Physeptone Tablets
Brand Information
| Brand name | Physeptone Tablets |
| Active ingredient | Methadone hydrochloride |
| Schedule | S8 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Physeptone Tablets.
Summary CMI
PHYSEPTONE tablets
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
WARNING: Important safety information is provided in a boxed warning in the full CMI. Read before using this medicine.
1. Why am I using PHYSEPTONE tablets?
PHYSEPTONE tablets contain the active ingredient methadone (as methadone hydrochloride). PHYSEPTONE is used for the relief of chronic, moderate to severe pain.
For more information, see Section 1. Why am I using PHYSEPTONE tablets? in the full CMI.
2. What should I know before I use PHYSEPTONE tablets?
Do not use if you have ever had an allergic reaction to methadone, any other opioids, or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I use PHYSEPTONE tablets? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with PHYSEPTONE tablets and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use PHYSEPTONE tablets?
- The usual dose for adults is half to one tablet taken 2 to 3 times a day, but this dosage may be adjusted by your doctor.
- Swallow the tablets with a glass of water.
- Do not stop taking PHYSEPTONE or change the dose without first checking with your doctor.
More instructions can be found in Section 4. How do I use PHYSEPTONE tablets? in the full CMI.
5. What should I know while using PHYSEPTONE tablets?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Drinking alcohol |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using PHYSEPTONE tablets? in the full CMI.
6. Are there any side effects?
Common side effects of PHYSEPTONE tablets include drowsiness, dizziness, light-headedness, nausea, vomiting, dry mouth, sweating, confusion, constipation, problems with urine flow, and tolerance and dependence. With prolonged use, a sudden decrease in dose or interruption of therapy may result in withdrawal symptoms. Serious side effects are associated with an allergic reaction. Symptoms of this include wheezing, swelling of the lips/mouth, difficulty breathing, hay fever, lumpy rash (hives), and fainting.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
WARNING
Limitations of use
PHYSEPTONE should only be given when your doctor decides that other treatment options are not able to effectively manage your pain or you cannot tolerate them.
Hazardous and harmful use
PHYSEPTONE poses risks of abuse, misuse and addiction which can lead to overdose and death. Your doctor will monitor you regularly during treatment.
Life threatening respiratory depression
PHYSEPTONE can cause life-threatening or fatal breathing problems (slow, shallow, unusual or no breathing) even when used as recommended. These problems can occur at any time during use, but the risk is higher when first starting PHYSEPTONE and after a dose increase, if you are older, or have an existing problem with your lungs. Your doctor will monitor you and change the dose as appropriate.
Use of other medicines while being given PHYSEPTONE
Using PHYSEPTONE with other medicines that can make you feel drowsy such as sleeping tablets (e.g. benzodiazepines), other pain relievers, antihistamines, antidepressants, antipsychotics, gabapentinoids (e.g. gabapentin and pregabalin), cannabis and alcohol may result in severe drowsiness, decreased awareness, breathing problems, coma and death. Your doctor will minimise the dose and duration of use; and monitor you for signs and symptoms of breathing difficulties and sedation. You must not drink alcohol while being given PHYSEPTONE.
PHYSEPTONE tablets
Active ingredient: methadone hydrochloride
Consumer Medicine Information (CMI)
This leaflet provides important information about using PHYSEPTONE tablets.
You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using PHYSEPTONE tablets.
Where to find information in this leaflet:
1. Why am I using PHYSEPTONE tablets?
2. What should I know before I use PHYSEPTONE tablets?
3. What if I am taking other medicines?
4. How do I use PHYSEPTONE tablets?
5. What should I know while using PHYSEPTONE tablets?
6. Are there any side effects?
7. Product details
1. Why am I using PHYSEPTONE tablets?
PHYSEPTONE tablets contain the active ingredient methadone, as methadone hydrochloride. Methadone belongs to a group of medicines called opioid analgesics.
PHYSEPTONE tablets are used for the relief of chronic, moderate to severe pain.
Ask your doctor if you have any questions about why PHYSEPTONE tablets have been prescribed for you.
Your doctor may have prescribed it for another reason.
2. What should I know before I use PHYSEPTONE tablets?
Warnings
Addiction
You can become addicted to PHYSEPTONE tablets even if you are given it exactly as prescribed. PHYSEPTONE tablets may become habit forming causing mental and physical dependence. If abused, it may become less able to reduce pain.
Dependence
As with all other opioid containing products, your body may become used to you being given this medicine. Using it may result in physical dependence. Physical dependence means that you may experience withdrawal symptoms if you stop using PHYSEPTONE tablets suddenly, so it is important to take it exactly as directed by your doctor.
Tolerance
Tolerance to PHYSEPTONE tablets may develop, which means that the effect of the medicine may decrease. If this happens, more may be needed to maintain the same effect.
Withdrawal
Continue taking your medicine for as long as your doctor tells you.
If you stop using this medicine suddenly, your pain may worsen, and you may experience some or all the following withdrawal symptoms:
- nervousness, restlessness, agitation, trouble sleeping or anxiety
- body aches, weakness or stomach cramps
- loss of appetite, nausea, vomiting or diarrhoea
- increased heart rate, breathing rate or pupil size
- watery eyes, runny nose, chills or yawning
- increased sweating.
PHYSEPTONE given to the mother during labour can cause breathing problems and signs of withdrawal in the newborn.
Do not take PHYSEPTONE tablets if:
- you are allergic to methadone hydrochloride, any other opioid drug, or any of the ingredients listed at the end of this leaflet.
- Some symptoms of an allergic reaction may include shortness of breath, wheezing or difficulty in breathing; swelling of the face, lips, tongue, or any other parts of the body; rash, itching or hives on the skin. - you are taking or have recently taken antidepressants of the type called monoamine oxidase inhibitors (MAOIs).
- the expiry date printed on the pack has passed.
- the packaging is torn or shows signs of tampering
- you have any of the following medical conditions:
- a lung disorder such as asthma, or any illness causing difficulty in breathing, especially if there is excessive phlegm or skin is bluish in colour.
- a recent head injury, or increased pressure in the head.
- a bowel condition known as ulcerative colitis.
- certain liver or kidney conditions.
- certain heart conditions.
- alcoholism.
- biliary and renal tract spasm.
Check with your doctor if you:
- are allergic to any other medicines, or any other substances, such as foods, preservatives, or dyes.
- have any other medical conditions, especially the following:
- hormone problems
- diabetes
- prostate disease
- phaeochromocytoma, a rare tumour of the adrenal gland. Symptoms include bouts of anxiety and headaches. There may be palpitations (banging of the heart felt in the chest), dizziness, weakness, nausea, vomiting, diarrhoea, dilated pupils, blurry vision, stomach pains and raised blood pressure. - take any other medicines for any other conditions or intend to drink alcohol.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor if you are or intend to become pregnant, are about to give birth, or are breastfeeding.
Use in children
PHYSEPTONE tablets are not recommended for use in children less than 18 years of age.
Use in the elderly
The doctor may prescribe a smaller dose in elderly patients.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with PHYSEPTONE tablets and affect how it works. These include:
- some antidepressant medicines (including some SSRIs, MAOIs, and tricyclic antidepressants)
- some antiviral medicines
- other drugs that may have a sedative effect
- diuretics
- laxatives
- fluconazole
- rifampicin
- phenytoin
- carbamazepine
- St John's Wort.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect PHYSEPTONE tablets.
4. How do I use PHYSEPTONE tablets?
How much to take
- The usual dose for adults is half to one tablet taken 2 to 3 times a day, but this dosage may be adjusted by your doctor.
- Do not take more than the recommended dose.
It can result in low blood sugar and other side effects.
How to take it
Swallow the tablets with a glass of water.
How long to take it for
Do not stop taking PHYSEPTONE tablets or change the dose without first checking with your doctor.
If you forget to use it
If you forget to take a dose, take it as soon as you remember and then go on as before, but remember not to take the tablets more often than recommended by your doctor.
If you take too much (overdose)
If you know that you or someone else have taken too many PHYSEPTONE tablets, urgent medical attention may be needed.
Keep the person awake by talking to them or gently shaking them every now and then.
Symptoms of overdose include:
- slow, unusual or difficult breathing
- drowsiness, dizziness or unconsciousness
- slow or weak heartbeat
- nausea, vomiting
- convulsions, fits
- confusion, memory loss
- difficulty walking
- changes in behaviour or personality.
You should immediately:
- phone triple zero (000) for an ambulance, or
- phone the Poisons Information Centre (by calling 13 11 26), or
- contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
Report any other medicine or alcohol which has been taken.
5. What should I know while using PHYSEPTONE tablets?
Things you should do
Tell your doctor if, for any reason, you have not taken your medicine exactly as directed.
Otherwise, your doctor may think that it was not working as it should and change your treatment unnecessarily.
Remind any other doctor, dentist, or pharmacist you visit that you are using PHYSEPTONE tablets.
Things you should not do
Do not give this medicine to anyone else, even if their symptoms seem similar to yours.
Do not use PHYSEPTONE to treat any other complaints unless your doctor says to.
Things to be careful of
Particular care should be taken when starting on treatment with PHYSEPTONE tablets or increasing the dose.
This medicine can decrease heart and breathing rates, which if severe may lead to death.
Speak to your doctor if you have any concerns.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how PHYSEPTONE tablets affect you.
As this medicine may cause drowsiness, it is recommended that you do not drive, use machinery or undertake any activities where alertness is required.
Drinking alcohol
Tell your doctor if you drink alcohol.
It is unwise to drink alcohol while using PHYSEPTONE tablets.
Looking after your medicine
Due to the high potential for abuse, misuse and addiction, it is advisable to store this medicine in a safe place, preferably locked.
Keep this medicine in the original container protected from light, where the temperature stays below 25°C.
Keep it where young children cannot reach it.
Getting rid of any unwanted medicine
If you no longer need to use this medicine or it is out of date, take it to any pharmacy for safe disposal.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
With prolonged use, the dose may have to be increased to achieve the same benefit, whilst a sudden decrease in dose or interruption of therapy may give rise to withdrawal symptoms.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
| Speak to your doctor if you have any of these side effects that may be associated with long-term use. |
Serious side effects
| Serious side effects | What to do |
Allergic reaction including:
| Phone triple zero (000) for an ambulance, call your doctor straight away or go to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What PHYSEPTONE tablets contain
| Active ingredient (main ingredient) |
|
| Other ingredients (inactive ingredients) |
|
| Potential allergens |
|
Do not take this medicine if you are allergic to any of these ingredients.
What PHYSEPTONE tablets look like
PHYSEPTONE tablets are white, uncoated, round, biconvex tablets, scored on one side. Available in blister packs of 20 tablets.
Australian Registration number: AUST R 76083
Who distributes PHYSEPTONE tablets
Aspen Pharmacare Australia Pty Ltd
34-36 Chandos St
St Leonards NSW 2065
Australia
This leaflet was revised in August 2025.
Brand Information
| Brand name | Physeptone Tablets |
| Active ingredient | Methadone hydrochloride |
| Schedule | S8 |
MIMS Revision Date: 01 October 2025
Hazardous and harmful use. Physeptone poses risks of hazardous and harmful use which can lead to overdose and death. Assess the patient's risk of hazardous and harmful use before prescribing and monitor the patient regularly during treatment (see Section 4.4 Special Warnings and Precautions for Use).
Life threatening respiratory depression. Serious, life-threatening or fatal respiratory depression may occur with the use of Physeptone. Be aware of situations which increase the risk of respiratory depression, modify dosing in patients at risk and monitor patients closely, especially on initiation or following a dose increase (see Section 4.4 Special Warnings and Precautions for Use).
Concomitant use of benzodiazepines and other central nervous system (CNS) depressants, including alcohol. Concomitant use of opioids with benzodiazepines, gabapentinoids, antihistamines, tricyclic antidepressants, antipsychotics, cannabis or other central nervous system (CNS) depressants, including alcohol, may result in profound sedation, respiratory depression, coma, and death. Limit dosages and durations to the minimum required; and monitor patients for signs and symptoms of respiratory depression and sedation. Caution patients not to drink alcohol while taking Physeptone.
1 Name of Medicine
Methadone hydrochloride.
2 Qualitative and Quantitative Composition
Methadone hydrochloride is a synthetic opioid analgesic with the general properties of morphine.
Physeptone tablets contain methadone hydrochloride 10 mg.
List of excipients with known effect. Lactose monohydrate.
Physeptone injection vials contain methadone hydrochloride 10 mg/1 mL (preservative free).
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Physeptone tablets. White, biconvex scored tablet on one side and plain on the other.
Physeptone injection. A clear, colourless solution free of particulate matter.
4 Clinical Particulars
4.1 Therapeutic Indications
Physeptone is indicated for the management of severe pain where:
other treatment options have failed, are contraindicated, not tolerated or are otherwise inappropriate to provide sufficient management of pain; and
the pain is opioid-responsive; and
requires daily, continuous, long-term treatment.
Physeptone is not indicated for use in chronic non-cancer pain other than in exceptional circumstances.
Physeptone is not indicated as an as-needed (PRN) analgesia.
Physeptone is not recommended for use in ambulant patients.
4.2 Dose and Method of Administration
Adults. Usual single dose 5-10 mg by mouth, subcutaneous or intramuscular injection.
Owing to its long plasma half-life, caution with repeated dosage should be observed in the very ill or elderly. The usual initial dose should be 5-10 mg 6-8 hourly, later adjusted to the degree of pain relief obtained. Doses administered more frequently than 6- to 8-hourly are liable to cause accumulation with increasing sedation and respiratory depression. In chronic use Physeptone should not be administered more than twice daily.
Methadone may be used in combination with non-narcotic analgesics to provide additive analgesia.
Where the drug is given orally for the control of pain associated with a chronic condition, it is wise to restrict the dose to the smallest amount which adequately controls the symptoms.
Physeptone has less hypnotic effect than morphine. If it is necessary to give a patient a potent analgesic for a prolonged period, some increase in dose may be necessary.
Children and adolescents less than 18 years of age. Physeptone is not recommended for use in this age group since documented clinical experience has been insufficient to establish a suitable dosage regimen. Furthermore, children are particularly sensitive to the respiratory and central nervous system depressant effects of methadone.
4.3 Contraindications
Physeptone, like other opioids, is contraindicated in patients with severe respiratory disease, acute respiratory disease and respiratory depression, especially in the presence of cyanosis and excessive bronchial secretions, and obstructive airways disease.
Physeptone should not be given during an attack of bronchial asthma.
Concurrent administration with monoamine oxidase inhibitors, or within 2 weeks of discontinuation of treatment with them.
Obstetric use is not recommended.
Physeptone is contraindicated in individuals who are hypersensitive to methadone.
Physeptone is contraindicated in the presence of acute alcoholism, head injury and raised intracranial pressure.
Physeptone, as with other opioids, is contraindicated in patients with ulcerative colitis, since it may precipitate toxic dilatation or spasm of the colon.
As with all narcotic analgesics, Physeptone should not be administered to patients with severe hepatic impairment as it may precipitate hepatic encephalopathy.
At the recommended dosages, Physeptone is contraindicated in biliary and renal tract spasm.
Methadone is contraindicated in individuals with existing QT prolongation, including those with congenital long QT syndrome (see Section 4.4 Special Warnings and Precautions for Use).
4.4 Special Warnings and Precautions for Use
Hazardous and harmful use. Physeptone contains the opioid methadone and is a potential drug of abuse, misuse and addiction. Addiction can occur in patients appropriately prescribed Physeptone at recommended doses. The possibility of addiction cannot be excluded and patients should be reminded of the necessity of adhering to the prescribed dosage. However, when used for pain relief in terminal care, the risk of dependence is of limited concern.
The risk of addiction is increased in patients with a personal or family history of substance abuse (including alcohol and prescription and illicit drugs) or mental illness. The risk also increases the longer the drug is used and with higher doses. Patients should be assessed for their risks for opioid abuse or addiction prior to being prescribed Physeptone.
All patients receiving opioids should be routinely monitored for signs of misuse and abuse. Opioids are sought by people with addiction and may be subject to diversion. Strategies to reduce these risks include prescribing the drug in the smallest appropriate quantity and advising the patient on the safe storage and proper disposal of any unused drug (see Section 6.4 Special Precautions for Storage; Section 6.6 Special Precautions for Disposal). Caution patients that abuse of oral or transdermal forms of opioids by parenteral administration can result in serious adverse events, which may be fatal.
Patients should be advised not to share Physeptone with anyone else.
Respiratory depression. Deaths due to cardiac arrhythmias and respiratory depression may occur, particularly in patients receiving methadone for analgesia during treatment initiation or conversion from other opioids.
Serious, life-threatening or fatal respiratory depression can occur with the use of opioids even when used as recommended. The peak depressive effects persist longer than peak analgesic effects, especially during the initial dosing period. It can occur at any time during the use of Physeptone but the risk is greatest during initiation of therapy or following an increase in dose. Patients should be monitored closely for respiratory depression at these times. The risk of life-threatening respiratory depression is also higher in elderly, frail, or debilitated patients, in patients with existing impairment of respiratory function (e.g. chronic obstructive pulmonary disease; asthma) and in patients with hepatic or hepatic impairment (see Use in hepatic impairment and Use in renal impairment). Opioids should be used with caution and with close monitoring in these patients (see Section 4.2 Dose and Method of Administration). The use of opioids is contraindicated in patients with severe respiratory disease, acute respiratory disease and respiratory depression (see Section 4.3 Contraindications).
The risk of respiratory depression is greater with the use of high doses of opioids, especially high potency and modified release formulations, and in opioid naive patients. Initiation of opioid treatment should be at the lower end of the dosage recommendations with careful titration of doses to achieve effective pain relief.
Careful calculation of equianalgesic doses is required when changing opioids or switching from immediate release to modified release formulations, together with consideration of pharmacological differences between opioids. Consider starting the new opioid at a reduced dose to account for individual variation in response.
Children are very sensitive to the depressant effects of methadone.
Tolerance, dependence and withdrawal. Neuroadaptation of the opioid receptors to repeated administration of opioids can produce tolerance and physical dependence. Tolerance is the need for increasing doses to maintain analgesia. Tolerance may occur to both the desired and undesired effects of the opioid. Physical dependence, which can occur after several days to weeks of continued opioid usage, results in withdrawal symptoms if the opioid is ceased abruptly or the dose is significantly reduced. Withdrawal symptoms can also occur following the administration of an opioid antagonist (e.g. naloxone) or partial agonist (e.g. buprenorphine). Withdrawal can result in some or all of the following symptoms: dysphoria, restlessness/agitation, lacrimation, rhinorrhoea, yawning, sweating, chills, myalgia, mydriasis, irritability, anxiety, increasing pain, backache, joint pain, weakness, abdominal cramps, insomnia, nausea, anorexia, vomiting, diarrhoea, increased blood pressure, increased respiratory rate and increased heart rate. When discontinuing Physeptone in a person who may be physically-dependent, the drug should not be ceased abruptly but withdrawn by tapering the dose gradually (see Ceasing opioids and see Section 4.2 Dose and Method of Administration).
Risks from concomitant use of benzodiazepines or other CNS depressants, including alcohol. Concomitant use of opioids and benzodiazepines or other CNS depressants, including alcohol, may result in sedation, respiratory depression, coma and death. Because of these risks, concomitant prescribing of Physeptone with CNS depressant medicines, such as other opioid analgesics, benzodiazepines, gabapentinoids, cannabis, sedatives, hypnotics, tricyclic antidepressants, antipsychotics, antihistamines, centrally-active anti-emetics and other CNS depressants, should be reserved for patients for whom other treatment options are not possible. If a decision is made to prescribe Physeptone concomitantly with any of the medicines, the lowest effective dose should be used, and the duration of treatment should be as short as possible. Patients should be followed closely for signs and symptoms of respiratory depression and sedation. Patients and their caregivers should be made aware of these symptoms. Patients and their caregivers should also be informed of the potential harms of consuming alcohol while taking Physeptone.
Use of opioids in chronic (long-term) non-cancer pain (CNCP). Opioid analgesics have an established role in the treatment of acute pain, cancer pain and palliative and end-of-life care. Current evidence does not generally support opioid analgesics in improving pain and function for most patients with chronic non-cancer pain. The development of tolerance and physical dependence and risks of adverse effects, including hazardous and harmful use, increase with the length of time a patient takes an opioid. The use of opioids for long-term treatment of CNCP is not recommended.
The use of an opioid to treat CNCP should only be considered after maximised nonpharmacological and non-opioid treatments have been tried and found ineffective, not tolerated or otherwise inadequate to provide sufficient management of pain. Opioids should only be prescribed as a component of comprehensive multidisciplinary and multimodal pain management.
Opioid therapy for CNCP should be initiated as a trial in accordance with clinical guidelines and after a comprehensive biopsychosocial assessment has established a cause for the pain and the appropriateness of opioid therapy for the patient (see Hazardous and harmful use, above). The expected outcome of therapy (pain reduction rather than complete abolition of pain, improved function and quality of life) should be discussed with the patient before commencing opioid treatment, with agreement to discontinue treatment if these objectives are not met.
Owing to the varied response to opioids between individuals, it is recommended that all patients be started at the lowest appropriate dose and titrated to achieve an adequate level of analgesia and functional improvement with minimum adverse reactions. Immediate-release products should not be used to treat chronic pain, but may be used for a short period in opioid-naïve patients to develop a level of tolerance before switching to a modified-release formulation. Careful and regular assessment and monitoring is required to establish the clinical need for ongoing treatment. Discontinue opioid therapy if there is no improvement of pain and/or function during the trial period or if there is any evidence of misuse or abuse. Treatment should only continue if the trial has demonstrated that the pain is opioid responsive and there has been functional improvement. The patient's condition should be reviewed regularly and the dose tapered off slowly if opioid treatment is no longer appropriate (see Ceasing opioids).
Accidental ingestion/exposure. Accidental ingestion or exposure of Physeptone, especially by children, can result in a fatal overdose of methadone. Patients and their caregivers should be given information on safe storage and disposal of unused Physeptone (see Section 6.4 Special Precautions for Storage; Section 6.6 Special Precautions for Disposal).
Hyperalgesia. Hyperalgesia may occur with the use of opioids, particularly at high doses. Hyperalgesia may manifest as an unexplained increase in pain, increased levels of pain with increasing opioid dosages or diffuse sensitivity not associated with the original pain. Hyperalgesia should not be confused with tolerance (see Tolerance, dependence and withdrawal). If opioid induced hyperalgesia is suspected, the dose should be reduced and tapered off if possible. A change to a different opioid may be required.
Ceasing opioids. Abrupt discontinuation or rapid decreasing of the dose in a person physically dependent on an opioid may result in serious withdrawal symptoms and uncontrolled pain (see Tolerance, dependence and withdrawal). Such symptoms may lead the patient to seek other sources of licit or illicit opioids. Opioids should not be ceased abruptly in a patient who is physically dependent but withdrawn by tapering the dose slowly. Factors to take into account when deciding how to discontinue or decrease therapy include the dose and duration of the opioid the patient has been taking, the type of pain being treated and the physical and psychological attributes of the patient. A multimodal approach to pain management should be in place before initiating an opioid analgesic taper. During tapering, patients require regular review and support to manage any increase in pain, psychological distress and withdrawal symptoms. There are no standard tapering schedules suitable for all patients and an individualised plan is necessary. In general, tapering should involve a dose reduction of no more than 10 percent to 25 percent every 2 to 4 weeks (see Section 4.2 Dose and Method of Administration). If the patient is experiencing increased pain or serious withdrawal symptoms, it may be necessary to go back to the previous dose until stable before proceeding with a more gradual taper.
When ceasing opioids in a patient who has a suspected opioid use disorder, the need for medication assisted treatment and/or referral to a specialist should be considered.
Physeptone should be used with caution in the presence of the following: hypothyroidism; adrenocortical insufficiency; hypopituitarism; prostatic hypertrophy; shock; diabetes mellitus.
Extreme caution should be exercised when administering Physeptone to patients with phaeochromocytoma, since aggravated hypertension has been reported in association with diamorphine.
In vivo and in vitro studies have demonstrated that methadone inhibits cardiac potassium channels and prolongs cardiac repolarisation (i.e. prolongs the QT interval). QT interval prolongation and serious arrhythmia (Torsade de Pointes) have been observed during treatment with methadone and appear to be more common with higher doses. Particular caution and careful monitoring is recommended in patients at risk of prolonged QT interval (e.g. cardiac hypertrophy, concomitant diuretic use, hypokalaemia, hypomagnesaemia), patients with a previous history of cardiac repolarisation prolongation, those taking medications affecting cardiac repolarisation or methadone metabolism, and in patients with an increased risk of arrhythmia (see Section 4.3 Contraindications; Section 4.5 Interactions with Other Medicines and Other Forms of Interactions). Patients developing QT prolongation while on methadone treatment should be evaluated for modifiable risk factors, such as concomitant medications with cardiac effects, drugs which might cause electrolyte abnormalities, and drugs which might act as inhibitors of methadone metabolism.
Cardiac repolarisation disorders. Methadone should be administered with particular caution to patients at risk for development of prolonged QT interval (see Section 4.4 Special Warnings and Precautions for Use; Section 4.3 Contraindications).
Hypoglycaemia. Hypoglycaemia has been observed in the context of methadone overdose or dose escalation. Regular monitoring of blood sugar is recommended during dose escalation (see Section 4.8; Section 4.9).
Adrenal insufficiency. Opioid analgesics may cause reversible adrenal insufficiency requiring monitoring and glucocorticoid replacement therapy. Symptoms of adrenal insufficiency may include nausea, vomiting, loss of appetite, fatigue, weakness, dizziness or low blood pressure.
Decreased sex hormone and increased prolactin. Long term use of opioid analgesics maybe associated with decreased sex hormone levels and increased prolactin. Symptoms include decreased libido, impotence or amenorrhea.
Sleep-related breathing disorders. Opioids can cause sleep-related breathing disorders including central sleep apnoea (CSA) and sleep-related hypoxemia. Opioid use increases the risk of CSA in a dose-dependent fashion. In patients who present with CSA, consider decreasing the total opioid dosage.
Neonatal withdrawal syndrome. Chronic use of methadone by the mother at the end of pregnancy may result in a withdrawal syndrome (e.g. hypertonia, neonatal tremor, neonatal agitation, myoclonus, convulsions, apnoea or bradycardia) in the neonate. In many reported cases the withdrawal was serious and required treatment. The syndrome is generally delayed for several hours to several days after birth. (See Section 4.6, Use in pregnancy).
Hepatobiliary disorders. Opioids may cause dysfunction and spasm of the sphincter of Oddi, thus raising intrabiliary pressure and increasing the risk of biliary tract symptoms and pancreatitis. Therefore, Physeptone has to be administered with caution in patients with pancreatitis and diseases of the biliary tract.
Gastrointestinal toxicity. Reports of significant oesophageal dysfunction have been observed via high-resolution manometry in patients taking opioid medicines on a long-term basis. Discontinuation or weaning of opioids should be considered in patients presenting with oesophageal complaints including but not limited to dysphagia, regurgitation, or non-cardiac chest pain.
Use in hepatic impairment. Particular care should be taken when methadone is to be used in patients with hepatic impairment as these patients metabolise methadone more slowly than normal patients. Where not contraindicated methadone should be given at less than the normal recommended dose and the patient's response used as a guide to further dosage requirements (see Section 4.3 Contraindications).
Use in renal impairment. Methadone should be used with caution in patients with renal dysfunction. The dosage interval should be increased to a minimum of 8-hourly when the glomerular filtration rate (GFR) is 10 to 50 mL/minute and to a minimum of 12-hourly when the GFR is below 10 mL/minute.
Use in the elderly. Methadone has a long plasma half life which may lead to accumulation, particularly if renal function is impaired (see Use in renal impairment).
In common with other opioids, methadone may cause confusion in this age group, therefore careful monitoring is advised.
Paediatric use. Methadone is not recommended for use in children less than 18 years of age since documented clinical experience has been insufficient to establish a suitable dosage regimen; furthermore, children are particularly sensitive to the respiratory and central nervous system effects of methadone.
Effects on laboratory tests. The serum BSP retention test may be increased (hepatotoxic effect or spasm of sphincter of Oddi). Plasma cortisol may be increased in response to cold to an extent not seen in controls. An increase in the serum albumin, prolactin and immunoglobulin IgG levels may be seen as a response to chronic administration. A significant decrease in serum indocyanine green level has been observed in a small series of patients with normal liver function tests. PCO2 may be increased due to decreased pulmonary ventilation. False positive urine pregnancy tests have occurred, mainly with the Gravindex test. Physiological changes in thyroid hormones may be seen - decrease in serum thyroxine (T4), a decrease in free thyroxine and an increase in triiodothyronine (T3).
4.5 Interactions with Other Medicines and Other Forms of Interactions
Methadone is metabolised by various cytochrome P450 (CYP450) enzymes. Therefore, coadministration of drugs known to interfere with CYP450 enzymes may affect its clinical activity.
Some compounds may increase the metabolism of methadone, e.g. rifampicin, phenytoin, carbamazepine, St. John's wort, and antiretroviral agents used in the treatment of HIV infection (particularly nevirapine, efavirenz and some protease inhibitors). This has the potential to result in withdrawal symptoms.
Patients who are also taking enzyme inducers such as carbamazepine, may require higher than typical doses of methadone.
Some compounds may decrease the metabolism of methadone, e.g. fluconazole and some selective serotonin re-uptake inhibitors (SSRIs), particularly fluvoxamine. This may increase the likelihood of methadone toxicity.
In addition to compounds that may decrease the metabolism of methadone, extreme caution is necessary when any drug known to have the potential to prolong the QT interval is prescribed in conjunction with methadone (see Section 4.4 Special Warnings and Precautions for Use). Interactions may occur with methadone and potentially arrhythmogenic agents, such as class I and III antiarrhythmics, some neuroleptics and tricyclic antidepressants, and calcium channel blockers. Caution should also be exercised when prescribing concomitant drugs capable of inducing electrolyte disturbances that may prolong the QT interval (hypomagnesaemia, hypokalaemia). These include diuretics, laxatives and in rare cases mineralocorticoid hormones.
Methadone can also affect the metabolism of other drugs. Plasma concentrations of some drugs may be increased, e.g. nelfinavir, zidovudine, fluconazole and desipramine, whereas concentrations of others may be decreased, e.g. abacavir and amprenavir.
Monoamine oxidase inhibitors (MAOIs) may prolong and enhance the respiratory depressant effects of methadone. Opioids and MAOIs used together may cause fatal hypotension and coma.
The general depressant effects of methadone may be enhanced by other centrally-acting agents such as other opioids, alcohol, antihistamines, antipsychotics, barbiturates, benzodiazepines, cannabis, centrally-acting anti-emetics, gabapentinoids, hypnotics, neuromuscular blocking agents, phenothiazines, sedatives, tricyclic antidepressants, tranquillisers and other CNS depressants (see Section 4.4 Special Warnings and Precautions for Use, Risks from concomitant use of benzodiazepines or other CNS depressants, including alcohol). Some psychotropic drugs, however, may potentiate the analgesic effects of methadone.
Propranolol has been reported to enhance the lethality of toxic doses of opioids in animals. Although the significance of this finding is not known for man, caution should be exercised when such drugs are co-administered.
Opioid analgesics may antagonise the effects of agents that stimulate gastrointestinal motility (metoclopramide, domperidone, cisapride).
Anticholinergics increase the risk of constipation, urinary retention and so on.
Antihypertensives may aggravate the hypotensive effects of opioid analgesics.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. Methadone does not appear to impair human female fertility.
Studies in men on methadone maintenance programs have shown that methadone reduces serum testosterone and markedly depresses the ejaculate volume and sperm motility. The sperm counts of methadone subjects were twice that of controls but this reflected the lack of dilution from seminal secretions. A reduction in libido has been reported as well as impotence, delayed, and/or failed ejaculation.
Use in pregnancy. (Category C)
There is insufficient evidence on which to determine the safety profile of methadone in pregnancy, therefore, it should only be used if the potential benefit outweighs the potential risk.
Narcotic analgesics may cause respiratory depression in the newborn infant. During the last 2-3 hours before expected delivery these products should only be used after weighing the needs of the mother against the risk to the foetus. Methadone is not recommended for use during labour because its prolonged duration of action increases the risk of respiratory depression in the neonate.
Like other opiates, methadone crosses the placenta during pregnancy, and most neonates born to mothers on methadone maintenance will suffer from withdrawal if left untreated.
Withdrawal symptoms may be observed in infants born to mothers receiving methadone treatment consisting of central nervous system, gastrointestinal, and respiratory disturbances. Abstinence syndrome may not occur in the neonate for some days after birth. Therefore, in addition to initial monitoring of respiratory depression, neonates should undergo prolonged monitoring for signs and symptoms of withdrawal.
Infants born to mothers on methadone treatment have been reported to have smaller birth weights when compared to infants of non-drug exposed mothers. The infants born to mothers on methadone treatment were not small for gestational age, and by six months of age, these infants did not exhibit any general development sequelae.
Use in lactation. Caution should be exercised when methadone is administered to a nursing woman due to the risks of sedation and respiratory depression in the infant. Serious harm, including death, has been reported in infants following exposure to methadone through breast feeding.
Breast feeding is permissible in mothers receiving methadone for maintenance therapy but specialist care from obstetric and paediatric staff with experience in such management is required. The baby should be monitored to avoid sedation. Therefore, breast feeding mothers should be counselled on how to identify respiratory depression and sedation in their babies and when it may be necessary to seek immediate medical care. The dose of methadone should be as low as possible.
Methadone is distributed into breast milk, with a mean ratio of milk to plasma concentration of 0.44. However, doses of methadone to the infant via breast milk are low, estimated at 3% of maternal doses, on average, and insufficient to prevent neonatal abstinence syndrome in infants born to mothers on methadone maintenance.
From theoretical considerations methadone is likely to be excreted in breast milk. Withdrawal symptoms can occur in the infant. Assays of breast milk from methadone maintained mothers showed methadone concentrations of 0.17 to 5.6 microgram/mL.
4.7 Effects on Ability to Drive and Use Machines
In common with other opioids, Physeptone may produce orthostatic hypotension and drowsiness in ambulatory patients. They should be cautioned, therefore, against driving vehicles, operating machinery or other activities requiring vigilance.
4.8 Adverse Effects (Undesirable Effects)
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
* Adverse reactions denoted with an asterisk appear to be more common in ambulatory patients and in those receiving oral therapy.
Respiratory. The major side effect of methadone is respiratory depression.
Frequency (not known): central sleep apnoea syndrome.
Gastrointestinal. Reported events include nausea*, vomiting*, dry mouth*, loss of appetite and constipation. Nausea and vomiting appear to be more frequent after oral administration than after injection. Less common reactions include stomach cramps or pain. Methadone, in common with other opioids, may cause spasm of the biliary tract (see Section 4.3 Contraindications).
Frequency (not known): pancreatitis.
Hepatobiliary. Frequency (not known): spasm of sphincter of Oddi.
Neurological. Reported events include dizziness*, drowsiness*, light-headedness*, sweating*, confusion*, weakness, fatigue and low blood pressure. Less common reaction includes blurred vision. Euphoria has been reported at higher doses in tolerant patients. Methadone is reported to produce less euphoria than morphine.
Cardiovascular. Hypotension, collapse, and generalised oedema have occasionally been reported. Less common reactions include bradycardia, tachycardia and palpitations. ECG changes including QT prolongation and Torsade de Pointes have occurred very rarely, usually in patients with risk factors or receiving high doses of methadone (see Section 4.4 Special Warnings and Precautions for Use). In rare cases a hypersensitive subject may react with a sudden transient fall in blood pressure; this is short-lived and self-terminating.
Renal. Methadone, in common with other opioids, may cause spasm of the renal tract (see Section 4.3 Contraindications). It also possesses antidiuretic properties, and urinary retention or hesitancy has been reported.
Endocrine. Prolonged use of methadone in men has been reported to be associated with the development of gynaecomastia. Long term use may also cause decreased libido, impotence and amenorrhea.
Frequency (not known): adrenal insufficiency, androgen deficiency.
Withdrawal (abstinence) syndrome. Chronic use of opioid analgesics may be associated with the development of physical dependence. An abstinence syndrome may be precipitated when opioid administration is suddenly discontinued or opioid antagonists administered. Withdrawal symptoms that may be observed after discontinuation of opioid use include body aches, diarrhoea, piloerection, anorexia, nervousness or restlessness, rhinorrhoea, sneezing, tremors or shivering, abdominal colic, nausea, sleep disturbance, unusual increase in sweating and yawning, weakness, tachycardia and unexplained fever. With appropriate dose adjustments and gradual withdrawal these symptoms are usually mild.
In known drug addicts, Physeptone has produced withdrawal symptoms but these are mild. Tolerance and dependence of the morphine type may occur.
Side effects are more common and more severe in ambulant patients.
Subcutaneous administration may cause local irritation.
Metabolism and nutrition disorders. Frequency (not known): hypoglycaemia.
4.9 Overdose
Toxic leukoencephalopathy has been observed with opioid overdose.
Symptoms. Toxic doses of methadone cause unconsciousness, pin-point pupils, slow shallow respiration, cyanosis and weak pulse, profound respiratory depression, hypotension, circulatory failure and pulmonary oedema, coma and death. Mydriasis may replace miosis as asphyxia intervenes. Drowsiness, floppiness, pin-point pupils and apnoea have been reported in children. Often there is a 2-3 hour delay between ingestion and the appearance of symptoms. Hypoglycaemia has been reported. These symptoms and signs of overdosage parallel those for other opioids.
Treatment. General supportive measures, including ECG monitoring, should be employed as required. Lavage, dialysis and CNS stimulation are contraindicated. The specific opioid antagonist naloxone is the treatment of choice for the reversal of coma and the restoration of spontaneous respiration. Intravenous naloxone should be given and repeated at 5-10 minute intervals to attain full benefit. Intravenous infusion is the preferred route of administration in the management of methadone overdose. Because of the short half-life of naloxone relative to the long half-life of methadone, continuous infusion reduces the possibility of prolonged respiratory depression and the risk of relapse, which can occur suddenly. It should be noted that QT prolongation will not be reversed by naloxone.
In opioid dependent patients the administration of the usual dose of an opioid antagonist will precipitate an acute withdrawal syndrome. The severity of this syndrome will depend on the degree of physical dependence and the dose of the antagonist administered. The use of an opioid antagonist in such a person should be avoided if possible. If it must be used to treat serious respiratory depression in the physically dependent person the antagonist should be administered with extreme care and by titration with smaller than usual doses of the antagonist.
Acidification of the urine will increase the rate of elimination of the drug via the kidney.
Patients should be monitored closely for at least 48 hours after apparent recovery in case of relapse, since the duration of action of the antagonist may be substantially shorter than that of methadone.
The use of other respiratory or central stimulants is not recommended.
Methadone is not dialysable by either peritoneal or haemodialysis.
For information on the management of overdose, contact the Poisons Information Centre for advice on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. The pharmacological actions of methadone are qualitatively similar to those of morphine. Significant quantitative differences are its effective analgesic activity after administration by the oral route, and its tendency to show persistent effects with repeated administration.
Clinical trials. No data available.
5.2 Pharmacokinetic Properties
Absorption. Methadone hydrochloride is readily absorbed after administration by mouth and has high oral bioavailability. Peak plasma concentrations have been reported 1 to 5 hours after oral administration of a single dose in tablet form.
Plasma concentrations have been found to vary widely during methadone maintenance therapy with large differences between patients and wide fluctuations in individual patients. Declining concentrations have been reported during methadone maintenance suggesting that tolerance occurs, possibly as a result of auto-induction of hepatic microsomal enzymes.
Distribution. Methadone undergoes considerable tissue distribution, and protein binding is reported to be 60 to 90% with α1-acid glycoprotein being the main binding protein in plasma.
Metabolism. Metabolism to the major metabolite 2-ethylidine-1,5- dimethyl-3,3- diphenylpyrrolidine and the minor metabolite 2-ethyl-3,3- diphenyl-5-methylpyrrolidine, both of them inactive, occurs in the liver. These metabolites are excreted in the faeces and urine together with unchanged methadone. Other metabolites, including methadol and normethadol (reported to be pharmacologically active), have also been described but account for a small proportion of the dose. The liver may also serve as a major storage site of unchanged methadone which is taken up, bound nonspecifically by the liver and released again mainly unchanged.
Excretion. Methadone has a half-life of about 15 hours after a single dose in nontolerant subjects. After chronic administration the half-life is about 22 hours. However, marked interindividual variations in kinetics have been observed with methadone. Elimination half-lives vary considerably (a range of 15 to 60 hours has been reported) and careful adjustment of dosage is necessary with repeated administration.
5.3 Preclinical Safety Data
Mutagenic potential. Methadone did not exhibit demonstrable mutagenic activity in a wide range of standard in vitro and in vivo mutagenicity assays. However, in a Dominant Lethal assay in mice, treatment with methadone at doses between 1 and 6 mg/kg was associated with increased pre-implantation deaths and chromosomal aberrations of sperm cells when compared with controls.
Genotoxicity/carcinogenicity. Long term carcinogenicity tests in rodents did not reveal any evidence of methadone-related neoplasia.
Teratogenic potential. No teratogenic effects have been observed in standard teratogenicity studies in rats and rabbits given methadone at doses from ten to fifty times the average daily human maintenance dose. Developmental abnormalities of the central nervous system have been reported in hamsters and mice given high doses in early pregnancy.
6 Pharmaceutical Particulars
6.1 List of Excipients
Physeptone tablets contain the inactive ingredients gelatin, glycerol, lactose monohydrate, maize starch and magnesium stearate.
Physeptone injection vials contains water for injections to 1 mL.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C. Store in a dry place. Protect from light.
6.5 Nature and Contents of Container
Physeptone tablets. Clear PVC/Al blister packs of 20 tablets.
Physeptone injection vials. A clear type 1 glass vial. Packs of 5 x 1 mL vials.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Methadone is a racemic mixture and levo-methadone is the active isomer. Methadone occurs as odourless, colourless crystals or white crystalline powder. It is soluble in water, freely soluble in alcohol and chloroform; practically insoluble in ether and in glycerol.
The chemical name for methadone hydrochloride is 6-Dimethylamino-4,4-diphenyl-3-heptanone hydrochloride. Molecular formula: C21H27NO,HCl. Relative molecular mass: 345.9.
Chemical structure.
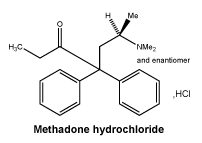
7 Medicine Schedule (Poisons Standard)
S8 - Controlled Drug.
Date of Revision
22 August 2025
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.