Roxithromycin Sandoz
Brand Information
| Brand name | Roxithromycin Sandoz |
| Active ingredient | Roxithromycin |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Roxithromycin Sandoz.
Summary CMI
Roxithromycin Sandoz®
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using Roxithromycin Sandoz?
Roxithromycin Sandoz contains the active ingredient roxithromycin. Roxithromycin Sandoz is used to treat infections in different parts of the body caused by bacteria. For more information, see Section 1. Why am I using Roxithromycin Sandoz? in the full CMI.
2. What should I know before I use Roxithromycin Sandoz?
Do not use if you have ever had an allergic reaction to roxithromycin or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding. For more information, see Section 2. What should I know before I use Roxithromycin Sandoz? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with Roxithromycin Sandoz and affect how it works. A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use Roxithromycin Sandoz?
- The recommended adult dosage is 300 mg per day.
- The recommended dosage for children more than 40 kg is one 150 mg tablet twice daily.
More instructions can be found in Section 4. How do I use Roxithromycin Sandoz? in the full CMI.
5. What should I know while using Roxithromycin Sandoz?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Drinking alcohol |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using Roxithromycin Sandoz? in the full CMI.
6. Are there any side effects?
Common side effects include: rash; loss of appetite. Refer to the CMI for all side effects. For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
Roxithromycin Sandoz®
Active ingredient(s): roxithromycin (rocks-e-throw-my-sin)
Consumer Medicine Information (CMI)
This leaflet provides important information about using Roxithromycin Sandoz. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using Roxithromycin Sandoz.
Where to find information in this leaflet:
1. Why am I using Roxithromycin Sandoz?
2. What should I know before I use Roxithromycin Sandoz?
3. What if I am taking other medicines?
4. How do I use Roxithromycin Sandoz?
5. What should I know while using Roxithromycin Sandoz?
6. Are there any side effects?
7. Product details
1. Why am I using Roxithromycin Sandoz?
Roxithromycin Sandoz contains the active ingredient roxithromycin. Roxithromycin Sandoz is an antibiotic that belongs to a group of medicines called macrolides. These antibiotics work by killing or stopping the growth of the bacteria that are causing your infection.
Roxithromycin Sandoz, like other antibiotics, does not work against viral infections such as the flu.
Roxithromycin Sandoz is used to treat infections in different parts of the body caused by bacteria. For example:
- acute pharyngitis (sore throat and discomfort when swallowing)
- tonsillitis
- sinusitis
- acute bronchitis (infection of the bronchi causing coughing)
- exacerbation of chronic bronchitis
- pneumonia (lung infection characterised by fever, malaise, headache)
- skin and soft tissue infections
- non gonococcal urethritis
- impetigo (bacterial infection causing sores on the skin)
2. What should I know before I use Roxithromycin Sandoz?
Warnings
Do not use Roxithromycin Sandoz if:
- you are allergic to roxithromycin, or any other macrolide antibiotic e.g. azithromycin, clarithromycin or erythromycin, any of the ingredients listed at the end of this leaflet. Symptoms of an allergic reaction may include skin rash, itching, shortness of breath, or swelling of the face, lips or tongue which cause difficulty in swallowing or breathing.
Always check the ingredients to make sure you can use this medicine. - you have severe liver problems
- if you are taking certain migraine headache medicines called ergot alkaloids e.g. Cafergot, Dihydergot (not all brands listed)
- the product has expired or the packaging appears tampered with.
Check with your doctor if you:
- have allergies to any other substances, such as foods, preservatives or dyes
- are pregnant or intend to become pregnant
- are breastfeeding or plan to breastfeed
- have or have had the following medical conditions:
- kidney problems (impaired function)
- liver problems (hepatic cirrhosis with jaundice and/ or ascites) - have any other medical conditions
- take any medicines for any other condition
- plan to have surgery.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Tell your doctor or pharmacist if you are pregnant or intend to become pregnant. Like most medicines of this kind, Roxithromycin Sandoz is not recommended for use during pregnancy. Your doctor or pharmacist will discuss the risks and benefits of taking it if you are pregnant
Tell your doctor or pharmacist if you are breastfeeding or plan to breastfeed. Roxithromycin Sandoz passes into breast milk. Your doctor or pharmacist will discuss the risks and benefits of taking it if you are breastfeeding or planning to breastfeed.
Use in the Elderly
Roxithromycin Sandoz can be used in the elderly with no dosage adjustment required.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may be affected by Roxithromycin Sandoz, or may affect how it works. These include:
- Theophylline (Neulin), a medicine used to treat asthma
- some medicines for migraine headache such as ergotamine (Cafergot) or dihydroergotamine (Dihydergot tablets)
- disopyramide, a medicine to treat irregular heart rhythms
- terfenadine and astemizole, over the counter medicines used to treat allergies
- warfarin (Coumadin, Marevan), a medicine used to prevent blood clots
- digoxin (Lanoxin, Sigmaxin), a medicine used to treat heart failure
- midazolam (Hypnovel, Midazolam Sandoz), used to induce sleep before operations
- ciclosporin (Neoral, Cicoral, Cysporin, Sandimmun), a medicine used to prevent organ transplant rejection or to treat certain problems with the immune system
- cisapride, a medicine used to treat gastrointestinal problems
- pimozide (Orap), an antipsychotic medicine
- hydroxychloroquine or chloroquine, used to treat conditions including rheumatoid arthritis, or to treat or prevent malaria. Taking these medicines at the same time as Roxithromycin Sandoz may increase the chance of you getting side effects that affect your heart.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect Roxithromycin Sandoz.
4. How do I use Roxithromycin Sandoz?
How much to take
- The recommended adult dosage is 300 mg per day which may be taken according to one of the following alternative dosage regimens:
- one 300 mg tablet once a day, or
- one 150 mg tablet twice a day, or
- two 150 mg tablets once a day
However, depending on your condition and how you react to the medicine, your doctor may ask you to take a different dose. - The recommended dosage for children more than 40 kg is one 150 mg tablet twice daily. The dosage of Roxithromycin Sandoz given to children is dependent on the child's weight.
- Your doctor will tell you exactly how much to take.
- Follow the instructions provided and use Roxithromycin Sandoz until your doctor tells you to stop
When to take/use Roxithromycin Sandoz
- Roxithromycin Sandoz should be taken at least 15 minutes before food or on an empty stomach (i.e. more than 3 hours after a meal).
- Roxithromycin Sandoz works best if you take it on an empty stomach.
How to take Roxithromycin Sandoz
- Swallow the tablets whole with a glass of water.
How long to take Roxithromycin Sandoz
- For treating infections, Roxithromycin Sandoz is usually taken for 5 to 10 days. However, your doctor may prescribe Roxithromycin Sandoz for longer periods
- Continue taking the tablets until you finish the pack or until your doctor or pharmacist tells you to stop
If you forget to use Roxithromycin Sandoz
Roxithromycin Sandoz should be used regularly at the same time each day.
If it is almost time for your next dose, skip the dose you missed and take your next dose when you are meant to.
Do not take a double dose to make up for the dose you missed.
If you use too much Roxithromycin Sandoz
If you think that you have used too much Roxithromycin Sandoz, you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
5. What should I know while using Roxithromycin Sandoz?
Things you should do
- If the symptoms of your infection do not improve within a few days, or if they become worse, tell your doctor.
- If you get severe diarrhoea tell your doctor, pharmacist or nurse immediately. Do this even if it occurs several weeks after Roxithromycin Sandoz has been stopped. Diarrhoea may mean that you have a serious condition affecting your bowel. You may need urgent medical care. Do not take any diarrhoea medicine without first checking with your doctor.
- If you get a sore, white mouth or tongue while taking, or soon after stopping Roxithromycin Sandoz, tell your doctor or pharmacist. Also tell your doctor or pharmacist if you get vaginal itching or discharge. This may mean you have a fungal/yeast infection called thrush. Sometimes the use of Roxithromycin Sandoz allows fungi/yeast to grow and the above symptoms to occur. Roxithromycin Sandoz does not work against fungi/yeast.
- Tell all the doctors, dentists and pharmacists who are treating you that you are taking Roxithromycin Sandoz.
- If you are about to start taking any new medicine, tell your doctor and pharmacist that you are taking Roxithromycin Sandoz
- If you plan to have surgery that needs a general anaesthetic tell your doctor or dentist that you are taking this medicine.
Call your doctor straight away if you:
- become pregnant while you are taking Roxithromycin Sandoz, tell your doctor or pharmacist immediately.
Things you should not do
- Do not take more than the recommended dose unless your doctor or pharmacist tells you to.
- Do not give this medicine to anyone else, even if they have the same condition as you.
- Do not use this medicine to treat any other complaints unless your doctor tells you to.
- Do not stop taking your tablets because you are feeling better, unless advised by your doctor or pharmacist.
If you do not complete the full course prescribed by your doctor, all of the bacteria causing your infection may not be killed. These bacteria may continue to grow and multiply so that your infection may not clear completely or it may return.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how Roxithromycin Sandoz affects you.
Drinking alcohol
Tell your doctor if you drink alcohol.
Looking after your medicine
- Keep the medicine in a cool dry place where the temperature stays below 25°C.
- Keep your tablets in the blister pack until it is time to take them.
Follow the instructions in the carton on how to take care of your medicine properly.
Store it in a cool dry place away from moisture, heat or sunlight; for example, do not store it:
- in the bathroom or near a sink, or
- in the car or on window sills.
Do not use this medicine after the expiry date.
Keep it where young children cannot reach it.
Getting rid of any unwanted medicine
If you no longer need to use this medicine or it is out of date, take it to any pharmacy for safe disposal.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
Fungal related
| Speak to your doctor if you have any of these less serious side effects and they worry you. They are generally mild and short-lived. |
Serious side effects
| Serious side effects | What to do |
Gut or Gastrointestinal related
| Tell your doctor or pharmacist immediately if you notice any of the following, particularly if they occur several weeks after stopping treatment with Roxithromycin Sandoz. These are rare but serious side effects. You may have a serious condition affecting your bowel. Therefore, you may need urgent medical attention Do not take any diarrhoea medicine without first checking with your doctor. |
Infection related
| Stop taking this medicine and call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. These are very serious side effects. If you have them, you may have had a serious allergic reaction to Roxithromycin Sandoz. You may need urgent medical attention or hospitalisation. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What Roxithromycin Sandoz contains
| Active ingredient (main ingredient) | roxithromycin |
| Other ingredients (inactive ingredients) |
|
| Potential allergens |
|
Do not take this medicine if you are allergic to any of these ingredients.
What Roxithromycin Sandoz looks like
Roxithromycin Sandoz 150 mg – white, round, convex film-coated tablets, scored on one side, embossment R150 on the other side. Pack size of 10 tablets (Aust R100989).
Roxithromycin Sandoz 300 mg – white, round, convex film-coated tablets, scored on one side, embossment R300 on the other side. Pack size of 5 tablets (AUST R 101028).
Who distributes Roxithromycin Sandoz
Sandoz Pty Ltd
100 Pacific Highway
North Sydney, NSW 2060
Australia
Tel: 1800 726 369
This leaflet was revised in January 2026.
®Registered Trade Mark. The trade marks mentioned in this material are the property of their respective owners.
Brand Information
| Brand name | Roxithromycin Sandoz |
| Active ingredient | Roxithromycin |
| Schedule | S4 |
MIMS Revision Date: 01 March 2026
1 Name of Medicine
Roxithromycin.
2 Qualitative and Quantitative Composition
Each Roxithromycin Sandoz 150 mg film-coated tablets contains 150 mg roxithromycin.
Each Roxithromycin Sandoz 300 mg film-coated tablets contains 300 mg roxithromycin.
It is a white crystalline powder.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Roxithromycin Sandoz 150 mg film-coated tablets. White, round, convex film-coated tablets, scored on one face, embossment R 150.
Roxithromycin Sandoz 300 mg film-coated tablets. White, round, convex film-coated tablets, scored on one face, embossment R 300.
4 Clinical Particulars
4.1 Therapeutic Indications
Adults. Roxithromycin Sandoz is indicated for the treatment of the following types of mild to moderately severe infections in adults caused by or likely to be caused by susceptible microorganisms.
Upper respiratory tract infection: acute pharyngitis, tonsillitis and sinusitis.
Lower respiratory tract infection: acute bronchitis and acute exacerbations of chronic bronchitis; community acquired pneumonia.
Skin and skin structure infections.
Nongonococcal urethritis.
Children. Roxithromycin Sandoz 150 mg tablets are indicated for the treatment of the following mild to moderately severe infections in children caused by or likely to be caused by susceptible microorganisms: acute pharyngitis; acute tonsillitis; impetigo.
Appropriate culture and sensitivity tests should be performed when necessary to determine organism susceptibility and thus treatment suitability. Therapy with roxithromycin may be initiated before results of these tests are known; once results become available, appropriate therapy should be continued.
4.2 Dose and Method of Administration
Dosage. Adults. The recommended dosage is 300 mg per day which may be taken according to one of the following dosage regimens.
Usual dosage. Roxithromycin Sandoz 300 mg tablets: one tablet daily.
Roxithromycin Sandoz 150 mg tablets: one tablet twice daily, or two tablets once daily.
For atypical pneumonia, the recommended dosage is 150 mg twice daily.
The usual duration of treatment is five to ten days depending on the indication and clinical response. Streptococcal throat infections require at least ten days of therapy. A small proportion of patients with nongonococcal genital infections may require 20 days for complete cure.
Children. The recommended dose and duration of treatment should not be exceeded in children (see Section 4.4 Special Warnings and Precautions for Use).
Roxithromycin Sandoz is administered twice daily at a dose of 5 to 8 mg/kg/day. Recommended dosage regimens are as follows.
40 kg and over. One Roxithromycin Sandoz 150 mg tablet morning and evening. Roxithromycin Sandoz is not recommended for children of under 40 kg.
The usual duration of treatment is five to ten days depending on the indication and clinical response. Streptococcal throat infections require ten days of therapy. The duration of treatment should not exceed ten days.
Method of administration. Roxithromycin Sandoz should be taken at least 15 minutes before food or on an empty stomach (i.e. more than three hours after a meal).
Roxithromycin Sandoz 150 mg and 300 mg film-coated tablets must be swallowed whole with a drink.
Dosage adjustment. Renal impairment. Roxithromycin Sandoz 300 mg tablets: one tablet daily.
Roxithromycin Sandoz 150 mg tablets: one tablet twice daily or two tablets once daily.
Elderly. Roxithromycin Sandoz 300 mg tablets: one tablet daily.
Roxithromycin Sandoz 150 mg tablets: one tablet twice daily or two tablets once daily.
4.3 Contraindications
Hypersensitivity to roxithromycin, macrolides, including erythromycin or to any of the excipients.
Severely impaired hepatic function (see Section 4.4 Special Warnings and Precautions for Use).
Concomitant therapy with vasoconstrictive ergot alkaloids (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Coadministration with medicinal products with narrow therapeutic windows and which are substrates of CYP3A4 (e.g. astemizole, cisapride, pimozide and terfenadine) (see Section 4.4 Special Warnings and Precautions for Use).
4.4 Special Warnings and Precautions for Use
Roxithromycin, like erythromycin, has been shown in vitro to elicit a concentration dependent lengthening in cardiac action potential duration. Such an effect is manifested only at supratherapeutic concentrations. Accordingly, the recommended doses should not be exceeded.
Prolonged or repeated use of antibiotics including roxithromycin may result in superinfection by resistant organisms. In the event of superinfection, roxithromycin should be discontinued and appropriate therapy instituted.
When indicated, incision, drainage or other appropriate surgical procedures should be performed in conjunction with antibiotic therapy.
Antibiotic associated pseudomembranous colitis has been reported with many antibiotics. A toxin produced by Clostridium difficile appears to be the primary cause.
Clostridium difficile-associated disease: diarrhoea, particularly if severe, persistent and/or bloody, during or after treatment with roxithromycin, may be symptomatic of pseudomembranous colitis (see Section 4.8 Adverse Effects (Undesirable Effects)). If pseudomembranous colitis is suspected, roxithromycin must be stopped immediately.
The severity of the colitis may range from mild to life threatening. It is important to consider this diagnosis in patients who develop diarrhoea particularly if severe, persistent and/or bloody, or colitis in association with antibiotic use (this may occur during treatment and up to several weeks after cessation of antibiotic therapy). Mild cases usually respond to drug discontinuation alone. However, in moderate to severe cases, appropriate therapy with a suitable oral antibacterial agent effective against Clostridium difficile should be considered. Fluids, electrolytes and protein replacement therapy should be provided when indicated.
Drugs that delay peristalsis, e.g. opiates and diphenoxylate with atropine (e.g. Lomotil), may prolong and/or worsen the condition and should not be used.
As with other macrolides, roxithromycin may have the potential to aggravate myasthenia gravis.
Cases of severe bullous skin reactions such as Stevens-Johnson Syndrome or Toxic Epidermal Necrosis have been reported with roxithromycin (see Section 4.8 Adverse Effects (Undesirable Effects)). If symptoms or signs of SJS or TEN (e.g. progressive skin rash often with blisters or mucosal lesions) are present, roxithromycin treatment should be discontinued.
Severe vasoconstriction ("ergotism") with possibly necrosis of the extremities has been reported when macrolides antibiotics have been associated with vasoconstrictive ergot alkaloids. Absence of treatment by these alkaloids must always be checked before prescribing roxithromycin.
Increased INR levels have been reported in patients when roxithromycin and coumarin anticoagulants are used concomitantly. Patients using roxithromycin and coumarin anticoagulants should be closely monitored (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Prolongation of the QT interval. Ventricular arrhythmias associated with prolonged QT interval, including ventricular tachycardia and torsades de pointes have been reported with macrolide antibiotics including roxithromycin.
Prescribers should consider the risk of QT prolongation (which can be fatal) when weighing the risks and benefits of roxithromycin for at-risk groups including:
Patients predisposed to QT interval prolongation such as those with a history of torsades de pointes or congenital long QT syndrome.
Patients taking other medication known to prolong the QT interval such as antiarrhythmics of classes IA and III; antipsychotic agents; antidepressants; and fluoroquinolones.
Patients with electrolyte disturbance, particularly in cases of hypokalaemia and hypomagnesaemia.
Patients with clinically relevant bradycardia, cardiac arrhythmia or cardiac insufficiency.
Carefully consider the balance of benefits and risks before prescribing roxithromycin or other macrolides for any patients taking hydroxychloroquine or chloroquine, because of the potential for an increased risk of cardiovascular events and cardiovascular mortality (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions).
Monitoring of the liver and kidney function and the blood counts is recommended especially during long-term treatment.
Use in hepatic impairment. The safety of roxithromycin has not been demonstrated in patients with impaired hepatic function. Caution should be exercised if Roxithromycin Sandoz is administered to patients with impaired hepatic function, in severe cases, use of roxithromycin is not recommended. If administered to patients with severely impaired hepatic function (e.g. hepatic cirrhosis with jaundice and/or ascites), consideration should be given to reducing the daily dosage to half the usual dosage.
Use in renal impairment. The safety of roxithromycin has not been demonstrated in patients with impaired renal function. Caution should be exercised if roxithromycin is administered to patients with impaired renal function.
Renal excretion of roxithromycin and its metabolites accounts for a small amount of an oral dose. The dosage should be kept unchanged in renal insufficiency.
Use in the elderly. No dosage adjustment is required in elderly patients.
Paediatric use. In young animal studies, high oral doses of roxithromycin were associated with bone growth plate abnormalities. However no abnormalities were observed in the animals at doses resulting in unbound plasma roxithromycin concentrations that were 10 to 15 times higher than the unbound concentration measured in children receiving the therapeutic dose. The maintenance of such safety margins is primarily dependent on high affinity binding of roxithromycin to plasma alpha-1 acid glycoprotein and will be compromised by any circumstances attenuating the extent of this binding. It is recommended that the approved paediatric dosage regimen (i.e. 5 to 8 mg/kg/day for a maximum of ten days) be adhered to strictly.
Neutropenia was observed in children treated with roxithromycin. 31.6% of 402 children in clinical trials had a neutrophil count below the lower limit of the normal range (3,500/mm3) at the conclusion of therapy with roxithromycin. Of these, 4% had a neutrophil count of less than 1,500/mm3 and 1.2% had a count of less than 1,000/mm3. It is not known whether this is an effect of the drug, or whether it reflects a normal fluctuation of the neutrophil count or a response to infection in children.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Roxithromycin has a much lower affinity for cytochrome P450 than erythromycin, and consequently has fewer interactions. Interactions may be observed, however, with drugs that bind to alpha-1 acid glycoprotein, e.g. disopyramide.
Roxithromycin does not appear to interact with oral contraceptives containing oestrogens and progestogens, prednisolone, carbamazepine, ranitidine or antacids.
Ergot alkaloids. Reactions of ergotism with possible peripheral necrosis have been reported after concomitant therapy of macrolides with vasoconstrictive ergot alkaloids, particularly ergotamine and dihydroergotamine. Because a clinical interaction with roxithromycin cannot be excluded, administration of roxithromycin to patients taking ergot alkaloids is contraindicated. Absence of treatment with these alkaloids must always be checked before prescribing roxithromycin.
Theophylline. A study in normal subjects, concurrently administered roxithromycin and theophylline, has shown some increase in the plasma concentration of the latter. While a change in dosage is usually not required, patients with high levels of theophylline at commencement of treatment should have levels monitored.
Disopyramide. An in vitro study has shown that roxithromycin can displace protein bound disopyramide; such an effect in vivo could result in increased serum levels of disopyramide. Consequently ECG and, if possible, disopyramide serum levels should be monitored.
Terfenadine. Some macrolide antibiotics (e.g. erythromycin) may increase serum levels of terfenadine. This can result in severe cardiovascular adverse events, including QT prolongation, torsades de pointes and other ventricular arrhythmias. Such a reaction has not been documented with roxithromycin, which has a much lower affinity for cytochrome P450 than erythromycin. However, in the absence of a systematic interaction study, concomitant administration of roxithromycin and terfenadine is not recommended.
Astemizole, cisapride, pimozide. Other drugs, such as astemizole, cisapride or pimozide, which are metabolised by the hepatic isozyme CYP3A4, have been associated with QT interval prolongation and/or cardiac arrhythmias (typically torsades de pointes) as a result of an increase in their serum level subsequent to interaction with significant inhibitors of this isozyme, including some macrolide antibacterials. Although roxithromycin has no or limited ability to complex CYP3A4 and therefore to inhibit the metabolism of other drugs processed by this isozyme, a potential for clinical interaction of roxithromycin with the above mentioned drugs cannot be either ascertained or ruled out in confidence; therefore, concomitant administration of roxithromycin and such drugs is not recommended.
Roxithromycin, like other macrolides, should be used with caution in patients receiving class IA and class III antiarrhythmic agents (see Section 4.4 Special Warnings and Precautions for Use).
Vitamin K antagonists. While no interaction was observed in volunteer studies, roxithromycin appears to interact with warfarin. Increases in prothrombin time (international normalised ratio (INR)) have been reported in patients treated concomitantly with roxithromycin and warfarin or the related vitamin K antagonist phenprocoumon, and severe bleeding episodes have occurred as a consequence. INR should be monitored during combined treatment with roxithromycin and vitamin K antagonists.
Hydroxychloroquine or chloroquine. Observational data have shown that co-administration of azithromycin with hydroxychloroquine in patients with rheumatoid arthritis is associated with an increased risk of cardiovascular events and cardiovascular mortality. Because of the potential for a similar risk with other macrolides when used in combination with hydroxychloroquine or chloroquine, careful consideration should be given to the balance of benefits and risks before prescribing roxithromycin for any patients taking hydroxychloroquine or chloroquine.
Digoxin and other cardiac glycosides. A study in healthy volunteers has shown that roxithromycin may increase the absorption of digoxin. This effect, common to other macrolides, may very rarely result in cardiac glycoside toxicity. This may be manifested by symptoms such as nausea, vomiting, diarrhoea, headache or dizziness; cardiac glycoside toxicity may also elicit heart conduction and/or rhythm disorders. Consequently, in patients treated with roxithromycin and digoxin or another cardiac glycoside, ECG and, if possible, the serum level of the cardiac glycoside should be monitored; this is mandatory if symptoms which may suggest cardiac glycoside overdosage occur.
HMG-CoA reductase inhibitors. When roxithromycin and an HMG-CoA reductase inhibitor (statin) are combined, there is a potential risk of muscle related adverse events, such as rhabdomyolysis due to a possible increase of the statin exposure.
Caution should be exercised when a statin is combined with roxithromycin and patients should be monitored for signs and symptoms of myopathy.
Midazolam. Roxithromycin, like other macrolides, may increase the area under the midazolam concentration time curve and the midazolam half-life, therefore the effects of midazolam may be enhanced and prolonged in patients treated with roxithromycin. There is no conclusive evidence for an interaction between roxithromycin and triazolam.
Bromocriptine. Roxithromycin may increase the AUC and plasma concentrations of bromocriptine, which could lead to an increased risk for adverse effects of the compound.
Rifabutin. Roxithromycin can increase the plasma concentration of rifabutin.
Theophylline and cyclosporin. A slight increase in plasma concentrations of theophylline or cyclosporin A has been observed. This does not generally necessitate altering the usual dosage.
CYP3A. Roxithromycin is a weak CYP3A inhibitor. The effect of roxithromycin on exposure to drugs predominantly cleared by CYP3A metabolism would be expected to be 2-fold or less. Caution should be exercised when roxithromycin is concomitantly prescribed with drugs metabolised by CYP3A (such as rifabutin and bromocriptine).
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. There was no effect on the fertility of rats treated with roxithromycin at oral doses up to 180 mg/kg/day.
Use in pregnancy. (Category B1)
Reproductive studies in rats, mice and rabbits at doses of 100, 400 and 135 mg/kg/day, respectively, did not demonstrate evidence of developmental abnormalities. In rats, at doses above 180 mg/kg/day, there was evidence of embryotoxicity and maternotoxicity. The safety of roxithromycin for the human fetus has not been established.
Use in lactation. Small amounts of roxithromycin are excreted in the breast milk. Breastfeeding or treatment of the mother should be discontinued as necessary.
4.7 Effects on Ability to Drive and Use Machines
Attention should be drawn to the possibility of dizziness, visual impairment and blurred vision.
4.8 Adverse Effects (Undesirable Effects)
Roxithromycin is generally well tolerated. In clinical trials, treatment discontinuation due to adverse reactions occurred in only 1.2% of adult patients and 1.0% of children. The following side effects or serious adverse events possibly associated with roxithromycin have been reported.
Gastrointestinal. Nausea, vomiting, epigastric pain (dyspepsia), diarrhoea (sometimes containing blood), anorexia, flatulence, pseudomembranous colitis. In clinical studies, the incidence of gastrointestinal events was higher with the 300 mg once daily dosage regimen than with 150 mg twice daily. Symptoms of pancreatitis have been observed; most patients had received other drugs for which pancreatitis is a known adverse reaction.
Hypersensitivity. Urticaria, rash, pruritus, angioedema. Rarely, serious allergic reactions may occur, e.g. asthma, bronchospasm, anaphylactic like reactions, anaphylactic shock, purpura, glottic oedema, generalised oedema, erythema multiforme, exfoliative dermatitis, acute generalised exanthematous pustulosis (AGEP), Stevens-Johnson syndrome, and Toxic Epidermal Necrosis (TEN) (see Section 4.4 Special Warnings and Precautions for Use).
Hepatic. Moderate increases in serum transaminases (AST and ALT) and/or alkaline phosphatase levels have been observed and are somewhat more likely to occur in the elderly (> 65 years). Acute cholestatic hepatitis and acute hepatocellular injury (sometimes with jaundice) are rarely reported.
Infections and infestations. Superinfection (on prolonged use), Clostridium difficile colitis (pseudomembranous colitis).
Blood and lymphatic system disorders. Eosinophilia, agranulocytosis, neutropenia, thrombocytopenia.
Immune system disorders. Anaphylactic shock.
Cardiac disorders. QT interval prolongation, ventricular tachycardia, Torsade de pointes.
Other. Bronchospasm, hallucination, confusion, headache, dizziness, paraesthesia, tinnitus, malaise, moniliasis (candidiasis), pancreatitis, disorders of taste and/or smell, visual impairment, blurred vision, temporary deafness, hypoacusis and vertigo.
Prolonged use of antibiotics including roxithromycin may result in superinfection; overgrowth of non-susceptible organisms. Repeated evaluation of the patient's condition is essential. In the event of superinfection, appropriate measures should be taken.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
Symptomatic treatment should be provided as required. There is no specific antidote.
For information on the management of overdose, contact the Poison Information Centre on 131126 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Roxithromycin is a semisynthetic macrolide antibiotic.
Mechanism of action. Microbiology. Roxithromycin is bacteriostatic at low concentrations and bactericidal at high concentrations. It binds to the 50S subunit of the 70S ribosome, thereby disrupting bacterial protein synthesis.
A prolonged postantibiotic effect has been observed with roxithromycin. Whilst the clinical significance of this remains uncertain, it supports the rationale for once daily dosing. Although clinical data have demonstrated the efficacy and safety of once daily dosing in adults, these have not been demonstrated in children.
At plasma concentrations achieved with the recommended therapeutic doses, roxithromycin has been demonstrated to have in vitro and clinical activity against the following microorganisms: Streptococcus pneumoniae, Strep. pyogenes, Mycoplasma pneumoniae, Moraxella catarrhalis, Ureaplasma urealyticum and Chlamydia sp.
Roxithromycin has been demonstrated to have clinical activity against the following microorganisms which are partially sensitive in vitro to roxithromycin: Haemophilus influenzae and Staphylococcus aureus, except methicillin resistant Staph. aureus (MRSA).
The following strains of microorganisms are resistant: multiresistant Staph. aureus, Enterobacteriaceae, Pseudomonas sp. and Acinetobacter sp.
Susceptibility testing. Dilution or diffusion techniques. Either quantitative (MIC) or breakpoint, should be used following a regularly updated, recognised and standardised method (e.g. NCCLS). Standardised susceptibility test procedures require the use of laboratory control microorganisms to control the technical aspects of the laboratory procedures.
A report of 'susceptible' indicates that a pathogen is likely to be inhibited if the antimicrobial compound in the blood reaches the concentrations usually achievable. A report of 'intermediate' indicates that the result should be considered equivocal, and if the microorganism is not fully susceptible to alternative, clinically feasible drugs, the test should be repeated. This category implies possible clinical applicability in body sites where the drug is physiologically concentrated or in situations where high dosage of drug can be used. This category also provides a buffer zone, which prevents small uncontrolled technical factors from causing major discrepancies in interpretation. A report of 'resistant' indicates that the pathogen is not likely to be inhibited if the antimicrobial compound in the blood reaches the concentrations usually achievable; other therapy should be selected.
Note. The prevalence of resistance may vary geographically for selected species and local information on resistance is desirable, particularly when treating severe infections.
Using the National Committee for Clinical Laboratory Standard (NCCLS) method of susceptibility testing with a 15 microgram roxithromycin disc, susceptible organisms other than Haemophilus influenzae produce zones of inhibition 21 mm or greater. A zone size of 10 to 20 mm should be considered intermediate and a zone size of 9 mm or less indicates resistance. A bacterial isolate may be considered susceptible if the MIC value for roxithromycin is less than or equal to 1 mg/L. Organisms are considered resistant if the MIC value is greater than 8 mg/L.
For Haemophilus influenzae, zones of inhibition 10 mm or greater indicate susceptibility when CO2 incubation and the HTM agar is used with a 15 microgram roxithromycin disc. An isolate may be considered susceptible if the MIC value for roxithromycin is less than or equal to 8 mg/L.
Clinical trials. No data available.
5.2 Pharmacokinetic Properties
Absorption. Roxithromycin is absorbed after oral administration with an absolute bioavailability of approximately 50%. Peak plasma concentrations following administration of 150 and 300 mg film coated tablets are achieved in young and elderly adult patients approximately one to two hours postdose.
As food intake delays absorption, Roxithromycin Sandoz should be administered at least 15 minutes before food or, alternatively, on an empty stomach (i.e. more than three hours after a meal).
Absorption is not linear; with increasing doses in the range 150 to 300 mg, peak plasma levels and area under the curve (AUC) do not increase in proportion to the dose.
After repeated administration of 2.5 mg/kg every 12 hours to children, the average peak plasma concentration at steady state was 9 mg/L and the AUC was 61 mg.h/L.
Following administration of a single oral dose of roxithromycin 150 mg to healthy young adults, the mean peak plasma concentration was 6.6 mg/L and the AUC was 69 mg.h/L. At steady state following doses of 150 mg twice daily, the mean peak plasma concentration was 9.3 mg/L and the AUC was 71 mg.h/L.
In elderly patients, the mean peak plasma concentration following a single 150 mg dose was 9.1 mg/L and the AUC was 148 mg.h/L. At steady state, a dosage regimen of 150 mg twice daily produced a mean peak plasma concentration of 11.3 mg/L and an AUC of 83 mg.h/L.
Following administration of a single oral dose of roxithromycin 300 mg to healthy young adults, the mean peak plasma concentration was 9.7 mg/L and the AUC was 98 mg.h/L. At steady state following doses of 300 mg once daily, the mean peak plasma concentration was 10.9 mg/L and the AUC was 77 mg.h/L.
In elderly patients, the mean peak plasma concentration following a single 300 mg dose was 10.8 mg/L and the AUC was 197 mg.h/L.
After administration of a single oral dose of Roxithromycin Sandoz 150 mg to healthy male and female adults, the mean peak plasma concentration was 6.58 mg/L and the AUC was 94.98 mg.hour/L.
After administration of a single oral dose of Roxithromycin Sandoz 300 mg to healthy male and female adults, the mean peak plasma concentration was 10.10 mg/L and the AUC was 143.48 mg.hour/L.
Distribution. Roxithromycin is 92 to 96% bound to plasma proteins (principally alpha-1 acid glycoprotein, but also albumin) at concentrations less than 4.2 mg/L. The binding is saturable; in subjects with normal plasma levels of alpha-1 acid glycoprotein, the extent of binding decreases when plasma concentrations of roxithromycin exceed 4.2 mg/L. At a plasma concentration of 8.4 mg/L approximately 87% of the drug is protein bound.
Roxithromycin is highly concentrated in polymorphonuclear leucocytes and macrophages, where levels 30 times those in serum have been reported.
Metabolism. Roxithromycin undergoes limited metabolism in the body, presumably in the liver. The major metabolite is descladinose roxithromycin. Two minor metabolites have also been identified. Plasma levels of roxithromycin are approximately twice those of all metabolites; a similar ratio is seen in the urine and faeces.
Approximately 7% of a dose is excreted in the urine and 13% is eliminated via the lungs. Faecal excretion, which represents the unabsorbed fraction and the small proportion excreted by the liver, accounts for approximately 53% of the dose. The fate of the remainder is unknown.
When roxithromycin plasma levels are above 4.2 mg/L, renal clearance increases because reduced plasma protein binding (see Distribution) causes increased levels of unbound roxithromycin which may be excreted by the kidneys.
Excretion. The mean half-life of roxithromycin is approximately 12 hours in young adults and 20 hours in children. The apparently longer half-life in children does not cause excessive accumulation; minimum concentration (Cmin) and AUC values are comparable for adults and children.
The half-life is prolonged to 25 hours in patients with impaired hepatic function and 18 hours in patients with renal insufficiency.
The mean half-life in elderly patients is approximately 27 hours.
5.3 Preclinical Safety Data
Genotoxicity. Roxithromycin has shown no mutagenic potential in standard laboratory tests for gene mutation and chromosomal damage.
Carcinogenicity. Long-term studies in animals have not been performed to evaluate the carcinogenic potential of roxithromycin.
6 Pharmaceutical Particulars
6.1 List of Excipients
Roxithromycin Sandoz tablets also contain inactive (excipients) ingredients: microcrystalline cellulose, povidone, croscarmellose sodium, silicon dioxide, lactose monohydrate, hypromellose, titanium dioxide, magnesium stearate, macrogol 4000, poloxamer.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
For information on interactions with other medicines and other forms of interactions, see Section 4.5.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C.
6.5 Nature and Contents of Container
Roxithromycin Sandoz 150 mg film-coated tablets. Available in PVC/Al blister packs of 10 tablets.
Roxithromycin Sandoz 300 mg film-coated tablets. Available in PVC/Al blister packs of 5 tablets.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of in accordance with local requirements.
6.7 Physicochemical Properties
Chemical structure. The chemical name of roxithromycin is erythromycin- [O-[(2-methoxyethoxy)- methyl]oxime]. Its molecular formula is C41H76N2O15 (MW: 837.1) and its chemical structure is:
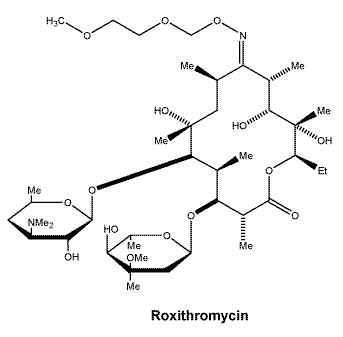
7 Medicine Schedule (Poisons Standard)
S4 - Prescription Only Medicine.
Date of First Approval
11 July 2006
Date of Revision
15 January 2026
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.