Maxidex
Brand Information
| Brand name | Maxidex |
| Active ingredient | Dexamethasone |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Maxidex.
Summary CMI
Maxidex®
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using Maxidex?
Maxidex contains the active ingredient Dexamethasone. Maxidex is used to treat certain inflammatory eye conditions and injury of the cornea caused by chemical, heat burns or foreign bodies.
For more information, see Section 1. Why am I using Maxidex? in the full CMI.
2. What should I know before I use Maxidex?
Do not use if you have ever had an allergic reaction to Maxidex or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I use Maxidex? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with Maxidex and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use Maxidex?
- Follow the instructions carefully provided by your doctor.
- Use one or two drops in the affected eye(s) as prescribed by your doctor.
More instructions can be found in Section 4. How do I use Maxidex? in the full CMI.
5. What should I know while using Maxidex?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using Maxidex? in the full CMI.
6. Are there any side effects?
Common side effects include discomfort in eye(s), feeling that something is in your eye(s), excessive secretion of tears from the eye(s), blurred vision, increased sensitivity to light, eye irritation.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
Maxidex® Eye Drops
Active ingredient: Dexamethasone
Consumer Medicine Information (CMI)
This leaflet provides important information about using Maxidex. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using Maxidex.
Where to find information in this leaflet:
1. Why am I using Maxidex?
2. What should I know before I use Maxidex?
3. What if I am taking other medicines?
4. How do I use Maxidex?
5. What should I know while using Maxidex?
6. Are there any side effects?
7. Product details
1. Why am I using Maxidex?
Maxidex contains the active ingredient Dexamethasone.
Maxidex belongs to the group of medicines called corticosteroids.
Maxidex is used to treat certain inflammatory conditions and injury of the cornea caused by chemical, heat burns or foreign bodies. It helps in reducing swelling and relieves symptoms such as redness and soreness of eyes.
2. What should I know before I use Maxidex?
Warnings
Do not use Maxidex:
- If you are allergic to Dexamethasone, or any of the ingredients listed at the end of this leaflet. Always check the ingredients to make sure you can use this medicine. Symptoms of an allergic reaction may include shortness of breath, difficulty breathing, swelling of the face, lips, tongue or other parts of the body, rash, hives.
- If the safety seal around the closure and neck area is broken or if the bottle/packaging shows signs of tampering
- In children and elderly patients
- If you suffer from:
- Any viral infections of eyes, symptoms such as eye pain, blurred vision, redness, light sensitivity, irritation
- Tuberculosis of the eye, symptoms include eye redness, eye pain, headache, blurred vision
- Fungal eye diseases, symptoms include watery eyes, redness, eye discomfort, itching, irritation, eye pain
- Untreated parasitic eye infections, symptoms include vision problems, foreign body sensation, eye swelling
- Mycobacterial eye infections, symptoms include eye discharge, sensitivity to light, blurred vision
- Untreated bacterial eye infections, symptoms include excessive tearing, blurred vision, sensitivity to light.
Check with your doctor if you:
- have any other medical conditions
- take any medicines for any other condition
- suffer from symptoms such as dry eye, eye pain, vision problems and problems with cornea
- have a family or personal history of glaucoma (an eye condition that damages the optic nerve) or high myopia (severe nearsightedness)
- have diabetes
- suffer from any liver or kidney problems.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor if you are pregnant or intend to become pregnant.
Maxidex is not recommended in pregnant women.
Your doctor will advise you regarding the possible risks and benefits of using Maxidex during pregnancy.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
Your doctor will advise you regarding the possible risks and benefits of using Maxidex during breastfeeding.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with Maxidex and affect how it works.
- Tell your doctor if you take any of the following medicines:
- Non-Steroidal Anti-Inflammatory Drugs (NSAIDs), e.g. salicylates, ibuprofen or aspirin.
- Other corticosteroids or steroid medicines
- Ritonavir or cobicistat, drugs used to treat viral infections
- Anticholinergic medicines e.g. atropine.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect Maxidex.
4. How do I use Maxidex?
How much to use
- Follow the instructions provided and use Maxidex until your doctor tells you to stop.
- Use one or two drops topically in the conjunctival sac(s) as prescribed by your doctor.
- The dose of Maxidex depends on the severity of your condition. In severe diseases, your doctor may advise you to use the drops hourly.
- In mild diseases, your doctor may advise you to use drops up to four to six times daily.
- If you do not understand your dose, contact your doctor or pharmacist.
When to use Maxidex
- Maxidex should be used as prescribed by your doctor.
How to use Maxidex
- Sitting or lying down position might make the process simpler.
- Remove contact lenses if you are wearing them before using the eye drops.
- Shake the bottle well prior to use.
- Follow the steps below to use Maxidex:
- Wash your hands thoroughly with soap and water.
- Before using a bottle for the first time, break the safety seal around the neck area and throw the loose plastic ring away.
- Remove the cap from the bottle.
- Mix the contents of the bottle by inverting 5 to 10 times.
- Hold the bottle upside down in one hand between your thumb and middle finger (refer diagram 1).
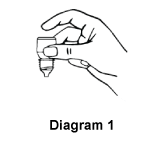
- Tilt your head back, gently pull down the lower eyelid of your eye to form a pouch/pocket.
- Place the tip of the bottle close to your eye. Do not touch the tip to your eye as this may cause injury to the eye.
- Do not touch the dropper tip to your eyelid or surrounding areas or any surface to avoid contamination of the dropper tip and solution.
- Release the required number of drops as advised by your doctor into the pouch/pocket formed between the eye and eyelid gently tapping or pressing the base of the bottle with your forefinger (refer diagrams 2 and 3).
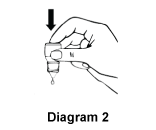
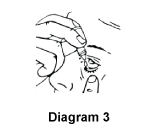
- Gently close your eyes. Do not blink or rub your eye(s).
- When your eye is closed, place your index finger against the inside corner of your eye and press against your nose for about two minutes. This will help to prevent the medicine from draining through the tear duct to the nose and throat, from where it can be absorbed into other parts of your body and may result in less side effects.
- If necessary, repeat the above steps for the other eye.
- If you want to use any other eye drops, wait at least 5 minutes after using Maxidex. Eye ointments should be used last.
- It is normal for a small amount of eye drops to spill onto your cheek since your eyelid can only hold less than one drop at a time. Wipe away any spillage with a tissue.
- Replace the cap on the bottle and close it tightly.
- Always keep the bottle tightly closed when not in use.
- Wash your hands again with soap and water to remove any residue.
- Wait for 15 minutes before putting your contact lenses in.
- Discard Maxidex Eye Drops 4 weeks after opening it.
If you forget to use Maxidex
Maxidex should be used as prescribed by your doctor. If you miss your dose at the usual time, put the drops that you missed in your eye(s) as soon as you remember, and then go back to using them as advised by your doctor.
If it is almost time for your next dose, skip the dose you missed and take your next dose when you are meant to.
Do not take a double dose to make up for the dose you missed.
If you use too much Maxidex
If you think that you have used too much Maxidex, you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
If you accidentally use several Maxidex Eye Drops in your eyes, immediately wash your eyes with lukewarm water.
5. What should I know while using Maxidex?
Things you should do
- Maxidex Eye Drops are for eye use only.
- Do not put Maxidex into your eye(s) while wearing contact lenses.
- Remove soft contact lenses before using Maxidex.
- Benzalkonium chloride, one of the ingredients in Maxidex may cause eye irritation and is known to discolour soft contact lenses.
- Put your lenses back in 15 minutes after using the eye drops.
Call your doctor straight away if you:
- notice any signs of allergic reaction.
- develop symptoms such as blurred vision or other vision problems.
- become pregnant, plan to become pregnant or if you are breast feeding while using Maxidex.
- notice any symptoms of infection in your eye(s) such as eye redness, eye pain, sensitivity of light. Maxidex may mask infections and prolong use may suppress the immune system leading to further infections of the eye.
Remind any doctor, dentist, pharmacist or specialist you visit that you are using Maxidex.
Things you should not do
- Do not stop using this medicine suddenly.
- Do not give Maxidex to anyone else, even if they seem to have the same condition as you.
- Do not touch the dropper tip to your eyelids, surrounding areas or any other surfaces.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how Maxidex affects you.
Maxidex may cause temporary blurred vision or other vision problems in some people and may affect the ability to drive or use machines.
If blurred vision occurs after use, wait until your vision clears before driving or using machinery.
Looking after your medicine
- Store below 25°C
- Do not Freeze.
Follow the instructions in the carton on how to take care of your medicine properly.
Store it in a cool dry place away from moisture, heat or sunlight; for example, do not store it:
- in the bathroom or near a sink, or
- in the car or on window sills.
Keep it where young children cannot reach it.
When to discard your medicine
Discard Maxidex Eye Drops 4 weeks after opening.
Getting rid of any unwanted medicine
If you no longer need to use this medicine or it is out of date, take it to any pharmacy for safe disposal.
Do not use this medicine after the expiry date.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
Eye problems:
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
Eye problems:
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What Maxidex contains
| Active ingredient (main ingredient) | 1 mg/mL dexamethasone |
| Other ingredients (inactive ingredients) | dibasic anhydrous sodium phosphate, polysorbate 80 (Tween 80), disodium edetate, sodium chloride, hypromellose and purified water. Citric acid monohydate and/or sodium hydroxide are used to adjust the pH. The suspension is preserved with benzalkonium chloride (0.1 mg/mL). |
| Potential allergens | May contain sulfites from the manufacturing process. |
Do not take this medicine if you are allergic to any of these ingredients.
What Maxidex looks like
Maxidex is white to pale yellow, opaque suspension with no agglomerates and is supplied in a 5 mL LDPE bottle with a LDPE plug and PP closure.
Australian registration number
AUST R: 25354
Who distributes Maxidex
Maxidex is supplied in Australia by:
Novartis Pharmaceuticals Australia Pty Limited
ABN 18 004 244 160
54 Waterloo Road Macquarie Park NSW 2113 Telephone: 1-800-671-203.
Web site: www.novartis.com.au
© Novartis Pharmaceuticals Australia Pty Limited 2025
® Registered trademark.
This leaflet was prepared in September 2025.
(max181122c_V2 based on PI max181122i)
Brand Information
| Brand name | Maxidex |
| Active ingredient | Dexamethasone |
| Schedule | S4 |
MIMS Revision Date: 01 January 2023
1 Name of Medicine
Dexamethasone.
2 Qualitative and Quantitative Composition
Maxidex eye drops contain 1 mg/mL dexamethasone and is preserved with benzalkonium chloride (0.1 mg/mL).
May contain potential allergen sulfites from the manufacturing process.
For a full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
The eye drops are a white to pale yellow, opaque suspension with no agglomerates.
4 Clinical Particulars
4.1 Therapeutic Indications
Steroid responsive inflammatory conditions of the palpebral and bulbar conjunctiva, cornea and anterior segment of the globe, such as allergic conjunctivitis, acne rosacea, superficial punctate keratitis, herpes zoster keratitis, iritis, cyclitis, selected infective conjunctivitis when the inherent hazard of steroid use is accepted to obtain an advisable diminution in oedema and inflammation; corneal injury from chemical radiation or thermal burns or penetration of foreign bodies.
4.2 Dose and Method of Administration
One or two drops topically in the conjunctival sac(s). In severe disease, drops may be used hourly, being tapered to discontinuation as the inflammation subsides. In mild disease, drops may be used up to four to six times daily.
Nasolacrimal occlusion or gently closing the eyelid after administration is recommended. This may reduce the systemic absorption of medicinal products administered via the ocular route and result in a decrease in systemic adverse reactions.
Instructions to patients. Shake bottle well before using.
No contact lenses should be worn under Maxidex eye drops treatment (see Section 4.4 Special Warnings and Precautions for Use).
To prevent contaminating the dropper tip and solution, care should be taken not to touch the eyelids or surrounding areas with the dropper tip of the bottle.
If more than 1 topical ophthalmic medicinal product is being used, the medicines must be administered at least 5 minutes apart. Ointments should be administered last.
4.3 Contraindications
Maxidex eye drops are contraindicated in epithelial herpes simplex (dendritic keratitis), vaccinia, varicella and most other viral diseases of the cornea and conjunctiva, tuberculosis of the eye, fungal disease of ocular structures or untreated parasitic eye infections, mycobacterial ocular infections or untreated bacterial eye infections.
Those persons who have shown hypersensitivity to any component of this preparation.
4.4 Special Warnings and Precautions for Use
Not for injection or oral ingestion.
This drug is not effective in the treatment of Sjogren's keratoconjunctivitis. The extensive and/or prolonged use of ophthalmic steroids increases the risk of ocular complications and could cause systemic side effects. If the inflammatory condition does not respond within a reasonable period during the course of the therapy, other forms of therapy should be instituted to reduce these risks.
Prolonged use of ophthalmic steroids may result in ocular hypertension and/or glaucoma, with damage to the optic nerve, defect in visual acuity and fields of vision and posterior subcapsular cataract formation. The risk of corticosteroid-induced raised intraocular pressure is increased for a patient with a family or personal history of glaucoma or high myopia. If these products are used for 10 days or longer, intraocular pressure should be routinely and frequently monitored even though it may be difficult in children and uncooperative patients. The risk of corticosteroid-induced ocular hypertension may be greater in children and may occur earlier than in adults. Maxidex eye drops is not approved for use in paediatric patients. The risk of corticosteroid induced raised intraocular pressure and/or cataract formation is increased in predisposed patients (e.g. diabetes). Risk-benefit should be considered in a patient with diabetes mellitus as they may be predisposed to an increase in posterior subcapsular cataract formation.
Cushing's syndrome and/or adrenal suppression associated with systemic absorption of ophthalmic dexamethasone may occur after intensive or long-term continuous therapy in predisposed patients, including children and patients treated with CYP3A4 inhibitors (including ritonavir and cobicistat), see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions. In these cases, treatment should not be discontinued abruptly, but progressively tapered.
Corticosteroids may mask infection, reduce resistance to, enhance existing or established bacterial, viral, fungal or parasitic infection. Prolonged use may suppress the immune response and thus increase the hazard of secondary ocular infections. The possibility of persistent fungal infections of the cornea should be considered after prolonged corticosteroid dosing.
Fungal infection should be suspected in patients with persistent corneal ulceration who have been or are receiving these drugs, and corticosteroids therapy should be discontinued if fungal infection occurs.
Topical ophthalmic corticosteroids may slow corneal wound healing. Topical NSAIDs are also known to slow or delay healing. Concomitant use of topical NSAIDs and topical steroids may increase the potential for healing problems.
Ocular herpes simplex has occurred in patients under systemic or local corticosteroid therapy for other conditions. Employment of corticosteroid medication in the treatment of herpes simplex other than epithelial herpes simplex keratitis, in which it is contraindicated, requires great caution and only in conjunction with antiviral therapy; periodic slit-lamp microscopy is essential.
In those diseases causing thinning of the cornea or sclera, perforations have been known to occur with the use of topical corticosteroids.
Maxidex eye drops contains benzalkonium chloride which may cause eye irritation and is known to discolour soft contact lenses. Avoid contact with soft contact lenses. In case patients are allowed to wear contact lenses, they must be instructed to remove contact lenses prior to application of Maxidex eye drops and wait at least 15 minutes before reinsertion.
Visual disturbance. Visual disturbance may be reported with systemic and topical corticosteroid use. If a patient presents with symptoms such as blurred vision or other visual disturbances, the patient should be considered for referral to an ophthalmologist for evaluation of possible causes which may include cataract, glaucoma or rare diseases such as central serous chorioretinopathy (CSCR) which have been reported after use of systemic and topical corticosteroids.
Use in hepatic impairment. The safety and efficacy of Maxidex in patients with hepatic impairment has not been established.
Use in renal impairment. The safety and efficacy of Maxidex in patients with renal impairment has not been established.
Use in the elderly. The safety and efficacy of Maxidex in elderly patients have not been established.
Paediatric use. The safety and effectiveness of Maxidex eye drops in paediatric patients have not been established. However, increased susceptibility to raised IOP and cataract formation have been described in the literature.
4.5 Interactions with Other Medicines and Other Forms of Interactions
An additional increase in intraocular pressure cannot be excluded if dexamethasone is used concomitantly with atropine or other anticholinergics which themselves may lead to IOP elevations in predisposed patients.
Concomitant use of topical steroids and topical NSAIDs may increase the potential for corneal healing problems.
CYP3A4 inhibitors including ritonavir and cobicistat may increase systemic exposure resulting in increased risk of adrenal suppression/Cushing's syndrome. (See Section 4.4 Special Warnings and Precautions for Use.) The combination should be avoided unless the benefit outweighs the increased risk of systemic corticosteroid side-effects, in which case patients should be monitored for systemic corticosteroid effects.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. Studies have not been performed to evaluate the effect of topical ocular administration of dexamethasone on fertility. There is limited clinical data to evaluate the effect of dexamethasone on male or female fertility. No study has been conducted in animals to investigate the effect of Maxidex eye drops on fertility.
Use in pregnancy. (Category B3)
Reduced placental and birthweights have been recorded in both animals and humans after long-term treatment with corticosteroid.
There are no adequate or well-controlled studies in pregnant women. Currently available clinical data provides no conclusive evidence that corticosteroids caused an increased incidence of congenital abnormalities. Prolonged or repeated use during pregnancy was associated with an increased risk of intra-uterine growth retardation, although this did not appear to be evident following short-term treatment. Topical corticosteroids should not be used extensively in pregnant women in large amounts or for prolonged periods of time. Infants born of mothers who have received substantial doses of corticosteroids during pregnancy should be observed carefully for signs of hypoadrenalism.
Maxidex eye drops should not be used in pregnancy unless the potential benefit to the mother outweighs the potential risk to the embryo or foetus.
Use in lactation. Systemically administered corticosteroids appear in human milk and could suppress growth, interfere with endogenous corticosteroid production or cause other untoward effects. It is not known whether topical administration of corticosteroids could result in sufficient systemic absorption to produce detectable quantities in human milk. A risk to the suckling child cannot be excluded. Because many drugs are excreted in milk, caution should be exercised when Maxidex eye drops is administered to a nursing woman. A decision must be made whether to discontinue breast-feeding or to discontinue/abstain from Maxidex eye drops therapy taking into account the benefit of breast-feeding for the child and the benefit of therapy for the woman.
4.7 Effects on Ability to Drive and Use Machines
Instillation of eye drops may cause transient blurring of vision or other visual disturbances may affect the ability to drive or use machines. If blurred vision occurs at instillation, the patient must wait until the vision clears before driving or using machinery.
4.8 Adverse Effects (Undesirable Effects)
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
The following adverse events have been reported following use of this or other topical ophthalmic steroid preparations.
Eye disorders. Rare (≥ 0.01%, < 0.1%): visual acuity reduced, subcapsular cataract, glaucoma, visual field defect, eyelid ptosis, mydriasis.
Infections and infestations. Rare (≥ 0.01%, < 0.1%): eye infection (exacerbation or secondary).
Injury, poisoning and procedural complications. Very rare (< 0.01%): corneal perforation.
Investigations. Uncommon (≥ 0.1%, < 1%): intraocular pressure increased.
Skin and subcutaneous tissue disorders. Rare (≥ 0.01%, < 0.1%): rash, periorbital oedema.
Post-marketing events. The following adverse reactions are classified according to the following convention: very common, common, uncommon, rare, very rare, or not known (cannot be estimated from the available data), according to system organ classes. Within each frequency-grouping, adverse reactions are presented in order of decreasing seriousness. The adverse reactions have been observed during clinical trials and post-marketing experience with Maxidex eye drops.
Eye disorders. Common (≥ 1% to < 10%): ocular discomfort.
Uncommon (≥ 0.1% to < 1%): keratitis, conjunctivitis, keratoconjunctivitis sicca, corneal staining, photophobia, vision blurred (see Section 4.4 Special Warnings and Precautions for Use), eye pruritus, foreign body sensation in eyes, lacrimation increased, abnormal sensation in eye, eyelid margin crusting, eye irritation, ocular hyperaemia.
Not known: glaucoma, ulcerative keratitis, intraocular pressure increased, visual acuity reduced, corneal erosion, eyelid ptosis, eye pain, mydriasis.
Immune system disorders. Not known: hypersensitivity.
Nervous system disorders. Uncommon (≥ 0.1% to < 1%): dysgeusia.
Not known: dizziness, headache.
Endocrine disorders. Not known: Cushing's syndrome, adrenal insufficiency.
4.9 Overdose
For information on the management of overdose, contact the Poison Information Centre on 13 11 26 (Australia).
A topical overdose of Maxidex eye drops may be flushed from the eye(s) with tepid water. Accidental ingestion of Maxidex eye drops is not likely to be associated with toxicity. Treatment of any overdose is symptomatic and supportive.
lf acute overdose is suspected, Maxidex eye drops must be ceased immediately and appropriate assessment, monitoring and treatment commenced.
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Topical ocular steroid administration has been demonstrated to be effective in the treatment of inflammatory non-infectious diseases of the anterior eye segment, the cornea, and conjunctiva.
Systemic administration is however required for the treatment of posterior eye segment disease.
Mechanism of action. Dexamethasone is an 11-hydroxy-16-methyl glucocorticoid fluorinated in the 9α position.
The therapeutic use of dexamethasone is based on its pronounced anti-inflammatory activity which is 25 to 30 times higher than that of cortisol while dexamethasone-induced side effects such as retention of sodium and water, loss in potassium and abnormal glucose metabolism are minimal in comparison to cortisol.
The mechanism of action of synthetic steroids is similar to that of cortisol. They bind to specific intracellular receptor proteins. The specific mechanism responsible for the suppression of inflammatory and allergic reactions is not fully understood. Inhibition of the synthesis of specific proteins involved in chemotoxic and immunological processes and other changes in leukocyte and macrophage function appear to be of importance.
Clinical trials. No data available.
5.2 Pharmacokinetic Properties
The determination of the ocular availability of dexamethasone after topical ocular administration is based on patients undergoing cataract extraction. The maximum aqueous humor level was reached within 2 hours. The subsequent level decrease resulted in a half-life of 3 hours.
Placental transfer. Like all corticosteroids, dexamethasone can cross the placental barrier. This forms the basis for the prophylactic administration of corticosteroids to pregnant women in imminent premature birth to promote fetal lung maturation.
Excretion into human milk. It is not known whether topical administration of corticosteroids could result in sufficient systemic absorption to produce detectable quantities in human milk. Because many drugs are excreted in milk, caution should be exercised when Maxidex eye drops is administered to a nursing woman.
5.3 Preclinical Safety Data
Genotoxicity. Dexamethasone was negative in some bacterial reverse gene mutation assays, but the results are not conclusive and dexamethasone was found to be clastogenic both in vitro in human blood lymphocytes and in vivo in mice.
Carcinogenicity. No study has been conducted in animals to investigate the carcinogenic potential of Maxidex eye drops.
Studies in animals have shown reproductive toxicity. In animal studies, corticosteroids have caused abortion and various types of malformations (cleft palate and multiple skeletal abnormalities). Reduced placental and birth weights have been recorded in both animals and humans after long-term treatment with corticosteroid. The teratogenicity of dexamethasone has also been demonstrated in mice and rabbits following topical ophthalmic application in multiple of the recommended therapeutic dose.
6 Pharmaceutical Particulars
6.1 List of Excipients
Maxidex eye drops contain 1 mg/mL dexamethasone, together with dibasic anhydrous sodium phosphate, polysorbate 80 (Tween 80), disodium edetate, sodium chloride, hypromellose and purified water. Citric acid monohydrate and/or sodium hydroxide are used to adjust the pH. The suspension is preserved with benzalkonium chloride (0.1 mg/mL).
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
Discard container 4 weeks after opening.
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C. Do not freeze.
6.5 Nature and Contents of Container
The eye drops are supplied in a 5 mL LDPE bottle with a LDPE plug and PP closure.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Chemical name: pregna-1,4-diene-3,20-dione,9-fluoro-11,17,21-trihydroxy-16-methyl-,(11β,16α).
Chemical structure.
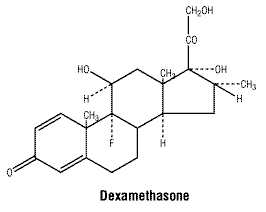
CAS number. 50-02-2.
7 Medicine Schedule (Poisons Standard)
Prescription Only Medicine (S4).
Date of First Approval
15 October 1991
Date of Revision
18 November 2022
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.