaction of oral iron medications but this is considered of no clinical relevance and is underreported.
Other commonly seen side effects were gastrointestinal disorders (nausea, constipation, diarrhoea and abdominal pain).
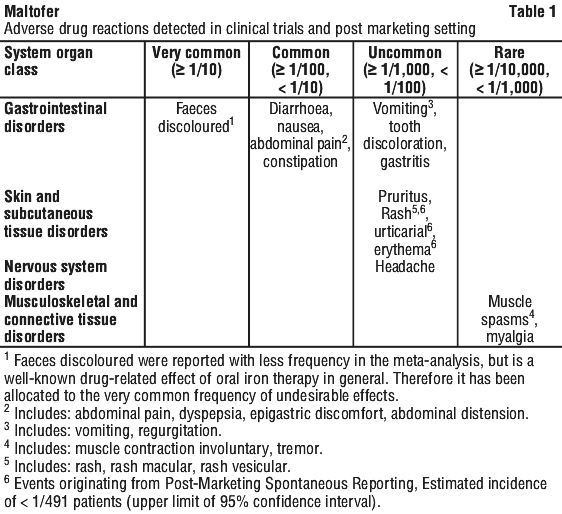
Laboratory abnormalities. No data available.
Reporting suspected adverse reactions. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
In case of overdose, intoxication or iron accumulation are unlikely with Maltofer. No cases of accidental poisoning with fatal outcome have been reported due to the low toxicity of iron polymaltose and controlled uptake of iron.
Acute overdose of iron polymaltose may cause headache, nausea, vomiting, diarrhoea, abdominal pain, lack of appetite or bloating.
In general, overdosage of iron causes haemosiderosis and consequent cirrhosis of the liver, diabetes and heart failure. Periodic monitoring of serum ferritin may be useful in recognizing a deleterious, progressive accumulation of iron.
Overdosage should be treated with supportive measures and, if required, an iron chelating agent.
For the information of the management of overdose, contact the Poison Information Centre on 131126 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. The polynuclear iron core of iron polymaltose is hypothesized to have a structure similar to that of the physiological iron storage protein ferritin. Iron polymaltose is a stable complex and does not release large amounts of iron under physiological conditions. Because of its size, the extent of diffusion of iron polymaltose through the membrane of the mucosa is about 40 times less than that of most water soluble iron(II) salts, existing in aqueous solution as hexaqua-iron(II) ion complex. Iron from iron polymaltose is taken up in the gut via an active mechanism.
The intended pharmacological action of iron polymaltose is to provide utilisable iron to target tissues. Iron polymaltose is effective in delivering iron across enterocytes to the iron transport protein transferrin and the iron storage protein ferritin. This iron is subsequently incorporated into haemoglobin during synthesis of red blood cells and thus facilitates correction of iron deficiency and anaemia.
Clinical trials. The efficacy of Maltofer in normalising Hb and replenishing iron store levels has been demonstrated in several randomised, placebo or reference therapy controlled clinical trials conducted in adults and adolescents (greater than 12 years of age) with varying iron status.
Adults and adolescents. Eleven controlled clinical studies have been performed with Maltofer in adult subjects, including 9 trials where Maltofer was compared to treatment with ferrous preparations, 2 placebo controlled trials, and one trial comparing Maltofer to no treatment. These trials included a total of approximately 900 subjects, with approximately 500 receiving Maltofer. The clinical data available for iron deficiency anaemia are up to 3 months of treatment, and up to 6 months of treatment for iron deficiency without anaemia.
No efficacy data is available related to Hb or serum ferritin concentrations after 6 months of Maltofer treatment in nonanaemic patients with iron deficiency.
Placebo controlled clinical trials in adults. There were 2 placebo controlled trials that included a total of 91 subjects, of whom 37 received Maltofer chewable tablets.
In a randomised, placebo controlled, single blind study, Macintosh and Jacobs compared 56 days of treatment with Maltofer chewable tablets containing 100 mg iron twice daily versus placebo. The subjects were healthy males who had donated blood in the preceding 12 months. At the start of the study, subjects had normal Hb (≥ 135 g/L) and either normal (serum ferritin 50-150 nanogram/mL) or deficient (serum ferritin < 20 nanogram/mL) iron stores. Treatments were administered with food. A significant rise in Hb (from 143 to 150 g/L; p = 0.03) and repletion of body iron stores (rise in serum ferritin from 16.2 to 43.2 nanogram/mL; p = 0.002) was seen in iron deficient (ID) subjects (n = 11) treated with Maltofer. In ID subjects receiving placebo (n = 12), there was no statistically significant Hb change (143 to 149 g/L; p = 0.064), although a small but statistically significant rise in serum ferritin (16.7 to 27.3 nanogram/mL; p = 0.02) was observed. Neither placebo nor Maltofer produced a statistically significant change in Hb or serum ferritin in the non-ID control subjects. This study confirms that Maltofer will replenish iron stores in ID subjects, but not in non-ID subjects.
The second clinical trial primarily tested the hypothesis that the availability of iron influences lipid peroxidation. All male subjects (n = 45) with iron deficiency (serum ferritin ≤ 30 microgram/L and some exhibited hypochromic microcytic anaemia) were randomized into three parallel groups and treated with either, Maltofer, ferrous sulfate (FS), or placebo for 6 months, twice daily with meals. Subjects received 200 mg of iron/day as Maltofer chewable tablets, or 180 mg/day of iron as microcapsulated FS, or placebo. A 50 mg ascorbic acid tablet was taken together with the FS or placebo supplements. Three subjects in the FS group, and 2 in the Maltofer group reported stomach problems. In both groups, 1 subject discontinued treatment because of stomach problems, while for the three remaining, the dose was halved. When compared with the placebo, both FS and Maltofer treatments increased Hb, serum and erythrocyte ferritin levels. Hb increased in the Maltofer group (3.3 ± 2.2 g/L) and the FS group (1.5 ± 1.5 g/L) (Table 2). The increase in serum ferritin (a routine clinical diagnostic marker for anaemia) from baseline was significantly greater in the FS group (2.2-fold) than the Maltofer group (1.3-fold), whereas erythrocytic ferritin (diagnostic marker not routinely used in the clinical setting) increased similarly in both active treatment groups (+36% FS; +27% Maltofer) (Table 2).

Short-term reference controlled studies (< 12 weeks duration). In a double blind study, the efficacy and tolerability of Maltofer was compared with FS for the treatment of iron deficiency anaemia (IDA) in adults. 121 adults with IDA (defined as Hb 8.5-12.0 g/dL, MCH < 28 picogram and/or MCHC < 33 g/dL) were randomised to receive either Maltofer chewable tablets (100 mg iron twice daily [200 mg iron/day] with meals) or FS (60 mg iron three times daily [180 mg iron/day] 30 minutes before meals)] for 9 weeks. The intention to treat analysis (ITT) included 104 patients (52 patients in each group: 7 male, 45 female). In total, 89 patients completed the 9 week study, and 17 in the Maltofer group and 15 in the FS group discontinued before the end of the study. In total, 47 patients completed the study per protocol (PP). At week 9, Hb results for the two study arms for all patients in the 'all patients efficacy analysis' (i.e. ITT analysis) and 'patients in the PP analysis with at least 9 weeks treatment' are summarized in Table 3. At 9 weeks visit, the Hb levels were below the limit of normal range for 50% (20/40) treated with Maltofer compared with 29.5% (13/44) of patients treated with FS.
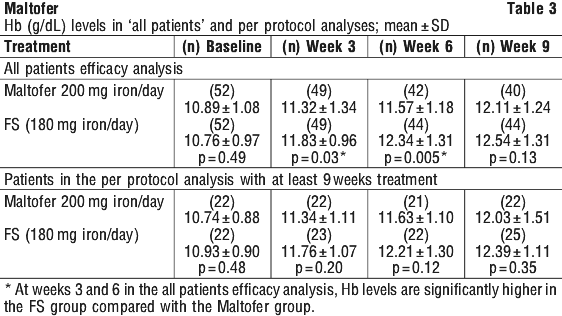

Studies in adolescents (aged 15-18 years). More than 130 adolescents have been treated with Maltofer in clinical trials. The efficacy results seen in adolescents were comparable to the results seen in adults.
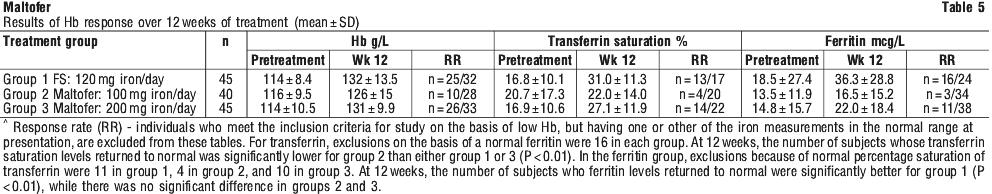
In a placebo controlled study of 120 adolescents, aged 15 to 18 years, Maltofer was shown to improve the iron status of adolescents with iron deficiency (with and without anaemia). Subjects were divided into 4 groups with 30 subjects/group: placebo, control supplement, iron deficient (TSAT* < 16%; Hb ≥ 105/115 g/L F/M), iron deficiency with anaemia (TSAT < 16%; Hb < 105/115 g/L F/M). The 3 active treatment groups received Maltofer 100 mg iron/day, 6 days/week, for 8 months. At end of the study, all 3 treatment groups demonstrated significant increases in iron parameters compared to the placebo group, including correction of iron deficiency, anaemia and improvement in iron stores (Table 6). The greatest increase in Hb (+33 g/L) was seen in the IDA group. No gastrointestinal adverse effects were reported.
*TSAT: transferrin saturation.
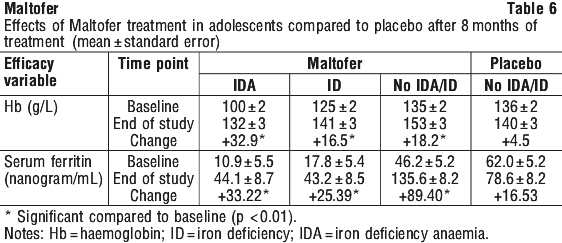
5.2 Pharmacokinetic Properties
The iron of iron polymaltose is absorbed by a controlled mechanism in the small intestine and unabsorbed iron is excreted via faeces. After absorption, iron is transferred to the blood, where it is bound to transferrin and distributed to the sites of demand, or stored as ferritin in liver and spleen. Most iron is incorporated into the oxygen-transport protein haemoglobin (Hb) during erythropoiesis in the bone marrow. The iron from erythrocytes is recycled at the end of their life span. The breakdown products of polymaltose (maltose and gluconate) are converted into glucose which is metabolised.
Studies with radiolabelled iron polymaltose showed a good correlation between iron absorption (quantified by whole body count) and the iron incorporation into Hb. Similar to other oral iron preparations, the relative absorption of iron decreases with increasing doses. The relative amount of absorbed iron correlates positively with the extent of iron deficiency (i.e. the higher the iron deficiency, the better the relative absorption). No negative impact of food on the bioavailability of iron from iron polymaltose was found: a significantly increased bioavailability of iron (7.3 fold) with concomitant food intake was demonstrated in one clinical study, while 3 studies showed a positive trend (1.1 to 2.1 fold increased bioavailability) but no clinically relevant effects.
5.3 Preclinical Safety Data
Nonclinical data established with iron polymaltose revealed no special hazard for humans based on conventional studies of single dose and repeated dose toxicity, genotoxicity and reproductive and developmental toxicity.
Carcinogenicity. No long-term studies of tumourigenic potential are available.
Genotoxicity. Iron polymaltose was not genotoxic in a conventional battery of in vitro and in vivo tests.
Teratogenicity. Embryo-foetal toxicity studies of iron polymaltose in animals did not reveal any foetal risk. Treatment of rats and rabbits with iron polymaltose during organogenesis did not induce any teratogenic or embryolethal effects. Based on these animal studies, there is no evidence of a risk during the first trimester.
No effects of iron polymaltose on the pre- and post-natal development of offspring were observed in a study in rats, in which dams were treated from Day 6 after mating to Day 20 of lactation, inclusive.
Other. The LD50 for iron polymaltose, as determined in animal studies with mice or rats was greater than an orally administered dose of 2,000 mg of iron per kilogram body weight. The available nonclinical data on toxicity after a single dose and repeated administration have yielded no further information that has not already been mentioned in other sections.
6 Pharmaceutical Particulars
6.1 List of Excipients
Maltofer tablets. Crospovidone, hyprolose, hypromellose, iron oxide red, iron oxide yellow, macrogol 6000, magnesium stearate, cellulose - microcrystalline and titanium dioxide.
Maltofer syrup. Cream flavour, ethanol, methyl hydroxybenzoate, propyl hydroxybenzoate, water - purified, sodium hydroxide, sorbitol solution (70%) (noncrystallising), and sucrose.
Maltofer drops. Water - purified, sucrose, cream flavour, sodium methyl hydroxybenzoate, sodium propyl hydroxybenzoate and sodium hydroxide.
6.2 Incompatibilities
Incompatibilities not identified as part of the registration of this medicine. See Section 4.5 Interactions with Other Medicines and Other Forms of Interactions.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C.
Keep in the original package (i.e. outer carton) in order to protect from light.
6.5 Nature and Contents of Container
Maltofer tablets are available in pack sizes of 30 or 100 film-coated tablets packed in aluminium blister packs.
Maltofer syrup oral liquid is available in a 150 mL Type III brown glass bottle closed with a child resistant and tamper-evident screw cap. A measuring cup for administration covers the screw cap.
Maltofer drops oral liquid is available in a 30 mL Type III brown glass bottle with child resistant inserted dropper applicator and closed with a tamper-evident screw cap.
Note. Not all formulations of Maltofer may be marketed in Australia.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Chemical structure. Iron polymaltose, the active substance of Maltofer, is a macromolecular complex in which polynuclear iron(III)-hydroxide is stabilized by polymaltose. It contains about 53% (m/m)* iron(III)-hydroxide, equivalent to about 27% (m/m) of iron, about 36% (m/m) polymaltose ligand, less than 6.4% (m/m) sodium chloride and less than 10% (m/m) of water.
*Mass fraction mass/mass.
CAS number. 53858-86-9.
7 Medicine Schedule (Poisons Standard)
S2 (Pharmacy medicine).
Date of Revision
12 February 2026
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.