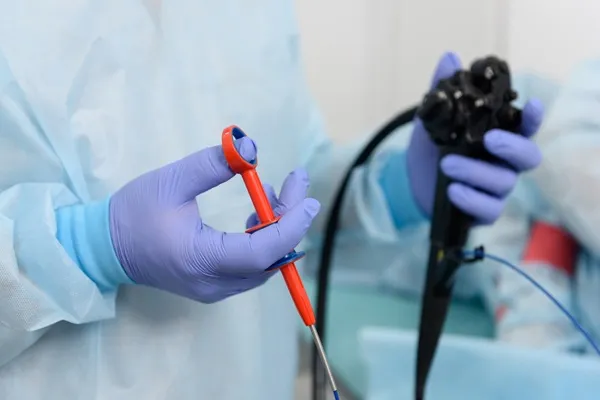
Heavy menstrual bleeding hub
Access to effective, minimally invasive treatments where appropriate, is essential to providing better care for women with heavy menstrual bleeding.
Developed as part of our Better Care Everywhere initiative, this hub supports clinicians and health service organisations to improve care for women with heavy menstrual bleeding, to ensure they are offered the least invasive and most effective treatment for their clinical needs and can make an informed choice from the range of treatments.
Heavy menstrual bleeding can have a debilitating impact on women, affecting their physical, social, emotional and economic wellbeing. Often women are unaware of the range of options for treating their heavy menstrual bleeding, and that very effective treatments can be provided by their general practitioner.
To improve patient outcomes in the treatment of benign causes of heavy menstrual bleeding, women should be offered the least invasive and most effective treatment options appropriate to their clinical needs and preferences, and be able to make an informed choice from a range of treatments suitable to their individual situation.
Our Better Care Everywhere hubs outline what appropriate care looks like across priority clinical topics. In each hub you will find a mix of:
- best practice information on the condition, treatment or procedure
- insights on where and why care may vary from evidence-based practice.
Each hub also includes a practical toolkit to support clinicians and health service organisations address the drivers of low-value care to deliver sustainable, high-quality care.
Other hubs include:
Learn more about the Better Care Everywhere initiative and the six evidence-based actions that underpin the toolkits.
1 in 4 women
of reproductive age affected
Around 50%
of women do not seek medical care
Over 60%
are iron deficient
Best practice quick links
Clinical Care Standard
Fact sheet

Success story

Atlas report prompts focus on treatment of heavy menstrual bleeding locally
Findings in the Australian Atlas of Healthcare Variation series prompted Ballarat gynaecologist Dr Natasha Frawley to review the use of hysterectomy to treat heavy menstrual bleeding at the local hospital.
Variation focus area: hysterectomy
Hysterectomy, for women 15 years and over, between 2014-15 and 2021-22
Hysterectomy is one treatment option for heavy menstrual bleeding, but it is a more invasive approach that involves major surgery and a number of associated risks. The Atlas Focus Report: Heavy Menstrual Bleeding shows a 20% decrease in the rate of hysterectomy since 2014-15, when it was first reported in the Second Australian Atlas of Healthcare Variation (2017). In response to these findings, the Heavy Menstrual Bleeding Clinical Care Standard was first released in 2017 and updated in 2024. While a reduction in hysterectomy rates is encouraging, rates in Australia remain significantly higher than for similar countries like New Zealand and the United Kingdom.
The data also show a rural-urban disparity, with hysterectomy rates higher in regional areas than major cities and remote areas, indicating that potentially less invasive treatments for heavy menstrual bleeding are not being consistently accessed across Australia.
5-fold difference
between the local area with the highest rate of hysterectomy and the local area with the lowest rate in 2021-22
Why rates vary
- Differences in awareness of the range of treatment options
- Treatment costs
- Limited availability of services, such as quality ultrasound, IUD insertion and relevant specialist care
- Limited availability of clinicians with knowledge, skills, equipment and capacity to deliver hysterectomy alternatives
- Limited availability of culturally safe care for First Nations women
- Compounded effects for women in rural and remote areas related to availability of care, isolation and cost.
What more can be done?
- Help women to feel comfortable talking about menstrual issues, a sensitive topic for many.
- Ask women about their menstrual health – to help identify if bleeding is unusual and can be treated.
- Learn more about alternative treatments to hysterectomy, and how to access them.
- Inform women about their treatment options, and the risks and benefits to them.
- Use data in the Atlas Focus Report to view hysterectomy and endometrial ablation rates in your area and reflect on what it means for your practice and patients.
- Refer to the Better Care Everywhere Toolkit: Heavy menstrual bleeding below for tools and resources that support best practice for the treatment of heavy menstrual bleeding.
- Use the interactive Atlas Focus Report to view hysterectomy and endometrial ablation rates in your area. When substantial variation exists, investigate whether appropriate care is being delivered.
- Implement the Heavy Menstrual Bleeding Clinical Care Standard and use its indicators to support local quality improvement.
- Build appropriate skills such as hormonal IUD insertion in primary care.
- Establish referral pathways for treatments such as hormonal IUD, endometrial ablation and uterine artery embolisation.
- Make information available to patients about the range of treatment options.
- Check local guidance is consistent with the Heavy Menstrual Bleeding Clinical Care Standard (see our HealthPathways checklist).
- Act to improve cultural safety and provide culturally appropriate models of care to suit local needs.
- Refer to the Better Care Everywhere Toolkit: Heavy menstrual bleeding below for tools and resources that support best practice for the treatment of heavy menstrual bleeding.
- Talk to your healthcare provider if you have heavy periods, to understand what is normal.
- If you are worried, ask your doctor to assess what could be causing your heavy menstrual bleeding.
- Ask your doctor or other healthcare provider about treatments that may be suitable for you.
- Request a referral to a specialist if you are considering surgical or other procedures.
- Consider the risks and benefits of treatments to make an informed choice about your preferred option.
- Click the Decisions tab in the Better Care Everywhere Toolkit: Heavy menstrual bleeding below for more resources to help you talk with your doctor about the most suitable treatment for you.
Better Care Everywhere Toolkit: Heavy menstrual bleeding
This toolkit includes resources to help improve the treatment of heavy menstrual bleeding and is designed for health professionals and health service organisations. Resources are organised into six evidence-based actions that address unwarranted clinical variation.
Focus on one strategy to start, or use all six to deliver safer, more consistent and sustainable health care.
Learn more about the six evidenced-based actions in the Better Care Everywhere Toolkit and their role in addressing unwarranted clinical variation.
Better Systems
Better Systems
Better systems refer to the combination of culture, systems and processes that health service organisations need to have to deliver care that is consistently high-quality and improving.
Best practice systems provide the right environment for a clear, system-wide approach to minimise unwarranted clinical variation and the potential for low-value care.
Appropriate clinical governance systems ensure that everyone knows what best-practice looks like, that systems are set up to measure when care varies from best practice and staff are supported to act when care varies more than it should or for the wrong reasons.
Guidance, tools and resources
National Model for Clinical Governance
A national model which identified six foundations of clinical governance that when combined underpin an organisational approach to delivering consistently high-quality and improving care.
- Use to: Establish the systems needed to consistently identify and act to address unwarranted clinical variation.
- Useful for: Boards and Chief Executive Officers of health service organisations.
National Safety and Quality Primary and Community Healthcare Standards
The National Safety and Quality Primary and Community Healthcare Standards aim to protect the public from harm and improve the quality of health care delivered.
- Use to: Describe the processes and structures that are needed to deliver safe and high-quality health care in primary and community settings.
- Useful for: All professionals (health and non-health) involved in the delivery of primary and community services.
National Safety and Quality Health Service (NSQHS Standards)
The Standards provide a nationally consistent statement of the level of care consumers can expect from health service organisations.
- Use to: Set the standard of care that patients should expect from your acute care health service. Action 1.27 and 1.28 ensures health service organisations use evidence-based guidance and measure when care varies from this standard.
- Useful for: All professionals (health and non-health) involved in the delivery of acute care services.
Healthcare Sustainability and Resilience Module
The Module provides a framework of actions for health service organisations to integrate environmental sustainability and climate resilience strategies to deliver high-quality care.
- Use to: Support the development of adaptation and mitigation strategies for climate and environmental risk. Action 2b includes reviewing clinical practice to identify and address healthcare variation and unnecessary use of resources.
- Useful for: Sustainability Managers, Safety and Quality Managers.
User Guide for Reviewing Clinical Variation
This User Guide presents a six-step approach to the review of clinical variation data, and case studies that put those steps into action.
- Use to: Support implementation of Action 1.28 of the NSQHS Standards.
- Useful for: health service organisations, Safety and Quality Managers.
Better Insights
Better Insights
Better insights refer to the meaningful use of data to improve the care for women with heavy menstrual bleeding.
Using data to understand where the treatment of heavy menstrual bleeding differs from best practice is critical to improving the diagnosis and management of the condition in Australia.
You can use the data in our report to:
- Prompt reflection and review your individual or your practice’s results in comparison to national, state and local area trends.
- Identify key areas for improvement to benefit patients.
- Develop heavy menstrual bleeding-focussed quality improvement activities that are meaningful to you and your patients.
Guidance, tools and resources
Atlas Focus Report
Interactive maps and graphs show national trends and geographical variation in the more invasive treatment options for heavy menstrual bleeding.
- Use to: View rates of hysterectomy and endometrial ablation in your local area and reflect on what it means for your practice and patients.
- Useful for: policy makers, Primary Health Networks, Safety and Quality Managers, Quality Improvement Managers, sustainability specialists.
Highlights Report
This six-page report outlines key findings and recommended actions from the Atlas Focus Report.
- Use to: View a summary of key findings from the report.
- Useful for: policy makers, Primary Health Networks, Safety and Quality Managers, Quality Improvement Managers, sustainability specialists.
Better Practice
Better Practice
Better practice for the treatment of heavy menstrual bleeding involves providing care that is patient-centred, safe, effective, accessible and integrated.
Consider whether care is consistent with evidence-based guidance for the treatment of heavy menstrual bleeding. This includes offering women with heavy menstrual bleeding the least invasive and most effective treatment appropriate to their clinical needs and preference.
Guidance, tools and resources
Heavy Menstrual Bleeding Clinical Care Standard
Describes high quality care for women with heavy menstrual bleeding, according to evidence-based guidelines.
- Use to: Understand the priority aspects of care for women with heavy menstrual bleeding and enable them to make an informed choice from the range of treatments suitable to their individual situation.
- Useful for: clinicians, healthcare services organisations, patients.
Information for Clinicians – Heavy Menstrual Bleeding CCS
This factsheet provides an explanation of what each of the quality statement means for clinicians and links to resources to support clinicians to implement the care described in the Clinical Care Standard.
- Use to: Improve the quality of care for women with heavy menstrual bleeding and ensure that they can make an informed choice from the range of treatments suitable to their individual situation.
- Useful for: clinicians, health service organisations.
Consumer Guide – Heavy Menstrual Bleeding CCS
This guide explains each of the eight-quality statement listed in the Heavy Menstrual Bleeding Clinical Care Standard.
- Use to: Understand the statements and what it means for patients.
- Useful for: patients, carers.
Better Decisions
Better Decisions
Better decisions involve making choices that are patient-centred and considers individual values, preferences and circumstances. It involves engaging in shared decision-making, where clinicians and patients work together to provide care that best meets the patient’s needs and goals.
Better shared decision-making can address unwarranted clinical variation by making information available to patients about the range of treatment options and ensuring that patients consider the risks and benefits of each treatment, enabling them to make an informed choice about their care.
Guidance, tools and resources
Ask, Share, Know
A practical guide that will help consumers make shared decisions with their health professionals.
- Use to: Help improve your conversation with your health professional when asking about tests, treatment and care options. This can help you to make the treatment decision that is right for you.
- Useful for: patients, carers.
Heavy Menstrual Bleeding – Treatment Options
This fact sheet provides an overview of treatment options for heavy menstrual bleeding.
- Use to: Support discussions between clinicians and women about their treatment options.
- Useful for: patients, carers, clinicians.
Better Monitoring
Better Monitoring
Better monitoring means continually measuring and refining quality improvement activities to reduce unwarranted clinical variation.
Measurement is fundamental to providing better care, as meaningful indicators are required to assess the effectiveness of quality improvement initiatives and guide decision-making. By routinely measuring how care is delivered and where it differs, we can see where clinical variation is occurring, but identification of variation is only the first step, further investigation and action at a local level is essential to make sure data on clinical variation leads to better care.
Guidance, tools and resources
Heavy Menstrual Bleeding CCS indicators
A set of seven indicators to support local monitoring of the care recommended in the Heavy Menstrual Bleeding Clinical Care Standard.
- Use to: monitor how health service organisations are implementing the care recommended in the Heavy Menstrual Bleeding Clinical Care Standard.
- Useful for: health service organisations, Safety and Quality Managers, Hospital Managers.
Better Networks
Better Networks
Better networks mean bringing people together with common interests and goals to learn, share and support efforts to reduce unwarranted clinical variation. Through these networks, clinicians can collaborate and apply shared learnings to promote stewardship of resources and reduce duplication of work.
Networks can address unwarranted clinical variation by providing a platform for sharing evidence, experiences and best practice. This supports the standardisation of care and ensures patients receive consistent and high-quality care regardless of where they are being treated.
Communities of Practice/Networks
Australasian Gynaecological Endoscopy and Surgery (AGES) Society
AGES is an international society of Gynaecologists, providing education and professional engagement opportunities for members.
- Use to: Bring gynaecologists together for educational and networking purposes.
- Useful for: Gynaecologists.
Jean Hailes for Women’s Health
A national not-for-profit organisation dedicated to improving women's health across Australia, through every life stage.
- Use to: Learn about women’s health and access evidence-based information to guide clinical care and self-management.
- Useful for: clinicians, patients and careers.
Case studies
Embedding gynaecologists in primary care improves care for Aboriginal women
Derbarl Yerrigan Health Service in Perth has improved care for Aboriginal women with gynaecological conditions such as heavy menstrual bleeding by establishing a gynaecology clinic that ensures culturally safe care.
Atlas report findings prompt local focus on treatment of heavy menstrual bleeding
Findings in the Australian Atlas of Healthcare Variation series prompted Ballarat gynaecologist Dr Natasha Frawley to review the use of hysterectomy to treat heavy menstrual bleeding at the local hospital.