Zavedos
Brand Information
| Brand name | Zavedos |
| Active ingredient | Idarubicin hydrochloride |
| Schedule | S4 |
Consumer Medicine Information (CMI) leaflet
Please read this leaflet carefully before you start using the Zavedos.
Summary CMI
ZAVEDOS®
Consumer Medicine Information (CMI) summary
The full CMI on the next page has more details. If you are worried about using this medicine, speak to your doctor or pharmacist.
1. Why am I being given ZAVEDOS?
ZAVEDOS contains the active ingredient idarubicin hydrochloride. ZAVEDOS is used to treat a type of leukemia in adults known as AML (acute myelogenous leukaemia).
For more information, see Section 1. Why am I being given ZAVEDOS? in the full CMI.
2. What should I know before I am given ZAVEDOS?
You will not be given ZAVEDOS if you have ever had an allergic reaction to idarubicin hydrochloride, other similar medicines for cancer or any of the ingredients listed at the end of the CMI.
Talk to your doctor if you have any other medical conditions especially problems with your heart, take any other medicines, or are pregnant or unsure if you are pregnant or are breastfeeding.
For more information, see Section 2. What should I know before I am given ZAVEDOS? in the full CMI.
3. What if I am taking other medicines?
Some medicines may interfere with ZAVEDOS and affect how it works.
A list of these medicines is in Section 3. What if I am taking other medicines? in the full CMI.
4. How is ZAVEDOS given?
ZAVEDOS is injected slowly into a vein. It must only be given by a doctor or nurse. Your doctor will decide what dose, how often, and how long you will receive it.
More instructions can be found in Section 4. How is ZAVEDOS given? in the full CMI.
5. What should I know while being given ZAVEDOS?
| Things you should do |
|
| Things you should not do |
|
| Driving or using machines |
|
For more information, see Section 5. What should I know while being given ZAVEDOS? in the full CMI.
6. Are there any side effects?
Side effects may include: red-coloured urine for 1-2 days after treatment, nausea, vomiting, diarrhoea, loss of appetite, stomach pain & discomfort, mouth ulcers, redness & irritation of the throat & mouth with difficulty in swallowing & eating, skin changes, loss of hair, hot flushes, allergic reactions; skin rash; itching; redness of the skin or hives; signs of infection; signs of anaemia, bleeding or bruising more easily than normal; shock due to a dangerous drop in blood pressure which may lead to collapse & coma; signs of sepsis or blood poisoning; chest pain; abnormal heartbeat; fast heartbeat; shortness of breath; swelling in the feet or legs due to fluid build-up; vomiting blood or bleeding from the back passage; black sticky bowel motions or bloody diarrhoea; swelling and redness along a vein which is extremely tender when touched.
For more information, including what to do if you have any side effects, see Section 6. Are there any side effects? in the full CMI.
Full CMI
ZAVEDOS®
Active ingredient: idarubicin hydrochloride
Consumer Medicine Information (CMI)
This leaflet provides important information about using ZAVEDOS. You should also speak to your doctor or pharmacist if you would like further information or if you have any concerns or questions about using ZAVEDOS.
Where to find information in this leaflet:
1. Why am I being given ZAVEDOS?
2. What should I know before I am given ZAVEDOS?
3. What if I am taking other medicines?
4. How is ZAVEDOS given?
5. What should I know while being given ZAVEDOS?
6. Are there any side effects?
7. Product details
1. Why am I being given ZAVEDOS?
ZAVEDOS contains the active ingredient idarubicin hydrochloride.
ZAVEDOS is used to treat a type of leukaemia in adults known as AML (acute myelogenous leukaemia). It works by stopping cancer cells from growing and multiplying. It may be used alone or in combination with other chemotherapy.
Your doctor may have prescribed ZAVEDOS for another reason.
Ask your doctor if you have any questions about why ZAVEDOS has been prescribed for you.
There is no evidence that ZAVEDOS is addictive.
ZAVEDOS is only available with a doctor's prescription.
2. What should I know before I am given ZAVEDOS?
Warnings
You should not be given ZAVEDOS if:
- you are allergic to idarubicin hydrochloride, or any of the ingredients listed at the end of this leaflet.
- you are allergic to any other similar medicines for cancer, e.g., daunorubicin, doxorubicin, epirubicin, mitoxantrone
- Some of the symptoms of an allergic reaction may include:
- shortness of breath, wheezing or difficulty breathing
- swelling of the face, lips, tongue or other parts of the body
- rash, itching or hives on the skin. - you have severe kidney problems
- you have severe liver problems
- you have severe heart problems including heart failure, abnormal heartbeat or a recent heart attack
- you have a severe infection, with signs such as fever, severe chills, sore throat or mouth ulcers
- you have a reduced number of red or white blood cells or platelets
- you have previously received the full course of treatment with the maximum dose of idarubicin or other similar medicines e.g., daunorubicin, doxorubicin, epirubicin, mitozantrone/mitoxantrone
- you are pregnant or trying to become pregnant.
Tell your doctor if you have or have had any medical conditions, especially the following:
- kidney disease
- liver disease
- heart disease
- previous treatment with ZAVEDOS or any other chemotherapy
- previous radiation therapy
- anaemia
- bone marrow transplant
- bone marrow depression, a blood disorder with low platelet, red blood and white blood cell counts
- infection or high temperature, severe chills, sore throat or mouth ulcers
- stomach ulcers, or vomiting blood or bleeding from the back passage.
During treatment, you may be at risk of developing certain side effects. It is important you understand these risks and how to monitor for them. See additional information under Section 6. Are there any side effects?
Pregnancy and breastfeeding
You should not be given ZAVEDOS if you are pregnant or intend to become pregnant or your partner is trying to become pregnant.
This medicine may cause birth defects if you or your partner is being treated with it.
Talk to your doctor if you are breastfeeding or intend to breastfeed.
Women should not breastfeed during treatment with ZAVEDOS and for at least 14 days after the last dose.
Consult your doctor or midwife if you have any concerns about being unable to breastfeed for this period.
Contraception
Talk to your doctor about an effective contraceptive method and fertility preservation before starting your treatment with ZAVEDOS.
Women of childbearing potential should use effective contraception during treatment with ZAVEDOS and for at least 6.5 months after the final dose. Men with female partners of childbearing potential must use an effective contraception during treatment and for at least 3.5 months after the final dose. If planning for conception, it is advisable to seek genetic counselling.
3. What if I am taking other medicines?
Tell your doctor or pharmacist if you are taking any other medicines, including any medicines, vitamins or supplements that you buy without a prescription from your pharmacy, supermarket or health food shop.
Some medicines may interfere with ZAVEDOS and affect how it works. These include:
- other medicines for cancer
- some medicines for heart problems, including calcium channel blockers, used to treat high blood pressure and angina
- certain medicines that may affect your liver and kidney function, e.g. some antibiotics and antifungals vaccines.
These medicines may increase some side effects of ZAVEDOS including the effects on the heart, blood cells, the stomach or bowels, and reduce the body's ability to fight infection.
Check with your doctor or pharmacist if you are not sure about what medicines, vitamins or supplements you are taking and if these affect ZAVEDOS.
4. How is ZAVEDOS given?
How much and how long is it given
ZAVEDOS is given in a clinical setting by a nurse or doctor.
Your doctor will decide what dose, how often and how long you will receive it. This depends on your condition and other factors, such as your weight.
How ZAVEDOS is given
ZAVEDOS is injected slowly into a vein.
If too much ZAVEDOS is given
Since ZAVEDOS is given in a hospital or clinic under the supervision of a doctor, it is very unlikely that you will be given too much of the medicine. Your doctor or nurse will be monitoring your progress and checking the medicine that you are given.
If you think that you may have been given too much ZAVEDOS, you may need urgent medical attention.
Symptoms of an overdose may include the side effects listed in Section 6. Are there any side effects? but are usually of a more severe nature
5. What should I know while being given ZAVEDOS?
Things you should do
Keep all appointments with your doctor so that your progress can be checked.
You will have regular tests to monitor your blood count, kidney and liver function, and your heart before, during and after treatment.
If you are going to have surgery, tell the surgeon, anaesthetist or dentist that you are taking this medicine.
Call your doctor straight away if you:
- or your partner becomes pregnant while you are taking or just after you stop taking ZAVEDOS
- develop redness or swelling at the injection site.
Things to be careful of
Take the following precautions to reduce your risk of infection or bleeding:
- Avoid people who have infections. Check with your doctor immediately if you think you may be getting an infection, or if you get a fever, chills, cough, hoarse throat, lower back or side pain or find it painful or difficult to urinate
- Be careful when using a toothbrush, toothpick, or dental floss. Your doctor, dentist, nurse or pharmacist may recommend other ways to clean your teeth and gums. Check with your doctor before having any dental work
- Be careful not to cut yourself when you are using sharp objects such as a razor or nail cutters
- Avoid contact sports or other situations where you may bruise or get injured.
Driving or using machines
Be careful before you drive or use any machines or tools until you know how ZAVEDOS affects you.
6. Are there any side effects?
All medicines can have side effects. If you do experience any side effects, most of them are minor and temporary. However, some side effects may need medical attention.
See the information below and, if you need to, ask your doctor or pharmacist if you have any further questions about side effects.
Side effects
| Side effects | What to do |
Renal disorders
| Speak to your doctor if you have any of these side effects and they worry you. |
More serious side effects
| More serious side effects | What to do |
Cardiac disorders
| Call your doctor straight away, or go straight to the Emergency Department at your nearest hospital if you notice any of these more serious side effects. |
Some side effects (for example, an increase in liver enzyme levels) can only be found when your doctor does tests from time to time to check your progress.
Tell your doctor or pharmacist if you notice anything else that may be making you feel unwell.
Other side effects not listed here may occur in some people.
Reporting side effects
After you have received medical advice for any side effects you experience, you can report side effects to the Therapeutic Goods Administration online at www.tga.gov.au/reporting-problems. By reporting side effects, you can help provide more information on the safety of this medicine.
Always make sure you speak to your doctor or pharmacist before you decide to stop taking any of your medicines.
7. Product details
This medicine is only available with a doctor's prescription.
What ZAVEDOS contains
| Active ingredient (main ingredient) | idarubicin hydrochloride |
| Other ingredients (inactive ingredients) | glycerol hydrochloric acid water |
Do not take this medicine if you are allergic to any of these ingredients.
ZAVEDOS does not contain lactose, sucrose, gluten, tartrazine or any other azo dyes.
What ZAVEDOS looks like
ZAVEDOS is a red-orange coloured solution contained in a plastic or a glass vial.
Australian Registration Numbers
ZAVEDOS idarubicin hydrochloride 5mg/5mL injection vial - ARTG R 67397
ZAVEDOS idarubicin hydrochloride 10mg/10mL injection vial - ARTG R 67398
Who distributes ZAVEDOS
Pfizer Australia Pty Ltd
Sydney NSW
Toll Free Number: 1800 675 229
www.pfizermedicalinformation.com.au
This leaflet was prepared in July 2025.
® Registered Trademark
Brand Information
| Brand name | Zavedos |
| Active ingredient | Idarubicin hydrochloride |
| Schedule | S4 |
MIMS Revision Date: 01 September 2023
1 Name of Medicine
Idarubicin hydrochloride.
2 Qualitative and Quantitative Composition
Each vial contains 5 mg/5 mL or 10 mg/10 mL of idarubicin hydrochloride.
For the full list of excipients, see Section 6.1 List of Excipients.
3 Pharmaceutical Form
Solution for injection. Red-orange, clear, mobile solution, free from particles.
4 Clinical Particulars
4.1 Therapeutic Indications
Zavedos is indicated for use in acute myelogenous leukaemia (AML) in adults for remission induction in untreated patients or for remission induction in relapsed or refractory patients. Zavedos may be used in combination chemotherapy regimens involving other cytotoxic agents.
4.2 Dose and Method of Administration
Dose. For induction therapy in adult patients with AML, the following dose schedules are recommended.
Zavedos 12 mg/m2 daily for three days by slow (10-15 min) intravenous injection in combination with cytarabine 100 mg/m2 daily given by continuous infusion for seven days. In patients with unequivocal evidence of leukaemia after the first induction course, a second course may be administered. Administration of the second course should be delayed in patients who experienced severe mucositis, until recovery from this toxicity has occurred, and a dose reduction of 25% is recommended.
Dosage adjustment. Hepatic and renal impairment. Zavedos should not be administered in patients with severe renal and liver impairment (see Section 4.3 Contraindications). Dose adjustment should be considered in patients with moderate liver and renal impairment (see Section 5.2 Pharmacokinetic Properties; Section 4.4 Special Warnings and Precautions for Use). With anthracyclines a 50% dose reduction is generally employed if bilirubin levels are in the range 20.4-51.0 micromole/L.
All dosage schedules should take into account the haematological status of the patient and all the doses of other cytotoxic drugs when used in combination.
Method of administration. Intravenous infusion.
Zavedos solution for injection must be administrated only by the intravenous route and should be given via tubing of a freely running intravenous infusion of 0.9% sodium chloride injection, taking 10-15 minutes over the injection.
The tubing should be attached to a butterfly needle or other suitable device and inserted preferably into a large vein. This technique minimises the risk of thrombosis or perivenous extravasation, which can lead to severe cellulitis and necrosis. Venous sclerosis may result from injection into small veins or repeated injections in the same vein.
Care in the administration of Zavedos will reduce the chance of perivenous infiltration. It may also decrease the chance of local reactions such as urticaria and erythematous streaking.
During intravenous administration of Zavedos, extravasation may occur, with or without an accompanying stinging or burning sensation, even if blood returns well on aspiration of the infusion needle. If any signs or symptoms of extravasation have occurred, the injection or infusion should be immediately terminated and restarted in another vein. If it is known or suspected that subcutaneous extravasation has occurred, it is recommended that intermittent ice packs (½ hour immediately, then ½ hour 4 times per day for 3 days) be placed on the area of extravasation and that the affected extremity be elevated.
Because of the progressive nature of extravasation reactions, the area of injection should be frequently examined and plastic surgery consultations obtained early if there is any sign of local reaction such as pain, erythema, oedema or vesication. If ulceration begins or there is persistent pain at the site of extravasation, early wide excision of the involved area should be considered. Also see Section 4.4 Special Warnings and Precautions for Use, Effects at site of injection.
Instructions for use and handling and disposal. Caution in handling and preparation of the solution must be exercised, as skin reactions associated with Zavedos may occur. Skin exposed accidentally to Zavedos should be washed thoroughly with water, soap and water or sodium bicarbonate solution and, if the eyes are involved, standard irrigation techniques should be used immediately. Medical attention should be sought. The following protective recommendations are given due to the toxic nature of the substance.
Personnel should be trained in good technique for handling Zavedos.
Pregnant staff should be excluded from working with Zavedos.
The use of goggles, disposable masks and gloves and protective gowns are recommended during preparation and administration of the drug.
A designated area should be defined (preferably under a laminar flow system). The work surface should be protected by disposable, plastic backed absorbent paper.
All items used for administration or cleaning, including gloves, should be placed in high-risk waste disposal bags for high temperature incineration.
Spillage or leakage should be treated with dilute sodium hypochlorite (1% available chlorine) solution, preferably by soaking, and then water. All cleaning materials should be disposed of as indicated previously.
4.3 Contraindications
Zavedos therapy is contraindicated in patients with severe renal and liver impairment or patients with uncontrolled infections. It should also not be administered to individuals with hypersensitivity to idarubicin or any other component of the product (see Section 6.1 List of Excipients) and/or other anthracyclines.
Zavedos therapy is contraindicated in patients with severe myocardial insufficiency, recent myocardial infarction, severe arrhythmias, persistent myelosuppression, or previous treatment with maximum cumulative doses of idarubicin and/or other anthracyclines and anthracenediones.
Zavedos therapy is contraindicated in pregnant women or women wishing to become pregnant (see Section 4.6 Fertility, Pregnancy and Lactation, Use in pregnancy).
4.4 Special Warnings and Precautions for Use
General. Zavedos is intended for use under the direction of those experienced in leukaemia chemotherapy. Close monitoring for toxicity is mandatory.
Facilities with laboratory and supportive resources adequate to monitor drug tolerability and protect and maintain a patient compromised by drug toxicity should be available. It must be possible to treat a severe haemorrhagic condition and/or severe infection rapidly and effectively.
The drug should not be given to patients with pre-existing bone marrow depression induced by previous drug therapy or radiotherapy unless the benefit warrants the risk.
Patients should recover from acute toxicities of prior cytotoxic treatment (such as stomatitis, neutropenia, thrombocytopenia and generalised infections) before beginning treatment with idarubicin.
Pre-existing heart disease and previous therapy with anthracyclines, especially at high cumulative doses, or other potentially cardiotoxic agents are cofactors for increased risk of idarubicin induced cardiac toxicity; the benefit to risk ratio of idarubicin therapy in such patients should be weighed before starting treatment with Zavedos. Like most other cytotoxic agents, idarubicin has mutagenic properties and is carcinogenic in rats.
Haematologic toxicity. Zavedos is a potent bone marrow suppressant. Myelosuppression, primarily of leucocytes, will therefore occur in all patients given a therapeutic dose of this agent and careful haematological monitoring including granulocytes, red cells and platelets is required.
Secondary leukaemia. Secondary leukaemia, with or without a preleukaemic phase, has been reported in patients treated with anthracyclines, including idarubicin. Secondary leukaemia is more common when such drugs are given in combination with DNA damaging antineoplastic agents, when patients have been heavily pretreated with cytotoxic drugs, or when doses of the anthracyclines have been escalated. These leukaemias can have a 1 to 3 year latency period.
Cardiac function. Cardiotoxicity is a risk of anthracycline treatment that may be manifested by early (acute) or late (delayed) events.
Early (acute) events. Early cardiotoxicity of idarubicin consists mainly of sinus tachycardia and/or electrocardiogram (ECG) abnormalities, such as nonspecific ST-T wave changes. Tachyarrhythmias, including premature ventricular contractions and ventricular tachycardia, bradycardia, as well as atrioventricular and bundle branch block have also been reported. These effects do not usually predict subsequent development of delayed cardiotoxicity.
Late (delayed) events. Delayed cardiotoxicity usually develops late in the course of therapy or within 2 to 3 months after completion of treatment, but later events, several months to years after completion of treatment have also been reported. Delayed cardiomyopathy is manifested by reduced left ventricular ejection fraction (LVEF) and/or signs and symptoms of CHF such as dyspnoea, pulmonary oedema, dependent oedema, cardiomegaly and hepatomegaly, oliguria, ascites, pleural effusion and gallop rhythm. Subacute effects such as pericarditis/ myocarditis have also been reported. Life threatening CHF is the most severe form of anthracycline induced cardiomyopathy and represents the cumulative dose limiting toxicity of the drug.
Myocardial toxicity, as manifested by potentially fatal congestive heart failure, acute life threatening arrhythmias or other cardiomyopathies, may occur during therapy or several weeks after termination of therapy.
Idarubicin related cardiomyopathy was reported in 5% of patients who received cumulative intravenous doses of 150 to 290 mg/m2. Although cumulative dose limits are yet to be defined, available data on patients treated with Zavedos capsules indicate that total cumulative doses up to at least 400 mg/m2 have a low probability of cardiotoxicity. Should congestive heart failure (CHF) occur, treatment with digitalis, diuretics, sodium restriction and bed rest is indicated.
Cardiac function should be monitored carefully during treatment in order to minimise the risk of cardiac toxicity of the type described for other anthracycline compounds. Risk factors for cardiac toxicity include concomitant or previous radiation to the mediastinal/ pericardial area, previous treatment with other anthracyclines or anthracenediones at high cumulative doses, and concomitant use of drugs with the ability to suppress cardiac contractility or other potentially cardiotoxic agents (e.g. trastuzumab). Anthracyclines including idarubicin should not be administered in combination with other cardiotoxic agents unless the patient's cardiac function is closely monitored (see Section 4.5 Interactions with Other Medicines and Other Forms of Interactions). Patients receiving anthracyclines after stopping treatment with other cardiotoxic agents, especially those with long half-lives such as trastuzumab (variable half-life; washout period up to 7 months), may also be at an increased risk of developing cardiotoxicity.
Note: Trastuzumab emtansine has a shorter half-life of approximately 4 days. The half-life of trastuzumab is variable. Trastuzumab (Herceptin) may persist in the circulation for up to 7 months. Therefore, physicians should avoid anthracycline based therapy for up to 7 months after stopping trastuzumab when possible. If anthracyclines are used before this time, careful monitoring of cardiac function is recommended.
The benefit to risk ratio of Zavedos therapy in such patients should be weighed before starting treatment. The risk of such myocardial toxicity may also be higher in patients with a pre-existing heart disease or particular clinical situation due to their disease (anaemia, bone marrow depression, infections, leukaemic pericarditis and/or myocarditis).
While there is no reliable method for predicting acute congestive heart failure, cardiomyopathy induced by anthracyclines is usually associated with persistent QRS voltage reduction, increase beyond normal limits of the systolic time interval (PEP/LET) and decrease of the left ventricular ejection fraction (LVEF) from pretreatment baseline values.
Assessment of cardiac function (evaluation of LVEF) with an ECG and either a multiple gated acquisition (MUGA) scan or an echocardiogram (ECHO) should be performed prior to starting therapy with Zavedos. Repeated MUGA or ECHO determinations of LVEF should be performed, particularly with higher, cumulative anthracycline doses. The technique used for assessment should be consistent throughout follow-up. Early clinical diagnosis of drug induced myocardial damage appears to be important for pharmacological treatment to be useful.
Gastrointestinal disorders. Severe enterocolitis with perforation has been reported rarely. The risk of perforation may be increased by instrumental intervention. The possibility of perforation should be considered in patients who develop severe abdominal pain and appropriate steps for diagnosis and management should be taken.
Use in hepatic impairment. Since impairment of hepatic function may affect the disposition of idarubicin, liver function should be evaluated with conventional clinical laboratory tests (using serum bilirubin) prior to and during treatment. Idarubicin is contraindicated in severe hepatic impairment. Also see Section 4.2 Dose and Method of Administration.
Use in renal impairment. Since impairment of renal function may affect the disposition of idarubicin, kidney function should be evaluated with conventional clinical laboratory tests (using serum creatinine as indicators) prior to and during treatment. Idarubicin is contraindicated in severe renal impairment. Also see Section 4.2 Dose and Method of Administration.
Tumour lysis syndrome. Idarubicin may induce hyperuricaemia as a consequence of the extensive purine catabolism that accompanies drug induced rapid lysis of neoplastic cells ('tumour lysis syndrome'). Blood uric acid levels, potassium, calcium, phosphate and creatinine should be evaluated after initial treatment. Hydration, urine alkalinisation and prophylaxis with allopurinol to prevent hyperuricaemia may minimise potential complications of tumour lysis syndrome. Appropriate measures must be taken to control any systemic infection before beginning therapy.
Effects at site of injection. With intravenous administered Zavedos, extravasation at the site of injection can cause pain, severe local tissue lesions (vesication, severe cellulitis) and necrosis. Extravasation may occur, with or without accompanying stinging or burning sensation, even if blood returns well on aspiration of the infusion needle. If signs or symptoms of extravasation occur, the injection or infusion should be terminated immediately and restarted in another vein (see Section 4.2 Dose and Method of Administration).
Phlebosclerosis may result from an injection into a small vessel or from previous injections into the same vein.
Immunosuppressant effects/ increased susceptibility to infections. Administration of live or live attenuated vaccines in patients immunocompromised by chemotherapeutic agents including idarubicin may result in serious or fatal infections. Vaccination with a live vaccine should be avoided in patients receiving idarubicin. Killed or inactivated vaccines may be administered; however, the response to such vaccines may be diminished.
Embryo-fetal toxicity. Idarubicin can cause genotoxicity. An effective method of contraception is required for both male and female patients during and for a period after treatment with idarubicin. Patients desiring to have children after completion of therapy should be advised to obtain genetic counselling if appropriate and available (see Section 4.6 Fertility, Pregnancy and Lactation; Section 5.3 Preclinical Safety Data).
Other. Thrombophlebitis and thromboembolic phenomena, including pulmonary embolism, have been coincidentally reported with the use of idarubicin. The risk of thrombophlebitis at the injection site may be minimised by following the recommended procedure for administration.
Use in the elderly. No data available.
Paediatric use. In infants and children there appears to be a greater susceptibility to anthracycline induced cardiac toxicity, and a long-term periodic evaluation of cardiac function has to be performed.
Effects on laboratory tests. No data available.
4.5 Interactions with Other Medicines and Other Forms of Interactions
Zavedos is a potent myelosuppressant, and combination chemotherapy regimens which contain other agents having a similar action may be expected to lead to additive myelosuppressive effects, especially with regard to bone marrow/ haematologic and gastrointestinal effects (see Section 4.4 Special Warnings and Precautions for Use).
The use of idarubicin in combination chemotherapy with other potentially cardiotoxic drugs, as well as the concomitant use of other cardioactive compounds (e.g. calcium channel blockers), requires monitoring of cardiac function throughout treatment (see Section 4.4 Special Warnings and Precautions for Use).
Changes in hepatic or renal function induced by concomitant therapies may affect idarubicin metabolism, pharmacokinetics and therapeutic efficacy and/or toxicity (see Section 4.4 Special Warnings and Precautions for Use).
An additive myelosuppressant effect may occur when radiotherapy is given concomitantly or within 2-3 weeks prior to treatment with idarubicin.
4.6 Fertility, Pregnancy and Lactation
Effects on fertility. Idarubicin can induce chromosomal damage in human spermatozoa. For this reason, males undergoing treatment with idarubicin should use effective contraceptive methods. Both men and women should seek advice on fertility preservation before treatment.
Use in pregnancy. (Category D)
Zavedos should not be used during pregnancy (see Section 4.3 Contraindications).
There is no information as to whether idarubicin adversely affects fertility or causes teratogenesis in humans. However, it is teratogenic and embryotoxic in rats at intravenous doses of 0.7-1.4 mg/m2/day. In rabbits, no evidence of teratogenicity was seen at the highest dose tested (2.2 mg/m2/day or one-fifth of the human intravenous dose), which caused some maternal deaths. If the patient becomes pregnant during therapy, the patient should be informed of the potential hazard to the fetus.
Women of childbearing potential/contraception in males and females. Women of childbearing potential should be advised to avoid becoming pregnant during treatment. Women of childbearing potential should be advised to use effective contraception during treatment with idarubicin and for at least 6.5 months after the last dose. Men with female partners of childbearing potential should be advised to use effective contraception during treatment with idarubicin and for at least 3.5 months after the last dose.
Use in lactation. It is not known whether idarubicin or its metabolites are excreted in human milk. Because many drugs, including other anthracyclines, are excreted in human milk and because of the potential for serious adverse reactions in nursing infants from idarubicin, advise lactating women not to breastfeed during treatment with idarubicin and for at least 14 days after last dose.
4.7 Effects on Ability to Drive and Use Machines
The effect of idarubicin on the ability to drive or use machinery has not been systematically evaluated. Special care should be taken if it is essential that patients drive or operate machinery while undergoing treatment with Zavedos, especially if in a debilitated condition.
4.8 Adverse Effects (Undesirable Effects)
Severe myelosuppression and cardiac toxicity are the two major adverse effects. Most side effects are dose dependent, e.g. bone marrow depression and cardiotoxicity. All side effects except cardiomyopathy are reversible.
Adverse reactions that occur more frequently than 1% include:
Infections and infestations. Infection, sepsis/septicaemia.
Neoplasms benign, malignant and unspecified. Secondary leukemias (acute myeloid leukaemia and myelodysplastic syndrome).
Immune system disorders. Anaphylaxis.
Blood and lymphatic system disorders. Anaemia, leucopenia, neutropenia, thrombocytopenia and bone marrow depression.
Gastrointestinal disorders. Abdominal pain or burning sensation, acute nausea and vomiting, mucositis/stomatitis, oesophagitis, diarrhoea, burning sensation, erosions/ulceration, gastrointestinal tract bleeding, colitis (including severe enterocolitis/neutropenic enterocolitis with perforation).
Skin and subcutaneous tissue disorders. Alopecia, skin rash/itch, acral erythema, alopecia, hypersensitivity of irradiated skin ('radiation recall reaction'), local toxicity, skin changes, skin and nail hyperpigmentation, urticaria.
Renal disorders. Idarubicin may impart a red colour to the urine for 1-2 days after administration and patients should be advised that this is no cause for alarm.
Cardiac disorders. Cardiomyopathy, sinus tachycardia, tachyarrhythmias, atrioventricular and bundle branch block, subacute effects such as pericarditis/myocarditis.
Vascular disorders. Phlebitis, thrombophlebitis, thromboembolism, vasomotor instability (hot flushes), haemorrhage, shock.
Metabolism and nutrition disorders. Anorexia, dehydration, hyperuricaemia.
General disorders and administration site conditions. Fever, chills.
Investigations. Asymptomatic reductions in left ventricular ejection fraction, ECG abnormalities, elevation of liver enzymes and bilirubin.
Description of selected adverse events. Myelosuppression. Haematological toxicity occurs in all patients receiving therapeutic doses of Zavedos and severe myelosuppression is the major toxicity associated with Zavedos therapy. Leucopenia is usually severe, with neutrophils as the white blood cell most significantly affected; thrombocytopenia and anaemia may also occur. During the period of myelosuppression, patients are at the risk of developing infection and bleeding which may be life-threatening or fatal.
Leucocyte and platelet nadirs are usually reached 10 to 14 days following administration of the drug, however cell counts generally return to normal levels during the third week.
Clinical consequences of bone marrow/ haematological toxicity may be fever, infections, sepsis/ septicaemia, septic shock, haemorrhages, tissue hypoxia or death. Intravenous antibiotics should be given in the presence of febrile neutropenia.
Gastrointestinal disorders. Nausea and/or vomiting, mucositis (usually involving the oral mucosa and appearing 3-10 days after starting treatment), abdominal pain or burning sensation, diarrhoea and oesophagitis may occur but severe (WHO grade 4) gastrointestinal toxicity is reported in less than 5% of patients.
Severe vomiting and diarrhoea may cause dehydration. Nausea and vomiting may be prevented or alleviated by the administration of appropriate antiemetic therapy.
Severe enterocolitis (neutropenic enterocolitis) with perforation has been reported. The possibility of perforation should be considered in patients who develop severe abdominal pain and appropriate steps for diagnosis and management should be taken.
Skin and subcutaneous tissue disorders. Alopecia is reported frequently and dermatological reactions including rash/ itch, urticaria and a bullous erythrodermatous rash of the palms and soles can occur. The dermatological reactions are usually attributable to concomitant antibiotic therapy, skin changes, skin and nail hyperpigmentation, hypersensitivity of irradiated skin ('radiation recall reaction'), acral erythema, local toxicity and local reactions including hives at the injection site have been reported.
Cardiac disorders. As in the case of other anthracyclines, cardiac toxicity, as manifested by congestive heart failure (frequently attributed to fluid overload), serious life threatening arrhythmias including atrial fibrillation, chest pain, myocardial infarction and asymptomatic declines in LVEF have been reported in patients undergoing induction therapy for AML (see Section 4.4 Special Warnings and Precautions for Use). Myocardial insufficiency and arrhythmias are usually reversible and occur in the setting of sepsis, anaemia and aggressive intravenous fluid administration. The events were reported more frequently in patients over age 60 years and in those with pre-existing cardiac disease. Serious cardiac impairment may be prevented through regular surveillance during the course of treatment (see Section 4.4 Special Warnings and Precautions for Use). Subacute effects, such as pericarditis/ myocarditis, have also been reported.
Hepatic and renal disorders. Changes in hepatic and renal function tests are severe (grade 4) in less than 5% of patients, are usually transient and occur in the setting of sepsis and while patients are receiving potentially hepatotoxic and nephrotoxic antibiotics and antifungal agents.
Reporting suspected adverse effects. Reporting suspected adverse reactions after registration of the medicinal product is important. It allows continued monitoring of the benefit-risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions at www.tga.gov.au/reporting-problems.
4.9 Overdose
Very high doses of idarubicin may be expected to cause acute myocardial toxicity within 24 hours and severe myelosuppression within one or two weeks. Delayed cardiac failure has been seen with the anthracyclines up to several months after an overdose.
Two cases of fatal overdosage in patients receiving therapy for AML have been reported. The doses were 135 mg/m2 over 3 days and 45 mg/m2 of idarubicin and 90 mg/m2 of daunorubicin over a 3 day period.
There is no known antidote to Zavedos. Treatment should aim to support the patient and should utilise such measures as blood transfusions, reverse barrier nursing, antibiotics and symptomatic treatment of mucositis. Patients should be observed carefully and if signs of cardiac failure arise, should be treated along conventional lines.
Disposition studies with idarubicin in patients with severe renal failure or in those undergoing dialysis have not been carried out. The profound multicompartment behaviour, extensive extravascular distribution and tissue binding, coupled with the low unbound fraction available in the plasma pool, make it unlikely that therapeutic efficacy or toxicity would be altered by conventional peritoneal haemodialysis.
For information on the management of overdose, contact the Poisons Information Centre on 13 11 26 (Australia).
5 Pharmacological Properties
5.1 Pharmacodynamic Properties
Zavedos is a semi synthetic antineoplastic anthracycline for intravenous use.
Mechanism of action. Idarubicin is a cytotoxic agent. It is a DNA intercalating agent which reacts with topoisomerase II and has an inhibitory effect on nucleic acid synthesis. The compound has a high lipophilicity which results in an increased rate of cellular uptake compared with doxorubicin and daunorubicin.
Pharmacodynamic effects. Idarubicin has been shown to have a higher potency with respect to daunorubicin and to be an effective agent against murine leukaemia and lymphomas. Studies in vitro on human and murine anthracycline resistant cells have shown a lower degree of cross resistance for idarubicin compared with doxorubicin and daunorubicin. Cardiotoxicity studies in animals have indicated that idarubicin has a better therapeutic index than daunorubicin and doxorubicin. The main metabolite, idarubicinol, has shown antitumour activities in experimental models both in vitro and in vivo. In the rat, idarubicinol administered at the same doses as the parent drug is less cardiotoxic than idarubicin.
Clinical trials. No data available.
5.2 Pharmacokinetic Properties
Intravenous. After intravenous administration of idarubicin, there is triphasic disposition in plasma. Estimates of the plasma half-life for the parent compound range from 10 to 35 hours. Idarubicin is extensively metabolised to an active metabolite, idarubicinol, which has a plasma half-life ranging from 41 to 69 hours.
The plasma clearance is higher than the expected hepatic plasma flow, indicating extensive extrahepatic metabolism. Protein binding in plasma is 97% for idarubicin and 94% for idarubicinol. For both compounds, the binding is concentration independent.
Peak cellular idarubicin concentrations are reached a few minutes after injection. Idarubicin and idarubicinol concentrations in nucleated blood and bone marrow cells are more than a hundred times the plasma concentrations. Idarubicin elimination half-life in cells is about 15 hours and is similar to that in plasma. The elimination half-life for idarubicinol in cells is 72 hours.
Excretion takes place via the liver and kidneys, mainly in the form of idarubicinol. After intravenous administration of 13 mg/m2 14C-idarubicin, 33% of the dose was excreted in urine and 39% in faeces after 14 days. Idarubicin excreted unchanged in urine accounts for 2-7% of the dose, and idarubicinol, 9-13%. In a patient with percutaneous biliary drainage, 17% of the dose was eliminated through the bile (as idarubicin plus idarubicinol) over five days.
Special populations. Renal impairment. Only limited information is available regarding the effect of an impaired renal function on the pharmacokinetics of idarubicin. A significant correlation is reported between the plasma clearance of idarubicin after intravenous dosing and creatinine clearance. In a study comparing patients with creatinine clearance < 60 mL/min and those with normal creatinine clearance, idarubicin AUC was increased on average by 38% and idarubicinol AUC by 120% in the patients with reduced creatinine clearance; however, there was considerable variability.
Hepatic impairment. There is also limited information on the effect of impaired liver function on the pharmacokinetics of idarubicin. In a study comparing patients with liver metastases and mild liver impairment and those with normal liver function, there were no significant differences in idarubicin and idarubicinol pharmacokinetic parameters. However, in a patient with severe liver impairment, elimination of idarubicin was significantly delayed, the plasma elimination half-life being 112 hours.
5.3 Preclinical Safety Data
Genotoxicity. Idarubicin was genotoxic in most of the in vitro or in vivo tests performed. Idarubicin was mutagenic in vitro in reverse mutation assays with Salmonella typhimurium and Saccharomyces cerevisiae D4. In forward mutation assays in vitro, idarubicin was mutagenic in Chinese hamster V79 cells but not in Schizosaccharomyces pombe P1, either in vitro or ex vivo. Idarubicin was clastogenic in human lymphocytes and induced unscheduled DNA synthesis in rat hepatocytes in vitro and was clastogenic in the mouse micronucleus test in vivo.
Carcinogenicity. Long-term carcinogenicity studies have not been conducted with idarubicin, but like most other cytotoxic agents, idarubicin has mutagenic properties and is carcinogenic in rats. In male dogs, testicular atrophy with inhibition of spermatogenesis and sperm maturation was observed at threshold idarubicin doses 1.8 mg/m2 administered intravenously or 3 mg/m2 administered orally (3 days/week for 13 weeks). These effects were not readily reversible after an eight week recovery period.
6 Pharmaceutical Particulars
6.1 List of Excipients
Glycerol, hydrochloric acid for adjustment to pH 3.5, water for injections.
6.2 Incompatibilities
Zavedos is not to be mixed with heparin since this causes precipitation, not to be mixed with alkaline solutions, since this causes rapid degradation of Zavedos, and it is not recommended that it be mixed with other drugs.
6.3 Shelf Life
In Australia, information on the shelf life can be found on the public summary of the Australian Register of Therapeutic Goods (ARTG). The expiry date can be found on the packaging.
6.4 Special Precautions for Storage
Store at 2°C to 8°C. Refrigerate. Do not freeze. Protect from light.
6.5 Nature and Contents of Container
Zavedos solution for injection is supplied in single use only, polypropylene and Type I glass vials.
Not all presentations may be marketed.
6.6 Special Precautions for Disposal
All items used for administration or cleaning, including gloves should be placed in high-risk, waste disposal bags for high temperature incineration.
In Australia, any unused medicine or waste material should be disposed of by taking to your local pharmacy.
6.7 Physicochemical Properties
Idarubicin hydrochloride is an odourless red-orange powder, slightly soluble in water, with a melting point of 173°C - 174°C. The molecular formula is C26H27NO9.HCl and the molecular weight is 533.95.
Chemical structure.
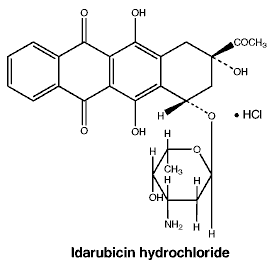
CAS number. 57852-57-0.
7 Medicine Schedule (Poisons Standard)
S4, Prescription Only Medicine.
Date of First Approval
19 August 1999
Date of Revision
26 July 2023
Summary Table of Changes

Reasonable care is taken to provide accurate information at the time of creation. This information is not intended as a substitute for medical advice and should not be exclusively relied on to manage or diagnose a medical condition. The Australian Commission on Safety and Quality in Health Care disclaims all liability (including for negligence) for any loss, damage, injury or any other negative effects resulting from reliance on or use of this information. Read our full disclaimer. This website uses cookies. Read our privacy policy.