Vasodrine
Brand Information
| Brand name | Vasodrine |
| Active ingredient | Midodrine hydrochloride |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Vasodrine.
Summary CMI
VASODRINE
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I taking VASODRINE?
VASODRINE contains the active ingredient midodrine hydrochloride. VASODRINE is used to treat severe forms of low blood pressure in adults when other treatments are proven unsatisfactory.
For more information, see Section 1. Why am I taking VASODRINE? in the full CMI.
2. What should I know before I take VASODRINE?
Do not use if you have ever had an allergic reaction to VASODRINE or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions, take any other medicines, or are pregnant or plan to become pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I take VASODRINE? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with VASODRINE and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I take VASODRINE?
- Your doctor will advise the correct dose for you.
- Swallow the tablets whole with a full glass of water. The tablets may be taken with food.
- The last daily dose should be taken at least 4 hours before your bedtime.
More instructions can be found in Section 4. How do I take VASODRINE? in the full CMI.
5. What should I know while taking VASODRINE?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while taking VASODRINE? in the full CMI.
6. Are there any side effects?
Common side effects include: goose bumps; headache; nausea (feeling sick); heartburn; flushing; chills; increased tear production; sleep disturbances including difficulty sleeping. Tell your doctor if you have abdominal pain; being sick (vomiting); diarrhoea; tingling and itching of the skin and scalp; urge to urinate, difficulty urinating and/or pain when urinating; inflammation of the lining inside the mouth; restlessness, excitability and irritability; dizziness; anxiety, feelings of confusion; slowed heart rate.
Serious side effects include: shortness of breath; wheezing or difficulty breathing; swelling of the face, lips, tongue or other parts of the body; rash, itching or hives on the skin; pounding in the ears; stroke; palpitations, irregular heartbeat; chest pain; blurred vision, visual changes; severe or persistent headache; disorder of the skin or mucous membranes starting with a fever and flu like symptoms and rash.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
VASODRINE
Active ingredient: midodrine hydrochloride (mid-OH-drean HIGH-droe-KLOR-ide)
Consumer Medicine Information (CMI)
This leaflet provides important information about taking VASODRINE. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about taking VASODRINE.
Where to find information in this leaflet:
1. Why am I taking VASODRINE?
2. What should I know before I take VASODRINE?
3. What if I am taking other medicines?
4. How do I take VASODRINE?
5. What should I know while taking VASODRINE?
6. Are there any side effects?
7. Product details
1. Why am I taking VASODRINE?
VASODRINE contains the active ingredient midodrine hydrochloride. It works by raising your blood pressure. VASODRINE belongs to a group of medicines called adrenergic agents.
VASODRINE is used to is used to treat severe forms of low blood pressure in adults when other treatments are proven unsatisfactory.
2. What should I know before I take VASODRINE?
Warnings
Do not take VASODRINE if you:
- are allergic to midodrine hydrochloride, or any of the ingredients listed at the end of this leaflet.
Some of the symptoms of an allergic reaction may include: shortness of breath, wheezing or difficulty breathing, swelling of the face, lips, tongue or other parts of the body, rash, itching or hives on the skin.
Always check the ingredients to make sure you can use this medicine. - have high blood pressure
- have a condition called vasovagal hypotension (low blood pressure)
- have a slow pulse
- have certain forms of cardiovascular disease e.g. heart attack, heart failure, blood vessel disease, changes in heart rhythm
- have elevated pressure in the eye (glaucoma) or poor vision because of damage to the eye caused by diabetes
- have an overactive thyroid gland (hyperthyroidism)
- have difficulty passing urine
- have severe kidney disease or inflammation of the kidneys
- have hormonal disorders caused by a rare tumour in the adrenal gland, which sits near the kidney (phaeochromocytoma)
- have prostate problems
- are under 18 years of age. The safety and efficacy of VASODRINE in children has not been established.
Do not take this medicine after the expiry date printed on the pack or if the packaging is torn or shows signs of tampering. If it has expired or is damaged, return it to your pharmacist for disposal.
Check with your doctor if you:
- have high blood pressure when you lie down. If this applies to you then: regular monitoring of your blood pressure will be required when you are lying down and standing up as there may be a risk of your blood pressure rising when you lie down, for example, at night. If your blood pressure rises when you lie down and reducing the dose does not correct this problem, then treatment with this medicine must be stopped. Patients with a history of strokes will need to be monitored. Patients undergoing long term treatment require kidney and blood pressure monitoring.
- have a serious disorder of the nervous system (autonomic nervous system disorders), since taking VASODRINE may lead to a further drop in blood pressure when you stand up. If this occurs, further treatment with VASODRINE should be stopped
- have a disease of the arteries which leads to circulation problems including pain or cramps in the stomach after eating, or pain or cramps in the legs while walking
- have a disease of the prostate, as you may find passing urine is difficult when taking VASODRINE.
- have diabetes
- have any other medical conditions
- take any medicines for any other condition
- have allergies to any other medicines, foods, preservatives or dyes.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. Your doctor may also perform some tests such as checking your kidney function and blood pressure before you start using this medicine. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
Check with your doctor if you are pregnant or intend to become pregnant.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
Using this medicine while pregnant or breastfeeding is not recommended.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines and VASODRINE may interfere with each other. These include:
- vasoconstrictors (medicines that narrow blood vessels) and sympathomimetic agents (medicines that have a stimulating effect on certain parts of the nervous system. These drugs include reserpine and guanethidine.
- tricyclic antidepressants and MAO-inhibitors (medicines used to treat depression)
- hormones for the thyroid (used when the thyroid is not working properly)
- dihydroergotamine (medicine used to treat migraines)
- antihistamines (medicines used to treat allergy such as hay fever)
- decongestants
- some appetite suppressants
- drugs which cause hypertension such as methyldopa
- prazosin (medicines used to treat heart disease)
- corticosteroid preparations such as fludrocortisone acetate (an anti-inflammatory medicine)
- digitalis preparations (medicines used to treat heart disease) or other glycoside preparations
- medicines that may slow down the heart rate
- promethazine (medicine used to treat allergies and help with vomiting)
- quinidine (medicine used to change the way the heart beats)
- antibiotics and antivirals (medicines used to treat infections).
These medicines may be affected by VASODRINE or may affect how well it works. Some may enhance or block the effects of midodrine or affect the heartbeat. Others will require that decrease your salt intake. You may need different amounts of your medicines, or you may need to take different medicines.
If you are taking medicines which directly or indirectly reduce your heart rate, your doctor will closely monitor you while you are taking VASODRINE.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect VASODRINE.
4. How do I take VASODRINE?
How much to take
- Follow all directions given to you by your doctor or pharmacist carefully. They may differ from the information contained in this leaflet. If you do not understand the instructions, ask your pharmacist for help.
- Your doctor will decide your dose and tell you how long you should take this medicine.
- The usual recommended starting dose is one 2.5 mg tablet three times each day.
- This dose may be increased weekly by your doctor up to your maintenance dose. The dose may be increased to a dose of four 2.5 mg tablets, or two 5 mg tablets (10 mg) three times daily, which is the usual maintenance dose of 30 mg per day.
- The increase may occur over a longer time period in older patients.
- Swallow the tablets whole with a full glass of water. The tablets may be taken with food.
- Continue taking your medicine for as long as your doctor tells you. This medicine helps to control your condition, but does not cure it. It is important to keep taking your medicine even if you feel well.
- If you are taking medicines which directly or indirectly reduce your heart rate, your doctor will closely monitor you while you are taking VASODRINE.
When to take VASODRINE
- VASODRINE should be taken at about the same times each day. Taking it at the same times each day will have the best effect. It will also help you remember when to take it.
- Avoid taking this medicine in the late evening. The last daily dose should be taken at least 4 hours before your bedtime.
- Keep your head elevated when you lie down at night. This reduces the potential risk of rise in your blood pressure.
If you forget to take VASODRINE
VASODRINE should be used regularly at the same times each day. If you miss your dose at the usual time, take your dose as soon as you remember, and continue to take it as you would normally.
If it is almost time for your next dose, skip the dose you missed and take your next dose when you are meant to.
Do not take a double dose to make up for the dose you missed. This may increase the chance of you getting an unwanted side effect.
If you are not sure what to do, ask your doctor or pharmacist.
If you take too much VASODRINE
If you think that you have taken too much VASODRINE, you may need urgent medical attention.
You should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
Symptoms of an overdose may include:
- high blood pressure
- goose bumps and feeling cold
- slow heartbeat
- difficulty passing urine
5. What should I know while taking VASODRINE?
Things you should do
Remind any doctor, dentist or pharmacist you visit that you are taking VASODRINE.
If you are about to be started on any new medicine, remind your doctor and pharmacist that you are taking VASODRINE.
Tell any other doctors, dentists and pharmacists who treat you that you are taking this medicine.
If you are going to have surgery, tell the surgeon or anaesthetist that you are taking this medicine. It may affect other medicines used during surgery.
If you become pregnant while taking this medicine, tell your doctor immediately.
Keep all of your doctor's appointments so that your progress can be checked. During treatment with this medicine your blood pressure will be checked from time to time, and if necessary your dose adjusted.
It is important that you immediately report symptoms related to high blood pressure such as elevated heart rate, headache and blurred vision. Your doctor will then decide whether to adjust dosage or discontinue your treatment with VASODRINE.
Things you should not do
- Do not take VASODRINE to treat any other complaints unless your doctor tells you to.
- Do not give your medicine to anyone else, even if they have the same condition as you.
- Do not stop taking your medicine or lower the dosage without checking with your doctor.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how VASODRINE affects you.
VASODRINE may cause dizziness in some people
Looking after your medicine
- Keep your medicine in the original container. If you take it out of its original container it may not keep well.
- Keep your medicine below 25°C.
Store it in a cool dry place away from moisture, heat or sunlight; for example, do not store it:
- in the bathroom or near a sink, or
- in the car or on window sills.
Keep it where young children cannot reach it.
When to discard your medicine
If your doctor tells you to stop taking this medicine or the expiry date has passed, ask your pharmacist what to do with any medicine that is left over.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
| Speak to your doctor if you have any of these less serious side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
disorder of the skin or mucous membranes starting with a fever and flu-like symptoms and rash | Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. |
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What VASODRINE contains
| Active ingredient (main ingredient) | midodrine hydrochloride |
| Other ingredients (inactive ingredients) | microcrystalline cellulose maize starch magnesium stearate colloidal anhydrous silica |
Do not take this medicine if you are allergic to any of these ingredients.
This medicine does not contain lactose, sucrose, gluten, tartrazine or any other azo dyes.
This medicine is not addictive.
What VASODRINE looks like
VASODRINE 2.5 mg (containing 2.5 mg of midodrine hydrochloride) are white, flat, round tablets with 7 mm diameter and embossed with “2.5”
(AUST R 309183).
VASODRINE 5 mg (containing 5 mg of midodrine hydrochloride) are white, flat, round tablets with 10 mm diameter and embossed with “5”.
(AUST R 309184).
Available in blisters of 60, 90 and 500 tablets.
Not all strengths and presentations may be marketed.
Who distributes VASODRINE
Southern XP Pty Ltd
Unit 5/118 Church St
Hawthorn, VIC, 3122
Australia
Sponsor:
Southern XP IP Pty Ltd
Unit 5/118 Church Street
Hawthorn, VIC, 3122
Australia
This leaflet was prepared in August 2025.
Brand Information
| Brand name | Vasodrine |
| Active ingredient | Midodrine hydrochloride |
| Schedule | S4 |
MIMS Revision Date: 01 October 2025
Notes
Distributed by Southern XP Pty Ltd
1 Name of Medicine
Midodrine hydrochloride.
2 Qualitative and Quantitative Composition
Vasodrine tablets contain 2.5 and 5 mg of midodrine hydrochloride. For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Vasodrine 2.5 mg tablets are white, flat, round tablets with 7 mm diameter and embossed with "2.5".
Vasodrine 5 mg tablets are white, flat, round tablets with 10 mm diameter and embossed with "5".
4 Clinical Particulars
4.1 Therapeutic Indications
Vasodrine is indicated in adults for the treatment of severe symptomatic orthostatic hypotension due to autonomic dysfunction when exacerbating factors have been addressed and other forms of treatment remain inadequate.
4.2 Dose and Method of Administration
Dosage. The initiation of midodrine should be undertaken under close medical supervision in a controlled clinical setting by a specialist with expertise in the treatment of severe orthostatic hypotension.
Initial dose: 2.5 mg three times a day. Depending on the results of supine and standing blood pressure recordings, this dose may be increased weekly up to a dose of 10 mg three times a day. This is the usual maintenance dosage, however, twice daily dosing may be appropriate for some patients.
The maximum recommended dose should not exceed 30 mg daily.
A careful evaluation of the response to treatment and of the overall balance of the expected benefits and risks needs to be undertaken before any dose increase or advice to continue therapy for long periods. Monitoring ambulatory blood pressure over a 24 hour period is recommended.
The last daily dose should be taken at least 4 hours before bedtime in order to prevent supine hypertension.
Vasodrine 2.5 or 5 mg tablets may be taken with food (see Section 5.2 Pharmacokinetic Properties).
Information for the patient. Patients should be advised that they may be started on a low dose and up-titrated on a weekly basis in 2.5 mg increments to a maximum of 10 mg three time daily (TDS). The timing of doses is important and will be individualised to the patient, doses should not be spread evenly over the day and midodrine should not be taken within the 4 hour interval prior to bedtime.
Midodrine can increase the urge to urinate and can lead to volume depletion and additional fluid intake may be required.
If a dose of medication is missed, the next dose should be taken as usual and then the patient should continue taking midodrine as prescribed. A double dose should not be taken due to the increased risk of supine hypertension.
Paediatric population. The safety and efficacy of midodrine in children have not been established. No data are available.
Elderly population. There is limited data on dosing in the elderly and there are no specific studies which have focused on a possible dose reduction in the elderly population. Cautious dose titration is recommended. A starting dose of 2.5 mg three times daily and increasing only at 2-3 monthly intervals, may be helpful in reducing adverse reactions in elderly patients.
Patients with renal impairment. There are no specific studies that have focused on a possible dose reduction in patients with renal impairment. Midodrine is contraindicated in patients with acute renal impairment and severe renal impairment (see Section 4.3 Contraindications).
Patients with hepatic impairment. There are no specific studies in this patient population (see Section 4.4 Special Warnings and Precautions for Use).
Method of administration. For oral use.
4.3 Contraindications
Hypersensitivity to the active substance or to any of the excipients listed in Section 6.1 List of Excipients.
Severe organic heart disease (e.g. bradycardia, heart attack, congestive heart failure, cardiac conduction disturbances or aortic aneurysm).
Hypertension.
Obliterative blood vessel disease, cerebrovascular occlusions and vessel spasms.
Acute kidney disease.
Acute nephritis.
Severe renal impairment (creatinine clearance of less than 30 mL/min).
Serious prostate disorder, hypertrophy of the prostate gland with residual urine volume increased.
Urinary retention.
Proliferative diabetic retinopathy.
Phaeochromocytoma.
Hyperthyroidism or thyrotoxicosis.
Narrow angle glaucoma.
Vasovagal hypotension.
4.4 Special Warnings and Precautions for Use
Severe orthostatic hypotension with supine hypertension. Because midodrine hydrochloride can cause marked elevation of supine blood pressure, it should only be used in patients whose lives are considerably impaired despite standard clinical care including non-pharmacologic treatment, plasma volume expansion and lifestyle alterations. The use of midodrine hydrochloride in the management of symptomatic orthostatic hypotension is based primarily on a change in a surrogate endpoint of effectiveness, an increase in systolic blood pressure measured one minute after standing, a surrogate endpoint considered likely to correspond to clinical benefits. At present, however, clinical benefits of midodrine hydrochloride, principally improved ability to carry out activities of daily life, have not been verified.
The number "needed to harm" for supine hypertension was 8 (95% CI 3-27), 12-14%.
Regular monitoring of supine and standing blood pressure is necessary due to the risk of hypertension in the supine position, e.g. at night. Patients should be told to report symptoms of supine hypertension immediately such as chest pain, palpitations, shortness of breath, headache and blurred vision, and should be monitored for these side effects by the treating physician. Patients with a history of cerebrovascular accidents (CVA) or known risk factors for CVA should be monitored closely. Supine hypertension may often be controlled by an adjustment to the dose. If supine hypertension occurs, which is not overcome by reducing the dose, treatment with midodrine must be stopped.
Patients with diabetes mellitus who show high blood pressure levels in supine position due to underlying neurological disorders (diabetic autonomic neuropathy) may suffer from supine hypertension with midodrine. Hence, caution is recommended.
The time of administration of the drug is important in this context. Avoid administration in the late evening. The last daily dose should be taken at least 4 hours before bedtime in order to prevent supine hypertension. The risk of supine hypertension occurring during the night can be reduced by elevating the head.
Severe disturbances of the autonomic nervous system. In patients suffering from a severe disturbance of the autonomic nervous system, administration of midodrine may lead to a further reduction of blood pressure when standing. If this occurs, further treatment with midodrine should be stopped.
Atherosclerotic disease. Caution must be observed in patients with atherosclerotic disease especially with symptoms of intestinal angina or claudication of the legs.
Prostate disorders. Caution is advised in patients with prostate disorders. Use of the drug may cause urinary retention.
Heart rate. Slowing of the heart rate may occur after midodrine administration, due to vagal reflex. Caution is advised when midodrine is used concomitantly with cardiac glycosides (such as digitalis preparations) and other agents that directly or indirectly reduce heart rate. Patients should be monitored for signs or symptoms suggesting bradycardia.
QT interval prolongation. A retrospective analysis of a large US managed care population database reported a mean QT prolongation of 15.2 ms (95% CI:1.0, 29.4 ms, n = 21) for midodrine with other unspecified concomitant drugs and non-significant increase in the a mean QT interval prolongation of 21.3 ms (95% CI: -8.2, 50.7 ms, n = 9) for subjects when midodrine was used as a single agent. Nonclinical experiments in dogs demonstrated a small, but significant increase in the QT interval. A few cases of Torsades de pointes, arrhythmia and ventricular arrhythmias have been reported in post-marketing surveillance databases. Caution is advised when using midodrine in patients who experience bradycardia, patients with congenital QT prolongation, patients taking antiarrhythmic medications or patients taking any other medications which prolong the QT interval.
Effects of long term use. There is a lack of safety data for long-term treatment with midodrine. It is advisable to monitor the renal function and blood pressure in patients undergoing long-term treatment with midodrine.
Use with antihypertensive agents. Midodrine should be used with caution in combination with antihypertensive medications.
Use in hepatic impairment. Treatment with midodrine has not been studied in patients with hepatic impairment. It is therefore recommended to evaluate the hepatic parameters before starting treatment with midodrine and on a regular basis.
Use in renal impairment. This medicine is contraindicated in patients with acute renal impairment or severe renal impairment (see Section 4.3 Contraindications). It is therefore recommended to evaluate the renal parameters before starting treatment with midodrine and on a regular basis.
Use in the elderly. There is limited data on dosing in the elderly and there are no specific studies which have focused on a possible dose reduction in the elderly population. Cautious dose titration is recommended (see Section 4.2 Dose and Method of Administration).
Paediatric use. No data available.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Sympathomimetics and other vasopressor agents. Concomitant treatment with sympathomimetics and other vasoconstrictive substances such as decongestants, some appetite suppressants and other drugs which cause hypertension such as methyldopa, reserpine, guanethidine, tricyclic antidepressants, antihistamines, thyroid hormones and MAO-inhibitors, including treatments that are available without prescription, should be avoided as a pronounced increase in blood pressure may occur.
Ergot alkaloids. Combined administration of midodrine and dihydroergotamine is not recommended based on alpha receptor interactions that may diminish any desired pressor effects.
Alpha-adrenergic antagonists. As with other specific α-adrenergic agonists, the effect of midodrine is blocked by α-adrenergic antagonists such as prazosin and phentolamine. Similarly, midodrine may reduce the hypotensive effect of prazosin.
Heart rate reducing drugs. Monitoring is recommended if midodrine is combined with other drugs that directly or indirectly reduce the heart rate.
Drugs which prolong the QT interval. Caution is advised when using midodrine in patients taking antiarrhythmic medications or patients taking any other medications which prolong the QT interval as a few cases of Torsades de pointes, arrhythmia and ventricular arrhythmias have been reported in post-marketing surveillance databases (see Section 4.4 Special Warnings and Precautions for Use).
Glycosides. Simultaneous use of digitalis or other glycoside preparations or psychopharmaceutical drugs (specifically tricyclic antidepressants, phenothiazines and atypical antipsychotics) is not recommended, as the heart rate reducing effect may be potentiated by midodrine and heart block may occur.
Corticosteroid preparations. Midodrine may potentiate or enhance the hypertensive effects of corticosteroid preparations. Patients being treated with midodrine in combination with mineralocorticoids or glucocorticoids (e.g. fludrocortisone) may be at increased risk of glaucoma/increased intraocular pressure and should be carefully monitored.
Antihypertensive agents. Caution is recommended when prescribing concomitant anti-hypertensive treatments (see Section 4.4 Special Warnings and Precautions for Use).
Potential pharmacokinetic interactions. The oral absorption of midodrine is facilitated by the intestinal coupled peptide transporter (PEPT1). Because PEPT1 can transport various peptide-like drugs, such as β-lactam antibiotics and antiviral drugs, there is potential for substrate competition and altered absorption via PEPT1 mediated transport.
The 5'-O-demethylation in human liver microsomes of desglymidodrine, the active metabolite of midodrine, was catalyzed primarily by CYP 2D6. CYP 1A2 and CYP2C19 were also found to catalyse formation of the desmethyl metabolite, although the activity was very low. Inhibitors of CYP2D6, such as quinidine, may enhance and prolong the activity of desglymidodrine.
Decreased clearance of medicinal products metabolised by CYP2D6 (e.g. promethazine) has been reported.
It appears possible, although there is no supporting experimental evidence, that the high renal clearance of desglymidodrine (a base) is due to active tubular secretion by the base-secreting system also responsible for the secretion of such drugs as metformin, cimetidine, ranitidine, procainamide, triamterene, flecainide, and quinidine. Thus, there may be a potential for drug-drug interactions with these drugs.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. Animal studies are insufficient with respect to the assessment of fertility.
Use in pregnancy. (Category C)
There are no data from the use of midodrine hydrochloride in pregnant women. Studies in animals have shown reproductive toxicity at maternally toxic doses. Midodrine increased the rate of embryo resorption, reduced foetal body weight in rats and rabbits, and decreased foetal survival in rabbits when given in doses 13 (rat) and 7 (rabbit) times the maximum human dose based on body surface area (mg/m2).
Vasodrine 2.5 or 5 mg tablets are not recommended during pregnancy and in women of childbearing potential not using contraception.
Use in lactation. It is unknown whether midodrine and its metabolites are excreted in human milk.
A risk to newborns/infants cannot be excluded. Vasodrine 2.5 or 5 mg tablets should not be used during breastfeeding.
4.7 Effects on Ability to Drive and Use Machines
Vasodrine 2.5 or 5 mg tablets have negligible influence on the ability to drive and use machines. However, patients who experience dizziness or light-headedness should refrain from driving or operating machinery.
4.8 Adverse Effects (Undesirable Effects)
Clinical trial experience. The most frequent adverse effects from the phase III clinical study (Low 19971) were pilomotor reactions and supine hypertension. The midodrine group had a significantly greater frequency of overall adverse events than placebo (p = 0.001). The most common adverse reactions of midodrine treatment resulting in discontinuation from the study were pilomotor reactions (n = 3), urinary urgency or frequency (n = 7) and supine hypertension (n = 5). See Table 1.
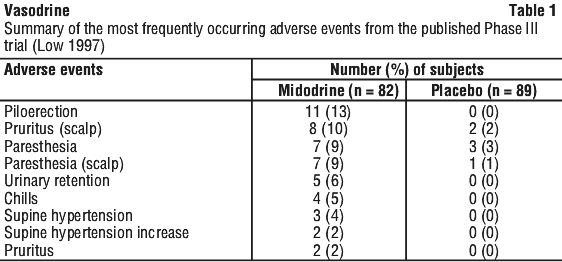
A second meta-analysis of 11 randomised controlled trials (The Izcovich 20143, n = 593) meta-analysis described the most frequently reported adverse effects as pilomotor reactions described as pruritus/tingling of the scalp, goose bumps, "prickly feeling", paraesthesia or piloerection, as well as chills and abdominal discomfort. Izcovich 2014 calculated a risk ratio for minor side effects to occur in midodrine-patients at 4.58 (95% CI 2.03-10.37) compared to placebo. The most frequent side effects that led to a discontinuation of midodrine were supine hypertension, pilomotor reactions, and urinary problems (urinary retention, hesitancy or urgency). The increased risk of supine hypertension in midodrine-treated patients compared to placebo was calculated as a risk ratio of 5.31 (95% CI 1.39-20.27, risk difference 7% [95% CI 2-11%].
Summary of the safety profile. The most frequent and very common adverse reactions related to midodrine therapy are piloerection, pruritus of the scalp and dysuria. See Table 2.
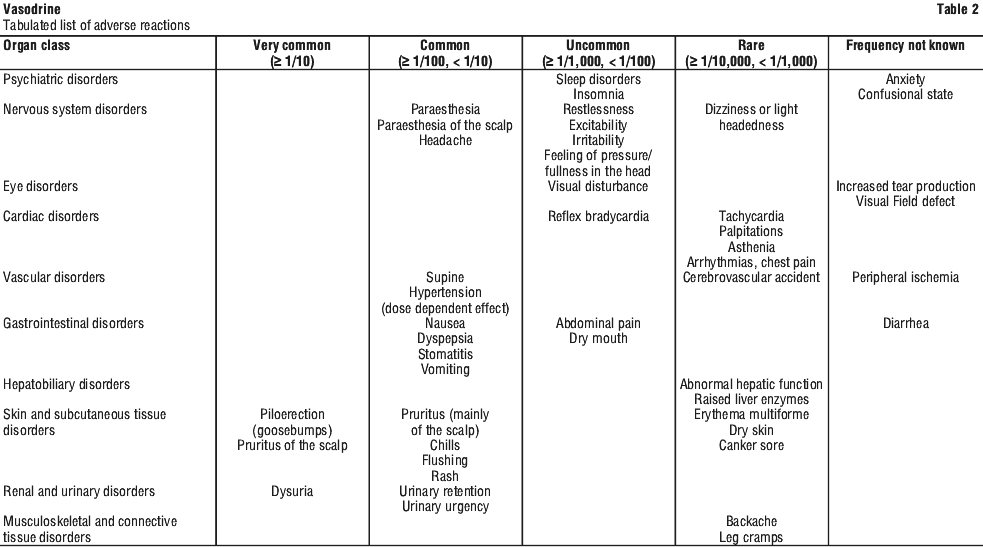
Very common (> 1/10); common (> 1/100, < 1/10); uncommon (> 1/1000, < 1/100); rare (> 1/10,000, < 1/1000); very rare (< 1/10,000).
Psychiatric disorders. Uncommon: sleep disorders, insomnia.
Nervous system disorders. Uncommon: restlessness, excitability, irritability.
Cardiac disorders. Uncommon: reflex bradycardia;
Rare: tachycardia.
Gastrointestinal disorders. Common: heartburn, stomatitis.
Hepatobiliary disorders. Rare: Hepatic function abnormal, raised liver enzymes.
Respiratory, thoracic and mediastinal disorders. Unknown: Respiratory failure.
Skin and subcutaneous tissue disorders. Common: flushing, skin rash;
Unknown: There have been cases of serious skin reactions, including Stevens-Johnson syndrome and toxic epidermal necrolysis, associated with the use of midodrine.
Vascular disorders. Common: supine hypertension (blood pressure above 180/110 mmHg) with daily doses above 30 mg;
Uncommon: supine hypertension (blood pressure above 180/110 mmHg) with daily doses above 7.5 mg.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
There are literature reports of adults ingesting from 50 mg to 350 mg midodrine as a single dose. Severe hypertension and bradycardia may occur.
The symptoms of overdose are the same as experienced with side effects. The following in particular may occur: severe hypertension, piloerection (goosebumps) and feeling cold, bradycardia (reflex bradycardia) and urinary retention.
Treatment. In addition to the main general supportive care measures, induced vomiting and the administration of an α-sympatholytic agent (e.g. nitroprusside, phentolamine, glyceryl trinitrate) is recommended, based on the pharmacology of the drug.
Bradycardia and bradycardic conduction disturbances can be blocked by atropine.
The active metabolite desglymidodrine is dialysable.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Midodrine is the rapidly absorbed prodrug of the pharmacologically active constituent desglymidodrine. Desglymidodrine is a sympathomimetic agent with a direct and selective effect on the peripheral α1-adrenergic receptors. This α1-stimulative effect induces vasoconstriction of the venous system (causing a reduction in venous pooling). The α1-adrenergic effects of desglymidodrine are almost wholly attributable to the (-) enantiomer of desglymidodrine. After taking midodrine, which is a racemic mixture, (+) desglymidodrine is also present, though this contributes almost nothing to the desired effect.
Desglymidodrine increases the peripheral arterial resistance, resulting in an increase in arterial blood pressure.
Nonclinical experiments showed that midodrine had a selective effect on blood flow in various vascular beds, with the most effect observed in the femoral artery, and least in the mesenteric artery.
Only limited data is available on the long-term effects of taking midodrine.
Stimulation of the α-adrenergic receptors of the bladder and the ureter increases the sphincter muscle tone.
Desglymidodrine has no β-adrenergic effects.
Clinical trials. The safety and efficacy of midodrine was evaluated in a published randomised, double-blind, parallel group phase III study (Low 1997, n = 171) in patients with orthostatic hypotension of any aetiology. Patients were included based on a measured reduction of supine-to-standing systolic blood pressure (BP) of at least 15 mmHg and symptoms of dizziness, lightheadedness and/or unsteadiness (collectively referred to as lightheadedness). Patients with pre-existing sustained supine hypertension above 180/110 mmHg were excluded.
Concomitant treatment with fludrocortisone acetate, high-salt diet and compression garments was permitted during the study.
The study design included a single-blind placebo one week run in period, a double-blind three week treatment period (midodrine 10 mg or placebo three times a day), and a two week single-blind placebo washout period. The primary efficacy endpoints were improvement in standing blood pressure (BP) and patients' recollection of symptoms of lightheadedness at weekly visits. The secondary endpoint was a global composite orthostatic symptom score independently rated by the investigator and the patient at the end of the treatment period which comprised of lightheadedness symptoms and improvements in the patients' ability to remain on their feet and perform orthostatic activities of daily living.
The mean age of patients was 60 years and the common underlying diagnoses were autonomic failure (Shy-Drager and Bradbury-Eggleston syndromes), diabetic autonomic neuropathy and Parkinson's disease. The study completion rate was 72% for the midodrine group (n = 59/82) and 90% for the placebo group, which was due to a higher rate number of adverse events in the midodrine group (see Section 4.8 Adverse Effects (Undesirable Effects)).
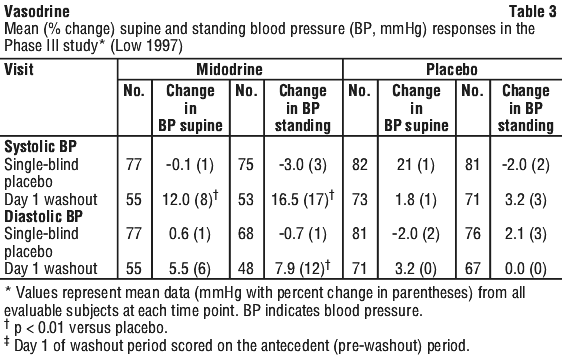
The supine and standing BP was measured before and one hour after the dose on week 2 to week 6 are shown in Table 3. The standing BP was significantly improved in the midodrine group compared with the placebo group (p < 0.001) during the treatment period. The mean increase in systolic BP was 21.8 mmHg for midodrine-treated patients, which was maintained throughout the duration of the treatment period and returned toward baseline during the washout period. A similar pattern of improvement was observed for diastolic BP. The percentage change in standing BP was approximately double the change in supine BP.
Both groups showed an improvement in symptoms during treatment relative to baseline. The mean improvement for the midodrine group was statistically greater than the placebo group at the end of the second week of treatment (p = 0.02) and approached significance at the end of the third week (p = 0.06). The improvement in the global composite orthostatic symptom score by investigators and patients also favoured midodrine treatment.
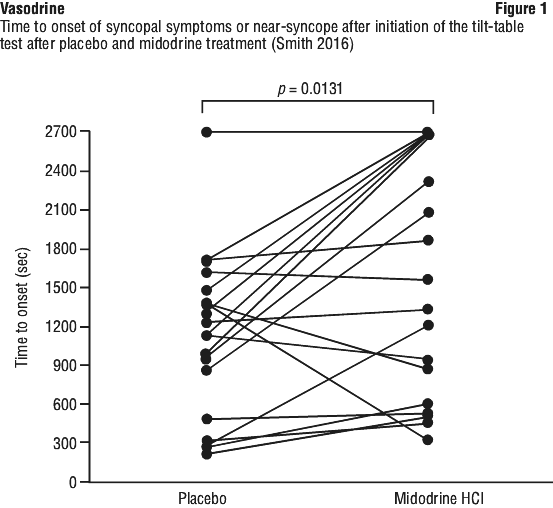
A total of 20 subjects were recruited, with 19 completing both arms. Patients were randomised into one of the two treatment sequences: midodrine followed by placebo or placebo followed by midodrine. Patients received midodrine at their pre-study dose or placebo and underwent a tilt-table test performed 1 h after administration of the treatment. The following day the alternative treatment was administered, and the tilt-table test was repeated 1 h after the treatment. The primary endpoint was the time to onset of syncopal symptoms or near-syncope (participants felt sufficiently dizzy, lightheaded, faint, or as if they were about to lose consciousness so that they requested the table to be returned to horizontal, or they looked to be about to lose consciousness based on investigator assessment) during the tilt-table test.
The final analysis set included 19 patients who completed the cross-over treatments. One patient did not complete the study due to technical problems with the tilt-table. The mean age of participants was 43.5 years (range 18-78) and the group was predominantly female (94.7%). The pre-study midodrine dose was 2.5 mg to 15 mg. Treatment with midodrine resulted in a statistically significant increase in the time to tilt-table induced syncopal symptoms or near-syncopal symptoms relative to placebo control (p = 0.0131). The least-squares mean time to onset of syncopal symptoms or near-syncope (mean ± SE) was 1626.6 ± 186.8 s after initiation of the tilt-table test after midodrine treatment and 1105.6 ± 186.8 s after the placebo (Figure 1).
5.2 Pharmacokinetic Properties
Absorption. The oral absorption of midodrine is facilitated by the intestinal coupled peptide transporter (PEPT1).
After oral administration, midodrine is rapidly absorbed. Peak plasma concentrations are reached after approximately 30 minutes, and the plasma concentration of the active metabolite, desglymidodrine, peaks after approximately 1 hour.
AUC and Cmax increase proportionally to the dose across a dosage range of 2.5-20 mg. Administration with food increases the AUC by approximately 25%, and the Cmax decreases by approximately 30%. The pharmacokinetics of desglymidodrine are not affected.
Distribution. Neither midodrine nor desgylmidodrine are bound to plasma proteins to any significant extent (less than 30%). Desglymidodrine diffuses poorly across the blood-brain barrier. Diffusion across the placenta has been reported. It is not known whether this drug is excreted in human milk.
Metabolism. Midodrine is partially hydrolysed before absorption (in the intestines), and partially after absorption (in plasma) by the separation of glycine, herewith generating the active metabolite, desglymidodrine. The mean plasma Cmax of desglymidodrine, peaks in approximately 1 hour, with a plasma half-life of approximately 3 hours after the oral administration. The elimination of desglymidodrine is primarily caused by an oxidating metabolism, followed by (partial) conjugation.
Excretion. Midodrine (8%), desglymidodrine (40%), and their degradation products (55%) are excreted in the urine by more than 90% within 24 hours in conjugated or non-conjugated forms. The plasma elimination half-life for midodrine is approximately 30 minutes and is approximately 3 hours for desglymidodrine. Elimination of the active (-) enantiomer of desglymidodrine is slower than the elimination of the inactive (+) enantiomer.
5.3 Preclinical Safety Data
Genotoxicity. Studies investigating the genotoxic potential of midodrine revealed no evidence of genotoxicity.
Carcinogenicity. In carcinogenic trials in rats, an increased tumour incidence in the testicular interstitial cells was observed; the relevance of this for humans is however unclear.
Long term studies have been conducted in rats and mice at dosages of 3 to 4 times the maximum recommended daily human dose on a mg/m2 basis, with no indication of carcinogenic effects related to midodrine.
6 Pharmaceutical Particulars
6.1 List of Excipients
Microcrystalline cellulose, pregelatinised maize starch, magnesium stearate, colloidal anhydrous silica.
6.2 Incompatibilities
Not applicable.
6.3 Shelf Life
27 months.
6.4 Special Precautions for Storage
Store below 25°C.
6.5 Nature and Contents of Container
PVC-PVDC/Aluminium foil blister.
2.5 mg. Packs of tablets 60, 90 and 500 tablets.
5 mg. Packs of tablets 60, 90 and 500 tablets.
Not all pack sizes may be marketed.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Chemical structure.
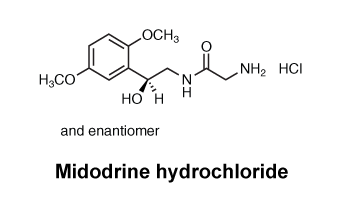
7 Medicine Schedule (Poisons Standard)
Schedule 4 - Prescription Only Medicine.
Date of First Approval
04 December 2019
Date of Revision
21 August 2025
Summary Table of Changes

References
1 Low PA, Gilden JL, Freeman R, et al. Efficacy of midodrine vs placebo in neurogenic orthostatic hypotension. A randomized, double-blind multicenter study. Midodrine Study Group. JAMA 1997;277:1046-1051.
2 Parsaik AK, Singh B, Altayar O, et al. Midodrine for orthostatic hypotension: a systematic review and meta-analysis of clinical trials. J Gen Intern Med. 2013;28(11):1496-1503.
3 Izcovich A, Gonzalez Malla C, Manzotti M, et al. Midodrine for orthostatic hypotension and recurrent reflex syncope: A systematic review. Neurology 2014;83:1170-1177.
4 Smith W, Wan H, Much D, et al. Clinical benefit of midodrine hydrochloride in symptomatic orthostatic hypotension: a phase 4, double-blind, placebo-controlled, randomized, tilt-table study. Clin Auton Res 2016; 26:269-277.
Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.