Xylocaine 10% Pump Spray
Brand Information
| Brand name | Xylocaine 10% Pump Spray |
| Active ingredient | Lidocaine (lignocaine) |
| Schedule | S2 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Xylocaine 10% Pump Spray.
Summary CMI
XYLOCAINE 10% pump spray
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I using XYLOCAINE 10% pump spray?
XYLOCAINE 10% pump spray contains the active ingredient lidocaine, an anaesthetic. XYLOCAINE 10% pump spray is used to produce temporary loss of sensation before certain types of medical examinations e.g. examination of your lungs. It is also used to help prevent pain associated with minor surgical procedures in the ear, nose and throat, to help prevent pain during the puncture of a cavity of the upper jaw, to help prevent pain and or discomfort at the dentist e.g. prior to injection, during general anaesthesia to prevent coughing, to help prevent pain during the final stages of childbirth, before the cutting or stitching of the perineum (skin between the vagina and anus).
For more information, see Section 1. Why am I using XYLOCAINE 10% pump spray? in the full CMI.
2. What should I know before I use XYLOCAINE 10% pump spray?
Do not use if you have ever had an allergic reaction to lidocaine, other local anaesthetics of the amide type or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions or take any other medicines.
For more information, see Section 2. What should I know before I use XYLOCAINE 10% pump spray? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with XYLOCAINE 10% pump spray and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How do I use XYLOCAINE 10% pump spray?
- The dose depends on the size of the area and the procedure involved. Your healthcare professional will use the dose that is suitable for you.
- Before using the spray, the bottle should be primed by pressing the piston once or twice.
More instructions can be found in Section 4. How do I use XYLOCAINE 10% pump spray? in the full CMI.
5. What should I know while using XYLOCAINE 10% pump spray?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
| Looking after your medicine |
|
For more information, see Section 5. What should I know while using XYLOCAINE 10% pump spray? in the full CMI.
6. Are there any side effects?
Tell your doctor, pharmacist or dentist as soon as possible if you do not feel well while you are being given XYLOCAINE 10% pump spray.
Some of the mild side effects include skin rash or irritation and drowsiness. Some of the serious side effects include wheezing or difficulty breathing, chest pain, severe rash or itching, increased sweating and numbness.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
XYLOCAINE 10% pump spray
Active ingredient: lidocaine
Consumer Medicine Information (CMI)
This leaflet provides important information about using XYLOCAINE 10% pump spray.
You should speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using XYLOCAINE 10% pump spray.
Where to find information in this leaflet:
1. Why am I using XYLOCAINE 10% pump spray?
2. What should I know before I use XYLOCAINE 10% pump spray?
3. What if I am taking other medicines?
4. How do I use XYLOCAINE 10% pump spray?
5. What should I know while using XYLOCAINE 10% pump spray?
6. Are there any side effects?
7. Product details
1. Why am I using XYLOCAINE 10% pump spray?
XYLOCAINE 10% pump spray contains the active ingredient lidocaine. It belongs to a group of medicines called local anaesthetics and works by producing a temporary loss of sensation in the area where it is applied.
XYLOCAINE 10% pump spray is used for the following reasons:
- to produce temporary loss of sensation in a part of the body before certain types of examination and instrumentation are performed by your doctor e.g. examination of your lungs. This may also help prevent coughing or gagging from the procedures.
- to help prevent pain associated with minor surgical procedures in the ear, nose and throat
- to help prevent pain during the puncture of a cavity of the upper jaw (the maxillary sinus)
- to help prevent pain and or discomfort at the dentist e.g. prior to injection
- during general anaesthesia to prevent coughing
- to help prevent pain during the final stages of childbirth, before the cutting or stitching of the perineum (skin between the vagina and anus).
Ask your healthcare professional if you have any questions about why XYLOCAINE 10% pump spray is used.
XYLOCAINE 10% pump spray is not addictive.
2. What should I know before I use XYLOCAINE 10% pump spray?
Warnings
Do not use XYLOCAINE 10% pump spray if:
- you are allergic to lidocaine, other local anaesthetics of the amide type or any of the ingredients listed at the end of this leaflet.
- some symptoms of an allergic reaction may include shortness of breath, wheezing or difficulty breathing, swelling of the face, lips tongue or other parts of the body and rash, itching or hives on the skin. - the expiry date printed on the pack has passed.
- the packaging is torn or shows signs of tampering.
Check with your doctor if you:
- have or have had any of these medical conditions:
- epilepsy
- heart problems
- liver problems
- kidney problems
- open wounds or infection where the spray will be used
- porphyria (a rare metabolic disorder characterised
by excessive levels of porphyrin in the blood and urine). Symptoms of acute porphyria include muscle pain or paralysis, seizures, disorientation, hallucination, bloody (red) urine, hypertension, abdominal pain, constipation and vomiting.
It may not be safe for you to use XYLOCAINE 10% pump spray if you have any of these conditions.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
There is no evidence available at the moment to show that being given XYLOCAINE 10% pump spray under your doctor's instructions is harmful to unborn babies.
Your baby can take in very small amounts of XYLOCAINE 10% pump spray from breast milk if you are breastfeeding. However, it is unlikely that the amount available to the baby will do it any harm.
3. What if I am taking other medicines?
Tell your doctor, pharmacist or dentist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines and XYLOCAINE 10% pump spray may interfere with each other. These include:
- anti-arrhythmic drugs e.g. amiodarone
- enzyme inducing drugs e.g. cimetidine or beta-blockers
- antiepileptic drugs e.g. phenobarbitone.
These medicines may affect the how it works (especially when XYLOCAINE 10% pump spray is given in repeated high doses over a long time). You may need different amounts of your medicines, or you may need to take different medicines.
4. How do I use XYLOCAINE 10% pump spray?
How much to use
This medicine is normally given by a doctor or a dentist in a clinic. For professional use only.
The dose depends on the size of the area and the procedure involved. Your healthcare professional will use the dose that is suitable for you.
How much is given
Each spray delivers 10 mg of lidocaine. The maximum dose is 20 sprays (200 mg).
In dentistry, the normal dose is 1-5 sprays. Two sprays per quarter of the mouth is recommended, with a maximum of 3 sprays per quarter of the mouth over 30 minutes.
In sinus procedures, 3 sprays are used.
In childbirth and procedures of the throat and windpipe, up to 20 sprays may be necessary.
In children, elderly or acutely ill patients, lower doses are used and depends on bodyweight and physical status.
How to use it
Before using the spray, the bottle should be primed by pressing the piston once or twice.
If you are given too much XYLOCAINE 10% pump spray
The medical professional giving you XYLOCAINE 10% pump spray will be experienced in its use, so it is extremely unlikely that you will be given too much.
Tell your doctor, nurse or dentist immediately if you experience any side effects after being given this medicine.
If any overdose occurs, you should immediately:
- phone the Poisons Information Centre
(by calling 13 11 26), or - contact your doctor, or
- go to the Emergency Department at your nearest hospital.
You should do this even if there are no signs of discomfort or poisoning.
Symptoms of overdose include light-headedness, drowsiness, dizziness and sometimes blurred vision. In the event of serious overdosage, trembling, seizures or unconsciousness may occur.
5. What should I know while using XYLOCAINE 10% pump spray?
Things you should do
Remind any health professional you visit that you are using XYLOCAINE 10% pump spray.
Things you should not do
- Do not eat or drink anything for at least 1 hour after being given XYLOCAINE 10% pump spray in the mouth or throat area.
You may swallow your food down the wrong way or burn or bite your mouth. - Be careful not to spray XYLOCAINE 10% pump spray near the eyes.
If any of the spray does go in the eye, rinse immediately with lots of water for at least 15 minutes and call your doctor.
Driving or using machines
Be careful driving or operating machinery after you have been given XYLOCAINE 10% pump spray.
Depending on the dose, you may be drowsy and your reflexes may be slow.
Looking after this medicine
XYLOCAINE 10% pump spray should be stored in a cool, dry place where the temperature stays below 25°C.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
XYLOCAINE 10% pump spray will help to prevent pain and discomfort in most people, but it may have unwanted side effects in a few people.
Tell your doctor, nurse or dentist as soon as possible if you do not feel well while you are using XYLOCAINE 10% pump spray.
See the information below and, if you need to, ask your healthcare professional if you have any further questions about side effects.
Less serious side effects
| Less serious side effects | What to do |
| Speak to your doctor or pharmacist if you have any of these mild side effects and they worry you. |
Serious side effects
| Serious side effects | What to do |
| Call your doctor or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. You may need urgent medical attention. Serious side effects are rare. |
XYLOCAINE 10% pump spray can pass into the bloodstream, and in high doses can cause more serious side effects. These may include:
| Call your doctor or go straight to the Emergency Department at your nearest hospital if you notice any of these serious side effects. You may need urgent medical attention. Serious side effects are rare. |
Tell your clinician if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
7. Product details
This medicine is available without a doctor's prescription. For professional use only.
What XYLOCAINE 10% pump spray contains
| Active ingredient (main ingredient) |
|
| Other ingredients (inactive ingredients) |
|
| Potential allergens |
|
Do not take this medicine if you are allergic to any of these ingredients.
What XYLOCAINE 10% pump spray looks like
XYLOCAINE 10% pump spray is a clear or almost clear slightly coloured liquid in a glass bottle closed by a spray head and pump assembly. Available in a pack size of 50 mL which is sufficient for 500 sprays.
The pack also contains one short single use disposable nozzle. Additional short and long disposable nozzles are available separately. Nozzles should not be reused and should be discarded immediately after use. Do not use the same nozzle on different people.
Australian Registration number: AUST R 134540
Who distributes XYLOCAINE 10% pump spray?
Aspen Pharmacare Australia Pty Ltd
34-36 Chandos St
St Leonards NSW 2065
Australia
This leaflet was revised in June 2025.
Brand Information
| Brand name | Xylocaine 10% Pump Spray |
| Active ingredient | Lidocaine (lignocaine) |
| Schedule | S2 |
MIMS Revision Date: 01 December 2024
1 Name of Medicine
Lidocaine.
2 Qualitative and Quantitative Composition
Xylocaine 10% Pump Spray contains lidocaine as the active ingredient.
Each metered dose from Xylocaine 10% Pump Spray delivers 0.1 mL and contains 10 mg lidocaine.
Excipients with known effect include alcohol and saccharin.
For the full list of excipients, see Section 6.1 List of Excipients.
Xylocaine 10% Pump Spray does not contain any CFC propellants.
3 Pharmaceutical Form
A clear or almost clear slightly coloured liquid in a glass bottle closed by a spray head and pump assembly.
4 Clinical Particulars
4.1 Therapeutic Indications
Xylocaine 10% Pump Spray is used for surface anaesthesia of the mucous membranes prior to the following procedures:
Otorhinolaryngology. To prepare for puncture of the maxillary sinus; for analgesia of the pharynx to prevent gagging and stress reactions when inserting instruments.
Dental practice. Before injections, treating minor abscesses, suture removal, deep scaling and to prevent gagging when taking intraoral impressions and X-rays.
General anaesthesia. To prevent coughing with an endotracheal tube in situ during light surgical anaesthesia.
Obstetrics. During the final stages of delivery and before episiotomy and perineal suturing as supplementary pain control.
4.2 Dose and Method of Administration
As with any local anaesthetic, reactions and complications are best averted by employing the minimal effective dosage. Debilitated, acutely ill or elderly patients and children should be given doses commensurate with their age and physical condition.
The dose of topical lidocaine should be taken into consideration in estimating the total dose of lidocaine if parenteral lidocaine is to be administered concomitantly.
The number of sprays used will depend on the extent of the area to be anaesthetised. It is unnecessary to dry the site prior to application. Each activation of the metered dose valve delivers 10 mg of lidocaine.
Before using the spray, the bottle should be primed by pressing the piston once or twice.
Additional short and long disposable nozzles are available separately. Nozzles should not be reused and should be discarded immediately after use. Do not use the same nozzle on different patients.
Adults. No more than 20 sprays (total dose 200 mg lidocaine) should be used in any adult to produce the desired anaesthetic effect.
Dental practice. 1 - 5 sprays to the mucous membranes. Two sprays per quadrant of oral mucosa are recommended as the upper limit and, under no circumstances should the dose exceed 3 sprays per quadrant of oral mucosa over 30 minutes.
Otorhinolaryngology. 3 sprays for puncture of the maxillary sinus.
During delivery. Up to 20 sprays.
Introduction of instruments and catheters into the respiratory and digestive tract. Up to 20 sprays for procedures in pharynx, larynx and trachea.
Children. In children aged 3 - 12 years, the dose should not exceed 3 mg/kg of bodyweight. When used mainly in the larynx and trachea the dose should be reduced to 1.5 mg/kg of bodyweight. In children under the age of 3, less concentrated lidocaine solutions are recommended.
4.3 Contraindications
Known history of hypersensitivity to lidocaine or other local anaesthetics of the amide type or to other components of the spray solution.
4.4 Special Warnings and Precautions for Use
Warning. Excessive dosage, or short intervals between doses, can result in high levels of lidocaine or its metabolites and serious adverse effects. Patients should be instructed to strictly adhere to the recommended dosage and administration guidelines.
The lowest dose that results in effective anaesthesia should be used to avoid high plasma levels and serious adverse effects. Tolerance to elevated blood levels varies with the status of the patient.
Dosage reduction. Debilitated, elderly and/or acutely ill patients, and children should be given reduced doses commensurate with their age and physical status.
Excessive absorption. Absorption from wound surfaces and mucous membranes is relatively high, especially in the bronchial tree. Such applications may therefore result in rapidly rising or excessive plasma concentrations, with an increased risk of toxic symptoms, such as convulsions. Because of the possibility of significant systemic absorption, Xylocaine 10% Pump Spray should be used with caution in patients with wounds, traumatised mucosa and/or sepsis in the region of the proposed application. The management of serious adverse reactions may require the use of resuscitative equipment, oxygen and other resuscitative drugs.
If the dose or site of administration is likely to result in high blood levels, lidocaine, in common with other local anaesthetics, should be used with caution in patients with epilepsy, impaired cardiac conduction, bradycardia, cardiovascular disease and heart failure, impaired hepatic function, severe shock, severe renal dysfunction, in elderly patients and patients with poor general health.
Eating and drinking. The use of topical anaesthetic agents in the oral cavity may interfere with swallowing and thus enhance the danger of aspiration of food or drink. For this reason, food or drink should not be ingested within 60 minutes of using local anaesthetics in the mouth or throat area. Numbness of the tongue or buccal mucosa may increase the danger of biting or heat trauma. Food, chewing gum or hot drinks should not be taken while the mouth or throat area is anaesthetised.
Contact with the eyes. Xylocaine 10% Pump Spray is not intended for ophthalmological use. If the spray inadvertently comes into contact with the eyes, rinse immediately with copious amounts of water for at least 15 minutes and seek medical advice.
Paralysed patients. In paralysed patients under general anaesthesia, higher blood concentrations may occur than in spontaneously breathing patients. Unparalysed patients are more likely to swallow a large proportion of the dose, which then undergoes first-pass hepatic metabolism following absorption from the gut.
Malignant hyperthermia. Many drugs used during the conduct of anaesthesia are considered potential triggering agents for familial malignant hyperthermia. It has been shown that the use of amide local anaesthetics in malignant hypothermia patients is generally safe, but cases of malignant hyperthermia have occasionally been documented after use.
Porphyric patients. Xylocaine 10% Pump Spray is probably porphyrinogenic and should only be used on patients with acute porphyria where there are strong or urgent indications. Appropriate precautions should be taken for all porphyric patients.
Directions for use of spray nozzles. The short spray nozzles for Xylocaine 10% Pump Spray are already bent to their final appearance and should not be manipulated any further. Inappropriate manipulation can weaken the integrity of the nozzle, which might lead to the nozzle tip being dislodged. The nozzle must not be shortened, otherwise the spray function will be destroyed. If used correctly, the nozzles pose no risk to the patient.
Each pack contains one short, single use, disposable nozzle. Additional short and long disposable nozzles are available separately. Nozzles should not be reused and should be discarded immediately after use. Do not use the same nozzle on different patients.
Hepatic impairment. See Section 4.4 Special Warnings and Precautions for Use, Excessive absorption.
Use in renal impairment. See Section 4.4 Special Warnings and Precautions for Use, Excessive absorption.
Use in the elderly. See Section 4.4 Special Warnings and Precautions for Use, Excessive absorption.
Paediatric use. See Section 4.4 Special Warnings and Precautions for Use, Dosage reduction.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Antiarrhythmic drugs. Lidocaine should be used with caution in patients receiving other local anaesthetics or agents structurally related to amide-type local anaesthetics e.g. antiarrhythmic drugs, such as mexiletine, since the toxic effects are additive.
Patients treated with anti-arrhythmic drugs class III (e.g. amiodarone) should be under close surveillance and ECG monitoring considered, since cardiac effects may be additive.
Specific interaction studies with lidocaine and anti-arrhythmic drugs class III (e.g. amiodarone) have not been performed, but caution is advised.
Xylocaine 10% Pump Spray should not be used on cuffs of endotracheal tubes (ETT) made of plastic. Lidocaine base in contact with both PVC and non-PVC cuffs of endotracheal tubes may cause damage of the cuff. This damage is described as pinholes, which may cause leakage that could lead to pressure loss in the cuff.
Enzyme inducing drugs. Drugs that reduce the clearance of lidocaine (e.g. cimetidine or beta-blockers) may cause potentially toxic plasma concentrations when lidocaine is given in repeated high doses over a long time period. Such interactions should therefore be of no clinical importance following short-term treatment with lidocaine (e.g. Xylocaine 10% Pump Spray) at recommended doses. Caution should be taken if any of these drugs are administered concurrently with lidocaine.
Phenytoin and other antiepileptic drugs such as phenobarbitone, primidone and carbamazepine, appear to enhance the metabolism of lidocaine but the significance of this effect is not known. Phenytoin and lidocaine have additive cardiac depressant effects.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. No data available.
Use in pregnancy. (Category A)
Lidocaine crosses the placental barrier and may be taken up by foetal tissues. When used for surface anaesthesia, lidocaine blood levels after normal doses are low so little drug is available for placental transfer.
There are, however, no adequate and well-controlled studies in pregnant women.
It is reasonable to assume that a large number of pregnant women and women of childbearing age have used lidocaine. No specific disturbances to the reproduction process have so far been reported.
Lidocaine is not contraindicated in labour and delivery.
Use in lactation. Lidocaine enters breast milk, but in such small quantities that there is generally no risk of affecting the child at therapeutic dose levels.
4.7 Effects on Ability to Drive and Use Machines
Depending on the dose, local anaesthetics may have a very mild effect on mental function and may temporarily impair locomotion and coordination.
4.8 Adverse Effects (Undesirable Effects)
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
Systemic adverse reactions are rare and may result from high plasma levels caused by excessive dosage or rapid absorption, or may result from a hypersensitivity, idiosyncrasy or reduced tolerance on the part of the patient. Such reactions are systemic in nature and involve the central nervous system and/or the cardiovascular system.
Central nervous system. CNS reactions are excitatory and/or depressant and may be characterised by rapid eyeball movement, speech paralysis, lightheadedness, nervousness, apprehension, euphoria, confusion, dizziness, drowsiness, tinnitus, blurred vision, vomiting, sensations of heat, cold or numbness, twitching, tremors, convulsions, unconsciousness and possibly respiratory arrest. The excitatory reactions may be brief or may not occur at all, in which case the first manifestations of toxicity may be drowsiness, progressing to unconsciousness and respiratory arrest.
Drowsiness following administration of lidocaine is usually an early sign of a high blood level of the drug and may occur as a result of rapid absorption.
Cardiovascular. Cardiovascular reactions are usually depressant and may be characterised by hypotension, myocardial depression, bradycardia and possibly cardiac arrest.
Allergic reactions. Allergic reactions may occur as a result of sensitivity either to the local anaesthetic agent or to other ingredients in the formulation. Allergic reactions as a result of sensitivity to lidocaine are extremely rare. The detection of sensitivity by skin testing is of doubtful value.
The extremely rare cases of allergy to local anaesthetic preparations have included bronchospasm, chest pain, dyspnoea, pruritus, rash, rhinitis, increased sweating, urticaria, sleepiness, dizziness, paraesthesia, oedema, and in the most severe instances anaphylactic shock. Several cases of contact dermatitis have been reported with the use of lidocaine.
Local reactions. Local irritation at the application site has been described. Following application to laryngeal mucosa before endotracheal intubation, reversible symptoms such as 'sore throat', 'hoarseness' and 'loss of voice' have been reported. The use of Xylocaine 10% Pump Spray provides surface anaesthesia during an endotracheal procedure but does not prevent post-intubation soreness.
4.9 Overdose
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
Management of local anaesthetic emergencies. The first consideration is prevention, best accomplished by careful and constant monitoring of cardiovascular and respiratory vital signs and the patient's state of consciousness after each local anaesthetic administration. At the first sign of change, oxygen should be administered.
Treatment. Should symptoms of systemic toxicity occur, the signs are anticipated to be similar in nature to those following the administration of local anaesthetics by other routes. Local anaesthetic toxicity is manifested by symptoms of nervous system excitation and, in severe cases, central nervous and cardiovascular depression.
If circulatory arrest should occur, immediate cardiopulmonary resuscitation should be instituted. Optimal oxygenation and ventilation and circulatory support as well as treatment of acidosis are of vital importance.
If convulsions or other severe neurological symptoms occur, such as CNS depression, then immediate attention is required for the maintenance of a patent airway and assisted or controlled ventilation with oxygen, via a positive airway pressure delivery system mask. Adequacy of the circulation should then be evaluated, bearing in mind that drugs used to treat convulsions depress the circulation when administered IV.
Should convulsions persist despite adequate respiratory support, and if the status of the circulation permits, appropriate anticonvulsant medication such as an ultra-short acting barbiturate or a benzodiazepine may be administered IV. The clinician should be familiar with these anticonvulsant drugs prior to use of local anaesthetics.
Dialysis is of negligible value in the treatment of acute overdosage with lidocaine.
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Mechanism of action. Lidocaine, the active ingredient of Xylocaine 10% Pump Spray, stabilises the neuronal membrane and prevents the initiation and conduction of nerve impulses, thereby effecting local anaesthetic action.
Xylocaine 10% Pump Spray acts on intact mucous membranes to provide prompt local anaesthetic action. Anaesthesia occurs usually within 1-5 minutes and the effect lasts for approximately 10-15 minutes.
Clinical trials. No data available.
5.2 Pharmacokinetic Properties
Absorption. Lidocaine may be absorbed following topical administration to mucous membranes, its rate of absorption and amount of dose absorbed depending upon concentration and total dose administered, the specific site of application and duration of exposure. In general, the rate of absorption occurs most rapidly after intratracheal and bronchial administration. Lidocaine is well absorbed from the gastrointestinal tract, but little intact drug appears in the circulation because of biotransformation in the liver. Lidocaine is metabolised rapidly by the liver, and metabolites and unchanged drug are excreted by the kidney.
Distribution. Excessive blood levels may cause changes in cardiac output, total peripheral resistance and mean arterial pressure. These changes may be attributable to a direct depressant effect of the anaesthetic agent on various components of the cardiovascular system.
Metabolism. Biotransformation includes oxidative N-dealkylation, ring hydroxylation, cleavage of the amide linkage and conjugation. The pharmacological/ toxicological actions of the metabolites are similar to, but not less potent than, those of lidocaine. Approximately 90% of lidocaine is excreted in the form of various metabolites, and less than 10% is excreted unchanged. The primary metabolite in urine is a conjugate of 4-hydroxy-2,6-dimethylaniline.
The plasma binding of lidocaine is dependent on drug concentration, and the fraction bound decreases with increasing concentration. At concentrations of 1 to 4 microgram of free base/mL, 60 to 80% of lidocaine is protein bound. Binding is also dependent on the plasma concentrations of the alpha-1-acid glycoprotein.
Lidocaine crosses the blood brain and placental barriers, presumably by passive diffusion.
Studies of lidocaine metabolism following IV bolus injection have shown that the elimination half-life is usually 1.5 to 2 hours. The half-life may be prolonged 2-fold or more in patients with liver dysfunction. Renal dysfunction does not affect lidocaine kinetics, but may increase the accumulation of metabolites.
Factors such as acidosis and the use of CNS stimulants and depressants affect the CNS levels of lidocaine required to produce overt systemic effects. Objective adverse manifestations become increasingly apparent with increasing venous plasma levels above 6.0 microgram free base/mL. In the rhesus monkey arterial blood levels of 18 to 21 microgram/mL have been shown to be the threshold for convulsive activity.
5.3 Preclinical Safety Data
Genotoxicity. Reproduction studies have been performed in rats at doses of 500 mg/kg/day and have revealed no evidence of harm to the foetus caused by lidocaine.
Carcinogenicity. Genotoxicity tests with lidocaine are inconclusive. In genotoxicity studies, a metabolite of lidocaine, 2,6-xylidine, showed evidence of activity in some tests but not in other tests. This metabolite has been shown to have carcinogenic potential (nasal and subcutaneous tumours) in preclinical toxicological studies evaluating chronic exposure.
6 Pharmaceutical Particulars
6.1 List of Excipients
Banana flavour PHL-131980, ethanol, macrogol 400, menthol, purified water and saccharin.
6.2 Incompatibilities
Incompatibilities were either not assessed or not identified as part of the registration of this medicine.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store below 25°C.
6.5 Nature and Contents of Container
Xylocaine 10% Pump Spray, 50 mL pump actuated glass bottle, equipped with a metering pump with immersion tube and one short, single use, disposable plastic nozzle. Each 100 microL metered dose delivers 10 mg of lidocaine. Additional short and long disposable nozzles are available separately.
6.6 Special Precautions for Disposal
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Lidocaine is a white or almost white crystalline powder, practically insoluble in water, very soluble in alcohol and in methylene chloride, freely soluble in ether.
The chemical name for lignocaine is 2-diethylamino-2', 6'-dimethylacetanilide.
Molecular formula: C14H22N2O, molecular weight: 234.3.
Chemical structure.
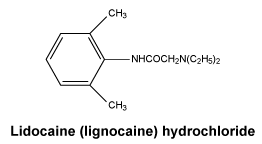
7 Medicine Schedule (Poisons Standard)
S2 - Pharmacy Medicine.
Date of First Approval
22 January 2007
Date of Revision
18 October 2024
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.