Rabeprazole-WGR Tablets
Brand Information
| Brand name | Rabeprazole-WGR Tablets |
| Active ingredient | Rabeprazole sodium |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Rabeprazole-WGR Tablets.
Summary CMI
RABEPRAZOLE-WGR Tablets
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using RABEPRAZOLE-WGR?
RABEPRAZOLE-WGR contains the active ingredient rabeprazole sodium. RABEPRAZOLE-WGR used to used to treat gastro-oesophageal reflux disease (GORD), commonly known as 'reflux'.
For more information, see Section 1. Why am I using RABEPRAZOLE-WGR? in the full CMI.
2. What should I know before I use RABEPRAZOLE-WGR?
Do not use if you have ever had an allergic reaction to rabeprazole sodium or any of the ingredients listed at the end of the CMI. Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I use RABEPRAZOLE-WGR? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with RABEPRAZOLE-WGR and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use RABEPRAZOLE-WGR?
- Use RABEPRAZOLE-WGR exactly as your doctor has prescribed. The dose of RABEPRAZOLE-WGR tablets is usually 20 mg but may vary from 10 mg to 40 mg per day depending on what condition you are being treated for and how severe it is.
- The usual dose is one tablet, to be taken once daily at the same time each day. Always swallow RABEPRAZOLE-WGR tablets whole.
More instructions can be found in Section 4. How do I use RABEPRAZOLE-WGR? in the full CMI.
5. What should I know while using RABEPRAZOLE-WGR?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using rabeprazole sodium? in the full CMI.
6. Are there any side effects?
RABEPRAZOLE-WGR is usually well tolerated but tell your doctor or pharmacist as soon as possible if you do not feel well while you are taking RABEPRAZOLE-WGR. The common side effects include headache, dizziness, diarrhoea, nausea, abdominal pain, wind, vomiting, constipation, runny or block nose, sore throat, cough, non-specific pain, back pain, muscle pain, rash, muscle weakness, physical weakness or lack of energy, flu-like syndrome, infection, insomnia, and chest pain. The serious side effects include allergic reactions; frequent infections; urinary tract infection, vision or taste disturbance, depression, feeling dizzy, faint, lightheaded or weak (hypotension), pain or indigestion, begin to vomit blood or food, pass black (blood-stained) stools, symptoms of bowel inflammation such as severe (watery or bloody) diarrhoea, fever, abdominal pain or tenderness.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
RABEPRAZOLE-WGR Tablets
Active ingredient(s): rabeprazole sodium
Consumer Medicine Information (CMI)
This leaflet provides important information about using RABEPRAZOLE-WGR. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using RABEPRAZOLE-WGR.
Where to find information in this leaflet:
1. Why am I using RABEPRAZOLE-WGR?
2. What should I know before I use RABEPRAZOLE-WGR?
3. What if I am taking other medicines?
4. How do I use RABEPRAZOLE-WGR?
5. What should I know while using RABEPRAZOLE-WGR?
6. Are there any side effects?
7. Product details
1. Why am I using RABEPRAZOLE-WGR?
RABEPRAZOLE-WGR contains the active ingredient rabeprazole sodium. RABEPRAZOLE-WGR is belongs to a group of medicines called proton pump inhibitors (PPIs). RABEPRAZOLE-WGR works by decreasing the amount of acid the stomach makes, to give relief from the symptoms and allow healing to take place. Your food will still be digested in the same way.
RABEPRAZOLE-WGR is used to treat:
- Gastro-oesophageal reflux disease:
RABEPRAZOLE-WGR is used to treat gastro-oesophageal reflux disease (GORD), commonly known as 'reflux'. This can be caused by food and acid from the stomach flowing the wrong way (reflux) back up the food pipe, also known as the oesophagus. Reflux can cause a burning sensation in the chest rising up to the throat, also known as heartburn. RABEPRAZOLE-WGR is also used to help stop gastro-oesophageal reflux disease from coming back or relapsing. - Peptic Ulcers:
RABEPRAZOLE-WGR is used to treat peptic ulcers. Depending on the position of the ulcer it is called a gastric or duodenal ulcer. A gastric ulcer occurs in the stomach. A duodenal ulcer occurs in the duodenum, which is the tube leading out of the stomach.
These ulcers can be caused by too much acid being made in the stomach.
Most people who have a peptic ulcer also have bacteria called Helicobacter pylori in their stomach. Your doctor may also prescribe a course of antibiotics (clarithromycin and amoxycillin) for you. When RABEPRAZOLE-WGR is taken with antibiotics, the combination therapy will kill the Helicobacter pylori and let your ulcer heal. - Chronic Gastritis:
The presence of the bacteria Helicobacter pylori may cause the stomach to become inflamed, resulting in pain, nausea and vomiting; all of which are signs of chronic gastritis.
When RABEPRAZOLE-WGR tablets are taken with antibiotics, they will help kill Helicobacter pylori and allow the stomach to heal.
Your doctor may have prescribed RABEPRAZOLE-WGR for another reason. Ask your doctor if you have any questions about why RABEPRAZOLE-WGR has been prescribed for you.
2. What should I know before I use RABEPRAZOLE-WGR?
Warnings
Do not use RABEPRAZOLE-WGR if:
- You are allergic to rabeprazole sodium, other PPIs (omeprazole, esomeprazole, lansoprazole, pantoprazole), or any of the ingredients listed at the end of this leaflet.
- Always check the ingredients to make sure you can use this medicine.
- The packaging is torn or shows signs of tampering.
Check with your doctor if you:
- have now, or have had in the past, liver problems
- take any medicines for any other condition
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor if you are pregnant or intend to become pregnant.
Talk to your doctor if you are breastfeeding or intend to breastfeed. It is not known if RABEPRAZOLE-WGR passes into breast milk.
Children and adolescents
RABEPRAZOLE-WGR should not be given to children under
18 years of age. Safety and effectiveness of RABEPRAZOLE-WGR in children has not been established.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with RABEPRAZOLE-WGR and affect how it works.
Do not take RABEPRAZOLE-WGR and tell your doctor or pharmacist if you are taking any of the following:
- atazanavir, a medicine used (with other antiretrovirals) to treat HIV1 infection.
- clopidogrel, an antiplatelet medicine.
You should not take RABEPRAZOLE-WGR while taking these medicines.
Also tell your doctor or pharmacist if you are taking any of the following:
- cyclosporin, a medicine used to treat several conditions including prevention of graft rejection following kidney, liver or heart transplantation; severe, active rheumatoid arthritis; severe skin diseases; kidney disease where other treatments have failed.
- methotrexate, a medicine used to treat some kinds of cancer. It is also used to treat psoriasis (skin disease) and rheumatoid arthritis.
- digoxin, a medicine used to treat heart problems.
- ketoconazole, a medicine used to treat fungal infections.
- mycophenolate mofetil, a medicine used to prevent organ rejection following kidney, liver or heart transplants.
- clarithromycin, a medicine used to treat infections.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect RABEPRAZOLE-WGR.
4. How do I use RABEPRAZOLE-WGR?
How much to take / use
- The usual dose is one tablet to be taken once daily.
- The dose of RABEPRAZOLE-WGR tablets is usually 20 mg, but may vary from 10 mg to 40 mg per day depending on what condition you are being treated for and how severe it is.
- For treating Helicobacter pylori infections in combination with antibiotics (clarithromycin and amoxycillin), the usual dose is one 20mg tablet twice daily, morning and evening, for 7 days.
- Follow the instructions provided and use RABEPRAZOLE-WGR until your doctor tells you to stop.
When to take RABEPRAZOLE-WGR
- RABEPRAZOLE-WGR should be used at the same time each day.
How to take RABEPRAZOLE-WGR
- RABEPRAZOLE-WGR should be swallowed whole, with a glass of water or other liquid.
- Do NOT crush or chew the tablets. They have a special coating, which protects them from the acid in your stomach. If the coating is broken by chewing, the tablets may not work.
- It does not matter if you take RABEPRAZOLE-WGR with food or on an empty stomach.
If you forget to use RABEPRAZOLE-WGR
RABEPRAZOLE-WGR should be used regularly at the same time each day. If you miss your dose at the usual time, take it as soon as you remember and then continue to take it as you would normally.
If it is almost time for your next dose, skip the dose you missed and take your next dose when you are meant to.
Do not take a double dose to make up for the dose you missed.
If you use too much RABEPRAZOLE-WGR
If you think that you have used too much RABEPRAZOLE-WGR, you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know while using RABEPRAZOLE-WGR?
Things you should do
- Use RABEPRAZOLE-WGR exactly as your doctor has prescribed.
- Always swallow RABEPRAZOLE-WGR tablets whole.
- Tell your doctor if you become pregnant while you are taking RABEPRAZOLE-WGR
Call your doctor straight away if you:
- Become pregnant while you are taking RABEPRAZOLE-WGR.
Remind any doctor, dentist or you visit that you are using RABEPRAZOLE-WGR.
Things you should not do
- Do not use RABEPRAZOLE-WGR to treat any other complaints unless your doctor says to.
- Do not give this medicine to anyone else, even if they have the same symptoms as you.
- Do not crush or chew the tablets.
- Do not give RABEPRAZOLE-WGR to children.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how RABEPRAZOLE-WGR affects you.
RABEPRAZOLE-WGR may cause dizziness in some people
Looking after your medicine
- Do not take RABEPRAZOLE-WGR tablets out of the blister pack until it is time to take them. If you take them out of the blister they may not keep well.
- Keep RABEPRAZOLE-WGR tablets in a cool dry place where the temperature is below 25°C. Do not keep RABEPRAZOLE-WGR in the refrigerator.
Follow the instructions in the carton on how to take care of your medicine properly.
Store it in a cool dry place away from moisture, heat or sunlight; for example, do not store it:
- in the bathroom or near a sink, or
- in the car or on window sills.
Keep it where young children cannot reach it.
Getting rid of any unwanted medicine
If you no longer need to use this medicine or it is out of date, take it to any pharmacy for safe disposal.
Do not use this medicine after the expiry date.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
Brain or nervous system related:
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
Allergic reactions:
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side affects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What RABEPRAZOLE-WGR contains
| Active ingredient (main ingredient) | rabeprazole sodium |
| Other ingredients (inactive ingredients) | Light magnesium oxide Mannitol Sodium starch glycollate Povidone (K-30) magnesium stearate Ethyl cellulose Diethyl phthalate Hypromellose phthalate Titanium dioxide Purified talc The 10mg tablet also contains iron oxide red The 20mg tablet contains iron oxide yellow. |
Do not take this medicine if you are allergic to any of these ingredients.
The tablets do not contain lactose or gluten.
What RABEPRAZOLE-WGR looks like
RABEPRAZOLE-WGR 10 mg (AUST R 189749):
Red biconvex enteric coated tablet, plain on both sides.
RABEPRAZOLE-WGR Rabeprazole 10 mg tablets are supplied in blister packs of 28 tablets.
RABEPRAZOLE-WGR 20 mg (AUST R 189750):
Yellow biconvex enteric coated tablet, plain on both sides.
RABEPRAZOLE-WGR Rabeprazole 20 mg tablets are supplied in blister packs of 30 tablets
Who distributes RABEPRAZOLE-WGR
Wagner Pharmaceuticals Pty Ltd
6 Albert Street
Preston, Victoria, 3072.
Tel: 1800 936 140
This leaflet was prepared in October 2025.
Brand Information
| Brand name | Rabeprazole-WGR Tablets |
| Active ingredient | Rabeprazole sodium |
| Schedule | S4 |
MIMS Revision Date: 01 April 2025
1 Name of Medicine
Rabeprazole sodium.
2 Qualitative and Quantitative Composition
Each enteric coated (EC) tablet contains 10 mg rabeprazole sodium (equivalent to 9.42 mg rabeprazole) or 20 mg rabeprazole sodium (equivalent to 18.85 mg rabeprazole), as the active ingredient.
For the full list of excipients see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Rabeprazole-WGR 10 mg are pink, round, biconvex delayed release tablets plain on both sides.
Rabeprazole-WGR 20 mg are yellow, round, biconvex delayed released tablets, plain on both sides.
4 Clinical Particulars
4.1 Therapeutic Indications
Rabeprazole-WGR is indicated for:
treatment and prevention of relapse of gastro-oesophageal reflux disease;
symptomatic treatment of gastro-oesophageal reflux disease;
treatment of duodenal ulcers;
treatment of gastric ulcers.
Patients whose gastric and duodenal ulceration is not associated with ingestion of non-steroidal anti-inflammatory drugs (NSAIDs) usually require treatment with antimicrobial agents in addition to antisecretory drugs whether on first presentation or on recurrence.
Rabeprazole-WGR is also indicated, in combination with clarithromycin and amoxicillin, for:
eradication of Helicobacter pylori in patients with peptic ulcer disease or chronic gastritis;
healing of peptic ulcers in patients with Helicobacter pylori associated ulcers.
4.2 Dose and Method of Administration
Rabeprazole-WGR tablets are intended for oral administration.
Rabeprazole-WGR tablets should not be chewed or crushed, but should be swallowed whole. Rabeprazole-WGR tablets should be taken at the same time each day to facilitate treatment compliance. Rabeprazole was taken with or without food in the pivotal clinical trials.
Adults. Treatment of active gastro-oesophageal reflux disease (GORD). The recommended oral dose for this condition is one 20 mg tablet to be taken once daily for four to eight weeks.
Prevention of relapse of gastro-oesophageal reflux disease (GORD). The recommended oral dose for preventing relapse of GORD, once healing is achieved, is one 10 mg tablet to be taken once daily.
If needed this dose should be increased to one 20 mg tablet to be taken once daily.
Symptomatic treatment of gastro-oesophageal reflux disease (GORD). Treatment should commence at 10 mg once daily in patients without oesophagitis. If no response, the dose should be increased to 20 mg once daily for four weeks. If symptom control has not been achieved within four weeks, the patient should be further investigated.
Once symptoms have resolved, subsequent symptom control can be achieved using an on-demand regimen of one 10 mg tablet to be taken once daily, when needed (see Section 4.4 Special Warnings and Precautions for Use).
Treatment of active duodenal ulcer and gastric ulcer. The recommended oral dose for both duodenal ulcer and gastric ulcer is one 20 mg tablet to be taken once daily.
Some patients with duodenal ulcer may respond to one 10 mg tablet taken once daily.
Most patients with active duodenal ulcer heal within four weeks. However a few patients may require an additional four weeks of therapy to achieve healing.
Most patients with gastric ulcer heal within six weeks. However, again a few patients may require an additional six weeks of therapy to achieve healing.
Eradication of H. pylori. Patients with gastro-duodenal ulcers or chronic gastritis due to H. pylori infection should be treated with: Rabeprazole-WGR 20 mg twice daily + clarithromycin 500 mg twice daily and amoxicillin 1 g twice daily for seven days.
Eradication of H. pylori with this regimen has been shown to result in the healing of duodenal or gastric ulcers without the need for continued ulcer therapy.
Use in children. Rabeprazole-WGR is not recommended for use in children as there is no experience of its use in this group.
Use in elderly patients. No dosage adjustment is necessary in elderly patients.
Use in patients with renal impairment. No dosage adjustment is necessary for patients with renal impairment.
There are no data on the use of rabeprazole in combination with antibiotic regimens in patients with renal impairment.
Use in patients with hepatic impairment. Patients with mild to moderate hepatic impairment experience higher exposure to rabeprazole sodium at a given dose than do healthy patients. Caution should be exercised in patients with severe hepatic impairment (see Section 4.4 Special Warnings and Precautions for Use).
There are no data on the use of rabeprazole in combination with antibiotic regimens in patients with hepatic impairment.
4.3 Contraindications
Rabeprazole-WGR is contraindicated in patients with known hypersensitivity to rabeprazole sodium, proton pump inhibitors, or any ingredient of this product.
4.4 Special Warnings and Precautions for Use
Symptomatic response to therapy with Rabeprazole-WGR does not preclude the presence of gastric malignancy, therefore the possibility of malignancy should be excluded prior to commencing treatment with Rabeprazole-WGR.
Patients using an on-demand regimen for symptomatic GORD should be further reviewed and/or investigated if symptoms persist beyond 6 months.
Acute tubulointerstitial nephritis. Acute tubulointerstitial nephritis (TIN) has been observed in patients taking proton-pump inhibitors (PPIs) including rabeprazole sodium. Acute tubulointerstitial nephritis may occur at any point during PPI therapy and is generally attributed to an idiopathic hypersensitivity reaction. Acute tubulointerstitial nephritis can progress to renal failure. Discontinue rabeprazole sodium if acute tubulointerstitial nephritis develops.
Cyanocobalamin (vitamin B-12) deficiency. Daily treatment with acid-suppressing medicines over a long period of time (e.g. longer than 3 years) may lead to malabsorption of cyanocobalamin (vitamin B-12) caused by hypo- or achlorhydria.
Hypomagnesaemia. Hypomagnesaemia, symptomatic and asymptomatic, has been reported rarely in patients treated with PPIs. Serious adverse events include tetany, arrhythmias, and seizures. In most patients, treatment of hypomagnesaemia required magnesium replacement and discontinuation of the PPI.
For patients expected to be on prolonged treatment or who take PPIs with medications such as digoxin or drugs that may cause hypomagnesaemia (e.g. diuretics), health care professionals may consider monitoring magnesium levels prior to initiation of PPI treatment and then periodically while treatment continues (see Section 4.8 Adverse Effects (Undesirable Effects)).
Hypomagnesaemia may lead to hypocalcaemia and/or hypokalaemia (see Section 4.8 Adverse Effects (Undesirable Effects)).
Fractures. Observational studies suggest that proton pump inhibitor (PPI) therapy may be associated with an increased risk for osteoporosis-related fractures of the hip, wrist, or spine. The risk of fracture was increased in patients who received high-dose, and long-term PPI therapy (a year or longer).
Concomitant use of rabeprazole with methotrexate. Literature suggests that concomitant use of PPIs with methotrexate (primarily at high dose; see methotrexate prescribing information) may elevate and prolong serum levels of methotrexate and/or its metabolite, possibly leading to methotrexate toxicities. In such high doses methotrexate administration, a temporary withdrawal of the PPI may be considered in some patients.
Clostridium difficile. Treatment with proton pump inhibitors may possibly increase the risk of gastrointestinal infections such as Clostridium difficile.
Subacute cutaneous lupus erythematosus. Subacute cutaneous lupus erythematosus (SCLE) has been reported with the use of PPIs. If lesions occur, especially in sun-exposed areas of the skin, and if accompanied by arthralgia, the patient should seek medical help promptly and the healthcare professionals should consider stopping rabeprazole. The occurrence of SCLE with previous PPI treatment may increase the risk of SCLE with other PPIs.
Fundic gland polyps. As with other PPIs, long-term use of rabeprazole is associated with an increased risk of fundic gland polyps (see Section 4.8 Adverse Effects (Undesirable Effects)). Most fundic gland polyps are asymptomatic. Patients with large or ulcerated polyps may be at risk of gastrointestinal bleeding or small intestinal blockage. Use the lowest dose and shortest duration of PPI therapy appropriate to the condition being treated.
Use in hepatic impairment. No dosage adjustment is necessary for patients with hepatic impairment. While no evidence of significant drug related safety problems was observed in patients with hepatic impairment, it is advised to exercise caution when treatment with Rabeprazole-WGR is first initiated in patients with severe hepatic dysfunction (see Section 4.2 Dose and Method of Administration).
Use in renal impairment. No data available.
Use in the elderly. No data available.
Paediatric use. No data available.
Effects on laboratory tests. PPI-induced decreases in gastric acidity may lead to increases in serum chromogranin A (CgA) levels, which may lead to erroneous interpretations of laboratory results in investigations for neuroendocrine tumors. To avoid this interference, temporarily stop rabeprazole treatment at least 14 days before assessing CgA levels and consider repeating the test if initial CgA levels are high.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Effect of rabeprazole sodium on other drugs - demonstrated interactions. In vitro studies with human liver microsomes indicated that rabeprazole sodium is metabolised by isoenzymes of CYP450 (CYP2C19 and CYP3A4).
Patients may need to be monitored when these drugs are taken together with rabeprazole.
Ciclosporin. In vitro incubations employing human liver microsomes indicated that rabeprazole inhibited ciclosporin metabolism with an IC50 of 62 micromolar, a concentration that is over 50 times higher than the Cmax in healthy volunteers following 14 days dosing with 20 mg rabeprazole. Although in vitro studies may not always be predictive of an in vivo status, these findings indicate that no interaction is expected between rabeprazole and ciclosporin.
Methotrexate. Case reports, published population pharmacokinetic studies and retrospective analyses suggest that concomitant administration of PPIs and methotrexate (primarily at high dose; see methotrexate prescribing information) may elevate and prolong serum levels of methotrexate and/or its metabolite hydroxymethotrexate. However, no formal drug interaction studies of methotrexate with PPIs have been conducted.
Digoxin. A 22% increase in trough digoxin levels was observed in normal subjects given both drugs concomitantly.
Ketoconazole. A 33% decrease in ketoconazole levels was observed in normal subjects given both drugs concomitantly.
Atazanavir. Co-administration of atazanavir with other proton pump inhibitors resulted in a substantial reduction in atazanavir exposure. The absorption of atazanavir is pH dependent. Therefore, Rabeprazole-WGR should not be co-administered with atazanavir.
Mycophenolate mofetil. Co-administration of proton-pump inhibitors with mycophenolate mofetil in healthy and transplant patients has been reported to reduce the exposure to the active metabolite, mycophenolic acid. This is possibly due to a decrease in mycophenolate mofetil solubility at an increased gastric pH. The clinical relevance of reduced mycophenolic acid exposure on organ rejection has not been established in transplant patients receiving proton pump inhibitors and mycophenolate mofetil. Use rabeprazole sodium with caution in transplant patients receiving mycophenolate mofetil.
Clopidogrel. Clopidogrel is metabolised to its active metabolite by CYP2C19. Inhibition of CYP2C19 by rabeprazole would be expected to result in reduced drug levels of the active metabolite of clopidogrel and a reduction in its antiplatelet activity and therefore its clinical efficacy. Concomitant use of rabeprazole with clopidogrel should be discouraged.
Effect of rabeprazole sodium on other drugs - theoretical interactions. Rabeprazole sodium produces sustained inhibition of gastric acid secretion. An interaction with compounds whose absorption depends on gastric pH may occur due to the magnitude of acid suppression seen with rabeprazole sodium.
Effect of rabeprazole sodium on other drugs - potential interactions that have been excluded. Studies in healthy subjects have shown that rabeprazole sodium does not have clinically significant interactions with other drugs metabolised by the CYP450 system. These studies included the drugs warfarin and theophylline (as single oral doses), phenytoin (as a single intravenous dose with supplemental oral dosing), diazepam (as a single intravenous dose) and amoxicillin (as single and multiple oral doses).
Taking rabeprazole with antacids produces no clinically relevant changes in plasma rabeprazole sodium concentrations.
Plasma concentrations of rabeprazole and the active metabolite of clarithromycin are increased by 24% and 50% respectively during concomitant administration. This is considered to be a useful interaction during H. pylori eradication.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. Rabeprazole at intravenous doses up to 30 mg/kg/day (plasma AUC of 8.8 microgram.hr/mL, about 10 times the human exposure at 20 mg/day) was found to have no effect on fertility and reproductive performance of male and female rats.
Use in pregnancy. (Category B1)
Teratology studies have been performed in rats at intravenous doses up to 50 mg/kg/day (plasma AUC of 11.8 microgram.hr/mL, about 13 or 6.5 times the human exposure at 20 mg/day and 40 mg/day respectively), and rabbits at intravenous doses up to 30 mg/kg/day (plasma AUC of 7.3 microgram.hr/mL, about 8 or 4 times the human exposure at 20 mg/day and 40 mg/day respectively) and have revealed no evidence of impaired fertility or harm to the foetus due to rabeprazole. There are no adequate and well controlled studies in pregnant women and post-marketing experience is very limited. Rabeprazole sodium should be used in pregnancy only if the potential benefit justifies the potential risk to the foetus.
Use in lactation. Following intravenous administration of 14C-labelled rabeprazole to lactating rats, radioactivity in milk reached levels that were about 2 to 7-fold higher than levels in the blood. Administration of rabeprazole to rats in gestation and during lactation at doses of 400 mg/kg/day (about 195 or 85 times a 20 mg or 40 mg human dose based on mg/m2) resulted in decreases in bodyweight gain of the pups.
It is not known whether rabeprazole sodium is excreted in human breast milk and there are no studies in lactating women. Since many drugs are excreted in milk and because of the potential for adverse reactions to nursing infants from rabeprazole sodium, a decision should be made to discontinue nursing or discontinue the drug, taking into account the importance of the drug to the mother.
4.7 Effects on Ability to Drive and Use Machines
The effects of this medicine on a person's ability to drive and use machines were not assessed as part of its registration.
4.8 Adverse Effects (Undesirable Effects)
Rabeprazole was generally well tolerated during clinical trials. The observed side effects have generally been mild or moderate and transient in nature. In the majority of cases, the incidence of the adverse events in the rabeprazole treatment group was equal to or less than that observed in the placebo control treatment group.
Only headaches, diarrhoea, abdominal pain, asthenia, flatulence, rash and dry mouth have been associated with the use of rabeprazole.
The adverse events, which may or may not be causally related to rabeprazole, reported in clinical trials are listed below in descending order of frequency.
Common (≥ 1% and < 10%). Nervous system. Headache, dizziness.
Gastrointestinal. Diarrhoea, nausea, abdominal pain, flatulence, vomiting, constipation.
Respiratory. Rhinitis, pharyngitis, cough.
Musculoskeletal. Non-specific pain, back pain, myalgia.
Skin. Rash.
Other. Asthenia, flu-like syndrome, infection, insomnia, chest pain.
Uncommon (≥ 0.1% and < 1%). Gastrointestinal. Dyspepsia, eructation, dry mouth.
Respiratory. Sinusitis, bronchitis.
Musculoskeletal. Arthralgia, leg cramps.
Urinary. Urinary tract infection.
Other. Fever, nervousness, somnolence, chills, peripheral oedema.
Rare (≥ 0.01% and < 0.1%). Gastrointestinal. Anorexia, gastritis, weight gain, stomatitis.
Skin. Pruritus, sweating.
Special senses. Vision or taste disturbances.
Haematologic. Leucocytosis.
Other. Depression.
Post-marketing experience. Erythema and rarely bullous reactions, urticarial skin eruptions and acute systemic allergic reactions, for example facial swelling, hypotension and dyspnoea have been reported in patients treated with rabeprazole. These usually resolved after discontinuation of therapy.
Erythema multiforme, tubulointerstitial nephritis (with possible progression to renal failure), gynaecomastia, myalgia and potential allergic reactions including anaphylactic reactions have been reported rarely. Hypomagnesaemia and blood dyscrasia including thrombocytopenia, neutropenia, leukopenia, pancytopenia, agranulocytosis and bicytopenia have been reported rarely.
Hypomagnesaemia has also been reported rarely. Hypocalcaemia and/or hypokalaemia have been reported, which may be related to the occurrence of hypomagnesaemia (see Section 4.4 Special Warnings and Precautions for Use).
There have also been reports of increased hepatic enzymes and serious hepatic dysfunction such as hepatitis and jaundice. Rare reports of hepatic encephalopathy have been received in patients with underlying cirrhosis.
There have been very rare reports of toxic epidermal necrolysis (TEN) and Stevens-Johnson syndrome and bullous rashes including subacute cutaneous lupus erythematosus.
There have been post-marketing reports of bone fractures and post-marketing reports of subacute cutaneous lupus erythematosus (SCLE) and fundic gland polyps (see Section 4.4 Special Warnings and Precautions for Use).
Gastrointestinal disorders. Frequency not known: Withdrawal of long-term PPI therapy can lead to aggravation of acid-related symptoms and may result in rebound acid hypersecretion.
Metabolism and nutrition disorders. Hyponatraemia.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
Symptoms. Experience to date with deliberate or accidental overdose is limited. The maximum established exposure has not exceeded 60 mg twice daily, or 160 mg once daily. Effects are generally minimal, representative of the known adverse event profile, and reversible without further medical intervention.
Treatment. No specific antidote is known. Rabeprazole sodium is extensively protein bound and is therefore not readily dialysable. As in any case of overdose, treatment should be symptomatic and general supportive measures should be used.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Rabeprazole sodium suppresses gastric acid secretion by the specific inhibition of the H+/K+-ATPase enzyme (proton pump) at the secretory surface of the gastric parietal cell thereby blocking the final step of acid production. This effect is dose-related and leads to inhibition of both basal and stimulated acid secretion irrespective of the stimulus. Animal studies indicate that after administration, rabeprazole sodium rapidly disappears from both the plasma and gastric mucosa.
Antisecretory activity. Oral administration of a 20 mg dose of rabeprazole sodium provides rapid and effective reduction of gastric acid secretion. The onset of the antisecretory effect occurs within one hour with the maximum effect occurring within two to four hours. Inhibition of basal and food stimulated acid secretion 23 hours after the first dose of rabeprazole sodium is 69% and 82% respectively, and the duration of inhibition lasts up to 48 hours. The duration of pharmacodynamic action is much longer than the pharmacokinetic half-life (approximately one hour) would predict. This effect is probably due to the prolonged binding of rabeprazole sodium to the parietal H+/K+-ATPase enzyme. The inhibitory effect of rabeprazole sodium on acid secretion increases slightly with repeated once daily dosing, achieving steady-state inhibition after three days. When the drug is discontinued, secretory activity normalises over 2 to 3 days.
Helicobacter pylori is associated with duodenal and gastric ulcer disease in approximately 95% and 70% of patients respectively. H. pylori is implicated as a major contributing factor in the development of gastritis and ulcers in such patients. Recent evidence also suggests a causative link between H. pylori and gastric carcinoma. H. pylori eradication therapy is appropriate in most patients with duodenal and gastric ulcer where the latter is not caused by non-steroidal anti-inflammatory drug (NSAID) ingestion (see Section 4.2 Dose and Method of Administration).
Serum gastrin effects. In clinical studies, patients were treated once daily with 10 or 20 mg rabeprazole sodium for up to 12 months duration. Serum gastrin levels increased during the first 2 to 8 weeks reflecting the inhibitory effects on acid secretion. Gastrin values returned to pre-treatment levels, usually within 1 to 2 weeks after discontinuation of therapy. In a maintenance study, which was subsequently extended up to 5 years duration, serum gastrin levels were only modestly raised in most patients.
Enterochromaffin-like (ECL) cell effects. Increased serum gastrin secondary to antisecretory agents stimulates proliferation of gastric ECL cells which, over time, may result in ECL cell hyperplasia in rats and mice and gastric carcinoids in rats, especially females (see Section 5.3 Preclinical Safety Data, Genotoxicity, Carcinogenicity; Section 4.6 Fertility, Pregnancy and Lactation, Effects on fertility).
In over 400 patients treated with rabeprazole sodium (10 or 20 mg/day) for up to one year, the incidence of ECL cell hyperplasia increased with time and dose, which is consistent with the pharmacological action of the proton pump inhibitor. No patient developed the adenomatoid, dysplastic or neoplastic changes of ECL cells in the gastric mucosa. No patient developed the carcinoid tumours observed in rats.
Clinical trials. At the time of registration, more than 3000 patients in the US, Europe and Japan had received rabeprazole sodium in both controlled and uncontrolled clinical studies.
The efficacy of rabeprazole was assessed in nine double blind, controlled, randomised, parallel group primary efficacy trials in patients with duodenal ulcer, gastric ulcer and gastro-oesophageal reflux disease. Three trials were conducted in each indication, a placebo controlled study and comparative studies with either ranitidine or omeprazole. In all these studies the primary efficacy variable used was ulcer or ulcerative GORD healing rates as determined by endoscopic examination.
A further three clinical trials were conducted to establish efficacy of rabeprazole in the long-term prevention of relapse of gastro-oesophageal reflux disease. Two studies were placebo controlled, whilst the other was actively controlled with omeprazole. In all three studies the primary efficacy variable used was the continued absence of oesophageal erosions or ulcerations as determined by endoscopic examination.
Treatment of erosive or ulcerative gastro-oesophageal reflux disease (GORD). In the placebo controlled study, 103 patients were treated for up to eight weeks either with placebo or rabeprazole 10, 20 or 40 mg once daily (od). Rabeprazole was significantly superior to placebo in producing endoscopic healing after four and eight weeks of treatment (p < 0.001).
Rabeprazole 20 mg once daily was also significantly more effective than placebo in terms of symptom relief, providing complete resolution of heartburn frequency, daytime heartburn severity, and decreasing the amount of antacid taken per day after four and eight weeks of treatment.
Rabeprazole 20 mg once daily was statistically superior to ranitidine 150 mg four times per day with respect to the percentage of patients healed at endoscopy and in symptom relief. Rabeprazole was also significantly more effective than ranitidine in terms of providing complete resolution of heartburn frequency, and daytime and night time heartburn severity; after four and eight weeks of treatment.
In an active controlled study of 202 patients treated with rabeprazole 20 mg once daily or omeprazole 20 mg once daily for up to eight weeks, rabeprazole was as effective as omeprazole in producing endoscopic healing. The percentages of patients healed at endoscopy at four and eight weeks are given in Table 1.

Prevention of relapse of gastro-oesophageal reflux disease (GORD). The prevention of relapse in patients with erosive or ulcerative GORD previously healed with gastric anti-secretory therapy was assessed in two U.S. multi-centre, double blind, placebo-controlled studies of 52 weeks duration. The two studies of identical design randomised 209 and 285 patients respectively, to receive either 10 mg or 20 mg of rabeprazole, or placebo once daily. In both studies rabeprazole was significantly superior to placebo in prevention of relapse of GORD.
In both multicentre trials, rabeprazole 10 mg once daily and 20 mg once daily were significantly more effective than placebo in preventing the recurrence of heartburn frequency (p < 0.001) as well as improving daytime (p < 0.001) and night time (p < 0.003) heartburn severity.
In the actively controlled European study, 243 patients were treated with a fixed dose of either omeprazole 20 mg once daily, or rabeprazole 10 mg or 20 mg once daily. Treatment with both 10 mg and 20 mg rabeprazole were as effective as omeprazole 20 mg in preventing GORD relapse (p = 0.5216 and p = 0.8004 respectively). See Table 2.

Symptomatic gastro-oesophageal reflux disease (GORD). On-demand treatment was assessed in a European multicentre, double-blind placebo-controlled randomised withdrawal study (n = 418) in endoscopically negative patients.
Following an acute open label phase, patients were randomised to receive rabeprazole 10 mg or placebo taken once daily, when required, over a six month period. Efficacy of rabeprazole 10 mg on-demand, in patients with complete heartburn relief at baseline was primarily evaluated by the unwillingness to continue the trial because of inadequate heartburn control. Overall, the proportion of patients discontinuing due to inadequate heartburn control was significantly higher for placebo (20%) compared to rabeprazole (6%) (p < 0.00001).
Patients were instructed to take study drug until they had experienced a full 24 hours free of heartburn, most patients in the rabeprazole group had maximum episode duration of 4 days or less. In addition, antacid use was about 2-fold higher in the placebo group than in the rabeprazole group (p = 0.0011). Treatment failure was associated with an increased antacid consumption.
Treatment of duodenal ulcers. In a US study (n = 100) rabeprazole 20 mg once daily was significantly superior to placebo in producing healing of endoscopically defined duodenal ulcers (p = 0.001) after four weeks treatment.
Patients treated for four weeks with rabeprazole 20 mg once daily reported significantly less ulcer pain frequency (p < 0.001). After 7 days treatment with rabeprazole 20 mg once daily, patients reported significantly less daytime (p = 0.013) and night time (p = 0.003) ulcer pain severity than patients treated with placebo. This difference continued for the whole study period. Additionally, rabeprazole 20 mg once daily was significantly more effective than placebo in reducing daily antacid use (p < 0.001).
In the ranitidine-controlled trial, 375 patients with endoscopically defined duodenal ulcers were treated with rabeprazole 20 mg once daily or ranitidine 150 mg twice daily for up to four weeks. Rabeprazole 20 mg once daily was significantly more effective than ranitidine 150 mg twice daily at producing complete healing of duodenal ulcers after 2 and 4 weeks (p = 0.002 and p = 0.017 respectively).
Rabeprazole 20 mg once daily was also significantly more effective than ranitidine 150 mg twice daily in producing complete resolution of ulcer pain frequency (week 2, p = 0.006), in alleviating night time ulcer pain severity (week 2, p = 0.044), and in reducing antacid consumption (p = 0.037).
In patients with endoscopically defined duodenal ulcers treated for up to four weeks, rabeprazole 20 mg once daily was as effective as omeprazole 20 mg once daily in producing healing of duodenal ulcers. The percentages of patients with endoscopic healing at two and four weeks are shown in Table 3.

Treatment of gastric ulcers. Rabeprazole was found to be significantly (p = 0.002) superior to placebo in producing endoscopically defined healing of gastric ulcers after 6 weeks in a placebo-controlled study assessing the effectiveness of rabeprazole 20 mg once daily versus placebo (p < 0.001).
The rates of endoscopic healing of gastric ulcers in patients treated with rabeprazole 20 mg once daily (n = 184) and ranitidine 150 mg two times per day (n = 180) were found to be equivalent after three and six weeks of treatment.
In a European multicentre study comparing rabeprazole 20 mg (n = 113) to omeprazole 20 mg (n = 114), the rates of endoscopic healing of gastric ulcers were found to be equivalent with the two treatments at three and six weeks. See Table 4.

H. pylori eradication. In a multicentre, randomised, controlled European study conducted to establish the efficacy of rabeprazole based triple therapy for H. pylori eradication in patients with peptic ulcer disease, the combination: Rabeprazole 20 mg twice daily with clarithromycin 500 mg twice daily and amoxicillin 1 g twice daily for a total of 7 days (n = 83), achieved an eradication rate of 94% and a healing rate for duodenal ulcers of 91%.
5.2 Pharmacokinetic Properties
Absorption. Rabeprazole-WGR tablets are enteric coated to allow rabeprazole sodium, which is acid labile, to pass through the stomach intact. Absorption is rapid, with peak plasma levels of rabeprazole sodium occurring approximately 3.5 hours after a 20 mg dose. Peak plasma concentrations (Cmax) of rabeprazole sodium and AUC are linear over the dose range of 10 mg to 40 mg.
Absolute bioavailability of an oral 20 mg dose (compared to intravenous administration) is about 52%, largely due to pre-systemic metabolism. Additionally, the bioavailability does not appear to increase with repeat administration. In healthy subjects, the plasma half-life is approximately one hour (range 0.7 to 1.5 hours) and the total body clearance is estimated to be 283 ± 98 mL/min.
Distribution. Rabeprazole sodium is approximately 97% bound to human plasma proteins. After intravenous administration the volume of distribution is 0.34 L/kg.
Metabolism. Rabeprazole sodium is metabolised through the cytochrome P450 (CYP450) hepatic drug metabolism system (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions). In humans, the thioether (M1) and carboxylic acid (M6) are the main plasma metabolites with the sulphone (M2), desmethyl thioether (M4) and mercapturic acid conjugate (M5) minor metabolites observed at lower levels. Only the desmethyl metabolite (M3) has a small amount of antisecretory activity, but its presence in plasma is minimal.
Excretion. Following a single 20 mg 14C-labelled oral dose of rabeprazole sodium, no unchanged drug was excreted in the urine. Approximately 90% of the dose was eliminated in urine mainly as the two metabolites: a mercapturic acid conjugate (M5) and a carboxylic acid (M6), plus two unknown metabolites also found in the species used in the toxicology studies. The remainder of the dose was recovered in faeces. Total recovery was 99.8%. This suggests low biliary excretion of the metabolites; with biotransformation and urinary excretion of water soluble metabolites as the primary route of elimination.
Special populations. Renal disease. In patients with stable, endstage, renal failure requiring maintenance haemodialysis (creatinine clearance ≤ 5 mL/min/1.73 m2), the pharmacokinetics of rabeprazole sodium was very similar to that in healthy volunteers.
Hepatic disease. In a single dose study of 10 patients with chronic mild to moderate compensated cirrhosis of the liver who were administered a 20 mg dose of rabeprazole, AUC0-24 was approximately doubled, the elimination half-life was 2 to 3-fold higher, and total body clearance was decreased to less than half compared to values in healthy men.
In a multiple dose study of 12 patients with mild to moderate hepatic impairment administered 20 mg rabeprazole once daily for eight days, AUC0-∞ and Cmax values increased approximately 30% compared to values in healthy age and gender matched subjects. These increases were not statistically significant.
No information exists on rabeprazole disposition in patients with severe hepatic impairment. Please see Section 4.2 Dose and Method of Administration for information on dosage adjustments in patients with hepatic impairment.
Geriatrics. Elimination of rabeprazole sodium was decreased in the elderly. Following 7 days of daily dosing with 20 mg of rabeprazole sodium, the AUC approximately doubled and the Cmax increased by 60% as compared to young healthy volunteers. However, there was no evidence of rabeprazole sodium accumulation.
5.3 Preclinical Safety Data
Note. In the following section, the relative exposure levels in animals have been calculated using a human dose of 20 mg/day, the maximum recommended rabeprazole dose for the treatment of GORD and active gastro-duodenal ulcers. For H. pylori eradication, the recommended dose of rabeprazole is 40 mg/day (20 mg b.i.d.) for one week; this should be taken into account when reviewing exposure figures.
Genotoxicity. Rabeprazole was positive in assays for gene mutations (the Ames test, forward gene mutation tests in Chinese hamster ovary cells (CHO/HGPRT) and mouse lymphoma cells (L5178Y/TK+/-)). Its demethylated metabolite was also positive in the Ames test. Rabeprazole was negative in assays for chromosomal damage (the in vitro Chinese hamster lung cell chromosome aberration test, the in vivo mouse micronucleus test), and in vitro and ex vivo rat hepatocyte unscheduled DNA synthesis (UDS) tests.
Carcinogenicity. In an 88/104 week carcinogenicity study in CD-1 mice, rabeprazole at oral doses up to 100 mg/kg/day did not produce any increased tumour occurrence. The highest tested dose produced a systemic exposure to rabeprazole (AUC) of 1.40 microgram.hr/mL which is 1.6 times the human exposure at the recommended dose for GORD (20 mg/day).
In a 104 week carcinogenicity study in SD rats, males were treated with oral doses of 5, 15, 30 and 60 mg/kg/day and females with 5, 15, 30, 60 and 120 mg/kg/day. Rabeprazole produced gastric enterochromaffin-like (ECL) cell hyperplasia in male and female rats and ECL cell carcinoid tumours in female rats at all doses. The lowest dose (5 mg/kg/day) produced a systemic exposure to rabeprazole (AUC) of about 0.1 microgram.hr/mL which is about 0.1 times the human exposure at 20 mg/day. In male rats, no treatment-related tumours were observed at doses up to 60 mg/kg/day producing a rabeprazole plasma exposure (AUC) of about 0.2 microgram.hr/mL (0.2 times the human exposure at 20 mg/day).
6 Pharmaceutical Particulars
6.1 List of Excipients
Light magnesium oxide, mannitol, sodium starch glycollate type A, povidone, magnesium stearate, ethylcellulose, diethyl phthalate, hypromellose phthalate, titanium dioxide, purified talc, iron oxide red (10 mg tablets only), iron oxide yellow (20 mg tablets only).
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C.
6.5 Nature and Contents of Container
10 mg tablets. Alu/Alu blister packs of 28 tablets.
20 mg tablets. Alu/Alu blister packs of 30 tablets.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Rabeprazole sodium is a substituted benzimidazole and belongs to the class of proton pump inhibitors. Its solubility in water is pH dependent, being very soluble in water at pH 9 to 11, and only slightly soluble in water at pH 8. It is very soluble in methanol, freely soluble in dichloromethane and practically insoluble in hexane. Rabeprazole has one chiral centre and is a racemate of two enantiomers.
Chemical structure.
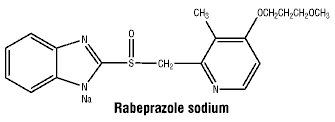
Molecular formula: C18H20N3NaO3S.
Molecular weight: 381.43.
CAS number. CAS-117976-89-3 (rabeprazole);
CAS-117976-90-6 (rabeprazole sodium).
7 Medicine Schedule (Poisons Standard)
S4 - Prescription Only Medicine.
Date of First Approval
09 July 2012
Date of Revision
04 February 2025
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.