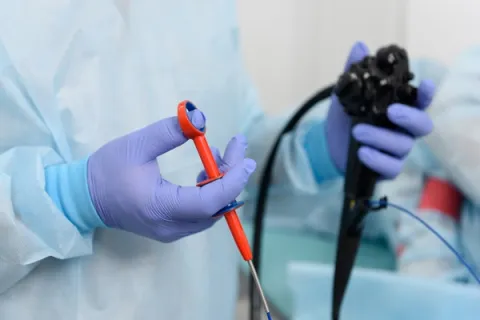
Colonoscopy hub
Ensuring appropriate use of colonoscopy, including performing repeat procedures when recommended, is essential to avoid unnecessary testing and ensure timely access for those who need it most.
Developed as part of our Better Care Everywhere initiative, this hub supports clinicians and health service organisations to improve care for people undergoing colonoscopy, to ensure the procedure is safe and of high quality and only performed when appropriate.
Colonoscopy refers to the examination of the entire large bowel using a colonoscope – a camera on a flexible tube. It is a complex task that requires the colonoscopist to manipulate the colonoscope effectively to visualise the bowel, while performing therapeutic interventions such as removing polyps or taking tissue samples when required.
Colonoscopy is often performed as a diagnostic intervention to investigate possible bowel cancer, either in people with symptoms and signs of bowel disease or those with an increased risk of bowel cancer. It may also be used to help diagnose the cause of symptoms in conditions such as inflammatory bowel disease.
Australia has one of the highest rates of bowel cancer in the world. Evidence-based guidelines describe when colonoscopy should be used and how frequently, according to the patient’s presenting symptoms, history and risk. National MBS-subsided data suggest that while some people are having repeat colonoscopies more often than necessary, others are missing out.
Our Better Care Everywhere hubs outline what appropriate care looks like across priority clinical topics. In each hub you will find a mix of:
- best practice information on the condition, treatment or procedure
- insights on where and why care may vary from evidence-based practice.
Each hub also includes a practical toolkit to support clinicians and health service organisations address the drivers of low-value care to deliver sustainable, high-quality care.
Other hubs include:
Learn more about the Better Care Everywhere initiative and the six evidence-based actions that underpin the toolkits.
Best practice quick links
Clinical Care Standard
Fact sheet

Success story

Strengthening foundations for auditing and oversight in colonoscopy care
The Northern NSW Local Health District redesigned their audit tool and reporting processes to build a stronger and more data-driven system that was supported by clinicians. This not only improved accreditation assessment results but ensured best practice was provided to patients. They were also the recipients of the Commission’s Clinical Care Standards Excellence Award.
Variation focus area: repeat colonoscopy
MBS-subsidised repeat colonoscopy before 3 years, 2013–14 and 2023–24
While some people may only need one colonoscopy to rule out potential bowel disease, others need repeat colonoscopies to monitor the large bowel (colon) for abnormalities, cancer or for the surveillance of chronic conditions. Timing for a repeat colonoscopy will depend on a person’s risk and previous results.
National data from the Atlas Focus Report: Colonoscopy raises concerns about growing inequity of access to colonoscopy based on where a person lives and their socioeconomic status. Overuse of colonoscopy in low-risk patients in some areas may be diverting resources away from where they are needed most, and may contribute to reduced access to colonoscopy for people in rural, remote and socioeconomically disadvantaged areas.
18-fold difference
in the local area with the highest rate compared to the local area with the lowest rate for MBS-subsided repeat colonoscopy before 3 years
Why rates vary
- Performing repeat colonoscopy earlier than guidelines recommend may be due to fear of missing pathology, malpractice concerns and patient and referrer expectations.
- Differences in the proportion of services subsidised by the MBS in each state and territory, which also varied over time.
- Awareness of bowel cancer symptoms and the National Bowel Cancer Screening Program (NBCSP), and participation in screening.
- Limited endoscopist workforce and infrastructure in some regional and remote areas.
What more can be done?
- Locate previous reports and confirm appropriateness of colonoscopy before arranging the procedure.
- Follow the Clinical Care Standard’s guidance for appropriate colonoscopy.
- Align intervals with clinical practice guidelines for surveillance colonoscopy.
- Provide reports to be recorded in the facility records, and upload to My Health Record, to enable accurate follow-up by other clinicians.
- Communicate the reason for the colonoscopy, its findings, all histology results and recommendations for follow-up in writing to the GP, all other relevant clinicians and the patient.
- Follow-up in writing to the person, their primary care provider and other clinicians.
- Refer to the Better Care Everywhere Toolkit: Colonoscopy below for tools and resources that support best practice use of colonoscopy.
- Review implementation of the Colonoscopy Clinical Care Standard, and associated policies and procedures, and monitor progress against the indicators in the Standard – see the Self-Assessment Tool.
- Provide regular education to clinicians about appropriate surveillance intervals.
- Conduct audits of repeat colonoscopy to ensure follow-up intervals align with evidence-based guidelines.
- Ensure systems are in place to allow access to previous colonoscopy and pathology results.
- Consider employing a colonoscopy liaison nurse if volumes of colonoscopy are high.
- Refer to the Better Care Everywhere Toolkit: Colonoscopy below for tools and resources that support best practice use of colonoscopy.
- Participate in the National Bowel Cancer Screening Program at recommended intervals.
- If your doctor recommends a colonoscopy, ask questions so you understand the reason, the risks and the benefits for you.
- Ask your colonoscopist to upload your colonoscopy report to My Health Record
- Reduce your risk factors for bowel cancer with lifestyle changes.
- Click the Decisions tab in the Better Care Everywhere Toolkit: Colonoscopy below for more resources to help you talk with your doctor about your colonoscopy.
- Mandate uploading of colonoscopy reports to My Health Record.
- Require justification of repeat colonoscopy intervals not aligned with guidelines to qualify for payments.
- Refer to the Better Care Everywhere Toolkit: Colonoscopy below for tools and resources that support best practice use of colonoscopy.
- Support trainee gastroenterologist positions in underserved areas, with flexible training models if necessary.
- Support training in colonoscopy for rural generalists, general practitioners and nurses.
- Provide training for clinicians about correct surveillance intervals.
- Promote exchange programs for regional/remote endoscopists with metropolitan colleagues to support the rural workforce.
- Develop decision support tools to support selection of appropriate surveillance intervals.
- Develop decision support tools to explain the absolute risk of bowel cancer at different ages to patients.
- Refer to the Better Care Everywhere Toolkit: Colonoscopy below for tools and resources that support best practice use of colonoscopy.
Better Care Everywhere Toolkit: Colonoscopy
This toolkit includes resources to help improve the use of colonoscopy and is designed for health professionals and health service organisations. Resources are organised into six evidence-based actions that address unwarranted clinical variation.
Focus on one strategy to start, or use all six to deliver safer, more consistent and sustainable health care.
Learn more about the six evidenced-based actions in the Better Care Everywhere Toolkit and their role in addressing unwarranted clinical variation.
Better Systems
Better Systems
Better systems means having the right culture, systems and processes to deliver consistently high-quality and improving care.
Best practice systems provide the right environment for a clear, system-wide approach to minimise unwarranted clinical variation and the potential for low-value care.
Appropriate clinical governance systems ensure that everyone knows what best-practice looks like, that systems are set up to measure when care varies from best practice and staff are supported to act when care varies more than it should or for the wrong reasons.
Guidance, tools and resources
National Model for Clinical Governance
A national model which identified six foundations of clinical governance that when combined underpin an organisational approach to delivering consistently high-quality and improving care.
- Use to: Establish the systems needed to consistently identify and act to address unwarranted clinical variation.
- Useful for: Boards and Chief Executive Officers of health service organisations.
National Safety and Quality Health Service (NSQHS) Standards
The Standards provide a nationally consistent statement of the level of care consumers can expect from health service organisations.
- Use to: Set the standard of care that patients should expect from your acute care health service. Action 1.27 and 1.28 states that health service organisations are required to use evidence-based guidance and measure when care varies from the standard.
- Useful for: All professionals (health and non-health) involved in the delivery of acute care services.
Advisory AS18/12: Implementing the Colonoscopy Clinical Care Standard
Describe assessment requirements for Actions 1.23, 1.24, 1.27b, and 1.28a of the National Safety and Quality Health Service (NSQHS) Standards for health service organisations implementing the Colonoscopy Clinical Care Standard.
- Use to: Better understand the assessment requirements for Actions 1.23, 1.24, 1.27b, and 1.28a of the NSQHS Standards for health service organisations implementing the Colonoscopy Clinical Care Standard.
- Useful for: health service administrators, assessors, colonoscopists, nurses.
Certification and Recertification of practising adult colonoscopists
Certification and re-certification in colonoscopy are mandatory for all practitioners working in health service organisations being assessed to the NSQHS Standards.
- Use to: Learn more about the mandatory requirements for certification and re-certification in adult colonoscopy for all practitioners working in health service organisations being assessed to the NSQHS Standards.
- Useful for: medical and surgical endoscopists, nurse endoscopists.
Healthcare Sustainability and Resilience Module
The Module provides a framework of actions for health service organisations to integrate environmental sustainability and climate resilience strategies to deliver high-quality care.
- Use to: Support the development of adaptation and mitigation strategies for climate and environmental risk. Action 2b includes reviewing clinical practice to identify and address healthcare variation and unnecessary use of resources.
- Useful for: Sustainability Managers, Safety and Quality Managers.
User Guide for Reviewing Clinical Variation
This User Guide presents a six-step approach to the review of clinical variation data, and case studies that put those steps into action.
- Use to: Support implementation of Action 1.28 of the NSQHS Standards.
- Useful for: health service organisations, Safety and Quality Managers.
Better Insights
Better Insights
Better insights refer to the meaningful use of data to improve the appropriate use and timing of colonoscopy for the diagnosis, monitoring and treatment of bowel cancer and other diseases.
Using data to understand where the use of colonoscopy differs from best practice is critical to improving the diagnosis and management of bowel cancer and other diseases in Australia.
You can use the data in our report to:
- Prompt reflection and review your individual or your practice’s results in comparison to national, state and local area trends.
- Identify key areas for improvement to benefit patients.
- Develop colonoscopy-focussed quality improvement activities that are meaningful to you and your patients.
Guidance, tools and resources
Atlas Focus Report: Colonoscopy
Interactive maps and graphs show national trends and geographical variation in the use of colonoscopy.
- Use to: View rates of repeat colonoscopy in your local area and reflect on what it means for your practice and patients.
- Useful for: policy makers, Primary Health Networks, Safety and Quality Managers, Quality improvement Managers, sustainability specialists
Highlights Report
This four-page report outlines key findings and recommended actions from the Atlas Focus Report: Colonoscopy.
- Use to: View a summary of key findings from the report.
- Useful for: colonoscopists, health service organisations, policy makers, clinical societies and colleges.
Better Practice
Better Practice
Better practice involves the appropriate use of colonoscopy in the diagnosis and treatment of bowel cancer.
Better clinical practice can address unwarranted clinical variation by ensuring care is delivered in line with evidence-based guidance.
Guidance, tools and resources
Colonoscopy Clinical Care Standard
Describes the level of care expected for people undergoing a colonoscopy.
- Use to: Improve the quality of care for people receiving a colonoscopy to maximise patient likelihood of benefit while reducing their risk of avoidable harm.
- Useful for: clinicians, health service organisations, patients.
Information for clinicians – Colonoscopy Clinical Care Standard
Guidance for clinicians on the nine quality statements from the Colonoscopy Clinical Care Standard.
- Use to: Ensure the safe and appropriate use of colonoscopy and reduce the risk of avoidable harm.
- Useful for: clinicians.
Information for healthcare services - Colonoscopy Clinical Care Standard
Guidance for healthcare services on the nine quality statements from the Colonoscopy Clinical Care Standard.
- Use to: Ensure the safe and appropriate use of colonoscopy and reduce the risk of avoidable harm.
- Useful for: health service organisations.
Self-Assessment Tool – Colonoscopy Clinical Care Standard
A self-assessment tool used by healthcare services to support ongoing quality improvement according to the priorities for the service.
- Use to: Ensure healthcare services are providing quality colonoscopy services in line with the requirements of the Colonoscopy Clinical Care Standard.
- Useful for: health service organisations, clinicians.
Launch of Colonoscopy Clinical Care Standard and Atlas Focus Report webinar
An expert panel discussion from the launch of the Colonoscopy Clinical Care Standard and Atlas Focus Report at the World Congress of Gastroenterology at Australian Gastroenterology Week 2025 conference.
- Use to: Understand the impact of the Colonoscopy Clinical Care Standard, ongoing disparity in access and the challenges in communication and information across the health system.
- Useful for: clinicians, policy makers.
Informed Consent - Fact sheet for clinicians
Ensuring informed consent is properly obtained is a legal, ethical and professional requirement on the part of all treating health professionals and supports person-centred care.
- Use to: Improve communication with patients on informed consent.
- Useful for: clinicians.
Colonoscopy Referral Information - fact sheet and referral template
A fact sheet and referral template outlining key components of a comprehensive referral, as described in Quality Statement 1 of the Colonoscopy Clinical Care Standard (2025).
- Use to: Ensure referrals for colonoscopies are comprehensive and complete.
- Useful for: referring clinicians, colonoscopy services and specialists.
Better Decisions
Better Decisions
Better decisions involve making choices that are patient-centred and considers individual values, preferences and circumstances. It involves engaging in shared decision-making, where clinicians and patients work together to provide care that best meets the patient’s needs and goals.
Better shared decision-making can address unwarranted clinical variation by making information available to patients about the range of treatment options and ensuring that patients consider the risks and benefits of each treatment, enabling them to make an informed choice about their care.
Guidance, tools and resources
Ask, Share, Know
A practical guide that will help consumers make shared decisions with their health professionals.
- Use to: Help improve your conversation with your health professional when asking about tests, treatment and care options. This can help you to make the treatment decision that is right for you.
- Useful for: patients, carers.
Information for consumers - Colonoscopy Clinical Care Standard
Describes the care that you can expect if you are having a colonoscopy.
- Use to: Understand what the standard contains and what care you should expect to receive if you are having a colonoscopy.
- Useful for: patients, carers.
Bowel cancer: How to reduce your risk
Describes actions that patients can take to reduce their risk of bowel cancer.
- Use to: Make healthy choices to help reduce your risk of bowel cancer.
- Useful for: patients, carers.
Better Monitoring
Better Monitoring
Better monitoring means continually measuring and refining quality improvement activities to improve the quality of care and reduce unwarranted clinical variation.
Measurement is fundamental to providing better care, as meaningful indicators are required to assess the effectiveness of quality improvement initiatives and guide decision-making. By routinely measuring how care is delivered and where it differs, we can see where clinical variation is occurring, but identification of variation is only the first step, further investigation and action at a local level is essential to make sure data on clinical variation leads to better care.
Guidance and tools
Colonoscopy CCS indicators
A set of indicators have been developed to support your local quality improvement activity.
- Use to: Monitor how health service organisations are implementing the care recommended in the Colonoscopy Clinical Care Standard.
- Useful for: health service organisations, Safety and Quality Managers, hospital managers, clinicians.
Better Networks
Better Networks
Better networks mean bringing people together with common interests and goals to learn, share and support efforts to reduce unwarranted clinical variation. Through these networks, clinicians can collaborate and apply shared learnings to promote stewardship of resources and reduce duplication of work.
Networks can address unwarranted clinical variation by providing a platform for sharing evidence, experiences and best practice. This supports the standardisation of care and ensures patients receive consistent and high-quality care regardless of where they are being treated.
Communities of practice/Networks
Gastroenterological Society of Australia (GESA)
GESA is a peak membership organisation for Australian healthcare professionals and researchers working in the fields of gastroenterology and hepatology.
- Use to: Bring together gastroenterology and hepatology health professionals in focus areas such as sustainability, private practice and more.
- Useful for: clinicians.
Case studies
Colonoscopy - Strengthening foundations for auditing and oversight in colonoscopy care
A short notice accreditation assessment found monitoring of clinical variation needed strengthening. Northern NSW Local Health District had 60 days to improve its monitoring and reporting processes, before the next follow-up assessment. They took stock and set about building a stronger, data-driven system that is supported by clinicians - starting with some innovative changes to their audit tool.
Explore more hubs
Chronic obstructive pulmonary disease (COPD)

Heavy menstrual bleeding