Neostigmine Juno
Brand Information
| Brand name | Neostigmine Juno |
| Active ingredient | Neostigmine methylsulfate |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Neostigmine Juno.
Summary CMI
NEOSTIGMINE JUNO
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I given Neostigmine Juno?
Neostigmine Juno contains the active ingredient neostigmine methylsulfate. Neostigmine Juno is used to increase movement of the muscles in the body and for reversing the action of certain muscle-relaxing medicines.
For more information, see Section 1. Why am I given Neostigmine Juno? in the full CMI.
2. What should I know before I am given Neostigmine Juno?
Do not use if you have ever had an allergic reaction to neostigmine methylsulfate or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I am given Neostigmine Juno? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with Neostigmine Juno and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How will I be given Neostigmine Juno?
Neostigmine Juno is an injection and will be given to you by a doctor or specially trained nurse in a hospital.
More instructions can be found in Section 4. How will I be given Neostigmine Juno? in the full CMI.
5. What should I know while using Neostigmine Juno?
| Things you should do | Tell your doctor if you have any of these medical conditions: Recent surgery involving the intestine or bladder, other intestinal or bladder problems, Asthma or any difficulty with breathing, heart disease or other heart problems, Any obstruction to your coronary arteries, Epilepsy, Low blood pressure, Parkinsons disease, Stomach ulcer, Kidney problems, Addison's disease, an overactive thyroid gland. |
| Driving or using machines |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using Neostigmine Juno? in the full CMI.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention. Some of the more common and/or serious side effects are: shivering, low oxygen levels, muscle weakness, muscle spasm, shortness of breath, rash, itching or skin irritation, changes in vision, slowed heart rate or palpitation, convulsions, low blood pressure.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
NEOSTIGMINE JUNO
Active ingredient: neostigmine methylsulfate
Consumer Medicine Information (CMI)
This leaflet provides important information about using Neostigmine Juno. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about Neostigmine Juno.
Where to find information in this leaflet:
1. Why am I given Neostigmine Juno?
2. What should I know before I am given Neostigmine Juno?
3. What if I am taking other medicines?
4. How will I be given Neostigmine Juno?
5. What should I know while using Neostigmine Juno?
6. Are there any side effects?
7. Product details
1. Why am I given Neostigmine Juno?
Neostigmine Juno contains the active ingredient neostigmine methylsulfate. Neostigmine Juno is a class of medicine known as a cholinesterase inhibitor. It works by stopping a chemical called acetylcholine, which stimulates muscle movement, from breaking down.
Neostigmine Juno is used:
- To reverse the effects of medicines that are used to stop muscles moving
- To activate the muscles in the bladder, stomach and intestine following surgery
- the treatment of myasthenia gravis
2. What should I know before I am given Neostigmine Juno?
Before you are given Neostigmine Juno your doctor will have carefully considered the situation and decided to use it. If any of the following applies to you, tell your doctor immediately.
Warnings
Do not use Neostigmine Juno if:
- You are allergic to neostigmine methylsulfate or any of the ingredients listed at the end of this leaflet; if you have an allergic reaction you may get a skin rash, hayfever, asthma or feel faint.
- At the same time you are receiving suxamethonium, a muscle relaxant given during surgery
- If you have a blockage of the intestines or urinary tract
- Peritonitis
- You have a condition where your bowel may no longer be functioning
Check with your doctor if you have or have had:
- Recent surgery involving the intestine or bladder
- Other intestinal or bladder problems
- Asthma or any difficulty with breathing
- Heart disease or other heart problems
- Any obstruction to your coronary arteries
- Epilepsy
- Low blood pressure
- Parkinsons disease
- Stomach ulcer
- Kidney problems
- Addison's disease
- An overactive thyroid gland
It may not be safe for you to be given Neostigmine Juno if you have any of these conditions.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
You should not be given Neostigmine Juno if you are pregnant or are likely to become pregnant unless the expected benefit outweighs any potential risk.
Check with your doctor if you are pregnant or intend to become pregnant.
You should not be given Neostigmine Juno if you are breastfeeding unless your doctor says so. It may make your baby arrive early if you are given it in the last weeks before your baby is due.
Your baby can take in very small amounts of Neostigmine Juno from breastmilk if you are breast feeding.
Talk to your doctor if you are breastfeeding about the risks and benefits involved.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with Neostigmine Juno and affect how it works. These include:
- Corticosteroids
- Atropine or glycopyrrolate
- Antibiotics
- Medicine for heart problems including beta blockers
- Lithium
- Chloroquinine and hydroxychloroquinine
- Quinine
Your doctor or pharmacist can tell you what to do if you are taking any of these medicines.
If you have not told your doctor about any of these things, tell them before you are given Neostigmine
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect Neostigmine Juno.
4. How will I be given Neostigmine Juno?
How you are given Neostigmine Juno
Neostigmine Juno will be given to you by a doctor or a specially trained nurse. It may be given just under the skin, into a muscle, or directly into the bloodstream. The dose will be carefully worked out depending on the procedure and your body weight.
If you are given too much Neostigmine Juno
Neostigmine Juno is given to you in a hospital under direct supervision of a doctor so it is extremely unlikely that you will be given too much.
However, symptoms of an overdose may include nausea, vomiting, muscle cramps, sweating, increased saliva and changes in heart rate.
Alert your doctor immediately.
5. What should I know while using Neostigmine Juno?
Things you should do
Driving or using machines
Be careful before you drive or use any machines or tools until you know how Neostigmine Juno affects you.
Neostigmine Juno may cause dizziness and muscle weakness in some people, you should not drive or operate machinery
Looking after your medicine
The hospital will store Neostigmine Juno under the correct recommended conditions.
It should be kept in a cool dry place away from moisture, heat or sunlight below 25°C
Getting rid of any unwanted medicine
Your doctor or pharmacist will dispose of any Neostigmine Juno that may be left over
Do not use this medicine after the expiry date.
6. Are there any side effects?
Tell your doctor or pharmacist as soon as possible if you do not feel well while you are receiving Neostigmine Juno Solution for Injection.
Neostigmine Juno Solution for Injection helps most people with muscle weakness but may have some unwanted side effects in a few people.
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
What Neostigmine Juno contains
| Active ingredient (main ingredient) |
|
| Other ingredients (inactive ingredients) |
|
Do not take this medicine if you are allergic to any of these ingredients.
What Neostigmine Juno looks like
Neostigmine Juno is supplied as a clear, colourless solution for injection in a glass ampoule
Neostigmine Juno is supplied as:
Neostigmine Juno 2.5mg/mL solution for injection
(AUST R 219054).
Who distributes Neostigmine Juno
Juno Pharmaceuticals Pty Ltd
15-17 Chapel Street,
Cremorne,
VIC 3121
Australia
This leaflet was prepared December 2025
Brand Information
| Brand name | Neostigmine Juno |
| Active ingredient | Neostigmine methylsulfate |
| Schedule | S4 |
MIMS Revision Date: 01 January 2026
1 Name of Medicine
Neostigmine methylsulfate.
2 Qualitative and Quantitative Composition
Neostigmine Juno injection contains 2.5 mg neostigmine methylsulfate in 1 mL solution.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Neostigmine Juno Solution for Injection is a clear, colourless sterile solution.
4 Clinical Particulars
4.1 Therapeutic Indications
Neostigmine is indicated for:
Reversal of the effects of non-depolarising neuromuscular blocking agents.
Prophylaxis and treatment of post-operative intestinal atony and urinary retention.
Treatment of myasthenia gravis during acute exacerbations, when the condition is severe or in neonates.
4.2 Dose and Method of Administration
Neostigmine Juno Solution for Injection can be given as an intramuscular (IM), intravenous (IV) or subcutaneous (SC) injection. The following doses are approximately equivalent in effect: 0.5 mg IV = 1.0-1.5 mg IM or SC.
When Neostigmine Juno Solution for Injection is given, a syringe of atropine sulfate or glycopyrrolate should be available to counteract severe cholinergic reactions, if they occur. Do not mix atropine with other drugs in the same syringe as compatibility data are not available.
Neostigmine Juno Solution for Injection in ampoules contains no antimicrobial agent. It should be used once and any residue discarded.
Antagonist to nondepolarising neuromuscular blockade. Usually, reversal of neuromuscular blockade with Neostigmine Juno Solution for Injection should not be attempted until spontaneous recovery from paralysis is evident. It is recommended that the patient be well ventilated and patent airway maintained until complete recovery of normal respiration is affirmed.
Neostigmine should be administered when the first twitch response is substantially greater than 10% of baseline, or when a second twitch is present.
Adequacy of the reversal of the neuromuscular block needs to be based on a clinical assessment of the patient and not train-of-four responses alone, unless quantitative (numeric) assessment is made of neuromuscular function.
Patients should be monitored for clinical signs of residual blockade (e.g. difficulty maintaining a patent airway, generalised weakness, inadequate ventilatory effort) following cessation of the anaesthetic and extubation.
Adults. A single dose of neostigmine 0.5 to 2.5 mg (0.04-0.07 mg/kg) to be administered simultaneously with atropine sulfate 0.6-1.2 mg (0.02 to 0.03 mg/kg) or glycopyrrolate 0.2 mg intravenously per 1 mg neostigmine or 0.008 mg/kg glycopyrrolate intravenously with 0.04 mg/kg neostigmine by slow IV injection over 1 minute is generally adequate for complete reversal of nondepolarising muscle relaxants within 5 to 15 minutes. The maximum recommended dose of neostigmine in adults is 5 mg as excess of this dose of neostigmine may produce depolarising neuromuscular block.
Children. The suggested dose in children is 0.04 mg/kg and atropine sulfate 0.02 mg/kg or glycopyrrolate 0.008 mg/kg by slow IV injection over 1 minute. Maximum recommended dose of neostigmine in children is 2.5 mg.
The two drugs are often given simultaneously, but in patients with bradycardia, the pulse rate should be increased to about 80 beats/minute e.g. with atropine before administering neostigmine.
Neostigmine and glycopyrrolate may be given in the same syringe.
The speed of recovery from neuromuscular blockade is primarily determined by the intensity of the block at the time of antagonism. It is also influenced by other factors including the presence of drugs (e.g. anaesthetic drugs, antibiotics and antiarrhythmic drugs) and physiological changes (e.g. electrolyte and acid-base imbalance, renal impairment). These factors may prevent successful reversal with Neostigmine Juno Solution for Injection or lead to recurarisation after apparently successful reversal. It is imperative that the patients should not be left unattended until these possibilities have been excluded.
Myasthenia gravis. Adults. 1 mg to 2.5 mg given as an IM or SC injection at intervals throughout the day when greater strength may be needed (e.g. mornings and before meals) giving a total daily dose of 5 to 20 mg. Duration of action of a single dose is 2 to 4 hours.
Neonates. 0.05-0.25 mg as an IM injection every 2-4 hours, half an hour before feeding. Treatment is not usually required beyond 8 weeks of age. Because the condition is usually self-limiting the daily dosage should gradually be reduced until the drug can be withdrawn.
Older children. 0.2 to 0.5 mg by injection as required. Dosage should be adjusted according to response.
When large doses of neostigmine are given to myasthenic patients, atropine sulfate may be required to counteract the muscarinic side effects.
Intestinal atony. Prophylaxis. 0.25 mg as an IM or SC injection before or immediately after the operation, repeated every 4 to 6 hours, for 2 to 3 days.
Treatment. 0.5 mg as an IM or SC injection repeated at intervals of 4 to 6 hours.
Urinary retention. Prophylaxis. 0.25 mg as an IM or SC injection as for intestinal atony.
Treatment. 0.5 mg as an IM or SC injection and apply heat to lower abdomen. After patient has voided continue 0.5 mg SC or IM every 3 hours for at least 5 injections. If there has been no urinary response within one hour of the first dose, the patient should be catheterised.
Dosage adjustment. Renal impairment. The duration of effect may be prolonged in patients with renal impairment since neostigmine is excreted mostly in the urine. Dosage adjustment may be needed for patients in renal failure.
Elderly. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or drug therapy.
4.3 Contraindications
Mechanical obstruction of gastrointestinal, urinary tract or doubtful bowel viability.
Known hypersensitivity to neostigmine or any excipients listed in Section 6.1.
Peritonitis (when used to promote peristalsis).
Bronchial asthma.
This medicine should not be given in conjunction with depolarising muscle relaxants such as suxamethonium as neostigmine potentiates the depolarising myoneural blocking effects of this agent.
4.4 Special Warnings and Precautions for Use
Neostigmine should be used with extreme caution in patients who have undergone recent intestinal or bladder surgery.
Administration of neostigmine to patients with intestinal anastomosis may produce rupture of the anastomosis or leakage of intestinal contents.
Neostigmine alone induces significant bronchoconstriction.
Use with caution in patients with, cardiac disease and cardiovascular disorders including arrhythmias, bradycardia, recent myocardial infarction or coronary occlusion, and hypotension as well as in patients with epilepsy, vagotonia, parkinsonism, peptic ulceration, renal impairment, Addison's disease or hyperthyroidism.
Patients who are hyperreactive to neostigmine experience a severe cholinergic reaction to the drug.
Neostigmine should not be given during cyclopropane or halothane anaesthesia; although it may be used after withdrawal of these agents.
With large doses, simultaneous parenteral administration of atropine sulfate or glycopyrrolate may be advisable. Atropine sulfate or glycopyrrolate should always be available along with other anti-shock medications (adrenaline) in case of hypersensitivity to neostigmine.
Neostigmine may prolong the depolarising neuromuscular blocking action of depolarising muscle relaxants such as suxamethonium and prolonged apnoea may result (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Neuromuscular function monitoring must be available for every patient in whom neuromuscular blockade has been induced and should be used whenever the anaesthetist is considering extubation following the use of non-depolarising neuromuscular blockade.
Re-administration of muscle relaxant shortly after use of neostigmine should be done with caution: competing at the neuromuscular junction there may be increased levels of acetylcholine and neostigmine has some direct postsynaptic cholinomimetic effects, thus resistance to muscle relaxation may be seen. There will still be some previously administered relaxant in the patient, thus prolonged recovery may also be seen.
The administration of sugammadex after neostigmine reversal may increase muscle relaxation as all muscle relaxant is removed and the neuromuscular inhibition by neostigmine is revealed.
As the severity of myasthenia gravis can fluctuate considerably, care is required to avoid cholinergic crisis due to overdosage with neostigmine (see Section 4.9 Overdose).
Use in renal impairment. Use neostigmine with caution in patients with renal impairment. Neostigmine is excreted mostly in the urine. Please also see Section 4.2 Dose and Method of Administration.
Use in the elderly. In a study of 59 patients over 65 years of age (32 with cardiovascular disease) receiving neostigmine 50 microgram/kg with glycopyrronium 10 microgram/kg, compared to previous studies in healthy adults, the initial increase in heart rate is higher, the subsequent falls in heart rate are less in elderly patients and the incidence of cardiac dysrhythmias was higher. In general, dose selection for an elderly patient should be cautious, usually starting at the low end of the dosing range, reflecting greater frequency of decreased hepatic, renal, or cardiac function, and of concomitant disease or drug therapy.
Paediatric use. Limited literature data available.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Corticosteroids. Corticosteroids may decrease the anticholinesterase effects of neostigmine. Conversely anticholinesterase effects may increase after stopping corticosteroids.
Depolarising muscle relaxants. Neostigmine may prolong the Phase I block of depolarising muscle relaxants such as suxamethonium. Prolonged muscle paralysis with extended periods of apnoea may occur unless IPPV (intermittent positive pressure ventilation) is maintained. Neostigmine effectively antagonises the effect of non-depolarizing muscle relaxants and this interaction is used to therapeutic advantage to reverse muscle relaxation after surgery.
Atropine or glycopyrrolate. Atropine or glycopyrrolate reverses the muscarinic effects of neostigmine. This interaction is used to counteract the muscarinic symptoms of neostigmine toxicity, however masking the signs of overdosage can lead to inadvertent induction of cholinergic crisis with the use of atropine or glycopyrrolate.
Aminoglycosides, local/general anaesthetics, antiarrhythmic agents. Anticholinesterase agents can be effective in reversing neuromuscular block induced by aminoglycoside antibiotics. Aminoglycoside antibiotics, local and some general anaesthetics, antiarrhythmic agents and other drugs that interfere with neuromuscular transmission should be used cautiously, if at all, in patients with myasthenia gravis. The dose of neostigmine may need to be increased accordingly.
Quinine, chloroquine, hydroxychloroquine, beta-blockers and lithium may reduce the effectiveness of treatment with neostigmine.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. No data available.
Use in pregnancy. (Category B2)
The maternal need for neostigmine may be absolute in the context of myasthenia gravis. Cholinergic effects in the neonate are rare.
The safety of neostigmine in pregnancy has not been established with respect to possible adverse effects on foetal development. Anticholinesterase agents may cause uterine irritability and induce premature labour when given IV to pregnant women near term. Therefore neostigmine should not be used in pregnant women or those likely to become pregnant unless the expected benefits outweigh any potential risk.
Use in lactation. Evidence indicates that only negligible amounts of neostigmine enter the breast milk; nevertheless, the possibility of adverse effects on the breastfeeding infant should be considered.
4.7 Effects on Ability to Drive and Use Machines
The effects of this medicine on a person's ability to drive and use machines were not assessed as part of its registration.
4.8 Adverse Effects (Undesirable Effects)
Inadequate reversal. Studies have shown ~31% to 50% of patients have clinically significant residual neuromuscular blockade with train-of-four ratios less than 0.90 following surgery.
Patients with train-of-four ratios less than 0.90 are at increased risk for hypoxemic events, impaired control of breathing during hypoxia, airway obstruction, postoperative pulmonary complications (there is an increase in the risk of aspiration) and symptoms of muscle weakness.
Clinical signs include:
Weakness (head lift, hand grip, eye-opening, or tongue protrusion).
Inability to smile, swallow, speak, cough, track objects with eyes; or inability to perform a deep or vital capacity breath.
Symptoms also include blurry vision, diplopia, facial weakness, facial numbness, and general weakness.
Adverse reactions. Adverse reactions in a study in 14 healthy volunteers receiving neostigmine 2.5 mg with glycopyrrolate 450 microgram repeated after 1/4 h in 9 of the volunteers included: muscle weakness 14 (100%), blurred vision 13 (93%), abdominal cramping 13 (93%), dry mouth 11 (79%), nausea 11 (79%), vomiting 1 (7%), none of these were seen in the 7 subjects receiving saline placebo. See Table 1.
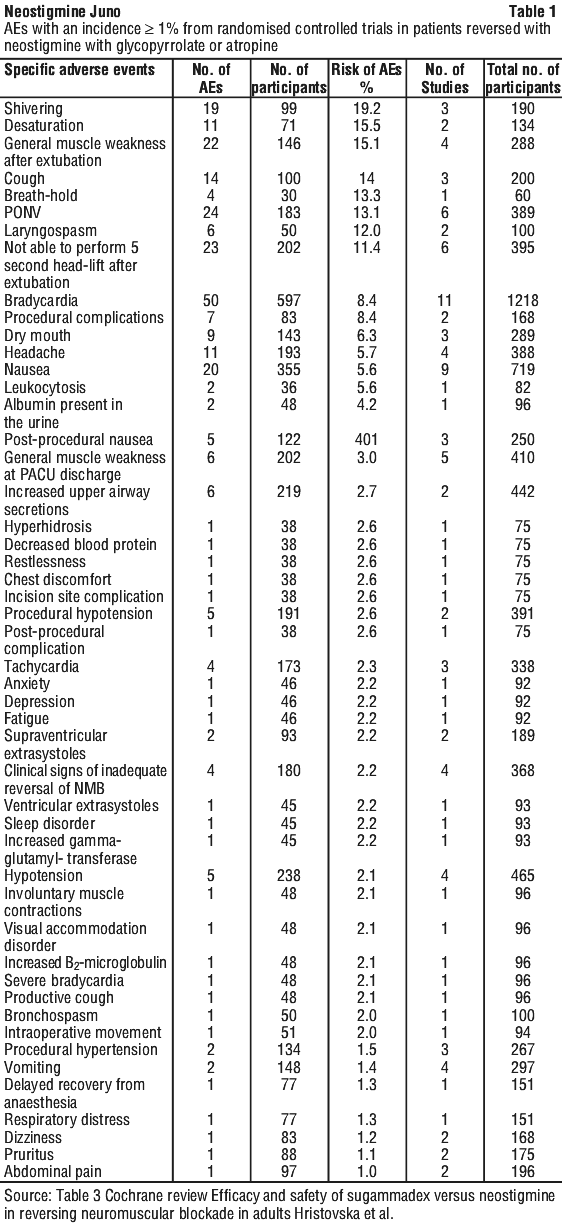
Central nervous system. Headache, dizziness, convulsions, loss of consciousness, coma, drowsiness, restlessness, ataxia, slurred speech, agitation, fear, cholinergic syndrome, myasthenia gravis (cholinergic crisis may be difficult to distinguish from myasthenia crisis).
Gastrointestinal. Nausea, vomiting, diarrhoea, abdominal cramps, flatulence, increased peristalsis, increased intestinal motility and involuntary defecation.
Genitourinary. Involuntary urination or desire to urinate.
Musculoskeletal. Muscle cramps, muscle spasm, fasciculation, general weakness and paralysis.
Respiratory. Increased oral, pharyngeal and bronchial secretions, dyspnoea, bronchospasm, respiratory depression, respiratory arrest, tight chest and wheezing.
Allergic. Allergic reactions including anaphylaxis, hypersensitivity, angioedema.
Skin. Rash, hyperhidrosis and urticaria.
Other. Increased sweating and salivation, miosis, vision changes, nystagmus and increased lacrimation.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
Overdosage with neostigmine can cause cholinergic crisis, which is characterised by increasing muscle weakness. Myasthenic crisis is due to an increase in severity of the disease and may be difficult to distinguish from cholinergic crisis on a symptomatic basis. Cholinergic crisis can lead to respiratory paralysis, which may result in death, while myasthenic crisis is extreme muscle weakness. The differentiation between the two crises is extremely important as treatment is different for each. The two types of crises can be differentiated by the use of edrophonium and clinical judgement.
Symptoms. Signs of overdosage due to muscarinic effects may include abdominal cramps, increased peristalsis, diarrhoea, nausea and vomiting, increased bronchial secretion, salivation, diaphoresis and miosis. Nicotinic effects consist of muscular cramps, fasciculations and general weakness. Bradycardia and hypotension may also occur.
Treatment. The treatment of cholinergic crisis requires the discontinuation of all cholinergic medication. The immediate use of atropine is also recommended, muscarinic effects are controlled with IV atropine sulfate (1 to 2 mg) followed by IM atropine sulfate every 2 to 4 hours. Assistance of ventilation may be required if respiration is severely depressed.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Neostigmine is an anticholinesterase agent which inhibits reversibly the hydrolysis of acetylcholine by competing with acetylcholine for attachment to acetylcholinesterase. As a result acetylcholine accumulates at cholinergic synapses and its effects are prolonged and exaggerated. Neostigmine is therefore capable of producing a generalised cholinergic response, including miosis, increased tonus of intestinal and skeletal musculature, constriction of bronchi and ureters, bradycardia and stimulation of salivary and sweat glands.
In addition neostigmine is used mainly for its direct cholinomimetic effect on skeletal muscle and to a lesser extent to increase the activity of smooth muscle.
Because of its quaternary ammonium structure, in moderate doses, neostigmine does not cross the blood-brain barrier to produce CNS effects. Extremely high doses, however produce CNS stimulation followed by CNS depression.
Pharmacodynamics. In healthy volunteers glycopyrrolate/neostigmine in combination produces muscle weakness in a dose related fashion, affecting hand grip strength, single twitch height, dysphagia and to some extent diplopia.
Neostigmine-induced weakness with characteristics of phase-1 depolarising neuromuscular blockade was evidenced by fasciculations of multiple muscle groups, depression of the single twitch height, no fade in train-of-four and increased neuromuscular blockade after the second dose of anticholinesterase agent and muscle weakness.
Thus residual post-operative weakness may be both inadequate reversal and neostigmine induced weakness (especially with large doses).
Respiratory muscle weakness produces decreased volumes (FEV1 and FVC).
Clinical trials. Only literature data available.
5.2 Pharmacokinetic Properties
Distribution. The major site of uptake of neostigmine is the liver.
Because of its quaternary ammonium structure, in moderate doses, neostigmine does not cross the blood-brain barrier to produce CNS effects.
Metabolism. Neostigmine is excreted in urine as unchanged drug (50%) and metabolites. It is metabolised partly by the hydrolysis of the ester linkage and partly by microsomal enzymes in the liver.
Excretion. Approximately 80% of a single IM dose of neostigmine is excreted in the urine in 24 hours, about 50% as unchanged drug and the remainder as metabolites. Following IV administration the elimination half-life ranges from 47 to 60 minutes and after IM administration 50 to 91 minutes.
5.3 Preclinical Safety Data
Genotoxicity. No data available.
Carcinogenicity. No data available.
6 Pharmaceutical Particulars
6.1 List of Excipients
Sodium chloride, water for injections.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C. Product is for single use in one patient only. Discard any residue.
6.5 Nature and Contents of Container
Neostigmine Juno Solution for Injection is available as 2.5 mg neostigmine methylsulfate in 1 mL colourless type 1 glass ampoules in cartons of 10 or 50 ampoules.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
Chemical name: (3-dimethyl-carbamoxyloxy) trimethylanilinium methyl sulfate.
Chemical structure.
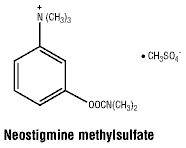
Molecular weight: 334.4.
Molecular formula: C13H22N2O6S.
7 Medicine Schedule (Poisons Standard)
Schedule 4 (Prescription only Medicine).
Date of First Approval
27 January 2015
Date of Revision
01 December 2025
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.