Tanilone Fatty Ointment
Brand Information
| Brand name | Tanilone Fatty Ointment |
| Active ingredient | Methylprednisolone aceponate |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Tanilone Fatty Ointment.
Summary CMI
TANILONE fatty ointment
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using TANILONE?
TANILONE fatty ointment contains the active ingredient methylprednisolone aceponate. It is used to relieve the redness, swelling, itching and irritation of the skin in eczema and psoriasis patients.
For more information, see Section 1. Why am I using TANILONE? in the full CMI.
2. What should I know before I use TANILONE?
Do not use if you have ever had an allergic reaction to methylprednisolone aceponate, other corticosteroid medicines applied to the skin or any of the ingredients listed at the end of the CMI.
Do not use on open wounds or other treated skin areas.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I use TANILONE? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with TANILONE and affect how it works.
For more information, see Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use this medicine?
Apply thinly to the affected area of skin.
More instructions can be found in Section 4. How do I use TANILONE? in the full CMI.
5. What should I know while using TANILONE?
| Things you should do |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using TANILONE? in the full CMI.
6. Are there any side effects?
Common side effects include itching, burning and redness.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
TANILONE fatty ointment
Active ingredient: methylprednisolone aceponate
Consumer Medicine Information (CMI)
This leaflet provides important information about using TANILONE fatty ointment.
You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using this medicine.
Where to find information in this leaflet:
1. Why am I using TANILONE?
2. What should I know before I use TANILONE?
3. What if I am taking other medicines?
4. How do I use this medicine?
5. What should I know while using TANILONE?
6. Are there any side effects?
7. Product details
1. Why am I using TANILONE?
TANILONE fatty ointment contains the active ingredient methylprednisolone aceponate, a corticosteroid suitable to put on the skin.
TANILONE is used to relieve the redness, swelling, itching and irritation of the skin in eczema and psoriasis.
Eczema is a skin condition with redness, swelling, oozing of fluid, crusting and later scaling. It is often very itchy.
Psoriasis is a skin disorder with raised, rough, reddened areas covered with dry, fine, silvery scales.
Ask your doctor if you have any questions about why TANILONE fatty ointment has been prescribed for you.
Your doctor may have prescribed it for another reason.
This medicine is not addictive.
2. What should I know before I use TANILONE?
Warnings
Do not use TANILONE if you are allergic to:
- any medicine containing methylprednisolone aceponate
- any of the ingredients listed at the end of this leaflet
- any other similar corticosteroid medicine that is applied to the skin.
Some of the symptoms of an allergic reaction may include shortness of breath, wheezing or difficulty breathing; swelling of the face, lips, tongue or other parts of the body; rash, itching or hives on the skin.
Do not use TANILONE if you have a virus such as chicken pox or shingles.
Do not use TANILONE if you have an over-active thyroid gland (hyperthyroidism).
Do not use TANILONE if the area of skin you are treating also has:
- an infection due to tuberculosis or syphilis
- a skin reaction following a vaccination.
Do not use TANILONE on your face if you have acne, rosacea, ulcers, atrophic skin disease or perioral dermatitis.
Your doctor will identify these conditions for you.
Keep TANILONE away from eyes.
Do not let TANILONE come into contact with deep open wounds or mucous membranes (such as inside your mouth, throat or nose). Do not swallow TANILONE.
TANILONE should be used only on the skin.
Do not use TANILONE in children under 4 months of age.
There is lack of experience with using TANILINE in this age group.
Pregnancy and breastfeeding
Check with your doctor if you are pregnant or intend to become pregnant.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
4. How do I use this medicine?
How much to use
- Apply thinly to the affected area of skin.
- Follow the instructions provided and use TANILONE fatty ointment until your doctor tells you to stop.
When to use it
Treatment of eczema:
Use TANILONE once a day to treat the affected skin or as directed by your doctor.
Treatment of psoriasis:
Use TANILONE once or twice a day on the patches of psoriasis or as directed by your doctor.
If you forget to use TANILONE
This medicine should be used regularly at the same time each day. If you forget to use it, use it as soon as you remember, then go on as before.
If you use too much TANILONE
If you think that you have used too much TANILONE, you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
If you use too much TANILONE or use it for a long time, you may notice the following in the treated area:
- your skin becomes thinner
- pink/purple stretch marks appear
- a network of tiny blood vessels appears.
Stop using TANILONE if you have these symptoms and tell your doctor. These symptoms usually disappear about two weeks after you stop using TANILONE.
5. What should I know while using TANILONE?
Things you should do
Stop using TANILONE if you develop a skin allergy.
If your eczema or psoriasis is infected, you must:
- use specific anti-infection treatments prescribed by your doctor
- stop using TANILONE if the infection spreads.
If you are going to start any new medicine, tell your doctor and pharmacist that you are using TANILONE.
If you become pregnant while using TANILONE, tell your doctor immediately.
Things you should not do
- Do not use this medicine to treat any other complaints unless your doctor tells you to.
- Do not give your medicine to anyone else, even if they have the same condition as you.
Driving or using machines
TANILONE is not expected to affect your ability to drive a car or operate machinery.
Looking after your medicine
Keep TANILONE in a cool dry place where the temperature stays below 25°C.
Do not store TANILONE or any other medicine in the bathroom or near a sink. Do not leave it on a window sill or in the car. Heat and dampness can destroy some medicines.
Keep it where young children cannot reach it.
Getting rid of any unwanted medicine
If you no longer need to use this medicine or it is out of date, take it to any pharmacy for safe disposal.
Do not use this medicine after the expiry date.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
| Speak to your doctor or pharmacist if you have any of these side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
| Speak to your doctor or pharmacist if you have any of these side effects and they worry you. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What TANILONE fatty ointment contains:
| Active ingredient (main ingredient) |
|
| Other ingredients (inactive ingredients) |
|
Do not use this medicine if you are allergic to any of these ingredients.
What TANILONE looks like
TANILONE fatty ointment is a white to yellowish translucent ointment. Pack size consists of a 15 g aluminium tube.
Australian Registration number: AUST R 376095
Who distributes TANILONE fatty ointment
Aspen Pharmacare Australia Pty Ltd
34-36 Chandos Street
St Leonards NSW 2065
Australia
This leaflet was revised in January 2025.
Brand Information
| Brand name | Tanilone Fatty Ointment |
| Active ingredient | Methylprednisolone aceponate |
| Schedule | S4 |
MIMS Revision Date: 01 July 2025
1 Name of Medicine
Methylprednisolone aceponate.
2 Qualitative and Quantitative Composition
Tanilone fatty ointment contains methylprednisolone aceponate 1 mg/g (0.1% w/w).
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
White to yellowish translucent ointment; free from lumps and gritty particles; free of visible contamination.
4 Clinical Particulars
4.1 Therapeutic Indications
Tanilone fatty ointment is indicated for the topical treatment of eczema and psoriasis in adults and children.
4.2 Dose and Method of Administration
For external topical use only. Keep away from eyes.
The duration of use should be less than 12 weeks in adults and less than 4 weeks in children.
Tanilone fatty ointment should usually be applied as a thin coating once per day to the affected areas. In the treatment of psoriasis, twice daily application may be required.
Tanilone fatty ointment is suitable for very dry skin and chronic stage of skin conditions which require an anhydrous base. The base has an occlusive effect. It is suitable for treatment of areas where the stratum corneum is particularly thick, such as the pressure areas of elbows, knees, palms and soles.
4.3 Contraindications
Tanilone is contraindicated in viral diseases (e.g. vaccinia, varicella/herpes zoster) and when tuberculous or syphilitic processes and post-vaccination skin reactions are present in the area to be treated. If rosacea, ulcers, atrophic skin diseases, acne vulgaris or perioral dermatitis are present, Tanilone must not be applied to the face.
Hypersensitivity to methylprednisolone aceponate or any component of the formulation.
Children under four months due to lack of experience.
4.4 Special Warnings and Precautions for Use
For external topical use only. Keep away from eyes.
Tanilone should not be allowed to come into contact with deep open wounds, mucosae or the eyes when being applied to the face.
Additional specific therapy is required in skin conditions infected with bacteria and/or fungi. Any spread of infection requires withdrawal of topical corticosteroid therapy.
If signs of hypersensitivity develop, Tanilone should be discontinued and appropriate treatment instituted.
Any of the side effects that have been reported following systemic use of corticosteroids, including adrenal suppression, may also occur with topical corticosteroids, especially in infants and children.
As known from systemically administered corticosteroids, glaucoma may also develop from using topical corticosteroids (e.g. after large-dose or extensive application over a prolonged period, application under occlusive dressings, or application to skin around or near the eyes).
Tanilone is a potent steroid formulated for topical application. As with all potent corticosteroids, the possibility of hypothalamic-pituitary-adrenal (HPA) axis suppression resulting from percutaneous absorption of methylprednisolone must be considered when initiating or reviewing therapy, as adequate studies are not available to define the degree of risk.
Treatment of large areas has been noted to produce some suppression of cortisol secretion, but plasma levels remain above the lower limit of the normal range and circadian rhythm is maintained. Nevertheless, when treating large areas, the duration of use should be kept as brief as possible.
Extensive application of topical corticosteroids to large areas of the body or for prolonged periods of time, in particular under occlusion, significantly increases the risk of side effects. This is particularly important in children who may absorb proportionately larger amounts of topical corticosteroid and thus be more susceptible to systemic toxicity.
Systemic absorption of topical corticosteroids will be increased if extensive body surface areas are treated or if the occlusive technique is used. Suitable precautions should be taken under these conditions or when long-term use is anticipated.
Local atrophy, telangiectasia and striae may occur after prolonged treatment or excessive application. Treatment should be discontinued if symptoms such as cutaneous atrophy occur (also see Section 4.8 Adverse Effects (Undesirable Effects)).
Thyrotoxic Periodic Paralysis (TPP) can occur in patients with hyperthyroidism and with methylprednisolone-induced hypokalaemia. TPP must be suspected in patients treated with methylprednisolone presenting signs or symptoms of muscle weakness, especially in patients with hyperthyroidism. If TPP is suspected, levels of blood potassium must be immediately monitored and adequately managed to ensure the restoration of normal levels of blood potassium.
There was no sensitising effect or potential in animal studies.
Some of the excipients in Tanilone fatty ointment may reduce the effectiveness of latex products such as condoms and diaphragms.
Visual disturbance. Visual disturbance may be reported with systemic and topical corticosteroid use. If a patient presents with symptoms such as blurred vision or other visual disturbances, the patient should be considered for referral to an ophthalmologist for evaluation of possible causes which may include cataract, glaucoma or rare diseases such as central serous chorioretinopathy (CSCR) which have been reported after use of systemic and topical corticosteroids.
Use in the elderly. No data available.
Paediatric use. In infants and children, plastic pants and napkins may act as occlusive dressings and increase absorption. Because of children's larger skin surface area to bodyweight ratio, paediatric patients may demonstrate greater susceptibility to topical corticosteroid-induced HPA axis suppression and Cushing's syndrome than adults. Chronic/long-term corticosteroid therapy may interfere with growth and development of children.
Use of topical corticosteroids in children should be limited to the least amount required for therapeutic effect.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
No specific information exists on interactions with other medications.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. No data available.
Use in pregnancy. (Category C)
There are no adequate data from the use of methylprednisolone aceponate fatty ointment in pregnant women.
Animal studies with methylprednisolone aceponate have shown embryolethal effects in rats dosed subcutaneously during the period of organogenesis at doses greater than 1 mg/kg/day and in rabbits following dermal application at doses greater than 0.25 mg/kg/day. No teratogenic effects were observed in rabbits, but in rats the incidence of ventricular septal defects and of cleft palate were increased at subcutaneous doses greater than 1 and 10 mg/kg/day. Epidemiological studies suggest that there could possibly be an increased risk of oral clefts among newborns or women who were treated with glucocorticosteroids during the first trimester of pregnancy. In general, the use of topical preparations containing corticoids should be avoided during the first trimester of pregnancy.
Reduced placental and birth weight have been recorded in animals and humans after long-term treatment. Since the possibility of suppression of the adrenal cortex in the newborn baby after long-term treatment must be considered, the needs of the mother must be carefully weighed against the risk to the foetus when prescribing these drugs. Maternal pulmonary oedema has been reported, with tocolysis and fluid overload.
The clinical indication for treatment with methylprednisolone aceponate must be carefully reviewed and the benefits weighed against the risks in pregnant and lactating women.
Treatment of large areas or prolonged use (greater than 4 weeks) must be avoided.
Use in lactation. It is not known whether methylprednisolone aceponate is secreted in breast milk. Methylprednisolone aceponate should be used during lactation only if benefits outweigh the risks.
Nursing mothers should avoid treatment over large areas, prolonged use or occlusive dressings. Tanilone should not be applied to the chest area during breast feeding to avoid possible ingestion by infants.
When considering use during lactation, note that after systemic administration, very small amounts of glucocorticoid may be present in breast milk. There is only a slight risk of exposure to methylprednisolone aceponate in breast milk following maternal dermal application at therapeutic doses, because the systemic absorption of methylprednisolone aceponate is minimal.
4.7 Effects on Ability to Drive and Use Machines
The effects of this medicine on a person's ability to drive and use machines were not assessed as part of its registration.
4.8 Adverse Effects (Undesirable Effects)
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
In clinical studies, most frequently observed side effects included application site folliculitis and application site burning.
Frequencies of side effects observed in clinical studies and given in Table 1 are defined according to the MedDRA frequency convention: very common (> 1/10); common (> 1/100, < 1/10); uncommon (> 1/1,000; < 1/100), rare (> 1/10,000, < 1/1,000); very rare (< 1/10,000), not known (cannot be estimated from available data). MedDRA version 12.0 was used for coding.

Post marketing. Eye disorders. Vision blurred.
4.9 Overdose
Excessive dosing may occur with prolonged or intensive topical use. See Section 4.8 Adverse Effects (Undesirable Effects) for further information.
Acute toxicity studies with methylprednisolone aceponate (namely oral ingestion, or single dermal application to a large area, under conditions favourable to absorption) do not indicate that any acute intoxication is expected.
For information on the management of overdose, contact the Poison Information Centre on 131126 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. After topical application, methylprednisolone aceponate fatty ointment has anti-inflammatory, anti-pruritic and vasoconstrictive actions.
As for all other glucocorticoids, the mechanism of action of methylprednisolone aceponate is not completely understood. It is known that methylprednisolone aceponate binds to the intracellular glucocorticoid receptor as does the principal metabolite 6α-methylprednisolone-17-propionate, which is formed by cleavage in the skin. The steroid-receptor complex binds to certain regions of DNA, inducing anti-inflammatory, anti-pruritic and vasoconstrictive effects.
Binding of methylprednisolone aceponate or its metabolites to the steroid receptor results in the induction of lipomodulin synthesis. Lipomodulin, a protein secondary messenger (also known as lipocortin 1 and macrocortin) inhibits release of arachidonic acid, which in turn inhibits the formation of inflammatory mediators, such as prostaglandins and leukotrienes.
The immunosuppressive action of glucocorticoids can be explained in part by their inhibitory effects on chemotaxis (inhibition of leukotriene synthesis). Glucocorticoids also have anti-mitotic activity, which is not well understood.
The vasoconstrictive activity of glucocorticoids results from the inhibition of prostaglandin synthesis. Prostaglandins have vasodilatory actions. Glucocorticoids also potentiate the vasoconstrictive effect of adrenaline.
Clinical trials. No data available.
5.2 Pharmacokinetic Properties
Absorption. When applied topically the concentration of methylprednisolone aceponate is highest in the outer layer of the epidermis (stratum corneum) and decreases progressively in the deeper strata.
The degree of percutaneous absorption of methylprednisolone aceponate varies according to the state of the skin (intact/inflamed/damaged), the formulation (ointment/fatty ointment/cream/lotion) and the conditions of application (ope/occlusion). Studies using the ointment, fatty ointment and cream formulations in juvenile and adult patients with neurodermatitis and psoriasis have shown that the percutaneous absorption on open application was slightly (≤ 2.5%) greater than the percutaneous absorption in volunteers with normal skin (0.2-1.5%). Occlusive dressing increased percutaneous absorption. When the superficial horny layer is removed before application of methylprednisolone aceponate, the corticoid levels in the skin are about three times higher than after application to intact skin.
Distribution. The systemic effects of methylprednisolone aceponate are minimal in both man and animals following application of a topically effective dose. After treatment of large areas in patients with skin disorders, the plasma cortisol values remain within the normal range; circadian cortisol rhythm is maintained and no reduction of cortisol has been ascertained in 24-hour urine.
Metabolism. Methylprednisolone aceponate is hydrolysed in the epidermis and dermis to the principal metabolite, 6α-methylprednisolone-17-propionate. This metabolite binds to the intracellular glucocorticoid receptor with higher affinity than methylprednisolone aceponate. The binding of 6α-methylprednisolone-17-propionate to the receptor is an indicator of "bioactivation" in the skin.
After absorption into the systemic circulation, the primary hydrolysis product of methylprednisolone aceponate, 6α-methylprednisolone-17-propionate, is rapidly conjugated with glucuronic acid, and as a result, inactivated.
Excretion. The principal metabolites of methylprednisolone aceponate are eliminated primarily via the kidneys. The half-life is about 16 hours. Following intravenous administration, excretion via the urine and faeces was complete within 7 days. There is no accumulation of methylprednisolone aceponate or metabolites in the body.
5.3 Preclinical Safety Data
Genotoxicity. Methylprednisolone aceponate did not elicit any genotoxic effects or chromosomal damage in in vitro and in vivo assays conducted in bacteria and mammalian cells.
Carcinogenicity. Animal studies to evaluate the carcinogenic potential of methylprednisolone aceponate have not been conducted. Other glucocorticoid drugs have been shown to cause hepatic tumours in rats and it must be assumed that methylprednisolone aceponate would have similar activity. However, in humans epidemiological surveys of many years of systemic glucocorticoid therapy have not revealed any evidence for a tumourigenic action of this substance class.
6 Pharmaceutical Particulars
6.1 List of Excipients
White soft paraffin, liquid paraffin, microcrystalline wax and hydrogenated castor oil.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C.
6.5 Nature and Contents of Container
Tanilone fatty ointment is available in aluminium tubes of 5 g (starter packs), 15 g, 20 g and 50 g.
Note. Not all pack sizes may be marketed.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
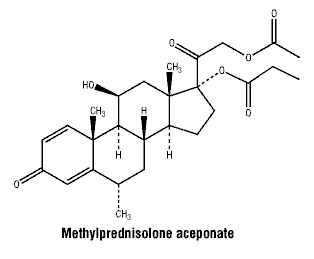
6.7 Physicochemical Properties
Methylprednisolone aceponate (MPA) is a white crystalline powder. It is soluble in methylene chloride, acetone and ethyl acetate and is sparingly soluble in hexane and ether.
The chemical name is 21-acetoxy-11β-hydroxy-6α-methyl-17-propionyloxy-1, 4- pregnadiene-3, 20- dione. The molecular formula is C27H36O7. The molecular weight is 472.58.
Chemical structure.
7 Medicine Schedule (Poisons Standard)
Schedule 4 - Prescription Only Medicine.
Date of First Approval
29 November 2022
Date of Revision
28 April 2025
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.