Phenylephrine BNM
Brand Information
| Brand name | Phenylephrine BNM |
| Active ingredient | Phenylephrine hydrochloride |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Phenylephrine BNM.
What is in this leaflet
Please read this leaflet carefully before you are given Phenylephrine BNM.
This leaflet answers some common questions about Phenylephrine BNM. It does not contain all the available information. The most up-to-date Consumer Medicine Information can be downloaded from www.ebs.tga.gov.au.
Reading this leaflet does not take the place of talking to your doctor or pharmacist.
All medicines have risks and benefits. Your doctor has weighed the risks associated with giving you Phenylephrine BNM against the benefits this medicine is expected to have for you.
If you have any concerns about being given this medicine, ask your doctor, pharmacist or nurse.
Keep this leaflet with the medicine. You may want to read it again.
What Phenylephrine BNM is used for
Phenylephrine BNM contains phenylephrine hydrochloride. It works by causing constriction (narrowing) of your blood vessels.
It belongs to a group of medicines called vasoconstrictors.
Phenylephrine BNM is used to help increase your blood pressure and slow down your heart, for example, during surgery.
Your doctor may have prescribed this medicine for another reason.
Ask your doctor if you have any questions about why it has been prescribed for you.
Phenylephrine BNM is only available with a doctor's prescription.
Phenylephrine BNM is not addictive.
Before you are given Phenylephrine BNM
Phenylephrine BNM is not suitable for everyone.
When you must not be given it
You must not be given Phenylephrine BNM if you are allergic to:
- Phenylephrine
- any of the ingredients listed at the end of this leaflet.
Symptoms of an allergic reaction may include:
- shortness of breath, wheezing or difficulty breathing
- swelling of the face, lips, tongue or other parts of the body
- rash, itching or hives on the skin.
You must not be given Phenylephrine BNM if you have:
- very high blood pressure
- a very fast heart beat (palpitations).
Do not use it after the expiry date printed on the pack. If you are given this medicine after the expiry date has passed, it may not work as well.
Do not use it if the packaging is torn or shows signs of tampering.
If you are not sure whether you should be given Phenylephrine BNM, talk to your doctor.
Before you are given it
Tell your doctor or pharmacist if you have allergies to any other medicines, foods, preservatives or dyes.
Tell your doctor if you have or have had any medical conditions, especially the following:
- thyroid disease
- slow heart rate
- other heart disease
- severe arteriosclerosis (a disease of the arteries).
Tell your doctor if you are pregnant or intend to become pregnant. Your doctor will discuss the risks and benefits of being given Phenylephrine BNM during pregnancy.
Tell your doctor if you are breast-feeding or plan to breastfeed. Your doctor will discuss the risks and benefits of being given Phenylephrine BNM when breastfeeding.
If you have not told your doctor or nurse about any of the above, tell them before you are given Phenylephrine BNM.
Taking other medicines
Tell your doctor if you are taking any other medicines, including any that you get without a prescription from your pharmacy, supermarket or health food shop.
Some medicines and Phenylephrine BNM may interfere with each other. These include:
- certain medicines to treat depression (such as monoamine oxidase inhibitors and tricyclic antidepressants).
- halothane anaesthetics (a type of medicine used as an anaesthetic).
- certain medicines (such as oxytocin) used to stimulate labour in pregnant women.
- certain medicines which restrict your blood vessels such as metaraminol.
The above medicines may be affected by Phenylephrine BNM, or may affect how well it works. You may need different amounts of your medicines or you may need to take different medicines.
Your doctor and pharmacist have more information on medicines to be careful with or avoid while being given Phenylephrine BNM.
How Phenylephrine BNM is given
How it is given
Phenylephrine BNM will be given by slow injection into a vein.
Your doctor will determine how you will be given this medicine. It may depend on why you need to use this drug.
Phenylephrine BNM must only be given by a doctor or nurse.
How much will be given
Your doctor will decide what dose and how long you will receive Phenylephrine BNM. The dose will be different, depending on how your doctor gives you Phenylephrine BNM and why you are being given it.
The need for more doses will depend on how well your body responds to the treatment. Your doctor will decide how many injections you need, and how often you should receive them.
While you are being given Phenylephrine BNM
Things you must do
Your doctor will monitor your blood pressure closely while you are being given Phenylephrine BNM.
If you are about to be started on any new medicine, tell your doctor and pharmacist that you are being given Phenylephrine BNM.
Likewise, tell any other doctors, dentists and pharmacists who are treating you that you are being given this medicine.
Things to be careful of
Be careful driving or operating machinery until you know how Phenylephrine BNM affects you.
Make sure you know how you react to Phenylephrine BNM before you drive, operate machinery or do anything else that could be dangerous.
Be careful when drinking alcohol while you are taking this medicine.
In case of overdose
If you are given too much (overdose)
As Phenylephrine BNM is given to you in hospital under the supervision of your doctor, it is very unlikely that you will receive too much.
Immediately tell your doctor or nurse if you think that you or anyone else has taken or been given too much Phenylephrine BNM.
If you are not in a hospital, immediately telephone your doctor or the Poisons Information Centre (telephone 13 11 26 in Australia), or go to Accident and Emergency at your nearest hospital, if you think that you or anyone else may have been given too much Phenylephrine BNM.
Do this even if there are no signs of discomfort or poisoning. You may need urgent medical attention.
Symptoms of an overdose may include sensation of fullness in the head, tingling in the hands or feet and irregular or fast heartbeat.
Side effects
Tell your doctor or pharmacist as soon as possible if you do not feel well while you are being given or after receiving Phenylephrine BNM.
Like all medicines, Phenylephrine BNM may occasionally cause side effects in some people. Sometimes they are serious, most of the time they are not. You may need medical attention if you get some of the side effects.
Ask your doctor or nurse to answer any questions you may have.
Tell your doctor or nurse if you notice any of the following and they worry you:
- headache
- restlessness
- excitability.
These are mild side effects.
Tell your doctor immediately if you notice any of the following:
- fast or irregular heartbeats (also called palpitations)
- very slow pulse
- sensation of fullness in the head
- tingling in the hands or feet.
These are very serious side effects. You may need urgent medical attention. Serious side effects are rare.
Tell your doctor or nurse if you notice anything else that is making you feel unwell. Other side effects not listed above may also occur in some patients.
Do not be alarmed by this list of possible side effects. You may not experience any of them.
After receiving Phenylephrine BNM
Storage
Phenylephrine BNM should only be given to you in hospital. It will be stored in a cool dry place away from the light, where the temperature stays below 25°C.
The ampoules should not be taken out of the box until just before they are to be used. This is because the medicine is affected by light.
Disposal
Any Phenylephrine BNM which has passed its expiry date, or is left in the container after use, will be disposed of in a safe manner by your doctor, nurse or pharmacist.
This is not all the information available on Phenylephrine BNM.
If you have any more questions or are not sure about anything, ask your doctor of pharmacist.
Product description
What it looks like
Phenylephrine BNM is a clear colourless sterile solution in a glass ampoule.
It is available in glass ampoules of 5 mL in pack size of 10 ampoules per carton.
Ingredients
Active ingredient:
- phenylephrine hydrochloride
Inactive ingredients:
- sodium chloride
- hydrochloric acid
- water for injections.
The solution is preservative free and sulfite free.
Sponsor details
Boucher & Muir Pty Ltd
Level 9, 76 Berry Street
North Sydney NSW 2060
AUST R 294004
Date of preparation
This leaflet was prepared on 4 October 2018
Brand Information
| Brand name | Phenylephrine BNM |
| Active ingredient | Phenylephrine hydrochloride |
| Schedule | S4 |
MIMS Revision Date: 01 July 2019
1 Name of Medicine
Phenylephrine hydrochloride.
2 Qualitative and Quantitative Composition
Each 1 mL solution of phenylephrine hydrochloride injection 0.1 mg/mL (0.01%) contains 0.1 mg phenylephrine hydrochloride.
Each 5 mL ampoule contains 0.5 mg phenylephrine hydrochloride as well as 45 mg sodium chloride (equivalent to 17.7 mg sodium).
For the full list of excipients, see Section 6.1 List of Excipients.
The solution is preservative free and sulfite free.
3 Pharmaceutical Form
Phenylephrine BNM is a clear, colourless, aqueous solution, free from visible particulates, in sterile form for parenteral injection. pH 3.0 - 5.0; Osmolarity: 270 to 300 mOsm/L.
4 Clinical Particulars
4.1 Therapeutic Indications
Phenylephrine hydrochloride is intended for the maintenance of an adequate level of blood pressure during spinal and inhalation anaesthesia. It is also employed to overcome paroxysmal supraventricular tachycardia.
4.2 Dose and Method of Administration
Phenylephrine BNM solution for injection 0.1 mg/mL (0.01%) is for slow intravenous injection. Phenylephrine BNM is not for subcutaneous or intramuscular administration.
Phenylephrine BNM contains no antimicrobial preservative. It is for use in one patient on one occasion only. Discard any residue.
It should only be administered by healthcare professionals with appropriate training and relevant experience.
The dose should be adjusted according to the pressor response.
Mild or moderate hypotension. Intravenously. Usual dose, 0.2 mg. Range, from 0.1 mg to 0.5 mg. Initial dose should not exceed 0.5 mg.
Injections should not be repeated more often than every 10 to 15 minutes. A 0.5 mg intravenous dose should elevate blood pressure for about 15 minutes.
Spinal anaesthesia - hypotension. Phenylephrine BNM solution for injection 0.1 mg/mL (0.01%) is not for subcutaneous or intramuscular administration. If subcutaneous or intramuscular phenylephrine treatment of hypotension during spinal anaesthesia is desired, other brands of phenylephrine are available.
For hypotensive emergencies during spinal anaesthesia, phenylephrine hydrochloride may be injected intravenously, using an initial dose of 0.2 mg. Any subsequent dose should not exceed the previous dose by more than 0.1 mg to 0.2 mg and no more than 0.5 mg should be administered in a single dose.
Paroxysmal supraventricular tachycardia. Rapid intravenous injection (within 20 to 30 seconds) is recommended; the initial dose should not exceed 0.5 mg, and subsequent doses, which are determined by the initial blood pressure response, should not exceed the preceding dose by more than 0.1 mg to 0.2 mg, and should never exceed 1 mg.
4.3 Contraindications
Phenylephrine hydrochloride should not be used in patients with severe hypertension, ventricular tachycardia, or in patients who are hypersensitive to it.
4.4 Special Warnings and Precautions for Use
General. Phenylephrine hydrochloride should be employed only with extreme caution in patients with hyperthyroidism, bradycardia, partial heart block, myocardial disease, or severe arteriosclerosis.
Use in labour and delivery. If used in conjunction with oxytocic medicines, the pressor effect of sympathomimetic pressor amines is potentiated. Therefore, if vasopressor drugs are used to correct hypotension, the obstetrician should be cautioned that some oxytocic drugs may cause severe persistent hypertension and that even a rupture of a cerebral blood vessel may occur during the postpartum period.
Use in the elderly. Phenylephrine hydrochloride should be employed only with extreme caution in elderly patients.
Paediatric use. The safety and efficacy of Phenylephrine BNM solution for injection 0.1 mg/mL (0.01%) in children have not been established. No data are available.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Vasopressors, particularly metaraminol, may cause serious cardiac arrhythmias during halothane anaesthesia and therefore should be used only with great caution or not at all.
Oxytocic medicines. The pressor effect of sympathomimetic pressor amines is potentiated (see Section 4.4 Special Warnings and Precautions for Use).
MAO inhibitors. The pressor effect of sympathomimetic pressor amines is markedly potentiated in patients receiving monoamine oxidase inhibitors (MAOI). Therefore, when initiating pressor therapy in these patients, the initial dose should be small and used with due caution. The pressor response of adrenergic agents may also be potentiated by tricyclic antidepressants.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. No data available.
Use in pregnancy. (Category B2)
Animal reproduction studies have not been conducted with phenylephrine hydrochloride. It is also not known whether phenylephrine hydrochloride can cause foetal harm when administered to a pregnant woman or can affect reproduction capacity. Data from animal studies show administration of phenylephrine during late pregnancy or labour may cause foetal hypoxia and bradycardia by increasing contractility of the uterus and decreasing uterine blood flow.
From human data, phenylephrine, when administered during labour or delivery, does not appear to influence Apgar scores. Phenylephrine hydrochloride should be given to a pregnant woman only if clearly needed.
Studies in animals are inadequate or may be lacking, but available data show no evidence of an increased occurrence of foetal damage.
Use in lactation. It is not known whether this medicine is excreted in human milk. Because many medicines are excreted in human milk, caution should be exercised when phenylephrine hydrochloride is administered to a nursing woman.
4.7 Effects on Ability to Drive and Use Machines
The effects of this medicine on a person's ability to drive and use machines were not assessed as part of its registration.
4.8 Adverse Effects (Undesirable Effects)
Headache, reflex bradycardia, excitability, restlessness, and rarely arrhythmias.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
Overdosage may induce ventricular extrasystoles and short paroxysms of ventricular tachycardia, a sensation of fullness in the head and tingling of the extremities. Should an excessive elevation of blood pressure occur, it may be immediately relieved by an α-adrenergic blocking agent, e.g. phentolamine.
The oral LD50 in the rat is 350 mg/kg, in the mouse 120 mg/kg.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Phenylephrine hydrochloride is a synthetic sympathomimetic agent.
Phenylephrine hydrochloride produces vasoconstriction that lasts longer than that of adrenaline and ephedrine. Responses are more sustained than those to adrenaline, lasting 20 minutes after intravenous and as long as 50 minutes after subcutaneous injection. Its action on the heart contrasts sharply with that of adrenaline and ephedrine, in that it slows the heart rate and increases the stroke output producing no disturbance in the rhythm of the pulse.
Phenylephrine hydrochloride is a powerful postsynaptic alpha-receptor stimulant with little effect on the beta-receptors of the heart. In therapeutic doses, it produces little if any stimulation of either the spinal cord or cerebrum. A singular advantage of this drug is the fact that repeated injections produce comparable effects.
The predominant actions of phenylephrine hydrochloride are on the cardiovascular system. Parenteral administration causes a rise in systolic and diastolic pressures in man and other species. Accompanying the pressor response to phenylephrine hydrochloride is a marked reflex bradycardia that can be blocked by atropine; after atropine, large doses of phenylephrine hydrochloride increase the heart rate only slightly. In man, cardiac output is slightly decreased, and peripheral resistance is considerably increased. Circulation time is slightly prolonged, and venous pressure is slightly increased; venous constriction is not marked. Most vascular beds are constricted; renal splanchnic, cutaneous, and limb blood flows are reduced but coronary blood flow is increased. Pulmonary vessels are constricted, and pulmonary arterial pressure is raised.
The drug is a powerful vasoconstrictor, with properties very similar to those of norepinephrine but almost completely lacking the chronotropic and inotropic actions on the heart. Cardiac irregularities are seen only very rarely even with large doses.
Clinical trials. No data available.
5.2 Pharmacokinetic Properties
No data available.
5.3 Preclinical Safety Data
Genotoxicity. No long-term animal studies have been performed to evaluate the potential of phenylephrine hydrochloride in this area.
Carcinogenicity. No long-term animal studies have been performed to evaluate the potential of phenylephrine hydrochloride in this area.
6 Pharmaceutical Particulars
6.1 List of Excipients
Phenylephrine BNM contains sodium chloride, hydrochloric acid and water for injections.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C.
Protect from light.
6.5 Nature and Contents of Container
Phenylephrine BNM solution for injection 0.1 mg/mL (0.01%) is available in 5 mL glass ampoules. It is supplied in packs of 10 ampoules per carton.
Each 5 mL ampoule contains 0.5 mg phenylephrine hydrochloride.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
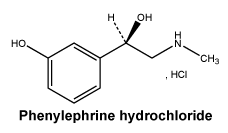
Chemically, phenylephrine hydrochloride is (-)-m-Hydroxy-a-[(methylamino) methyl] benzyl alcohol hydrochloride. It is a white or almost white, crystalline powder, freely soluble in water and in alcohol.
Molecular formula: C9H13NO2.HCl.
Molecular weight: 203.7.
Chemical structure. The chemical structure for phenylephrine hydrochloride is shown.
7 Medicine Schedule (Poisons Standard)
S4.
Date of First Approval
04 October 2018
Date of Revision
21 May 2019
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.