Movapo and Movapo PFS
Brand Information
| Brand name | Movapo and Movapo PFS |
| Active ingredient | Apomorphine hydrochloride hemihydrate |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Movapo and Movapo PFS.
Summary CMI
MOVAPO® and MOVAPO® PFS
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using MOVAPO or MOVAPO PFS?
MOVAPO or MOVAPO PFS contains the active ingredient apomorphine hydrochloride hemihydrate. MOVAPO and MOVAPO PFS are used in the treatment of Parkinson's disease to reduce the number and severity of bouts of freezing and stiffness (or “off” periods).
For more information, see Section 1. Why am I using MOVAPO or MOVAPO PFS? in the full CMI.
2. What should I know before I use MOVAPO or MOVAPO PFS?
Do not use if you have ever had an allergic reaction to apomorphine hydrochloride hemihydrate, sodium metabisulfite or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I use MOVAPO or MOVAPO PFS? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with MOVAPO or MOVAPO PFS and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use MOVAPO or MOVAPO PFS?
- Your doctor will tell you how much to use.
- MOVAPO and MOVAPO PFS are designed for injection under the skin (subcutaneous).
- You will be trained to recognise when and how to inject. Follow the instructions given by your doctor or pharmacist.
More instructions can be found in Section 4. How do I use MOVAPO and MOVAPO PFS? in the full CMI.
5. What should I know while using MOVAPO or MOVAPO PFS?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using MOVAPO or MOVAPO PFS? in the full CMI.
6. Are there any side effects?
Like all medicines, this medicine can cause side effects, although not everybody gets them. Some side effects can be serious and you need to know what symptoms to look out for. MOVAPO and MOVAPO PFS can cause allergic reactions which may be very serious. If you develop symptoms of allergic reaction, you may need urgent medical attention or hospitalisation.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
MOVAPO® and MOVAPO® PFS
Active ingredient(s): apomorphine (a-poe-MOR-feen) hydrochloride hemihydrate
Consumer Medicine Information (CMI)
This leaflet provides important information about using MOVAPO and MOVAPO Pre-Filled Syringe (PFS).
You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using MOVAPO and MOVAPO PFS.
Where to find information in this leaflet:
1. Why am I using MOVAPO or MOVAPO PFS?
2. What should I know before I use MOVAPO or MOVAPO PFS?
3. What if I am taking other medicines?
4. How do I use MOVAPO or MOVAPO PFS?
5. What should I know while using MOVAPO or MOVAPO PFS?
6. Are there any side effects?
7. Product details
1. Why am I using MOVAPO or MOVAPO PFS?
MOVAPO and MOVAPO PFS contains the active ingredient apomorphine hydrochloride hemihydrate. Apomorphine belongs to a group of medicines called dopaminergic compounds.
Apomorphine is used in the treatment of Parkinson's disease to reduce the number and severity of bouts of freezing and stiffness (or “off” periods). This medicine works by acting on dopamine receptors. These receptors help control movement by the body.
Ask your doctor if you have any questions about why this medicine has been prescribed for you. Your doctor may have prescribed it for another reason.
This medicine is not addictive.
2. What should I know before I use MOVAPO or MOVAPO PFS?
Warnings
Do not use MOVAPO or MOVAPO PFS if you have an allergy to:
- any medicine containing apomorphine or sodium metabisulfite
- any of the ingredients listed at the end of this leaflet
- certain types of pain killers such as morphine or other opioid analgesics
Some symptoms of allergic reaction may include shortness of breath, wheezing or difficulty breathing, swelling of the face, lips, tongue or other parts of the body, rash, itching or hives on the skin.
Always check the ingredients to make sure you can use this medicine.
Do not use MOVAPO or MOVAPO PFS if you have or have had any of the following medical conditions:
- Certain forms of dementia, e.g. Alzheimer's Disease
- Severe kidney or liver disease
- Problems with circulation of blood in the brain (cerebrovascular disease)
- Breathing problems (respiratory depression)
Do not use MOVAPO or MOVAPO PFS if:
- the packaging is torn or shows signs of tampering
- the expiry date printed on the pack has passed
- the solution has turned greed or if the solution is cloudy or you can see particles in it.
Check with your doctor if you:
- have allergies to any other medicines, foods, preservatives or dyes
- you have or have had any of the following medical conditions:
- a history of nausea and vomiting
- heart disease
- kidney disease
- liver disease
- lung disease
- problem gambling
- any addictive behaviour (e.g. sex, shopping or eating)
Before you use MOVAPO or MOVAPO PFS, your doctor will obtain an ECG (electrocardiogram) and will ask for a list of all medicines you take. This ECG will be repeated in the first days of your treatment and at any point if your doctor thinks this is needed. Your doctor will also ask you about other diseases you have, in particular concerning your heart. Some questions and investigations may be repeated at each medical visit. If you experience symptoms which may come from the heart, e.g. palpitations, fainting or near-fainting, you should report this to your doctor immediately. Also, if you experience diarrhoea or start a new medication, this should be reported to your doctor too.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor if you are pregnant or intend to become pregnant.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
Children and adolescents
MOVAPO and MOVAPO PFS should not be used in children and adolescents under the age of 18 years.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with MOVAPO or MOVAPO PFS and affect how it works.
These include:
- tetrabenazine, a medicine used to treat movement disorders
- metoclopramide, a medicine used to treat nausea
- medicines used to treat some psychiatric (mental) conditions (e.g. phenothiazines, haloperidol, flupenthixol)
- papaverine, a medicine which expands blood vessels
- amphetamines
- ondansetron, a medicine used to treat nausea and vomiting. This may result in a severe drop in blood pressure or loss of consciousness.
MOVAPO and MOVAPO PFS may affect these medicines and how well they work. You may need different amounts of your medicines, or different medicines.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect MOVAPO or MOVAPO PFS.
4. How do I use MOVAPO and MOVAPO PFS?
How much to use
- Your doctor will tell you what dose to use. This depends on your initial response to MOVAPO or MOVAPO PFS.
- Follow the instructions provided and use MOVAPO or MOVAPO PFS until your doctor tells you to stop.
When to use MOVAPO or MOVAPO PFS
- You and/or your carer will be trained by hospital staff to recognise when to use MOVAPO or MOVAPO PFS.
How to use MOVAPO or MOVAPO PFS
You will usually be in hospital when you start using this medicine. It is recommended you are given an anti-nausea drug (domperidone) for a few days, and that you will temporarily stop all other anti-Parkinsonian medication so that the correct dose of MOVAPO or MOVAPO PFS can be determined.
- MOVAPO and MOVAPO PFS is to be given as an injection under the skin (subcutaneously), usually in your lower abdomen or outer thigh. MOVAPO is either injected several times a day (intermittent injection) or continuously as an infusion (i.e. slow injection via a pump). MOVAPO PFS is injected continuously as an infusion.
- You and/or your carer will be trained by hospital staff on how to give the injections. If you do not understand the instructions, ask your doctor, nurse or pharmacist to help.
- It is advisable to change the site of injection every time you insert the needle to avoid getting lumps under the skin.
- When using MOVAPO ampoules for continuous infusion, it is recommended that MOVAPO is first diluted with an equal volume of sodium chloride 0.9% (normal saline).
- When using MOVAPO ampoules for intermittent injections, there is no need to dilute prior to use.
- When using MOVAPO PFS for continuous infusion, there is no need to dilute prior to use.
- This medicine is for individual patient use only.
If you use too much MOVAPO or MOVAPO PFS
If you think that you have used too much MOVAPO or MOVAPO PFS, you may need urgent medical attention. Symptoms of overdose may include severe nausea and vomiting, slow or troubled breathing, restlessness, hallucinations or unconsciousness.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know while using MOVAPO or MOVAPO PFS?
Things you should do
- If you plan to have surgery, tell the surgeon or anaesthetist you are taking this medicine. It may affect any medicines used during surgery.
- Keep all your doctor's appointments so that your progress can be checked.
Call your doctor straight away if you:
- are about to start on any new medication
- become pregnant
- have any symptoms which may come from your heart, e.g. palpitations, fainting, or near-fainting
- experience diarrhoea
Remind any doctor, dentist or pharmacist you visit that you are using MOVAPO or MOVAPO PFS.
Things you should not do
- Do not use MOVAPO or MOVAPO PFS to treat any other complaints unless your doctor tells you to.
- Do not give this medicine to anyone else, even if they have the same condition as you.
- Do not stop MOVAPO or MOVAPO PFS abruptly or change the dose, without speaking to your doctor to discuss a taper treatment plan.
- It is important not to suddenly stop taking your MOVAPO or MOVAPO PFS, unless advised to do so by your doctor. If you stop taking it suddenly, your condition may worsen, or you may have unwanted side effects. The dose will normally be reduced gradually over several days.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how MOVAPO or MOVAPO PFS affects you.
MOVAPO or MOVAPO PFS may cause drowsiness, sudden onset of sleepiness, dizziness or light-headedness in some people. If you have any of these symptoms do not drive, operate machinery or do anything else that could be dangerous.
Looking after your medicine
Store MOVAPO and MOVAPO PFS below 25°C.
- Do not freeze.
- Keep in the original carton to protect from light.
Follow the instructions in the carton on how to take care of your medicine properly.
Store it in a cool dry place away from moisture, heat or sunlight; for example, do not store it:
- in the bathroom or near a sink, or
- in the car or on window sills.
Keep it where young children cannot reach it.
When to discard your medicine
This medicine is for single use only. Once opened, the contents of the ampoule or pre-filled syringe should be used immediately. Discard any unused solution.
Getting rid of any unwanted medicine
If you no longer need to use this medicine or it is out of date, take it to any pharmacy for safe disposal.
Do not use this medicine after the expiry date.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
Gut related:
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
Nervous system or behaviour related:
| Call your doctor straight away if you notice any of these serious side effects. |
Very serious side effects
| Serious side effects | What to do |
Allergy related:
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these very serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What MOVAPO and MOVAPO PFS contains
| Active ingredient (main ingredient) | Apomorphine hydrochloride hemihydrate |
| Other ingredients (inactive ingredients) | Sodium metabisulfite Water for injections Hydrochloric acid Sodium hydroxide (MOVAPO only) |
| Potential allergens | Sodium metabisulfite |
Do not take this medicine if you are allergic to any of these ingredients.
What MOVAPO and MOVAPO PFS look like
MOVAPO 50 mg/5 mL is a clear, colourless, sterile solution, supplied in a box of 5 ampoules (AUST R 142093).
MOVAPO PFS 50 mg/10 mL is a clear, colourless, sterile solution, is supplied in a box of 5 pre-filled syringes (AUST R 129948).
Who distributes MOVAPO and MOVAPO PFS
In Australia:
STADA Pharmaceuticals Australia Pty Ltd
Suite 2.04, 26 Rodborough Road
Frenchs Forest NSW 2086
Australia
www.stada.com.au
In New Zealand:
CARSL Consulting
Clinical and Regulatory Services
24 Side Road, Parkhill Farm, RD10, Hastings
PO Box 766 Hastings
New Zealand
MOVAPO® is a registered trademark of Britannia Pharmaceuticals Limited.
This leaflet was prepared in January 2024.
Brand Information
| Brand name | Movapo and Movapo PFS |
| Active ingredient | Apomorphine hydrochloride hemihydrate |
| Schedule | S4 |
MIMS Revision Date: 01 March 2024
1 Name of Medicine
Apomorphine hydrochloride hemihydrate.
2 Qualitative and Quantitative Composition
Each 5 mL ampoule contains 50 mg apomorphine hydrochloride hemihydrate.
Sodium metabisulfite is included in the formulation as an antioxidant.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Solution for injection.
Movapo is a clear, colourless or almost colourless solution practically free from visible particles.
4 Clinical Particulars
4.1 Therapeutic Indications
Movapo is indicated to reduce the number and severity of 'off' phases in patients with Parkinson's disease severely disabled by motor fluctuations refractory to conventional therapy. Initiation of therapy with Movapo should be undertaken in a specialist unit in a hospital setting. Conventional therapy should be continued during 'on' phases.
4.2 Dose and Method of Administration
The optimal dosage of Movapo has to be determined on an individual patient basis. Hospital admission under appropriate specialist supervision is advised when establishing a patient's therapeutic regime.
It is essential that the patient is established on the antiemetic domperidone for at least 48-72 hours prior to initiation of therapy.
Patient selection. For patients in whom conventional therapy has failed, Movapo injections are only considered to be suitable for Parkinson's disease patients capable of recognising and anticipating 'off' phases in motor performance. Patients must be capable and motivated for Movapo to be used effectively. Adult patients through all age ranges have been successfully managed with apomorphine injections. Movapo is contraindicated in children and adolescents up to 18 years of age (see Section 4.3 Contraindications).
The elderly are well represented in the population of patients with Parkinson's disease and constitute a high proportion of those studied in clinical trials of apomorphine. The management of elderly patients treated with apomorphine has not differed from that of younger patients, except for the extra caution on commencing therapy, because of the risk of postural hypotension.
Patients who have shown a good 'on' period response during the initiation stage of apomorphine therapy, but whose overall control remains unsatisfactory using intermittent injections, or who require many and frequent injections, may be commenced on or transferred to continuous subcutaneous infusion by minipump and/or syringe driver.
The practical steps described below should be followed when commencing a patient on treatment:
Pre-treat with domperidone.
Discontinue all existing antiparkinsonian medication to provoke an 'off' phase in motor performance.
Determine the threshold dose response to Movapo that produces an unequivocal motor response.
Re-establish other antiparkinsonian agents.
Determine effective treatment regimen for Movapo injection.
Teach patient and/or carer how and when to administer.
Discharge from hospital.
Monitor frequently and adjust dosage regimen as appropriate.
Full details are given below.
Pretreatment. Domperidone is a peripherally acting dopamine receptor antagonist given by mouth to prevent nausea and vomiting. Domperidone is commenced 48-72 hours prior to the first dose of Movapo. When patients are stabilised with respect to dosage of Movapo, the dose of domperidone is reduced by 10 mg per day every week until mild nausea appears. The maintenance dose of domperidone is the lowest level which completely prevents nausea. Domperidone can usually be withdrawn after several weeks. Before the decision to initiate domperidone and apomorphine treatment, risk factors for QT interval prolongation in the individual patient should be carefully assessed to ensure that the benefit outweighs the risk (see Section 4.4 Special Warnings and Precautions for Use). The cardiovascular assessment should include an ECG and QT measurement. Patients with severe renal insufficiency will require the dosing interval of domperidone to be changed from three times a day to once or twice a day.
For further information regarding domperidone refer to the Product Information.
Provoking and assessing an 'off' phase. After at least 3 days of hospitalisation, all antiparkinsonian therapy is withheld overnight to provoke an 'off' phase in motor performance and to undertake a baseline motor assessment as follows:
(a) Alternate, unilateral hand tapping for 30 seconds on mounted digital counters (preferably 20 cm apart).
(b) Time taken to walk 12 metres.
(c) Clinical assessment of tremor and dyskinesia according to a four point scale (0 = nil, 1 = mild, 2 = moderate, 3 = severe).
(d) Scoring on a modified Webster disability scale to assess 12 features of parkinsonism (maximum disability score of 36).
Determination of the threshold dose. Following baseline motor assessment, the patient is challenged for Movapo responsiveness according to the following schedule:
1.5 mg Movapo (0.15 mL) is injected subcutaneously and the patient is observed over 30 minutes for motor responsiveness.
If no or poor response is obtained, a second dose of 3 mg Movapo (0.3 mL) is given 40 minutes after the first dose, and the patient observed for a further 30 minutes.
The dosage is increased in an incremental fashion every 40 minutes and the patient observed carefully for an unequivocal motor response. The third dose is 5 mg SC, and the fourth dose is 7 mg SC. If the patient shows no response to the 7 mg dose then the patient must be classified as a non-responder to Movapo and no further attempts to provoke a motor response should be made. If the patient shows only a mild response to the 7 mg dose, a maximum dose of 10 mg can be used to see if an unequivocal motor response is possible.
The lowest dose producing an unequivocal motor response is called the threshold dose. For the majority of patients the threshold dose is less than 7 mg Movapo (0.7 mL), although very occasionally it can be up to 10 mg Movapo (1.0 mL).
Motor responsiveness is judged to be positive if 2 or more of the following are seen:
(a) More than 15% increase in tapping score.
(b) More than 25% improvement in walking time.
(c) An improvement of at least 2 points of tremor score.
(d) An improvement of Webster's score of 3 or more.
Initiation of treatment. Following establishment of an acceptable threshold dose of Movapo, the patient should be restarted on conventional antiparkinsonian therapy.
A subcutaneous injection of the established threshold dose may then be given into the lower abdomen or outer thigh at the first signs of an 'off' phase. The patient should then be observed over the following hour and the quality of their 'on' phase noted. It may be appropriate to modify the dose of Movapo according to the patient's response.
Close monitoring of therapeutic benefits and adverse reactions under specialist supervision is required after initiation of treatment.
Movapo injection is administered by the subcutaneous route, either by intermittent injection or continuous infusion. Intermittent injection is either into the anterior abdominal wall or anterolateral thigh. The usual dosage range is 2.4 to 3.6 mg per injection; the maximum single dose being 6 mg and the maximum total daily dose being 50 mg.
To ensure accurate dosing, 1.0 mL insulin syringes should be used to administer intermittent injections. The intermittent injection is given in an undiluted form. For microbiological reasons, the contents of a syringe used for intermittent injections should be used within 24 hours of filling. Store in a refrigerator at 2 to 8°C between injections. Any solution remaining at the end of the day should be discarded and not reused on the following day.
Patients who have shown a good 'on' phase response during the initiation stage, but whose overall control remains unsatisfactory using intermittent injections, or who require many and frequent injections (e.g. 8-10 injections per day), may be commenced on or transferred to continuous subcutaneous infusion by minipump.
Continuous subcutaneous infusion of Movapo injection is effected via administration by portable syringe driven pump at a minimum dilution of 1:1 with sodium chloride 0.9% (normal saline). The dose should be titrated to the patient's response. Infusion rates can be commenced at 1 mg/hr, and then increased as necessary. The maximum daily dose should in general not exceed 200 mg/day. In clinical studies the required infusion rate varies between 1.25 and 5.5 mg/hr (equivalent to 0.02 and 0.08 mg/kg/hr), with most patients requiring (a total of) between 2 and 4 mg/hr.
Infusions should be run for waking hours only. Unless the patient is experiencing night time problems, 24 hour infusions are not advised. The infusion site should be changed every 12 hours. Prolonged infusion times are associated with local adverse effects to a more severe degree.
Monitoring treatment. Long term specialist supervision of patients is advised.
There is a high probability of adverse effects to Movapo therapy. The frequency and severity of adverse events should be monitored carefully at regular intervals and a reassessment of the patient carried out if appropriate. Adjustments to the dosage or discontinuation may be necessary.
4.3 Contraindications
Movapo is contraindicated in patients with a known hypersensitivity or allergy to apomorphine, morphine or chemically related products.
Movapo should not be administered to patients with pre-existing neuropsychiatric problems or dementias due to either pathological processes, e.g. Alzheimer's disease, or to patients whose 'on' response to L-dopa is marred by severe dyskinesia, hypotonia or psychotoxicity.
Movapo is also contraindicated in patients with inadequate renal or liver function, unstable coronary vascular disease, cerebrovascular disease, respiratory depression or CNS depression.
Movapo is contraindicated for children and adolescents under 18 years of age.
Movapo is contraindicated in patients with a known hypersensitivity to sodium metabisulfite.
Concomitant use with 5HT3 antagonists including antiemetics (for example ondansetron, granisetron, palonosetron) is contraindicated (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
4.4 Special Warnings and Precautions for Use
For subcutaneous use only (see Section 4.8 Adverse Effects (Undesirable Effects)).
Patients sensitive to morphine or its derivatives may be sensitive to Movapo. Movapo should therefore not be administered to patients with a known hypersensitivity or allergy to apomorphine, morphine or chemically related compounds (see Section 4.3 Contraindications).
Movapo contains sodium metabisulfite which may cause allergic type reactions, including anaphylactic symptoms and life threatening or less severe asthmatic episodes in susceptible people (see Section 4.3 Contraindications).
In patients with cardiac decompensation or cerebrovascular disease, vomiting may cause an increase in blood pressure that may lead to haemorrhage and vascular accidents. Apomorphine is therefore contraindicated in these patients (see Section 4.3 Contraindications).
Caution should be used in administering Movapo to patients with a predisposition to nausea and vomiting. Apomorphine may cause an increased risk of persistent vomiting. A risk/benefit assessment should be considered in these patients.
Since apomorphine may produce hypotension, even when given with domperidone pretreatment, care should be exercised in patients with pre-existing cardiac disease or in patients taking vasoactive medicinal products such as anti-hypertensives, and especially in patients with pre-existing postural hypotension.
Since apomorphine, especially at high doses, may have the potential for QT prolongation, caution should be exercised when treating patients at risk for Torsades de pointes arrhythmia.
When used in combination with domperidone, risk factors in the individual patient should be carefully assessed. This should be done before treatment initiation, and during treatment. Important risk factors include serious underlying heart conditions such as congestive cardiac failure, severe hepatic impairment or significant electrolyte disturbance. Also medication possibly affecting electrolyte balance, CYP3A4 metabolism or QT interval should be assessed.
Monitoring for an effect on the QTc interval is advisable. An ECG should be performed: prior to treatment with domperidone; during the treatment initiation phase; as clinically indicated thereafter.
The patient should be instructed to report possible cardiac symptoms including palpitations, syncope, or near-syncope. They should also report clinical changes that could lead to hypokalaemia, such as gastroenteritis or the initiation of diuretic therapy. At each medical visit, risk factors should be revisited.
Apomorphine is associated with local subcutaneous effects. These can sometimes be reduced by the rotation of injection sites or possibly by the use of ultrasound (if available) in order to avoid areas of nodularity and induration (see Section 4.8 Adverse Effects (Undesirable Effects)).
Haemolytic anaemia and thrombocytopenia have been reported in patients treated with apomorphine. Haematology tests should be undertaken at regular intervals as with levodopa, when given concomitantly with apomorphine.
Caution is advised when combining apomorphine with other medicinal products, especially those with a narrow therapeutic range (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Neuropsychiatric problems co-exist in many patients with advanced Parkinson's disease. There is evidence that for some patients neuropsychiatric disturbances may be exacerbated by apomorphine. Special care should be exercised when apomorphine is used in these patients. Apomorphine has been associated with somnolence and episodes of sudden sleep onset, particularly in patients with Parkinson's disease. Patients must be informed of this and advised to exercise caution while driving or operating machines during treatment with apomorphine. Patients who have experienced somnolence and/or an episode of sudden sleep onset must refrain from driving or operating machines. Furthermore, a reduction of dosage or termination of therapy may be considered.
The use of apomorphine in conjunction with levodopa treatment may cause Coombs' positive haemolytic anaemia. An initial screen prior to commencement of treatment and at 6 monthly intervals is recommended. In the event of the development of a haemolytic anaemia, a haematological specialist should be consulted. The dose of apomorphine and/or levodopa should be reduced, with careful monitoring of the patient's motor state. It may be necessary to discontinue treatment with levodopa and/or apomorphine in the event that it is not possible to control the anaemia satisfactorily.
Apomorphine should be used with caution in patients with endocrine, renal, pulmonary or cardiovascular disease.
Periodic evaluation of hepatic, haemopoietic, renal and cardiovascular function is advised.
Patients with severe renal insufficiency may require the dosing interval for domperidone to be less frequent (see Section 4.2 Dose and Method of Administration, Pretreatment).
Neuroleptic malignant syndrome. Symptoms suggestive of neuroleptic malignant syndrome (characterised by elevated temperature, muscular rigidity, altered consciousness, and autonomic instability) have been reported with abrupt withdrawal of dopaminergic therapy. Therefore, it is recommended to taper treatment (see Section 4.2 Dose and Method of Administration).
Dopamine agonist withdrawal syndrome. Symptoms suggestive of dopamine agonist withdrawal syndrome (for example, apathy, anxiety, depression, fatigue, sweating, and pain) have been reported with abrupt withdrawal of dopaminergic therapy, therefore, it is recommended to taper treatment (see Section 4.2 Dose and Method of Administration).
Impulse control disorders. Patients should be regularly monitored for the development of impulse control disorders. Patients and carers should be made aware that behavioural symptoms of impulse control disorders including pathological gambling, increased libido, hypersexuality, compulsive spending or buying, binge eating and compulsive eating can occur in patients treated with dopamine agonists including apomorphine. Dose reduction/tapered discontinuation should be considered if such symptoms develop.
Dopamine Dysregulation Syndrome (DDS) is an addictive disorder resulting in excessive use of Movapo seen in some patients treated with apomorphine. Before initiation of treatment, patients and caregivers should be warned of the potential risk of developing DDS.
Use in debilitated patients. Extra caution is also recommended in debilitated patients, since they may show an increased susceptibility or be more sensitive to the respiratory depressant effects of apomorphine.
Use in the elderly. Extra caution is also recommended in geriatric patients, since they may show an increased susceptibility or be more sensitive to the respiratory depressant effects of apomorphine. Extra caution is recommended during initiation of therapy in elderly patients because of the risk of postural hypotension.
Paediatric use. Movapo is contraindicated for children and adolescents under 18 years of age.
Effects on laboratory tests. Positive Coombs' tests have been reported for patients receiving apomorphine.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Patients selected for treatment with apomorphine are almost certain to be taking concomitant medications for their Parkinson's disease. In the initial stages of apomorphine therapy the patient should be monitored for unusual side-effects or signs of potentiation of effect.
Drugs which interfere with central amine mechanisms such as tetrabenazine, metoclopramide, antipsychotic dopamine blocking agents (such as phenothiazines, thioxanthines and butyrophenones), amphetamines and papaverine should be avoided. If their administration is considered essential, extreme care should be taken and the patient monitored for signs of potentiation, antagonism or other interactions and for any unusual adverse effects.
Neuroleptic medicinal products may have an antagonistic effect if used with apomorphine. There is a potential interaction between clozapine and apomorphine.
The possible side effects of apomorphine on the plasma concentrations of other medicinal products have not yet been studied. Therefore caution is advised when combining apomorphine with other medicinal products, especially those with a narrow therapeutic range.
Based on reports of profound hypotension and loss of consciousness when apomorphine was administered with ondansetron, the concomitant use of apomorphine with 5HT3 antagonists including antiemetics (for example ondansetron, granisetron, palonosetron) is contraindicated (see Section 4.3 Contraindications).
Antihypertensive and cardiac active medicinal drugs. Even when co-administered with domperidone, apomorphine may potentiate the antihypertensive effects of antihypertensive and cardiac active medicinal products.
It is recommended to avoid the administration of apomorphine with other drugs known to prolong the QT interval.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. In a fertility study in male rats, fertility was decreased at 2 mg/kg/day SC, one tenth that of the maximum recommended human dose (based on body surface area). Effects on female fertility have not been determined.
Use in pregnancy. (Category B3)
The safety of using apomorphine during pregnancy has not been established in either human or animal studies. Movapo should therefore not be used in pregnant women, or those likely to become pregnant.
Use in lactation. It is not known whether apomorphine is excreted in breast milk although problems in humans have not been documented. Nevertheless, because many drugs are excreted in human milk and because of the potential for serious adverse drug reactions due to apomorphine in breastfed infants, a decision should be made either to discontinue breastfeeding or the drug, taking into account the importance of the drug to the mother.
4.7 Effects on Ability to Drive and Use Machines
Apomorphine has varying degrees of impairment which influences the ability to drive and use machines.
Patients being treated with apomorphine and presenting with somnolence and/or sudden sleep episodes must be informed to refrain from driving or engaging in activities (e.g. operating machines) where impaired alertness may put themselves or others at risk of serious injury or death until such recurrent episodes and somnolence have resolved (also see Section 4.4 Special Warnings and Precautions for Use).
4.8 Adverse Effects (Undesirable Effects)
Very common (> 10%). Itchy nodular lesions at the injection site may be severe in patients on continuous subcutaneous infusions of Movapo injection. Most patients experience injection site reactions, particularly with continuous use. These may include subcutaneous nodules, induration (see Section 4.4 Special Warnings and Precautions for Use), erythema, tenderness and panniculitis. Various other local reactions (such as irritation, itching, bruising, fibrosis and pain) may also occur (see Section 4.4 Special Warnings and Precautions for Use). Care should be taken to ensure that areas of ulceration do not become infected.
Hallucinations have been reported.
Common (1-10%). Gastrointestinal side effects including nausea and vomiting appear to be the most prevalent adverse effects, however tolerance to these effects develops rapidly. Pre-treatment with domperidone may reduce or prevent these effects (see Section 4.2 Dose and Method of Administration).
Apomorphine is associated with somnolence. Drowsiness and sedation occur in most patients on initial treatment but these effects largely subside with repeated dosing, although in some patients these effects may persist. Tachyphylaxis to postural related faintness or syncope also occurs rapidly.
Neuropsychiatric disturbances (including confusion and visual hallucinations) have occurred during apomorphine therapy.
Yawning has been reported during apomorphine therapy.
Uncommon (0.1-1%). Apomorphine may induce dyskinesias during 'on' periods, which can be severe in some cases, and in a few patients may result in cessation of therapy. Apomorphine has been associated with sudden sleep onset episodes (see Section 4.4 Special Warnings and Precautions for Use).
Postural hypotension is seen infrequently and is usually transient (see Section 4.4 Special Warnings and Precautions for Use).
Breathing difficulties have been reported.
Local and generalised rashes have been reported. Injection site necrosis and ulceration have been reported.
Haemolytic anaemia and thrombocytopenia have been reported in patients treated with apomorphine.
Rare (0.01-0.1%). Eosinophilia has rarely occurred during treatment with apomorphine. Peripheral blood eosinophilia, elevated by up to 10%, has occurred in patients on continuous subcutaneous infusion of apomorphine. Blood counts returned to normal in about half of the patients who received treatment over one year.
Due to the presence of sodium metabisulfite, allergic reactions (including anaphylaxis and bronchospasm) may occur.
Not known (cannot be estimated from available data). Impulse control disorders including pathological gambling, increased libido, hypersexuality, compulsive spending or buying, binge eating and compulsive eating can occur in patients treated with dopamine agonists including apomorphine (see Section 4.4 Special Warnings and Precautions for Use).
Aggression and agitation have also been reported.
Headache has been reported.
Peripheral oedema has been reported.
Dopamine agonist withdrawal syndrome (apathy, anxiety, depression, fatigue, sweating and pain), see Section 4.4 Special Warnings and Precautions for Use.
Neuroleptic malignant syndrome, (see Section 4.4 Special Warnings and Precautions for Use).
Other adverse reactions to apomorphine that have been reported infrequently include transient rises in serum prolactin, stomatitis, transient metallic taste, rhinorrhoea, increased lacrimation, reduced facial hair growth, loss of libido and spontaneous penile erection.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems (Australia) or nzphvc.otago.ac.nz/reporting/ (New Zealand).
4.9 Overdose
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia) or National Poisons Centre on 0800 POISON or 0800 764766 (New Zealand).
Symptoms. The clinical features of overdose of Movapo are an extension of the pharmacological effects of the drug. They include nausea and persistent vomiting, dyskinesias, hypotension and acute circulatory failure, cardiac arrest, respiratory depression, drowsiness and central nervous system depression or stimulation, euphoria, restlessness and hallucinations and possibly coma and death. Concomitant use of domperidone may exacerbate the clinical features of overdose.
Treatment. An opioid antagonist such as naloxone may be given to treat excessive vomiting, central nervous system depression and respiratory depression due to Movapo overdose. Excessive vomiting may also be treated with domperidone. Atropine may be also used to treat bradycardia. To treat hypotension, appropriate measures should be taken e.g. raising the foot of the bed.
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Apomorphine is a directly acting dopamine receptor agonist, structurally related to dopamine. Apomorphine has high in vitro binding affinity for the dopamine D4 and D5 receptor (Ki: 4 and 14 nanoM respectively), moderate affinity (Ki: 26 to 130 nanoM) for the dopamine D2 and D3, adrenergic α1D, α2B, α2C receptors, serotonin 5HT1A, 5HT2A, 5HT2B, and 5HT2C receptors and low affinity for the dopamine D1 receptor (Ki: 370 nanoM). Apomorphine exhibits no affinity for the adrenergic β1 and β2 or histamine H1 receptors.
The effect of apomorphine as an antiparkinsonian agent is believed to be the result of direct stimulation of postsynaptic D2 dopamine receptors, but stimulation of presynaptic D2 dopamine receptors and antagonism of α2 adrenergic receptors may also be important. Apomorphine reduces the tremor, rigidity and bradykinesia in patients receiving levodopa. Apomorphine induces vomiting by direct stimulation of the medullary chemoreceptor trigger zone.
Clinical trials. No data available.
5.2 Pharmacokinetic Properties
The peripheral pharmacokinetics of apomorphine have been studied following subcutaneous injection, subcutaneous infusion and intravenous infusion.
Absorption. Following intramuscular or subcutaneous administration, apomorphine is reported to be well absorbed. Peak plasma concentration occurs as early as three minutes following subcutaneous bolus injection. The rapid and complete absorption from subcutaneous tissues and rapid clearance is believed to correlate with the rapid onset and brief duration of action respectively. Antiparkinsonian effects are observed within five minutes following subcutaneous bolus administration.
Distribution. The distribution half life of apomorphine was found to be five minutes. The volume of distribution, plasma clearance and half life were similar for subcutaneous injection, subcutaneous infusion and intravenous infusion.
Apomorphine reaches a concentration in the brain up to eight times higher than that in plasma, due to high lipid solubility which allows rapid equilibration between blood and tissue compartments.
Metabolism. Apomorphine is metabolised in the liver. Routes of metabolism in humans include sulfation, N-demethylation, glucuronidation and oxidation to norapomorphine by CYP2B6, CYP2C8 and CYP3A4. The major metabolite in humans after sublingual administration was apomorphine sulfate.
Excretion. Apomorphine is cleared rapidly. The elimination half life (t1/2) is about 33 minutes.
5.3 Preclinical Safety Data
Genotoxicity. In vitro genotoxicity studies demonstrated mutagenic and clastogenic effects, most likely due to products formed by oxidation of apomorphine. Apomorphine was not genotoxic in vivo in a mouse micronucleus test or in a rat unscheduled DNA synthesis test.
Carcinogenicity. No carcinogenicity studies have been performed.
6 Pharmaceutical Particulars
6.1 List of Excipients
Sodium metabisulfite, water for injections.
Sodium hydroxide and/or hydrochloric acid may also be included in the formulation to adjust the pH. The pH of the injection is 3.0 to 4.0.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
For microbiological reasons, the contents of a syringe used for intermittent injections should be used within 24 hours of filling. Store in a refrigerator at 2 to 8°C between injections. Any solution remaining at the end of the day should be discarded and not reused on the following day.
6.4 Special Precautions for Storage
Store below 25°C (Do not freeze). Protect from light.
6.5 Nature and Contents of Container
The ampoules are Type 1 clear glass.
Packs contain 5 x 5 mL ampoules.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
Chemical structure.
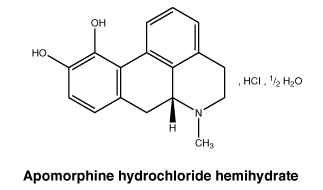
7 Medicine Schedule (Poisons Standard)
Schedule 4 - Prescription Only Medicine.
Date of First Approval
17 October 1996
Date of Revision
05 January 2024
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.