Suxamethonium Juno
Brand Information
| Brand name | Suxamethonium Juno |
| Active ingredient | Suxamethonium chloride dihydrate |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Suxamethonium Juno.
Summary CMI
SUXAMETHONIUM JUNO
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I given Suxamethonium Juno?
Suxamethonium Juno contains the active ingredient Suxamethonium. Suxamethonium Juno is used to stop your muscles moving during surgery or medical procedures
For more information, see Section 1. Why am I given Suxamethonium Juno? in the full CMI.
2. What should I know before I am given Suxamethonium Juno?
Do not use if you have ever had an allergic reaction to Suxamethonium or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I am given Suxamethonium? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with Suxamethonium Juno and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How will I be given Suxamethonium Juno?
Suxamethonium Juno is an injection and will be given to you by an anaesthetist. It will not be given to you until you are asleep from an anaesthetic.
More instructions can be found in Section 4. How will I be given Suxamethonium Juno? in the full CMI.
5. What should I know while using Suxamethonium Juno?
| Things you should do |
|
| Driving or using machines |
|
For more information, see Section 5. What should I know while using Suxamethonium Juno? in the full CMI.
6. Are there any side effects?
All Medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
Some of the more common and/or serious side effects are:
| Mild side effects | Serious side effects |
|
|
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
SUXAMETHONIUM JUNO
Active ingredient: Suxamethonium
Consumer Medicine Information (CMI)
This leaflet provides important information about using Suxamethonium Juno. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using Suxamethonium Juno.
Where to find information in this leaflet:
1. Why am I given Suxamethonium Juno?
2. What should I know before I am given Suxamethonium Juno?
3. What if I am taking other medicines?
4. How will I be given Suxamethonium Juno?
5. What should I know while using Suxamethonium Juno?
6. Are there any side effects?
7. Product details
1. Why am I given Suxamethonium Juno?
Suxamethonium Juno contains the active ingredient Suxamethonium. Suxamethonium Juno belongs to a group of medicines called neuromuscular blockers which work by stopping messages being sent from the nerves to the muscles.
Suxamethonium Juno is used to stop your muscles moving during surgery or medical procedures.
2. What should I know before I am given Suxamethonium Juno?
Warnings
Do not use Suxamethonium Juno if:
- you are allergic to Suxamethonium, or any of the ingredients listed at the end of this leaflet.
- Always check the ingredients to make sure you can use this medicine.
- Have an allergy to or any other related medicines.
You should not be given Suxamethonium Juno if you have or have had:
- Severe muscle stiffness and fever (malignant hyperthermia)
- A family history or malignant hyperthermia
- Muscle disease or weakness (e.g. myasthenia gravis ormuscular dystrophy, cerebral palsy, muscle wastingdisease, paralysis, motor neurone disesase)
- Glaucoma (increased pressure in the eye)
- Eye injuries
- Recent paraplegia
- Liver or kidney problems
- Severe burns
- High blood levels of potassium
- Prolonged infections
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
You should not be given Suxamethonium Juno if you are pregnant or breastfeeding unless your doctor says so
Check with your doctor if you are pregnant or intend to become pregnant.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
As with many medicines, Suxamethonium Juno may harm your developing or breastfeeding baby.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with Suxamethonium Juno and affect how it works.
- Quinine
- Chloroquine, hydroxychloroquine
- Contraceptive pill
- Medicines containing oestrogen
- Medicines for depression or mental illness
- Medicines for epilepsy or seizures e.g. phenytoin
- Some antibiotics
- Diuretics
- Corticosteroids
- Medicines for reflux or stomach ulcers e.g. cimetidine
- Asthma reliever medication e.g. Bricanyl®
- Medicines for high blood pressure or heart problems
- Quinidine or digoxin or verapamil
- Magnesium salts
- Eye drops for glaucoma
- Some anticancer medicines
- Medicines to treat Alzheimer's disease
- Medicines to treat myasthenia gravis
- Medicines for coughs, cold, sleeping or tablets for allergies
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect Suxamethonium Juno.
4. How will I be given Suxamethonium Juno?
How you are given Suxamethonium Juno
Suxamethonium Juno will be given to you by an anaesthetist. It will not be given to you until you are asleep from an anaesthetic.
It will be given by injection into your bloodstream or muscles. The dose you will be given will be carefully worked out depending on the length of the procedure, and your body weight. Children will be given reduced amounts of Suxamethonium Juno.
Since Suxamethonium Juno will stop your muscles moving, it may be necessary for the anaesthetist to help you breath while you are being given it.
If you are given too much Suxamethonium Juno
The anaesthetist giving you Suxamethonium Juno will be experiences in its use, so it will be extremely unlikely that you will be given too much.
Suxamethonium Juno doses should be carefully worked out, so problems with overdose are unlikely. There is another medicine called neostigmine which can be used if needed to reverse the effects of too much Suxamethonium Juno
5. What should I know while using Suxamethonium Juno?
Things you should do
Tell your doctor if you have any of these medical conditions:
- Heart or lung problems
- Malnutrition or severe dehydration
- Reduced red blood cells and iron stores (anaemia)
- Under-active thyroid gland
- Liver or kidney problems
- Fever
- Paraplegia
- Severe injuries
- Cancer
- Skin diseases
- Broken bones
- Muscle disease
- Severe burns
- Imbalance in the body's blood chemistry
Tell your doctor if you have recently been in contact with weed killer or insecticides.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how Suxamethonium affects you.
Looking after your medicine
The hospital will store Suxamethonium Juno under the correction conditions
Keep it where young children cannot reach it.
Getting rid of any unwanted medicine
Your doctor or pharmacist will dispose of any Suxamethonium Juno that may be left over.
Do not use this medicine after the expiry date.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Mild side effects
| Mild side effects | What to do |
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What Suxamethonium Juno contains
| Active ingredient (main ingredient) | Suxamethonium chloride dihydrate |
| Other ingredients (inactive ingredients) | Water for injections Hydrochloric acid for pH adjustment |
Do not take this medicine if you are allergic to any of these ingredients.
What Suxamethonium Juno looks like
Suxamethonium Juno is a clear, colourless solution supplied in 2 mL glass ampoules.
Suxamethonium is supplied as:
Suxamethonium Juno 100 mg/2mL injection (AUST R 320687)
Who distributes Suxamethonium Juno
Juno Pharmaceuticals Pty Ltd
15-17 Chapel Street,
Cremorne,
VIC 3121
www.junopharm.com.au
This leaflet was prepared in March 2026
Brand Information
| Brand name | Suxamethonium Juno |
| Active ingredient | Suxamethonium chloride dihydrate |
| Schedule | S4 |
MIMS Revision Date: 01 April 2026
1 Name of Medicine
Suxamethonium chloride dihydrate.
2 Qualitative and Quantitative Composition
2 mL sterile solution of pH 3.0-5.0 containing 100 mg of suxamethonium chloride dihydrate. Suxamethonium chloride dihydrate is a white or almost white, crystalline powder.
For the full list of excipients, see Section 6.1.
3 Pharmaceutical Form
Injection solution. Clear, colourless solution.
4 Clinical Particulars
4.1 Therapeutic Indications
For the production of skeletal muscle relaxation in anaesthesia. Suited for procedures requiring only brief relaxation such as endotracheal intubation, endoscopic examinations, orthopaedic manipulations, short surgical procedures and electro-convulsive therapy.
4.2 Dose and Method of Administration
Dosage is individualised and its administration should be determined after careful assessment of the patient. The dose of suxamethonium is dependent on bodyweight, the degree of muscle relaxation required and the response of individual patients. Suxamethonium causes paralysis of the respiratory muscles, therefore after administration, respiration must be controlled. It should not be administered to a conscious patient.
Suxamethonium should not be mixed with any neuromuscular blocking agent, nor with general anaesthetics such as short acting barbiturates (especially thiopental), nor any other therapeutic agent in the same syringe.
Suxamethonium Chloride Injection contains no antimicrobial agent. It should be used only once and any residue discarded.
An initial test dose of 0.1 mg/kg may be given intravenously to determine the patients response.
Adult. For short procedures, such as endotracheal intubation the usual adult dose is 0.6 mg/kg (range 0.3-1.1 mg/kg) administered IV over 10 to 30 seconds. This dose produces muscle relaxation in about 60 seconds and has a duration of approximately 4 to 6 minutes. Larger doses produce more prolonged muscle relaxation.
For more prolonged surgical procedures in an adult, suxamethonium is commonly given by IV infusion at a rate of 2.5-4.3 mg/minute. When given by intravenous infusion suxamethonium should be diluted to 0.1 to 0.2% (1-2 mg/mL) in 5% dextrose solution or sterile isotonic saline.
Children. Neonates and premature infants may be relatively resistant to suxamethonium.
The usual paediatric IV dose is 1 to 2 mg/kg. If necessary, additional doses maybe administered in accordance with the patient's response. Continuous IV infusions of suxamethonium are considered unsafe in neonates and children because of the risk of inducing malignant hyperthermia.
Intravenous bolus in children may result in profound bradycardia or on occasion asystole. This tends to be more common after a second dose. Pre-treatment with atropine can reduce the risk of bradycardia.
When a suitable vein is inaccessible, suxamethonium may occasionally be given by intramuscular injection. A suggested i.m. dose for adults and children may be up to 2.5 mg/kg but the total dose should not exceed 150 mg.
Diluted solutions of suxamethonium must be used within 24 hours of preparation. Discard unused solutions.
4.3 Contraindications
Suxamethonium is contraindicated in patients with a personal or familial history of malignant hyperthermia. Suxamethonium can trigger sustained myofibrillar contractions in susceptible individuals. If this occurs, all anaesthetic agents known to be associated with it (including suxamethonium) must be stopped and full supportive measures implemented immediately (see Section 4.4 Special Warnings and Precautions for Use, Malignant hyperthermia).
Suxamethonium is contraindicated in patients with genetically determined disorders of pseudocholinesterase, inherited atypical or low serum level of pseudocholinesterase. Prolonged and intensified neuromuscular blockade following suxamethonium administration may occur secondary to reduced plasma cholinesterase in the following states or pathological conditions; end stage hepatic failure, acute or chronic renal failure.
Suxamethonium is contraindicated in patients with myopathies associated with elevated creatinine phosphokinase (CPK) values, Duchenne's muscular dystrophy (increased risk of malignant hyperthermia, ventricular dysrhythmias and cardiac arrest secondary to acute rhabdomyolysis with hyperkalaemia), known hypersensitivity to suxamethonium or any excipients listed, see Section 6.1 List of Excipients, severe hyperkalaemia, acute narrow-angle glaucoma, and the presence of penetrating eye injuries (suxamethonium may cause a slight, transient increase in intraocular pressure).
It is also contraindicated in patients after the acute phase of injury following major burns, or multiple trauma, renal impairment with a raised plasma-potassium concentration, or in those with extensive muscle degeneration such as recent paraplegia and severe long-lasting sepsis because such patients may become severely hyperkalaemic when given suxamethonium, resulting in cardiac arrhythmia or arrest.
Patients recovering from major trauma or severe burns; the period of greatest risk of hyperkalaemia is from about 5 to 90 days after the injury and may be further prolonged if there is delayed healing due to persistent infection.
Suxamethonium should not be administered to a patient who is not fully anaesthetised. Neuromuscular function should be monitored when suxamethonium is being used over a prolonged period.
Suxamethonium is contraindicated in patients with neurological deficits involving acute major muscle wasting (upper and/or lower motor neurone lesions); the potential for potassium release occurs within the first 6 months after the acute onset of the neurological deficit and correlates with the degree and extent of muscle paralysis. Patients who have been immobilised for prolonged periods of time may be at similar risk.
Suxamethonium is contraindicated in patients with cerebral palsy.
Suxamethonium is contraindicated in patients with a personal or family history of congenital myotonic diseases such as myotonia congenita and dystrophia myotonica (risk of severe myotonic spasms and rigidity).
4.4 Special Warnings and Precautions for Use
Suxamethonium should only be administered under strict supervision of an anaesthetist familiar with its actions, characteristics and hazards who is skilled in the management of artificial respiration and only when facilities are instantly available for endotracheal intubation and for providing adequate ventilation of the patient, including the administration of oxygen under positive pressure. Be prepared to assist or control respiration.
Suxamethonium has no effect on consciousness, pain threshold or cerebration. It should therefore only be used with adequate anaesthesia.
When suxamethonium is given as an infusion, this should be monitored with care to avoid overdose.
During prolonged administration of suxamethonium, it is recommended that the patient is fully monitored with a peripheral nerve stimulator in order to avoid overdosage.
Tachyphylaxis occurs after repeated administration of suxamethonium.
Suxamethonium should be used with caution in ill and cachectic patients, in patients with acid-base disturbances or electrolyte imbalance, parenchymatous liver disease, obstructive jaundice, carcinomatosis, in those in contact with certain insecticides, e.g. organophosphorous compounds and in those receiving therapeutic radiation.
Suxamethonium should be used with caution in patients with fractures or muscle spasms because the initial muscle fasciculations may cause additional trauma.
Suxamethonium has no direct effect on the myocardium, but by stimulation of both autonomic ganglia and muscarinic receptors suxamethonium may cause changes in cardiac rhythm, including cardiac arrest.
Cross-sensitivity. High rates of cross-sensitivity (greater than 50%) between neuromuscular blocking agents have been reported. Allergic and non-allergic severe anaphylactic reactions to neuromuscular blocking agents including suxamethonium have been reported during anesthesia induction, sometimes in subjects who have never been exposed to muscle relaxants. The reactions have in some cases been life-threatening and fatal.
The common clinical manifestations are cutaneous eruption i.e. rash, erythema, which are generalised or limited to the injection site. This may be further complicated by anaphylactic shock and/or bronchospasm. In some cases, the bronchospasm and/or anaphylactic shock are not associated by cutaneous manifestations.
The appearance of the first signs requires the definitive discontinuation of the administration of Suxamethonium if not already completed, and the initiation of symptomatic treatment. Due to the potential severity of these reactions, the necessary precautions, such as the immediate availability of appropriate emergency treatment, should be taken.
Therefore, where possible, before administering suxamethonium, hypersensitivity to other neuromuscular blocking agents should be excluded. Suxamethonium, should only be used when absolutely essential in susceptible patients. Patients who experience a hypersensitivity reaction under general anaesthesia should be tested subsequently for hypersensitivity to other neuromuscular blockers.
Malignant hyperthermia. The abrupt onset of malignant hyperthermia, a very rare hypermetabolic process of skeletal muscle, may be triggered by suxamethonium. Early premonitory signs include muscle rigidity, tachycardia, tachypnoea unresponsive to increased depth of anaesthesia, evidence of increased oxygen requirement and carbon dioxide production, rising temperature and metabolic acidosis.
On evidence of these symptoms the anaesthetic and suxamethonium should be discontinued and supportive measures implemented including administration of oxygen, sodium bicarbonate, lowering of temperature, restoration of fluids and electrolyte balance, maintenance of adequate urinary output and administration of IV dantrolene according to a standard protocol.
Hyperkalaemia. The effects of suxamethonium can be exacerbated by hyperkalemia.
Administration of suxamethonium causes an immediate rise in serum potassium. This rise is normally small but may be prolonged and exaggerated in patients taking beta-blockers.
Great caution should also be observed in patients with pre-existing hyperkalaemia or electrolyte imbalance, uraemia, hemiplegia, paraplegia, extensive burns, massive trauma, diffuse intracranial lesions (head injury, encephalitis, ruptured cerebral aneurysm), tetanus, acute anterior horn cell disease, extensive denervation of skeletal muscle due to disease or injury of the CNS, or who have degenerative neuromuscular disease and in severe long-lasting sepsis. Such patients may become severely hyperkalaemic when given suxamethonium, resulting in cardiac arrhythmia or arrest (see Section 4.3 Contraindications).
With burns or trauma, the period of greatest risk is from about 10-90 days after the injury, but may be prolonged further if there is delayed healing or persistent infection. These patients may still react abnormally to suxamethonium 2 years after the injury. In neuromuscular disease the greatest risk period is usually from 3 weeks to 6 months after onset, but severe hyperkalaemia may occur after 24 to 48 hours or later than 6 months. Patients with severe sepsis for more than a week should be considered at risk of hyperkalaemia and suxamethonium should not be given until the infection has cleared.
Hyperkalaemia rhabdomyolysis. There is a risk of cardiac arrest from hyperkalaemia due to rhabdomyolysis, particularly in male patients with muscular dystrophy.
Low plasma pseudocholinesterase. Recovery from suxamethonium may occasionally be delayed possibly due to a low serum pseudocholinesterase level, this may occur in patients suffering from severe liver disease, cancer, malnutrition, severe dehydration, collagen diseases, severe anaemia, myxoedema, burns, pregnancy and the puerperium, severe infections, myocardial infarction, renal impairment and abnormal body temperature.
Also, exposure to neurotoxic insecticides or weed killers, anti-malarial or anti-cancer drugs, monoamine oxidase (MAO) inhibitors, contraceptive pill, pancuronium, chlorpromazine, ecothiopate or neostigmine may result in low levels of pseudocholinesterase.
In patients with low levels of plasma cholinesterase or with an abnormal pseudocholinesterase, suxamethonium should be used only with extreme caution and where the benefits of the drug are considered to outweigh the risks, and in reduced doses in such patients. If low pseudocholinesterase concentration is suspected slow administration of a small test dose of suxamethonium (5-10 mg as a 0.1% solution) should be considered.
Suxamethonium is rapidly hydrolysed by plasma cholinesterase which thereby limits the intensity and duration of the neuromuscular blockade. Deficiencies of this enzyme result in prolonged and intensified neuromuscular block.
Antidysrhythmic drugs. Suxamethonium should be administered with great caution in patients receiving quinidine and those who have been digitalised or who may have digitalis toxicity. In these circumstances the rise in serum potassium due to suxamethonium may possibly cause arrhythmias.
Delayed recovery. When recovery from suxamethonium is delayed, assisted respiration sufficient for full oxygenation, yet avoiding excessive elimination of carbon dioxide, should be maintained until paralysis ceases. This should be combined with light narcosis, e.g. nitrous oxide/oxygen mixture.
Neostigmine should not be given when prolonged apnoea follows a single dose of suxamethonium. Neostigmine and other anticholinesterase drugs may have the effect of intensifying the depolarisation block caused by suxamethonium.
Nondepolarising blockade. If suxamethonium is given repeatedly or over a prolonged period the depolarising block may change to one with characteristics of a nondepolarising block. This may be associated with prolonged respiratory depression and apnoea. Following a positive diagnosis of a nondepolarising blockade the administration of neostigmine preceded by atropine may be considered.
Debilitated patients. Use with caution in patients who are hypoxic or those who have cardiovascular, hepatic, pulmonary, metabolic or renal disorders or myasthenia gravis. The action of suxamethonium may be altered in these patients. Its use is not advisable in patients with phaeochromocytoma, neurological disorders or muscular disease. As suxamethonium produces muscle contractions before relaxation it should be used with caution in patients with bone fractures.
Suxamethonium should be avoided in patients with myotonias, as response is unpredictable.
Use in eye surgery. Suxamethonium causes a slight transient increase in intraocular pressure immediately after injection and during the fasciculation phase. It should therefore be used cautiously if at all during intraocular surgery and in patients with glaucoma.
Use in hepatic impairment. Use with caution in patients who have hepatic disorders. The action of suxamethonium may be altered in these patients.
Use in renal impairment. Use with caution in patients who have renal disorders. The action of suxamethonium may be altered in these patients. Patients with impaired renal function may occasionally experience prolonged apnoea due to accumulation of succinylmonocholine.
Use in the elderly. No data available.
Paediatric use. Neonates and premature infants may be relatively resistant to suxamethonium.
Intravenous bolus in children may result in profound bradycardia or on occasion, asystole. This tends to be more common after a second dose. Pre-treatment with atropine can reduce the risk of bradycardia.
Caution should be exercised when using suxamethonium in children, since paediatric patients are more likely to have an undiagnosed myopathy or an unknown predisposition to malignant hyperthermia and rhabdomyolysis, which places them at increased risk of serious adverse events following suxamethonium.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Co-administration of inhaled anaesthetics (cyclopane, diethylether, enflurane, desflurane, isoflurane, methyoxyflurane, halothane and nitrous oxide) may increase the incidence of dysrhythmias (especially bradycardia), apnoea and the occurrence of malignant hyperthermia in susceptible persons. Inhaled anaesthetics have little effect on the usual depolarising neuromuscular blockade of suxamethonium but may accelerate the onset and enhance the Phase II block (nondepolarising) that may be produced by repeated dosage of suxamethonium. Severe bradycardia and asystole have occurred when suxamethonium is used in anaesthetic regimens with propofol and opioids such as fentanyl.
Drugs which may enhance or prolong the effects of suxamethonium include lignocaine, procaine, oxytocin, oral contraceptives, oestrogens, piperacillin, some non-penicillin antibiotics, (streptomycin, neomycin, kanamycin, capreomycin, framycetin, colistin and polymyxins, aminoglycosides [amikacin, gentamicin, tobramycin], clindamycin, vancomycin), tacrine, beta-adrenergic blockers, trimethaphan, phenelzine, aprotinin, quinidine, promazine, lithium carbonate, phenytoin, carbamazepine, magnesium salts, quinine, chloroquine, cimetidine, terbutaline sulfate, high dose corticosteroids and cytostatic agents such as cyclophosphamide, thiotepa and azathioprine, selective serotonin reuptake inhibitors, chlorpromazine, morphine, morphine antagonists, pethidine, procainamide, procaine, cocaine, chloroprocaine, chlorethamine, tretamine, triethylene-melamine, bambuterol, diphenhydramine.
Diazepam may reduce the duration of neuromuscular blockade produced by suxamethonium.
Drugs which may have prolong blocking effect of suxamethonium include ketamine and propanidid.
Cardiac glycosides could prolong neuromuscular blocking effects of suxamethonium by possibly increasing the risk of bradycardia and other dysrhythmias, including ventricular dysrhythmias and cardiac arrest (see Section 4.4 Special Warnings and Precautions for Use; Section 4.8 Adverse Effects (Undesirable Effects)).
Concomitant digoxin or verapamil, and suxamethonium therapy has been reported to result in cardiac arrhythmias.
Amphotericin B and thiazide diuretics may increase the effects of suxamethonium secondary to induced electrolyte imbalance. Patients with hypokalemia or hypocalcaemia require reduced doses of suxamethonium.
Inhibitors of plasma cholinesterases such as neostigmine, pyridostigmine bromide, rivastigmine, donepezil, edrophonium, galantamine, metoclopramide, physostigmine and phospholine iodide can considerably prolong the depolarising action of suxamethonium. It is recommended that long-acting anticholinesterase inhibitor (ecothiopate) eye drops should be discontinued several months prior to administration of suxamethonium. Ecothiopate eye drops may prolong apnoea after suxamethonium administration has occurred.
Administration of suxamethonium prior to or with a nondepolarising muscle relaxant e.g. pancuronium, mivacurium can alter the intensity and/or duration of neuromuscular blockade.
Liver disease, cancer, pregnancy, dehydration, electrolyte imbalances and overdosage (due to excessive production of succinylmonocholine) may also prolong the action of suxamethonium.
Simultaneous administration of suxamethonium and atracurium significantly reduces the duration of suxamethonium.
Organophosphorous insecticides and metriphonate may prolong the neuromuscular effect of suxamethonium.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. No data available.
Use in pregnancy. (Category A)
Safety of the use of suxamethonium in pregnancy has not been established with respect to effects on foetal development. Therefore, suxamethonium should not be administered to pregnant women unless the potential benefit outweighs the possible hazards.
Plasma pseudocholinesterase levels are decreased in pregnancy and several days postpartum by approximately 25%, therefore a high proportion of these patients may be expected to show prolonged apnoea.
Suxamethonium crosses the placenta, but generally only in small amounts. Residual neuromuscular blockade may occasionally occur in the neonate after repeated high doses of suxamethonium to the mother during delivery by caesarean section.
Use in lactation. No data available.
4.7 Effects on Ability to Drive and Use Machines
The effects of this medicine on a person's ability to drive and use machines were not assessed as part of its registration.
4.8 Adverse Effects (Undesirable Effects)
The following adverse reactions have been reported following administration of suxamethonium:
Neuromuscular. Post-operative muscle pain, muscle fasciculation, rhabdomyolysis, myoglobinuria1, myoglobinaemia1, elevated creatine phosphokinase, hypertonia, trismus.
Cardiovascular. Bradycardia, tachycardia, arrhythmias, cardiac arrest2, hypertension, hypotension, tachyphylaxis, ventricular fibrillation as a result of hyperkalaemia.
Respiratory. Apnoea, prolonged respiratory failure, bronchospasm, increased bronchial secretions, pulmonary oedema in infants, prolonged respiratory depression3.
Endocrine, metabolic. Malignant hyperthermia, porphyria, hyperkalaemia.
Gastrointestinal. Increased intragastric pressure, increased bowel movements, increased gastric secretions, possible aspiration, excessive salivation.
Special senses. Increased intraocular pressure.
Immune system. Anaphylactic reactions.
Other. Rise in intracranial pressure, renal failure, precipitation or exacerbation of myasthenia gravis, hypersensitivity reactions (including circulatory collapse, flushing, rash, urticaria, bronchospasm and shock, which may lead to death), transient blood potassium increase, skin flushing.
1 Rhabdomyolysis has also been reported.
2 There are case reports of hyperkalaemia-related cardiac arrests following the administration of suxamethonium to patients with congenital cerebral palsy, tetanus, Duchenne muscular dystrophy, and closed head injury. Such events have also been reported rarely in children with hitherto undiagnosed muscular disorders.
3 Individuals with decreased plasma cholinesterase activity exhibit a prolonged response suxamethonium. Approximately 0.05% of the population has an inherited cause of reduced cholinesterase activity (see Section 4.4 Special Warnings and Precautions for Use).
Reporting of suspected adverse reactions. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
For information on the management of overdose, contact the Poison Information Centre on 131126 (Australia).
The most serious effects of overdosage are apnoea and prolonged muscle paralysis. It is essential to maintain the airway and adequate ventilation until spontaneous respiration is fully restored.
The use of neostigmine to reverse a nondepolarising block is a clinical decision which depends on the subject, the experience, and the judgment of the clinician. If neostigmine is used, its administration should be accompanied by an appropriate dose of atropine.
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Suxamethonium is an ultra short-acting depolarising-type neuromuscular blocking agent.
Suxamethonium combines with the cholinergic receptors of the motor end plate to produce depolarisation. Neuromuscular transmission is inhibited so long as an adequate concentration of suxamethonium remains at the receptor site.
Suxamethonium has no direct action on smooth muscle structures, including the uterus. Suxamethonium may produce slowing of heart rate via vagal stimulation.
When suxamethonium is administered over a prolonged period the characteristics of the neuromuscular block may change from the characteristic depolarising type to one resembling a nondepolarising block.
Clinical trials. No data available.
5.2 Pharmacokinetic Properties
Absorption. Suxamethonium has a rapid onset and a short duration of action. Following intravenous (IV) administration of a single therapeutic dose in healthy adults, complete muscle relaxation occurs within 1/2 to 1 minute, persists for about 2-3 minutes, and gradually dissipates within 10 minutes.
Following intramuscular (IM) administration the onset of action occurs in about 2-3 minutes, with a duration ranging from 10-30 minutes.
The duration of action is prolonged in patients with low plasma pseudocholinesterase concentration.
Distribution. Suxamethonium crosses the placenta, generally in small amounts.
Excretion. Plasma pseudocholinesterases hydrolyse suxamethonium to succinylmonocholine (relatively inactive) and choline. Approximately 10% of drug is excreted unchanged in the urine.
5.3 Preclinical Safety Data
Genotoxicity. No data available.
Carcinogenicity. No data available.
6 Pharmaceutical Particulars
6.1 List of Excipients
Water for injection; hydrochloric acid for pH adjustment.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store between 2°-8°C. Refrigerate, do not freeze.
6.5 Nature and Contents of Container
2 mL Type I clear glass ampoule in packs of 10 or 50.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Chemical structure.
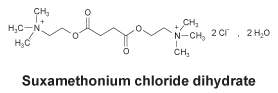
The chemical name for suxamethonium chloride is 2, 2'- succinyldioxybis(ethyltrimethylammonium) dichloride dihydrate.
7 Medicine Schedule (Poisons Standard)
Prescription only medicine (Schedule 4).
Date of First Approval
05 December 2019
Date of Revision
04 March 2026
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.