Chronic obstructive pulmonary disease (COPD) hub
By creating evidence-based guidance and considering the real experiences of people and health professionals, we’re able to provide better care for chronic obstructive pulmonary disease.
Developed as part of our Better Care Everywhere initiative, this hub supports clinicians and health service organisations to provide best practice care in the treatment of COPD to help improve health outcomes and quality of life for people living with the disease.
COPD is a progressive and debilitating respiratory condition. It is a leading cause of death in Australia and is associated with significant costs to the healthcare system. In 2020–21, an estimated $832 million was spent on COPD, and in 2023, it accounted for 50% of the total disease burden of respiratory conditions in Australia.
COPD can be life limiting and is characterised by chronic obstruction of airflow to the lung that interferes with normal breathing. COPD is not fully reversible.
Our Better Care Everywhere hubs outline what appropriate care looks like across priority clinical topics. In each hub you will find a mix of:
- best practice information on the condition, treatment or procedure
- insights on where and why care may vary from evidence-based practice.
Each hub also includes a practical toolkit to support clinicians and health service organisations address the drivers of low-value care to deliver sustainable, high-quality care.
Other hubs include:
Learn more about the Better Care Everywhere initiative and the six evidence-based actions that underpin the toolkits.
Best practice quick links
Better care, faster: Use our quick links for fast access to evidence-based guidance, factsheets and the latest news in the treatment of COPD. For the full suite of resources supporting better care in the treatment of COPD access our toolkit.
Clinical Care Standard

Fact sheet

Success story
A two-pronged solution for COPD testing
Two clinical champions coming at a problem from different perspectives have led to a local solution addressing the low rates of spirometry testing for diagnosing COPD in Western Australia.
Variation focus area: spirometry
Improve consistency in care: Take action to deliver better outcomes by understanding where care differs from best practice and learn about targeted steps to reduce unwarranted clinical variation in the treatment of COPD.
Spirometry for people 35 years and over, between 2015–16 and 2022–23
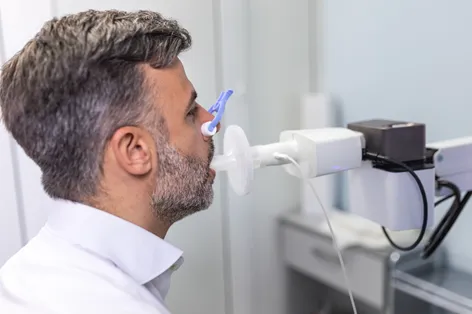
Spirometry is a breathing test that is essential for the accurate diagnosis and appropriate management of COPD. It helps to differentiate COPD from other lung diseases with similar symptoms, such as asthma, which is important for guiding treatment.
Despite the test being the gold standard for diagnosis of COPD, the Atlas Focus Report: COPD reported a 31% drop nationally in MBS-subsidised spirometry testing rates between 2015-16 and 2022-23. Without spirometry, patients are at risk of misdiagnosis and being prescribed medications that put them at unnecessary risk of pharmacological treatment they don’t need. The Atlas findings highlight an opportunity for improving early and accurate diagnosis, which is essential to ensure people receive the right treatment at the right time.
10-fold difference
between the local area with the highest rate & the local area with the lowest rate of spirometry in 2022-23
Why rates vary
- Barriers to provision in primary care such as cost of the machine, consumables and staff; low awareness of clinical benefit; lack of time; reduced level of interpretation skills.
- Limited access to laboratory testing including lack of spirometry in primary care or a reasonable referral option.
- Patient factors such as cost, lack of time, being unwell, difficulty travelling to other location if not in GP’s rooms.
- COVID and other infectious diseases may have contributed to ongoing concerns about potential spread of infectious diseases through spirometry.
What more can be done?
General Practitioners
- Use spirometry to confirm suspected diagnosis of COPD.
- Know where to refer patients locally for spirometry, if not available on-site.
- See Information for clinicians – COPD Clinical Care Standard for more details.
- Or refer to the Better Care Everywhere Toolkit: COPD below for tools and resources that support best practice for COPD care.
TIP
GP practices can sign up to MedicineInsight Practice Reports to receive customised reports to help you compare your data with the best care and results at a local, regional and national level.
Health Departments and Primary Health Networks
- Review spirometry remuneration payments and models of care.
- Support respiratory diagnostic hubs and outreach services for people with chronic lung symptoms and/or risk factors for chronic respiratory disease, targeting areas and populations with a high burden of COPD.
- Introduce a GP Practice Incentives Program (PIP) Quality Improvement (QI) Incentive initiative for spirometry.
- Provide GP and patient education programs about the need for spirometry.
- See the Atlas Focus Report: COPD for more details.
- Refer to the Better Care Everywhere Toolkit below for tools and resources that support best practice for COPD care.
Patients
- A breathing test called ‘spirometry’ is the only way to find out if you have COPD. You should have spirometry if you are over 35 years of age and:
- have one or more risk factors for COPD and symptoms of the disease
- have been told that you have COPD but have not had spirometry, even if you have been in hospital because of COPD symptoms.
- See Information for consumers – COPD Clinical Care Standard for more details.
- Click the Decisions tab in the Better Care Everywhere Toolkit below for more resources to help you talk with your doctor about the most suitable COPD care for you.
Better Care Everywhere Toolkit: COPD
This toolkit includes resources to help improve the treatment of COPD and is designed for health professionals and health service organisations. Resources are organised into six evidence-based actions that address unwarranted clinical variation.
Focus on one strategy to start, or use all six to deliver safer, more consistent and sustainable health care.
Learn more about the six evidenced-based actions in the Better Care Everywhere Toolkit and their role in addressing unwarranted clinical variation.
Better Systems
Better Systems
Better systems refer to the combination of culture, systems and processes that health service organisations need to have to deliver care that is consistently high-quality and improving.
Best practice systems provide the right environment for a clear, system-wide approach to minimise unwarranted clinical variation and the potential for low-value care.
Appropriate clinical governance systems ensure that everyone knows what best-practice looks like, that systems are set up to measure when care varies from best practice and staff are supported to act when care varies more than it should or for the wrong reasons.
Guidance, tools and resources
National Model for Clinical Governance
A national model which identified six foundations of clinical governance that when combined underpin an organisational approach to delivering consistently high-quality and improving care.
- Use to: Establish the systems needed to consistently identify and act to address unwarranted clinical variation.
- Useful for: Boards and Chief Executive Officers of health service organisations.
National Safety and Quality Health Service (NSQHS Standards)
The Standards provide a nationally consistent statement of the level of care consumers can expect from health service organisations.
- Use to: Set the standard of care that patients should expect from your acute care health service. Action 1.27 and 1.28 ensures health service organisations use evidence-based guidance and measure when care varies from this standard.
- Useful for: All professionals (health and non-health) involved in the delivery of acute care services.
Healthcare Sustainability and Resilience Module
The Module provides a framework of actions for health service organisations to integrate environmental sustainability and climate resilience strategies to deliver high-quality care.
- Use to: Support the development of adaptation and mitigation strategies for climate and environmental risk. Action 2b includes reviewing clinical practice to identify and address healthcare variation and unnecessary use of resources.
- Useful for: Sustainability Managers, Safety and Quality Managers.
User Guide for Reviewing Clinical Variation
This User Guide presents a six-step approach to the review of clinical variation data, and case studies that put those steps into action.
- Use to: Support implementation of Action 1.28 of the NSQHS Standards.
- Useful for: health service organisations, Safety and Quality Managers.
Better Insights
Better Insights
Better insights refer to the meaningful use of data to improve the care for people with COPD.
Using data to understand where the care of COPD differs from best practice is critical to improving the diagnosis and management of the condition in Australia.
You can use the data in our report to:
- Prompt reflection and review your individual or your practice’s results in comparison to national, state and local area trends.
- Identify key areas for improvement to benefit patients.
- Develop COPD-focussed quality improvement activities that are meaningful to you and your patients.
Guidance, tools and resources
Atlas Focus Report: COPD
Interactive maps and graphs show national trends and geographical variation in the treatment of COPD.
- Use to: View rates of spirometry and prescribing patterns in your local area and reflect on what it means for your practice and patients.
- Useful for: policy makers, Primary Health Networks, Safety and Quality Managers, Quality Improvement Managers, sustainability specialists.
MedicineInsight GP Snapshot: COPD
A primary care quality improvement program providing insights to participating GP practices on their own diagnosis and prescribing patterns.
- Use to: Access insights on how health technologies, medicines and tests are used in your practice. These insights can inform quality improvement measures for routine clinical practice and health outcomes for patients.
- Useful for: General Practice Managers, General Practitioners.
MedicineInsight Practice Reports: COPD
Personalised reports that provide confidential information designed for individual practices and general practitioners that are participating in the MedicineInsight program.
- Use for: Providing feedback on pharmacological management to support clinical reflective activities and can contribute to Continuing Professional Development requirements and quality improvement.
- Useful for: General Practitioners.
Practice Reflections: COPD
Personalised reports distributed directly to Australian GPs providing confidential information on their spirometry referral practices.
- Use to: Aid clinician-initiated professional development, self-reported CPD activity.
- Useful for: General Practitioners.
Highlights Report: COPD
This six-page report outlines key findings and recommended actions from the Atlas Focus Report: COPD.
- Use to: View a summary of key findings from the report.
- Useful for: policy makers, Primary Health Networks, Safety and Quality Managers, Quality Improvement Managers, sustainability specialists.
Better Practice
Better Practice
Better practice in the care of COPD involves providing care that is patient-centred, safe, effective, accessible and integrated.
Better clinical practice can address unwarranted clinical variation by ensuring care is delivered in line with evidence-based guidance on the treatment of COPD.
Guidance, tools and resources
COPD Clinical Care Standard
Provides guidance to clinicians and health service organisations on managing COPD.
- Use to: Improve the quality of care for people with COPD using the ten quality statements.
- Useful for: clinicians, health service organisations.
Safe use of spirometry in primary healthcare settings
This factsheet includes practical strategies to help reduce the risk of infection transmission during spirometry testing.
- Use to: Guide the appropriate use of spirometry in primary healthcare settings.
- Useful for: clinicians, health service organisations.
Documenting oxygen therapy and response for safety
This factsheet provides guidance for health service organisations and clinicians on processes to support appropriate documentation around the administration, and monitoring of oxygen therapy for adults in acute healthcare settings.
- Use to: Guide processes to support appropriate documentation around the administration, and monitoring of oxygen therapy for adults in acute healthcare settings.
- Useful for: clinicians, health service organisations.
Better Decisions
Better Decisions
Better decisions involve making choices that are patient-centred and considers individual values, preferences and circumstances. It involves engaging in shared decision-making, where clinicians and patients work together to provide care that best meets the patient’s needs and goals.
Better shared decision-making can address unwarranted clinical variation by making information available to patients about the range of treatment options and ensuring that patients consider the risks and benefits of each treatment, enabling them to make an informed choice about their care.
Guidance, tools and resources
Ask Share Know
A practical guide that will help consumers make shared decisions with their health professionals.
- Use to: Help improve your conversation with your health professional when asking about tests, treatment and care options. This can help you to make the treatment decision that is right for you.
- Useful for: patients, carers.
Better Monitoring
Better Monitoring
Better monitoring means continually measuring and refining quality improvement activities to reduce unwarranted clinical variation.
Measurement is fundamental to providing better care, as meaningful indicators are required to assess the effectiveness of quality improvement initiatives and guide decision-making. By routinely measuring how care is delivered and where it differs, we can see where clinical variation is occurring, but identification of variation is only the first step, further investigation and action at a local level is essential to make sure data on healthcare variation leads to better care.
Guidance, tools and resources
COPD Clinical Care Standard Indicators
A set of ten indicators to support monitoring of the care recommended in the Standard.
- Use to: monitor how health service organisations are implementing the care recommended in the COPD Clinical Care Standard.
- Useful for: health service organisations, Safety and Quality Managers, Hospital Managers, General Practitioners.
MedicineInsight CPD Guide: COPD 2025
A Quality Improvement Guide accompanying the MedicineInsight Practice Report: COPD 2025.
- Use to: Align COPD-focused quality improvement activities with best practice and identify key areas for improvement, benefiting patients. This activity can contribute to CPD requirements for participating GPs.
- Useful for: General Practitioners
Better Networks
Better Networks
Better networks mean bringing people together with common interests and goals to learn, share and support efforts to reduce unwarranted clinical variation. Through these networks, clinicians can collaborate and apply shared learnings to promote stewardship of resources and reduce duplication of work.
Networks can address unwarranted clinical variation by providing a platform for sharing evidence, experiences and best practice. This supports the standardisation of care and ensures patients receive consistent and high-quality care regardless of where they are being treated.
Communities of Practice/Networks
Pulmonary Rehabilitation network
- Use to: A forum for sharing ideas and providing peer support to new and developing programs and promote improved access to pulmonary rehabilitation across Australia.
- Useful for: clinicians
Australia and New Zealand Lung Cancer Nurses Forum (ANZ-LCNF)
- Use to: Bring nurses with a common focus on improving care and outcomes for patients with lung cancer together.
- Useful for: nurses